-
Atypical Hemolytic Uremic Syndrome
Gard
Atypical hemolytic uremic syndrome (aHUS) is a disease that causes abnormal blood clots to form in small blood vessels in the kidneys. ... In familiar cases, p redisposition to aHUS is inherited in an autosomal dominant or an autosomal recessive pattern of inheritance. Atypical hemolytic uremic syndrome differs from a more common condition called typical hemolytic uremic syndrome .CFH, DGKE, CD46, C3, CFB, THBD, CFHR3, CFHR1, CFI, VTN, BAAT, ADAMTS13, TRIM25, C17orf67, CAPG, C5, CFHR5, VWF, C4BPA, C5AR1, IGAN1, PLG, C4BPB, CRP, GRHPR, CFHR4, C3AR1, TNF, GPR182, CABIN1, HPLH1, SMARCAL1, KRT20, SPZ1, PRSS55, CRISP2, THBS1, CRYGD, HP, ETFA, FHL1, MTOR, G6PD, GPI, CR1, CPB1, CD40LG, SPTA1, IL5, CD36, MUC1, MS4A1, NHS, PIGA, MASP1, NFE2L2
-
Spondylocostal Dysostosis
Wikipedia
Axial skeleton growth disorder Jarcho-Levin Syndrome Radiograph depicting typical skeletal features of Jarcho-Levin syndrome, subtype spondylothoracic dysplasia . ... Specialty Medical genetics Spondylocostal dysostosis , also known as Jarcho-Levin syndrome (JLS) , is a rare, heritable axial skeleton growth disorder. ... These individuals will often develop pulmonary complications and die in infancy or early childhood. [1] [8] [9] [10] [11] The disparity in outcomes of those with the syndrome is related to the fact that Jarcho-Levin actually encompasses two or more distinct syndromes, each with its own range of prognoses. The syndromes currently recognized as subtypes of Jarcho-Levin are termed spondylothoracic dysplasia and spondylocostal dysostosis . ... PMID 5722643 . ^ a b Lavy, N.W.; Palmer, C.G.; Merritt, A.D. (1966). "A syndrome of bizarre vertebral anomalies".
-
Flotch Syndrome
Orphanet
FLOTCH syndrome is a rare, genetic, cutaneous disorder characterized by leuchonychia and multiple, recurrent pilar cysts, associated or not with ciliar dystrophy and/or koilonychia.
-
Post-Acute-Withdrawal Syndrome
Wikipedia
Find sources: "Post-acute-withdrawal syndrome" – news · newspapers · books · scholar · JSTOR ( December 2020 ) ( Learn how and when to remove this template message ) Post-acute-withdrawal syndrome Other names Post-withdrawal syndrome, protracted withdrawal syndrome, prolonged withdrawal syndromes Specialty Psychiatry , Toxicology Post-acute withdrawal syndrome ( PAWS ) is a hypothesized set of persistent impairments that occur after withdrawal from alcohol , [1] [2] opiates , benzodiazepines , antidepressants and other substances. [3] [4] [5] Infants born to mothers who used substances of dependence during pregnancy may also experience a post-acute withdrawal syndrome. [6] [7] While post-acute withdrawal syndrome has been reported by those in the recovery community, there have been few scientific studies supporting its existence. [8] Because of this, the disorder is not recognized by the Diagnostic and Statistical Manual of Mental Disorders [9] or major medical associations. ... Acamprosate has been found to be effective in alleviating some of the post acute withdrawal symptoms of alcohol withdrawal. [32] [33] Carbamazepine or trazodone may also be effective in the treatment of post acute withdrawal syndrome in regards to alcohol use. [34] [35] [36] Cognitive behavioral therapy can also help the post acute withdrawal syndrome especially when cravings are a prominent feature. [37] See also [ edit ] Alcohol withdrawal syndrome Antidepressant discontinuation syndrome Benzodiazepine withdrawal syndrome Opioid use disorder References [ edit ] ^ Stephen Rich J, Martin PR (2014). ... "Protracted benzodiazepine withdrawal syndrome mimicking psychotic depression" (PDF) . ... PMID 7892364 . ^ Nirenberg MJ (2013). "Dopamine agonist withdrawal syndrome: implications for patient care". ... "Double-blind, placebo-controlled study of the efficacy of trazodone in alcohol post-withdrawal syndrome: polysomnographic and clinical evaluations".
-
Fat Embolism Syndrome
Wikipedia
In 1970, Gurd defined the characteristics of this phenomenon. [7] Gurd later modified the fat embolism criteria together with Wilson, thus producing Gurd and Wilson's criteria for fat embolism syndrome in 1974. [7] In 1983, Schonfeld suggested a scoring system for the diagnosis of fat embolism syndrome. In 1987, Lindeque proposed another scoring system that diagnose fat embolism syndrome by using respiratory changes alone. ... C.; Gupta, N. (2013). "Fat embolism syndrome" . Lung India . 30 (1): 47–53. doi : 10.4103/0970-2113.106133 . ... "The use of corticosteroid for the prophylaxis of fat embolism syndrome in patients with long bone fracture" . ... "Do corticosteroids reduce the risk of fat embolism syndrome in patients with long-bone fractures?
-
Multiple Endocrine Neoplasia
Wikipedia
Although a variety of additional eponyms have been proposed for MEN2B (e.g. Williams-Pollock syndrome, Gorlin-Vickers syndrome, and Wagenmann–Froboese syndrome), none ever gained sufficient traction to merit continued use and, indeed, are all but abandoned in the medical literature. ... In 1954 Wermer noted that this syndrome was transmitted as a dominant trait. ... In 1968 Steiner et al. introduced the term "multiple endocrine neoplasia" (MEN) to describe disorders featuring combinations of endocrine tumors and proposed the terms 'Wermer syndrome' for MEN 1 and 'Sipple syndrome' for MEN 2. ... "Familial multiple endocrine neoplasia syndromes: components, classification, and nomenclature" . ... "Germ-line mutations in p27Kip1 cause a multiple endocrine neoplasia syndrome in rats and humans" . Proc. Natl.RET, CDKN1B, MEN1, GHRL, GHSR, CALCA, VHL, TICAM2, TMED7-TICAM2, TMED7, IFI27, ZNRD2, CIB1, PTH, PSMD9, PRKAR1A, DCTN6, H3P23, CASR, HPT, GDNF, CDC73, AIP, FGF2, SDHB, GAST, SST, PPY, POMC, FUT4, CDKN2C, SARDH, CXADR, CDKN3, FRS2, SDS, SMUG1, PDE11A, CDKN2A, NR1I3, GFRA4, MEA1, CD109, SMAD3, CXADRP1, CALB1, TRIM13, GNAS, PTEN, SDHD, PTPN11, RENBP, BCL2, RPA2, RYK, SDHC, SLC8A1, PDE8B, SORD, SPG7, GRN, TP53, NF1, ZNF22, ARR3
-
Hypotrichosis-Deafness Syndrome
Orphanet
A syndromic genetic deafness characterized by erythrokeratoderma, hypotrichosis, nail dystrophy and sensorineural hearing loss.
-
Aphalangy-Syndactyly-Microcephaly Syndrome
Orphanet
An extremely rare malformation syndrome characterized by the association of partial distal aphalangia with syndactyly, duplication of metatarsal IV, microcephaly, and mild intellectual disability.
- Kufor-Rakeb Syndrome Orphanet
-
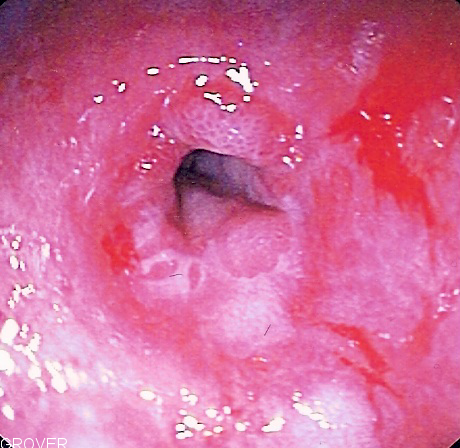
Esophageal Stricture
Wikipedia
. ^ Esophageal Stricture at eMedicine External links [ edit ] Classification D ICD - 10 : K22.2 ICD - 9-CM : 530.3 MeSH : D004940 DiseasesDB : 31502 External resources MedlinePlus : 000207 eMedicine : article/175098 MedlinePlus Encyclopedia : Esophageal Stricture v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Corticobasal Syndrome
Wikipedia
"Corticobasal syndrome: A diagnostic conundrum" . Dement Neuropsychol (Review). 10 (4): 267–75. doi : 10.1590/s1980-5764-2016dn1004003 . ... "Corticobasal degeneration and corticobasal syndrome: A review" . Clinical Parkinsonism & Related Disorders . 1 : 66–71. doi : 10.1016/j.prdoa.2019.08.005 . ISSN 2590-1125 . ^ Di Stasio F, Suppa A, Marsili L, et al. (May 2019). "Corticobasal syndrome: neuroimaging and neurophysiological advances". ... PMID 27042903 . ^ a b c Shimohata T, Aiba I, Nishizawa M (2016). "[Diagnoses of corticobasal syndrome and corticobasal degeneration]" . ... PMID 24521567 . ^ Hassan A, Whitwell JL, Josephs KA (November 2011). "The corticobasal syndrome-Alzheimer's disease conundrum" .
-
Idiopathic Postprandial Syndrome
Wikipedia
Idiopathic postprandial syndrome Symptoms Shakiness, sense of weakness Idiopathic postprandial syndrome , colloquially but incorrectly known by some as hypoglycemia , describes a collection of clinical signs and symptoms similar to medical hypoglycemia but without the demonstrably low blood glucose levels which characterise said condition. ... Contents 1 Signs and symptoms 2 Etymology and history of diagnosis 2.1 Non-disease 3 Adrenergic postprandial syndrome 4 See also 5 References Signs and symptoms [ edit ] The symptoms include many of the symptoms associated with milder degrees of hypoglycemia , especially the adrenergic symptoms, but do not progress to objective impairment of brain function, seizures, coma , or brain damage. [ citation needed ] Shakiness Sense of weakness Altered or depressed mood Confusion Fatigue Anxiety Paleness Perspiration Increased pulse or respiratory rate Hunger Etymology and history of diagnosis [ edit ] The term idiopathic postprandial syndrome , which literally means a syndrome that occurs after eating ( postprandial ) and is of unknown cause ( idiopathic ), was coined in an attempt to reserve the term hypoglycemia for those conditions in which low glucose levels could be demonstrated. [1] It was offered as a less confusing alternative to functional hypoglycemia and as a less pejorative alternative to "nonhypoglycemia" or "pseudohypoglycemia". The syndrome resembles reactive hypoglycemia except that low glucose is not found at the time of symptoms. The common usage of the term "hypoglycemia" was noted and countered by doctors writing in the Journal of the American Medical Association in the 1970s: The "syndrome of hypoglycemia" has become popular among patients and physicians alike, primarily because it seems to provide an explanation (?) ... Thus much more research is indicated to define the norms as well as to characterize the role and nature of the various gut factors and the responses of the beta cells to these factors. Adrenergic postprandial syndrome [ edit ] There is some evidence of the existence of a so-called "adrenergic postprandial syndrome": the glycemia is normal, and the symptoms are caused through autonomic adrenergic counterregulation. [6] Often, this syndrome is associated with emotional distress and anxious behaviour of the patient. [7] [8] See also [ edit ] Chronic Somogyi rebound (The "Somogyi effect") Idiopathic hypoglycemia Reactive hypoglycemia References [ edit ] ^ Charles MA, Hofeldt F, Shackelford A, et al. (1981).
-
Gastroenterocolitis
Wikipedia
. ^ "Stomach Flu (Gastroenteritis) Symptoms, Remedies, Diet & Contagion" . v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Poliosis
Wikipedia
In poliosis there is decreased or absent melanin in the hair bulbs of affected hair follicles; the melanocytes of the skin are usually not affected. [1] Contents 1 Associated medical conditions 2 Popular culture 3 References 4 External links Associated medical conditions [ edit ] Poliosis occurs in several genetic syndromes such as piebaldism , Waardenburg syndrome , neurofibromatosis type I , and tuberous sclerosis . [2] It can also occur in conditions such as vitiligo , Vogt–Koyanagi–Harada disease , alopecia areata , sarcoidosis , and in association with neoplasms and some medications. [1] Popular culture [ edit ] It is sometimes called a Mallen streak , after a fictional family with hereditary poliosis. ... External links [ edit ] Classification D ICD - 10 : L67.1 ( ILDS L67.150) DiseasesDB : 29296 SNOMED CT : 14240001 v t e Disorders of skin appendages Nail thickness: Onychogryphosis Onychauxis color: Beau's lines Yellow nail syndrome Leukonychia Azure lunula shape: Koilonychia Nail clubbing behavior: Onychotillomania Onychophagia other: Ingrown nail Anonychia ungrouped: Paronychia Acute Chronic Chevron nail Congenital onychodysplasia of the index fingers Green nails Half and half nails Hangnail Hapalonychia Hook nail Ingrown nail Lichen planus of the nails Longitudinal erythronychia Malalignment of the nail plate Median nail dystrophy Mees' lines Melanonychia Muehrcke's lines Nail–patella syndrome Onychoatrophy Onycholysis Onychomadesis Onychomatricoma Onychomycosis Onychophosis Onychoptosis defluvium Onychorrhexis Onychoschizia Platonychia Pincer nails Plummer's nail Psoriatic nails Pterygium inversum unguis Pterygium unguis Purpura of the nail bed Racquet nail Red lunulae Shell nail syndrome Splinter hemorrhage Spotted lunulae Staining of the nail plate Stippled nails Subungual hematoma Terry's nails Twenty-nail dystrophy Hair Hair loss / Baldness noncicatricial alopecia : Alopecia areata totalis universalis Ophiasis Androgenic alopecia (male-pattern baldness) Hypotrichosis Telogen effluvium Traction alopecia Lichen planopilaris Trichorrhexis nodosa Alopecia neoplastica Anagen effluvium Alopecia mucinosa cicatricial alopecia : Pseudopelade of Brocq Central centrifugal cicatricial alopecia Pressure alopecia Traumatic alopecia Tumor alopecia Hot comb alopecia Perifolliculitis capitis abscedens et suffodiens Graham-Little syndrome Folliculitis decalvans ungrouped: Triangular alopecia Frontal fibrosing alopecia Marie Unna hereditary hypotrichosis Hypertrichosis Hirsutism Acquired localised generalised patterned Congenital generalised localised X-linked Prepubertal Acneiform eruption Acne Acne vulgaris Acne conglobata Acne miliaris necrotica Tropical acne Infantile acne / Neonatal acne Excoriated acne Acne fulminans Acne medicamentosa (e.g., steroid acne ) Halogen acne Iododerma Bromoderma Chloracne Oil acne Tar acne Acne cosmetica Occupational acne Acne aestivalis Acne keloidalis nuchae Acne mechanica Acne with facial edema Pomade acne Acne necrotica Blackhead Lupus miliaris disseminatus faciei Rosacea Perioral dermatitis Granulomatous perioral dermatitis Phymatous rosacea Rhinophyma Blepharophyma Gnathophyma Metophyma Otophyma Papulopustular rosacea Lupoid rosacea Erythrotelangiectatic rosacea Glandular rosacea Gram-negative rosacea Steroid rosacea Ocular rosacea Persistent edema of rosacea Rosacea conglobata variants Periorificial dermatitis Pyoderma faciale Ungrouped Granulomatous facial dermatitis Idiopathic facial aseptic granuloma Periorbital dermatitis SAPHO syndrome Follicular cysts " Sebaceous cyst " Epidermoid cyst Trichilemmal cyst Steatocystoma simplex multiplex Milia Inflammation Folliculitis Folliculitis nares perforans Tufted folliculitis Pseudofolliculitis barbae Hidradenitis Hidradenitis suppurativa Recurrent palmoplantar hidradenitis Neutrophilic eccrine hidradenitis Ungrouped Acrokeratosis paraneoplastica of Bazex Acroosteolysis Bubble hair deformity Disseminate and recurrent infundibulofolliculitis Erosive pustular dermatitis of the scalp Erythromelanosis follicularis faciei et colli Hair casts Hair follicle nevus Intermittent hair–follicle dystrophy Keratosis pilaris atropicans Kinking hair Koenen's tumor Lichen planopilaris Lichen spinulosus Loose anagen syndrome Menkes kinky hair syndrome Monilethrix Parakeratosis pustulosa Pili ( Pili annulati Pili bifurcati Pili multigemini Pili pseudoannulati Pili torti ) Pityriasis amiantacea Plica neuropathica Poliosis Rubinstein–Taybi syndrome Setleis syndrome Traumatic anserine folliculosis Trichomegaly Trichomycosis axillaris Trichorrhexis ( Trichorrhexis invaginata Trichorrhexis nodosa ) Trichostasis spinulosa Uncombable hair syndrome Wooly hair nevus Sweat glands Eccrine Miliaria Colloid milium Miliaria crystalline Miliaria profunda Miliaria pustulosa Miliaria rubra Occlusion miliaria Postmiliarial hypohidrosis Granulosis rubra nasi Ross’ syndrome Anhidrosis Hyperhidrosis Generalized Gustatory Palmoplantar Apocrine Body odor Chromhidrosis Fox–Fordyce disease Sebaceous Sebaceous hyperplasia This cutaneous condition article is a stub .
-
Nephrosis
Wikipedia
Non-inflammatory kidney disease Not to be confused with necrosis , nephritis , or nephrotic syndrome . Nephrosis Specialty Nephrology Nephrosis is any of various forms of kidney disease (nephropathy). ... It is also defined as any purely degenerative disease of the renal tubules . [1] Nephrosis is characterized by a set of signs called the nephrotic syndrome . [2] Nephrosis can be a primary disorder or can be secondary to another disorder. [2] Nephrotic complications of another disorder can coexist with nephritic complications. ... External links [ edit ] Classification D MeSH : D009401 v t e Kidney disease Glomerular disease See Template:Glomerular disease Tubules Renal tubular acidosis proximal distal Acute tubular necrosis Genetic Fanconi syndrome Bartter syndrome Gitelman syndrome Liddle's syndrome Interstitium Interstitial nephritis Pyelonephritis Balkan endemic nephropathy Vascular Renal artery stenosis Renal ischemia Hypertensive nephropathy Renovascular hypertension Renal cortical necrosis General syndromes Nephritis Nephrosis Renal failure Acute renal failure Chronic kidney disease Uremia Other Analgesic nephropathy Renal osteodystrophy Nephroptosis Abderhalden–Kaufmann–Lignac syndrome Diabetes insipidus Nephrogenic Renal papilla Renal papillary necrosis Major calyx / pelvis Hydronephrosis Pyonephrosis Reflux nephropathy This article about a disease of the genitourinary system is a stub .VIM, F2, DDIT3, NES, EDN1, NPHS2, ALB, REN, AGT, EDNRB, SOD1, ICAM1, ITGB2, HPSE, DES, LAMB2, HAVCR1, LRP2, NPPB, NPPA, CCL1, IL1B, CX3CL1, SREBF2, STAR, PTPRU, PDPN, CCL7, CYP3A43, ACE, CD59, CFH, CX3CR1, CYP3A5, ANGPT1, ANGPT2, CYP11A1, CD36, CYP27B1, TGFB1, APOA1, NPHS1, VEGFA, CLDN1, OLFM1, SGPL1, TNFSF10, LGALSL, NSD3, CLDN7, CST3, NDST1, CTSL, TRPC6, STAT5A, STAT3, CYP2C19, CCL13, SALL1, PIK3CG, PIK3CD, PIK3CB, PIK3CA, HBEGF, EDNRA, MYOC, GATA3, ACTB
-
Foot Deformity
Wikipedia
References [ edit ] External links [ edit ] Classification D ICD - 10 : M20 - M21 , Q66 ICD - 9-CM : 734 - 735 , 755.6 MeSH : D005530 v t e Acquired musculoskeletal deformities Upper limb shoulder Winged scapula Adhesive capsulitis Rotator cuff tear Subacromial bursitis elbow Cubitus valgus Cubitus varus hand deformity Wrist drop Boutonniere deformity Swan neck deformity Mallet finger Lower limb hip Protrusio acetabuli Coxa valga Coxa vara leg Unequal leg length patella Luxating patella Chondromalacia patellae Patella baja Patella alta foot deformity Bunion/hallux valgus Hallux varus Hallux rigidus Hammer toe Foot drop Flat feet Club foot knee Genu recurvatum Head Cauliflower ear General terms Valgus deformity / Varus deformity Joint stiffness Ligamentous laxity v t e Congenital malformations and deformations of musculoskeletal system / musculoskeletal abnormality Appendicular limb / dysmelia Arms clavicle / shoulder Cleidocranial dysostosis Sprengel's deformity Wallis–Zieff–Goldblatt syndrome hand deformity Madelung's deformity Clinodactyly Oligodactyly Polydactyly Leg hip Hip dislocation / Hip dysplasia Upington disease Coxa valga Coxa vara knee Genu valgum Genu varum Genu recurvatum Discoid meniscus Congenital patellar dislocation Congenital knee dislocation foot deformity varus Club foot Pigeon toe valgus Flat feet Pes cavus Rocker bottom foot Hammer toe Either / both fingers and toes Polydactyly / Syndactyly Webbed toes Arachnodactyly Cenani–Lenz syndactylism Ectrodactyly Brachydactyly Stub thumb reduction deficits / limb Acheiropodia Ectromelia Phocomelia Amelia Hemimelia multiple joints Arthrogryposis Larsen syndrome RAPADILINO syndrome Axial Skull and face Craniosynostosis Scaphocephaly Oxycephaly Trigonocephaly Craniofacial dysostosis Crouzon syndrome Hypertelorism Hallermann–Streiff syndrome Treacher Collins syndrome other Macrocephaly Platybasia Craniodiaphyseal dysplasia Dolichocephaly Greig cephalopolysyndactyly syndrome Plagiocephaly Saddle nose Vertebral column Spinal curvature Scoliosis Klippel–Feil syndrome Spondylolisthesis Spina bifida occulta Sacralization Thoracic skeleton ribs : Cervical Bifid sternum : Pectus excavatum Pectus carinatum This article about Orthopedic surgery is a stub .SMARCD1, PIGB, CNTNAP1, MPZ, H19, TCF20, UROS, VRK1, ALPL, YARS1, CCN6, MCM3AP, TRIP11, ADAMTS3, SPTLC2, SLC9A6, CCT5, VPS13A, ATP13A2, CLCF1, AUTS2, SACS, SLC17A5, SLC25A24, EXOSC3, KMT5B, TMEM216, TYROBP, INPP5E, SYT1, DARS2, CHD3, CHRNG, COL2A1, CCBE1, CPT2, DHODH, DYNC1H1, PANK2, EXT1, GATA1, MYH14, HINT1, HK1, FAT4, IGF2, IGHMBP2, LMNA, MYH3, MYO9A, VPS33A, SLC18A2, SLC25A1, TRPV4, ATAD3A, GDF5, PMP22, GDAP1, SMN2, SMN1, HOXD13, GJB1, EEC1, SYT2, COL12A1, ALB
-
Blepharophimosis, Ptosis, Epicanthus Inversus Syndrome
Wikipedia
Rare genetic condition involving underdeveloped eyelids Blepharophimosis, ptosis, epicanthus inversus syndrome Other names Blepharophimosis types 1 and 2 18-year-old female with BPES type 1 This condition is inherited in an autosomal dominant manner. Blepharophimosis, ptosis, epicanthus inversus syndrome ( BPES ) is a rare disease characterized by the conditions it is named after: blepharophimosis , ptosis and epicanthus inversus . ... Other disorders that appear similar include Waardenburg syndrome and Ohdo blepharophimosis syndrome . [1] Treatment [ edit ] The main treatment is symptomatic, since the underlying genetic defect cannot be corrected as of 2015. ... It affects slightly more males than females. [1] References [ edit ] ^ a b c d e f g "Blepharophimosis, Ptosis, Epicanthus Inversus Syndrome - NORD (National Organization for Rare Disorders)" .
-
Epizootic Ulcerative Syndrome
Wikipedia
Epizootic ulcerative syndrome (EUS), also known as mycotic granulomatosis (MG) or red spot disease (RSD), is a disease caused by the water mould Aphanomyces invadans . ... In countries free of epizootic ulcerative syndrome, quarantine and health certificates are necessary for the movement of all live fish to prevent the introduction of the disease. References [ edit ] Epizootic Ulcerative Syndrome, reviewed and published by Wikivet at http://en.wikivet.net/Epizootic_Ulcerative_Syndrome , accessed 08/09/2011. v t e Fish diseases and parasites Pathogens Aeromonas salmonicida Nervous necrosis virus Columnaris Enteric redmouth Fin rot Fish dropsy Flavobacterium Hematopoietic necrosis Heterosigma akashiwo Hole in the head Hypodermal and hematopoietic necrosis Infectious pancreatic necrosis Koi herpes virus Mycobacterium marinum Novirhabdovirus Pfiesteria piscicida Photobacterium damselae ssp piscicida Salmon anemia Streptococcus iniae Spring viraemia of carp Taura syndrome UDN VHS White spot Yellowhead Parasites Abergasilus Amoebic gill disease Anisakis Carp lice Ceratomyxa shasta Clinostomum marginatum Dactylogyrus vastator Diphyllobothrium Cymothoa exigua Eustrongylidosis Epizootic ulcerative syndrome Flukes Glugea Gyrodactylus salaris Henneguya zschokkei Ich (freshwater) Ich (marine) Kudoa thyrsites Lernaeocera branchialis Microsporidia Monogenea Myxobolus cerebralis Myxosporea Nanophyetus salmincola Pseudorhabdosynochus spp.
-
Joubert Syndrome 33
Omim
A number sign (#) is used with this entry because of evidence that Joubert syndrome-33 (JBTS33) is caused by homozygous or compound heterozygous mutation in the PIBF1 gene (607532) on chromosome 13q21. Description Joubert syndrome represents a classic ciliopathy characterized by hypotonia, ataxia, cognitive impairment, and a distinctive brain malformation, the 'molar tooth sign.' ... For a discussion of genetic heterogeneity of Joubert syndrome, see JBTS1 (213300). Clinical Features Wheway et al. (2015) reported 6 children with Joubert syndrome from 4 Hutterite families, designated H1 to H4. ... Molecular Genetics By whole-exome sequencing in 2 brothers with Joubert syndrome from a family of Schmiedeleut Hutterite descent (family H1), who were negative for mutations in known JBTS-associated genes, Wheway et al. (2015) identified homozygosity for a missense mutation in the PIBF1 gene (D637A; 607532.0001) for which their parents were heterozygous.
-
Wobbly Hedgehog Syndrome
Wikipedia
Wobbly hedgehog syndrome ( WHS ) is a progressive, degenerative, neurological disease of the African pygmy hedgehog . [1] [2] The cause is believed to be genetic. [3] Nearly 10 percent of pet African pygmy hedgehogs are affected, [2] due to their limited bloodlines. [4] Symptoms [ edit ] The disease slowly degrades the hedgehog's muscle control. ... A tentative diagnosis can be based purely on the clinical signs, but definitive diagnosis is only possible from post-mortem examination of spinal cord and brain tissues. [1] The hedgehog's health will deteriorate over the course of weeks or months, and in the advanced stages of this disease, they become completely immobilized, making euthanasia a recommended consideration. [1] Most animals die within two years of diagnosis. [5] Symptoms usually begin in hedgehogs before they reach two years old, but can occur at any age. [6] Treatment [ edit ] There is no known cure for WHS, which has been compared to human multiple sclerosis . [5] Various vitamin supplements, antibiotic and steroid treatments have been used; some appear to temporarily improve the signs or slow the progression of the disease, but as signs of WHS wax and wane, it is difficult to assess the benefit of treatments. [2] No treatment has been shown to prevent the progression of paralysis. [2] References [ edit ] ^ a b c Axelson, Rick. "Wobbly hedgehog syndrome" . VCA Animal Hospitals . Retrieved 5 June 2014 . ^ a b c d Graesser, Donnasue; Spraker, Terry R.; Dressen, Priscilla; Garner, Michael M.; Raymond, James T.; Terwilliger, Gordon; Kim, Jung; Madri, Joseph A. (January 2006). "Wobbly hedgehog syndrome in African pygmy hedgehogs ( Atelerix spp.)". Journal of Exotic Pet Medicine . 15 (1): 59–65. doi : 10.1053/j.jepm.2005.11.010 . ^ Storm, Pat; Graesser, Donnasue (July 2007). "Wobbly hedgehog syndrome: A genetic disease?" (PDF) . The Hedgehog Welfare Society Newsletter . ... "What helps with wobbly hedgehog syndrome? Joe Inglis explains" . Metro .