-
Abdominal Obesity-Metabolic Syndrome 3
Omim
A number sign (#) is used with this entry because of evidence that abdominal obesity-metabolic syndrome-3 (AOMS3) is caused by heterozygous mutation in the DYRK1B gene (604556) on chromosome 19q13. For a general phenotypic description and a discussion of genetic heterogeneity of abdominal obesity-metabolic syndrome, see 605552. Clinical Features Keramati et al. (2014) studied 3 large multigenerational families from a community in southwest Iran in which 25 affected members had early-onset myocardial infarction or coronary artery disease as well as central obesity, type 2 diabetes, and hypertension, a constellation of features that met the standard definition of metabolic syndrome. ... Molecular Genetics Keramati et al. (2014) performed whole-exome sequencing in the probands from 2 of 3 multigenerational Iranian families with metabolic syndrome and early-onset coronary artery disease and identified a heterozygous missense mutation in the DYRK1B gene (R102C; 604556.0001) that segregated with disease in all 3 families. ... DNA samples from family members of 1 of the patients showed a consistent pattern of cosegregation of the mutation with features of metabolic syndrome in an autosomal dominant fashion. ... He et al. (2014) noted that the R102C mutation induces increased expression of PPARG (601487) and PGC1A (604517), which are associated with plasma levels of adipokines that play crucial roles in the metabolic syndrome, including adiponectin (605441), leptin (164160), resistin (605565), and FGF21 (609436).
-
Otophyma
Wikipedia
You can help Wikipedia by expanding it . v t e v t e Disorders of skin appendages Nail thickness: Onychogryphosis Onychauxis color: Beau's lines Yellow nail syndrome Leukonychia Azure lunula shape: Koilonychia Nail clubbing behavior: Onychotillomania Onychophagia other: Ingrown nail Anonychia ungrouped: Paronychia Acute Chronic Chevron nail Congenital onychodysplasia of the index fingers Green nails Half and half nails Hangnail Hapalonychia Hook nail Ingrown nail Lichen planus of the nails Longitudinal erythronychia Malalignment of the nail plate Median nail dystrophy Mees' lines Melanonychia Muehrcke's lines Nail–patella syndrome Onychoatrophy Onycholysis Onychomadesis Onychomatricoma Onychomycosis Onychophosis Onychoptosis defluvium Onychorrhexis Onychoschizia Platonychia Pincer nails Plummer's nail Psoriatic nails Pterygium inversum unguis Pterygium unguis Purpura of the nail bed Racquet nail Red lunulae Shell nail syndrome Splinter hemorrhage Spotted lunulae Staining of the nail plate Stippled nails Subungual hematoma Terry's nails Twenty-nail dystrophy Hair Hair loss / Baldness noncicatricial alopecia : Alopecia areata totalis universalis Ophiasis Androgenic alopecia (male-pattern baldness) Hypotrichosis Telogen effluvium Traction alopecia Lichen planopilaris Trichorrhexis nodosa Alopecia neoplastica Anagen effluvium Alopecia mucinosa cicatricial alopecia : Pseudopelade of Brocq Central centrifugal cicatricial alopecia Pressure alopecia Traumatic alopecia Tumor alopecia Hot comb alopecia Perifolliculitis capitis abscedens et suffodiens Graham-Little syndrome Folliculitis decalvans ungrouped: Triangular alopecia Frontal fibrosing alopecia Marie Unna hereditary hypotrichosis Hypertrichosis Hirsutism Acquired localised generalised patterned Congenital generalised localised X-linked Prepubertal Acneiform eruption Acne Acne vulgaris Acne conglobata Acne miliaris necrotica Tropical acne Infantile acne / Neonatal acne Excoriated acne Acne fulminans Acne medicamentosa (e.g., steroid acne ) Halogen acne Iododerma Bromoderma Chloracne Oil acne Tar acne Acne cosmetica Occupational acne Acne aestivalis Acne keloidalis nuchae Acne mechanica Acne with facial edema Pomade acne Acne necrotica Blackhead Lupus miliaris disseminatus faciei Rosacea Perioral dermatitis Granulomatous perioral dermatitis Phymatous rosacea Rhinophyma Blepharophyma Gnathophyma Metophyma Otophyma Papulopustular rosacea Lupoid rosacea Erythrotelangiectatic rosacea Glandular rosacea Gram-negative rosacea Steroid rosacea Ocular rosacea Persistent edema of rosacea Rosacea conglobata variants Periorificial dermatitis Pyoderma faciale Ungrouped Granulomatous facial dermatitis Idiopathic facial aseptic granuloma Periorbital dermatitis SAPHO syndrome Follicular cysts " Sebaceous cyst " Epidermoid cyst Trichilemmal cyst Steatocystoma simplex multiplex Milia Inflammation Folliculitis Folliculitis nares perforans Tufted folliculitis Pseudofolliculitis barbae Hidradenitis Hidradenitis suppurativa Recurrent palmoplantar hidradenitis Neutrophilic eccrine hidradenitis Ungrouped Acrokeratosis paraneoplastica of Bazex Acroosteolysis Bubble hair deformity Disseminate and recurrent infundibulofolliculitis Erosive pustular dermatitis of the scalp Erythromelanosis follicularis faciei et colli Hair casts Hair follicle nevus Intermittent hair–follicle dystrophy Keratosis pilaris atropicans Kinking hair Koenen's tumor Lichen planopilaris Lichen spinulosus Loose anagen syndrome Menkes kinky hair syndrome Monilethrix Parakeratosis pustulosa Pili ( Pili annulati Pili bifurcati Pili multigemini Pili pseudoannulati Pili torti ) Pityriasis amiantacea Plica neuropathica Poliosis Rubinstein–Taybi syndrome Setleis syndrome Traumatic anserine folliculosis Trichomegaly Trichomycosis axillaris Trichorrhexis ( Trichorrhexis invaginata Trichorrhexis nodosa ) Trichostasis spinulosa Uncombable hair syndrome Wooly hair nevus Sweat glands Eccrine Miliaria Colloid milium Miliaria crystalline Miliaria profunda Miliaria pustulosa Miliaria rubra Occlusion miliaria Postmiliarial hypohidrosis Granulosis rubra nasi Ross’ syndrome Anhidrosis Hyperhidrosis Generalized Gustatory Palmoplantar Apocrine Body odor Chromhidrosis Fox–Fordyce disease Sebaceous Sebaceous hyperplasia
-
Metophyma
Wikipedia
You can help Wikipedia by expanding it . v t e v t e Disorders of skin appendages Nail thickness: Onychogryphosis Onychauxis color: Beau's lines Yellow nail syndrome Leukonychia Azure lunula shape: Koilonychia Nail clubbing behavior: Onychotillomania Onychophagia other: Ingrown nail Anonychia ungrouped: Paronychia Acute Chronic Chevron nail Congenital onychodysplasia of the index fingers Green nails Half and half nails Hangnail Hapalonychia Hook nail Ingrown nail Lichen planus of the nails Longitudinal erythronychia Malalignment of the nail plate Median nail dystrophy Mees' lines Melanonychia Muehrcke's lines Nail–patella syndrome Onychoatrophy Onycholysis Onychomadesis Onychomatricoma Onychomycosis Onychophosis Onychoptosis defluvium Onychorrhexis Onychoschizia Platonychia Pincer nails Plummer's nail Psoriatic nails Pterygium inversum unguis Pterygium unguis Purpura of the nail bed Racquet nail Red lunulae Shell nail syndrome Splinter hemorrhage Spotted lunulae Staining of the nail plate Stippled nails Subungual hematoma Terry's nails Twenty-nail dystrophy Hair Hair loss / Baldness noncicatricial alopecia : Alopecia areata totalis universalis Ophiasis Androgenic alopecia (male-pattern baldness) Hypotrichosis Telogen effluvium Traction alopecia Lichen planopilaris Trichorrhexis nodosa Alopecia neoplastica Anagen effluvium Alopecia mucinosa cicatricial alopecia : Pseudopelade of Brocq Central centrifugal cicatricial alopecia Pressure alopecia Traumatic alopecia Tumor alopecia Hot comb alopecia Perifolliculitis capitis abscedens et suffodiens Graham-Little syndrome Folliculitis decalvans ungrouped: Triangular alopecia Frontal fibrosing alopecia Marie Unna hereditary hypotrichosis Hypertrichosis Hirsutism Acquired localised generalised patterned Congenital generalised localised X-linked Prepubertal Acneiform eruption Acne Acne vulgaris Acne conglobata Acne miliaris necrotica Tropical acne Infantile acne / Neonatal acne Excoriated acne Acne fulminans Acne medicamentosa (e.g., steroid acne ) Halogen acne Iododerma Bromoderma Chloracne Oil acne Tar acne Acne cosmetica Occupational acne Acne aestivalis Acne keloidalis nuchae Acne mechanica Acne with facial edema Pomade acne Acne necrotica Blackhead Lupus miliaris disseminatus faciei Rosacea Perioral dermatitis Granulomatous perioral dermatitis Phymatous rosacea Rhinophyma Blepharophyma Gnathophyma Metophyma Otophyma Papulopustular rosacea Lupoid rosacea Erythrotelangiectatic rosacea Glandular rosacea Gram-negative rosacea Steroid rosacea Ocular rosacea Persistent edema of rosacea Rosacea conglobata variants Periorificial dermatitis Pyoderma faciale Ungrouped Granulomatous facial dermatitis Idiopathic facial aseptic granuloma Periorbital dermatitis SAPHO syndrome Follicular cysts " Sebaceous cyst " Epidermoid cyst Trichilemmal cyst Steatocystoma simplex multiplex Milia Inflammation Folliculitis Folliculitis nares perforans Tufted folliculitis Pseudofolliculitis barbae Hidradenitis Hidradenitis suppurativa Recurrent palmoplantar hidradenitis Neutrophilic eccrine hidradenitis Ungrouped Acrokeratosis paraneoplastica of Bazex Acroosteolysis Bubble hair deformity Disseminate and recurrent infundibulofolliculitis Erosive pustular dermatitis of the scalp Erythromelanosis follicularis faciei et colli Hair casts Hair follicle nevus Intermittent hair–follicle dystrophy Keratosis pilaris atropicans Kinking hair Koenen's tumor Lichen planopilaris Lichen spinulosus Loose anagen syndrome Menkes kinky hair syndrome Monilethrix Parakeratosis pustulosa Pili ( Pili annulati Pili bifurcati Pili multigemini Pili pseudoannulati Pili torti ) Pityriasis amiantacea Plica neuropathica Poliosis Rubinstein–Taybi syndrome Setleis syndrome Traumatic anserine folliculosis Trichomegaly Trichomycosis axillaris Trichorrhexis ( Trichorrhexis invaginata Trichorrhexis nodosa ) Trichostasis spinulosa Uncombable hair syndrome Wooly hair nevus Sweat glands Eccrine Miliaria Colloid milium Miliaria crystalline Miliaria profunda Miliaria pustulosa Miliaria rubra Occlusion miliaria Postmiliarial hypohidrosis Granulosis rubra nasi Ross’ syndrome Anhidrosis Hyperhidrosis Generalized Gustatory Palmoplantar Apocrine Body odor Chromhidrosis Fox–Fordyce disease Sebaceous Sebaceous hyperplasia
-
Blepharophyma
Wikipedia
ISBN 0-07-138076-0 . v t e Disorders of skin appendages Nail thickness: Onychogryphosis Onychauxis color: Beau's lines Yellow nail syndrome Leukonychia Azure lunula shape: Koilonychia Nail clubbing behavior: Onychotillomania Onychophagia other: Ingrown nail Anonychia ungrouped: Paronychia Acute Chronic Chevron nail Congenital onychodysplasia of the index fingers Green nails Half and half nails Hangnail Hapalonychia Hook nail Ingrown nail Lichen planus of the nails Longitudinal erythronychia Malalignment of the nail plate Median nail dystrophy Mees' lines Melanonychia Muehrcke's lines Nail–patella syndrome Onychoatrophy Onycholysis Onychomadesis Onychomatricoma Onychomycosis Onychophosis Onychoptosis defluvium Onychorrhexis Onychoschizia Platonychia Pincer nails Plummer's nail Psoriatic nails Pterygium inversum unguis Pterygium unguis Purpura of the nail bed Racquet nail Red lunulae Shell nail syndrome Splinter hemorrhage Spotted lunulae Staining of the nail plate Stippled nails Subungual hematoma Terry's nails Twenty-nail dystrophy Hair Hair loss / Baldness noncicatricial alopecia : Alopecia areata totalis universalis Ophiasis Androgenic alopecia (male-pattern baldness) Hypotrichosis Telogen effluvium Traction alopecia Lichen planopilaris Trichorrhexis nodosa Alopecia neoplastica Anagen effluvium Alopecia mucinosa cicatricial alopecia : Pseudopelade of Brocq Central centrifugal cicatricial alopecia Pressure alopecia Traumatic alopecia Tumor alopecia Hot comb alopecia Perifolliculitis capitis abscedens et suffodiens Graham-Little syndrome Folliculitis decalvans ungrouped: Triangular alopecia Frontal fibrosing alopecia Marie Unna hereditary hypotrichosis Hypertrichosis Hirsutism Acquired localised generalised patterned Congenital generalised localised X-linked Prepubertal Acneiform eruption Acne Acne vulgaris Acne conglobata Acne miliaris necrotica Tropical acne Infantile acne / Neonatal acne Excoriated acne Acne fulminans Acne medicamentosa (e.g., steroid acne ) Halogen acne Iododerma Bromoderma Chloracne Oil acne Tar acne Acne cosmetica Occupational acne Acne aestivalis Acne keloidalis nuchae Acne mechanica Acne with facial edema Pomade acne Acne necrotica Blackhead Lupus miliaris disseminatus faciei Rosacea Perioral dermatitis Granulomatous perioral dermatitis Phymatous rosacea Rhinophyma Blepharophyma Gnathophyma Metophyma Otophyma Papulopustular rosacea Lupoid rosacea Erythrotelangiectatic rosacea Glandular rosacea Gram-negative rosacea Steroid rosacea Ocular rosacea Persistent edema of rosacea Rosacea conglobata variants Periorificial dermatitis Pyoderma faciale Ungrouped Granulomatous facial dermatitis Idiopathic facial aseptic granuloma Periorbital dermatitis SAPHO syndrome Follicular cysts " Sebaceous cyst " Epidermoid cyst Trichilemmal cyst Steatocystoma simplex multiplex Milia Inflammation Folliculitis Folliculitis nares perforans Tufted folliculitis Pseudofolliculitis barbae Hidradenitis Hidradenitis suppurativa Recurrent palmoplantar hidradenitis Neutrophilic eccrine hidradenitis Ungrouped Acrokeratosis paraneoplastica of Bazex Acroosteolysis Bubble hair deformity Disseminate and recurrent infundibulofolliculitis Erosive pustular dermatitis of the scalp Erythromelanosis follicularis faciei et colli Hair casts Hair follicle nevus Intermittent hair–follicle dystrophy Keratosis pilaris atropicans Kinking hair Koenen's tumor Lichen planopilaris Lichen spinulosus Loose anagen syndrome Menkes kinky hair syndrome Monilethrix Parakeratosis pustulosa Pili ( Pili annulati Pili bifurcati Pili multigemini Pili pseudoannulati Pili torti ) Pityriasis amiantacea Plica neuropathica Poliosis Rubinstein–Taybi syndrome Setleis syndrome Traumatic anserine folliculosis Trichomegaly Trichomycosis axillaris Trichorrhexis ( Trichorrhexis invaginata Trichorrhexis nodosa ) Trichostasis spinulosa Uncombable hair syndrome Wooly hair nevus Sweat glands Eccrine Miliaria Colloid milium Miliaria crystalline Miliaria profunda Miliaria pustulosa Miliaria rubra Occlusion miliaria Postmiliarial hypohidrosis Granulosis rubra nasi Ross’ syndrome Anhidrosis Hyperhidrosis Generalized Gustatory Palmoplantar Apocrine Body odor Chromhidrosis Fox–Fordyce disease Sebaceous Sebaceous hyperplasia This cutaneous condition article is a stub .
-
Foal Immunodeficiency Syndrome
Wikipedia
Foal immunodeficiency syndrome (FIS), originally known as Fell pony syndrome , mainly affects two breeds of ponies: the Fell and Dales . ... "Screening for foal immunodeficiency syndrome". The Veterinary Record . 169 (25): 653–4. doi : 10.1136/vr.d8118 . PMID 22184351 . ^ a b c Scholes, SF; Holliman, A; May, PD; Holmes, MA (7 February 1998). "A syndrome of anaemia, immunodeficiency and peripheral ganglionopathy in Fell pony foals". ... "Foal immunodeficiency syndrome: carrier testing has markedly reduced disease incidence". ... PMID 23486505 . ^ "Foal immunodeficiency syndrome (FIS)" . www.animalgenetics.us .
-
Vasoplegic Syndrome
Wikipedia
Vasoplegic syndrome ( VPS ) is a postperfusion syndrome characterized by low systemic vascular resistance and a high cardiac output . ... "Is incidence of postoperative vasoplegic syndrome different between off-pump and on-pump coronary artery bypass grafting surgery?" ... "[Study of mechanism of vasoplegic syndrome for open heart surgery]". Zhonghua Yi Xue Za Zhi (in Chinese). 82 (2): 127–30. ... "Critical Care | Full text | Vasoplegic syndrome after cardiopulmonary bypass surgery – associated factors and clinical outcomes: a nested case-control study" . ... PMID 18473936 . ^ Gomes WJ, Carvalho AC, Palma JH, Gonçalves Júnior I, Buffolo E (1994). "[Vasoplegic syndrome: a new dilemma]". Rev Assoc Med Bras . 40 (4): 304.
-
Atelosteogenesis, Type Ii
Wikipedia
National Library of Medicine Further reading [ edit ] GeneReviews/NCBI/NIH/UW entry on Atelosteogenesis Type 2, McAlister Dysplasia, de la Chapelle Dysplasia OMIM entries on Atelosteogenesis Type 2 External links [ edit ] Classification D ICD - 10 : Q77.5 OMIM : 256050 MeSH : C535395 DiseasesDB : 33349 External resources Orphanet : 56304 v t e Osteochondrodysplasia Osteodysplasia/ / osteodystrophy Diaphysis Camurati–Engelmann disease Metaphysis Metaphyseal dysplasia Jansen's metaphyseal chondrodysplasia Schmid metaphyseal chondrodysplasia Epiphysis Spondyloepiphyseal dysplasia congenita Multiple epiphyseal dysplasia Otospondylomegaepiphyseal dysplasia Osteosclerosis Raine syndrome Osteopoikilosis Osteopetrosis Other/ungrouped FLNB Boomerang dysplasia Opsismodysplasia Polyostotic fibrous dysplasia McCune–Albright syndrome Chondrodysplasia / chondrodystrophy (including dwarfism ) Osteochondroma osteochondromatosis Hereditary multiple exostoses Chondroma / enchondroma enchondromatosis Ollier disease Maffucci syndrome Growth factor receptor FGFR2 : Antley–Bixler syndrome FGFR3 : Achondroplasia Hypochondroplasia Thanatophoric dysplasia COL2A1 collagen disease Achondrogenesis type 2 Hypochondrogenesis SLC26A2 sulfation defect Achondrogenesis type 1B Autosomal recessive multiple epiphyseal dysplasia Atelosteogenesis, type II Diastrophic dysplasia Chondrodysplasia punctata Rhizomelic chondrodysplasia punctata Conradi–Hünermann syndrome Other dwarfism Fibrochondrogenesis Short rib – polydactyly syndrome Majewski's polydactyly syndrome Léri–Weill dyschondrosteosis v t e Genetic disorder , membrane: Solute carrier disorders 1-10 SLC1A3 Episodic ataxia 6 SLC2A1 De Vivo disease SLC2A5 Fructose malabsorption SLC2A10 Arterial tortuosity syndrome SLC3A1 Cystinuria SLC4A1 Hereditary spherocytosis 4 / Hereditary elliptocytosis 4 SLC4A11 Congenital endothelial dystrophy type 2 Fuchs' dystrophy 4 SLC5A1 Glucose-galactose malabsorption SLC5A2 Renal glycosuria SLC5A5 Thyroid dyshormonogenesis type 1 SLC6A19 Hartnup disease SLC7A7 Lysinuric protein intolerance SLC7A9 Cystinuria 11-20 SLC11A1 Crohn's disease SLC12A3 Gitelman syndrome SLC16A1 HHF7 SLC16A2 Allan–Herndon–Dudley syndrome SLC17A5 Salla disease SLC17A8 DFNA25 21-40 SLC26A2 Multiple epiphyseal dysplasia 4 Achondrogenesis type 1B Recessive multiple epiphyseal dysplasia Atelosteogenesis, type II Diastrophic dysplasia SLC26A4 Pendred syndrome SLC35C1 CDOG 2C SLC39A4 Acrodermatitis enteropathica SLC40A1 African iron overload see also solute carrier family
-
Glomerulonephritis
Wikipedia
This inflammation typically results in one or both of the nephrotic or nephritic syndromes . [2] : 500 Nephrotic syndrome [ edit ] Main article: Nephrotic syndrome The nephrotic syndrome is characterised by the finding of edema in a person with increased protein in the urine and decreased protein in the blood , with increased fat in the blood . ... Minimal change disease typically presents with edema , an increase in proteins passed from urine and decrease in blood protein levels, and an increase in circulating lipids (i.e., nephrotic syndrome ) and is the most common cause of the nephrotic syndrome in children. ... It is likely to present as a nephrotic syndrome. This form of glomerulonephritis may be associated with conditions such as HIV and heroin abuse, or inherited as Alport syndrome . ... These forms present with the nephritic syndrome , hypocomplementemia , and have a poor prognosis. ... ISBN 978-0-7020-3084-0 . ^ The Nephrotic Syndrome Stephan R. Orth, M.D., and Eberhard Ritz, M.D.AGT, IL1B, ADM, CCL1, PPARG, CCL7, WT1, FAS, TNF, NPHS1, ALB, CCL2, IL10, IL6, COL4A3, CXCL8, CCL5, IL2, IL18, IL2RA, NGF, IFNG, JUND, MIR10B, MIR100, CCL4, CCL3, ESR1, POMC, CFD, DES, CXCR3, ACE, MMP9, C3, SERPINE1, MMP1, AGTR1, PDGFB, PDGFD, APOE, FOS, GAS6, SPP1, PTAFR, GJA5, PRF1, CX3CR1, COL3A1, RGS2, MMP3, ITGB1, AXL, LTBP1, LTC4S, AGTR2, AIF1, ITGB3, SMAD1, ALOX5AP, ALOX15, ANXA5, TBXAS1, ITGA3, RNLS, PLEKHA7, CX3CL1, C6, MS4A1, FBN1, CD59, VHL, CFHR5, APOL1, KIF1B, ITGB4, SDHAF2, FH, MUC1, TPRKB, MPO, MDH2, PLEC, COQ2, RASGRP1, MAX, CFI, DLST, FAH, CLCN5, SDHA, SDHB, LAGE3, SDHC, SLC25A11, SDHD, RET, TP53RK, CASP10, ELP1, IGAN1, CD81, LMX1B, C4A, WDR19, DGKE, FASLG, TMEM127, OSGEP, PRKCD, TGFB1, CFH, VEGFA, BCL2, THY1, IL17A, TLR3, REN, COL4A5, FCGR3B, PLA2R1, PLB1, PRTN3, MYH9, SPG7, IL4, FOXP3, YWHAZ, MMP2, PLA2G1B, IGHA1, CST3, CRP, FCAR, TLR9, CD46, PPARA, TNFRSF1B, TGM2, TLR4, UCHL1, SYK, PLG, SCGB1A1, PON1, MEFV, TRIM21, MIF, SELE, TNFRSF6B, CCN3, NOS3, MYD88, PADI4, RUNX1, CSF3, CD74, HGF, HLA-DRB1, NLRP3, CDKN2A, ICAM1, DDR1, ACKR2, FN1, CR1, IL1A, SMUG1, TLR7, CD40LG, ALOX5, CXCL10, CTLA4, CCN2, APCS, ITGAM, ITGB2, CXCR4, PAGR1, DHX40, MTSS2, NPHS2, FGF23, IKBKG, CNDP1, COL18A1, CD276, FOXP2, BAP1, ITGA8, CHP1, EGLN3, MIR146A, LOC102724971, LOC102723407, PGR-AS1, TLR5, C20orf181, HNP1, HSP90B1, UBC, WG, RHOV, DBA2, UMOD, VCAM1, LAYN, POC5, EMB, RBM45, VIM, C1GALT1, ZMYM2, SRR, PDE5A, PDGFC, ANKRD1, CERT1, HAVCR1, GREM1, PAMR1, EIF1, DIANPH, CDK2AP2, TNIP1, IL17RA, CADM1, IKZF1, MYL9, TLR1, ANP32B, CABIN1, HPSE, CIC, SUB1, RPP14, MMRN1, IKZF3, SIGLEC7, HPLH1, HHAT, NR2E3, OTUB1, KHSRP, PSIP1, BECN1, RNPC3, TNFSF13, SF3B6, DTL, IRAK4, EXOSC3, IGK, IL22, CD274, PER2, SPHK1, LAMTOR2, TAAR5, USP2, SLC33A1, CD163, THEMIS2, ABCA1, PDGFRB, TIMP1, FLII, ATN1, HBEGF, EGF, ELANE, EPHX2, ERBB2, ERN1, ETV6, FCGR2A, FCGR3A, FHL1, FOXD1, FLI1, FOSB, DDIT3, GAST, GALNS, GDNF, GLP1R, CXCL1, HCLS1, HLA-A, HLA-DQB1, HMGB1, HRAS, HSPA5, IFNA1, IFNA2, DNASE1, DCN, THBD, C5AR1, ACTN4, ADAM10, AHCY, ABCD1, AKR1B1, ART1, ATD, ATM, ATR, TNFRSF17, BRAF, SERPING1, C3AR1, C9, CYP2B6, CAST, CASP1, CD28, CD38, CD40, CD48, CD79A, CCR4, CCR6, CNN1, CP, CUX1, CYBB, IFNA13, IGF1, IKBKB, SELL, MAPK1, MAP2K7, MASP1, RARA, PLAAT4, BRD2, RPS27A, S100A8, S100A9, S100A10, SERPINB3, CCL13, CCL22, SELP, IL1RN, SLAMF1, SLC5A1, SLC5A2, SNRPA, STAT1, STAT3, STAT4, TAGLN, MAP3K7, TCF3, TFRC, TGFB1I1, TGFBR2, PKN1, PRKCA, SERPINA1, ABCB1, IL2RB, IL13, IRF5, ISG20, ITGA2, JUN, JUNB, KIT, LOX, SH2D1A, SMAD3, DNAJB9, KITLG, CXCL9, MIP, MMP11, MMP12, MSN, NEO1, NEUROG1, NTRK1, NTS, TNFRSF11B, P2RX7, P2RY2, PCNA, ACR, H3P8
-
Chromosome 9p Deletion Syndrome
Omim
A number sign (#) is used with this entry because it represents a contiguous gene deletion syndrome. Also see chromosome 9p24.3 deletion syndrome (154230), which results in 46,XY gonadal dysgenesis. ... The clinical features fitted well with the previously described 9p- syndrome based on patients with more extensive deletions. ... Shashi et al. (1994) described choanal atresia in a patient with the 9p- syndrome; Huret et al. (1988) had earlier reported the association in a single case. Swinkels et al. (2008) reported 13 presumably unrelated Dutch patients with 9p syndrome. Ages ranged from 3 months to 42 years; there were 8 females and 5 males. ... The combined data indicated that the critical region for the 9p deletion syndrome mapped to a 4 to 6-Mb region in 9p23-p22 between D9S286 to D9S285.
-
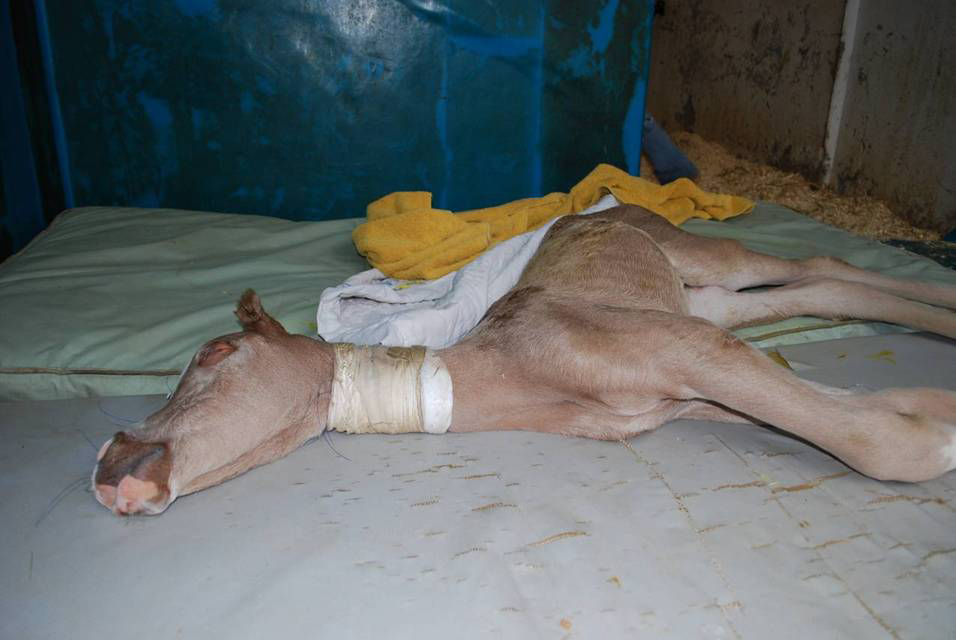
Lavender Foal Syndrome
Wikipedia
A foal with lavender foal syndrome exhibiting opisthotonus , a common clinical sign of the disorder Lavender foal syndrome ( LFS ), also called coat color dilution lethal ( CCDL ), is an autosomal recessive genetic disease that affects newborn foals of certain Arabian horse bloodlines. ... PMID 20419149 . ^ a b "01 Lavender Foal Syndrome - VeterinaryPartner.com - a VIN company!" ... "The carrier prevalence of severe combined immunodeficiency, lavender foal syndrome and cerebellar abiotrophy in Arabian horses in South Africa" (PDF) . ... "Coat Color Dilution Lethal ("lavender foal syndrome"): A Tetany Condition of Arabian Foals" (PDF) . ... Archived from the original (PDF) on 2009-12-19. ^ "Lavender Foal Syndrome (LFS)/Coat Color Dilution Lethal (CCDL)" (PDF) .
-
Genodermatosis
Wikipedia
Specialty Dermatology , Medical genetics Causes Family history; gene mutation; chromosome abnormality Genodermatosis is a hereditary skin disease with three inherited modes including single gene inheritance, multiple gene inheritance and chromosome inheritance. [1] There are many different types of genodermatosis, the prevalence of genodermatosis ranges from 1 per 6000 people to 1 per 500,000 people. [2] Genodermatosis has influence on the texture, color and structure of skin cuticle and connective tissue, specific lesion site and clinical manifestations on the body vary depending on the type. [3] In the spite of the variety and complexity of genodermatosis, there are still some common methods that can help people diagnose. [4] After diagnosis, different types of genodermatosis require different levels of therapy including interventions, nursing interventions and treatments. [5] Among that, research of therapy for some new, complex and rare types are still in the developing stage. [6] The impact of genodermatosis not only can be seen in body but also can be seen in all aspects of patients’ life, including but not limited to psychological, family life, economic conditions and social activities. [5] [7] Accordingly, the patients need treatment, support and help in these areas. [5] Contents 1 Hereditary Modes 1.1 Single gene (Monogenic) 1.1.1 Autosomal dominant inheritance 1.1.2 Autosomal recessive inheritance 1.1.3 X-linked dominant inheritance 1.1.4 X-linked recessive inheritance 1.2 Multiple gene (Polygenic) 1.3 Chromosome 2 Types 2.1 Common types 2.1.1 Ichthyosis 2.2 Rare types 2.2.1 Michelin tyre baby syndrome 2.2.2 Epidermolysis bullosa 2.2.3 Pachyonychia congenita 2.2.4 Epidermolytic palmoplantar keratoderma 2.2.5 Hereditary benign intraepithelial dyskeratosis 2.2.6 Epidermolytic hyperkeratosis 2.2.7 Hidrotic ectodermal dysplasia 3 Diagnostic Methods 4 Therapy 4.1 Prevention and Care 4.1.1 Ichthyosis 4.1.2 Epidermolysis bullosa 4.1.3 Epidermolytic hyperkeratosis 4.1.4 Pachyonychia congenita 4.1.5 Neurofibromatosis type I 4.2 Therapeutic Methods 5 Effects 6 See also 7 References 8 External links Hereditary Modes [ edit ] Genodermatosis is inherited in three modes: single gene inheritance, multiple gene inheritance and chromosome inheritance. [1] Single gene (Monogenic) [ edit ] Single gene inheritance of genodermatosis refers to the inheritance of a skin disease caused by one genetic abnormality and single gene heredity is divided into four kinds mainly. [2] Autosomal dominant inheritance [ edit ] The first kind is autosomal dominant inheritance, in this kind of inheritance, patients can be of any sex and their genodermatosis are often inherited from one of the parents. [2] Cases of skin disease that may be inherited in this kind of mode include epidermolysis bullosa simplex (EBS), acute intermittent porphyrin, white sponge nevus , ichthyosis , epidermolytic palmoplantar keratoderma, hereditary benign intraepithelial dyskeratosis and so on. [1] [2] [8] [9] Autosomal recessive inheritance [ edit ] The second kind is autosomal recessive inheritance, in this kind of inheritance, patients can be of any sex and inbreeding tends to lead to this inheritance. [2] Cases of skin disease that may be inherited in this kind of mode include epidermolysis bullosa , xeroderma pigmentosum , acrodermatitis enteropathica , ichthyosis and so on. [1] [2] X-linked dominant inheritance [ edit ] The third kind is X-linked dominant inheritance, in this kind of inheritance, patients can be of any sex. [2] Male patients can pass the disease on to their sons and the chances of female patients passing it to their daughters or sons are almost equal. [2] Cases of skin disease that may be inherited in this kind of mode include incontinentia pigmenti , focal dermal hypoplasia and so on. [1] [8] X-linked recessive inheritance [ edit ] The last kind is X-linked recessive inheritance, in this kind of inheritance, patients can be of any sex and the prevalence in men is higher than that in women. [2] Male patients cannot pass the disease on to their sons. [2] Cases of skin disease that may be inherited in this kind of mode include fabry disease , anhidrotic ectodermal dysplasia , dyskeratosis congenita and so on. [1] [2] Multiple gene (Polygenic) [ edit ] Multiple gene inheritance of genodermatosis refers to the inheritance of a skin disease caused by multiple genetic abnormalities. [2] Cases of skin disease that may be inherited in this mode include vitiligo , psoriasis , pemphigus vulgaris , systemic lupus erythematosus and so on. [2] [8] Chromosome [ edit ] Chromosome inheritance of genodermatosis refers to the inheritance of a skin disease caused by chromosome abnormality. ... Common types [ edit ] Ichthyosis [ edit ] Ichthyosis refers mainly to ichthyosis vulgaris , a common genodermatosis, people with this disease have a fishy, dry skin, which usually appears in early childhood and may disappear in adulthood. [10] The prevalence of ichthyosis vulgaris is high, affecting almost 1 per 250 people. [11] There are also rare types of ichthyosis, such as epidermolytic hyperkeratosis, harlequin ichthyosis and so on. [8] Rare types [ edit ] Michelin tyre baby syndrome [ edit ] Michelin tyre baby syndrome is a rare genodermatosis that occurs at birth, the skin of the patients is stacked symmetrically in layers like the image of the Michelin tyre’s mascot, which is also how this disease got its name. [12] Epidermolysis bullosa [ edit ] Epidermolysis bullosa is a rare type of genodermatosis, people with this disease have blisters on their skin and this disease is never completely cured for a lifetime. [13] Epidermolysis bullosa is mainly subdivided into four types: dystrophic epidermolysis bullosa , epidermolysis bullosa simplex, junctional epidermolysis bullosa and kindler syndrome . [13] Almost 1 in 50,000 people has epidermolysis bullosa. [14] Pachyonychia congenita [ edit ] Dystrophic epidermolysis bullosa Epidermolytic hyperkeratosis Hidrotic ectodermal dysplasia Pachyonychia congenita is a rare type of genodermatosis, its clinical manifestations are abnormal enlargement of fingernails or toenails, excessive or poor palmoplantar keratinization, excessive sweating in the palmar or the plantar. [15] Between 5000 and 10000 people in the world suffer from pachyonychia congenita. [16] Epidermolytic palmoplantar keratoderma [ edit ] Epidermolytic palmoplantar keratoderma often appears at birth and it is almost impossible to be cured completely. [9] The clinical manifestations of this disease include excessive palmoplantar keratinization, the palmar or plantar become yellow divergently with around the edges or abnormally excessive sweating and clinical manifestation appear in a symmetrical form on the body. [9] Hereditary benign intraepithelial dyskeratosis [ edit ] Hereditary benign intraepithelial dyskeratosis is a rare type of genodermatosis that may occur in infancy and early childhood, its symptoms often appear in the patients’ eyes and mouths. [17] The patients’ eyes appear red due to the dilatation of superficial vessels and appearance of conjunctival plaques in their eyes, patients may have variable-size, thick, soft and white plaques in their mouth. [17] Spring is an acute episode of symptoms, such as itching, erythema, photophobia and so on. [17] Epidermolytic hyperkeratosis [ edit ] Epidermolytic hyperkeratosis is a rare genodermatosis which is also referred to as disorder of cornification type 3 and bullous congenital ichthyosiform erthroderma, affecting almost 1 per 200,000 - 300,000 people. [18] They also stated that its clinical manifestations often begin at birth with large rashes all over the body, and the patients’ skin will be so sensitive that even mild wounds can cause blisters and peeling. Potential complications of this disease include electrolyte disturbances , sepsis and so on. [18] Hidrotic ectodermal dysplasia [ edit ] Hidrotic ectodermal dysplasia is a rare genodermatosis which is also known as Clouston syndrome. The patients’ nails may be too thick, too brittle, too bent or have different colors, their hair also appear mottled, sparse and other abnormalities. [19] These symptoms often begin when the patient is an infant. [19] Diagnostic Methods [ edit ] Genodermatosis is often rare and varied, but diagnostic methods have some commonalities, the diagnosis of rare genodermatosis is basically divided into six steps: 1. ... ProQuest 68849936 . ^ a b National Center for Advancing Translational Sciences. (2020). Clouston syndrome. Retrieved from https://rarediseases.info.nih.gov/diseases/2056/clouston-syndrome ^ a b c d e f g Silverberg, Nanette (July 2020). ... External links [ edit ] Classification D MeSH : D012873 SNOMED CT : 239001006 v t e Congenital malformations and deformations of integument / skin disease Genodermatosis Congenital ichthyosis / erythrokeratodermia AD Ichthyosis vulgaris AR Congenital ichthyosiform erythroderma : Epidermolytic hyperkeratosis Lamellar ichthyosis Harlequin-type ichthyosis Netherton syndrome Zunich–Kaye syndrome Sjögren–Larsson syndrome XR X-linked ichthyosis Ungrouped Ichthyosis bullosa of Siemens Ichthyosis follicularis Ichthyosis prematurity syndrome Ichthyosis–sclerosing cholangitis syndrome Nonbullous congenital ichthyosiform erythroderma Ichthyosis linearis circumflexa Ichthyosis hystrix EB and related EBS EBS-K EBS-WC EBS-DM EBS-OG EBS-MD EBS-MP JEB JEB-H Mitis Generalized atrophic JEB-PA DEB DDEB RDEB related: Costello syndrome Kindler syndrome Laryngoonychocutaneous syndrome Skin fragility syndrome Ectodermal dysplasia Naegeli syndrome / Dermatopathia pigmentosa reticularis Hay–Wells syndrome Hypohidrotic ectodermal dysplasia Focal dermal hypoplasia Ellis–van Creveld syndrome Rapp–Hodgkin syndrome / Hay–Wells syndrome Elastic / Connective Ehlers–Danlos syndromes Cutis laxa ( Gerodermia osteodysplastica ) Popliteal pterygium syndrome Pseudoxanthoma elasticum Van der Woude syndrome Hyperkeratosis / keratinopathy PPK diffuse : Diffuse epidermolytic palmoplantar keratoderma Diffuse nonepidermolytic palmoplantar keratoderma Palmoplantar keratoderma of Sybert Meleda disease syndromic connexin Bart–Pumphrey syndrome Clouston's hidrotic ectodermal dysplasia Vohwinkel syndrome Corneodermatoosseous syndrome plakoglobin Naxos syndrome Scleroatrophic syndrome of Huriez Olmsted syndrome Cathepsin C Papillon–Lefèvre syndrome Haim–Munk syndrome Camisa disease focal : Focal palmoplantar keratoderma with oral mucosal hyperkeratosis Focal palmoplantar and gingival keratosis Howel–Evans syndrome Pachyonychia congenita Pachyonychia congenita type I Pachyonychia congenita type II Striate palmoplantar keratoderma Tyrosinemia type II punctate : Acrokeratoelastoidosis of Costa Focal acral hyperkeratosis Keratosis punctata palmaris et plantaris Keratosis punctata of the palmar creases Schöpf–Schulz–Passarge syndrome Porokeratosis plantaris discreta Spiny keratoderma ungrouped: Palmoplantar keratoderma and spastic paraplegia desmoplakin Carvajal syndrome connexin Erythrokeratodermia variabilis HID / KID Other Meleda disease Keratosis pilaris ATP2A2 Darier's disease Dyskeratosis congenita Lelis syndrome Dyskeratosis congenita Keratolytic winter erythema Keratosis follicularis spinulosa decalvans Keratosis linearis with ichthyosis congenita and sclerosing keratoderma syndrome Keratosis pilaris atrophicans faciei Keratosis pilaris Other cadherin EEM syndrome immune system Hereditary lymphedema Mastocytosis / Urticaria pigmentosa Hailey–Hailey see also Template:Congenital malformations and deformations of skin appendages , Template:Phakomatoses , Template:Pigmentation disorders , Template:DNA replication and repair-deficiency disorder Developmental anomalies Midline Dermoid cyst Encephalocele Nasal glioma PHACE association Sinus pericranii Nevus Capillary hemangioma Port-wine stain Nevus flammeus nuchae Other/ungrouped Aplasia cutis congenita Amniotic band syndrome Branchial cyst Cavernous venous malformation Accessory nail of the fifth toe Bronchogenic cyst Congenital cartilaginous rest of the neck Congenital hypertrophy of the lateral fold of the hallux Congenital lip pit Congenital malformations of the dermatoglyphs Congenital preauricular fistula Congenital smooth muscle hamartoma Cystic lymphatic malformation Median raphe cyst Melanotic neuroectodermal tumor of infancy Mongolian spot Nasolacrimal duct cyst Omphalomesenteric duct cyst Poland anomaly Rapidly involuting congenital hemangioma Rosenthal–Kloepfer syndrome Skin dimple Superficial lymphatic malformation Thyroglossal duct cyst Verrucous vascular malformation BirthmarkFYN, COL7A1, KRT10, DUH1, FLCN, ECM1, IKBKG, ATP2A2, KRT1, USB1, ADAR, KRT9, KRT5, PKP1, POMP, EBP, ADA, MBTPS2, SLC29A3, DSP, TRPV3, KRT14, FOXP3, SASH1, SPINK5, UBL5, FERMT1, SLURP1, CHST8, SUV39H2, HSDL1, GJB4, TMC8, FLG2, GJB6, TGM1, ABCB6, GJB2, BRAF, CDSN, CTSC, COL17A1, DSG1, EDA, ERCC2, GJA1, GJB3, HAND2, IGFBP3, ITGA6, ITGB4, KRT16, PTCH1, FZD6, CRLF1, SNAP29, GTF2H5
-
Thyrocerebrorenal Syndrome
Orphanet
A rare syndromic renal disorder characterized by renal, neurologic and thyroid disease, associated with thrombocytopenia.
-
Otofacial Syndrome
Wikipedia
Unsourced or poorly sourced material may be challenged and removed . Find sources: "Otofacial syndrome" – news · newspapers · books · scholar · JSTOR ( July 2018 ) Otofacial syndrome Specialty Oral and maxillofacial surgeon Otofacial syndrome is an extraordinarily rare congenital deformity in which a person is born without a mandible , and, consequently, without a chin . ... Retrieved 2008-12-19 . v t e Congenital malformations and deformations of face and neck Face jaw : Otocephaly mouth : Macrostomia Microstomia lip : Macrocheilia Microcheilia chin : Microgenia multiple/other: Hallermann–Streiff syndrome Branchial cleft cyst Neck Webbed neck Ungrouped Preauricular sinus and cyst This article about a congenital malformation is a stub .
-
Palipraxia
Wikipedia
Palipraxia is a rare complex tic involving the involuntary repetition of one's own movements. [1] It is associated with Tourette syndrome [1] [2] and may be associated with epilepsy . [3] References [ edit ] ^ a b Ludolph AG, Roessner V, Münchau A, Müller-Vahl K (November 2012). "Tourette syndrome and other tic disorders in childhood, adolescence and adulthood" . ... "Are there distinct subtypes in Tourette syndrome? Pure-Tourette syndrome versus Tourette syndrome-plus, and simple versus complex tics" . ... Epilepsia . 50 (6): 1616–9. doi : 10.1111/j.1528-1167.2008.01980.x . PMID 19175395 . v t e Tourette syndrome Main Causes and origins History Societal and cultural aspects Management Terms Coprolalia Copropraxia Echolalia Echophenomenon Echopraxia Palilalia Palipraxia PANDAS Premonitory urge Sensory phenomena Tic Tic disorder Tourettism People Jean-Martin Charcot Donald J. ... Shapiro Organizations Tourette Association of America Tourette Canada Tourettes Action Yale Child Study Center Media Front of the Class Hichki I Have Tourette's but Tourette's Doesn't Have Me John's Not Mad " Le Petit Tourette " Maze Motherless Brooklyn Quit It The Secret Life of Lele Pons The Tic Code Tic Talk: Living with Tourette Syndrome This article about a medical condition affecting the nervous system is a stub .
-
Traumatic Neuroma
Wikipedia
External links [ edit ] Classification D ICD - 10 : T87.3 ICD - 9-CM : 950 - 957 ICD-O : M9570/0 v t e Neurotrauma Traumatic brain injury Intracranial hemorrhage Intra-axial Intraparenchymal hemorrhage Intraventricular hemorrhage Extra-axial Subdural hematoma Epidural hematoma Subarachnoid hemorrhage Brain herniation Cerebral contusion Cerebral laceration Concussion Post-concussion syndrome Second-impact syndrome Dementia pugilistica Chronic traumatic encephalopathy Diffuse axonal injury Abusive head trauma Penetrating head injury Spinal cord injury Anterior spinal artery syndrome Brown-Séquard syndrome Cauda equina syndrome Central cord syndrome Paraplegia Posterior cord syndrome Spinal cord injury without radiographic abnormality Tetraplegia (Quadriplegia) Peripheral nerves Nerve injury Peripheral nerve injury classification Wallerian degeneration Injury of accessory nerve Brachial plexus injury Traumatic neuroma This article about a medical condition affecting the nervous system is a stub .
-
Illum Syndrome
Omim
Clinical Features Illum et al. (1988) reported 3 sibs and Schrander-Stumpel et al. (1991) reported 3 unrelated patients with a lethal syndrome of arthrogryposis multiplex congenita with whistling face. ... The presumed autosomal recessive inheritance as well as the phenotypic differences excludes the Freeman-Sheldon form of whistling face syndrome (193700). A recessive form of whistling face syndrome has been proposed; see 277720. ... Chong et al. (2015) suggested that the patients reported by Schrander-Stumpel et al. (1991) and Di Rocco et al. (1992) had CLIFAHDD (616266) rather than Illum syndrome. They suspected that these patients likely had mutations in the NALCN gene (611549).
-
Aprosencephaly Syndrome
Omim
Townes et al. (1988) suggested that the XK aprosencephaly syndrome may be an autosomal recessive disorder. ... Renzetti et al. (2005) reported a girl with XK syndrome born to Libyan parents. She had a sloping forehead, microphthalmia, beaked nose, absent right thumb, and cutaneous syndactyly of toes 2 and 3. ... Renzetti et al. (2005) reviewed the literature concerning XK syndrome and commented on the clinical variability and heterogeneity of the disorder. ... Nomenclature Lurie et al. (1979) coined the term 'aprosencephaly' and suggested the designation 'XK aprosencephaly syndrome,' with 'X' referring to the unknown surname of the patient described by Garcia and Duncan (1977) and 'K' to the surname of their patient.
-
Frontoocular Syndrome
Omim
Clinical Features Schneider et al. (2000) reported a mother and her 2 daughters with an apparently novel syndrome including the features of trigonocephaly due to coronal and metopic craniosynostosis, hypotelorism, proptosis, ptosis, epicanthal folds, hypoplastic supraorbital ridges, elevated nasal bridge, thin philtrum, high-arched palate, and a narrow bifrontal region. ... The authors called the disorder frontoocular syndrome. Descartes and Franklin (2004) described a second case of mother and daughter with frontoocular syndrome. ... Inheritance Schneider et al. (2000) suggested that the frontoocular syndrome is an autosomal dominant condition, but could not rule out the possibility of X-linked dominant inheritance.
-
Enamel-Renal Syndrome
Wikipedia
Unsourced material may be challenged and removed. Find sources: "Enamel-renal syndrome" – news · newspapers · books · scholar · JSTOR ( December 2018 ) ( Learn how and when to remove this template message ) ( Learn how and when to remove this template message ) Enamel-Renal syndrome Autosomal recessive pattern is the inheritance manner of this condition Specialty Gastroenterology Enamel-Renal syndrome is a rare autosomal recessive condition. [1] This condition is also known as idiopathic multicentric osteolysis with nephropathy . ... Differential diagnosis [ edit ] Epidermolysis bullosa Jalili syndrome Raine syndrome Tricho-dento-osseous syndrome Treatment [ edit ] There is no specific treatment for this condition currently known and management of its various features is the norm. History [ edit ] This condition was first described in 1972. [2] References [ edit ] ^ Jaureguiberry G, De la Dure-Molla M, Parry D, Quentric M, Himmerkus N, Koike T, Poulter J, Klootwijk E, Robinette SL, Howie AJ, Patel V, Figueres ML, Stanescu HC, Issler N, Nicholson JK, Bockenhauer D, Laing C, Walsh SB, McCredie DA, Povey S, Asselin A, Picard A, Coulomb A, Medlar AJ, Bailleul-Forestier I, Verloes A, Le Caignec C, Roussey G, Guiol J, Isidor B, Logan C, Shore R, Johnson C, Inglehearn C, Al-Bahlani S, Schmittbuhl M, Clauss F, Huckert M, Laugel V, Ginglinger E, Pajarola S, Spartà G, Bartholdi D, Rauch A, Addor MC, Yamaguti PM, Safatle HP, Acevedo AC, Martelli-Júnior H, dos Santos Netos PE, Coletta RD, Gruessel S, Sandmann C, Ruehmann D, Langman CB, Scheinman SJ, Ozdemir-Ozenen D, Hart TC, Hart PS, Neugebauer U, Schlatter E, Houillier P, Gahl WA, Vikkula M, Bloch-Zupan A, Bleich M, Kitagawa H, Unwin RJ, Mighell A, Berdal A, Kleta R (2013) Nephrocalcinosis (Enamel Renal Syndrome) caused by autosomal recessive FAM20A Mutations.
-
Balloon Syndrome
Wikipedia
Rare condition in hedgehogs Hedgehog suffering from balloon syndrome before deflating Balloon syndrome is a rare condition in hedgehogs in which gas is trapped under the skin as a result of injury or infection, causing the animal to inflate. ... Instead, there is a lot of connective tissue under the skin, sectioning areas off into little compartments of air. Though it's called balloon syndrome, in most cases the hedgehogs 'puff up more like Bubble Wrap,' he said". [5] References [ edit ] ^ a b Forshaw, Hugh. " ' Care and Treatment of Sick and Injured Hedgehogs" (PDF) . britishhedgehogs.org.uk . ... Retrieved 11 June 2017 . ^ "Hedgehog 'blown up like beach ball' has balloon syndrome" . BBC News Online . BBC. 11 June 2017 . Retrieved 11 June 2017 . ^ a b "Balloon syndrome hedgehog is 'popped ' " . BBC News Online . ... Retrieved 11 June 2017 . ^ a b c Miller, Sara G. (31 July 2017). "Rare 'Balloon Syndrome' Causes Hedgehog to Puff Up Like a Beach Ball" .