-
Pellucid Marginal Degeneration
Wikipedia
External links [ edit ] Classification D ICD - 10 : H18.7 ICD - 9-CM : 371.48 DiseasesDB : 33144 External resources eMedicine : article/1196382 v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
Placenta Accreta Spectrum
Wikipedia
Additional reported risk factors for placenta accreta include maternal age and multiparity , other prior uterine surgery , prior uterine curettage, uterine irradiation, endometrial ablation , Asherman syndrome, uterine leiomyomata , uterine anomalies , hypertensive disorders of pregnancy [ citation needed ] , and smoking. The condition is increased in incidence by the presence of scar tissue i.e. Asherman's syndrome usually from past uterine surgery, especially from a past dilation and curettage , [3] (which is used for many indications including miscarriage , termination , and postpartum hemorrhage ), myomectomy , [4] or caesarean section . ... Complications [ edit ] Damage to local organs (e.g., bowel , bladder ,uterus and neurovascular structures in the retroperitoneum and lateral pelvic sidewalls from placental implantation and its removal; Postoperative bleeding requiring repeated surgery; Amniotic fluid embolism ; Complications (such as dilutional coagulopathy , consumptive coagulopathy , acute transfusion reactions , transfusion-associated lung injury , acute respiratory distress syndrome , and electrolyte abnormalities ) caused by transfusion of large volumes of blood products, crystalloids , and other volume expanders; Postoperative thromboembolism , infection , multisystem organ failure , and maternal death . ... "Hysteroscopic treatment of severe Asherman's syndrome and subsequent fertility" . Human Reproduction . 14 (5): 1230–3. doi : 10.1093/humrep/14.5.1230 . ... "Placenta accreta: An association with fibroids and Asherman syndrome". Journal of Ultrasound in Medicine . 27 (11): 1623–8. doi : 10.7863/jum.2008.27.11.1623 .
-
Hematuria
Wikipedia
A glomerular etiology is suggested by dysmorphic red blood cells, protein, and cellular casts in the urine. [3] This requires the consultation of a nephrologist. [3] Common causes include: IgA nephropathy Thin glomerular basement membrane disease Hereditary nephritis (Alport's disease) Benign familial hematuria Glomerulonephritis Idiopathic hematuria is hematuria with an unknown cause. It is considered a glomerular syndrome. [5] Non-glomerular hematuria [4] [ edit ] Upper urinary tract [ edit ] Urinary stones (i.e. kidney stone ) Pyelonephritis Kidney cancer Ureteral cancer Lower urinary tract [ edit ] Urinary tract infection (UTI) Benign prostatic hyperplasia (BPH) Strenuous exercise Bladder cancer Urethral cancer Microscopic hematuria [ edit ] Microscopic hematuria requires medical testing for detection. ... Non-urinary hematuria [ edit ] Trauma , especially at the genitourinary area Vaginal bleeding Children [ edit ] Common causes of hematuria in children are: [7] congenital abnormalities – Non-vascular – ureteropelvic junction obstruction, posterior urethral valves, urethral prolapse, urethral diverticula, multicystic dysplastic kidney Vascular – arteriovenous malformations, hereditary hemorrhagic telangiectasias, renal vascular thromboses Acute nephritis Coagulopathy Urinary stones IgA nephropathy Post-streptococcal glomerulonephritis benign familial hematuria sickle cell trait or disease Alport syndrome Diagnosis [ edit ] After conducting a thorough history and physical examination, further medical testing is warranted. ... External links [ edit ] Classification D ICD - 10 : N02 , R31 ICD - 9-CM : 599.7 , 791.2 MeSH : D006417 DiseasesDB : 19635 External resources MedlinePlus : 003138 eMedicine : ped/951 Patient UK : Hematuria Media related to Hematuria at Wikimedia Commons v t e Kidney disease Glomerular disease See Template:Glomerular disease Tubules Renal tubular acidosis proximal distal Acute tubular necrosis Genetic Fanconi syndrome Bartter syndrome Gitelman syndrome Liddle's syndrome Interstitium Interstitial nephritis Pyelonephritis Balkan endemic nephropathy Vascular Renal artery stenosis Renal ischemia Hypertensive nephropathy Renovascular hypertension Renal cortical necrosis General syndromes Nephritis Nephrosis Renal failure Acute renal failure Chronic kidney disease Uremia Other Analgesic nephropathy Renal osteodystrophy Nephroptosis Abderhalden–Kaufmann–Lignac syndrome Diabetes insipidus Nephrogenic Renal papilla Renal papillary necrosis Major calyx / pelvis Hydronephrosis Pyonephrosis Reflux nephropathy v t e Components and results of urine tests Components Albumin Myoglobin hCG Leukocyte esterase Urine pregnancy test Ketone bodies Glucose Urobilinogen Bilirubin Creatinine RBC WBC Urinary casts Chemical properties Urine specific gravity Isosthenuria Urine osmolality Hypersthenuria Urine pH Urine anion gap Abnormal findings Red blood cells Hematuria ( Microscopic hematuria ) White blood cells Eosinophiluria Proteinuria Albuminuria / Microalbuminuria Albumin/creatinine ratio Urine protein/creatinine ratio Myoglobinuria Hemoglobinuria Bence Jones protein Small molecules Glycosuria Ketonuria Bilirubinuria Hyperuricosuria Aminoaciduria Other Bacteriuria Chyluria Crystalluria Authority control NDL : 00565683COL4A5, CFHR5, COL4A1, LMX1B, MYH9, ASPG, POMC, F7, PLAU, FOS, COL4A4, COL4A3, C3, B2M, NUMA1, NPM1, OCRL, NOTCH2, KIF1B, CD2AP, POU6F2, IL17RA, KANK2, PRDX1, MYO1E, SERPINF2, TMEM127, AGGF1, ITGA6, ITGA2, ITGA2B, ITGB3, ITGB4, SDHAF2, BCOR, LYZ, SMAD4, MAX, CD46, MDH2, PTPN22, MMACHC, PRTN3, PML, SPRY2, TSC1, TSC2, CLDN16, UMPS, YAP1, VHL, WT1, PRKAR1A, ZBTB16, TRIM28, SLC25A11, TRIP13, NUP93, GRHPR, TRAF3IP2, THBD, TGFB1, SRCAP, STAT5B, STAT4, STAT3, SPP1, SDHD, SDHC, SDHB, SDHA, RET, REST, RARA, CFI, TREX1, NUP133, IRAK1, DNASE1L3, IL17F, CLDN19, SCARB2, EFL1, GBA, GATA3, SLC37A4, TBL1XR1, FH, CD109, FGA, FIP1L1, F10, SLITRK6, IL17RC, DIS3L2, LMNB2, ENG, CCDC97, CLCNKB, DLST, HOGA1, GDF2, NABP1, H19, CLEC7A, HPRT1, HMOX1, HLA-DPB1, ACVRL1, HLA-DPA1, AGXT, CFH, HBB, MFF-DT, APOA1, C1R, APRT, CFB, GP1BB, IRF2BP2, GP1BA, GPC3, BRCA2, GLA, C1QA, CTLA4, IGAN1, CRP, TNF, KL, GPT, LAMC2, HPGDS, LAMA5, GSTP1, ALB, RAPGEF5, IGHA1, IQGAP3, AGT, ACE, CSF2, SFXN1, CX3CR1, INF2, TNFSF13B, ABCB6, MIR4511, GDF15, GSTK1, TLR9, RASSF1, ZMYND10, PCA3, PSAT1, FAM107A, RBM46, RNU1-1, SPAG8, CMIP, SLCO6A1, NID2, CFHR3, C1QL1, FCRLB, UBE2C, NPEPPS, ACAT1, GSTO1, CYP2C9, IL1RN, HSD11B2, HGF, PDIA3, GH1, GCH1, FN1, FGFR3, FCGR2B, FBN2, F3, F2, ESR1, DPYD, CYP1A1, IL17A, CRH, COL6A1, COL4A6, CLCN5, CISH, CDK5, CD14, CAT, CA9, BMP4, BCL2, KLK3, AMBP, ALCAM, IL6, KRT7, ADIPOQ, MAPK8, NRP1, IKBKG, FGF23, VIM, VEGFA, UBE2N, TWIST1, TLR4, TERT, SLC5A2, SGK1, CXCL12, PTGS2, PROS1, PLAG1, LASP1, PHEX, ACR, NOS3, NEUROG1, NEO1, MYBPH, MTHFR, COX2, MECP2, MCM5, MBL2, MB, MAT1A, LRPAP1, MTCO2P12
-
Eye Disease
Wikipedia
Version for 2007. [2] References [ edit ] WHO ICD-10 — Chapter VII Diseases of the eye and adnexa (H00-H59) v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis v t e Congenital malformations and deformations of eyes Adnexa Eyelid Ptosis Ectropion Entropion Distichia Blepharophimosis Ablepharon Marcus Gunn phenomenon Lacrimal apparatus Congenital lacrimal duct obstruction Globe Entire eye Anophthalmia ( Cystic eyeball , Cryptophthalmos ) Microphthalmia Lens Ectopia lentis Aphakia Iris Aniridia Anterior segment Axenfeld–Rieger syndrome Cornea Keratoglobus Megalocornea Other Buphthalmos Coloboma ( Coloboma of optic nerve ) Hydrophthalmos Norrie disease Medicine portalRPGRIP1L, PAX6, ABCA4, CHM, CACNA1F, MYOC, OAT, SOX2, OTX2, RPE65, BEST1, BMP4, CRB1, NDP, CNGA3, NYX, CRX, GUCY2D, MFRP, SEMA4A, STRA6, LRAT, GPR143, RPGR, CNNM4, KCNV2, CERKL, PDE6B, RDH5, SNRNP200, TOPORS, IQCB1, MFN2, ABHD12, WHRN, NR2E3, USH1C, FSCN2, PRPF6, MERTK, ZNF423, CIB2, PRPF8, SDCCAG8, VAX1, AIPL1, TSPAN12, GRIP1, ATP13A2, TRIM32, RIMS1, PRPF3, SLC24A1, WFS1, UNC119, PROM1, PLA2G5, POMC, PPT1, RBP3, RBP4, PRPH2, RGR, RHO, RLBP1, ROM1, RP9, RP1, RP2, RS1, SAG, ELOVL4, TIMP3, TULP1, TYR, TYRP1, USH2A, CLRN1, WT1, ALMS1, MKKS, FZD4, OFD1, ADAM9, RGS9, PRPF31, FLVCR1, TCTN3, ADGRV1, KCTD7, RDH12, B3GLCT, ZNF513, BBS5, USH1G, TTC8, C1QTNF5, CEP41, CACNA2D4, CDHR1, TMEM67, RAX2, TMEM126A, FAM161A, C8orf37, FREM1, BBS12, RD3, GPR179, PCARE, RGS9BP, KIF7, EYS, LRIT3, FREM2, LCA5, VSX2, CYP4V2, SLC24A5, NPHP4, MFSD8, ARL13B, ARL6, LRMDA, NPHP3, PITPNM3, SPATA7, BBS7, CLN6, MKS1, BCOR, AHI1, CNGB3, LZTFL1, TMEM216, SLC45A2, WDPCP, IMPG2, PITX2, BBS9, INVS, KLHL7, CABP4, RPGRIP1, TTC21B, OPA3, CEP290, FRAS1, PDZD7, DHDDS, TCTN2, BBS10, CC2D2A, TCTN1, CPLANE1, PCDH15, TMEM237, SMOC1, CDH23, PITX3, PRCD, HARS1, COL11A1, IMPDH1, COL9A1, COL4A1, COL2A1, CNGB1, CLN5, KCNJ13, CLN3, TPP1, CDH3, LRP5, CA4, MAK, TRPM1, MTTP, COL9A2, COL11A2, BBS2, VCAN, GRM6, GNAT2, GNAT1, FOXE3, FOXC1, GUCA1A, EFEMP1, GUCA1B, HCCS, CLN8, TIMM8A, IDH3B, CYP27A1, CYP1B1, CTSD, BBS4, CNGA1, BBS1, NPHP1, PHYH, PEX7, PDE6H, PDE6G, PDE6C, PDE6A, OPA1, OCA2, NRL, GRN, MYO7A, SCD, TSHR, VEGFA, CTLA4, HLA-DRB1, ARMS2, CFH, AMD1, AMD1P2, ICAM1, TNF, RBM45, CAPN5, NLRP3, IL13, SERPINF1, TTR, CD80, ADM, SIRT1, CTNNB1, MYP2, OLFM2, PLXNA2, IFNG, NRP1, ENO1, AKR1B1, CFTR, HLA-A, MAGEE1, TLR8, ENO2, TLR9, EDNRA, EDN1, CTNNBL1, EPRS1, UACA, GOT2, HCA1, SMIM10L2B, GJA8, GHRH, GDNF, FOXO1, PNPLA2, MIR301A, CCHCR1, MIR204, MIR145, F3, MIR132, ADAMTS18, CYP2C19, DNASE1, ADRB2, ADAMTS17, CASQ2, CDKN1B, CDS1, TAMM41, LINC01193, CCR7, ALB, CXCR3, APEX1, AHR, ARSI, ATM, HAVCR2, MAP3K8, DLG4, CRK, CRYAA, CRYBA1, MAPK14, PARP1, CCN2, IFNL2, HM13, CYP2C9, CYP2C18, CRB2, SRD5A3, DGKG, SMIM10L2A, NDEL1, PIK3CD, ANGPTL4, MYC, MPZ, LTBP3, VDR, VHL, LTBP2, LTA, LOX, DEK, AIMP2, LDHA, USP11, KDR, ITGB2, CDS2, TNFRSF14, MYP3, ITGB1, ITGAM, SQSTM1, SELENBP1, ITGAL, TNNT3, ABL1, IL18, TF, PPARA, MAPK1, PRL, PSMB9, PTGER4, PTPN12, PDGFRB, PDCD1, CDK16, P2RX7, RPE, NPY, NFKB1, CCL19, CCL21, SHBG, SOX11, SRPK1, SULT1E1, TBX3, TEAD1, CXCL10, ADIPOQ, GRIK5, SIRT3, HLA-DQB1, HLA-DQA1, HLA-DPB1, RNF19A, SOSTDC1, WWTR1, POLDIP2, SERPINA1, PTPN22, FGF21, FOXD3, GSTT1, GSTP1, CHIA, HCAR1, GSTM3, GSTM1, CD274, TMOD3, CPSF1, UBIAD1, HLA-DRA, HMGB1, GRAP2, HMOX1, IL16, IL12B, CXCL8, OPTN, IL6, PRG4, EFS, YAP1, OLFM1, IL1B, CCN1, IGF1R, AHSA1, POSTN, GNB5, IGF1, PPARGC1A, WIF1, ATF6, HTC2, HSP90AA1, TG
-
Proteinuria
Wikipedia
Severe proteinurina can cause nephrotic syndrome in which there is worsening swelling of the body. Contents 1 Signs and symptoms 2 Causes 2.1 Conditions with proteinuria 2.2 Bence–Jones proteinuria 3 Pathophysiology 3.1 Albumin and immunoglobins 4 Diagnosis 4.1 Analysis 5 Treatment 6 See also 7 References 8 External links Signs and symptoms [ edit ] Proteinuria often doesn't cause any symptoms and it may be discovered incidentally. [ citation needed ] Foamy urine is considered a cardinal sign of proteinuria, but only a third of people with foamy urine have proteinuria as the underlying cause. [1] It may also be caused by bilirubin in the urine ( bilirubinuria ), [2] retrograde ejaculation , pneumaturia (air bubbles in the urine) due to a fistula , [3] or drugs such as pyridium . [2] Causes [ edit ] There are three main mechanisms to cause proteinuria: Due to disease in the glomerulus Because of increased quantity of proteins in serum (overflow proteinuria) Due to low reabsorption at proximal tubule ( Fanconi syndrome ) Proteinuria can also be caused by certain biological agents, such as bevacizumab (Avastin) used in cancer treatment. ... Conditions with proteinuria [ edit ] Proteinuria may be a feature of the following conditions: [6] Dental mercury amalgam Nephrotic syndromes (i.e. intrinsic kidney failure ) Pre-eclampsia Eclampsia Toxic lesions of kidneys Amyloidosis Collagen vascular diseases (e.g. systemic lupus erythematosus ) Dehydration Glomerular diseases, such as membranous glomerulonephritis , focal segmental glomerulonephritis , minimal change disease ( lipoid nephrosis ) Strenuous exercise Stress Benign orthostatic (postural) proteinuria Focal segmental glomerulosclerosis (FSGS) IgA nephropathy (i.e. Berger's disease) IgM nephropathy Membranoproliferative glomerulonephritis Membranous nephropathy Minimal change disease Sarcoidosis Alport syndrome Diabetes mellitus ( diabetic nephropathy ) Drugs (e.g. ... HIV , syphilis , hepatitis , poststreptococcal infection , urinary schistosomiasis ) Aminoaciduria Fanconi syndrome in association with Wilson disease Hypertensive nephrosclerosis Interstitial nephritis Sickle cell disease Hemoglobinuria Multiple myeloma Myoglobinuria Organ rejection : [8] Ebola virus disease Nail–patella syndrome Familial Mediterranean fever HELLP syndrome Systemic lupus erythematosus Granulomatosis with polyangiitis Rheumatoid arthritis Glycogen storage disease type 1 [9] Goodpasture syndrome Henoch–Schönlein purpura A urinary tract infection which has spread to the kidney(s) Sjögren syndrome Post-infectious glomerulonephritis Living kidney donor [10] Polycystic kidney disease [11] This list is incomplete ; you can help by adding missing items with reliable sources .LMX1B, TGFB1, HAVCR1, AGTR1, NPHS1, INF2, TRPC6, MYH9, APOE, SPP1, COL4A5, HLA-DRB1, PAK2, PTGS2, REN, DPP4, SCNN1A, PPARA, POMC, CYBB, PAK1, NCK1, MPV17, LEP, LAMB2, IL1RN, IFNG, GUSB, CFH, HLA-B, NR4A1, DNASE1, HLA-DQA1, CTSL, AGT, MUC16, CTSB, ALB, ALOX5AP, SOD1, VEGFA, FAS, RHOA, CLCN5, NPHS2, NCK2, CXCL10, SORCS1, NCKAP5, TMEM163, ICAM1, LEPR, NCF2, MGAT5, RAB38, OPTN, CD55, C6, SERPINA1, VTN, CLU, SNRPD1, SLC9A1, SDC1, ACE, NPPB, ACTN4, HMOX1, PSTPIP1, SNAP29, GTF2IRD1, LPIN2, MAGI2, MAFB, AMMECR1, C3, SLC35A1, CORIN, WDR4, ADAMTS13, TREX1, FASTKD2, FAN1, KIF1B, NUP160, CD2AP, SLC7A7, BAZ1B, C1R, SGPL1, COL4A4, COL4A3, VHL, CLCNKB, CLIP2, WT1, ZAP70, TRIM25, ERCC8, CUBN, LAGE3, SLC25A11, SCARB2, OFD1, ITGA8, DGKE, APOL1, KCNE5, KANK2, COX6B1, CFB, NUP85, COQ8B, B2M, AMN, SLITRK6, COA8, LMNB2, WDR73, COX14, ATP7B, TP53RK, ARHGDIA, COX20, STOX1, APOA1, MFF-DT, PET100, VPS33A, WDR19, SH2B1, NUP107, MMACHC, PTPN22, TBL2, C1QA, SMARCAL1, TPRKB, COQ6, PLCE1, TACO1, ANLN, TBC1D8B, SARS2, SDHAF2, OSGEP, TMEM127, NUP133, PDSS2, HLA-DPB1, THBD, TRNS2, MDH2, G6PC, COX1, COX2, COX3, ND1, ND4, ND5, ND6, TRNE, TRNF, TRNH, TRNK, TRNL1, TRNN, TRNQ, TRNS1, HNF1B, MEFV, CD46, FN1, MAX, HNF4A, HLA-DPA1, CFI, GTF2I, GSN, GLA, INSR, IRAK1, ITGA3, GDNF, LCAT, GBA, GATA3, LIMK1, SLC37A4, LRP2, LYZ, TRNW, HELLPAR, MYO1E, SDHA, PTPRO, EHHADH, RET, RFC2, SAA1, DNASE1L3, SCO1, DLST, SDHB, PRTN3, SDHC, SDHD, CTNS, SLC12A3, CTLA4, COX10, COX8A, STAT4, FLT1, ELN, PRODH, ACSL4, FOXC2, NEU1, NOS3, NOTCH2, FH, OCRL, PRDX1, ERCC4, FGA, PAX2, PMM2, ERCC6, HPSE, F3, ADIPOQ, ADM, ACKR1, NR3C2, HPSE2, HP, ACE2, TFPI
-
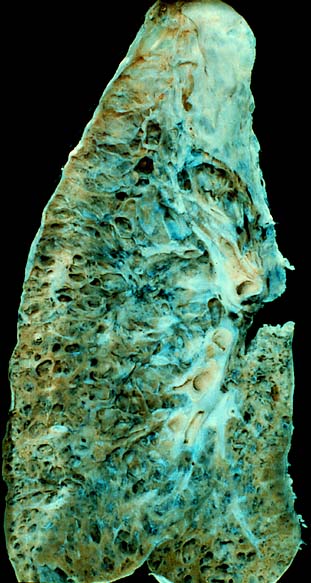
Interstitial Lung Disease
Wikipedia
They represent the majority of cases of interstitial lung diseases (up to two-thirds of cases). [8] They were subclassified by the American Thoracic Society in 2002 into 7 subgroups: [ citation needed ] Idiopathic pulmonary fibrosis (IPF): the most common subgroup Desquamative interstitial pneumonia (DIP) Acute interstitial pneumonia (AIP): also known as Hamman-Rich syndrome Nonspecific interstitial pneumonia (NSIP) Respiratory bronchiolitis-associated interstitial lung disease (RB-ILD) Cryptogenic organizing pneumonia (COP): also known as Bronchiolitis Obliterans Organizing Pneumonia (BOOP) Lymphoid interstitial pneumonia (LIP) Secondary [ edit ] Secondary ILDs are those diseases with a known etiology, including: Connective tissue and Autoimmune diseases Sarcoidosis Rheumatoid arthritis Systemic lupus erythematosus Systemic sclerosis Polymyositis Dermatomyositis Antisynthetase syndrome Inhaled substances Inorganic Silicosis Asbestosis Berylliosis Industrial printing chemicals (e.g. carbon black, ink mist) Organic Hypersensitivity pneumonitis (Extrinisic allergic alveolitis) Drug-induced Antibiotics Chemotherapeutic drugs Antiarrhythmic agents Infection Coronavirus disease 2019 [9] Atypical pneumonia Pneumocystis pneumonia (PCP) Tuberculosis Chlamydia trachomatis Respiratory Syncytial Virus Malignancy Lymphangitic carcinomatosis Predominately in children Diffuse developmental disorders Growth abnormalities deficient alveolarisation Infant conditions of undefined cause ILD related to alveolar surfactant region Diagnosis [ edit ] Pneumocystis pneumonia can present with interstitial lung disease, as seen in the reticular markings on this AP chest x-ray . ... The HRCT therefore provides approximately 10 times more resolution than the conventional CT chest, allowing the HRCT to elicit details that cannot otherwise be visualized. [10] [12] Radiologic appearance alone however is not adequate and should be interpreted in the clinical context, keeping in mind the temporal profile of the disease process. [10] Interstitial lung diseases can be classified according to radiologic patterns. [10] Pattern of opacities [ edit ] Consolidation Acute: Alveolar hemorrhage syndromes, acute eosinophilic pneumonia, acute interstitial pneumonia, cryptogenic organizing pneumonia Chronic: Chronic eosinophilic pneumonia, cryptogenic organizing pneumonia, lymphoproliferative disorders, pulmonary alveolar proteinosis , sarcoidosis Linear or reticular opacities Acute: Pulmonary edema Chronic: Idiopathic pulmonary fibrosis, connective tissue associated interstitial lung diseases, asbestosis, sarcoidosis, hypersensitivity pneumonitis, drug-induced lung disease Small nodules Acute: Hypersensitivity pneumonitis Chronic: Hypersensitivity pneumonitis, sarcoidosis, silicosis, coal workers pneumoconiosis, respiratory bronchiolitis, alveolar microlithiasis Cystic airspaces Chronic: Pulmonary langerhans cell histiocytosis, pulmonary lymphangioleiomyomatosis, honeycomb lung caused by IPF or other diseases Ground glass opacities Acute: Alveolar hemorrhage syndromes, pulmonary edema, hypersensitivity pneumonitis, acute inhalational exposures, drug-induced lung diseases, acute interstitial pneumonia Chronic: Nonspecific interstitial pneumonia, respiratory bronchiolitis associated interstitial lung disease, desquamative interstitial pneumonia, drug-induced lung diseases, pulmonary alveolar proteinosis Thickened alveolar septa Acute: Pulmonary edema Chronic: Lymphangitic carcinomatosis, pulmonary alveolar proteinosis, sarcoidosis, pulmonary veno occlusive disease [10] Distribution [ edit ] Upper lung predominance Pulmonary Langerhans cell histiocytosis, silicosis, coal workers pneumoconiosis, carmustine related pulmonary fibrosis, respiratory broncholitis associated with interstitial lung disease. ... Testing is available for ILDs related to alveolar surfactant region [ edit ] Surfactant-Protein-B Deficiency (Mutations in SFTPB ) Surfactant-Protein-C Deficiency (Mutations in SFTPC ) ABCA3-Deficiency (Mutations in ABCA3 ) Brain Lung Thyroid Syndrome (Mutations in TTF1 ) Congenital Pulmonary Alveolar Proteinosis (Mutations in CSFR2A, CSFR2B) Diffuse developmental disorder [ edit ] Alveolar Capillary Dysplasia (Mutations in FoxF1 ) Idiopathic pulmonary fibrosis [ edit ] Mutations in telomerase reverse transcriptase ( TERT ) Mutations in telomerase RNA component (TERC) Mutations in the regulator of telomere elongation helicase 1 (RTEL1) Mutations in poly(A)-specific ribonuclease (PARN) Treatment [ edit ] ILD is not a single disease, but encompasses many different pathological processes. ... External links [ edit ] Classification D ICD - 10 : J84.9 ICD - 9-CM : 518.89 , 508.1 , 515 , 516.3 , 714.81 , 770.7 MeSH : D017563 External resources Orphanet : 182095 00736 at CHORUS v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisSFTPC, COPA, FARSB, SOD2, IL18, IL1A, CCL2, MUC5B, SFTPB, HLA-DRB1, ITGA3, STING1, MUC2, NKX2-1, MARS1, TRIM21, ZKSCAN1, WNT3, AP3D1, NSF, SMPD1, SFTPD, AKAP13, MUC1, MAPT, IVD, FAM13A, CTNNA3, ATP11A, LINC02210, LINC02210-CRHR1, TSBP1-AS1, MAPT-AS1, ADAMTS7P4, KRTAP5-4, KANSL1, COPD, RNF168, SPPL2C, LRRC34, DPP9, ERF, DISP2, ACTRT3, STN1, DEPTOR, CSMD1, IFIH1, INPP5E, BTNL2, MYNN, TOLLIP, GBA, ABCA3, LINC02689, SCARB2, DSP, EGFR, CRP, TNF, ALK, PLF, RGS6, CHI3L1, RASA1, SLC27A5, DCPS, CEL, SLURP1, RIEG2, PRTN3, PARP9, RBM45, CCL18, TGFB1, SMUG1, TRIM33, PAH, MORC3, IFNG, MMP7, PADI4, PROS2P, IL17A, SFTPA1, CXCL8, IL2, CD274, IL1B, ADAM17, TERT, CSF2, TNFSF13B, ACR, SFTPA2, CYCS, KRT20, FLI1, PADI3, WNT5A, BLK, CABIN1, ABCA4, TP53, CXCL13, CAV1, FLNA, HARS1, FEV, GPT, TFF1, CRYGD, IL33, MS4A1, CX3CL1, HARS2, ROS1, CXCL10, CDC42EP1, PLEKHM3, HSPA4, ALB, IFNA1, IFNA13, IGF1, BTG3, IL4, IL6, IL10, IRF5, CNTRL, COX8A, AP3B1, LOXL2, TRBV28, TRBV20-1, CXCR6, PSS, MPC1, CD226, ACTB, SCLY, CD40LG, PADI2, SEC14L2, LILRB1, FOXP3, CD53, ERVK-12, IL17RA, PRPF31, ADH5, ERVK-11, CNMD, ERVK-2, BRD4, TRBV3-1, HPGDS, WDHD1, ERVK-22, PSIP1, BICD2, MIR7-1, TLR9, AQP4, HPS4, BCL2, BPIFB1, PIK3IP1, FOXP4, PGA3, C11orf40, IL34, ATF3, AKT1, CD22, SPAAR, FAS, AIRE, MIR7-3, GLIS3, ALOX5AP, ALOX5, MIR7-2, MIR200C, TSLP, BDNF, NT5C1A, SLA2, ADM, BANK1, RNPC3, CD19, CD14, MIR214, NCF1, CXCL16, ACE2, NOD2, CANX, CALR, PINK1, FSD1, KLF5, SLC2A10, MAP1LC3B, PGA4, FSD1L, POSTN, ETS1, YAP1, DNASE1L3, IL1RN, IL15, EGF, ITGAE, ITGAM, SLC26A3, KIT, KRT7, KRT14, LGALS1, LYZ, CYP2B6, NTF3, MATN1, MMP1, MMP9, MPO, MRC1, MSN, MST1, CX3CR1, CTNNB1, MUC5AC, NARS1, IDUA, ICAM2, ICAM1, HSPG2, FCER2, FCGR2B, FCN2, FGF2, FOXF1, FOLR2, FOSL2, ELN, GH1, GLRX, GPR15, GSTM1, HCRT, HDAC2, HGF, HLA-B, HLA-DPB1, EIF2B1, HLA-DRB5, HPS1, HSPA1A, HSPA1B, HSP90AA1, CCN2, PDGFA, TRAIP, EIF2B4, VCAM1, VEGFA, EZR, VTN, VWF, CCR3, FBN1, CXCR4, HMGA2, SEMA7A, FCN3, EIF2B2, PGA5, EIF2S2, LRRFIP1, CD163, PPIG, COX5A, NTN1, ITM2B, CXCL14, CCS, CENPB, PLXNC1, TTF1, TNFRSF1B, TNFRSF1A, COL4A5, PLG, SERPINF2, PSMB2, PTPRC, BRD2, S100A9, SAFB, CSF2RA, CCL3, CCL5, CCL17, CCL21, SELPLG, CPOX, SNRNP70, SPP1, SSTR2, STAT3, STAT4, TAL1, TRB, TGFA, TGFBR1, CHIT1
-
Stargardt Disease
Wikipedia
External links [ edit ] Classification D ICD - 10 : H35.5 ICD - 9-CM : 362.75 OMIM : 248200 MeSH : D000080362 DiseasesDB : 31282 SNOMED CT : 70099003 External resources Orphanet : 827 NCBI Genetic Testing Registry v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis v t e Genetic disorder , membrane: ABC-transporter disorders ABCA ABCA1 ( Tangier disease ) ABCA3 ( Surfactant metabolism dysfunction 3 ) ABCA4 ( Stargardt disease 1 , Retinitis pigmentosa 19 ) ABCA12 ( Harlequin-type ichthyosis , Lamellar ichthyosis 2 ) ABCB ABCB4 ( Progressive familial intrahepatic cholestasis 3 ) ABCB7 ( ASAT ) ABCB11 ( Progressive familial intrahepatic cholestasis 2 ) ABCC ABCC2 ( Dubin–Johnson syndrome ) ABCC6 ( Pseudoxanthoma elasticum ) ABCC7 ( Cystic fibrosis ) ABCC8 ( HHF1 , TNDM2 ) ABCC9 ( Dilated cardiomyopathy 1O ) ABCD ABCD1 ( Adrenoleukodystrophy , Adrenomyeloneuropathy ) ABCG ABCG5 ( Sitosterolemia ) ABCG8 ( Gallbladder disease 4, Sitosterolemia ) see also ABC transporters
-
Cardiogenic Shock
Wikipedia
"Inotropic agents and vasodilator strategies for the treatment of cardiogenic shock or low cardiac output syndrome" . The Cochrane Database of Systematic Reviews . 1 : CD009669. doi : 10.1002/14651858.CD009669.pub3 . ... "Cardiogenic shock with resultant multiple organ dysfunction syndrome" . Nursing Critical Care . 14 (4): 26–33. doi : 10.1097/01.CCN.0000565132.49413.54 . ^ "UpToDate" . ^ International Trauma Life Support for Emergency Care Providers (8 ed.). ... Flower, Churchhill Livingstone, Elsevier, 6th Edition [ page needed ] External links [ edit ] Classification D ICD - 10 : R57.0 ICD - 9-CM : 785.51 MeSH : D012770 DiseasesDB : 29216 External resources MedlinePlus : 000185 eMedicine : med/285 Cardiogenic Shock by eMedicine v t e Shock Distributive Septic shock Neurogenic shock Anaphylactic shock Toxic shock syndrome Obstructive Abdominal compartment syndrome Low volume Hemorrhage Hypovolemia Osmotic shock Other Spinal shock Cryptic shock Vasodilatory shock v t e Intensive care medicine Health science Medicine Medical specialities Respiratory therapy General terms Intensive care unit (ICU) Neonatal intensive care unit (NICU) Pediatric intensive care unit (PICU) Coronary care unit (CCU) Critical illness insurance Conditions Organ system failure Shock sequence SIRS Sepsis Severe sepsis Septic shock Multiple organ dysfunction syndrome Other shock Cardiogenic shock Distributive shock Anaphylaxis Obstructive shock Neurogenic shock Spinal shock Vasodilatory shock Organ failure Acute renal failure Acute respiratory distress syndrome Acute liver failure Respiratory failure Multiple organ dysfunction syndrome Neonatal infection Polytrauma Coma Complications Critical illness polyneuropathy / myopathy Critical illness–related corticosteroid insufficiency Decubitus ulcers Fungemia Stress hyperglycemia Stress ulcer Iatrogenesis Methicillin-resistant Staphylococcus aureus Oxygen toxicity Refeeding syndrome Ventilator-associated lung injury Ventilator-associated pneumonia Dialytrauma Diagnosis Arterial blood gas Catheter Arterial line Central venous catheter Pulmonary artery catheter Blood cultures Screening cultures Life-supporting treatments Airway management Chest tube Dialysis Enteral feeding Goal-directed therapy Induced coma Mechanical ventilation Therapeutic hypothermia Total parenteral nutrition Tracheal intubation Drugs Analgesics Antibiotics Antithrombotics Inotropes Intravenous fluids Neuromuscular-blocking drugs Recombinant activated protein C Sedatives Stress ulcer prevention drugs Vasopressors ICU scoring systems APACHE II Glasgow Coma Scale PIM2 SAPS II SAPS III SOFA Physiology Hemodynamics Hypotension Level of consciousness Acid–base imbalance Water-electrolyte imbalance Organisations Society of Critical Care Medicine Surviving Sepsis Campaign European Society of Paediatric and Neonatal Intensive Care Related specialties Anesthesiology Cardiology Internal medicine Neurology Pediatrics Pulmonology Surgery Traumatology v t e Symptoms and signs relating to the circulatory system Chest pain Referred pain Angina Levine's sign Auscultation Heart sounds Split S2 S3 S4 Gallop rhythm Heart murmur Systolic Functional murmur Still's murmur Diastolic Pulmonary insufficiency Graham Steell murmur Continuous Carey Coombs murmur Mitral insufficiency Presystolic murmur Pericardial friction rub Heart click Bruit carotid Pulse Tachycardia Bradycardia Pulsus paradoxus doubled Pulsus bisferiens Pulsus bigeminus Pulsus alternans Other Palpitations Apex beat Cœur en sabot Jugular venous pressure Cannon A waves Hyperaemia Shock Cardiogenic Obstructive Hypovolemic Distributive See further Template:Shock Cardiovascular disease Aortic insufficiency Collapsing pulse De Musset's sign Duroziez's sign Müller's sign Austin Flint murmur Mayne's sign Other endocardium endocarditis : Roth's spot Janeway lesion / Osler's node Bracht–Wachter bodies Pericardium Cardiac tamponade / Pericardial effusion : Beck's triad Ewart's sign Other rheumatic fever : Anitschkow cell Aschoff body EKG J wave Gallavardin phenomenon Vascular disease Arterial aortic aneurysm Cardarelli's sign Oliver's sign pulmonary embolism Right heart strain radial artery sufficiency Allen's test pseudohypertension thrombus Lines of Zahn Adson's sign arteriovenous fistula Nicoladoni sign Venous Friedreich's sign Caput medusae Kussmaul's sign Trendelenburg test superior vena cava syndrome Pemberton's sign
-
Genetics Of Obesity
Wikipedia
Part of a series on Human body weight General concepts Obesity ( Epidemiology ) Overweight Underweight Body shape Weight gain Weight loss Gestational weight gain Diet (nutrition) Weight management Overnutrition Childhood obesity ( Epidemiology ) Medical concepts Adipose tissue Classification of obesity Genetics of obesity Metabolic syndrome ( Epidemiology of metabolic syndrome ) Metabolically healthy obesity Obesity paradox Measurements Body adiposity index Body mass index Body fat percentage Body Shape Index Corpulence index Lean body mass Relative Fat Mass Waist–hip ratio Waist-to-height ratio Related conditions Diabetes ( Type 1 ) Eating disorder ( Anorexia • Bulimia • Binge eating disorder ) Food addiction Hyperthyroidism Malnutrition RED-S Starvation ( Starvation response ) PCOS Obesity-associated morbidity Arteriosclerosis Atherosclerosis Fatty liver disease GERD Heart disease Hypertension Obesity and cancer Osteoarthritis Prediabetes Sleep apnea Type 2 diabetes Management of obesity Anti-obesity medication Bariatrics Bariatric surgery Dieting ( List of diets ) Caloric deficit Exercise ( outline ) Liposuction Obesity medicine Weight loss camp Weight loss coaching Yo-yo effect Social aspects Comfort food Fast food ( Criticism ) Fat acceptance movement Fat fetishism Health at Every Size Hunger Obesity and the environment Sedentary lifestyle Social determinants of obesity Social stigma of obesity Weight cutting Weight class v t e A 1680 painting by Juan Carreño de Miranda of a girl presumed to have Prader-Willi syndrome [1] Like many other medical conditions, obesity is the result of an interplay between environmental and genetic factors. [2] [3] Studies have identified variants in several genes that may contribute to weight gain and body fat distribution; although, only in a few cases are genes the primary cause of obesity. [4] [5] Polymorphisms in various genes controlling appetite and metabolism predispose to obesity under certain dietary conditions. ... Some of these obesogenic or leptogenic genes may influence the obese individual's response to weight loss or weight management. [8] Contents 1 Genes 2 Genetic syndromes 3 See also 4 References Genes [ edit ] Although genetic deficiencies are currently considered rare, variations in these genes may predispose to common obesity. [9] [10] [11] Many candidate genes are highly expressed in the central nervous system . [12] Several additional loci have been identified. [13] Also, several quantitative trait loci for BMI have been identified. ... However, there are still challenges associated with detecting gene-gene interactions for obesity. [32] Genetic syndromes [ edit ] The term "non-syndromic obesity" is sometimes used to exclude these conditions. [33] In people with early-onset severe obesity (defined by an onset before 10 years of age and body mass index over three standard deviations above normal), 7% harbor a single locus mutation. [34] See also [ edit ] New World Syndrome Nutritional genomics Related: Human genetic variation References [ edit ] ^ Mary Jones. "Case Study: Cataplexy and SOREMPs Without Excessive Daytime Sleepiness in Prader Willi Syndrome. Is This the Beginning of Narcolepsy in a Five Year Old?" ... "The genetic contribution to non-syndromic human obesity". Nat. Rev. Genet . 10 (7): 431–42. doi : 10.1038/nrg2594 .
-
Diabetic Cardiomyopathy
Wikipedia
PMID 12742294 . v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever v t e Diabetes Types Type 1 Type 2 LADA Gestational diabetes Diabetes and pregnancy Prediabetes Impaired fasting glucose Impaired glucose tolerance Insulin resistance KPD MODY Neonatal Transient Permanent Type 3c (pancreatogenic) Type 3 Blood tests Blood sugar level Glycosylated hemoglobin Glucose tolerance test Postprandial glucose test Fructosamine Glucose test C-peptide Noninvasive glucose monitor Insulin tolerance test Management Diabetic diet Anti-diabetic drugs Insulin therapy intensive conventional pulsatile Cure Embryonic stem cells Artificial pancreas Other Gastric bypass surgery Complications Diabetic comas Hypoglycemia Ketoacidosis Hyperosmolar hyperglycemic state Diabetic foot ulcer Neuropathic arthropathy Organs in diabetes Blood vessels Muscle Kidney Nerves Retina Heart Diabetic skin disease Diabetic dermopathy Diabetic bulla Diabetic cheiroarthropathy Neuropathic ulcer Hyperglycemia Hypoglycemia Other Glossary of diabetes History of diabetes Notable people with type 1 diabetesATP2A2, AGT, SPP1, KLK1, APOA1, SLC25A4, RYR2, TNF, NFE2L2, AGTR2, INS, IGF1, PPARA, MAPK3, ACE2, PLN, MAPK1, CASR, NPPA, ACE, CTNNB1, HMOX1, BCL2, CASP9, CASP12, IL10, AGER, MYLK2, ERBB4, ERBB2, NOS3, ADIPOR1, ATP7A, CASQ2, BAD, A2M, TERT, SLC8A1, CASP8, ADIPOQ, XDH, CFL1, NRG1, CASP3, SIRT1, NLRP3, GABPA, MST1, FGF21, PRKAA1, PIK3CG, SIRT3, SLC5A2, KCNQ1OT1, PRKAB1, PRKAA2, REN, EDN1, DECR1, GCG, ATP6AP2, SLC2A1, TNNI3, TXNIP, MME, FOXO1, AKT1, PIK3CD, PIM1, SYK, GRK2, PIK3CB, PIK3CA, PPARG, BGLAP, MIR22, FGF19, MIR34A, GSK3B, PDE5A, KEAP1, IAPP, RBFOX2, DDAH2, DDAH1, BCL6, DAPK2, RNF19A, POLDIP2, ATF3, GSN, FGL2, NEDD4L, NR1H4, KL, CAV3, GRAP2, AIM2, ELMO1, MED13, MICU1, TBC1D1, SMC2, AHSA1, OGA, MAT2B, CEACAM1, INPP5F, RABGEF1, APRT, TOR2A, PYCARD, MIR18A, MIR193A, MIR195, MIR19B1, MIR200B, MIR21, MIR221, MIR92A2, MIAT, MIR451A, MIR503, MIR551B, CCR2, MIR675, ADRB2, ENHO, NEAT1, TAS2R12P, LIN28A, STS, SIRT6, TERF2IP, RETN, KLF4, NOD2, GSDMD, TINCR, CERS5, MTDH, TXNRD3, RLN3, ACVR1C, GPBAR1, LONP1, AIMP2, XPR1, PRKCD, MFAP1, MMP9, MYH6, FGF1, NGF, EPO, EPHB2, OPA1, PAEP, SERPINE1, PHB, EGFR, EGF, PTPA, DUSP5, MECP2, MAOA, SMAD7, CXCL8, GLP1R, HSD11B1, GJA1, IGF1R, IGF2, IL1B, IL17A, SMAD2, CXCL10, FN1, FOXO3, KNG1, LEP, LGALS3, DPP4, DCN, DIRAS3, CYP2J2, TLR2, TLR3, CRK, TP53, VDAC1, VDR, VEGFA, VEGFB, BEST1, CD36, BECN1, HDAC3, NR1I2, APLN, TAX1BP1, TGFB1, CRP, HNF1A, ROS1, MAPK8, NECTIN1, RAP1A, PARP1, RENBP, RLN2, RPS6KA1, STAT3, CYP2B6, SGK1, ST3GAL4, CTH, CSF3, MAPK14, NKILA
-
Combined Oxidative Phosphorylation Deficiency 39
Omim
More variable features may include hypotonia, seizures, and features of Leigh syndrome (256000) on brain imaging. There are variable deficiencies of the mitochondrial respiratory chain enzyme complexes in patient tissues (summary by Glasgow et al., 2017). ... Brain imaging of the younger sib showed progressive cerebellar atrophy and abnormal signals restricted to the midbrain suggestive of Leigh syndrome. By age 7 years, she was ventilator-dependent and bedridden with spasticity, bradycardia, and lack of developmental progress. ... Brain imaging in both patients showed T2-weighted abnormalities in the basal ganglia, consistent with Leigh syndrome, as well as abnormalities in other brain regions, including volume loss in the corpus callosum and cerebellum. ... INHERITANCE - Autosomal recessive GROWTH Other - Intrauterine growth retardation (in some patients) HEAD & NECK Head - Microcephaly (in some patients) Face - Myopathic facies Mouth - Drooling SKELETAL - Arthrogryposis multiplex congenita (in some patients) - Contractures (in some patients) MUSCLE, SOFT TISSUES - Hypotonia, axial - Hypertonia, limbs NEUROLOGIC Central Nervous System - Developmental delay - Developmental regression - Loss of motor skills - Speech delay - Loss of language - Loss of ambulation (in some patients) - Poor fine motor skills - Dysarthria - Dystonia - Involuntary movements - Spasticity - Seizures, refractory (in some patients) - Hypsarrhythmia (in some patients) - Brain imaging shows white matter abnormalities consistent with Leigh syndrome - Corpus callosum abnormalities - Cerebellar abnormalities - Cerebral volume loss - Enlarged ventricles - Pachygyria (in some patients) - Simplified gyral pattern (in some patients) METABOLIC FEATURES - Hypoglycemia (in some patients) Diabetes mellitus (in some patients) LABORATORY ABNORMALITIES - Increased serum lactate - Increased CSF lactate - Decreased mitochondrial respiratory chain activities, variable, in multiple tissues MISCELLANEOUS - Onset in first years of life - Some patients may have normal early development and then show regression MOLECULAR BASIS - Caused by mutation in the mitochondrial elongation factor G2 gene (GFM2, 606544.0001 ) ▲ Close
-
Idiopathic Head Tremor In Dogs
Wikipedia
Hormonal fluctuations may be a factor as well, since idiopathic head tremors are often more pronounced during estrus . [5] Diagnosis [ edit ] The diagnosis of idiopathic head tremors in dogs is based on signalment and medical history. [5] It is considered a diagnosis of exclusion, meaning other possible causes must be investigated and ruled out before diagnosing idiopathic head tremors. [6] Differential diagnoses include primary neurologic diseases like cerebellar disorders, steroid -responsive tremor syndrome ("little white shaker syndrome"), and exposure to toxins . ... "Clinical and Breed Characteristics of Idiopathic Head Tremor Syndrome in 291 Dogs: A Retrospective Study" . ... "Clinical and Breed Characteristics of Idiopathic Head Tremor Syndrome in 291 Dogs: A Retrospective Study" .
-
Crisscross Heart
Wikipedia
External links [ edit ] Classification D ICD - 10 : Q24.8 MeSH : D003420 DiseasesDB : 32853 SNOMED CT : 253269002 External resources Orphanet : 1461 v t e Congenital heart defects Heart septal defect Aortopulmonary septal defect Double outlet right ventricle Taussig–Bing syndrome Transposition of the great vessels dextro levo Persistent truncus arteriosus Aortopulmonary window Atrial septal defect Sinus venosus atrial septal defect Lutembacher's syndrome Ventricular septal defect Tetralogy of Fallot Atrioventricular septal defect Ostium primum Consequences Cardiac shunt Cyanotic heart disease Eisenmenger syndrome Valvular heart disease Right pulmonary valves stenosis insufficiency absence tricuspid valves stenosis atresia Ebstein's anomaly Left aortic valves stenosis insufficiency bicuspid mitral valves stenosis regurgitation Other Underdeveloped heart chambers right left Uhl anomaly Dextrocardia Levocardia Cor triatriatum Crisscross heart Brugada syndrome Coronary artery anomaly Anomalous aortic origin of a coronary artery Ventricular inversion
-
Epilepsia Partialis Continua
Wikipedia
External links [ edit ] Classification D ICD - 10 : G40.5 ICD - 9-CM : 345.7 MeSH : D017036 External resources eMedicine : neuro/653 v t e Seizures and epilepsy Basics Seizure types Aura (warning sign) Postictal state Epileptogenesis Neonatal seizure Epilepsy in children Management Anticonvulsants Investigations Electroencephalography Epileptologist Personal issues Epilepsy and driving Epilepsy and employment Seizure types Focal Seizures Simple partial Complex partial Gelastic seizure Epilepsy Temporal lobe epilepsy Frontal lobe epilepsy Rolandic epilepsy Nocturnal epilepsy Panayiotopoulos syndrome Vertiginous epilepsy Generalised Tonic–clonic Absence seizure Atonic seizure Automatism Benign familial neonatal seizures Lennox–Gastaut syndrome Myoclonic astatic epilepsy Epileptic spasms Status epilepticus Epilepsia partialis continua Complex partial status epilepticus Myoclonic epilepsy Progressive myoclonus epilepsy Dentatorubral–pallidoluysian atrophy Unverricht–Lundborg disease MERRF syndrome Lafora disease Juvenile myoclonic epilepsy Non-epileptic seizure Febrile seizure Psychogenic non-epileptic seizure Related disorders Sudden unexpected death in epilepsy Todd's paresis Landau–Kleffner syndrome Epilepsy in animals Organizations Citizens United for Research in Epilepsy (US) Epilepsy Action (UK) Epilepsy Action Australia Epilepsy Foundation (US) Epilepsy Outlook (UK) Epilepsy Research UK Epilepsy Society (UK)
-
Köhler Disease
Wikipedia
Classification D ICD - 10 : M92.6 ICD - 9-CM : 732.5 DiseasesDB : 7204 External resources eMedicine : orthoped/410 Orphanet : 2054 v t e Bone and joint disease Bone Inflammation endocrine : Osteitis fibrosa cystica Brown tumor infection : Osteomyelitis Sequestrum Involucrum Sesamoiditis Brodie abscess Periostitis Vertebral osteomyelitis Metabolic Bone density Osteoporosis Juvenile Osteopenia Osteomalacia Paget's disease of bone Hypophosphatasia Bone resorption Osteolysis Hajdu–Cheney syndrome Ainhum Gorham's disease Other Ischaemia Avascular necrosis Osteonecrosis of the jaw Complex regional pain syndrome Hypertrophic pulmonary osteoarthropathy Nonossifying fibroma Pseudarthrosis Stress fracture Fibrous dysplasia Monostotic Polyostotic Skeletal fluorosis bone cyst Aneurysmal bone cyst Hyperostosis Infantile cortical hyperostosis Osteosclerosis Melorheostosis Pycnodysostosis Joint Chondritis Relapsing polychondritis Other Tietze's syndrome Combined Osteochondritis Osteochondritis dissecans Child leg: hip Legg–Calvé–Perthes syndrome tibia Osgood–Schlatter disease Blount's disease foot Köhler disease Sever's disease spine Scheuermann's_disease arm: wrist Kienböck's disease elbow Panner disease
-
Macrophagic Myofasciitis
Wikipedia
Macrophagic myofasciitis Other names MMF Specialty Histopathology Pseudomedical diagnosis Macrophagic myofasciitis Pseudomedical diagnosis Risks Nocebo This article is part of a series on Alternative medicine General information Alternative medicine Alternative veterinary medicine Quackery (Health fraud) History of alternative medicine Rise of modern medicine Pseudoscience Antiscience Skepticism Skeptical movement National Center for Complementary and Integrative Health Terminology of alternative medicine Therapeutic nihilism Fringe medicine and science Acupressure Acupuncture Alkaline diet Anthroposophic medicine Apitherapy Applied kinesiology Aromatherapy Auriculotherapy Bates method Black salve Bodywork Bonesetter Bowen technique Breathwork Fake COVID-19 treatments Cancer treatments Charcoal cleanse Chiropractic Chiropractic treatment techniques Vertebral subluxation Christian Science Chromotherapy Colon cleansing Coffee enema Colorpuncture Colloidal silver Craniosacral therapy Crystal healing Cupping therapy Dental amalgam controversy Detoxification Foot detox Ear candling Energy medicine Esoteric energy Therapeutic touch Fabunan Antiviral Injection Facilitated communication Feldenkrais Method Functional medicine Hair analysis Herbal medicine Holistic dentistry Hologram bracelet Homeopathy Bach flower remedies Biological terrain assessment Hypnotherapy Iridology Ionized jewelry Jilly Juice Lightning Process Lymphotherapy Medical intuitive Mesmerism Magnet therapy Manual therapy Megavitamin therapy Mind–body interventions MMS Myofascial release NAET Naturopathy Oil pulling Orgone Orthomolecular medicine Orthopathy Osteomyology Osteopathy Ozone therapy Parapsychology Phrenology Psychic surgery Psychodermatology Radionics Rapid prompting method RBOP Reiki Reflexology Rolfing Scientific racism ThetaHealing Thought Field Therapy Urophagia Vaginal steaming Vision therapy Vitalism Young blood transfusion Zero balancing Conspiracy theories ( list ) Big Pharma conspiracy theory HIV/AIDS denialism OPV AIDS hypothesis Anti-vaccination Vaccines and autism MMR vaccine and autism Water fluoridation controversy GMO conspiracy theories Misinformation related to the COVID-19 pandemic Classifications Alternative medical systems Mind–body intervention Biologically-based therapy Manipulative methods Energy therapy Traditional medicine African Muti Southern Africa Ayurveda Ayurvedic acupressure Dosha Maharishi Vedic Approach to Health Balneotherapy Brazilian Bush medicine Cambodian Chinese Blood stasis Chinese herbology Dit Da Gua sha Gill plate trade Meridian Moxibustion Pressure point Qi San Jiao Tui na Zang-fu Chumash Curandero Faith healing Iranian Jamu Kambo Japanese Korean Mien Shiang Mongolian Prophetic medicine Shamanism Shiatsu Siddha Sri Lankan Thai massage Tibetan Unani Vietnamese Diagnoses Adrenal fatigue Aerotoxic syndrome Candida hypersensitivity Chronic Lyme disease Electromagnetic hypersensitivity Heavy legs Leaky gut syndrome Multiple chemical sensitivity Wilson's temperature syndrome v t e Macrophagic myofasciitis ( MMF ) is a histopathological finding involving inflammatory microphage formations with aluminium-containing crystal inclusions and associated microscopic muscle necrosis in biopsy samples of the deltoid muscle. ... A MMF disorder has been compared to autoimmune/inflammatory syndrome induced by adjuvants . [3] [4] A case-controlled study in France found those with MMF were more likely to have received aluminium-containing vaccines.
-
Mediastinal Germ Cell Tumor
Wikipedia
They are much less common than germ cell tumors arising in the testes , and account for only 1 to 5% of all germ cell neoplasms . Syndromes associated with mediastinal germ cell tumors include Hematologic Neoplasia and Klinefelter's syndrome . [4] History [ edit ] Malignant mediastinal germ cell tumors of various histologies were first described as a clinical entity approximately 50 years ago. [ when? ... "Metastatic mediastinal mature teratoma with malignant transformation in a young man with an adenocarcinoma in a Klinefelter's syndrome: Case report and review of the literature". ... PMID 29673950 . ^ C R Nichols; N A Heerema; C Palmer (1987). "Klinefelter's syndrome associated with mediastinal germ cell neoplasms" .
-
Deafness, Autosomal Dominant 34, With Or Without Inflammation
Omim
Heterozygous mutation in the NLRP3 gene can also cause several autoinflammatory disorders, including familial cold autoinflammatory syndrome-1 (FCAS1; 120100), Muckle-Wells syndrome (MWS; 191900), and CINCA syndrome (CINCA; 607115). ... Kurima et al. (2000) noted that the locus overlapped that of Muckle-Wells syndrome (191900), and suggested that they may be allelic disorders.
-
Laryngeal Cyst
Wikipedia
External links [ edit ] Classification D External resources eMedicine : article/837630 article/866019 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis
-
Sulfhemoglobinemia
Wikipedia
Paul's Hospital after falling asleep in a kneeling position, which caused compartment syndrome and a buildup of pressure in his legs. ... S2CID 39437785 . ^ "Patient bleeds dark green blood" , BBC News , 8 June 2007 ^ "Dark Green Blood In The Operating Theatre" , Medical News Today , June 8, 2007 External links [ edit ] Cancer Web Project Online Medical Dictionary Classification D ICD - 10 : D74.8 ICD - 9-CM : 289.7 MeSH : D013436 External resources MedlinePlus : 003371 v t e Diseases of red blood cells ↑ Polycythemia Polycythemia vera ↓ Anemia Nutritional Micro- : Iron-deficiency anemia Plummer–Vinson syndrome Macro- : Megaloblastic anemia Pernicious anemia Hemolytic (mostly normo- ) Hereditary enzymopathy : Glucose-6-phosphate dehydrogenase deficiency glycolysis pyruvate kinase deficiency triosephosphate isomerase deficiency hexokinase deficiency hemoglobinopathy : Thalassemia alpha beta delta Sickle cell disease / trait Hereditary persistence of fetal hemoglobin membrane : Hereditary spherocytosis Minkowski–Chauffard syndrome Hereditary elliptocytosis Southeast Asian ovalocytosis Hereditary stomatocytosis Acquired AIHA Warm antibody autoimmune hemolytic anemia Cold agglutinin disease Donath–Landsteiner hemolytic anemia Paroxysmal cold hemoglobinuria Mixed autoimmune hemolytic anemia membrane paroxysmal nocturnal hemoglobinuria Microangiopathic hemolytic anemia Thrombotic microangiopathy Hemolytic–uremic syndrome Drug-induced autoimmune Drug-induced nonautoimmune Hemolytic disease of the newborn Aplastic (mostly normo- ) Hereditary : Fanconi anemia Diamond–Blackfan anemia Acquired: Pure red cell aplasia Sideroblastic anemia Myelophthisic Blood tests Mean corpuscular volume normocytic microcytic macrocytic Mean corpuscular hemoglobin concentration normochromic hypochromic Other Methemoglobinemia Sulfhemoglobinemia Reticulocytopenia v t e Proteins that contain heme ( hemoproteins ) Globins Hemoglobin Subunits Alpha locus on 16 : α HBA1 HBA2 pseudo ζ HBZ θ HBQ1 μ HBM Beta locus on 11 : β HBB δ HBD γ HBG1 HBG2 ε HBE1 Tetramers stages of development: Embryonic HbE Gower 1 (ζ 2 ε 2 ) HbE Gower 2 (α 2 ε 2 ) HbE Portland I (ζ 2 γ 2 ) HbE Portland II (ζ 2 β 2 ) Fetal HbF/Fetal (α 2 γ 2 ) HbA (α 2 β 2 ) Adult HbA (α 2 β 2 ) HbA 2 (α 2 δ 2 ) HbF/Fetal (α 2 γ 2 ) pathology: HbH (β 4 ) Barts (γ 4 ) HbS (α 2 β S 2 ) HbC (α 2 β C 2 ) HbE (α 2 β E 2 ) HbO (α 2 β O 2 ) Compounds Carboxyhemoglobin Carbaminohemoglobin Oxyhemoglobin / Deoxyhemoglobin Sulfhemoglobin Other human Glycated hemoglobin Methemoglobin Nonhuman Chlorocruorin Erythrocruorin Other human: Myoglobin Metmyoglobin Neuroglobin Cytoglobin plant: Leghemoglobin Other Cytochrome Cytochrome b Cytochrome P450 Methemalbumin see also disorders of globin and globulin proteins