-
Musculoskeletal Disorder
Wikipedia
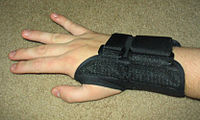
See also: Musculoskeletal injury Musculoskeletal disorders Carpal tunnel syndrome is a common musculoskeletal disorder, and is often treated with a splint . Specialty Rheumatology Musculoskeletal disorders (MSDs) are injuries or pain in the human musculoskeletal system , including the joints , ligaments , muscles , nerves , tendons , and structures that support limbs, neck and back. [1] MSDs can arise from a sudden exertion (e.g., lifting a heavy object), [2] or they can arise from making the same motions repeatedly repetitive strain, or from repeated exposure to force, vibration, or awkward posture. [3] Injuries and pain in the musculoskeletal system caused by acute traumatic events like a car accident or fall are not considered musculoskeletal disorders. [4] MSDs can affect many different parts of the body including upper and lower back, neck, shoulders and extremities (arms, legs, feet, and hands). [5] Examples of MSDs include carpal tunnel syndrome , epicondylitis , tendinitis , back pain , tension neck syndrome, and hand-arm vibration syndrome. [3] Contents 1 Causes 1.1 Biomechanical 1.2 Individual differences 1.3 Psychosocial 1.4 Occupational 2 Diagnosis 3 Prevention 3.1 Workplace controls 3.2 Ergonomics 4 Epidemiology 4.1 General population 4.2 Workplace 5 See also 6 References 7 External links Causes [ edit ] MSDs can arise from the interaction of physical factors with ergonomic, psychological, social, and occupational factors. [6] Biomechanical [ edit ] MSDs are caused by biomechanical load which is the force that must be applied to do tasks, the duration of the force applied, and the frequency with which tasks are performed. [7] Activities involving heavy loads can result in acute injury, but most occupation-related MSDs are from motions that are repetitive, or from maintaining a static position. [8] Even activities that do not require a lot of force can result in muscle damage if the activity is repeated often enough at short intervals. [8] MSD risk factors involve doing tasks with heavy force, repetition, or maintaining a nonneutral posture. [8] Of particular concern is the combination of heavy load with repetition. [8] Although poor posture is often blamed for lower back pain, a systematic review of the literature failed to find a consistent connection. [9] Individual differences [ edit ] People vary in their tendency to get MSDs. ... Postures which are less natural, such as twisting of or tension in the upper body, are typically contributors to the development of MSDs due to the unnatural biomechanical load of these postures. [3] [16] There is evidence that posture contributes to MSDs of the neck, shoulder, and back. [3] Repeated motion is another risk factor for MSDs of occupational origin because workers can perform the same movements repeatedly over long periods of time (e.g. typing leading to carpal tunnel syndrome , lifting heavy objects leading to herniated discs/slipped discs), which can wear on the joints and muscles involved in the motion in question. [3] [17] Workers doing repetitive motions at a high pace of work with little recovery time and workers with little to no control over the timing of motions (e.g. workers on assembly lines ) are also prone to MSDs due to the motion of their work. [16] Force needed to perform actions on the job can also be associated with higher MSD risk in workers, because movements which require more force can fatigue muscles quicker which can lead to injury and/or pain. [3] Additionally, exposure to vibration (experienced by truck drivers or construction workers , for example) and extreme hot or cold temperatures can affect a worker's ability to judge force and strength, which can lead to development of MSDs. [16] Vibration exposure is also associated with hand-arm vibration syndrome, which has symptoms of lack of blood circulation to the fingers, nerve compression, tingling, and/or numbness. [18] Diagnosis [ edit ] Assessment of MSDs is based on self-reports of symptoms and pain as well as physical examination by a doctor. [3] Doctors rely on medical history, recreational and occupational hazards, intensity of pain, a physical exam to locate the source of the pain, and sometimes lab tests, X-rays , or an MRI [19] Doctors look for specific criteria to diagnose each different musculoskeletal disorder, based on location, type, and intensity of pain, as well as what kind of restricted or painful movement a patient is experiencing. [3] A popular measure of MSDs is the Nordic Questionnaire that has a picture of the body with various areas labeled and asks the individual to indicate in which areas they have experienced pain, and in which areas has the pain interfered with normal activity. [5] Prevention [ edit ] Prevention of MSDs relies upon identification of risk factors, either by self-report, observation on the job, or measurement of posture which could lead to MSDs. [20] Once risk factors have been determined, there are several intervention methods which could be used to prevent the development of MSDs. ... Silver Spring, MD. ^ https://www.ncbi.nlm.nih.gov/m/pubmed/24337029/ External links [ edit ] Classification D MeSH : D009140 SNOMED CT : 928000 Musculoskeletal disorders Single Entry Point European Agency for Safety and Health at Work (OSHA) Good Practices to prevent Musculoskeletal disorders European Agency for Safety and Health at Work (OSHA) Musculoskeletal disorders homepage Health and Safety Executive (HSE) Hazards and risks associated with manual handling of loads in the workplace European Agency for Safety and Health at Work (OSHA) National Institute for Occupational Safety and Health Musculoskeletal Health Program [1] v t e Diseases of joints General Arthritis Monoarthritis Oligoarthritis Polyarthritis Symptoms Joint pain Joint stiffness Inflammatory Infectious Septic arthritis Tuberculosis arthritis Crystal Chondrocalcinosis CPPD (Psudogout) Gout Seronegative Reactive arthritis Psoriatic arthritis Ankylosing spondylitis Other Juvenile idiopathic arthritis Rheumatoid arthritis Felty's syndrome Palindromic rheumatism Adult-onset Still's disease Noninflammatory Hemarthrosis Osteoarthritis Heberden's node Bouchard's nodes Osteophyte
-
Peripheral Nerve Injuries
Mayo_clinic
Causes Peripheral nerves can be damaged in several ways: Injury from an accident, a fall or sports, which can stretch, compress, crush or cut nerves Medical conditions, such as diabetes, Guillain-Barre syndrome and carpal tunnel syndrome Autoimmune diseases including lupus, rheumatoid arthritis and Sjogren's syndrome Other causes include narrowing of the arteries, hormonal imbalances and tumors.
-
Keratosis Follicularis Spinulosa Decalvans, X-Linked
Omim
A number sign (#) is used with this entry because of evidence that X-linked keratosis follicularis spinulosa decalvans (KFSDX) is caused by mutation in the MBTPS2 gene (300294). See also IFAP syndrome (308205), an allelic disorder with an overlapping phenotype. ... The findings suggested that KFSDX and IFAP syndrome are related along a similar disease spectrum. ... INHERITANCE - X-linked recessive HEAD & NECK Face - Facial erythema Eyes - Photophobia - Blepharitis - Conjunctivitis - Keratitis - Corneal dystrophy - Sparse eyelashes - Sparse eyebrows SKIN, NAILS, & HAIR Skin - Dry, bumpy skin - Keratosis pilaris - Folliculitis - Follicular hyperkeratotic papules - Folliculitis of the scalp, trunk, and extensor surfaces of the extremities - Palmoplantar keratoderma Skin Histology - Epidermal hyperplasia - Perifollicular inflammatory infiltrate - Perifollicular fibrosis Nails - Dystrophic nails Hair - Alopecia, beginning in the occiput - Scarring alopecia - Sparse eyelashes - Sparse eyebrows MISCELLANEOUS - Genetic heterogeneity - Onset in infancy or early childhood - Carrier females may have mild features - Allelic disorder to IFAP syndrome ( 308205 ) MOLECULAR BASIS - Caused by mutation in the membrane-bound transcription factor protease, site 2 gene (MBTPS2, 300294.0006 ) ▲ Close
-
Bone Marrow Failure
Wikipedia
Epidemiology [ edit ] For those with severe bone marrow failure, the cumulative incidence of resulting stem cell transplantation or death was greater than 70% by individuals 60 years of age. [6] The incidence of bone marrow failure is triphasic: one peak at two to five years during childhood (due to inherited causes), and two peaks in adulthood, between 20 to 25 years old and after 60 years old (from acquired causes). [7] One in ten individuals with bone marrow failure have unsuspected Fanconi anemia (FA). [7] FA is the most common inherited bone marrow failure with an incidence of one to five episodes per million individuals. [7] The carrier frequency for FA is 1 in 200 to 300, however this differs by ethnicity. [7] In Europe and North America, the incidence of acquired aplastic anemia is rare with two episodes per million people each year, yet in Asia rises with 3.9 to 7.4 episodes per million people each year. [8] While acquired aplastic anemia with an unknown cause is rare, it is commonly permanent and life threatening as half of those with this condition die within the first six months. [9] The prevalence of bone marrow failure is over three times higher in Japan and East Asia than in the United States and Europe. [9] When one's body fails to produce blood cell lines, the morbidity and mortality rate increases. [9] Myelodysplastic syndromes (MDS) is a form of blood cancer found within the bone marrow in which the body no longer produces enough healthy, normal blood cells. [10] MDS are a frequently unrecognized and rare group of bone marrow failure disorders, yet the incidence rate has rose from 143 reported cases in 1973 to approximately 15,000 cases in the United States each year. ... "Cancer in the National Cancer Institute Inherited Bone Marrow Failure Syndrome Cohort After Fifteen Years of Follow-Up". ... "What is MDS?" . Myelodysplastic Syndromes Foundation, Inc . ^ Kitchen, Rose.
-
Glomerulopathy With Fibronectin Deposits 1
Omim
Other features included hypertension and nephrotic syndrome in 2 patients, and otosclerosis in 1. ... Related features included generalized distal renal tubular acidosis type IV, hypertension, and the nephrotic syndrome. Younger individuals in the later generations frequently had unexplained microalbuminuria, which may have indicated incipient glomerular disease. ... INHERITANCE - Autosomal dominant CARDIOVASCULAR Vascular - Hypertension due to renal disease GENITOURINARY Kidneys - Proteinuria - Microscopic hematuria - Nephrotic syndrome - Renal failure - End-stage renal disease - Renal tubular acidosis type IV - Enlarged glomeruli - Mesangial, transmembranous, subepithelial, and subendothelial fibrillar deposits which show immunoreactivity to fibronectin MISCELLANEOUS - Onset of proteinuria in the third to fourth decades - Onset of end-stage renal disease 15 to 20 years after onset - Slow progression ▲ Close
-
Anomalous Pulmonary Venous Connection
Wikipedia
In less severe cases, with smaller amounts of blood flow, diagnosis may be delayed until adulthood, when it can be confused with other causes of pulmonary hypertension. [4] There is also evidence that a significant number of mild cases are never diagnosed, or diagnosed incidentally. [5] It is associated with other vascular anomalies, and some genetic syndromes such as Turner syndrome . Diagnosis [ edit ] It can be diagnosed with CT scan , angiography , transesophageal echocardiography , or cardiac MRI . [6] [7] Unfortunately, less invasive and expensive testing, such as transthoracic echocardiography and CT scanning are generally less sensitive. ... External links [ edit ] Classification D ICD - 10 : Q26.2 - Q26.4 ICD - 9-CM : 747.41 - 747.42 External resources eMedicine : ped/2816 v t e Congenital vascular defects / Vascular malformation Great arteries / other arteries Aorta Patent ductus arteriosus Coarctation of the aorta Interrupted aortic arch Double aortic arch Right-sided aortic arch Overriding aorta Aneurysm of sinus of Valsalva Vascular ring Pulmonary artery Pulmonary atresia Stenosis of pulmonary artery Subclavian artery Aberrant subclavian artery Umbilical artery Single umbilical artery Great veins Superior / inferior vena cava Congenital stenosis of vena cava Persistent left superior vena cava Pulmonary vein Anomalous pulmonary venous connection ( Total , Partial ) Scimitar syndrome Arteriovenous malformation Cerebral arteriovenous malformation
-
Hypocholesterolemia
Wikipedia
It is found mostly in Jewish populations. [11] hypobetalipoproteinemia - a genetic disease that causes cholesterol readings below 50 mg/dl [11] manganese deficiency Smith–Lemli–Opitz syndrome Marfan syndrome leukemias and other hematological diseases [12] Diagnosis [ edit ] Classification [ edit ] According to the American Heart Association in 1994, only total cholesterol levels below 160 mg/dL or 4.1 mmol/l are to be classified as "hypocholesterolemia". [2] However, this is not agreed on universally and some put the level lower. ... External links [ edit ] Classification D ICD - 10 : E78.6 ICD - 9-CM : 272.5 v t e Inborn error of lipid metabolism : dyslipidemia Hyperlipidemia Hypercholesterolemia / Hypertriglyceridemia Lipoprotein lipase deficiency/Type Ia Familial apoprotein CII deficiency/Type Ib Familial hypercholesterolemia/Type IIa Combined hyperlipidemia/Type IIb Familial dysbetalipoproteinemia/Type III Familial hypertriglyceridemia/Type IV Xanthoma/Xanthomatosis Hypolipoproteinemia Hypoalphalipoproteinemia/HDL Lecithin cholesterol acyltransferase deficiency Tangier disease Hypobetalipoproteinemia/LDL Abetalipoproteinemia Apolipoprotein B deficiency Chylomicron retention disease Lipodystrophy Barraquer–Simons syndrome Other Lipomatosis Adiposis dolorosa Lipoid proteinosis APOA1 familial renal amyloidosisPCSK9, SAR1B, ABCA1, PEX12, FLCN, UBE3B, HSD3B7, CCT5, MSMO1, DHCR7, PMM2, APOB, CAV1, PIK3CD, PIK3CA, PIK3CG, LDLR, CD44, PIK3CB, MTTP, ACTB, IL6, CXCR4, HMGCR, CNBP, XBP1, AHSA1, GRAP2, XPR1, TM4SF5, TRPA1, AIMP2, CAV2, SACM1L, VEGFA, UCP3, UCP1, TNF, SREBF2, SREBF1, SOD1, SLC6A3, SLC2A4, TRPV1, TBC1D9, ANXA6, ROS1, ADAM10, ANTXR2, NLRP3, PRRT2, AGT, AGTR1, PRDM16, CFAP97, NGLY1, TRPV6, HDL3, RXFP3, AKT1, TAS2R14, NPC1L1, ANGPTL3, POLDIP2, RNF19A, BACE1, APOA4, RGS2, RHO, CASP1, KCNK3, ITIH4, CXCL10, CXCL8, HTR3A, HSD11B1, FDFT1, FASN, F3, ERN1, EGF, EFNB2, DSC2, CAT, CYBB, CYBA, MAPK14, CRK, CP, LCAT, MAP3K5, CDC42, MFAP1, PTK2, MAPK8, MAPK3, MAPK1, PRKCB, PRKCA, APP, APRT, AQP2, ACP3, AQP4, SERPINI1, ABCB1, BRAF, P2RX7, OSBP, NOS3, MVD, MUC5AC, MIR214
-
Annular Pancreas
Wikipedia
External links [ edit ] Classification D ICD - 10 : Q45.1 ICD - 9-CM : 751.7 OMIM : 167750 MeSH : C536376 C536376, C536376 External resources MedlinePlus : 001142 v t e Congenital malformations and deformations of digestive system Upper GI tract Tongue , mouth and pharynx Cleft lip and palate Van der Woude syndrome tongue Ankyloglossia Macroglossia Hypoglossia Esophagus EA/TEF Esophageal atresia: types A, B, C, and D Tracheoesophageal fistula: types B, C, D and E esophageal rings Esophageal web (upper) Schatzki ring (lower) Stomach Pyloric stenosis Hiatus hernia Lower GI tract Intestines Intestinal atresia Duodenal atresia Meckel's diverticulum Hirschsprung's disease Intestinal malrotation Dolichocolon Enteric duplication cyst Rectum / anal canal Imperforate anus Rectovestibular fistula Persistent cloaca Rectal atresia Accessory Pancreas Annular pancreas Accessory pancreas Johanson–Blizzard syndrome Pancreas divisum Bile duct Choledochal cysts Caroli disease Biliary atresia Liver Alagille syndrome Polycystic liver disease
-
Chronic Mountain Sickness
Wikipedia
External links [ edit ] Classification D ICD - 10 : T70.2 ICD - 9-CM : E902.0 DiseasesDB : 29615 ^ Online calculator illustrating blood oxygen carrying capacity at altitude v t e Consequences of external causes Temperature Elevated Hyperthermia Heat syncope Reduced Hypothermia Immersion foot syndromes Trench foot Tropical immersion foot Warm water immersion foot Chilblains Frostbite Aerosol burn Cold intolerance Acrocyanosis Erythrocyanosis crurum Radiation Radiation poisoning Radiation burn Chronic radiation keratosis Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy Radiation acne Radiation-induced cancer Radiation recall reaction Radiation-induced erythema multiforme Radiation-induced hypertrophic scar Radiation-induced keloid Radiation-induced morphea Air Hypoxia / Asphyxia Barotrauma Aerosinusitis Decompression sickness High altitude Altitude sickness Chronic mountain sickness Death zone HAPE HACE Food Starvation Maltreatment Physical abuse Sexual abuse Psychological abuse Travel Motion sickness Seasickness Airsickness Space adaptation syndrome Adverse effect Hypersensitivity Anaphylaxis Angioedema Allergy Arthus reaction Adverse drug reaction Other Electrical injury Drowning Lightning injuries Ungrouped skin conditions resulting from physical factors Dermatosis neglecta Pinch mark Pseudoverrucous papules and nodules Sclerosing lymphangitis Tropical anhidrotic asthenia UV-sensitive syndrome environmental skin conditions Electrical burn frictional/traumatic/sports Black heel and palm Equestrian perniosis Jogger's nipple Pulling boat hands Runner's rump Surfer's knots Tennis toe Vibration white finger Weathering nodule of ear Wrestler's ear Coral cut Painful fat herniation Uranium dermatosis iv use Skin pop scar Skin track Slap mark Pseudoacanthosis nigricans Narcotic dermopathy
-
Cat Skin Disorders
Wikipedia
Hereditary and developmental skin diseases [ edit ] Some diseases are inherent abnormalities of skin structure or function. These include skin fragility syndrome (Ehlers-Danlos), hereditary hypotrichosis and congenital or hereditary alopecia . ... In cats, this includes one of the most devastating cat skin disorders, feline acquired skin fragility syndrome. The pathogenesis of this rare syndrome is unknown.
-
Pruritic Urticarial Papules And Plaques Of Pregnancy
Wikipedia
. ^ Pruritic Urticarial Papules and Plaques of Pregnancy~treatment at eMedicine External links [ edit ] Classification D ICD - 10 : O99.7 ( ILDS O99.740) MeSH : C535817 DiseasesDB : 30030 External resources eMedicine : derm/351 v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy Category
-
Lupus Headache
Wikipedia
The 1999 American College of Rheumatology case definitions of neuropsychiatric syndromes in SLE do not define lupus headache, but rather propose several headache disorders loosely based on the International Headache Society (IHS) classification. ... Diagnosis [ edit ] Although specific complications of SLE may cause headache (such as cerebral venous sinus thrombosis or posterior reversible encephalopathy syndrome ), it remains unclear whether specific investigations (such as lumbar puncture or magnetic resonance imaging , MRI) are needed in lupus patients presenting with headache. ... PMID 12369649 . ^ Bernatsky S, Pineau CA, Lee JL, Clarke AE (2006). "Headache, Raynaud's syndrome and serotonin receptor agonists in systemic lupus erythematosus" .
-
Feline Hepatic Lipidosis
Wikipedia
Note the ears and eye-membrane Feline hepatic lipidosis , also known as feline fatty liver syndrome , is one of the most common forms of liver disease of cats. [1] The disease officially has no known cause, though obesity is known to increase the risk. [2] The disease begins when the cat stops eating from a loss of appetite, forcing the liver to convert body fat into usable energy. ... Archived 2007-09-28 at the Wayback Machine ^ a b c "Feline Hepatic Lipidosis (Fatty Liver Syndrome)" . Archived from the original on 2007-08-29 . Retrieved 2007-09-02 . ^ Feline Hepatic Lipidosis—Fatty Liver Disease in Cats ^ [1] ^ Sarah Wootten DVM, " Why Is My Cat Not Eating?" , The Idle Cat ^ Fatty Liver Syndrom—Ways to encourage anorexic cats to eat v t e Domestic cats Felinology Anatomy Genetics Dwarf cat Kitten Odd-eyed cat Squitten Coat genetics Bicolor cat Black cat Calico cat Tabby cat Tortoiseshell cat Health Aging Declawing Diet dental health senior Neutering Spaying Vaccination Behavior Body language Catfight Catnip valerian Communication Meow Purr Kneading Intelligence Play and toys Righting reflex Senses Human–cat interaction Ailurophobia Animal-assisted therapy Bodega cat Cat cafés Cat massage Cat meat Cat-scratch disease Cat show Cats in ancient Egypt Cultural depictions Internet Farm cat Feral cat Cats and Islam Lolcat National Cat Day Puppy cat Ship's cat Zoonosis Registries American Cat Fanciers Association Associazione Nazionale Felina Italiana Canadian Cat Association Cat Aficionado Association Cat Fanciers' Association Fédération Internationale Féline Governing Council of the Cat Fancy Southern Africa Cat Council The International Cat Association World Cat Congress World Cat Federation Breeds ( full list ) ( experimental ) Fully domestic Abyssinian American Curl American Shorthair Balinese Brazilian Shorthair British Shorthair Birman Bombay Burmese Burmilla California Spangled Chartreux Chinese Li Hua Colorpoint Shorthair Cornish Rex Cymric Devon Rex Donskoy Egyptian Mau European Shorthair Exotic Shorthair German Rex Himalayan Japanese Bobtail Javanese Khao Manee Korat Kurilian Bobtail Lykoi Maine Coon Manx Munchkin Norwegian Forest Ocicat Ojos Azules Oriental Shorthair Persian Peterbald Pixie-bob Raas Ragdoll Ragamuffin Russian Blue Scottish Fold Selkirk Rex Siamese Siberian Singapura Snowshoe Somali Sphynx Thai Traditional Persian Tonkinese Toyger Turkish Angora Turkish Van Hybrid Bengal Chausie Highlander Savannah Serengeti Landraces Aegean Cyprus Domestic long-haired Domestic short-haired Kellas Sokoke Van Diseases and disorders Acne Asthma Calicivirus Congenital sensorineural deafness Feline corneal sequestrum Flea Heartworm Hepatic lipidosis Hypertrophic cardiomyopathy Immunodeficiency virus Infectious peritonitis Leukemia virus Lower urinary tract disease Panleukopenia Polydactyly Rabies Ringworm Roundworm Skin disorders Tick Toxoplasmosis Viral rhinotracheitis Book Category
-
Paralytic Shellfish Poisoning
Wikipedia
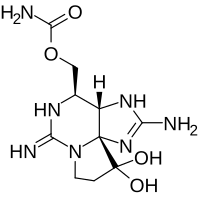
Syndrome of shellfish poisoning Paralytic shellfish poisoning The saxitoxin molecule shown in its unionized state. Paralytic shellfish poisoning ( PSP ) is one of the four recognized syndromes of shellfish poisoning , which share some common features and are primarily associated with bivalve mollusks (such as mussels , clams , oysters and scallops ). ... External links [ edit ] Toxicity, Shellfish v t e Poisoning Toxicity Overdose History of poison Inorganic Metals Toxic metals Beryllium Cadmium Lead Mercury Nickel Silver Thallium Tin Dietary minerals Chromium Cobalt Copper Iron Manganese Zinc Metalloids Arsenic Nonmetals Sulfuric acid Selenium Chlorine Fluoride Organic Phosphorus Pesticides Aluminium phosphide Organophosphates Nitrogen Cyanide Nicotine Nitrogen dioxide poisoning CHO alcohol Ethanol Ethylene glycol Methanol Carbon monoxide Oxygen Toluene Pharmaceutical Drug overdoses Nervous Anticholinesterase Aspirin Barbiturates Benzodiazepines Cocaine Lithium Opioids Paracetamol Tricyclic antidepressants Cardiovascular Digoxin Dipyridamole Vitamin poisoning Vitamin A Vitamin D Vitamin E Megavitamin-B 6 syndrome Biological 1 Fish / seafood Ciguatera Haff disease Ichthyoallyeinotoxism Scombroid Shellfish poisoning Amnesic Diarrhetic Neurotoxic Paralytic Other vertebrates amphibian venom Batrachotoxin Bombesin Bufotenin Physalaemin birds / quail Coturnism snake venom Alpha-Bungarotoxin Ancrod Batroxobin Arthropods Arthropod bites and stings bee sting / bee venom Apamin Melittin scorpion venom Charybdotoxin spider venom Latrotoxin / Latrodectism Loxoscelism tick paralysis Plants / fungi Cinchonism Ergotism Lathyrism Locoism Mushrooms Strychnine 1 including venoms , toxins , foodborne illnesses .
-
Chorionic Hematoma
Wikipedia
Journal Isr Med Assoc J. 2003 Jun;5(6):422-4 v t e Pregnancy and childbirth Planning Birth control Natural family planning Pre-conception counseling Conception Assisted reproductive technology Artificial insemination Fertility medication In vitro fertilisation Fertility awareness Unintended pregnancy Testing 3D ultrasound Obstetric ultrasonography Pregnancy test Home testing Prenatal diagnosis Prenatal Anatomy Amniotic fluid Amniotic sac Endometrium Placenta Development Fundal height Gestational age Human embryogenesis Maternal physiological changes Postpartum physiological changes Care Nutrition Environmental toxicants In pregnancy Prenatal Concomitant conditions Drinking Diabetes mellitus Smoking Vaping SLE Sexual activity during pregnancy Procedures Amniocentesis Cardiotocography Chorionic villus sampling Nonstress test Abortion Childbirth Preparation Bradley method Hypnobirthing Lamaze Nesting instinct Roles Doula Birth attendant Men's roles Midwife Obstetrician Perinatal nurse Traditional birth attendant Delivery Bloody show Childbirth positions Home birth Multiple birth Natural childbirth Pelvimetry / Bishop score Cervical dilation Cervical effacement Position Presentation Breech Cephalic Shoulder Rupture of membranes Unassisted childbirth Uterine contraction Water birth Postpartum Maternal Postpartum confinement Sex after pregnancy Psychiatric disorders of childbirth Postpartum physiological changes Roles Doula Health visitor Lactation consultant Monthly nurse Confinement nanny Infant Adaptation to extrauterine life Child care Congenital disorders Obstetric history Gravidity and parity v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy Category
-
Choledochal Cysts
Wikipedia
External links [ edit ] Classification D ICD - 10 : Q44.4 ICD - 9-CM : 751.69 MeSH : D015529 DiseasesDB : 2527 External resources eMedicine : article/172099 article/366004 article/934267 v t e Cystic diseases Respiratory system Langerhans cell histiocytosis Lymphangioleiomyomatosis Cystic bronchiectasis Skin stratified squamous: follicular infundibulum Epidermoid cyst and Proliferating epidermoid cyst Milia Eruptive vellus hair cyst outer root sheath Trichilemmal cyst and Pilar cyst and Proliferating trichilemmal cyst and Malignant trichilemmal cyst sebaceous duct Steatocystoma multiplex and Steatocystoma simplex Keratocyst nonstratified squamous: Cutaneous ciliated cyst Hidrocystoma no epithelium: Pseudocyst of the auricle Mucocele other and ungrouped: Cutaneous columnar cyst Keratin implantation cyst Verrucous cyst Adenoid cystic carcinoma Breast cyst Human musculoskeletal system Cystic hygroma Human digestive system oral cavity: Cysts of the jaws Odontogenic cyst Periapical cyst Dentigerous cyst Odontogenic keratocyst Nasopalatine duct cyst liver: Polycystic liver disease Congenital hepatic fibrosis Peliosis hepatis bile duct: Biliary hamartomas Caroli disease Choledochal cysts Bile duct hamartoma Nervous system Cystic leukoencephalopathy Genitourinary system Polycystic kidney disease Autosomal dominant polycystic kidney Autosomal recessive polycystic kidney Medullary cystic kidney disease Nephronophthisis Congenital cystic dysplasia Other conditions Hydatid cyst Von Hippel–Lindau disease Tuberous sclerosis v t e Congenital malformations and deformations of digestive system Upper GI tract Tongue , mouth and pharynx Cleft lip and palate Van der Woude syndrome tongue Ankyloglossia Macroglossia Hypoglossia Esophagus EA/TEF Esophageal atresia: types A, B, C, and D Tracheoesophageal fistula: types B, C, D and E esophageal rings Esophageal web (upper) Schatzki ring (lower) Stomach Pyloric stenosis Hiatus hernia Lower GI tract Intestines Intestinal atresia Duodenal atresia Meckel's diverticulum Hirschsprung's disease Intestinal malrotation Dolichocolon Enteric duplication cyst Rectum / anal canal Imperforate anus Rectovestibular fistula Persistent cloaca Rectal atresia Accessory Pancreas Annular pancreas Accessory pancreas Johanson–Blizzard syndrome Pancreas divisum Bile duct Choledochal cysts Caroli disease Biliary atresia Liver Alagille syndrome Polycystic liver disease
-
Vaginitis Emphysematosa
Wikipedia
PMID 11769034 . v t e Female diseases of the pelvis and genitals Internal Adnexa Ovary Endometriosis of ovary Female infertility Anovulation Poor ovarian reserve Mittelschmerz Oophoritis Ovarian apoplexy Ovarian cyst Corpus luteum cyst Follicular cyst of ovary Theca lutein cyst Ovarian hyperstimulation syndrome Ovarian torsion Fallopian tube Female infertility Fallopian tube obstruction Hematosalpinx Hydrosalpinx Salpingitis Uterus Endometrium Asherman's syndrome Dysfunctional uterine bleeding Endometrial hyperplasia Endometrial polyp Endometriosis Endometritis Menstruation Flow Amenorrhoea Hypomenorrhea Oligomenorrhea Pain Dysmenorrhea PMS Timing Menometrorrhagia Menorrhagia Metrorrhagia Female infertility Recurrent miscarriage Myometrium Adenomyosis Parametrium Parametritis Cervix Cervical dysplasia Cervical incompetence Cervical polyp Cervicitis Female infertility Cervical stenosis Nabothian cyst General Hematometra / Pyometra Retroverted uterus Vagina Hematocolpos / Hydrocolpos Leukorrhea / Vaginal discharge Vaginitis Atrophic vaginitis Bacterial vaginosis Candidal vulvovaginitis Hydrocolpos Sexual dysfunction Dyspareunia Hypoactive sexual desire disorder Sexual arousal disorder Vaginismus Urogenital fistulas Ureterovaginal Vesicovaginal Obstetric fistula Rectovaginal fistula Prolapse Cystocele Enterocele Rectocele Sigmoidocele Urethrocele Vaginal bleeding Postcoital bleeding Other / general Pelvic congestion syndrome Pelvic inflammatory disease External Vulva Bartholin's cyst Kraurosis vulvae Vestibular papillomatosis Vulvitis Vulvodynia Clitoral hood or clitoris Persistent genital arousal disorder v t e Female reproductive system Internal Adnexa Ovaries Follicles corpus hemorrhagicum luteum albicans Theca of follicle externa interna Follicular antrum Follicular fluid Corona radiata Zona pellucida Membrana granulosa Perivitelline space Other Germinal epithelium Tunica albuginea cortex Cumulus oophorus Stroma Medulla Fallopian tubes Isthmus Ampulla Infundibulum Fimbria Ostium Ligaments Ovarian ligament Suspensory ligament Wolffian vestiges Gartner's duct Epoophoron Vesicular appendages of epoophoron Paroophoron Uterus Regions Body Uterine cavity Fundus Cervix External orifice Cervical canal Internal orifice Supravaginal portion Vaginal portion Uterine horns Layers Endometrium epithelium Myometrium Perimetrium Parametrium Ligaments Round ligament Broad ligament Cardinal ligament Uterosacral ligament Pubocervical ligament General Uterine glands Vagina Fossa of vestibule of vagina Vaginal fornix Hymen Vaginal rugae Support structures Vaginal epithelium External Vulva Labia Mons pubis Labia majora Anterior commissure Posterior commissure Pudendal cleft Labia minora Frenulum of labia minora Frenulum of clitoris Vulval vestibule Interlabial sulci Bulb of vestibule Vaginal orifice vestibular glands/ducts Bartholin's glands/Bartholin's ducts Skene's glands/Skene's ducts Clitoris Crus of clitoris Body of clitoris ( Corpus cavernosum ) Clitoral glans Hood Urethra Urethral crest Other G-spot Urethral sponge Perineal sponge This women's health related article is a stub .
-
Xanthinuria
Wikipedia
External links [ edit ] Classification D ICD - 10 : E79.8 ICD - 9-CM : 277.2 OMIM : 278300 603592 MeSH : C566358, C566358, C562584 C562584, C566358, C566358, C562584 DiseasesDB : 14194 SNOMED CT : 190919008 External resources eMedicine : ped/2452 Xanthinuria at NIH 's Office of Rare Diseases v t e Inborn error of purine–pyrimidine metabolism Purine metabolism Anabolism Adenylosuccinate lyase deficiency Adenosine Monophosphate Deaminase Deficiency type 1 Nucleotide salvage Lesch–Nyhan syndrome / Hyperuricemia Adenine phosphoribosyltransferase deficiency Catabolism Adenosine deaminase deficiency Purine nucleoside phosphorylase deficiency Xanthinuria Gout Mitochondrial neurogastrointestinal encephalopathy syndrome Pyrimidine metabolism Anabolism Orotic aciduria Miller syndrome Catabolism Dihydropyrimidine dehydrogenase deficiency v t e Purine receptor modulators Receptor ( ligands ) P0 ( adenine ) Agonists: 8-Aminoadenine Adenine P1 ( adenosine ) Agonists: 2-(1-Hexynyl)- N -methyladenosine 2-Cl-IB-MECA 2'-MeCCPA 4'-O-β-D-Glucosyl-9-O-(6''-deoxysaccharosyl)olivil 5'- N -ethylcarboxamidoadenosine Adenosine ADP AMP Apadenoson ATL-146e ATP BAY 60–6583 Binodenoson Capadenoson CCPA CGS-21680 CP-532,903 Evodenoson GR 79236 LUF-5835 LUF-5845 N 6 -Cyclopentyladenosine Namodenoson Neladenoson dalanate Piclidenoson Regadenoson SDZ WAG 994 Selodenoson Sonedenoson Tecadenoson UK-432,097 Antagonists: 8-Chlorotheophylline 8-Phenyl-1,3-dipropylxanthine 8-Phenyltheophylline Acefylline Aminophylline ATL-444 Bamifylline Cafedrine Caffeine Caffeine citrate Cartazolate CGH-2466 CGS-15943 Choline theophyllinate Ciforadenant CPX CVT-6883 Dimethazan DMPX DPCPX Dyphylline Enprofylline Etazolate Fenethylline IBMX Isovaleric acid Istradefylline KF-26777 MRE3008F20 MRS-1220 MRS-1334 MRS-1706 MRS-1754 MRS-3777 Paraxanthine Pentoxifylline Preladenant Propentofylline Proxyphylline PSB-10 PSB-11 PSB-36 PSB-603 PSB-788 PSB-1115 Reversine Rolofylline SCH-442,416 SCH-58261 Theacrine Theobromine Theodrenaline Theophylline Tozadenant Tracazolate VUF-5574 ZM-241,385 P2 ( nucleotide ) P2X ( ATP ) Agonists: 2-Me-SATP α,β-Me-ATP Adenosine ADP AMP Ap4A Ap5A ATP ATPγS BzATP Cibacron blue CTP D-β,γ-Me-ATP GTP HT-AMP Ivermectin L-β,γ-Me-ATP MRS-2219 PAPET-ATP UTP Zinc Antagonists: 5-BDBD A-317491 A-438079 A-740003 A-804598 A-839977 AF-353 AZ-10606120 AZ-11645373 BBG Calcium Calmidazolium Chelerythrine Copper Emodin ( Rheum officinale ) Evans Blue Gefapixant GW-791343 HMA Ip5I isoPPADS JNJ-47965567 KN-04 KN-62 Magnesium MRS-2159 NF-023 NF-110 NF-157 NF-279 NF-449 Opiranserin (VVZ-149) Oxidized-ATP Phenol Red Phenolphthalein PPADS PPNDS PSB-12062 Puerarin ( Radix puerariae ) Purotoxin 1 RB-2 Ro 0437626 Ro 51 RO-3 Sodium ferulate ( Angelica sinensis , Ligusticum wallichii ) Suramin TC-P 262 Tetramethylpyrazine (ligustrazine) ( Ligusticum wallichii ) TNP-ATP Zinc P2Y Agonists: 2-Me-SADP 2-Me-SATP 2-Thio-UTP 5-Br-UDP 5-OMe-UDP α,β-Me-ATP Adenosine ADP ADPβS Ap3A AR-C 67085MX ATP ATPγS CTP dATP Denufosol Diquafosol IDP ITP INS-365 INS-37217 MRS-2365 MRS-2690 MRS-2693 MRS-2768 MRS-2957 MRS-4062 NF-546 PAPET-ATP PSB-0474 PSB-1114 UDP UDPβS UDP-galactose UDP-glucose UDP-N-acetylglucosamine Up3U UTP UTPγS Antagonists: 2-Me-SAMP A3P5PS AMPαS Ap4A AR-C 66096 AR-C 67085MX AR-C 69931MX AR-C 118925XX ATP BzATP C1330-7 Cangrelor Clopidogrel Elinogrel Ip5I MRS-2179 MRS-2211 MRS-2279 MRS-2395 MRS-2500 MRS-2578 NF-157 NF-340 PIT PPADS Prasugrel PSB-0739 RB-2 Regrelor Suramin Ticagrelor Ticlopidine UDP Transporter ( blockers ) CNTs 6-Hydroxy-7-methoxyflavone Adenosine dMeThPmR Estradiol KGO-2142 KGO-2173 MeThPmR Phloridzin Progesterone ENTs Barbiturates Benzodiazepines Cilostazol Dilazep Dipyridamole Estradiol Ethanol Hexobendine NBMPR Pentoxifylline Progesterone Propentofylline PMAT Decynium-22 Enzyme ( inhibitors ) XO Allopurinol Amflutizole Benzbromarone Caffeic acid Cinnamaldehyde Cinnamomum osmophloeum Febuxostat Myo-inositol Kaempferol Myricetin Niraxostat Oxipurinol Phytic acid Pistacia integerrima Propolis Quercetin Tisopurine Topiroxostat Others Aminopterin Azathioprine Methotrexate Mycophenolic acid Pemetrexed Pralatrexate Many others Others Precursors: Adenine Adenosine AMP ADP ATP Cytosine Cytidine CMP CDP CTP Guanine Guanosine GMP GDP GTP Hypoxanthine Inosine IMP IDP ITP Ribose Uracil Uridine UMP UDP UTP Others: Chrysophanol ( rhubarb ) See also: Receptor/signaling modulators
-
Pseudomonas Infection
Wikipedia
External links [ edit ] Classification D ICD - 10 : B96.5, J15.1, P23.5 ICD - 9-CM : 041.7 , 482.1 MeSH : D011552 v t e Proteobacteria -associated Gram-negative bacterial infections α Rickettsiales Rickettsiaceae / ( Rickettsioses ) Typhus Rickettsia typhi Murine typhus Rickettsia prowazekii Epidemic typhus , Brill–Zinsser disease , Flying squirrel typhus Spotted fever Tick-borne Rickettsia rickettsii Rocky Mountain spotted fever Rickettsia conorii Boutonneuse fever Rickettsia japonica Japanese spotted fever Rickettsia sibirica North Asian tick typhus Rickettsia australis Queensland tick typhus Rickettsia honei Flinders Island spotted fever Rickettsia africae African tick bite fever Rickettsia parkeri American tick bite fever Rickettsia aeschlimannii Rickettsia aeschlimannii infection Mite-borne Rickettsia akari Rickettsialpox Orientia tsutsugamushi Scrub typhus Flea-borne Rickettsia felis Flea-borne spotted fever Anaplasmataceae Ehrlichiosis : Anaplasma phagocytophilum Human granulocytic anaplasmosis , Anaplasmosis Ehrlichia chaffeensis Human monocytotropic ehrlichiosis Ehrlichia ewingii Ehrlichiosis ewingii infection Rhizobiales Brucellaceae Brucella abortus Brucellosis Bartonellaceae Bartonellosis : Bartonella henselae Cat-scratch disease Bartonella quintana Trench fever Either B. henselae or B. quintana Bacillary angiomatosis Bartonella bacilliformis Carrion's disease , Verruga peruana β Neisseriales M+ Neisseria meningitidis/meningococcus Meningococcal disease , Waterhouse–Friderichsen syndrome , Meningococcal septicaemia M− Neisseria gonorrhoeae/gonococcus Gonorrhea ungrouped: Eikenella corrodens / Kingella kingae HACEK Chromobacterium violaceum Chromobacteriosis infection Burkholderiales Burkholderia pseudomallei Melioidosis Burkholderia mallei Glanders Burkholderia cepacia complex Bordetella pertussis / Bordetella parapertussis Pertussis γ Enterobacteriales ( OX− ) Lac+ Klebsiella pneumoniae Rhinoscleroma , Pneumonia Klebsiella granulomatis Granuloma inguinale Klebsiella oxytoca Escherichia coli : Enterotoxigenic Enteroinvasive Enterohemorrhagic O157:H7 O104:H4 Hemolytic-uremic syndrome Enterobacter aerogenes / Enterobacter cloacae Slow/weak Serratia marcescens Serratia infection Citrobacter koseri / Citrobacter freundii Lac− H2S+ Salmonella enterica Typhoid fever , Paratyphoid fever , Salmonellosis H2S− Shigella dysenteriae / sonnei / flexneri / boydii Shigellosis , Bacillary dysentery Proteus mirabilis / Proteus vulgaris Yersinia pestis Plague / Bubonic plague Yersinia enterocolitica Yersiniosis Yersinia pseudotuberculosis Far East scarlet-like fever Pasteurellales Haemophilus : H. influenzae Haemophilus meningitis Brazilian purpuric fever H. ducreyi Chancroid H. parainfluenzae HACEK Pasteurella multocida Pasteurellosis Actinobacillus Actinobacillosis Aggregatibacter actinomycetemcomitans HACEK Legionellales Legionella pneumophila / Legionella longbeachae Legionnaires' disease Coxiella burnetii Q fever Thiotrichales Francisella tularensis Tularemia Vibrionaceae Vibrio cholerae Cholera Vibrio vulnificus Vibrio parahaemolyticus Vibrio alginolyticus Plesiomonas shigelloides Pseudomonadales Pseudomonas aeruginosa Pseudomonas infection Moraxella catarrhalis Acinetobacter baumannii Xanthomonadaceae Stenotrophomonas maltophilia Cardiobacteriaceae Cardiobacterium hominis HACEK Aeromonadales Aeromonas hydrophila / Aeromonas veronii Aeromonas infection ε Campylobacterales Campylobacter jejuni Campylobacteriosis , Guillain–Barré syndrome Helicobacter pylori Peptic ulcer , MALT lymphoma , Gastric cancer Helicobacter cinaedi Helicobacter cellulitis
-
Fetal Rhabdomyoma
Wikipedia
Contents 1 Signs and symptoms 2 Pathophysiology 2.1 Gross pathology 2.2 Microscopic pathology 3 Diagnosis 3.1 Ancillary testing 3.2 Differential diagnosis 4 Management 5 Epidemiology 6 References Signs and symptoms [ edit ] Most fetal rhabdomyomas are tumors that develop in the head and neck or in the genital region. [1] There are a number of cases which have been seen in association with Gorlin syndrome . [2] [3] However, cardiac myxomas are known to be associated with tuberous sclerosis . ... Pediatr Surg Int 1997;12(7):544-7. ^ Watson J, Depasquale K, Ghaderi M, Zwillenberg S. Nevoid basal cell carcinoma syndrome and fetal rhabdomyoma: a case study. ... Neural variant of fetal rhabdomyoma and naevoid basal cell carcinoma syndrome. Histopathology 1996;29(3):247-52. ^ Walsh SN, Hurt MA.