-
Multiple System Atrophy
Orphanet
Clinical manifestations include autonomic failure (orthostatic hypotension, syncope, respiratory disturbances (sleep apnea, stridor and inspiratory sighs), constipation, bladder dysfunction (early urinary incontinence), erectile dysfunction in males and Raynaud syndrome). In some cases, pyramidal signs (generalized hyperreflexia and positive Babinski sign) are observed. MSA-p, a form of MSA with predominant parkinsonian features, comprises bradykinesia, rigidity, irregular jerky postural tremor and abnormal postures (camptocormia, Pisa syndrome and disproportionate antecollis). ... Differential diagnosis Differential diagnosis of MSA-p includes Parkinson's disease and other atypical parkinsonian disorders (progressive supranuclear palsy, corticobasal syndrome). Differential diagnosis of MSA-c includes dominantly inherited spinocerebellar ataxias (SCAs 1, 2, 3, 6, and 7), fragile X-associated tremor/ataxia syndrome (FXTAS) and mitochondriopathies ( POLG1 gene mutations).
-
Nonsyndromic Hearing Loss And Deafness, Dfnb1
Gene_reviews
For example, among families segregating autosomal recessive nonsyndromic hearing impairment, GJB2 variants are causally related to congenital hereditary hearing impairment in: 25% of Palestinian families [Shahin et al 2002] An estimated 24% of Altaians from Siberia [Posukh et al 2005] 18% of Han Chinese [Duan et al 2015] 16% of the Iranian deaf population [Bazazzadegan et al 2012] 15% of Hui people [Duan et al 2015] 11% of Tibetan families [Duan et al 2015] Differential Diagnosis See Hereditary Hearing Loss and Deafness Overview for information on the genes causing nonsyndromic hereditary hearing loss and deafness. Table 3. Autosomal Recessive Syndromes Involving Hearing Loss View in own window Syndrome Distinctive Feature in Addition to Hearing Loss Gene(s) Hearing Loss Comments Usher syndrome type I Retinitis pigmentosa 1 See footnote 2 Congenital bilateral profound sensorineural hearing loss Vestibular areflexia w/delay in motor milestones (delayed sitting & walking) Unless fitted w/a cochlear implant, individuals w/Usher syndrome type 1 do not typically develop speech. RP develops in adolescence, resulting in progressively constricted visual fields & impaired visual acuity Usher syndrome type II USH2A ADGRV1 DFNB31 Congenital bilateral sensorineural hearing loss: mild-moderate in low frequencies; severe-profound in higher frequencies Intact vestibular responses w/no delay in motor milestones Clinical distinction between Usher syndrome types I & II: children w/type I usually delayed in walking until age 18 mos – 2 yrs (because of vestibular involvement); children w/type II usually begin walking at ~1 yr Usher syndrome type III CLRN1 Postlingual progressive sensorineural hearing loss Late-onset RP Variable impairment of vestibular function Older individuals w/Usher syndrome type III may have profound hearing loss & vestibular disturbance resembling Usher syndrome type I Pendred syndrome Thyroid enlargement SLC26A4 3 Hearing impairment usually congenital & often severe-profound (mild-moderate progressive hearing impairment also occurs) Bilateral dilation of the vestibular aqueduct 4 w/ or w/out cochlear hypoplasia 5 Either an abnormal perchlorate discharge test or goiter Thyroid abnormality variable 6 Vestibular function usually abnormal Jervell and Lange-Nielsen syndrome Cardiac conduction defects; long QTc, usually >500 msec KCNQ1 KCNE1 Congenital profound bilateral sensorineural hearing loss Long QTc is associated w/tachyarrhythmias, which may culminate in syncope or sudden death; >50% of untreated children w/JLNS die before age 15 years 7 Classic presentation: deaf child who experiences syncopal episodes during periods of stress, exercise, or fright Consider JLNS in any child w/congenital sensorineural deafness & negative DFNB1 testing – esp. w/a history of syncope or seizure or family history of sudden death before age 40 years 1. ... Pathogenic variants in genes at a minimum of nine different loci cause Usher syndrome type I. Genes at six of these loci – MYO7A (USH1B), USH1C , CDH23 (USH1D), PCDH15 (USH1F), USH1G , and CIB2 (USH1J) – have been identified. 3. Pendred syndrome and DFNB4 comprise a phenotypic spectrum caused by biallelic pathogenic variants in SLC26A4 (the most common cause), or double heterozygosity in either SLC26A4 and FOXI1 or SLC26A4 and KCNJ10 . 4. ... Autosomal recessive nonsyndromic hearing loss without an identifiable GJB2 variant and with progression of hearing loss: With a dilated vestibular aqueduct on thin-cut computed tomography (CT) of the temporal bones suggests DFNB4 [Azaiez et al 2007]; With a Mondini malformation on thin-cut CT of the temporal bones suggests Pendred syndrome. A perchlorate test and molecular genetic testing of SLC26A4 should be considered [Azaiez et al 2007].
-
Scleroderma, Familial Progressive
Omim
Gabrielli et al. (2009) provided a detailed review of scleroderma, including clinical manifestations and pathophysiology. See also Reynolds syndrome (613471), which shares some clinical features with scleroderma and CREST syndrome. ... Black et al. (1983) found in scleroderma due to vinyl chloride the same relationship to HLA types B8 and DR3 and the same anticentromere and other antibodies as in idiopathic scleroderma. CREST Syndrome Winterbauer (1964) defined and named the CRST syndrome (calcinosis, Raynaud syndrome, sclerodactyly, telangiectasia), a variant of scleroderma, when he was a Johns Hopkins medical student. (The CRST syndrome simulates hereditary telangiectasia; see 187300.) ... Frayha et al. (1977) described the CRST syndrome in mother and daughter. McColl and Buchanan (1994) described the CREST syndrome in 2 sisters of 1 family and a grandmother and grandson in a second family. ... Cytogenetics Rittner et al. (1988) found increased chromosomal breakage rate (ICBR) in 27 of 28 patients with systemic sclerosis; 5 patients with CREST syndrome, 4 with incomplete CREST, 1 with overlapping syndrome, and 18 with progressive systemic sclerosis were studied.IRF5, STAT4, CD247, TNIP1, PSORS1C1, CCN2, HLA-DQB1, COL1A2, CCN1, RHOB, SIRT1, HDAC5, S1PR5, SIRT7, PHF21A, XYLT2, ACTA2, NECTIN2, FOSL2, FBN1, FLI1, FSTL1, TGFBR1, CSF1, COL3A1, PTPN22, HLA-DPB1, PAH, TNFAIP3, BLK, DNASE1L3, PXK, ITGAM, NOTCH4, LMNA, WRN, JAZF1, TNPO3, LBR, IL12RB2, NFKB1, TYK2, KIAA0319L, SOX5, SMG7, CYP21A2, RNPC3, CRP, LINC01924, AVEN, RBM45, PRR12, VEGFA, PSORS1C2, DGKQ, CSK, IL13, ARHGAP31, ACE, EDN1, GSDMA, SAMD9L, DDX6, TPI1P2, TLR4, IL12RB1, IL10, IL6, IL4, TNF, IL17A, IL1B, IL1A, MSH5, IFNG, CDHR5, TNXB, NUP85, HSPA1L, NAB1, NCF2, HLA-DRB1, UROS, HLA-DRA, HLA-DQB2, HLA-DPA1, LRMDA, HFE, GRB10, GRB2, COL1A1, ZC3H10, CXCL8, MMP1, PHRF1, FN1, UROD, TIMP1, LINC00305, ANKS1A, MUC22, LEMD3, ATG5, TGFB1, IKZF2, AP4B1-AS1, HLA-DPA2, SLC29A3, POLD1, CCL2, GSDMB, SS18L1, AGER, SMAD3, MSH5-SAPCD1, ESYT1, STK19, ACR, IL12A-AS1, SLC12A3, PTPN11, LINC01500, CHRM5, CLCNKB, ICAM1, IFNA1, TOP1, CTLA4, IFNA13, FOXP3, CAV1, NOS3, BTG3, TNFSF13B, MMP9, HGF, PF4, HLA-DQA1, IL2, MMRN1, PPARG, CCL18, ACTB, CD19, CD226, MUC1, MIR21, MAPK1, MS4A1, IL22, KRT20, AIF1, ADIPOQ, CXCL10, HLA-C, SPARC, MMP2, IL33, MMP12, FAM167A, FLII, SMAD2, LGALS3, IL21, GEM, STAT3, AGT, DKK1, TSSK1B, IRAK1, TNC, FAS, POSTN, TGFBI, ENG, MIR29A, MIR155, CD40, BANK1, KIR3DL1, EGF, PLAU, BCL2, HIF1A, PSS, SMAD7, SFTPD, CD40LG, GRAP2, MAPK3, FGF2, TRIM21, DECR1, CDH11, VWF, CENPA, IGFBP3, TLR9, MAPK14, SELE, TNFSF14, AHSA1, CRK, AIMP2, GDF15, MMP3, CCL5, CD34, THBS1, HT, SERPINE1, CD28, CD22, KL, TSLP, FBL, POLDIP2, TNFSF4, RNF19A, FCGR3A, PLOD2, SELP, EXOSC10, AKT1, KIR2DS1, GSTK1, SELL, SLCO6A1, PTGS2, AGTR1, CENPB, IL18, CYCS, CXCR2, IL13RA1, IL2RA, PLG, PTPRC, TNFRSF14, CHI3L1, CXCL13, IL6ST, TRBV20OR9-2, CXCR4, NLRP3, TGFB2, CCL21, CXCL12, CCR7, POLR3A, HLA-A, HLA-B, EDNRA, ESR1, GATA3, IL23R, MUC5B, IRF7, TLR2, CEBPZ, SRF, SPP1, EGR1, HLA-G, MIF, IFNL1, GRN, MTOR, CD69, CD70, KIR2DS2, COL18A1, IL23A, DCN, SNRNP70, EGFR, TGFBR2, PTX3, CASP1, PDGFRB, MECP2, MET, TAP1, SMAD4, DDX19A, TAP2, MCAM, NAT2, TAL1, PRTN3, SERPINE2, PIK3CA, PIK3CB, PIK3CD, PIK3CG, PLAUR, SERPINF2, PMP22, HPGDS, SLPI, SERPINF1, RARRES2, REN, TSSK2, ROS1, S100A4, S100A7, S100A9, CCL7, CX3CL1, PI3, ICOS, MPO, NOS2, MPZ, TAGLN, GDE1, MYBL2, SCLY, SLC27A5, NFE2L2, NM, TLR8, TLR7, PDGFRA, EGFL7, TNFRSF11B, ADAMTS13, P4HB, IL21R, NOX4, RO60, TBX21, PDGFA, SRY, IRF8, EDNRB, GSTM1, COMP, CSF2, CTNNB1, DDX46, CYP2B6, CYP2D6, DNMT1, DPP4, LRPPRC, LOX, EPHB2, VDR, EZH2, PTK2B, PLD4, FCGR3B, FCN2, VCAM1, DBA2, IL17F, FOS, FOSB, ACKR1, GABPA, GPI, MIR126, CCR8, CCR6, BLM, TNFSF10, ADAM8, NR0B1, PDE5A, ALOX5, CCR2, AQP3, IKBKG, DHX16, ATM, BCL6, KLF5, CENPC, CD163, CASP3, SERPINH1, CD14, CD86, CD58, CD68, MIR196A1, FGF23, MIR150, CEL, CXCR3, SDC2, GSTT1, KRT7, IFN1@, IFNAR1, JUNB, TNNC1, TNFRSF1B, IGFBP5, IL1R1, KIR3DL2, IL1RN, SEMA4A, SMOC1, IL16, ISG20, ITGA5, TIMP2, KIR2DL2, ITGB2, THY1, KCNA5, JUN, JUND, RETN, KLK1, PARP9, HRAS, ATP8B4, HLA-DRB5, HAX1, TRAF6, ZBP1, LGALS9, LEP, WDR11, GZMA, TP53, TWIST1, GTF2I, COPB2, MSC, ASAP2, SLC33A1, ICOSLG, KLF4, CCL27, APLN, OSMR, EIF2S2, SMG1, KDM6B, UTP14A, PAPOLA, UTS2, EIF2B4, SPAG9, MBD4, ACSBG1, BICD2, EIF2B2, EIF2B5, PLCL2, TIMELESS, SLIT2, FHL5, UBE4A, PPIG, SUB1, TNFSF15, SPIN1, ZNRD2, EBI3, SEMA4D, RPP14, NXF1, LIAS, CDK2AP2, TAB1, ZMPSTE24, EMG1, SEMA3A, UBE4B, CDC42EP1, RNPS1, MAGI2, CNTRL, PLAA, NLRP1, TSIX, NID2, TUSC2, PDAP1, ACOT7, BMS1, TREX1, WIF1, ROCK2, RPP38, CXCL14, SEMA3E, MRPS30, DIABLO, SYNE1, CARD16, H4-16, IL34, LRRC34, SPAAR, HFM1, APOBEC3A, PRSS55, IFNL3, NANOS2, STING1, FCRL6, ACTBL2, LINC01193, DNAAF3, FAM111B, MMP21, CDCA5, MIR130B, PRRT2, SHCBP1, STN1, TRPM3, PDCD1LG2, SLC38A1, TLR10, FCRL4, LOXL4, NT5C1A, IL1F10, SPZ1, TUBA1C, HAVCR2, SYS1, INTS4, ENHO, MIR142, SIRT3, NCF1, MIR542, MIR618, TSPY3, POTEF, MIR708, C20orf181, CD24, TSPY10, MIR3606, OTUD6B-AS1, MIR5196, APOBEC3A_B, PGR-AS1, UPK3B, MTCO2P12, LGALS7B, POTEM, MIR145, MIR483, MIR146A, MIR17, MIR200C, MIR206, MIR26B, MIR30A, MIR17HG, POTEKP, MIR135B, MIR151A, PLF, KIR2DL5B, H4C15, MIR202, MIR193B, SUV39H2, NAA16, GGCT, IL17B, DLL1, TRBV28, TRBV20-1, TRBV3-1, LAMTOR2, FLVCR1, RGCC, SETD2, TBK1, TRPM5, IL19, EFEMP2, KLK12, DUOX2, MBL3P, RBMS3, BBC3, WNK1, DNAI1, CBX5, MMD, SEC14L2, RBFOX2, SMUG1, FAM215A, PLD3, IL17RA, POLR1A, TSKU, LRIT1, PRPF31, ERAL1, GREM1, HAVCR1, ASAP1, TAS2R13, SOST, TNFRSF12A, GOPC, CD248, SMURF1, MRTFA, SPG16, TRIB3, SCAF1, SIGIRR, TRPV4, RXFP1, FBRS, CHST8, GORASP1, SMURF2, IL25, PTLAH, DOK5, IL26, ROBO4, CSAD, OTUD6B, RTRAF, SF3B6, CD244, DUOX1, FBLIM1, IFT122, FAM20A, MTPAP, SLC47A1, CHRNA9, CARMIL1, HHAT, CDK5R1, CXCL5, NRP1, HLA-DMB, HLA-DPB2, HMGB1, HOXA9, HOXD13, HP, HPRT1, HSPA4, HSP90AA1, HSP90AB1, HSPG2, HTR2A, ICAM2, ID2, IFI16, IFIT1, IFNAR2, IGF1, HLA-DOA, HLA-DMA, IL2RB, HDC, FGF6, VEGFD, FKBP1A, FOXC1, FOXO3, FLNB, FLT1, FLT4, FOLR2, FPR2, GAB1, GCHFR, GLB1, GLI1, GSK3B, GYPA, HCL2, IL1RAP, IL3, MMP10, KIR2DS3, KNG1, KRAS, KRT1, LAG3, LGALS7, LIF, LIFR, LOXL2, LTA, SMAD1, MBD1, MBL2, CD46, MEFV, MFGE8, KITLG, MIP, KLRB1, KIR2DL3, IL6R, KDR, IL7R, IL9, IL10RB, IL11, IL12A, IL13RA2, TNFRSF9, IDO1, IRF4, ITGA2, ITGAL, ITGAV, ITGB3, ITGB5, ITGB8, JAK1, JAK2, FCGR2B, FCGR2A, F8, AQP1, ABCC6, RHOA, RHOC, ATF3, BGN, BMP6, BMPR2, BPI, BST2, CALCA, CAPG, CAST, CAT, RUNX3, CBL, CD1A, CD1D, AR, APOH, F2R, APOE, ABL1, ACACA, ACP3, ACTG1, ACTG2, ACVRL1, ADA, ADORA2A, PARP1, APLNR, ALB, ALDH3A2, ALOX5AP, ANGPT1, ANGPT2, ANXA1, AIRE, TNFRSF8, CD36, CD44, CD72, CYP1A1, CYP2C9, DDT, DLAT, DNAH5, ATN1, DSG2, HBEGF, ECE1, EDA, EGR2, EGR3, EIF2B1, ELANE, EP300, EPHA1, ETS1, CYBB, CYBA, CTSV, CHRM3, CDC42, CDH5, CDK5, CDK6, CDKN2A, CDSN, CENPE, CCR3, CTSG, LTB4R, CNR1, CNR2, CRYGD, CST3, CST4, NKX2-5, KMT2A, MMP14, NRP2, TBX1, TEK, TERC, TG, TIMP3, TIMP4, TLR3, TLR5, TM7SF2, TNFRSF1A, TPI1, TPO, CRISP2, TRPC1, TSHR, TSPY1, TTN, TNFRSF4, TRB, ADAM17, SUMO1, TAC1, SNAI2, SMN1, SMN2, SIGLEC1, SOAT1, SOD1, SOD3, SOX2, SP1, SPG7, SRPK2, SSB, STAT5A, STAT5B, STAT6, SULT1E1, SYT1, TXN, SCGB1A1, MNAT1, H4C11, H4C8, H4C2, H4C5, H4C13, H4C14, LTBP4, NR0B2, MMP23B, MMP23A, FCN3, USO1, RTCA, SSNA1, OASL, MBTPS1, TNFSF13, TNFRSF10B, H4C3, H4C12, EZR, H4C6, VIM, VIP, VIPR2, VTN, WNT1, WNT3, XRCC1, XRCC4, YY1, PTP4A1, EOS, ARHGEF5, CDR3, H4C9, AXIN2, H4C1, H4C4, SLC25A1, SLC11A1, SLC6A4, DDR2, OXCT1, P2RX7, PAK3, PAM, REG3A, PCBD1, PCM1, PDCD1, PDE4A, PDGFB, ENPP2, PGF, PGGT1B, PGM1, ABCB1, SERPINA1, PIK3C2B, OAS2, YBX1, ST3GAL1, NPPB, MS, MSN, MSR1, MT1G, MT3, COX2, MTHFR, MUC2, MX1, MYB, MYBPH, MYC, NDN, NFIC, NFIX, NOS1, NOTCH1, PLAT, POMC, PRKCA, PRKCB, S100A6, SCN9A, CCL17, CCL19, CCL24, CCL25, CXCL6, CXCL11, SERPINA3, XCL1, SDC1, SDHC, SELPLG, SFRP1, SFRP4, SFTPB, ST6GAL1, RXRB, RORC, ROCK1, PTBP1, PRKCD, PRKG1, MAP2K7, EIF2AK2, PRL, PRS, PSMB6, PTEN, RNASE3, PTGIR, PVR, PXN, RAC1, RAG2, RELA, RHCE, H3P8
-
Central Pontine Myelinolysis
Wikipedia
The authors intentionally avoided the term ‘demyelination’ to describe the condition, in order to differentiate this condition from multiple sclerosis and other neuroinflammatory disorders. [2] Since this original description, demyelination in other areas of the central nervous system associated with osmotic stress has been described outside the pons (extrapontine). [3] Osmotic demyelination syndrome ( ODS ) is the term used for both central pontine myelinolysis and extrapontine myelinolysis. [4] Central pontine myelinolysis, and osmotic demyelination syndrome, present most commonly as a complication of treatment of patients with profound hyponatremia (low sodium ), which can result from a varied spectrum of conditions, based on different mechanisms. ... There is a case report of central pontine myelinolysis occurring in the context of refeeding syndrome , in the absence of hyponatremia. [2] It has also been known to occur in patients suffering withdrawal symptoms of chronic alcoholism . [1] In these instances, occurrence may be entirely unrelated to hyponatremia or rapid correction of hyponatremia. ... "Centropontine myelinolysis related to refeeding syndrome in an adolescent suffering from anorexia nervosa". ... PMID 22343870 . ^ Abbott R, Silber E, Felber J, Ekpo E (October 2005). "Osmotic demyelination syndrome" . BMJ . 331 (7520): 829–30. doi : 10.1136/bmj.331.7520.829 . ... External links [ edit ] Classification D ICD - 10 : G37.2 MeSH : D017590 SNOMED CT : 6807001 MedPix Images of Osmotic Myelinolysis v t e Multiple sclerosis and other demyelinating diseases of the central nervous system Signs and symptoms Ataxia Depression Diplopia Dysarthria Dysphagia Fatigue Incontinence Nystagmus Optic neuritis Pain Uhthoff's phenomenon Investigations and diagnosis Multiple sclerosis diagnosis McDonald criteria Poser criteria Clinical Clinically isolated syndrome Expanded Disability Status Scale Serological and CSF Oligoclonal bands Radiological Radiologically isolated syndrome Lesional demyelinations of the central nervous system Dawson's fingers Approved [ by whom?
-
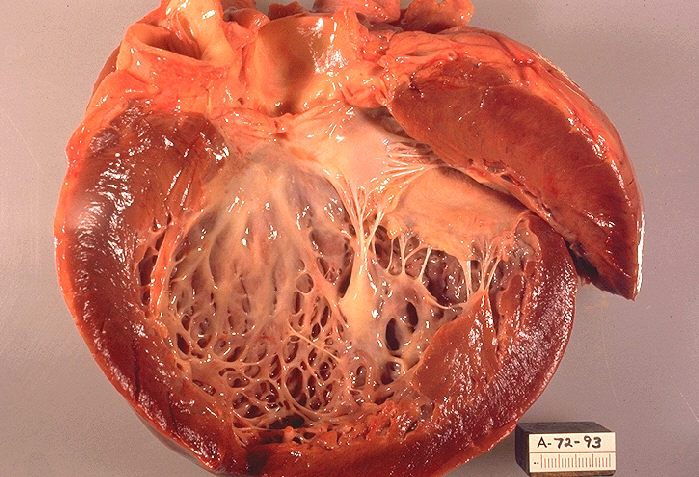
Cardiomyopathy
Wikipedia
Specialty Cardiology Symptoms Shortness of breath , feeling tired , swelling of the legs [1] Complications Heart failure , irregular heart beat , sudden cardiac death [1] [2] Types Hypertrophic cardiomyopathy , dilated cardiomyopathy , restrictive cardiomyopathy , arrhythmogenic right ventricular dysplasia , takotsubo cardiomyopathy [3] Causes Unknown, genetic , alcohol , heavy metals , amyloidosis , stress [3] [4] Treatment Depends on type and symptoms [5] Frequency 2.5 million with myocarditis (2015) [6] Deaths 354,000 with myocarditis (2015) [7] Cardiomyopathy is a group of diseases that affect the heart muscle . [1] Early on there may be few or no symptoms. [1] As the disease worsens, shortness of breath , feeling tired , and swelling of the legs may occur, due to the onset of heart failure . [1] An irregular heart beat and fainting may occur. [1] Those affected are at an increased risk of sudden cardiac death . [2] Types of cardiomyopathy include hypertrophic cardiomyopathy , dilated cardiomyopathy , restrictive cardiomyopathy , arrhythmogenic right ventricular dysplasia , and Takotsubo cardiomyopathy (broken heart syndrome). [3] In hypertrophic cardiomyopathy the heart muscle enlarges and thickens. [3] In dilated cardiomyopathy the ventricles enlarge and weaken. [3] In restrictive cardiomyopathy the ventricle stiffens. [3] In many cases, the cause cannot be determined. [4] Hypertrophic cardiomyopathy is usually inherited , whereas dilated cardiomyopathy is inherited in about one third of cases. [4] Dilated cardiomyopathy may also result from alcohol , heavy metals , coronary artery disease , cocaine use, and viral infections . [4] Restrictive cardiomyopathy may be caused by amyloidosis , hemochromatosis , and some cancer treatments . [4] Broken heart syndrome is caused by extreme emotional or physical stress. [3] Treatment depends on the type of cardiomyopathy and the severity of symptoms. [5] Treatments may include lifestyle changes, medications, or surgery. [5] Surgery may include a ventricular assist device or heart transplant . [5] In 2015 cardiomyopathy and myocarditis affected 2.5 million people. [6] Hypertrophic cardiomyopathy affects about 1 in 500 people while dilated cardiomyopathy affects 1 in 2,500. [3] [8] They resulted in 354,000 deaths up from 294,000 in 1990. [7] [9] Arrhythmogenic right ventricular dysplasia is more common in young people. [2] Contents 1 Signs and symptoms 2 Causes 3 Mechanism 4 Diagnosis 4.1 Classification 5 Treatment 6 See also 7 References 8 Further reading 9 External links Signs and symptoms [ edit ] The arrhythmia, ventricular fibrillation , seen on an ECG Symptoms of cardiomyopathies may include fatigue, swelling of the lower extremities and shortness of breath after exertion. [10] Additional symptoms of the condition may include arrhythmia , fainting, and dizziness. [10] Causes [ edit ] Cardiomyopathies are either confined to the heart or are part of a generalized systemic disorder, both often leading to cardiovascular death or progressive heart failure-related disability. ... Cardiomyocyte alterations and their persistent responses at the cellular level cause changes that are correlated with sudden cardiac death and other cardiac problems. [20] Diagnosis [ edit ] Normal sinus rhythm/EKG Among the diagnostic procedures done to determine a cardiomyopathy are: [10] Physical exam Family history Blood test ECG Echocardiogram Stress test Genetic testing Classification [ edit ] Structural categories of cardiomyopathy Stained microscopic section of heart muscle in hypertrophic cardiomyopathy Cardiomyopathies can be classified using different criteria: [21] Primary/intrinsic cardiomyopathies [22] Genetic Hypertrophic cardiomyopathy (HCM) Arrhythmogenic right ventricular cardiomyopathy (ARVC) LV non-compaction Ion Channelopathies Dilated cardiomyopathy (DCM) Restrictive cardiomyopathy (RCM) Acquired Stress cardiomyopathy Myocarditis , inflammation of and injury to heart tissue due in part to its infiltration by lymphocytes and monocytes [23] [24] Eosinophilic myocarditis , inflammation of and injury to heart tissue due in part to its infiltration by eosinophils [23] Ischemic cardiomyopathy (not formally included in the classification as a direct result of another cardiac problem) [22] Secondary/extrinsic cardiomyopathies [22] Metabolic/storage Fabry's disease Hemochromatosis Endomyocardial Endomyocardial fibrosis Hypereosinophilic syndrome Endocrine Diabetes mellitus Hyperthyroidism Acromegaly Cardiofacial Noonan syndrome Neuromuscular Muscular dystrophy Friedreich's ataxia Other Obesity-associated cardiomyopathy [25] Treatment [ edit ] Treatment may include suggestion of lifestyle changes to better manage the condition. ... PMID 27166925 . ^ Lipshultz, Steven E.; Messiah, Sarah E.; Miller, Tracie L. (5 April 2012). Pediatric Metabolic Syndrome: Comprehensive Clinical Review and Related Health Issues . ... Scholia has a topic profile for Cardiomyopathy . v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever Authority control NDL : 00571053PLN, TNNT2, MYBPC3, DMD, TNNI3, TNF, DES, SGCD, CRYAB, TAZ, EMD, MYH7, PRKAG2, DSP, PKP2, TTN, TTR, LAMP2, VCL, CSRP3, DSG2, ACTC1, TPM1, DSC2, RYR2, MYL2, GLA, RBM20, MYPN, NEXN, SGCB, POLG, TMEM43, MYOT, JPH2, EPG5, JUP, MYL3, LDB3, AGT, ABCC9, MYH6, SCN5A, SCO2, GAA, TNNC1, IL6, SOD2, MAPK3, CAV3, SLC22A5, IL1B, STAT3, CAT, LPL, HGF, PTPN11, PSEN1, NDUFS2, ANKRD1, TMEM70, MAPK1, IL1A, PRKAA2, FKTN, ATF3, CASQ2, MAPK14, IL4, CBR1, TLR2, RAF1, ACTN2, FASLG, RIT1, ITGB1, LIMS2, OLR1, NDUFV2, PARP1, MAP2K1, SOS1, ADRB2, EDN1, TCAP, AKT1, EPO, MYOZ2, PPP1R1A, APP, PPARD, GRK2, ADORA2A, TRIM63, ADCY5, COX1, POMC, CS, THPO, CYP2C9, ADCYAP1, MYOCD, HRAS, HSPE1, HSPD1, NPPB, MAPT, NEBL, MAP2K2, YWHAH, GATAD1, MAPK11, BRAF, KRAS, LAMA4, LDHA, BDKRB2, AVPR2, AVP, PRKCE, RHOJ, NRAS, PDK2, DTNA, FAS, MAP3K5, PTGS2, REEP1, PDLIM3, AQP2, PPARGC1A, NOS1, IFNG, TXN, UTS2R, RAD51, CCL2, ITGA7, NOS3, MIF, ADAM10, ACSL1, PDE2A, IGF1R, FKBP1B, FLNC, LRP1, LMNA, GOT1, FXN, TP53, ATP5F1B, XDH, TIMP2, UTS2, CASR, FHL1, HADHA, PNPLA2, ALPK3, GYG1, HFE, FKRP, SYNE2, HADHB, NPPA, VCP, CPT2, KCNQ1, ANO5, COX15, SDHD, POMT1, ATP6, GBE1, IDH2, MYO18B, GYS1, IDUA, DCAF8, MMUT, MPLKIP, C1QBP, AGL, TRIP4, HAMP, USP9X, DPM3, NEB, TPM3, PEX13, H19-ICR, PEX14, SLC40A1, BMP2, CENPE, RMRP, SLC25A20, GNE, GMPPB, SLC25A42, TPM2, CLPB, PEX7, HPS1, HNRNPA2B1, HNRNPA1, MIPEP, PEX16, IGF2, CDKN1C, ARSB, CDH23, WFS1, PEX10, KCNH1, POMT2, AQP4, XK, PEX19, GTF2H5, H19, PEX5, ACADS, ACTA1, RNF113A, KLHL41, KBTBD13, LAMA2, USP8, CEP85L, ACTB, UQCRFS1, PEX2, PEX6, RRM2B, PEX26, TK2, RAB3GAP2, PEX1, TTN-AS1, ALG1, KCNQ1OT1, AIP, GPC4, TFR2, TRNT, ACE, POMGNT1, NEU1, ERCC3, D2HGDH, ERCC2, PHYH, DLD, AHCY, ATAD3A, PCCB, AQP4-AS1, BAG3, PEX11B, GABPA, VAC14, PMM2, CISD2, PCCA, POMK, HBB, DSG2-AS1, SCN1B, GUSB, GTF2E2, GSN, GTPBP3, NFE2L2, RNASEH1, LTBP4, MYLK2, PEX12, PEX3, RPL36A-HNRNPH2, ABHD5, FIG4, GPC3, PPARA, CALR, GJA1, UTRN, PIK3CA, MYO6, SLC25A4, MGAM, CALCR, IGF1, CCR5, ILK, DECR1, SLC6A8, TGFB1, SI, PIK3CD, MEF2A, PIK3CG, PIK3CB, TRPV2, SIRT3, ADRB1, PRL, FGF21, LGALS3, S100A1, GATA4, TAC1, NLRP3, SLC5A1, SYNE1, EGFR, PPARGC1B, CYBB, HJV, CTNNB1, TLR3, NKX2-5, CSF3, BEST1, DNM1L, RND3, APRT, PRPF6, AARS2, KL, MBL2, REN, MFAP1, GH1, ACAD9, MYOF, HLA-DRB1, IL18, ADIPOQ, HIF1A, GLB1, S100B, PDE5A, VEGFA, HGS, MAPK8, PGM1, PRKCA, MASP2, RBCK1, GDF15, VIP, DENR, SSPN, APLN, TSFM, KEAP1, CTNNA3, MFN2, TLR4, MTO1, HSPB7, SDS, SDHB, SRSF5, PLEC, DAPK2, RBFOX2, SLC5A2, MLYCD, SIRT1, SLN, PPARG, TNNI3K, SUMO2, SORD, BSCL2, TAB2, ROS1, RIPK3, PPA2, TFAM, TRNT1, NAT2, TNC, MTFMT, DUSP4, COL3A1, SHROOM3, MYH7B, ERBB2, KLK1, ACE2, EYA4, PRDM16, RERE, RBM45, ESRRB, HSPB6, IL17A, MIR29C, ATN1, APOO, GNPTAB, IL1RN, CCN1, CYP2D6, FHL2, FHOD3, HMOX1, FOXO3, SESN2, MTOR, G6PD, COA6, MIR146A, RBFOX1, LCN2, MTTP, MYH2, COX2, ND1, MIR499A, SLC25A5, DMPK, CCR2, SARDH, ALDH2, ACTA2, ACADVL, NGF, NOS2, DAG1, CYP1A1, ALAS2, HARS1, DNAH8, NR3C2, RBM24, CRMP1, BIN1, CPT1A, CMYA5, SLCO1B1, THEMIS, HEXIM1, SENP5, TPCN2, CAVIN1, LINC-PINT, PIKFYVE, GOLGA6A, BOLA3, PDLIM5, HPSE, MARCHF8, LRRC10, NDUFS7, CHCHD10, GSTK1, PPP1R13L, SOX2-OT, JMJD1C, MPEG1, MYL12A, CD300C, PDE10A, CELF1, CAVIN4, FNDC5, TLR9, MIR122, ARFGEF2, HDAC6, MIAT, USP15, MIR323A, COA5, MIR378A, MIR424, MIR448, ELMO1, H4C15, BMS1, MIR410, SART3, RGS6, ADAMTS2, SDHAF1, HOTAIR, CHST3, HAND2, ABCG2, AK6, HAND1, MHRT, HDAC5, TNFSF12-TNFSF13, ABCC5, MIR29B1, MIR155, MIR18A, MIR195, MIR21, MIR221, MYL9, MIR23B, TUBA1B, MIR29A, MICU1, UBE4B, ABCB6, MIR29B2, EBI3, NAMPT, BCAP31, MIR320A, KIF20A, PPIF, MIR34A, ACTR2, MIR34B, EHD1, TBC1D1, UBR1, BTNL2, UBQLN1, MDFIC, EMC7, CELF4, CHPT1, LRRC7, SENP1, CD274, ALS2, CACNG8, SENP2, SLC28A3, MYLIP, UBE2T, ASTE1, TMBIM1, NOD2, MCAT, MTMR14, MARCKSL1, HPGDS, TWNK, TAX1BP3, IMMT, ERBIN, TRPM4, KLHL24, SNRK, RMND1, TNFRSF12A, COQ4, STX17, MOCOS, RCBTB1, CHDH, STAP2, FIS1, TRMU, AGK, DCAF6, IRX4, BEX1, TMEM126B, NOX3, ZC4H2, ANGPTL8, FSD1, MYH14, CACYBP, LAMP3, CALR3, ZFPM2, LRRC39, UFL1, DNAJC19, SPATA18, EMB, SLCO6A1, MGA, WDTC1, DKK1, RAB3GAP1, ISM2, MLXIP, STK38, UNC45B, ADAMTS13, LIAS, AMOTL1, XIRP1, NLRP6, H4-16, NNT, FBXO32, EVA1A, EHMT1, PANK2, PPP1R2C, LATS2, ITCH, FSD1L, TSSK1B, FBXL4, LDLRAP1, TOR1AIP1, PRRT2, MLIP, PART1, MYLK3, TIMM50, FNIP1, TGS1, MYL12B, EGLN3, SMUG1, TBX20, RPS27, LONP1, GFAP, GFI1, GNB3, GRK5, GPX3, GSK3A, GTS, GZMB, HAS3, HTT, HDAC2, HLA-B, HLA-C, HLA-DPB1, HMGB1, HSF2, GFER, FUT4, HSPA8, FOSL2, ECHS1, EDNRA, EDNRB, EPHB2, ESRRA, FAAH, FABP4, FABP3, FANCC, FANCF, FAP, FBN1, FGA, FGFR4, FOXO1, HSPA5, HSPB1, MME, KCNMA1, KDR, KNG1, LEP, LEPR, LORICRIN, LOXL2, LSAMP, SH2D1A, MAFD2, MATN1, SMCP, MEF2C, MEFV, MEIS1, MGAT1, KCNN3, KCNJ2, HSP90AA1, KCNH2, ICAM1, IGHG3, IL2RA, IL4R, IL7, IL10, IL12B, IL13, IL15, CXCL10, ISG20, ITGAM, ITGAX, ITGB6, KARS1, DUSP1, DSG1, DPYD, APOA1, APOE, ARSD, ARVD3, ATP2A2, AVPR1A, BDNF, BPI, BRCA1, BRCA2, C3, C5, C5AR1, VPS51, CA2, CAD, APOB, BIRC5, DPP4, APCS, ABL2, ABR, ACACA, ADAM8, ADM, ADPRH, ADRA1D, ADRA1A, ADRB3, AGTR1, AKT2, AKR1B1, ANGPT2, ANPEP, ANXA1, CASP1, CASP3, CBR3, CCNT1, CREM, CRP, CSNK2A2, CCN2, CTSB, CTSD, CTSL, CUX1, CYP2C19, CYP2E1, CYP19A1, CYP27B1, DCN, DIO2, DNM2, CR1, COX6B1, COMP, CDK2, CD34, CD36, SCARB1, SCARB2, CD69, CDH2, CDK9, COL4A1, CFL1, CFL2, CFTR, CMA1, CNR1, COL1A1, MLF1, MMP1, CD163, TFAP2A, THBS4, TIMP1, TIMP3, TJP1, TMPO, TRAF3, TRAF6, TRPC3, TRPM2, TSHR, TTK, TYK2, UBE3A, UCP2, VAV1, THBS3, PRDX2, VEGFB, TCF7L2, SLC18A3, SMARCA4, SMPD1, SUMO3, SOX2, SPARC, SPN, SPP1, SRI, SRF, SST, SULT1E1, STIM1, STRN, TACR1, VDR, WNT1, MMP9, H4C5, H4C14, LOH19CR1, ATRN, TP63, BECN1, TNFSF12, NRP1, CCN5, KAT2B, PER2, GYG2, SPAG9, IL1RL1, MSC, TSPOAP1, H4C13, H4C2, YWHAE, H4C8, ZBTB17, ALMS1, CXCR4, TFEB, FGF23, TCL1A, SLC14A2, DYSF, H4C9, H4C1, H4C4, H4C6, H4C12, H4C11, H4C3, SLC9A1, SLC8A1, SIX1, NPR1, PAH, SERPINE1, PCBP1, SERPINA5, PCMT1, PCNT, PDCD1, PDK4, PGC, PGK1, ABCB1, SLC25A3, PIM1, PKP1, POLR2A, OXTR, CCN3, ST3GAL4, NDUFS6, MMP14, MPO, MRE11, MST1, MT1B, CYTB, ND4, RNR2, TRNV, MUC2, MYBPC2, GADD45B, MYL4, NAGA, NDUFA5, PON1, PPA1, PPIA, PPID, RNASE4, ROCK1, RPL32, RPS19, AARS1, S100A6, S100A8, S100A9, SCD, SCO1, SDHA, SELP, SGCA, SGCG, SGSH, RLN2, RGS2, RAC1, MAPK7, PRH1, PRH2, PRKAA1, PRKAB1, PRKCB, PRKG1, MAP2K6, RAB6A, PSEN2, PTEN, PTH, PTHLH, PTPRC, RAB1A, SIRT1-AS
-
Hypoparathyroidism
Gard
Other causes, include low blood magnesium levels, a side effect of radioactive iodine treatment for hyperthyroidism , metabolic alkalosis , DiGeorge syndrome , and type I polyglandular autoimmune syndrome .CASR, GCM2, PTH, GATA3, AIRE, TBX1, PTH1R, FAM111A, HADHB, TRNW, COX2, TBX2, COX1, LIG4, ND1, NKX2-1, COX3, TRNF, ND4, ND5, ND6, TRNH, TRNL1, TRNQ, TRNS1, TRNS2, HBB, HIRA, HADHA, COMT, JMJD1C, ABCC6, PTRH1, ARVCF, ATP7B, NSUN2, COL4A5, RREB1, IRX5, SEC24C, UFD1, GP1BB, SOX3, QRSL1, FGF23, PTHLH, TRIM13, NR1I3, NUDT11, TBCE, VDR, SPG7, PHPT1, CXADRP1, CXADR, PRKAR1A, ARR3, HPT, ASAH1, SEA, ACKR3, AP2S1, CALCA, BRS3, CHD7, CORO7, STS, CLDN14, POF1B, NLRP5, TRPM6, HT, ADRA2B, PTPN22, CTLA4, CXCR6, FMR1, SSTR4, ADRA1A, HSP90AA1, TCF21, GPR42, GNA11, ST8SIA4, PTMS, FHL1, LPAR2, EDNRA, DIAPH2, DGCR, DGCR2, ADH1A
-
Toluene Embryopathy
Orphanet
A neurodevelopmental teratologic syndrome due to prenatal exposure to toluene. ... The features of toluene embryopathy often overlap with those seen in fetal alcohol syndrome.
-
Severe Congenital Hypochromic Anemia With Ringed Sideroblasts
Orphanet
STEAP3/TSAP6-related sideroblastic anemia is a very rare severe non-syndromic hypochromic anemia, which is characterized by transfusion-dependent hypochromic, poorly regenerative anemia, iron overload, resembling non-syndromic sideroblastic anemia (see this term) except for increased erythrocyte protoporphyrin levels.
-
List Of Voice Disorders
Wikipedia
These include: Vocal fold nodules Vocal fold cysts Vocal cord paresis Reinke's edema Spasmodic dysphonia Foreign accent syndrome Bogart–Bacall syndrome Laryngeal papillomatosis Laryngitis See also [ edit ] Aphasia Dysphonia Human voice Laryngectomy Parkinson's disease Speech disorder Vocology Voice changes during puberty References [ edit ] ^ Titze, I.R. (1994).
-
Craniofacial Cleft
Wikipedia
The combination of a Tessier number 6-7-8 is seen in the Treacher Collins syndrome . Tessier number 7 is more related to hemifacial microsomia and number 8 is more related to Goldenhar syndrome . ... Within craniofacial disorders and abnormalities , orofacial clefts, and specifically cleft lip (CL) and cleft palate (CP) are the most common in humans. [9] Occurrences of CL/P are most often (around seventy percent of cases) isolated and nonsyndromic, meaning they are not associated with a syndrome or inherited genetic conditions. [9] [10] Around thirty percent occur with other structural variances, and over 500 syndromes have been identified in which clefting is a principal feature. [9] [10] Clefting can result from teratogens , an agent that disrupts embryo development such as, radiation, maternal infection, chemicals, or drugs. [9] [10] Chromosomal abnormalities or mutations at single gene loci have also contributed to clefting development. [9] [10] Genetic causes are linked with most craniofacial syndromes, and CL/P and other orofacial clefts are recognized as heterogeneous disorders , meaning there are multiple recognized causes. [9] [11] Orofacial clefts have great phenotypic diversity, and their associated genetic environments have called for vast research and investigation. ... These clefts are also seen in various syndromes like Treacher Collins syndrome and hemifacial microsomia, which makes the treatment much more complicated. In this case, treatment of mouth anomalies is a part of the treatment of the syndrome. See also [ edit ] Related articles Ectrodactyly–ectodermal dysplasia–cleft syndrome Cleft hand Cleft lip and palate Syndromes Treacher Collins syndrome Hemifacial microsomia Goldenhar syndrome References [ edit ] ^ Moore, MH (1996). ... Mutations in SPECC1L, encoding sperm antigen with calponin homology and coiled-coil domains 1-like, are found in some cases of autosomal dominant Opitz G/BBB syndrome. J. Med. Genet. 52, 104–110. ^ Wilcox, A.
-
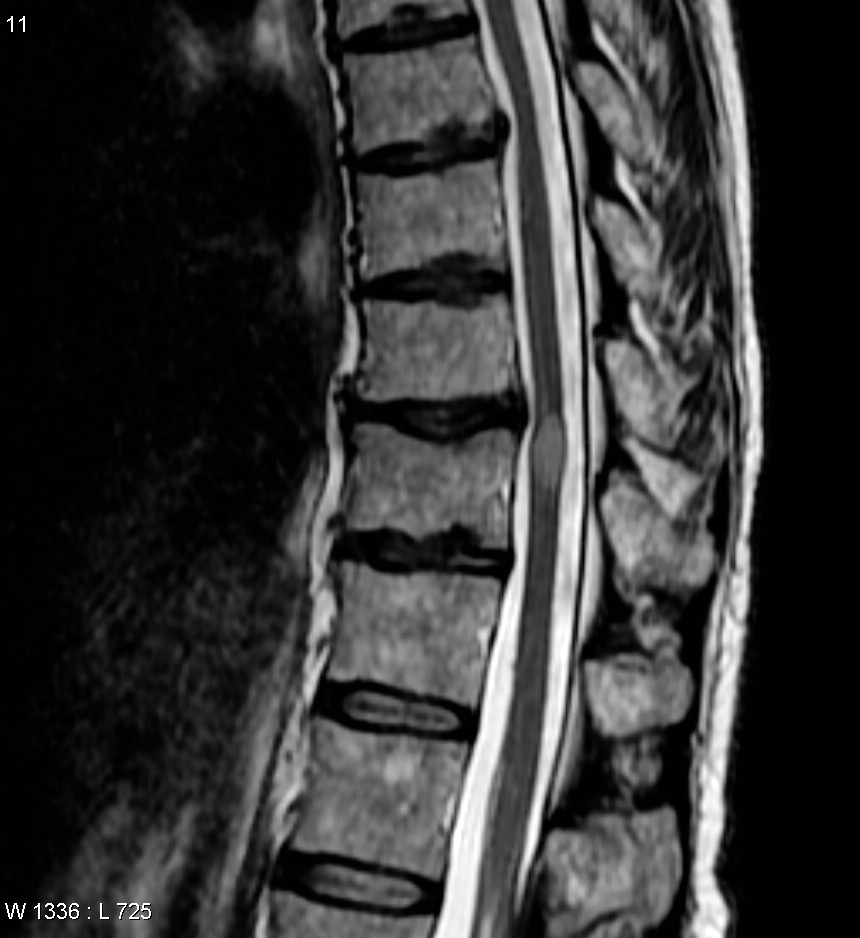
Transverse Myelitis
Wikipedia
Lyme disease gives rise to neuroborreliosis which is seen in a small percentage (4 to 5 per cent) of acute transverse myelitis cases. [12] The diarrhea-causing bacteria Campylobacter jejuni is also a reported cause of transverse myelitis. [13] Other associated causes include the helminth infection schistosomiasis , spinal cord injuries, vascular disorders that impede the blood flow through vessels of the spinal cord, and paraneoplastic syndrome . [10] Pathophysiology [ edit ] This progressive loss of the fatty myelin sheath surrounding the nerves in the affected spinal cord occurs for unclear reasons following infections or due to multiple sclerosis . ... Diagnostic criteria [ edit ] In 2002, the Transverse Myelitis Consortium Working Group proposed the following diagnostic criteria for idiopathic acute transverse myelitis: [17] Inclusion criteria Motor, sensory or autonomic dysfunction attributable to spinal cord Signs and symptoms on both sides of the body (not necessarily symmetrical) Clearly defined sensory level Signs of inflammation ( pleocytosis of the cerebrospinal fluid , or elevated immunoglobulin G , or evidence of inflammation on gadolinium -enhanced (MRI) Magnetic resonance imaging) Peak of this condition can occur anytime between 4 hours to 21 days after onset Exclusion criteria Irradiation of the spine (e.g., radiotherapy ) in the last 10 years Evidence of thrombosis of the anterior spinal artery Evidence of extra-axial compression on neuroimaging Evidence of arteriovenous malformation (abnormal flow voids on surface of spine) Evidence of connective tissue disease , e.g. sarcoidosis , Behçet's disease , Sjögren's syndrome , systemic lupus erythematosus or mixed connective tissue disease Evidence of optic neuritis (diagnostic of neuromyelitis optica ) Evidence of infection ( syphilis , Lyme disease , Human immunodeficiency virus , Human T-lymphotropic virus 1 , mycoplasma , Herpes simplex virus , Varicella-zoster virus , Epstein-Barr virus , cytomegalovirus , Human herpesvirus 6 or enteroviruses ) Evidence of multiple sclerosis (abnormalities detected on MRI and presence of oligoclonal antibodies in cerebrospinal fluid (CSF)) Investigations [ edit ] Individuals who develop TM are typically transferred to a neurologist or neurosurgeon who can urgently investigate the patient in a hospital. ... In an article in The Lancet , Ford suggested that acute myelitis could be a post-infection syndrome in most cases (i.e. a result of the body's immune response attacking and damaging the spinal cord) rather than an infectious disease where a virus or some other infectious agent caused paralysis. ... External links [ edit ] Classification D ICD - 10 : G37.3 ICD - 9-CM : 323.82 , 341.2 MeSH : D009188 DiseasesDB : 13265 Scholia has a topic profile for Transverse myelitis . v t e Focal lesions of the spinal cord General Myelopathy Myelitis Spinal cord compression By location Brown-Séquard syndrome Posterior cord syndrome Anterior cord syndrome Central cord syndrome Cauda equina syndrome Other Polio Demyelinating disease Transverse myelitis Tropical spastic paraparesis Epidural abscess Syringomyelia Syringobulbia Morvan's syndrome Sensory ataxia Tabes dorsalis Abadie's sign Subacute combined degeneration of spinal cord Vascular myelopathy Anterior spinal artery syndrome Foix–Alajouanine syndrome v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Paraneoplastic syndromes Endocrine Hypercalcaemia SIADH Zollinger–Ellison syndrome Cushing's syndrome Hematological Multicentric reticulohistiocytosis Nonbacterial thrombotic endocarditis Neurological Paraneoplastic cerebellar degeneration Encephalomyelitis Limbic encephalitis Opsoclonus Polymyositis Transverse myelitis Lambert–Eaton myasthenic syndrome Anti-NMDA receptor encephalitis Musculoskeletal Dermatomyositis Hypertrophic osteopathy Mucocutaneous reactive erythema Erythema gyratum repens Necrolytic migratory erythema papulosquamous Acanthosis nigricans Ichthyosis acquisita Acrokeratosis paraneoplastica of Bazex Extramammary Paget's disease Florid cutaneous papillomatosis Leser-Trélat sign Pityriasis rotunda Tripe palms Other Febrile neutrophilic dermatosis Pyoderma gangrenosum Paraneoplastic pemphigus
- Marie Unna Hereditary Hypotrichosis Orphanet
-
Patella Aplasia-Hypoplasia
Omim
Clinical Features Aplasia or hypoplasia of the patella, except as a feature of the nail-patella syndrome (NPS; 161200), is rare. Familial occurrence was reported by Bernhang and Levine (1973) and by Kiss et al. (1977). ... Bongers et al. (2004) stated that mutations in the TBX4 gene (601719), which cause the small patella syndrome (147891), are unlikely to cause PTLAH because the gene maps outside the critical region for PTLAH. ... Heterogeneity Bongers et al. (2002) described a family with isolated patella aplasia-hypoplasia in 3 generations in which linkage to the nail-patella syndrome locus on 9q34 and the PTLAH locus on 17q was excluded.
-
Non-Rhizomelic Chondrodysplasia Punctata
Orphanet
Clinical description X-linked dominant chondrodysplasia punctata (or Conradi-Hünermann-Happle syndrome; see this term) is characterized by the association of asymmetrical limbs, lamellar ichthyosiform erythroderma and cataract that may be unilateral. ... Other forms of non-rhizomelic chondrodysplasia punctata include chondrodysplasia punctata tibial-metacarpal type, Toriello-Higgins-Miller syndrome and chondrodysplasia punctata, Sheffield type (see these terms). ... Calcifications around the epiphyses may also be caused by fetal alcohol syndrome (see this term) and may be seen in fetuses born to mothers with disseminated lupus erythematosus (see this term).
-
Hereditary Dentin Defect
Orphanet
Differential diagnosis Differential diagnoses include hypocalcified forms of amelogenesis imperfecta, congenital erythropoietic porphyria, conditions leading to early tooth loss (Kostmann syndrome, cyclic neutropenia, Chediak-Higashi syndrome, histiocytosis X and Papillon-Lefevre syndrome), permanent teeth discoloration due to tetracyclines, and Vitamin D-dependent and vitamin D-resistant rickets (see these terms).
-
Diabetic Embryopathy
Orphanet
These ageneses are described as either isolated or of part of multiple malformation syndromes that are more common in individuals with maternal diabetes: caudal regression syndrome (a rare anomaly of the lower body pole that represents a continuum of congenital malformations ranging from isolated sacral agenesis to absence of the lumbosacral spine and major visceral anomalies) and DiGeorge anomaly (velo-cardio-facial syndrome).
-
Polyarthritis
Wikipedia
This condition is termed alphavirus polyarthritis syndrome. Sindbis virus , which is endemic in Northern Europe, Africa, the Middle East, and Australia, is the most widely distributed of the alphaviruses causing polyarthritis, though infection is usually mild or asymptomatic. ... Sometimes there is previous history of inflammatory joint problems and bilateral edema of lower limbs. Alphavirus Polyarthritis Syndrome has an incubation period of 3–21 days, depending on the specific virus, with either a gradual or sudden onset of fever, arthralgias, headache, and lymphadenitis and conjunctivitis in some forms. ... See also [ edit ] Polyarteritis nodosa External links [ edit ] Classification D ICD - 10 : M13.0 ICD - 9-CM : 711 - 716 MeSH : D001168 SNOMED CT : 416956002 v t e Diseases of joints General Arthritis Monoarthritis Oligoarthritis Polyarthritis Symptoms Joint pain Joint stiffness Inflammatory Infectious Septic arthritis Tuberculosis arthritis Crystal Chondrocalcinosis CPPD (Psudogout) Gout Seronegative Reactive arthritis Psoriatic arthritis Ankylosing spondylitis Other Juvenile idiopathic arthritis Rheumatoid arthritis Felty's syndrome Palindromic rheumatism Adult-onset Still's disease Noninflammatory Hemarthrosis Osteoarthritis Heberden's node Bouchard's nodes OsteophyteZFP36, COPA, HP, CD69, COL2A1, NOD2, PTPN22, DMP1, PTPN2, STAT4, MEFV, TNF, IL2RB, IL2RA, HLA-DRB1, NLRP1, ENPP1, CPT2, ANKRD55, CD247, RBM45, ACAN, HLA-C, CRYGD, GPI, RPS19, CRP, MBL2, VTCN1, PTH, PSMA6, SMUG1, TRAF1, TNFRSF1B, IL23A, CARD14, MBL3P, SHOC2, PRORP, RNPC3, HSPA14, IRF5, PDCD1, HK1, BRAF, CD40LG, LRBA, CDH11, VCAN, CTLA4, CTSK, DNASE2, ATN1, HLA-A, MMP14, HLA-DQA1, HSPD1, IL1B, IL10, IL17A, ALOX5, LTA, MMP1, MMP3, OR10A4
-
Basaloid Follicular Hamartoma
Wikipedia
External links [ edit ] Classification D ICD - 10 : Q82.5 OMIM : 605827 External resources Orphanet : 168632 v t e Cancers of skin and associated structures Glands Sweat gland Eccrine Papillary eccrine adenoma Eccrine carcinoma Eccrine nevus Syringofibroadenoma Spiradenoma Apocrine Cylindroma Dermal cylindroma Syringocystadenoma papilliferum Papillary hidradenoma Hidrocystoma Apocrine gland carcinoma Apocrine nevus Eccrine / apocrine Syringoma Hidradenoma or Acrospiroma / Hidradenocarcinoma Ceruminous adenoma Sebaceous gland Nevus sebaceous Muir–Torre syndrome Sebaceous carcinoma Sebaceous adenoma Sebaceoma Sebaceous nevus syndrome Sebaceous hyperplasia Mantleoma Hair Pilomatricoma / Malignant pilomatricoma Trichoepithelioma Multiple familial trichoepithelioma Solitary trichoepithelioma Desmoplastic trichoepithelioma Generalized trichoepithelioma Trichodiscoma Trichoblastoma Fibrofolliculoma Trichilemmoma Trichilemmal carcinoma Proliferating trichilemmal cyst Giant solitary trichoepithelioma Trichoadenoma Trichofolliculoma Dilated pore Isthmicoma Fibrofolliculoma Perifollicular fibroma Birt–Hogg–Dubé syndrome Hamartoma Basaloid follicular hamartoma Folliculosebaceous cystic hamartoma Folliculosebaceous-apocrine hamartoma Nails Neoplasms of the nailbed This Epidermal nevi, neoplasms, cysts article is a stub .
-
Thymus Hyperplasia
Wikipedia
External links [ edit ] Classification D ICD - 10 : E32.0 ICD - 9-CM : 254.0 MeSH : D013952 v t e Lymphatic disease : organ and vessel diseases Thymus Abscess Hyperplasia Hypoplasia DiGeorge syndrome Ectopic thymus Thymoma Thymic carcinoma Spleen Asplenia Asplenia with cardiovascular anomalies Accessory spleen Polysplenia Wandering spleen Splenomegaly Banti's syndrome Splenic infarction Splenic tumor Lymph node Lymphadenopathy Generalized lymphadenopathy Castleman's disease Intranodal palisaded myofibroblastoma Kikuchi disease Tonsils see Template:Respiratory pathology Lymphatic vessels Lymphangitis Lymphangiectasia Lymphedema Primary lymphedema Congenital lymphedema Lymphedema praecox Lymphedema tarda Lymphedema–distichiasis syndrome Milroy's disease Secondary lymphedema Bullous lymphedema Factitial lymphedema Postinflammatory lymphedema Postmastectomy lymphangiosarcoma Waldmann disease This article related to pathology is a stub .
-
Kraurosis Vulvae
Wikipedia
External links [ edit ] Classification D ICD - 10 : N90.4 ( ILDS N90.410) MeSH : D007724 DiseasesDB : 33803 v t e Female diseases of the pelvis and genitals Internal Adnexa Ovary Endometriosis of ovary Female infertility Anovulation Poor ovarian reserve Mittelschmerz Oophoritis Ovarian apoplexy Ovarian cyst Corpus luteum cyst Follicular cyst of ovary Theca lutein cyst Ovarian hyperstimulation syndrome Ovarian torsion Fallopian tube Female infertility Fallopian tube obstruction Hematosalpinx Hydrosalpinx Salpingitis Uterus Endometrium Asherman's syndrome Dysfunctional uterine bleeding Endometrial hyperplasia Endometrial polyp Endometriosis Endometritis Menstruation Flow Amenorrhoea Hypomenorrhea Oligomenorrhea Pain Dysmenorrhea PMS Timing Menometrorrhagia Menorrhagia Metrorrhagia Female infertility Recurrent miscarriage Myometrium Adenomyosis Parametrium Parametritis Cervix Cervical dysplasia Cervical incompetence Cervical polyp Cervicitis Female infertility Cervical stenosis Nabothian cyst General Hematometra / Pyometra Retroverted uterus Vagina Hematocolpos / Hydrocolpos Leukorrhea / Vaginal discharge Vaginitis Atrophic vaginitis Bacterial vaginosis Candidal vulvovaginitis Hydrocolpos Sexual dysfunction Dyspareunia Hypoactive sexual desire disorder Sexual arousal disorder Vaginismus Urogenital fistulas Ureterovaginal Vesicovaginal Obstetric fistula Rectovaginal fistula Prolapse Cystocele Enterocele Rectocele Sigmoidocele Urethrocele Vaginal bleeding Postcoital bleeding Other / general Pelvic congestion syndrome Pelvic inflammatory disease External Vulva Bartholin's cyst Kraurosis vulvae Vestibular papillomatosis Vulvitis Vulvodynia Clitoral hood or clitoris Persistent genital arousal disorder This dermatology article is a stub .