-
Rfc1 Canvas / Spectrum Disorder
Gene_reviews
Vertigo and hearing loss are not part of the syndrome but (as they are common in the general population) can independently occur. ... Typical age of onset: <25 yrs Frequent muscle weakness, pyramidal involvement (Babinski signs) & skeletal deformities (pes cavus, scoliosis) Assoc cardiomyopathy & diabetes Vision & hearing loss MT-ATP6 MT-TL1 1 mtDNA deletion NARP; MIDD/MELAS; Kearns-Sayre syndrome (See mtDNA Deletion Syndromes.) ... Mead et al [2013] Sensory Neuronopathy As sensory neuronopathy was identified in all individuals with genetically confirmed diagnoses and tends to appear early in the disease course, the differential diagnosis should initially encompass causes of acquired sensory neuronopathy including: Paraneoplastic syndrome Sjogren syndrome Acute and chronic immune-mediated disorders Metabolic disorders (diabetes mellitus, vitamin B 12 deficiency, copper deficiency) Toxins (alcohol, pyridoxine, platinum derivatives, pyridoxine intoxication) Late-Onset Cerebellar Ataxia Multisystem atrophy (MSA), a rapidly progressive neurodegenerative disease, is the main differential diagnosis in an individual with late-onset cerebellar ataxia [Fan et al 2020, Sullivan et al 2020, Wan et al 2020]. ... Additional causes of progressive cerebellar impairment to consider include: paraneoplastic syndromes; toxic, nutritional, vascular, and inflammatory conditions; and idiopathic (i.e., idiopathic late-onset cerebellar) ataxia. ... When bilateral vestibular hypofunction occurs with hearing and visual loss, Usher syndrome type I and Usher syndrome type II should also be considered.
-
Nr0b1-Related Adrenal Hypoplasia Congenita
Gene_reviews
This form of adrenal hypoplasia usually has normal mineralocorticoid secretion, although transient hyponatremia can be seen in severe cases [Guran et al 2016]. Syndromes with AHC or AHC-like manifestations as a feature include the following: Pena-Shokeir syndrome, type 1 (fetal akinesia deformation sequence) (OMIM 208150) Holoprosencephaly, alobar type Meckel syndrome (OMIM 249000) SeRKAL (46,XX se x r eversal with dysgenesis of k idneys, a drenals, and l ungs) caused by biallelic pathogenic variants in WNT4 (OMIM 611812) IMAGe syndrome ( i ntrauterine growth retardation, m etaphyseal dysplasia, A HC, ge nital abnormalities) caused by pathogenic variants in CDKN1C . Growth restriction is a key component of this condition. MIRAGE syndrome ( m yelodysplasia, i nfection, r estriction of growth, a drenal hypoplasia, g enital phenotypes, e nteropathy) caused by pathogenic variants in SAMD9 . Monosomy 7 can occur and is associated with the development of myelodysplastic syndrome. Triple A ( a chalasia, a ddisonianism, a lachrima) or Allgrove syndrome caused by biallelic pathogenic variants in AAAS (OMIM 231550) Natural killer cell and glucocorticoid deficiency with DNA repair defect (NKGCD) caused by biallelic pathogenic variants in MCM4 (encoding DNA replication licensing factor MCM4) (OMIM 609981) Primary adrenal insufficiency and steroid-resistant nephrotic syndrome caused by biallelic pathogenic variants in SGPL1 (see Sphingosine Phosphate Lyase Insufficiency Syndrome). ... Chromosomal abnormalities with AHC or AHC-like manifestations as a feature: Tetraploidy Triploidy Trisomy 19 Trisomy 21 5p duplication 11q- syndrome (OMIM 147791) Other forms of primary adrenal failure may need to be considered in boys presenting with primary adrenal failure: X-linked adrenoleukodystrophy (X-ALD) affects the nervous system white matter and the adrenal cortex. ... Other metabolic causes; for example, Wolman disease (see Lysosomal Acid Lipase Deficiency), mitochondrial disease (see Mitochondrial Disorders Overview and a recent review by Chow et al [2017]), and Smith-Lemli-Opitz syndrome) Autoimmune syndromes (e.g., polyglandular endocrine disease caused by mutation of AIRE ; OMIM 240300) Extrinsic (e.g., mechanical, infective, or drug-related) causes Management Evaluations Following Initial Diagnosis To assess the extent of disease and needs in an individual diagnosed with NR0B1- related adrenal hypoplasia congenita, the following evaluations are recommended under the care of an experienced pediatric endocrinologist.
-
Large For Gestational Age
Wikipedia
Taller, heavier parents tend to have larger babies. [22] Genetic disorders of overgrowth (e.g. Beckwith–Wiedemann syndrome , Sotos syndrome , Perlman syndrome , Simpson-Golabi-Behmel syndrome [23] ) are often characterized by macrosomia. [24] [25] Other risk factors [ edit ] Gestational age: pregnancies that go beyond 40 weeks increase incidence of an LGA infant [21] Fetal sex: male infants tend to weigh more than female infants [5] Obesity prior to pregnancy and maternal weight gain above recommended guidelines during pregnancy [26] [27] [28] Multiparity: giving birth to previous LGA infants vs. non-LGA infants [5] Frozen embryo transfer as fertility treatment, as compared with fresh embryo transfer or no artificial assistance [29] [30] Diagnosis [ edit ] Diagnosing fetal macrosomia cannot be performed until after birth, as evaluating a baby's weight in the womb may be inaccurate. [21] While ultrasound has been the primary method for diagnosing LGA, this form of fetal weight assessment remains imprecise, as the fetus is a highly variable structure in regards to density and weight— no matter the gestational age. [21] Ultrasonography involves an algorithm that incorporates biometric measurements of the fetus, such as biparietal diameter (BPD), head circumference (HC), abdominal circumference (AC), and femur length (FL), to calculate the estimated fetal weight (EFW). [31] Variability of fetal weight estimations has been linked to differences due to sensitivity and specificity of ultrasound algorithms as well as to the individual performing the ultrasound examination. [32] In addition to sonography, fetal weight can also be assessed using clinical and maternal methods. ... OCLC 1001668564 . ^ Sajorda BJ, Gonzalez-Gandolfi CX, Hathaway ER, Kalish JM (1993–2020). "Simpson-Golabi-Behmel Syndrome Type 1" . GeneReviews [Internet] . ... PMID 20301398 . ^ "Beckwith-Wiedemann syndrome" . Genetics Home Reference . Retrieved 2020-07-30 . ^ Vora N, Bianchi DW (October 2009). "Genetic considerations in the prenatal diagnosis of overgrowth syndromes" . Prenatal Diagnosis . 29 (10): 923–9. doi : 10.1002/pd.2319 . ... External links [ edit ] Classification D ICD - 10 : P08 ICD - 9-CM : 766 MeSH : D005320 DiseasesDB : 21929 External resources MedlinePlus : 002251 eMedicine : med/3279 v t e Conditions originating in the perinatal period / fetal disease Maternal factors complicating pregnancy, labour or delivery placenta Placenta praevia Placental insufficiency Twin-to-twin transfusion syndrome chorion / amnion Chorioamnionitis umbilical cord Umbilical cord prolapse Nuchal cord Single umbilical artery presentation Breech birth Asynclitism Shoulder presentation Growth Small for gestational age / Large for gestational age Preterm birth / Postterm pregnancy Intrauterine growth restriction Birth trauma scalp Cephalohematoma Chignon Caput succedaneum Subgaleal hemorrhage Brachial plexus injury Erb's palsy Klumpke paralysis Affected systems Respiratory Intrauterine hypoxia Infant respiratory distress syndrome Transient tachypnea of the newborn Meconium aspiration syndrome Pleural disease Pneumothorax Pneumomediastinum Wilson–Mikity syndrome Bronchopulmonary dysplasia Cardiovascular Pneumopericardium Persistent fetal circulation Bleeding and hematologic disease Vitamin K deficiency bleeding HDN ABO Anti-Kell Rh c Rh D Rh E Hydrops fetalis Hyperbilirubinemia Kernicterus Neonatal jaundice Velamentous cord insertion Intraventricular hemorrhage Germinal matrix hemorrhage Anemia of prematurity Gastrointestinal Ileus Necrotizing enterocolitis Meconium peritonitis Integument and thermoregulation Erythema toxicum Sclerema neonatorum Nervous system Perinatal asphyxia Periventricular leukomalacia Musculoskeletal Gray baby syndrome muscle tone Congenital hypertonia Congenital hypotonia Infections Vertically transmitted infection Neonatal infection rubella herpes simplex mycoplasma hominis ureaplasma urealyticum Omphalitis Neonatal sepsis Group B streptococcal infection Neonatal conjunctivitis Other Miscarriage Perinatal mortality Stillbirth Infant mortality Neonatal withdrawal
-
Confabulation
Wikipedia
Presentation [ edit ] Associated neurological and psychological conditions [ edit ] Confabulations are often symptoms of various syndromes and psychopathologies in the adult population including: Korsakoff's syndrome , Alzheimer's disease , schizophrenia , and traumatic brain injury . ... D.; Guerrini, I; Marshall, E. J. (2009). "The Korsakoff Syndrome: Clinical Aspects, Psychology and Treatment" . ... Confabulation behavior and false memories in Korsakoff's syndrome: role of source memory and executive functioning. ... "Frontal amnesia and the dysexecutive syndrome". Brain and Cognition . 7 (2): 212–30. doi : 10.1016/0278-2626(88)90031-0 . ... "A Case of Probable Korsakoff's Syndrome: A Syndrome of Frontal Lobe and Diencephalic Structural Pathogenesis and a Comparison with Medial Temporal Lobe Dementias" .
- Tetra-Amelia Orphanet
-
1q21.1 Recurrent Microdeletion
Gene_reviews
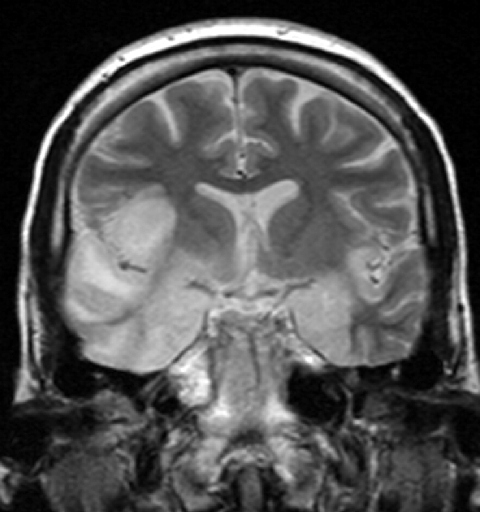
The 1q21.1 recurrent microdeletion itself does not appear to lead to a clinically recognizable syndrome as some persons with the deletion have no obvious clinical findings and others have variable findings that most commonly include microcephaly (50%), mild intellectual disability (30%), mildly dysmorphic facial features, and eye abnormalities (26%). ... However, there is not a clinically recognizable syndrome, as a subset of persons with the deletion do not have obvious clinical findings. ... Two individuals with the deletion had Mayer-Rokitansky-Kuster-Hauser syndrome [Chen et al 2015]. Skeletal malformations are variable and include craniosynostosis, scoliosis, joint laxity, brachydactyly with or without short distal phalanges, broad thumbs, clinodactyly of the fifth finger, clubfoot, small feet, pes planus , broad or duplicated/bifid great toes, overlapping or syndactyly of the toes, and polydactyly of the hands or feet. ... Differential Diagnosis The 22q11.2 microdeletion syndrome is the most common microdeletion syndrome and has several features that overlap with those seen in individuals with the 1q21.1 recurrent microdeletion: developmental delays, learning disabilities (though the predominant nonverbal learning disability seen in 22q11.2 microdeletions is not seen in the 1q21.1 recurrent microdeletion), intellectual disability, behavioral abnormalities, short stature, eye abnormalities, cardiac defects, and schizophrenia. However, persons with the recurrent 1q21.1 microdeletion do not have the typical facial characteristics seen in the 22q11.2 microdeletion syndrome. Management Evaluations Following Initial Diagnosis To establish the extent of disease and needs of an individual diagnosed with the 1q21.1 recurrent microdeletion, the following evaluations should be considered: Ophthalmologic examination if there are concerns about vision Cardiac evaluation if there are suggestive features clinically or on physical examination Brain imaging if microcephaly, macrocephaly, and/or neurologic findings are present Renal ultrasound examination Comprehensive developmental assessment for motor and language delays, which may include evaluations for autism spectrum disorders, intellectual disability, ADHD, and hearing loss Neurology consultation if significant hypotonia, seizures, tics, or tremors are present Psychiatric evaluation if evidence of mental illness is present Consultation with a medical geneticist and/or genetic counselor Treatment of Manifestations The following are indicated: Routine treatment of ophthalmologic, cardiac, and neurologic findings Speech, occupational, and physical therapies, as appropriate Specialized learning programs to meet individual needs No specific antiepileptic or antipsychotic medications are indicated.
-
Herpesviral Encephalitis
Wikipedia
Classification D ICD - 10 : B00.4 ICD - 9-CM : 054.3 External resources eMedicine : article/1165183 article/341142 v t e Infectious diseases – viral systemic diseases Oncovirus DNA virus HBV Hepatocellular carcinoma HPV Cervical cancer Anal cancer Penile cancer Vulvar cancer Vaginal cancer Oropharyngeal cancer KSHV Kaposi's sarcoma EBV Nasopharyngeal carcinoma Burkitt's lymphoma Hodgkin lymphoma Follicular dendritic cell sarcoma Extranodal NK/T-cell lymphoma, nasal type MCPyV Merkel-cell carcinoma RNA virus HCV Hepatocellular carcinoma Splenic marginal zone lymphoma HTLV-I Adult T-cell leukemia/lymphoma Immune disorders HIV AIDS Central nervous system Encephalitis / meningitis DNA virus Human polyomavirus 2 Progressive multifocal leukoencephalopathy RNA virus MeV Subacute sclerosing panencephalitis LCV Lymphocytic choriomeningitis Arbovirus encephalitis Orthomyxoviridae (probable) Encephalitis lethargica RV Rabies Chandipura vesiculovirus Herpesviral meningitis Ramsay Hunt syndrome type 2 Myelitis Poliovirus Poliomyelitis Post-polio syndrome HTLV-I Tropical spastic paraparesis Eye Cytomegalovirus Cytomegalovirus retinitis HSV Herpes of the eye Cardiovascular CBV Pericarditis Myocarditis Respiratory system / acute viral nasopharyngitis / viral pneumonia DNA virus Epstein–Barr virus EBV infection / Infectious mononucleosis Cytomegalovirus RNA virus IV : Human coronavirus 229E / NL63 / HKU1 / OC43 Common cold MERS coronavirus Middle East respiratory syndrome SARS coronavirus Severe acute respiratory syndrome SARS coronavirus 2 Coronavirus disease 2019 V , Orthomyxoviridae : Influenza virus A / B / C / D Influenza / Avian influenza V, Paramyxoviridae : Human parainfluenza viruses Parainfluenza Human orthopneumovirus hMPV Human digestive system Pharynx / Esophagus MuV Mumps Cytomegalovirus Cytomegalovirus esophagitis Gastroenteritis / diarrhea DNA virus Adenovirus Adenovirus infection RNA virus Rotavirus Norovirus Astrovirus Coronavirus Hepatitis DNA virus HBV ( B ) RNA virus CBV HAV ( A ) HCV ( C ) HDV ( D ) HEV ( E ) HGV ( G ) Pancreatitis CBV Urogenital BK virus MuV Mumps v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis
-
Myopathy, Congenital, With Fiber-Type Disproportion
Omim
Exclusion criteria consisted of insufficient clinical information; a coexisting disorder of muscle or the nervous system; 2 or more syndromal features present; histologic features of a muscular dystrophy; and a coefficient of variation greater than 250 for type 2 fibers. ... Gerdes et al. (1994) suggested that congenital fiber-type disproportion in this family was dominantly inherited with variable expressivity, and that the translocation breakpoints may represent candidate gene regions. The chromosome 1p36 deletion syndrome (607872) is characterized by hypotonia, moderate to severe developmental and growth retardation, and characteristic craniofacial dysmorphism (Shapira et al., 1997; Slavotinek et al., 1999). Muscle hypotonia and delayed motor development are almost constant features of the syndrome. Colmenares et al. (2002) suggested that the SKI protooncogene (164780) may contribute to phenotypes common in 1p36 deletion syndrome, particularly to facial clefting; Ski -/- mice showed features reminiscent of the syndrome. Okamoto et al. (2002) described a patient with the 1p36 deletion syndrome in whom FISH demonstrated that the SKI gene was deleted.
-
Denture-Related Stomatitis
Wikipedia
External links [ edit ] Classification D ICD - 10 : K12.1 MeSH : D013282 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Epulis Fissuratum
Wikipedia
External links [ edit ] Classification D DiseasesDB : 32595 External resources eMedicine : article/1077440 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Gingival Cyst
Wikipedia
External links [ edit ] Classification D ICD - 10 : K09.0 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Colorado Tick Fever
Wikipedia
Aspirin is not recommended for children, as it has been linked to Reye’s syndrome in some viral illnesses. Salicylates should not be used because of thrombocytopenia , and the rare occurrence of bleeding disorders. ... External links [ edit ] Classification D ICD - 10 : A93.2 ICD - 9-CM : 066.1 MeSH : D003121 DiseasesDB : 31134 External resources MedlinePlus : 000675 eMedicine : emerg/586 Orphanet : 83595 v t e Tick-borne diseases and infestations Diseases Bacterial infections Rickettsiales Anaplasmosis Boutonneuse fever Ehrlichiosis ( Human granulocytic , Human monocytotropic , Human E. ewingii infection ) Scrub typhus Spotted fever rickettsiosis Pacific Coast tick fever American tick bite fever rickettsialpox Rocky Mountain spotted fever ) Spirochaete Baggio–Yoshinari syndrome Lyme disease Relapsing fever borreliosis Thiotrichales Tularemia Viral infections Bhanja virus Bourbon virus Colorado tick fever Crimean–Congo hemorrhagic fever Heartland bandavirus Kemerovo tickborne viral fever Kyasanur Forest disease Omsk hemorrhagic fever Powassan encephalitis Severe fever with thrombocytopenia syndrome Tete orthobunyavirus Tick-borne encephalitis Protozoan infections Babesiosis Other diseases Tick paralysis Alpha-gal allergy Southern tick-associated rash illness Infestations Tick infestation Species and bites Amblyomma Amblyomma americanum Amblyomma cajennense Amblyomma triguttatum Dermacentor Dermacentor andersoni Dermacentor variabilis Ixodes Ixodes cornuatus Ixodes holocyclus Ixodes pacificus Ixodes ricinus Ixodes scapularis Ornithodoros Ornithodoros gurneyi Ornithodoros hermsi Ornithodoros moubata Other Rhipicephalus sanguineus v t e Zoonotic viral diseases (A80–B34, 042–079 ) Arthropod -borne Mosquito -borne Bunyavirales Arbovirus encephalitides : La Crosse encephalitis LACV Batai virus BATV Bwamba Fever BWAV California encephalitis CEV Jamestown Canyon encephalitis Tete virus Tahyna virus TAHV Viral hemorrhagic fevers : Rift Valley fever RVFV Bunyamwera fever BUNV Ngari virus NRIV Flaviviridae Arbovirus encephalitides : Japanese encephalitis JEV Australian encephalitis MVEV KUNV Saint Louis encephalitis SLEV Usutu virus West Nile fever WNV Viral hemorrhagic fevers : Dengue fever DENV-1-4 Yellow fever YFV Zika fever Zika virus Togaviridae Arbovirus encephalitides : Eastern equine encephalomyelitis EEEV Western equine encephalomyelitis WEEV Venezuelan equine encephalomyelitis VEEV Chikungunya CHIKV O'nyong'nyong fever ONNV Pogosta disease Sindbis virus Ross River fever RRV Semliki Forest virus Reoviridae Banna virus encephalitis Tick -borne Bunyavirales Viral hemorrhagic fevers : Bhanja virus Crimean–Congo hemorrhagic fever (CCHFV) Heartland virus Severe fever with thrombocytopenia syndrome ( Huaiyangshan banyangvirus ) Tete virus Flaviviridae Arbovirus encephalitides : Tick-borne encephalitis TBEV Powassan encephalitis POWV Viral hemorrhagic fevers : Omsk hemorrhagic fever OHFV Kyasanur Forest disease KFDV AHFV Langat virus LGTV Orthomyxoviridae Bourbon virus Reoviridae Colorado tick fever CTFV Kemerovo tickborne viral fever Sandfly -borne Bunyavirales Adria virus (ADRV) Oropouche fever Oropouche virus Pappataci fever Toscana virus Sandfly fever Naples virus Rhabdoviridae Chandipura virus Mammal -borne Rodent -borne Arenaviridae Viral hemorrhagic fevers : Lassa fever LASV Venezuelan hemorrhagic fever GTOV Argentine hemorrhagic fever JUNV Brazilian hemorrhagic fever SABV Bolivian hemorrhagic fever MACV LUJV CHPV Bunyavirales Hemorrhagic fever with renal syndrome DOBV HTNV PUUV SEOV AMRV THAIV Hantavirus pulmonary syndrome ANDV SNV Herpesviridae Murid gammaherpesvirus 4 Bat -borne Filoviridae BDBV SUDV TAFV Marburg virus disease MARV RAVV Rhabdoviridae Rabies ABLV MOKV DUVV LBV CHPV Paramyxoviridae Henipavirus encephalitis HeV NiV Coronaviridae SARS-related coronavirus SARS-CoV MERS-CoV SARS-CoV-2 Primate -borne Herpesviridae Macacine alphaherpesvirus 1 Retroviridae Simian foamy virus HTLV-1 HTLV-2 Poxviridae Tanapox Yaba monkey tumor virus Multiple vectors Rhabdoviridae Rabies RABV Mokola virus Poxviridae Monkeypox
-
Cherry Angioma
Wikipedia
"Glomeruloid hemangioma in POEMS syndrome shows two different immunophenotypic endothelial cells". ... Anais Brasileiros de Dermatologia . 79 : 83–89. doi : 10.1590/S0365-05962004000100010 . v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension
-
Camptocormia
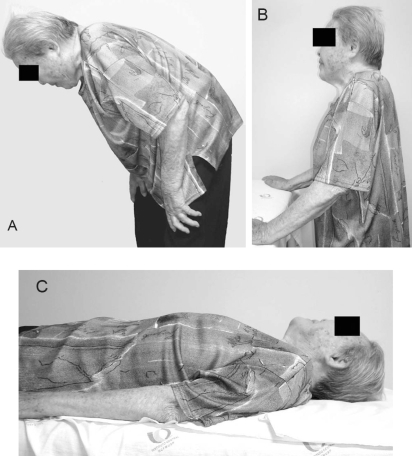
Wikipedia
It can be abated when lying down. [1] Camptocormia , also known as bent spine syndrome (BSS), is a symptom of a multitude of diseases that is most commonly seen in the elderly. ... This classification differentiates it from a similar syndrome known as kyphosis . [2] Although camptocormia is a symptom of many diseases, there are two common origins: neurological and muscular. ... The current medically preferred term for the condition is bent spine syndrome , because of the psychological origin associated with camptocormia . [2] Camptocormia in the elderly [ edit ] BSS is not limited to the elderly but has an average age of onset of 66 years [2] and is more common amongst men. ... Muscle biopsies found to have variable muscle fiber sizes and even endomysial fibrosis may be markers of bent spine syndrome. In addition, disorganized internal architecture and little necrosis or regeneration is a marker of camptocormia. ... PMID 18568258 . ^ a b c d e f g h i j k l m n o Lenoir, Thibaut; Guedj, Nathalie; Boulu, Philippe; Guigui, Pierre; Benoist, Michel (2010-03-19). "Camptocormia: the bent spine syndrome, an update" . European Spine Journal . 19 (8): 1229–1237. doi : 10.1007/s00586-010-1370-5 .
-
Methylmalonyl-Coa Mutase Deficiency
Wikipedia
Liver and kidney transplants, and a low-protein diet all help regulate the effects of the diseases. [13] Prognosis [ edit ] Infant mortality is high for patients diagnosed with early onset; mortality can occur within less than 2 months, while children diagnosed with late-onset syndrome seem to have higher rates of survival. [14] Patients suffering from a complete lesion of mut0 have not only the poorest outcome of those suffering from methylaonyl-CoA mutase deficiency, but also of all individuals suffering from any form of methylmalonic acidemia. ... External links [ edit ] Classification D OMIM : 251000 DiseasesDB : 29509 Methylmalonyl-CoA mutase deficiency at NLM Genetics Home Reference Overview of all the structural information available in the PDB for UniProt : P22033 (Methylmalonyl-CoA mutase, mitochondrial) at the PDBe-KB . v t e Inborn error of amino acid metabolism K → acetyl-CoA Lysine /straight chain Glutaric acidemia type 1 type 2 Hyperlysinemia Pipecolic acidemia Saccharopinuria Leucine 3-hydroxy-3-methylglutaryl-CoA lyase deficiency 3-Methylcrotonyl-CoA carboxylase deficiency 3-Methylglutaconic aciduria 1 Isovaleric acidemia Maple syrup urine disease Tryptophan Hypertryptophanemia G G→ pyruvate → citrate Glycine D-Glyceric acidemia Glutathione synthetase deficiency Sarcosinemia Glycine → Creatine : GAMT deficiency Glycine encephalopathy G→ glutamate → α-ketoglutarate Histidine Carnosinemia Histidinemia Urocanic aciduria Proline Hyperprolinemia Prolidase deficiency Glutamate / glutamine SSADHD G→ propionyl-CoA → succinyl-CoA Valine Hypervalinemia Isobutyryl-CoA dehydrogenase deficiency Maple syrup urine disease Isoleucine 2-Methylbutyryl-CoA dehydrogenase deficiency Beta-ketothiolase deficiency Maple syrup urine disease Methionine Cystathioninuria Homocystinuria Hypermethioninemia General BC / OA Methylmalonic acidemia Methylmalonyl-CoA mutase deficiency Propionic acidemia G→ fumarate Phenylalanine / tyrosine Phenylketonuria 6-Pyruvoyltetrahydropterin synthase deficiency Tetrahydrobiopterin deficiency Tyrosinemia Alkaptonuria / Ochronosis Tyrosinemia type I Tyrosinemia type II Tyrosinemia type III / Hawkinsinuria Tyrosine → Melanin Albinism : Ocular albinism ( 1 ) Oculocutaneous albinism ( Hermansky–Pudlak syndrome ) Waardenburg syndrome Tyrosine → Norepinephrine Dopamine beta hydroxylase deficiency reverse: Brunner syndrome G→ oxaloacetate Urea cycle / Hyperammonemia ( arginine aspartate ) Argininemia Argininosuccinic aciduria Carbamoyl phosphate synthetase I deficiency Citrullinemia N-Acetylglutamate synthase deficiency Ornithine transcarbamylase deficiency / translocase deficiency Transport / IE of RTT Solute carrier family : Cystinuria Hartnup disease Iminoglycinuria Lysinuric protein intolerance Fanconi syndrome : Oculocerebrorenal syndrome Cystinosis Other 2-Hydroxyglutaric aciduria Aminoacylase 1 deficiency Ethylmalonic encephalopathy Fumarase deficiency Trimethylaminuria
-
Mucolipidosis Iii Gamma
Gene_reviews
Limited hip mobility and lower-limb pain can be significant and may result in waddling gait with age. Carpal tunnel syndrome develops in most affected individuals and may be clinically significant in the second and third decade [Raas-Rothschild et al 2004, Tüysüz et al 2018, Nampoothiri et al 2019]. ... Short neck reported in several individuals had no clinical significance [Tüysüz et al 2018]. Chronic pain syndrome significantly impairs the quality of life. It is common and mainly involves the hips, knees, and entire legs and sometimes the hands. Chronic pain syndrome is attributed to skeletal and connective tissue disease. ... Most individuals with ML IIIγ known to the authors originated from the Mediterranean region [Raas-Rothschild et al 2004, Encarnação et al 2009, Persichetti et al 2009]. 3. Also referred to as Morquio syndrome type B 4. Also referred to as Sly disease type B 5. Also referred to as Hunter syndrome 6. Also referred to as Hurler-Scheie syndrome or Scheie syndrome Other disorders to consider Rheumatologic disorders are often suspected in individuals with ML IIIγ because of slowly decreasing range of motion in large and small joints and increasing pain in the hips [Brik et al 1993].
-
Streptococcal Pharyngitis
Wikipedia
However, in children a throat culture is recommended to confirm the result. [8] Asymptomatic individuals should not be routinely tested with a throat culture or RADT because a certain percentage of the population persistently "carries" the streptococcal bacteria in their throat without any harmful results. [20] Differential diagnosis See also: Acute pharyngitis As the symptoms of streptococcal pharyngitis overlap with other conditions, it can be difficult to make the diagnosis clinically. [10] Coughing, nasal discharge, diarrhea , and red, irritated eyes in addition to fever and sore throat are more indicative of a viral sore throat than of strep throat. [10] The presence of marked lymph node enlargement along with sore throat, fever, and tonsillar enlargement may also occur in infectious mononucleosis . [21] Other conditions that may present similarly include epiglottitis , Kawasaki disease , acute retroviral syndrome , Lemierre's syndrome , Ludwig's angina , peritonsillar abscess , and retropharyngeal abscess . [5] Prevention Tonsillectomy may be a reasonable preventive measure in those with frequent throat infections (more than three a year). [22] However, the benefits are small and episodes typically lessen in time regardless of measures taken. [23] [24] [25] Recurrent episodes of pharyngitis which test positive for GAS may also represent a person who is a chronic carrier of GAS who is getting recurrent viral infections. [8] Treating people who have been exposed but who are without symptoms is not recommended. [8] Treating people who are carriers of GAS is not recommended as the risk of spread and complications is low. [8] Treatment Untreated streptococcal pharyngitis usually resolves within a few days. [10] Treatment with antibiotics shortens the duration of the acute illness by about 16 hours. [10] The primary reason for treatment with antibiotics is to reduce the risk of complications such as rheumatic fever and retropharyngeal abscesses . [10] Antibiotics prevent acute rheumatic fever if given within 9 days of the onset of symptoms. [13] Pain medication Pain medication such as NSAIDs and paracetamol (acetaminophen) helps in the management of pain associated with strep throat. [26] Viscous lidocaine may also be useful. [27] While steroids may help with the pain, [13] [28] they are not routinely recommended. [8] Aspirin may be used in adults but is not recommended in children due to the risk of Reye syndrome . [13] Antibiotics The antibiotic of choice in the United States for streptococcal pharyngitis is penicillin V , due to safety, cost, and effectiveness. [10] Amoxicillin is preferred in Europe. [29] In India, where the risk of rheumatic fever is higher, intramuscular benzathine penicillin G is the first choice for treatment. [13] Appropriate antibiotics decrease the average 3–5 day duration of symptoms by about one day, and also reduce contagiousness. [20] They are primarily prescribed to reduce rare complications such as rheumatic fever and peritonsillar abscess . [30] The arguments in favor of antibiotic treatment should be balanced by the consideration of possible side effects, [12] and it is reasonable to suggest that no antimicrobial treatment be given to healthy adults who have adverse reactions to medication or those at low risk of complications. [30] [31] Antibiotics are prescribed for strep throat at a higher rate than would be expected from how common it is. [32] Erythromycin and other macrolides or clindamycin are recommended for people with severe penicillin allergies . [10] [8] First-generation cephalosporins may be used in those with less severe allergies [10] and some evidence supports cephalosporins as superior to penicillin. [33] [34] These late-generation antibiotics show a similar effect when prescribed for 3–7 days in comparison to the standard 10-days of penicillin when used in areas of low rheumatic heart disease. [35] Streptococcal infections may also lead to acute glomerulonephritis ; however, the incidence of this side effect is not reduced by the use of antibiotics. [13] Prognosis The symptoms of strep throat usually improve within three to five days, irrespective of treatment. [20] Treatment with antibiotics reduces the risk of complications and transmission; children may return to school 24 hours after antibiotics are administered. [10] The risk of complications in adults is low. [8] In children, acute rheumatic fever is rare in most of the developed world. It is, however, the leading cause of acquired heart disease in India, sub-Saharan Africa, and some parts of Australia. [8] Complications arising from streptococcal throat infections include: Acute rheumatic fever [11] Scarlet fever [36] Streptococcal toxic shock syndrome [36] [37] Glomerulonephritis [38] PANDAS syndrome [39] [40] [41] Peritonsillar abscess [8] Cervical lymphadenitis [8] Mastoiditis [8] The economic cost of the disease in the United States in children is approximately $350 million annually. [8] Epidemiology Pharyngitis , the broader category into which Streptococcal pharyngitis falls, is diagnosed in 11 million people annually in the United States. [10] It is the cause of 15–40% of sore throats among children [7] [10] and 5–15% in adults. [8] Cases usually occur in late winter and early spring. [10] References ^ a b c d e f g h i j k l m n o p "Is It Strep Throat?" ... "Severe group A streptococcal infections associated with a toxic shock-like syndrome and scarlet fever toxin A". N. ... "CANS: Childhood acute neuropsychiatric syndromes". Eur J Paediatr Neurol (Review). 22 (2): 316–320. doi : 10.1016/j.ejpn.2018.01.011 . ... Classification D ICD - 10 : J02.0 ICD - 9-CM : 034.0 DiseasesDB : 12507 External resources MedlinePlus : 000639 eMedicine : med/1811 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis
-
Clonal Hypereosinophilia
Wikipedia
Historically, patients suffering the cited eosinophil-related syndromes were evaluated for causes of their eosinophilia such as those due to allergic disease, parasite or fungal infection, autoimmune disorders, and various well-known hematological malignancies (e.g. ... Discovery of genetic mutations underlining these eosinophilia syndromes lead to their removal from CEL-NOS or HES categories and classification as myeloid and lymphoid neoplasms associated with eosinophilia and abnormalities of PDGFRA, PDGFRB, FGFR1, and, tentatively, PCMA-JAK2 . ... These neoplasmas are sometimes termed, along with certain other Myelodysplastic syndromes associated with eosinophilia as myeloid neoplasms with eosinophilia, clonal eosinophilia, or primary eosinophilia. ... "Contemporary consensus proposal on criteria and classification of eosinophilic disorders and related syndromes" . The Journal of Allergy and Clinical Immunology . 130 (3): 607–612.e9. doi : 10.1016/j.jaci.2012.02.019 . ... "IgG4-related disease and lymphocyte-variant hypereosinophilic syndrome: A comparative case series" . European Journal of Haematology . 98 (4): 378–387. doi : 10.1111/ejh.12842 .
-
Celiac Disease
Gene_reviews
., peripheral neuropathy, ataxia, seizures, migraines, attention-deficit disorder, poor school performance) Osteoporosis/osteopenia Infertility and/or recurrent fetal loss Short stature and/or failure to thrive Delayed puberty Dental enamel defects Autoimmune disorders Individuals with disorders associated with celiac disease (e.g., Down syndrome, Turner syndrome, Williams syndrome, selective IgA deficiency, insulin-dependent diabetes mellitus, Sjögren syndrome, thyroiditis) Absence of history of self-limited enteritis and/or tropical sprue Laboratory findings Iron deficiency anemia Vitamin and/or mineral deficiencies (e.g., calcium, vitamin D, vitamin B 12 , folic acid) In individuals on a gluten-containing diet: Elevated serum tissue transglutaminase (tTG) IgA Elevated serum anti-deamidated gliadin-related peptide (a-DGP) IgA and IgG Elevated serum endomysial antibody (EMA) IgA ; highest specificity (~99%) but sensitivity subject to observer variability Note on measurement of serum total IgA to evaluate for IgA deficiency : Selective IgA deficiency is more prevalent in individuals with celiac disease (1:50). ... Other extraintestinal presentations include osteoporosis/osteopenia, dental enamel hypoplasia, infertility and/or recurrent fetal loss, vitamin deficiencies, abnormal liver function tests (typically elevated transaminases), fatigue, psychiatric syndromes, and various neurologic conditions including peripheral neuropathy, ataxia, seizures, migraines, attention-deficit hyperactivity disorder, and poor school performance. ... The prevalence of celiac disease is increased in individuals with the following disorders [NIH Consensus Committee 2005]: Down syndrome (prevalence of celiac disease: 5%-12%) Turner syndrome (~3%) Williams syndrome (3%-10%) Selective IgA deficiency (~2%-10%) Insulin-dependent diabetes mellitus (~6%) Sjögren syndrome (~5%) Autoimmune thyroid disease (~2%-4%) Differential Diagnosis The clinical manifestations of celiac disease overlap with several other conditions, including: Helicobacter pylori gastritis Irritable bowel syndrome Inflammatory bowel disease Tropical sprue Various neurologic syndromes, including myasthesia gravis and peripheral neuropathy Drug-induced small-bowel disease (e.g., nonsteroidal anti-inflammatory drugs, olmesartan) Small-bowel bacterial overgrowth Other (non-Celiac) Causes of Gluten Sensitivity Allergic (wheat allergy).MYO9B, HLA-DQB1, HLA-DQA1, BACH2, THEMIS, IL15, ZMIZ1, IFNG, CTLA4, HLA-DPB1, TGM2, ICOSLG, IL21, ETS1, MMP3, CXCL10, FCGR3A, MAGI2, UBD, CXCL11, MMP12, CD80, TFF1, APOB, TNFRSF9, ASAH2, CD36, CXCL9, LRAT, LPL, LCN2, CAPN8, TNFRSF14, CCR4, UGT1A4, IFI27, UPB1, SLC6A14, ACE, PIWIL2, VNN1, SOAT2, PCK1, RUNX3, GBP5, APOC3, S100A9, IL2, CD28, IL12A, SH2B3, ICOS, TAGAP, LPP, HLA-DQA2, IL23R, KIAA1109, CCR3, IL2RA, CIITA, ATG16L1, IL18R1, SMAD3, FUT2, PPP1R12B, FRMD4B, CD247, PUS10, MMEL1, ZNF335, PLEK, YDJC, NFIA, NCF2, POU2AF1, NKAIN2, IRF1-AS1, MST1, HECTD4, LURAP1L, SLC9A4, LINC02649, C1orf141, LINC01185, PTEN, CRB1, MROH3P, PTPRK, LINC01934, LINC00993, IL12A-AS1, IL6, IL10, LINC00824, IL12RB1, LINC01250, IL17A, INS-IGF2, MICA, IRF4, IRF5, AFF3, NONOP2, UQCRC2P1, C6orf99, ADCY7, ATXN2, RBM45, TNPO3, ELMO1, MYNN, SMG7, TNFSF15, INAVA, DLEU1, UBASH3A, SRCAP, IGF2-AS, ATXN2L, FNBP1, FOXP3, CNTNAP2, PHLDB1, ADGRL2, NRXN1, ARHGAP31, ERAP2, RMI2, LRRK2, SPIB, STAT3, STAT4, SUOX, TCF4, TNF, CARD9, WNT3, ANKRD30A, GATD3A, TMEM187, NKD1, ANKRD55, ACACA, PTPN2, DAG1, ABCC6, RUNX1, ZFP36L1, HLA-DRB1, GPR35, ACAD8, HP, PTPN22, IL18, LINC01193, IL18RAP, CFTR, PREP, CELIAC2, CXCL8, TLR4, AGA, HLA-A, IL1B, HT, HFE, IL4, IL22, NXF1, USO1, TLR2, TOR1A, FLNB, SEC14L2, FCGR2A, KIR3DL1, CD14, NOS2, INS, IL1A, TRBV20OR9-2, NLRP3, STAT1, HLA-C, ICAM1, MMP1, TGM6, IBD5, MBL2, PON1, VDR, GOT2, CXCR3, TPO, DMD, HSPA1A, EGFR, KLRK1, TAP2, DEFB1, GEM, KLRC4-KLRK1, NTS, CCR9, SLC11A2, HSPA1B, BEST1, TGFB1, IRF1, HMGB1, HLA-G, MYD88, ISYNA1, HLA-DRB4, NFKB1, RGS1, CRP, CCK, SCHIP1, TNFRSF8, VEGFA, TSLP, CD19, TXN, TNFAIP3, REG1A, CD38, TJP1, CD59, CX3CL1, SDC1, PARD3, TG, TFRC, TLR9, CDR3, HIF1A, CNR2, DLG5, HLA-DRB3, FAS, ISG20, PAEP, ATP12A, CTNNB1, ATP4A, HLA-DPA1, IL15RA, KLRC2, MLH1, MIF, DEFA5, IFNA13, IFNA1, IL12B, MTHFR, IL5, CLDN2, GHRL, TOLLIP, NELFCD, IL23A, ISCU, TBC1D9, COX8A, GINS2, ACSL5, CLDN3, CTSB, CX3CR1, CLEC16A, CCN2, TRDC, CADM1, B3GAT1, TRDD3, TRAV26-1, TRDJ1, DLL1, CD209, PGPEP1, IGHV5-51, HPGDS, SPINK4, LAMP3, CLDN15, GBGT1, CSN2, IBD6, ULK3, CR2, CPOX, TBC1D7, CHMP2B, QPCT, TLR7, IGF1, ODR4, BCL2, ATD, BAK1, BAX, GSTK1, IRGM, BCKDHB, STPG4, OR10A4, TICAM1, NAPEPLD, SLC30A8, OLIG3, TMPRSS6, CST13P, NKX2-3, BDNF, MIR155, DEFB103A, HCG14, KIR2DL5B, PARP1, ADRA1A, AHR, ALB, ALK, OCLN, LINC01672, AMELX, AD12, AMH, ANPEP, ZGLP1, CCR2, ANXA11, APC, CFB, TRIM69, CCR5, KIR2DL5A, CD34, IFIH1, CD44, CD48, C6orf47, ZFAT, CDKN2A, CDKN2D, SLCO6A1, PNPLA2, DEFB103B, CHI3L1, CLC, IFT122, SLC30A10, CCR1, FTO, VTCN1, CD86, EHMT1, ADAD1, IL17RE, CD1D, CD3E, CD3G, CD4, MTG1, CD8A, IL33, ATAD1, NCALD, PNPLA3, TRABD, NLRP1, BTNL8, CCDC33, FCGRT, DMRT1, NHS, SERPINF1, PDGFB, GRINA, PBX3, TNFRSF11B, NT5E, NOS1, NFKBIB, DUSP10, GTF2A1, NDUFA2, GZMB, NCAM1, MUC1, MSH5, MSH2, ABCB1, SERPINA1, PI3, SERPINE2, GNAO1, PTH, PSMB6, PRL, PRKCQ, PRKCD, PPP6C, PON3, PON2, PML, PLA2G4A, PIK3CG, PIK3CD, PIK3CB, PIK3CA, HLA-B, MME, MLN, KIR3DL2, KCNJ11, IRF2, IRAK1, INSR, HNRNPD, IL13, IL12RB2, HSPA2, HSPD1, IL9, IL6R, IDDM3, IL5RA, IL2RB, IGHA1, KIR2DS1, L1CAM, HLA-DMB, LCT, MICB, HLA-DOA, MGMT, MEFV, MCL1, SMAD7, SMAD2, LYZ, LTBR, LTA, LSAMP, HLA-DQB2, LMO2, LMO1, LGALS1, PTPRC, GLS, RAC2, NCR1, COX5A, F2, HSPB3, F9, FAAH, TNFSF13, MADD, IGFALS, MTOR, SCG2, ZFP36, YY1, FUT4, VIP, UBE2L3, ETFA, ERBB2, TPMT, ELN, LILRA3, BTNL3, DNAH8, TNFSF13B, GNA13, CD226, DPP4, KAT5, CLEC10A, SEMA3A, PRSS16, OPTN, ABCB6, EGF, ELAVL2, TSHR, TNFRSF1A, RAG1, GH1, GLB1, SOX9, SOD1, SLC22A4, SLC6A4, SGK1, SELL, SELE, GLI1, CCL5, CCL2, GLI2, S100B, GLP1R, SNORA73A, SPINK1, STAT6, GABBR1, GCG, CLDN5, TLR3, TIMP1, TIA1, GAD1, TGM1, TGFB3, TGFA, TFF3, GAD2, TRD, TCN2, GATA3, TBX1, TAP1, H3P13
-
Slc35a1-Cdg
Orphanet
SLC35A1-CDG is an extremely rare form of CDG syndrome (see this term) characterized clinically in the single reported case by repeated hemorrhagic incidents, including severe pulmonary hemorrhage.