-
Cord Colitis Syndrome
Wikipedia
"Cord colitis syndrome: a cause of granulomatous inflammation in the upper and lower gastrointestinal tract" . ... "Sequence-based discovery of Bradyrhizobium enterica in cord colitis syndrome" . The New England Journal of Medicine . 369 (6): 517–28. doi : 10.1056/nejmoa1211115 . ... "Sequence-based discovery of Bradyrhizobium enterica in cord colitis syndrome" . The New England Journal of Medicine . 369 (6): 517–28. doi : 10.1056/nejmoa1211115 . ... "Sequence-Based Discovery of Novel Bacteria, Bradyrhizobium Enterica, in Cord Colitis Syndrome" . New England Journal of Medicine . 369 (6): 517–528. doi : 10.1056/NEJMoa1211115 . ... "Bradyrhizobium enterica in Cord Colitis Syndrome". The New England Journal of Medicine . 369 (19): 1866–7. doi : 10.1056/NEJMc1311318 .
-
Cole-Carpenter Syndrome
Wikipedia
Cole-Carpenter syndrome Autosomal recessive pattern is the inheritance manner of this condition Specialty Medical genetics Cole-Carpenter syndrome is a rare autosomal recessive medical condition in humans. [1] It is characterised by dysmorphic features and a tendency to fractures. ... It is made by sequencing the P4HB, SEC24D and CRTAP genes. [ citation needed ] Differential diagnosis [ edit ] Pfeiffer syndrome Osteogenesis imperfecta Osteoglophonic dwarfism Treatment [ edit ] There is no specific treatment for this condition currently known and management of its various features is the norm. [ citation needed ] History [ edit ] This condition was first described in 1987. [1] References [ edit ] ^ a b Cole DEC, Carpenter, TO (1987) Bone fragility, craniosynostosis, ocular proptosis, hydrocephalus, and distinctive facial features: a newly recognized type of osteogenesis imperfecta. J Pediat 110: 76-80 ^ Rauch F, Fahiminiya S, Majewski J, Carrot-Zhang J, Boudko S, Glorieux F, Mort JS, Bächinger HP, Moffatt P (2015) Cole-Carpenter syndrome is caused by a heterozygous missense mutation in P4HB. Am J Hum Genet 96(3):425-431. doi: 10.1016/j.ajhg.2014.12.027 ^ Garbes L, Kim K, Rieß A, Hoyer-Kuhn H, Beleggia F, Bevot A, Kim MJ, Huh YH, Kweon HS, Savarirayan R, Amor D, Kakadia PM, Lindig T, Kagan KO, Becker J, Boyadjiev SA, Wollnik B, Semler O, Bohlander SK9, Kim J13, Netzer C (2015) Mutations in SEC24D, encoding a component of the COPII machinery, cause a syndromic form of osteogenesis imperfecta. ... Epub 2015 Feb 12. ^ Balasubramanian M, Pollitt RC, Chandler KE, Mughal MZ, Parker MJ, Dalton A, Arundel P, Offiah AC, Bishop NJ (2015) CRTAP mutation in a patient with Cole-Carpenter syndrome. Am J Med Genet A 167A(3):587-91. doi: 10.1002/ajmg.a.36916 Classification D OMIM : 112240 MeSH : C535963 C535963, C535963
-
Pediatric Acute-Onset Neuropsychiatric Syndrome
Wikipedia
Pediatric acute-onset neuropsychiatric syndrome Specialty Neuroimmunology Pediatric acute-onset neuropsychiatric syndrome ( PANS ) [1] is a disorder characterized by the sudden onset of obsessive-compulsive (OCD) symptoms or eating restrictions, concomitant with acute behavioral deterioration and/or motor/sensory changes in at least two of seven domains. [1] Those domains are anxiety, emotional lability and/or depression, irritability, aggressive or oppositional behavior, academic decline, cognitive decline, and sleep disruption. [1] The diagnosis necessitates a course that follows a relapsing–remitting pattern. ... "Clinical evaluation of youth with pediatric acute-onset neuropsychiatric syndrome (PANS): recommendations from the 2013 PANS Consensus Conference" . ... "Overview of Treatment of Pediatric Acute-Onset Neuropsychiatric Syndrome" . J Child Adolesc Psychopharmacol . 27 (7): 562–565. doi : 10.1089/cap.2017.0042 . ... "CANS: Childhood acute neuropsychiatric syndromes". Eur J Paediatr Neurol (Review). 22 (2): 316–320. doi : 10.1016/j.ejpn.2018.01.011 . ... "Clinical Management of Pediatric Acute-Onset Neuropsychiatric Syndrome: Part I-Psychiatric and Behavioral Interventions" .
-
Syringobulbia
Wikipedia
External links [ edit ] Classification D ICD - 10 : G95.0 ICD - 9-CM : 336.0 DiseasesDB : 12764 External resources eMedicine : neuro/359 14-182d. at Merck Manual of Diagnosis and Therapy Professional Edition v t e Focal lesions of the spinal cord General Myelopathy Myelitis Spinal cord compression By location Brown-Séquard syndrome Posterior cord syndrome Anterior cord syndrome Central cord syndrome Cauda equina syndrome Other Polio Demyelinating disease Transverse myelitis Tropical spastic paraparesis Epidural abscess Syringomyelia Syringobulbia Morvan's syndrome Sensory ataxia Tabes dorsalis Abadie's sign Subacute combined degeneration of spinal cord Vascular myelopathy Anterior spinal artery syndrome Foix–Alajouanine syndrome v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis This article related to pathology is a stub .
-
Cubitus Valgus
Wikipedia
{{cn} When present at birth, it can be an indication of Turner syndrome [1] or Noonan syndrome . It can also be acquired through fracture or other trauma. ... External links [ edit ] Image (congenital) Classification D ICD - 10 : M21.0 , Q74.0 ICD - 9-CM : 736.01 , 755.59 DiseasesDB : 29423 v t e Acquired musculoskeletal deformities Upper limb shoulder Winged scapula Adhesive capsulitis Rotator cuff tear Subacromial bursitis elbow Cubitus valgus Cubitus varus hand deformity Wrist drop Boutonniere deformity Swan neck deformity Mallet finger Lower limb hip Protrusio acetabuli Coxa valga Coxa vara leg Unequal leg length patella Luxating patella Chondromalacia patellae Patella baja Patella alta foot deformity Bunion/hallux valgus Hallux varus Hallux rigidus Hammer toe Foot drop Flat feet Club foot knee Genu recurvatum Head Cauliflower ear General terms Valgus deformity / Varus deformity Joint stiffness Ligamentous laxity v t e Congenital malformations and deformations of musculoskeletal system / musculoskeletal abnormality Appendicular limb / dysmelia Arms clavicle / shoulder Cleidocranial dysostosis Sprengel's deformity Wallis–Zieff–Goldblatt syndrome hand deformity Madelung's deformity Clinodactyly Oligodactyly Polydactyly Leg hip Hip dislocation / Hip dysplasia Upington disease Coxa valga Coxa vara knee Genu valgum Genu varum Genu recurvatum Discoid meniscus Congenital patellar dislocation Congenital knee dislocation foot deformity varus Club foot Pigeon toe valgus Flat feet Pes cavus Rocker bottom foot Hammer toe Either / both fingers and toes Polydactyly / Syndactyly Webbed toes Arachnodactyly Cenani–Lenz syndactylism Ectrodactyly Brachydactyly Stub thumb reduction deficits / limb Acheiropodia Ectromelia Phocomelia Amelia Hemimelia multiple joints Arthrogryposis Larsen syndrome RAPADILINO syndrome Axial Skull and face Craniosynostosis Scaphocephaly Oxycephaly Trigonocephaly Craniofacial dysostosis Crouzon syndrome Hypertelorism Hallermann–Streiff syndrome Treacher Collins syndrome other Macrocephaly Platybasia Craniodiaphyseal dysplasia Dolichocephaly Greig cephalopolysyndactyly syndrome Plagiocephaly Saddle nose Vertebral column Spinal curvature Scoliosis Klippel–Feil syndrome Spondylolisthesis Spina bifida occulta Sacralization Thoracic skeleton ribs : Cervical Bifid sternum : Pectus excavatum Pectus carinatum This article about a disease of musculoskeletal and connective tissue is a stub .
-
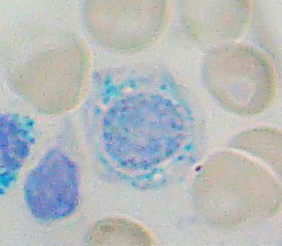
Sideroblastic Anemia
Wikipedia
The disorder may be caused either by a genetic disorder or indirectly as part of myelodysplastic syndrome , [2] which can develop into hematological malignancies (especially acute myeloid leukemia ). ... The autosomal recessive form is typically severe in presentation. Genetic syndromes: Rarely, sideroblastic anemia may be part of a congenital syndrome and present with associated findings, such as ataxia , myopathy , and pancreatic insufficiency . Acquired clonal sideroblastic anemia Clonal sideroblastic anemias fall under the broader category of myelodysplastic syndromes (MDS). Three forms exist and include refractory anemia with ringed sideroblasts (RARS), refractory anemia with ringed sideroblasts and thrombocytosis (RARS-T), and refractory cytopenia with multilineage dysplasia and ringed sideroblasts (RCMD-RS). ... PMID 18698088 . ^ Sideroblastic Anemias: Anemias Caused by Deficient Erythropoiesis at Merck Manual of Diagnosis and Therapy Professional Edition ^ " Sideroblast " at Dorland's Medical Dictionary [ dead link ] ^ Mufti, GJ; Bennett, JM; Goasguen, J; Bain, BJ; Baumann, I; Brunning, R; Cazzola, M; Fenaux, P; Germing, U; Hellström-Lindberg, E; Jinnai, I; Manabe, A; Matsuda, A; Niemeyer, CM; Sanz, G; Tomonaga, M; Vallespi, T; Yoshimi, A; International Working Group on Morphology of Myelodysplastic, Syndrome (Nov 2008). "Diagnosis and classification of myelodysplastic syndrome: International Working Group on Morphology of myelodysplastic syndrome (IWGM-MDS) consensus proposals for the definition and enumeration of myeloblasts and ring sideroblasts" . ... External links [ edit ] Classification D ICD - 10 : D64.0 - D64.3 ICD - 9-CM : 285.0 OMIM : 301310 206000 300751 MeSH : D000756 DiseasesDB : 12110 GeneReviews/NCBI/NIH/UW entry on X-Linked Sideroblastic Anemia and Ataxia v t e Diseases of red blood cells ↑ Polycythemia Polycythemia vera ↓ Anemia Nutritional Micro- : Iron-deficiency anemia Plummer–Vinson syndrome Macro- : Megaloblastic anemia Pernicious anemia Hemolytic (mostly normo- ) Hereditary enzymopathy : Glucose-6-phosphate dehydrogenase deficiency glycolysis pyruvate kinase deficiency triosephosphate isomerase deficiency hexokinase deficiency hemoglobinopathy : Thalassemia alpha beta delta Sickle cell disease / trait Hereditary persistence of fetal hemoglobin membrane : Hereditary spherocytosis Minkowski–Chauffard syndrome Hereditary elliptocytosis Southeast Asian ovalocytosis Hereditary stomatocytosis Acquired AIHA Warm antibody autoimmune hemolytic anemia Cold agglutinin disease Donath–Landsteiner hemolytic anemia Paroxysmal cold hemoglobinuria Mixed autoimmune hemolytic anemia membrane paroxysmal nocturnal hemoglobinuria Microangiopathic hemolytic anemia Thrombotic microangiopathy Hemolytic–uremic syndrome Drug-induced autoimmune Drug-induced nonautoimmune Hemolytic disease of the newborn Aplastic (mostly normo- ) Hereditary : Fanconi anemia Diamond–Blackfan anemia Acquired: Pure red cell aplasia Sideroblastic anemia Myelophthisic Blood tests Mean corpuscular volume normocytic microcytic macrocytic Mean corpuscular hemoglobin concentration normochromic hypochromic Other Methemoglobinemia Sulfhemoglobinemia Reticulocytopenia v t e Myeloid -related hematological malignancy CFU-GM / and other granulocytes CFU-GM Myelocyte AML : Acute myeloblastic leukemia M0 M1 M2 APL/M3 MP Chronic neutrophilic leukemia Monocyte AML AMoL/M5 Myeloid dendritic cell leukemia CML Philadelphia chromosome Accelerated phase chronic myelogenous leukemia Myelomonocyte AML M4 MD-MP Juvenile myelomonocytic leukemia Chronic myelomonocytic leukemia Other Histiocytosis CFU-Baso AML Acute basophilic CFU-Eos AML Acute eosinophilic MP Chronic eosinophilic leukemia / Hypereosinophilic syndrome MEP CFU-Meg MP Essential thrombocytosis Acute megakaryoblastic leukemia CFU-E AML Erythroleukemia/M6 MP Polycythemia vera MD Refractory anemia Refractory anemia with excess of blasts Chromosome 5q deletion syndrome Sideroblastic anemia Paroxysmal nocturnal hemoglobinuria Refractory cytopenia with multilineage dysplasia CFU-Mast Mastocytoma Mast cell leukemia Mast cell sarcoma Systemic mastocytosis Mastocytosis : Diffuse cutaneous mastocytosis Erythrodermic mastocytosis Adult type of generalized eruption of cutaneous mastocytosis Urticaria pigmentosa Mast cell sarcoma Solitary mastocytoma Systemic mastocytosis Xanthelasmoidal mastocytosis Multiple/unknown AML Acute panmyelosis with myelofibrosis Myeloid sarcoma MP Myelofibrosis Acute biphenotypic leukaemia v t e X-linked disorders X-linked recessive Immune Chronic granulomatous disease (CYBB) Wiskott–Aldrich syndrome X-linked severe combined immunodeficiency X-linked agammaglobulinemia Hyper-IgM syndrome type 1 IPEX X-linked lymphoproliferative disease Properdin deficiency Hematologic Haemophilia A Haemophilia B X-linked sideroblastic anemia Endocrine Androgen insensitivity syndrome / Spinal and bulbar muscular atrophy KAL1 Kallmann syndrome X-linked adrenal hypoplasia congenita Metabolic Amino acid : Ornithine transcarbamylase deficiency Oculocerebrorenal syndrome Dyslipidemia : Adrenoleukodystrophy Carbohydrate metabolism : Glucose-6-phosphate dehydrogenase deficiency Pyruvate dehydrogenase deficiency Danon disease/glycogen storage disease Type IIb Lipid storage disorder : Fabry's disease Mucopolysaccharidosis : Hunter syndrome Purine–pyrimidine metabolism : Lesch–Nyhan syndrome Mineral : Menkes disease / Occipital horn syndrome Nervous system X-linked intellectual disability : Coffin–Lowry syndrome MASA syndrome Alpha-thalassemia mental retardation syndrome Siderius X-linked mental retardation syndrome Eye disorders: Color blindness (red and green, but not blue) Ocular albinism ( 1 ) Norrie disease Choroideremia Other: Charcot–Marie–Tooth disease (CMTX2-3) Pelizaeus–Merzbacher disease SMAX2 Skin and related tissue Dyskeratosis congenita Hypohidrotic ectodermal dysplasia (EDA) X-linked ichthyosis X-linked endothelial corneal dystrophy Neuromuscular Becker's muscular dystrophy / Duchenne Centronuclear myopathy (MTM1) Conradi–Hünermann syndrome Emery–Dreifuss muscular dystrophy 1 Urologic Alport syndrome Dent's disease X-linked nephrogenic diabetes insipidus Bone / tooth AMELX Amelogenesis imperfecta No primary system Barth syndrome McLeod syndrome Smith–Fineman–Myers syndrome Simpson–Golabi–Behmel syndrome Mohr–Tranebjærg syndrome Nasodigitoacoustic syndrome X-linked dominant X-linked hypophosphatemia Focal dermal hypoplasia Fragile X syndrome Aicardi syndrome Incontinentia pigmenti Rett syndrome CHILD syndrome Lujan–Fryns syndrome Orofaciodigital syndrome 1 Craniofrontonasal dysplasia v t e Genetic disorder , membrane: ABC-transporter disorders ABCA ABCA1 ( Tangier disease ) ABCA3 ( Surfactant metabolism dysfunction 3 ) ABCA4 ( Stargardt disease 1 , Retinitis pigmentosa 19 ) ABCA12 ( Harlequin-type ichthyosis , Lamellar ichthyosis 2 ) ABCB ABCB4 ( Progressive familial intrahepatic cholestasis 3 ) ABCB7 ( ASAT ) ABCB11 ( Progressive familial intrahepatic cholestasis 2 ) ABCC ABCC2 ( Dubin–Johnson syndrome ) ABCC6 ( Pseudoxanthoma elasticum ) ABCC7 ( Cystic fibrosis ) ABCC8 ( HHF1 , TNDM2 ) ABCC9 ( Dilated cardiomyopathy 1O ) ABCD ABCD1 ( Adrenoleukodystrophy , Adrenomyeloneuropathy ) ABCG ABCG5 ( Sitosterolemia ) ABCG8 ( Gallbladder disease 4, Sitosterolemia ) see also ABC transporters
-
Chromosome 16p13.3 Deletion Syndrome
Gard
Chromosome 16p13.3 deletion syndrome is a chromosome abnormality that can affect many parts of the body. ... Although once thought to be a severe form of Rubinstein-Taybi syndrome , it is now emerging as a unique syndrome.
-
16p13.11 Microduplication Syndrome
Orphanet
16p13.11 microduplication syndrome is a recently described syndrome associated with variable clinical features including behavioral abnormalities, developmental delay, congenital heart defects and skeletal anomalies. ... Skeletal manifestations include hypermobility, craniosynostosis and polydactyly. Etiology This syndrome is caused by interstitial duplications encompassing 16p13.11.
-
Karak Syndrome
Wikipedia
Karak syndrome Specialty Neurology Karak syndrome is a neurological degenerative disorder involving excess cerebral iron accumulation. [1] The family who the disease was discovered in their siblings lived in Karak , a town in southern Jordan . [1] It is characterized by ataxia , inverted feet ( talipes calcaneovarus ), dysarthric scanning speech with dystonic features , dystonic movement of the tongue and facial muscles and choreiform movement was present in both upper and lower limbs , being more marked in the lower limbs, along with dystonic posture of the distal feet , bradykinesia present in both upper and lower limbs, dysmetria , dysdiadochokinesia , and intentional tremor were bilateral and symmetrical. [1] See also [ edit ] Neurodegeneration with brain iron accumulation Iron overload References [ edit ] ^ a b c Mubaidin A, Roberts E, Hampshire D, et al. (July 2003). "Karak syndrome: a novel degenerative disorder of the basal ganglia and cerebellum" .
-
15q13.3 Microduplication Syndrome
Gard
15q13.3 microduplication syndrome is a rare chromosomal disorder. ... People with 15q13.3 microduplication syndrome have an extra piece of genetic information on the long arm (q arm) of chromosome 15 . ... Other people may have developmental delay, intellectual disability, communication difficulties, behavioral and psychiatric problems (such as autistic features, emotional instability, attention-deficit hyperactivity disorder (ADHD), schizophrenia), feeding problems, difficulty sleeping ( insomnia ), low muscular tone (hypotonia) and seizures. Some people with this syndrome also have cleft palate. The duplication contains the CHRNA7 gene, which is believed to cause the the behavioral abnormalities and the cleft palate.
-
Amniotic Band Syndrome
Gard
Amniotic band syndrome refers to a condition in which bands develop from the inner lining of the amnion . ... The extrinsic theory states that amniotic band syndrome occurs due to factors found outside of the developing baby (externally); the intrinsic theory states that amniotic band syndrome occurs due to factors found within the baby (internally).
-
Heimler Syndrome 2
Omim
A number sign (#) is used with this entry because of evidence that Heimler syndrome-2 (HMLR2) is caused by compound heterozygous mutation in the PEX6 gene (601498) on chromosome 6p21. Description Heimler syndrome, which represents the mildest end of the peroxisomal biogenesis disorder spectrum (see PBD1A, 214100), is a rare autosomal recessive disorder characterized by sensorineural hearing loss, enamel hypoplasia of the secondary dentition, and nail abnormalities (Ratbi et al., 2015). For a discussion of genetic heterogeneity of Heimler syndrome, see HMLR1 (234580). Clinical Features Ong et al. (2006) reported monozygotic twin girls who both had mild clubfeet at birth that responded to orthotics. ... Molecular Genetics In 2 sisters from the UK with Heimler syndrome, Ratbi et al. (2015) performed whole-exome sequencing and identified compound heterozygosity for missense mutations in the PEX6 gene, P274L (601498.0010) and R644W (601498.0011). Sanger sequencing of the PEX1 (602136) and PEX6 genes in the monozygotic twin girls with Heimler syndrome who were originally reported by Ong et al. (2006) revealed compound heterozygosity for a frameshift (601498.0012) and a missense mutation (R601Q; 601498.0013) in the PEX6 gene.
-
Spondyloepimetaphyseal Dysplasia, Pakistani Type
Wikipedia
Other features that may form part of the syndrome include precocious costal calcification, small iliac bones , short femoral necks , coxa vara , short halluces and fused vertebral bodies. ... External links [ edit ] Classification D OMIM : 612847 v t e Lysosomal storage diseases : Inborn errors of carbohydrate metabolism ( Mucopolysaccharidoses ) Catabolism MPS I Hurler Syndrome , Hurler-Scheie Syndrome , Scheie Syndrome MPS II: Hunter Syndrome MPS III: Sanfilippo Syndrome MPS IV: Morquio Syndrome MPS VI: Maroteaux-Lamy Syndrome MPS VII: Sly Syndrome MPS IX: Hyaluronidase deficiency
-
Heel Pad Syndrome
Wikipedia
Heel pad syndrome Other names Heel fat pad syndrome, heel pad atrophy, heel fat pad atrophy Specialty Podiatry Heel pad syndrome is a pain that occurs in the center of the heel. [1] It is typically due to atrophy of the fat pad which makes up the heel. ... Diagnosis [ edit ] The main differential diagnosis of heel pad syndrome is plantar fasciitis . In heel pad syndrome all parts of the heel are tender while in plantar fasciitis typically only the part of the heel closer to the toes is sore. [2] Treatment [ edit ] Manual therapy and exercise have better efficacy in the long term than electrophysical agents and exercise for function, but not for pain. [3] Manual therapy and exercise are preferably focused at stretching the plantar fascia . [4] [ why? ... ISBN 9781416022077 . ^ Rasoulian, McElfresh, Elliott, Rodriguez. "Heel Fat Pad Syndrome - A Clinical Management Guideline" (PDF) .
-
Intraventricular Block
Wikipedia
PMID 5284231 . v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever This article about a medical condition affecting the circulatory system is a stub .
-
Bainbridge-Ropers Syndrome
Wikipedia
Bainbridge Ropers syndrome Bainbridge-Ropers syndrome is inherited in an autosomal dominant manner Specialty Medical genetics Bainbridge-Ropers syndrome is a very rare genetic disorder characterized by abnormalities including severe psychomotor development, feeding problems, severe postnatal growth delays, intellectual disabilities, and skeletal abnormalities. Contents 1 Signs and symptoms 2 Genetics 3 Diagnosis 3.1 Differential diagnosis 4 Treatment 5 History 6 References 7 External links Signs and symptoms [ edit ] Morphological features of this syndrome include: Arched eyebrows Anteverted nares Ulnar deviation of the hands Microcephaly Skeletal abnormalities, such as a “barrel chest”, extremely high arched palate Crowded teeth Hypotelorism (wide-set eyes) Scoliosis Genetics [ edit ] This condition is caused by a mutation in the ASXL3 gene, which is considered a de novo mutation . ... Differential diagnosis [ edit ] Bohring-Opitz syndrome Treatment [ edit ] There is no currently known treatment or cure for this condition. ... "De novo truncating mutations in ASXL3 are associated with a novel clinical phenotype with similarities to Bohring-Opitz syndrome" . Genome Medicine . 5 (2): 11. doi : 10.1186/gm415 .
-
Atrial Enlargement
Wikipedia
It can also affect both atria. [1] Types include: Left atrial enlargement Right atrial enlargement References [ edit ] ^ "ECG Learning Center - An introduction to clinical electrocardiography" . library.med.utah.edu . v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever This cardiovascular system article is a stub .
-
Serrated Polyposis Syndrome
Wikipedia
Serrated polyposis syndrome Other names Hyperplastic polyposis syndrome (former) Specialty Gastroenterology Symptoms Asymptomatic Complications Colorectal cancer (15-30%) [1] Usual onset 55 years of age (average) [2] Types Distal and proximal Causes Environmental and genetic factors Risk factors Smoking , Lymphoma [3] Diagnostic method Colonoscopy Treatment Surveillance colonoscopy Polypectomy Surgery Frequency 0.03 - 0.5%. [1] Serrated polyposis syndrome ( SPS ), previously known as hyperplastic polyposis syndrome, is a disorder characterized by the appearance of serrated polyps in the colon. ... However, most individuals with the syndrome do not have an associated germline mutation . ... "High prevalence of advanced colorectal neoplasia and serrated polyposis syndrome in Hodgkin lymphoma survivors" . ... PMID 31520728 . ^ a b c d e f g h i Dekker, E; Bleijenberg, A; Balaguer, F; Dutch-Spanish-British Serrated Polyposis Syndrome, collaboration. (May 2020). "Update on the World Health Organization Criteria for Diagnosis of Serrated Polyposis Syndrome" . ... "Extracolonic cancer risk in patients with serrated polyposis syndrome and their first-degree relatives".
-
Morvan's Syndrome
Wikipedia
Morvan's syndrome Specialty Neurology Symptoms Morvan's fibrillary chorea Morvan's syndrome is a rare, life-threatening autoimmune disease named after the nineteenth century French physician Augustin Marie Morvan . ... Raised serum levels of antibodies to VGKCs have been reported in three patients with Morvan's Syndrome. Binding of serum from a patient with Morvan's Syndrome to the hippocampus in a similar pattern of antibodies to known VGKC suggest that these antibodies can also cause CNS dysfunction. ... "Agrypnia Excitata: a generalized overactivity syndrome and a useful concept in the neurophysiopathology of sleep". ... Immunotherapy-reversed compulsive, monoaminergic, circadian rhythm disorder in Morvan syndrome. Neurology. 2008 9;71:2008-10. ^ a b c d e f Bajaj, B.K.; S. ... "An interesting case report of Morvan's syndrome from the Indian subcontinent" .
-
Recessive Intellectual Disability-Motor Dysfunction-Multiple Joint Contractures Syndrome
Orphanet
Recessive intellectual disability-motor dysfunction-multiple joint contractures syndrome is a rare, genetic, syndromic intellectual disabilty disorder characterized by severe intellectual disability, progressive, postnatal, multiple joint contractures and severe motor dysfunction.