-
Alazami-Yuan Syndrome
Omim
A number sign (#) is used with this entry because of evidence that Alazami-Yuan syndrome (ALYUS) is caused by homozygous mutation in the TAF6 gene (602955) on chromosome 7q22. ... These features were reminiscent of Cornelia de Lange syndrome (see, e.g., CDLS1, 122470). Family history revealed 2 deceased infant sibs with similar features.
-
Surgical Shock
Wikipedia
It is commonly due to a loss of blood which results in insufficient blood volume . [1] References [ edit ] ^ Stewart, John (1999), "Types of surgical shock", Clinical Care for Lawyers , Cavendish, pp. 255–256, ISBN 9781843143581 v t e Intensive care medicine Health science Medicine Medical specialities Respiratory therapy General terms Intensive care unit (ICU) Neonatal intensive care unit (NICU) Pediatric intensive care unit (PICU) Coronary care unit (CCU) Critical illness insurance Conditions Organ system failure Shock sequence SIRS Sepsis Severe sepsis Septic shock Multiple organ dysfunction syndrome Other shock Cardiogenic shock Distributive shock Anaphylaxis Obstructive shock Neurogenic shock Spinal shock Vasodilatory shock Organ failure Acute renal failure Acute respiratory distress syndrome Acute liver failure Respiratory failure Multiple organ dysfunction syndrome Neonatal infection Polytrauma Coma Complications Critical illness polyneuropathy / myopathy Critical illness–related corticosteroid insufficiency Decubitus ulcers Fungemia Stress hyperglycemia Stress ulcer Iatrogenesis Methicillin-resistant Staphylococcus aureus Oxygen toxicity Refeeding syndrome Ventilator-associated lung injury Ventilator-associated pneumonia Dialytrauma Diagnosis Arterial blood gas Catheter Arterial line Central venous catheter Pulmonary artery catheter Blood cultures Screening cultures Life-supporting treatments Airway management Chest tube Dialysis Enteral feeding Goal-directed therapy Induced coma Mechanical ventilation Therapeutic hypothermia Total parenteral nutrition Tracheal intubation Drugs Analgesics Antibiotics Antithrombotics Inotropes Intravenous fluids Neuromuscular-blocking drugs Recombinant activated protein C Sedatives Stress ulcer prevention drugs Vasopressors ICU scoring systems APACHE II Glasgow Coma Scale PIM2 SAPS II SAPS III SOFA Physiology Hemodynamics Hypotension Level of consciousness Acid–base imbalance Water-electrolyte imbalance Organisations Society of Critical Care Medicine Surviving Sepsis Campaign European Society of Paediatric and Neonatal Intensive Care Related specialties Anesthesiology Cardiology Internal medicine Neurology Pediatrics Pulmonology Surgery Traumatology v t e Symptoms and signs relating to the circulatory system Chest pain Referred pain Angina Levine's sign Auscultation Heart sounds Split S2 S3 S4 Gallop rhythm Heart murmur Systolic Functional murmur Still's murmur Diastolic Pulmonary insufficiency Graham Steell murmur Continuous Carey Coombs murmur Mitral insufficiency Presystolic murmur Pericardial friction rub Heart click Bruit carotid Pulse Tachycardia Bradycardia Pulsus paradoxus doubled Pulsus bisferiens Pulsus bigeminus Pulsus alternans Other Palpitations Apex beat Cœur en sabot Jugular venous pressure Cannon A waves Hyperaemia Shock Cardiogenic Obstructive Hypovolemic Distributive See further Template:Shock Cardiovascular disease Aortic insufficiency Collapsing pulse De Musset's sign Duroziez's sign Müller's sign Austin Flint murmur Mayne's sign Other endocardium endocarditis : Roth's spot Janeway lesion / Osler's node Bracht–Wachter bodies Pericardium Cardiac tamponade / Pericardial effusion : Beck's triad Ewart's sign Other rheumatic fever : Anitschkow cell Aschoff body EKG J wave Gallavardin phenomenon Vascular disease Arterial aortic aneurysm Cardarelli's sign Oliver's sign pulmonary embolism Right heart strain radial artery sufficiency Allen's test pseudohypertension thrombus Lines of Zahn Adson's sign arteriovenous fistula Nicoladoni sign Venous Friedreich's sign Caput medusae Kussmaul's sign Trendelenburg test superior vena cava syndrome Pemberton's sign This surgery article is a stub .
-
Megacystis-Microcolon-Intestinal Hypoperistalsis Syndrome
Medlineplus
Megacystis-microcolon-intestinal hypoperistalsis syndrome (MMIHS) is a severe disorder affecting the muscles that line the bladder and intestines . ... Learn more about the genes associated with Megacystis-microcolon-intestinal hypoperistalsis syndrome ACTG2 MYH11 Additional Information from NCBI Gene: LMOD1 MYLK Inheritance Pattern When caused by ACTG2 gene mutations, MMIHS follows an autosomal dominant pattern , which means one copy of the altered gene in each cell is sufficient to cause the disorder.
-
Noncompaction Cardiomyopathy
Wikipedia
Cardiac Abnormalities of the origin of the left coronary artery Pulmonary atresia Stenosis Right or Left ventricle obstruction Hypoplastic left ventricle Mitral regurgitation Neuromuscular (Pertaining to both nerves and muscles) Becker's muscular dystrophy Mitochondrial myopathy Polyneuropathy and metabolic myopathy Genetic related Emery–Dreifuss muscular dystrophy Myotubular cardiomyopathy Barth syndrome Genetics [ edit ] The American Heart Association 's 2006 classification of cardiomyopathies considers noncompaction cardiomyopathy a genetic cardiomyopathy. [5] Mutations in LDB3 (also known as "Cypher/ZASP") have been described in patients with the condition. [6] There is recent information in which NCC has been seen in combination with 1q21.1 deletion Syndrome . [7] Furthermore mutations in Titin ( TTN ), RBM20 and also LMNA could be detected in a large cohort of LVNC patients. [8] Loss-of-function variants in the NONO gene have been associated with an X-linked form of noncompaction cardiomyopathy in males who also often present with developmental delays. [9] In addition, a small in-frame deletion was identified in the DES gene, encoding the intermediate filament protein desmin. [10] Diagnosis [ edit ] Trabeculation of the ventricles is normal, as are prominent, discrete muscular bundles greater than 2mm. ... Myocardial sinusoids is considered not an accurate term as endothelium lines the intertrabecular recesses. See also [ edit ] Barth syndrome Emery–Dreifuss muscular dystrophy Myotubular myopathy References [ edit ] ^ Pignatelli RH, McMahon CJ, Dreyer WJ, Denfield SW, Price J, Belmont JW, et al. ... External links [ edit ] Classification D OMIM : 601493 MeSH : D056830 v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever v t e Congenital heart defects Heart septal defect Aortopulmonary septal defect Double outlet right ventricle Taussig–Bing syndrome Transposition of the great vessels dextro levo Persistent truncus arteriosus Aortopulmonary window Atrial septal defect Sinus venosus atrial septal defect Lutembacher's syndrome Ventricular septal defect Tetralogy of Fallot Atrioventricular septal defect Ostium primum Consequences Cardiac shunt Cyanotic heart disease Eisenmenger syndrome Valvular heart disease Right pulmonary valves stenosis insufficiency absence tricuspid valves stenosis atresia Ebstein's anomaly Left aortic valves stenosis insufficiency bicuspid mitral valves stenosis regurgitation Other Underdeveloped heart chambers right left Uhl anomaly Dextrocardia Levocardia Cor triatriatum Crisscross heart Brugada syndrome Coronary artery anomaly Anomalous aortic origin of a coronary artery Ventricular inversion
-
Congenital Mirror Movements
Gene_reviews
They usually disappear completely before age seven years and tend to recur gradually in old age [Bonnet et al 2010, Koerte et al 2010]. Syndromes with early-onset (congenital) mirror movements. ... When the diagnosis is in doubt, brain and cervical MRI may be considered in children or adolescents with mirror movements. Table 2. Syndromes with Early-Onset Mirror Movements View in own window Disorder Gene(s) MOI Mirror Movements Other Features ANOS1 Kallmann syndrome (KS) (See Isolated GnRH Deficiency.) ... Nevoid basal cell carcinoma syndrome (Gorlin syndrome) PTCH1 (PTCH2) 6 SUFU AD MM reported in 1 person 7 Multiple basal cell carcinomas, jaw keratocysts, & skeletal malformations Seckel syndrome (OMIM PS210600) ATR CENPJ CEP152 CEP63 DNA2 NIN NSMCE2 RBBP8 TRAIP AR 1 reported person w/MM 8 Primary microcephaly, intellectual disability, & often prenatal-onset growth restriction Wildervanck syndrome (OMIM 314600) Unknown XL? 1 reported person w/MM 9 Klippel-Feil syndrome w/congenital perceptive deafness & Duane syndrome 10 Affected persons are almost exclusively female. ... Högen et al [2012] 10. Duane syndrome = abducens palsy with narrowing of the palpebral fissure Acquired mirror movements.
-
Brain Herniation
Wikipedia
Other possibilities resulting from brain stem distortion include lethargy , slow heart rate, and pupil dilation . [8] Uncal herniation may advance to central herniation. [6] The sliding uncus syndrome represents uncal herniation without alteration in the level of consciousness and other sequelae mentioned above. ... Upwards herniation, on the other hand, can be radiographically characterized by obliteration of the quadrigeminal cistern. Intracranial hypotension syndrome has been known to mimic downwards transtentorial herniation. ... Connective tissue disorders, such as Ehlers Danlos syndrome , can be associated. For further evaluation of tonsillar herniation, CINE flow studies are used. ... Retrieved 2020-07-31 . ^ Halliday A. "Cerebral Herniation Syndromes" (PDF) . Oregon Neurosurgery Specialists. ^ Smith, Julian; Joe J. ... Retrieved on January 28, 2007. ^ a b c Hudson K (2006). "Brain Herniation Syndromes - 2 Nursing CEs" . Dynamic Nursing Education .
-
Pericardial Effusion
Wikipedia
Tuberculosis is the leading cause of pericardial effusion in the developing world, with the mortality rate ranging from 17-40%. [5] Fungal: Histoplasma, Candida Protozoal: Echinococcus, Trichinosis , Toxoplasma Cardiac injury syndromes: Heart surgery [6] ( postpericardiotomy syndrome ), post-myocardial infarction ( Dressler's syndrome ), coronary interventions such as drug eluting stents. ... Cardiac inflammation: idiopathic pericarditis is the most common inflammatory cause of pericardial effusion in the United States. [7] Autoimmune: lupus , rheumatoid arthritis , [8] Sjögren syndrome, scleroderma, Dressler's syndrome , sarcoidosis Drug hypersensitivity/ side effects: Chemotherapy drugs (doxorubicin and cyclophosphamide), Minoxidil Others: kidney failure, uremia Non-Inflammatory Causes: [5] Neoplastic: pericardial effusions may present as primary manifestations of underlying malignancy in patients. [5] Primary tumor : the most common primary pericardial tumor is mesothelioma . ... Pericardial irregular thickening and/or nodularity, focal, or diffuse FDG uptake on PET scan and lack of preserved fat plane with an adjacent tumor are strongly suggestive of cancer spread from other parts of the body. [9] Metabolic: hypothyroidism (myxedema coma), severe protein deficiency Traumatic: penetrating or blunt chest trauma, aortic dissection Reduced lymphatic drainage: congestive heart failure, nephrotic syndrome Diagnosis [ edit ] Chest X-ray showing a massive pericardial effusion: Water bottle sign EKG: sinus tachycardia with low QRS voltage and electrical alternans Some patients with pericardial effusions may present with no symptoms and the diagnosis can be an incidental finding due to imaging of other illnesses. ... Pericardiocentesis is usually guided by an echocardiogram to determine the exact location of the effusion and the optimal location of puncture site to minimize risk of complications. [4] After the procedure, the aspirated fluid is analyzed for gross appearance (color, consistency, bloody), cell count, and concentration of glucose, protein, and other cellular components (for example lactate dehydrogenase ). [11] Fluid may be also sent for gram stain, acid fast stain, or culture if high suspicion of infectious cause. [1] Bloody fluids may also be evaluated for malignant cells. [11] Fluid analysis may result in: transudative effusion: due to non-inflammatory causes ( congestive heart failure , myxoedema , nephrotic syndrome ) exudative effusion: inflammatory or malignant causes ( tuberculosis , spread from empyema , metastasis ) hemorrhagic effusion: high blood concentration (trauma, rupture of aneurysms, malignant effusion) A CT scan showing a pericardial effusion A large anechoic (black) pericardial effusion as seen on ultrasound. ... Biochemia medica vol. 24,1 123-37. 15 Feb. 2014, doi:10.11613/BM.2014.014 External links [ edit ] Classification D ICD - 10 : I30 , I31.3 ICD - 9-CM : 423.9 MeSH : D010490 DiseasesDB : 2128 External resources eMedicine : med/1786 Patient UK : Pericardial effusion v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic feverPLAT, PTGS2, ACADVL, GBA, LMNA, SMAD4, MYBPC3, PTPN14, RIT1, SLC12A3, SPP1, STAT4, ADAMTS3, KIAA0586, ABCC9, AARS2, CDH23, FAT4, ALG9, PLVAP, NLRP3, CCBE1, TMEM151B, IRAK1, PMM2, C1QA, CLCNKB, EPHB4, SCARB2, DNASE1L3, C1R, ALB, CRP, IL6, SMUG1, EGFR, ADA, IL10, CNP, TLR7, CABIN1, MAPK14, ADIPOQ, PKD2L1, VEGFA, TYR, FOXP3, IFNG, ELAC2, TLR8, KRT20, TP53, MS4A1, CAT, ADGRV1, CARD16, EMB, MIRLET7B, MIR126, MIR21, AKT1, MIR423, C20orf181, TPT1, TAZ, TNNI3, FABP4, IL1B, IL2RA, IL5, IL6ST, CXCL8, IL13, GATA1, ISG20, KRAS, LEP, FLT4, MLANA, MET, MMP9, NPPB, TNF, NPPC, PAH, PDCD1, ERBB2, POU2F2, EMP2, S100A1, S100B, CCL2, EDN1, SLC22A2, ACE, IGF1, TGFBR1, MIR3184
-
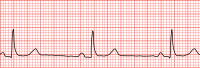
Bradycardia
Wikipedia
Highly trained athletes may also have athletic heart syndrome , a very slow resting heart rate that occurs as a sport adaptation and helps prevent tachycardia during training. [3] The term "relative bradycardia" is used to refer to a heart rate that, although not actually below 60 BPM, is still considered too slow for the individual's current medical condition. ... Studies have found that 50–85% of conditioned athletes have benign sinus bradycardia, as compared to 23% of the general population studied. [6] The heart muscle of athletes has become conditioned to have a higher stroke volume , so requires fewer contractions to circulate the same volume of blood. [5] The third, sick sinus syndrome , covers conditions that include severe sinus bradycardia, sinoatrial block , sinus arrest , and bradycardia-tachycardia syndrome ( atrial fibrillation , atrial flutter , and paroxysmal supraventricular tachycardia ). [5] Atrioventricular junction [ edit ] An AV-junctional rhythm , or atrioventricular nodal bradycardia, is usually caused by the absence of the electrical impulse from the sinus node . ... With SA node dysfunction (sometimes called sick sinus syndrome), there may be disordered automaticity or impaired conduction of the impulse from the SA node into the surrounding atrial tissue (an "exit block"). ... ISBN 978-0-7817-5125-4 . ^ Ward, Bryan G.; Rippe, J.M. (1992). "11". Athletic Heart Syndrome . Clinical Sports Medicine. p. 259. ^ "AV Junctional Rhythm Disturbances (for Professionals)" . ... External links [ edit ] Classification D ICD - 10 : R00.1 ICD - 9-CM : 427.81 , 659.7 , 785.9 , 779.81 MeSH : D001919 External resources Patient UK : Bradycardia v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever v t e Symptoms and signs relating to the circulatory system Chest pain Referred pain Angina Levine's sign Auscultation Heart sounds Split S2 S3 S4 Gallop rhythm Heart murmur Systolic Functional murmur Still's murmur Diastolic Pulmonary insufficiency Graham Steell murmur Continuous Carey Coombs murmur Mitral insufficiency Presystolic murmur Pericardial friction rub Heart click Bruit carotid Pulse Tachycardia Bradycardia Pulsus paradoxus doubled Pulsus bisferiens Pulsus bigeminus Pulsus alternans Other Palpitations Apex beat Cœur en sabot Jugular venous pressure Cannon A waves Hyperaemia Shock Cardiogenic Obstructive Hypovolemic Distributive See further Template:Shock Cardiovascular disease Aortic insufficiency Collapsing pulse De Musset's sign Duroziez's sign Müller's sign Austin Flint murmur Mayne's sign Other endocardium endocarditis : Roth's spot Janeway lesion / Osler's node Bracht–Wachter bodies Pericardium Cardiac tamponade / Pericardial effusion : Beck's triad Ewart's sign Other rheumatic fever : Anitschkow cell Aschoff body EKG J wave Gallavardin phenomenon Vascular disease Arterial aortic aneurysm Cardarelli's sign Oliver's sign pulmonary embolism Right heart strain radial artery sufficiency Allen's test pseudohypertension thrombus Lines of Zahn Adson's sign arteriovenous fistula Nicoladoni sign Venous Friedreich's sign Caput medusae Kussmaul's sign Trendelenburg test superior vena cava syndrome Pemberton's signTAC1, CACNA1D, ADORA1, PDYN, HTR1A, KNG1, LHB, AGT, NTS, NISCH, POMC, GCG, PRL, UTS2, TACR1, TRH, GNRH1, GNAI2, EDN2, EDN1, DRD2, CYP2D6, EDN3, CYP1A1, CRH, CHRM2, MC4R, TRPM4, BRAT1, SGO1, TMEM43, GNB5, COQ9, QRICH1, LIPT1, MAGEL2, USP18, BSCL2, PPA2, HTRA2, PAX8, PRKAG2, AGPAT2, NPPA, GLUL, TSPYL1, DST, CACNA1C, CACNA2D1, SLC25A20, CASQ2, CAV1, FOS, CAVIN1, KCNH2, KCNJ2, KCNQ1, LMNA, PPARG, SCN9A, HCN4, SCN5A, ANK2
-
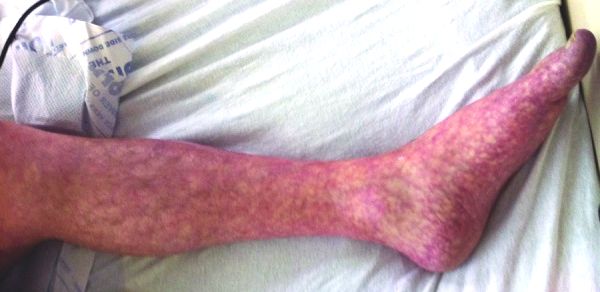
Livedo Reticularis
Wikipedia
"Livedo reticularis and digital infarcts: a syndrome due to cholesterol emboli arising from atheromatous abdominal aortic aneurysms". ... "Polymerase ε1 mutation in a human syndrome with facial dysmorphism, immunodeficiency, livedo, and short stature ('FILS syndrome')" (PDF) . ... "Mucocutaneous disorders in children with down syndrome: case-controlled study". Genet. ... "Mucocutaneous findings in 100 children with Down syndrome". Pediatr Dermatol . 24 (3): 317–20. doi : 10.1111/j.1525-1470.2007.00412.x . ... "Cutaneous manifestations of Churg–Strauss syndrome: Report of two cases and review of the literature".
-
Pyloric Stenosis
Wikipedia
External links [ edit ] 00675 at CHORUS Peristaltic waves video on NEJM Classification D ICD - 10 : Q40.0 ICD - 9-CM : 537.0 , 750.5 MeSH : D046248 DiseasesDB : 11060 External resources MedlinePlus : 000970 eMedicine : emerg/397 radio/358 , article/929829 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum v t e Congenital malformations and deformations of digestive system Upper GI tract Tongue , mouth and pharynx Cleft lip and palate Van der Woude syndrome tongue Ankyloglossia Macroglossia Hypoglossia Esophagus EA/TEF Esophageal atresia: types A, B, C, and D Tracheoesophageal fistula: types B, C, D and E esophageal rings Esophageal web (upper) Schatzki ring (lower) Stomach Pyloric stenosis Hiatus hernia Lower GI tract Intestines Intestinal atresia Duodenal atresia Meckel's diverticulum Hirschsprung's disease Intestinal malrotation Dolichocolon Enteric duplication cyst Rectum / anal canal Imperforate anus Rectovestibular fistula Persistent cloaca Rectal atresia Accessory Pancreas Annular pancreas Accessory pancreas Johanson–Blizzard syndrome Pancreas divisum Bile duct Choledochal cysts Caroli disease Biliary atresia Liver Alagille syndrome Polycystic liver diseaseAGTR2, TSPAN7, SH2B1, NIPBL, FTSJ1, NEDD4L, IQSEC2, CNKSR2, IL1RAPL1, MID2, ARFGEF2, AGPAT2, MED12, FIG4, HDAC4, FRMPD4, ADAMTS3, ARHGEF6, PEX16, SMC3, PEX11B, KCNAB2, PEX3, LTBP4, NAA10, SMC1A, USP9X, ZNF41, ZNF711, AUTS2, BSCL2, BCOR, ALG13, USP27X, ZNF81, CAVIN1, ARX, TMTC3, CCBE1, PTCHD1, RAB39B, NEK9, SLC9A7, SLC2A10, COL18A1, FAT4, PPP2R3C, CYBC1, UPF3B, MTMR14, PRDM16, CXorf56, PIEZO2, HDAC8, ERMARD, VAC14, PEX26, CHD7, SETD5, SLC35A2, TFAP2A, BIN1, HNF1B, LAMC2, LAMB3, LAMA3, HRAS, HNF4A, HCFC1, GDI1, GABRD, FOS, FLNA, FLI1, FGFR2, ACSL4, DNM2, DMD, DLG3, DHODH, DHCR7, CYBB, CYBA, CRKL, CLCN4, SERPINH1, CAV1, BCR, RERE, ARF1, MAP1B, MECP2, KMT2A, PPARG, TBX3, SYP, SMARCB1, SKI, RYR1, RPS6KA3, RAD21, PEX5, PEX2, PEX19, MAPK1, PPP2R5D, PEX14, MTM1, PEX13, PEX12, PEX10, PEX6, PEX1, PAK3, OTC, NPHS1, NEFH, NCF4, NCF2, MYF6, NCF1
-
Actg2-Related Disorders
Gene_reviews
Bladder involvement can range from neonatal megacystis and megaureter (with its most extreme form of prune belly syndrome) at the more severe end, to recurrent urinary tract infections and bladder dysfunction at the milder end. ... Nomenclature Megacystis-microcolon-intestinal hypoperistalsis syndrome (MMIHS) may also be referred to as familial visceral myopathy or Berdon syndrome. ... Chronic atrial and intestinal dysrhythmia (CAID) is the constellation of sick sinus syndrome (SSS) with aberrant sinus node pacing in the heart and intestinal pseudoobstruction [Chetaille et al 2014]. ... T he combination of CIPO, Barrett esophagus, and cardiac abnormalities caused by biallelic pathogenic variants in RAD21 is called Mungan syndrome [Bonora et al 2015]. Bladder involvement has not been reported. ... Other Causes of Bowel Obstruction In neonates, the clinical presentation of intestinal hypoperistalsis syndrome can mimic other causes of bowel obstruction, such as Hirschsprung disease.
-
Esco2 Spectrum Disorder
Gene_reviews
Diagnosis ESCO2 spectrum disorder comprises a phenotypic continuum that ranges from Roberts syndrome at the severe end to SC phocomelia at the milder end. ... Note: PCS/HR is different from premature sister chromatid separation (PSCS) described in Cornelia de Lange syndrome and premature centromere division (PCD) associated with mosaic variegated aneuploidy syndrome, in which separation and splaying involves not only the centromeric regions but also the entire sister chromatids [Plaja et al 2001, Kaur et al 2005]. ... They named this condition the pseudothalidomide or SC syndrome (for the initials of the surnames of the 2 families described) [Herrmann et al 1969]. ... Other synonyms used for Roberts syndrome in the past are Appelt-Gerken-Lenz syndrome, hypomelia-hypotrichosis-facial hemangioma syndrome, tetraphocomelia-cleft palate syndrome, and pseudothalidomide syndrome. ... Phenotypic overlap of Baller-Gerold and Roberts syndrome was noted in an individual with bicoronal synostosis and bilateral radial hypoplasia, initially diagnosed with Baller-Gerold syndrome and later found to have premature centromere separation [Huson et al 1990]. 7.
-
Cystinosis
Gene_reviews
Growth hormone administration improves height velocity in prepubertal children. Renal tubular Fanconi syndrome. Infants with untreated nephropathic cystinosis show signs of renal tubular Fanconi syndrome – i.e., generalized proximal tubular dysfunction – as early as age six months. ... Differential Diagnosis Renal tubular Fanconi syndrome. Untreated nephropathic cystinosis is the most common identifiable cause of renal tubular Fanconi syndrome in childhood. ... Inheritance is autosomal recessive. Lowe syndrome (oculocerebrorenal syndrome) is found in males and involves the eyes (cataracts, glaucoma, decreased visual acuity), central nervous system (hypotonia, intellectual disability), and kidneys (Fanconi syndrome). ... Glucosuria associated with renal tubular Fanconi syndrome can result in misdiagnosis as diabetes mellitus. ... Electrolyte abnormalities can suggest Bartter syndrome. The rickets of cystinosis can falsely suggest vitamin D-deficient rickets.
-
Temporomandibular Joint Dysfunction
Wikipedia
This article is about the syndrome with joint pain. For the range of diseases affecting the joint, see Temporomandibular joint pathology . ... For example, in the United Kingdom , the term pain dysfunction syndrome is in common use. [5] In the United States, the term temporomandibular disorder is generally favored. ... In addition to those already mentioned, examples include temporomandibular joint pain dysfunction syndrome , temporomandibular pain dysfunction syndrome , temporomandibular joint syndrome , temporomandibular dysfunction syndrome , temporomandibular dysfunction , temporomandibular disorder , temporomandibular syndrome , facial arthromyalgia , myofacial pain dysfunction syndrome , craniomandibular dysfunction (CMD), myofacial pain dysfunction , masticatory myalgia , mandibular dysfunction , and Costen's syndrome . ... For example: "Temporomandibular Pain and Dysfunction Syndrome – Aching in the muscles of mastication, sometimes with an occasional brief severe pain on chewing, often associated with restricted jaw movement and clicking or popping sounds." ... This classification, which effectively divides TMD into 2 syndromes, is followed by the American Academy of Orofacial Pain. [4] However, since most people with TMD could be placed into both of these groups, which makes a single diagnosis difficult when this classification is used.
-
Fibromyalgia
Wikipedia
"Cognitive dysfunction in fibromyalgia and chronic fatigue syndrome: new trends and future directions". ... "Emotional, physical, and sexual abuse in fibromyalgia syndrome: a systematic review with meta-analysis". ... "Psychological trauma and functional somatic syndromes: a systematic review and meta-analysis" . ... "Induction of neurasthenic musculoskeletal pain syndrome by selective sleep stage deprivation". ... "Chronic Widespread Pain and Fibromyalgia Syndrome: Life-Course Risk Markers in Young People" .ACR, COMT, TNF, BDNF, TAC1, CRP, HTR2A, SLC6A4, IL6, ASIC3, IL1B, IGF1, FMR1, OPRM1, MEFV, IL1A, IL4, CXCL8, IL10, NLRP3, NGF, MAOA, CAT, TSPO, NRXN3, PRKAA2, IL37, TRPV1, NOS3, POMC, PRKAA1, PRKAB1, TACR1, SOD1, CCL2, HLA-B, SLC6A3, NR3C1, GRIN2B, MIR145, TRPV2, GOLPH3, PCSK1N, TCP1, VDR, TAC4, TTN, TSHR, TRPM2, TPO, ANPEP, THAS, TF, MIRLET7D, CPP, TRPV3, TAL1, MIR143, APOC1, NPS, SNAP25, PSS, APOE, VEGFA, SCG2, C11orf40, MYT1L, PSIP1, ADRM1, PPARGC1A, CPQ, ABCB6, MFN2, SCLY, TP53INP2, CCL24, ZNF77, KLK4, ADIPOQ, EMB, ALB, HTR3B, DOCK11, NOL3, HT, CES2, PCLAF, CRH, CCL11, FES, HTR3A, HSD11B1, HP, HLA-A, HFE, GSR, GPX1, GH1, GCH1, MTOR, CHRM3, F2, IGF1R, ESR1, EPHA4, ENO1, EFNA4, EDN1, TSC22D3, DRD3, ACE, CSF2, CSF1R, CRYGD, CASP1, IGFALS, CCL4, OPRD1, SCN9A, PTGS2, PTH, MAPK8, CCR5, PNOC, ENPP2, PCYT1A, CNTN3, ADRB2, OPRL1, NPY, FAS, NOS2, NOS1, MTHFR, CYTB, MOS, MAOB, LNPEP, LEP, LAMC2, L1CAM, KRT7, RN7SL263P
-
Ehlers-Danlos Syndrome, Beasley-Cohen Type
Omim
Beasley and Cohen (1979) described a family they considered to have a novel form of presumably autosomal recessive EDS. Two of 7 sibs in a consanguineous Chinese family were affected. The proband was a 25-year-old man with hyperextensible joints, bilateral inguinal hernias, hyperelastic skin, chronically dislocated left hip, and 'lop' ears. The sister of the proband had most of the same physical findings as her brother, including narrow face, small eyes, and midface deficiency that differed from unaffected family members. Audiogram revealed moderate hearing reduction at all frequencies. She had apparent cataracts. Both sibs were mentally retarded. Easy bruisability, difficulty with wound healing, prominent veins, pseudotumors, and elastosis perforans were not present; scarring was minimal and sclerae were normal.
-
Growth Failure, Microcephaly, Mental Retardation, Cataracts, Large Joint Contractures, Osteoporosis, Cortical Dysplasia, And Cerebellar Atrophy
Omim
Shotelersuk et al. (2003) described a Thai sister and brother, born of healthy, unrelated parents, with a combination of features interpreted as representing a novel autosomal recessive multiple congenital anomalies/mental retardation (MCA/MR) syndrome. Both sibs had postnatal-onset growth deficiency, microcephaly with cortical dysplasia and cerebellar atrophy, bilateral lenticular cataracts, prominent supraorbital ridges, large joint contractures, severe osteoporosis, and mental retardation. ... Shotelersuk et al. (2003) compared and contrasted the syndrome in these 2 sibs with other syndromes characterized by microcephaly, mental retardation, growth failure, and childhood cataracts.
-
Hereditary Papillary Renal Cell Carcinoma
Orphanet
Hereditary papillary renal cell carcinoma (HPRCC) is a familial renal cancer syndrome characterised by a predisposition for developing bilateral and multifocal type 1 papillary renal carcinomas. ... Papillary carcinomas represent 10-15% of all RCCs but the annual incidence of familial RCC syndromes is less than 1 in 1,500,000. Etiology The syndrome is associated with germline mutations in the MET proto-oncogene (7q31) encoding a hepatocyte growth factor-responsive tyrosine kinase receptor.
-
Craniosynostosis Syndrome, Autosomal Recessive
Omim
Clinical Features Blair et al. (2000) described a consanguineous family of Pakistani origin in which 3 of 5 sibs had craniosynostosis of variable presentation. In addition, they had other congenital abnormalities, principally affecting ocular and limb development. The eldest daughter had global developmental delay from an early age, long face with a prominent nasal bridge, inner canthal distance of 3.2 cm, short philtrum with narrow upper lip, highly arched palate, cleft uvula, and a left divergent squint with abnormal eye movements and associated elevation of each eye on adduction. The next oldest daughter also had global developmental delay from an early age, long face with a prominent nasal bridge, short philtrum and narrow upper lip, asymmetric, low-set, and posteriorly rotated ears, bilateral colobomata of the iris, choroid, and optic disc associated with microphthalmia, horizontal pendular nystagmus, convergent squint, long and narrow fingers, and bilateral postaxial duplication of the fifth toe. Mapping Using intragenic and flanking microsatellite markers, Blair et al. (2000) developed linkage evidence that the disorder in this family was not caused by a mutation in any of the then-known craniosynostosis loci, including FGFR1 (136350), FGFR2 (176943), FGFR3 (134934), MSX2 (123101), and TWIST1 (601622).
-
Apocrine Gland Carcinoma
Wikipedia
ISBN 0-7216-2921-0 . v t e Cancers of skin and associated structures Glands Sweat gland Eccrine Papillary eccrine adenoma Eccrine carcinoma Eccrine nevus Syringofibroadenoma Spiradenoma Apocrine Cylindroma Dermal cylindroma Syringocystadenoma papilliferum Papillary hidradenoma Hidrocystoma Apocrine gland carcinoma Apocrine nevus Eccrine / apocrine Syringoma Hidradenoma or Acrospiroma / Hidradenocarcinoma Ceruminous adenoma Sebaceous gland Nevus sebaceous Muir–Torre syndrome Sebaceous carcinoma Sebaceous adenoma Sebaceoma Sebaceous nevus syndrome Sebaceous hyperplasia Mantleoma Hair Pilomatricoma / Malignant pilomatricoma Trichoepithelioma Multiple familial trichoepithelioma Solitary trichoepithelioma Desmoplastic trichoepithelioma Generalized trichoepithelioma Trichodiscoma Trichoblastoma Fibrofolliculoma Trichilemmoma Trichilemmal carcinoma Proliferating trichilemmal cyst Giant solitary trichoepithelioma Trichoadenoma Trichofolliculoma Dilated pore Isthmicoma Fibrofolliculoma Perifollicular fibroma Birt–Hogg–Dubé syndrome Hamartoma Basaloid follicular hamartoma Folliculosebaceous cystic hamartoma Folliculosebaceous-apocrine hamartoma Nails Neoplasms of the nailbed This Epidermal nevi, neoplasms, cysts article is a stub .