-
Overactive Bladder
Wikipedia
Wet variants are more common than dry variants. [22] The distinction is not absolute; one study suggested that many classified as "dry" were actually "wet" and that people with no history of any leakage may have had other syndromes. [23] OAB is distinct from stress urinary incontinence , but when they occur together, the condition is usually known as mixed incontinence. ... PMID 27935011 . ^ Abrams, Paul (2011). Overactive bladder syndrome and urinary incontinence . Oxford: Oxford University Press. pp. 7–8. ... "[Physiopathology of overactive bladder syndrome]". Urologia . 79 (1): 24–35. doi : 10.5301/RU.2012.8972 . ... "Future perspectives in pharmacological treatments options for overactive bladder syndrome". Eur Urol Review . 7 (2): 120–126. ^ Sacco E, Pinto F, Bassi P (April 2008). ... "Investigational drug therapies for overactive bladder syndrome: the potential alternatives to anticholinergics".
-
Obsessive–compulsive Personality Disorder
Wikipedia
OCPD is highly comorbid with other personality disorders , Asperger's syndrome , [9] [10] eating disorders , [11] anxiety , mood disorders , and substance use disorders . [4] The disorder is the most common personality disorder in the United States, [12] and is diagnosed twice as often in males as in females, [5] however, there is evidence to suggest the prevalence between men and women is equal. [4] Contents 1 Signs and symptoms 1.1 Attention to order and perfection 1.2 Devotion to productivity 1.3 Rigidity 1.4 Restricted emotions and interpersonal functioning 1.5 Interpersonal control 1.6 Millon's subtypes 1.6.1 The Conscientious Compulsive 1.6.2 The Puritanical Compulsive 1.6.3 The Bureaucratic Compulsive 1.6.4 The Parsimonious Compulsive 1.6.5 The Bedevilled Compulsive 2 Cause 3 Diagnosis 3.1 DSM-5 3.1.1 Alternative model for diagnosis 3.1.2 Differential diagnosis 3.2 ICD-10 4 Comorbidity 4.1 Obsessive-compulsive disorder 4.2 Asperger's syndrome 4.3 Eating disorders 4.4 Other disorders and conditions 5 Treatment 6 Epidemiology 7 History 8 See also 9 References 10 Further reading 11 External links Signs and symptoms [ edit ] Obsessive-compulsive personality disorder (OCPD) is marked by an excessive obsession with rules, lists, schedules, and order; a need for perfectionism that interferes with efficiency and the ability to complete tasks; a devotion to productivity that hinders interpersonal relationships and leisure time; rigidity and zealousness on matters of morality and ethics ; an inability to delegate responsibilities or work to others; restricted functioning in interpersonal relationships; restricted expression of emotion and affect ; and a need for control over one's environment and self. [5] [13] Some of OCPD's symptoms are persistent and stable, whilst others are unstable. ... Comorbidity [ edit ] Several disorders have been observed to have a higher risk of comorbidity with OCPD, they include: obsessive-compulsive disorder , eating disorders , Asperger's syndrome , depression , and anxiety . Obsessive-compulsive disorder [ edit ] OCPD is often confused with obsessive - compulsive disorder (OCD). ... In contrast, the trait of perfectionism may improve the outcome of treatment as patients are likely to complete homework assigned to them with determination. [20] The findings with regards to pharmacological treatment has also been mixed, with some studies showing a lower reception to SRIs in OCD patients with comorbid OCPD, with others showing no relationship. [20] Comorbidity between OCD and OCPD has been linked to a more severe presentation of symptoms, [22] a younger age of onset, [20] more significant impairment in functioning, poorer insight, [23] and higher comorbidity of depression and anxiety. [23] Asperger's syndrome [ edit ] There are considerable similarities and overlap between Asperger's syndrome and OCPD, [9] such as list-making, inflexible adherence to rules, and obsessive aspects of Asperger's syndrome , although the latter may be distinguished from OCPD especially regarding affective behaviors, worse social skills, difficulties with Theory of Mind and intense intellectual interests, e.g. an ability to recall every aspect of a hobby. [24] A 2009 study involving adult autistic people found that 40% of those diagnosed with Asperger's syndrome met the diagnostic requirements for a comorbid OCPD diagnosis. [10] Eating disorders [ edit ] In people with eating disorders , 13% also have OCPD. [4] Regardless of the prevalence of the full-fledged OCPD among eating disordered samples, the presence of this personality disorder or its traits, such as perfectionism, has been found to be positively correlated with a range of complications in eating disorders and a negative outcome, as opposed to impulsive features—those linked with histrionic personality disorder , for example—which predict a better outcome from treatment. [25] OCPD predicts more severe symptoms of Anorexia Nervosa , [26] and worse remission rates, [26] however, OCPD and perfectionistic traits predicted a higher acceptance of treatment, which was defined as undergoing 5 weeks of treatment. [26] People with Anorexia Nervosa who exercise excessively display a higher prevalence of several OCPD traits when compared to their counterparts who did not exercise excessively. [27] The traits included self-imposed perfectionism , and the childhood OCPD traits of being rule-bound and cautious. ... ISBN 978-0-89042-554-1 . ^ a b Gillberg C, Billstedt E (November 2000). "Autism and Asperger syndrome: coexistence with other clinical disorders". ... "Diagnosis and differential diagnosis of Asperger syndrome" . Advances in Psychiatric Treatment . 7 (4): 310–318. doi : 10.1192/apt.7.4.310 .
-
Nerve Injury
Wikipedia
Several of these can also boost the regenerative capacity of CNS neurons, making them potential therapeutic targets for treating spinal cord injury and stroke. [3] Role of Schwann cells [ edit ] Guillain–Barré syndrome – nerve damage Schwann cells are active in Wallerian degeneration. ... External links [ edit ] Classification D ICD - 10 : T14.4 v t e Neurotrauma Traumatic brain injury Intracranial hemorrhage Intra-axial Intraparenchymal hemorrhage Intraventricular hemorrhage Extra-axial Subdural hematoma Epidural hematoma Subarachnoid hemorrhage Brain herniation Cerebral contusion Cerebral laceration Concussion Post-concussion syndrome Second-impact syndrome Dementia pugilistica Chronic traumatic encephalopathy Diffuse axonal injury Abusive head trauma Penetrating head injury Spinal cord injury Anterior spinal artery syndrome Brown-Séquard syndrome Cauda equina syndrome Central cord syndrome Paraplegia Posterior cord syndrome Spinal cord injury without radiographic abnormality Tetraplegia (Quadriplegia) Peripheral nerves Nerve injury Peripheral nerve injury classification Wallerian degeneration Injury of accessory nerve Brachial plexus injury Traumatic neuroma
-
Placenta Praevia
Wikipedia
External links [ edit ] Classification D ICD - 10 : O44 , P02.0 ICD - 9-CM : 641.0 , 641.1 MeSH : D010923 External resources MedlinePlus : 000900 v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy Category v t e Conditions originating in the perinatal period / fetal disease Maternal factors complicating pregnancy, labour or delivery placenta Placenta praevia Placental insufficiency Twin-to-twin transfusion syndrome chorion / amnion Chorioamnionitis umbilical cord Umbilical cord prolapse Nuchal cord Single umbilical artery presentation Breech birth Asynclitism Shoulder presentation Growth Small for gestational age / Large for gestational age Preterm birth / Postterm pregnancy Intrauterine growth restriction Birth trauma scalp Cephalohematoma Chignon Caput succedaneum Subgaleal hemorrhage Brachial plexus injury Erb's palsy Klumpke paralysis Affected systems Respiratory Intrauterine hypoxia Infant respiratory distress syndrome Transient tachypnea of the newborn Meconium aspiration syndrome Pleural disease Pneumothorax Pneumomediastinum Wilson–Mikity syndrome Bronchopulmonary dysplasia Cardiovascular Pneumopericardium Persistent fetal circulation Bleeding and hematologic disease Vitamin K deficiency bleeding HDN ABO Anti-Kell Rh c Rh D Rh E Hydrops fetalis Hyperbilirubinemia Kernicterus Neonatal jaundice Velamentous cord insertion Intraventricular hemorrhage Germinal matrix hemorrhage Anemia of prematurity Gastrointestinal Ileus Necrotizing enterocolitis Meconium peritonitis Integument and thermoregulation Erythema toxicum Sclerema neonatorum Nervous system Perinatal asphyxia Periventricular leukomalacia Musculoskeletal Gray baby syndrome muscle tone Congenital hypertonia Congenital hypotonia Infections Vertically transmitted infection Neonatal infection rubella herpes simplex mycoplasma hominis ureaplasma urealyticum Omphalitis Neonatal sepsis Group B streptococcal infection Neonatal conjunctivitis Other Miscarriage Perinatal mortality Stillbirth Infant mortality Neonatal withdrawal
-
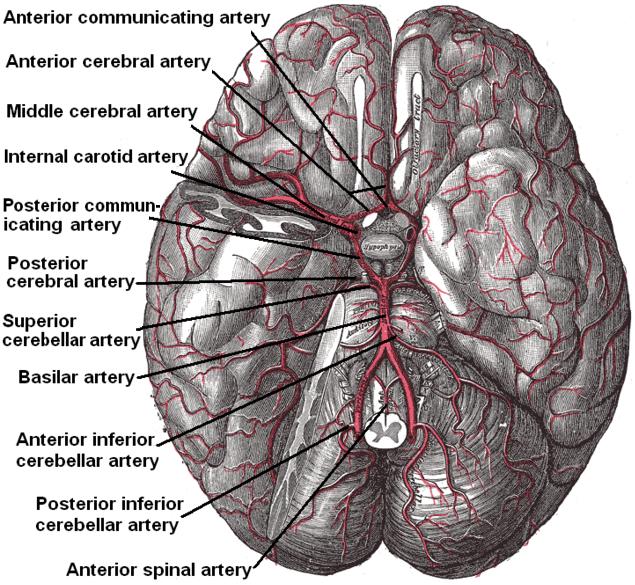
Cerebral Hypoxia
Wikipedia
Problems after delivery can include severe prematurity, severe lung or heart disease, serious infections, trauma to the brain or skull, congenital malformations of the brain or very low blood pressure in the baby [16] and due to suffocation in cases of Münchausen syndrome by proxy . [17] The severity of a neonatal hypoxic-ischaemic brain injury may be assessed using Sarnat staging , which is based on clinical presentation and EEG findings, and also using MRI . [18] Mechanism [ edit ] Main article: Mechanism of anoxic depolarization in the brain Details of the mechanism of damage from cerebral hypoxia, along with anoxic depolarization, can be found here: Mechanism of anoxic depolarization in the brain Diagnosis [ edit ] Classification [ edit ] Cerebral hypoxia is typically grouped into four categories depending on the severity and location of the brain's oxygen deprivation: [19] Aneurysm in a cerebral artery, one cause of hypoxic anoxic injury (HAI). ... External links [ edit ] Classification D ICD - 9-CM : 437.9 MeSH : D002534 SNOMED CT : 389088001 External resources MedlinePlus : 001435 Hypoxia experiment v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension
-
Isca2-Related Mitochondrial Disorder
Gene_reviews
Disorders to Consider in the Differential Diagnosis of ISCA2 -Related Mitochondrial Disorder (IRMD) View in own window Disorder Gene(s) MOI Clinical Features of This Disorder Overlapping w/IRMD Distinguishing from IRMD Multiple mitochondrial dysfunctions syndrome 1 NFU1 AR Feeding difficulties Muscle weakness Decreasing responsiveness Neurologic regression White matter lesions on brain MRI Lactic acidosis ↓ activity of mt respiratory complexes Pulmonary hypertension Obstructive vasculopathy Spongiform degeneration & white matter necrosis Onset soon after birth Multiple mitochondrial dysfunctions syndrome 2 BOLA3 AR Optic atrophy Visual impairment Spasticity Leukodystrophy Spinal cord lesions Lactic acidosis Onset in infancy ↓ activity of mt respiratory complexes Cardiomyopathy Hepatomegaly Extrapyramidal signs Ataxia Myoclonus Multiple mitochondrial dysfunctions syndrome 3 IBA57 AR White matter abnormalities Lactic acidosis ↓ activity of mt respiratory complexes Onset in utero Intrauterine growth restriction Microcephaly Dysmorphic features (retrognathia, high-arched palate, widely spaced nipples) Arthrogryposis Severe hypotonia Polymicrogyria Hypoplasia of the corpus callosum Hypoplasia of the medulla oblongata ISCA1 -related multiple mitochondrial dysfunctions syndrome ISCA1 AR Neurologic regression White matter abnormalities Lactic acidosis Abnormalities of cortical migration Metachromatic leukodystrophy ARSA or PSAP AR Neurologic regression Leukodystrophy Spasticity Optic atrophy ↑ urinary sulfatide excretion Krabbe disease GALC AR Neurologic regression Leukodystrophy Spasticity Optic atrophy Pattern of MRI findings, incl involvement of thalami & caudate Leukoencephalopathy with brain stem and spinal cord involvement and lactate elevation DARS2 AR Neurologic regression ↑ lactate in serum & MR spectroscopy Pattern of MRI findings Childhood ataxia with central nervous system hypomyelination/vanishing white matter EIF2B1 EIF2B2 EIF2B3 EIF2B4 EIF2B5 AR Neurologic regression Leukodystrophy Spasticity Optic atrophy Unsteady gait Pattern of MRI findings Ovarian dysgenesis in females Canavan disease ASPA AR Neurologic regression Leukodystrophy Optic atrophy Macrocephaly Pattern of MRI findings Increased N-acetyl-L-aspartate in urine Alexander disease GFAP AD Neurologic regression Leukodystrophy Spasticity Optic atrophy Macrocephaly Pattern of MRI findings Leigh syndrome Hetero-geneous AR XL mt Neurologic regression ↑ lactate in serum & MR spectroscopy Hypertrophic cardiomyopathy Hypertrichosis Renal tubulopathy Liver involvement Bilateral symmetric T 2 -weighted hyperintensities in the basal ganglia &/or brain stem on MRI Basal ganglia involvement AD = autosomal dominant; AR = autosomal recessive; MOI = mode of inheritance; mt = mitochondrial; XL = X-linked Other leukodystrophies and lysosomal storage diseases. ... See Multiple Mitochondrial Dysfunctions Syndrome: OMIM Phenotypic Series to view genes associated with this phenotype in OMIM.
-
Pneumococcal Infection
Wikipedia
External links [ edit ] Classification D MeSH : D011008 November 2nd: World Pneumonia Day Website Pneumococcal Vaccine Accelerated Development and Introduction Plan v t e Firmicutes (low- G+C ) Infectious diseases Bacterial diseases : G+ Bacilli Lactobacillales ( Cat- ) Streptococcus α optochin susceptible S. pneumoniae Pneumococcal infection optochin resistant Viridans streptococci : S. mitis S. mutans S. oralis S. sanguinis S. sobrinus S. anginosus group β A bacitracin susceptible: S. pyogenes Group A streptococcal infection Streptococcal pharyngitis Scarlet fever Erysipelas Rheumatic fever B bacitracin resistant, CAMP test +: S. agalactiae Group B streptococcal infection ungrouped Streptococcus iniae Cutaneous Streptococcus iniae infection γ D BEA +: Streptococcus bovis Enterococcus BEA +: Enterococcus faecalis Urinary tract infection Enterococcus faecium Bacillales ( Cat+ ) Staphylococcus Cg+ S. aureus Staphylococcal scalded skin syndrome Toxic shock syndrome MRSA Cg- novobiocin susceptible S. epidermidis novobiocin resistant S. saprophyticus Bacillus Bacillus anthracis Anthrax Bacillus cereus Food poisoning Listeria Listeria monocytogenes Listeriosis Clostridia Clostridium ( spore -forming) motile: Clostridium difficile Pseudomembranous colitis Clostridium botulinum Botulism Clostridium tetani Tetanus nonmotile: Clostridium perfringens Gas gangrene Clostridial necrotizing enteritis Finegoldia (non-spore forming) Finegoldia magna Mollicutes Mycoplasmataceae Ureaplasma urealyticum Ureaplasma infection Mycoplasma genitalium Mycoplasma pneumoniae Mycoplasma pneumonia Anaeroplasmatales Erysipelothrix rhusiopathiae Erysipeloid v t e Meningitis and other diseases of meninges Meningitis Arachnoiditis Bacterial Tuberculous Haemophilus Pneumococcal Viral Herpesviral Fungal Cryptococcal Aseptic Drug-induced Other Meningoencephalitis v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisTIRAP, CRP, IL10, NLRP3, IL6, MBL2, TLR2, TLR4, IL1B, SPDYA, PTAFR, TNF, IFNG, VWF, IL17A, IL22, GAPDH, EEF1A1, CASP1, PER2, AIM2, CLOCK, ICOS, FSTL1, VCAM1, IL37, SPP1, IL17B, SELPLG, PYCARD, AGTR1, TBX21, MYDGF, IL27, IL31RA, TSLP, COLEC11, NFKBIZ, IL22RA1, SBNO1, NOX4, SARS2, IL17D, TLR7, IRAK4, IL20, CXCL5, SELP, MAPK3, CCL5, CCL2, IGHA1, IFNAR1, IFNA13, IFNA1, HIF1A, FN1, FLT3LG, FCN2, FCGR2A, ESR2, ENO1, DLD, CSF3, CD14, STS, IGHG3, IL1A, CXCL8, MUC5AC, SARS1, PTX3, ARNTL, PIK3CD, NT5E, TONSL, MUC1, CXCL10, MPO, CD99, SMAD7, LTA, LCN2, ITIH4, CCR2
-
Adhesive Capsulitis Of The Shoulder
Wikipedia
This generally lasts from 5 to 26 months. [7] Physical exam findings include restricted range of motion in all planes of movement in both active and passive range of motion . [8] This contrasts with conditions such as shoulder impingement syndrome or rotator cuff tendinitis in which the active range of motion is restricted but passive range of motion is normal. ... Symptoms in people with diabetes may be more protracted than in the non-diabetic population. [28] See also [ edit ] Calcific tendinitis Milwaukee shoulder syndrome References [ edit ] ^ a b c d e f g h i j k l m n o p q r s t u Ramirez, J (1 March 2019). ... External links [ edit ] Classification D ICD - 10 : M75.0 ICD - 9-CM : 726.0 DiseasesDB : 34114 External resources MedlinePlus : 000455 eMedicine : orthoped/372 v t e Soft tissue disorders Capsular joint Synoviopathy Synovitis / Tenosynovitis Calcific tendinitis Stenosing tenosynovitis Trigger finger De Quervain syndrome Transient synovitis Ganglion cyst osteochondromatosis Synovial osteochondromatosis Plica syndrome villonodular synovitis Giant-cell tumor of the tendon sheath Bursopathy Bursitis Olecranon Prepatellar Trochanteric Subacromial Achilles Retrocalcaneal Ischial Iliopsoas Synovial cyst Baker's cyst Calcific bursitis Noncapsular joint Symptoms Ligamentous laxity Hypermobility Enthesopathy / Enthesitis / Tendinopathy upper limb Adhesive capsulitis of shoulder Impingement syndrome Rotator cuff tear Golfer's elbow Tennis elbow lower limb Iliotibial band syndrome Patellar tendinitis Achilles tendinitis Calcaneal spur Metatarsalgia Bone spur other/general: Tendinitis / Tendinosis Nonjoint Fasciopathy Fasciitis : Plantar Nodular Necrotizing Eosinophilic Fibromatosis / contracture Dupuytren's contracture Plantar fibromatosis Aggressive fibromatosis Knuckle pads Authority control NDL : 00562580
-
Intention Tremor
Wikipedia
These include a variety of neurological disorders, such as stroke , alcoholism , alcohol withdrawal , peripheral neuropathy , Wilson's disease , Creutzfeldt–Jakob disease , Guillain–Barré syndrome and fragile X syndrome , as well as brain tumors , low blood sugar , hyperthyroidism , hypoparathyroidism , insulinoma , normal aging, and traumatic brain injury . [1] [5] [6] [7] Holmes tremor , a rubral or midbrain tremor, is another form of tremor that includes intention tremors, among other symptoms. ... "Differential diagnosis of common tremor syndromes" . Postgraduate Medical Journal . 81 (962): 756–62. doi : 10.1136/pgmj.2005.032979 . ... “Fragile X-Associated Tremor/Ataxia Syndrome-An Older Face of the Fragile X Gene.” 2007. ... External links [ edit ] Classification D ICD - 10 : G25.2 ICD - 9-CM : 333.1 MeSH : D014202 v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis
-
Pituitary Pars Intermedia Dysfunction
Wikipedia
Contents 1 Pathophysiology 1.1 Dopaminergic control of the pars intermedia 1.2 POMC 2 Age and breed prevalence 3 Clinical signs 3.1 Laboratory findings 3.2 Differentiating from Equine Metabolic Syndrome 4 Diagnosis 4.1 Plasma ACTH concentration 4.2 Thyrotropin-releasing hormone stimulation test 4.3 Dexamethasone suppression test 4.4 Urinary corticoid-to-creatinine ratio 4.5 Plasma cortisol concentration 4.6 Current recommendations for testing 5 Insulin dysregulation 5.1 Testing for insulin resistance 5.2 Management of insulin resistance 6 Treatment 7 See also 8 References Pathophysiology [ edit ] Unlike the human and canine forms of Cushing's disease , which most commonly affect the pars distalis region of the pituitary gland, equine Cushing's disease is a result of hyperplasia or adenoma formation in the pars intermedia. [2] This adenoma then secretes excessive amounts of normal products, leading to clinical signs. ... Persistent hyperglycemia and glucosuria are very commonly seen. [1] Hyperlipidemia may be present, especially in ponies. [1] Other abnormalities associated with the disease include mild anemia, neurophilia, lymphopenia, eosinopenia, and increased liver enzymes. [2] Differentiating from Equine Metabolic Syndrome [ edit ] PPID shares similarities to Equine Metabolic Syndrome , which also causes regional adiposity, laminitis, and insulin resistance. ... In these horses, the thyrotropin-releasing hormone stimulation test should either be used as an initial screening test, or to confirm a false resting ACTH. [11] Insulin dysregulation [ edit ] Insulin dysregulation is commonly seen in horses with PPID or equine metabolic syndrome , and is associated with obesity. ... Other clinical signs, such as hirsutism, potbellied appearance, muscle wasting, laminitic episodes, and increased predisposition to infection usually take between 30 days and 1 year to improve. [11] Cyproheptadine may be added to the treatment regime in horses that are inadequately responding to pergolide, [11] but is usually only used in horses with advanced PPID on high doses of pergolide. [13] See also [ edit ] Equine metabolic syndrome Henneke horse body condition scoring system References [ edit ] ^ a b c d e f g h i j k l m n o p q r s Stephen M. ... PMID 25641552 . ^ Frank, N., Geor, R.J., Bailey, S.R., Durham, A.E. and Johnson, P.J. (2010), Equine Metabolic Syndrome. Journal of Veterinary Internal Medicine, 24: 467–475. doi: 10.1111/j.1939-1676.2010.0503.x ^ a b c d e f g h i Drs.
-
Eclabium
Wikipedia
Biomedical Papers . 164 (4): 357–365. doi : 10.5507/bp.2020.050 . v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease Category:Lip disorders
-
Nasal Polyp
Wikipedia
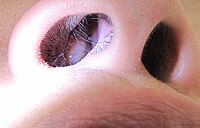
Nasal polyps A nasal polyp Specialty Otorhinolaryngology Symptoms Trouble breathing through the nose, loss of smell , decreased taste, post nasal drip , runny nose [1] Complications Sinusitis , broadening of the nose [2] [3] Causes Unclear [1] Risk factors Allergies , cystic fibrosis , aspirin sensitivity , certain infections [1] Diagnostic method Looking up the nose, CT scan [1] Treatment Steroid nasal spray , surgery , antihistamines [1] Frequency ~4% [1] Nasal polyps ( NP ) are noncancerous growths within the nose or sinuses . [1] Symptoms include trouble breathing through the nose, loss of smell , decreased taste, post nasal drip , and a runny nose . [1] The growths are sac-like , movable, and nontender, though face pain may occasionally occur. [1] They typically occur in both nostrils in those who are affected. [1] Complications may include sinusitis and broadening of the nose. [2] The exact cause is unclear. [1] They may be related to chronic inflammation of the lining of the sinuses. [1] They occur more commonly among people who have allergies , cystic fibrosis , aspirin sensitivity , or certain infections. [1] The polyp itself represents an overgrowth of the mucous membranes. [1] Diagnosis may occur by looking up the nose. [1] A CT scan may be used to determine the number of polyps and help plan surgery. [1] Treatment is typically with steroids , often in the form of a nasal spray . [1] If this is not effective, surgery may be considered. [1] The condition often recurs following surgery; thus, continued use of a steroid nasal spray is often recommended. [1] Antihistamines may help with symptoms but do not change the underlying disease. [1] Antibiotics are not required for treatment unless an infection occurs. [1] About 4% of people currently have nasal polyps while up to 40% of people develop them at some point in their life. [1] They most often occur after the age of 20 and are more frequent in males than females. [1] Nasal polyps have been described since the time of the Ancient Egyptians . [4] Contents 1 Signs and symptoms 2 Causes 3 Pathophysiology 4 Diagnosis 4.1 Types 4.2 CT scan 4.3 Histology 4.4 Differential diagnosis 5 Treatment 5.1 Surgery 6 Epidemiology 7 References 8 External links Signs and symptoms [ edit ] Symptoms of polyps include nasal congestion , sinusitis , loss of smell , thick nasal discharge, facial pressure, nasal speech, and mouth breathing. [5] Recurrent sinusitis can result from polyps. [2] Long-term, nasal polyps can cause destruction of the nasal bones and widening of the nose. [2] As polyps grow larger, they eventually prolapse into the nasal cavity resulting in symptoms. [6] The most prominent symptoms of nasal polyps is blockage of the nasal passage. [7] People with nasal polyps due to aspirin intolerance often have symptoms known as Samter's triad, which consists of asthma worse with aspirin, a skin rash caused by aspirin, and chronic nasal polyps. [5] Causes [ edit ] The exact cause of nasal polyps is unclear. [1] They are, however, commonly associated with conditions that cause long term inflammation of the sinuses. [8] This includes chronic rhinosinusitis , asthma , aspirin sensitivity, and cystic fibrosis . [8] Various additional diseases associated with polyp formation include: [9] Allergic fungal sinusitis Kartagener's syndrome Young's syndrome Eosinophilic granulomatosis with polyangiitis Nasal mastocytosis Chronic rhinosinusitis is a common medical condition characterized by symptoms of sinus inflammation lasting at least 12 weeks. ... Classification D ICD - 10 : J33 ICD - 9-CM : 471 MeSH : D009298 External resources MedlinePlus : 001641 eMedicine : ent/334 ent/335 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis v t e Medicine Specialties and subspecialties Surgery Cardiac surgery Cardiothoracic surgery Colorectal surgery Eye surgery General surgery Neurosurgery Oral and maxillofacial surgery Orthopedic surgery Hand surgery Otolaryngology ENT Pediatric surgery Plastic surgery Reproductive surgery Surgical oncology Transplant surgery Trauma surgery Urology Andrology Vascular surgery Internal medicine Allergy / Immunology Angiology Cardiology Endocrinology Gastroenterology Hepatology Geriatrics Hematology Hospital medicine Infectious disease Nephrology Oncology Pulmonology Rheumatology Obstetrics and gynaecology Gynaecology Gynecologic oncology Maternal–fetal medicine Obstetrics Reproductive endocrinology and infertility Urogynecology Diagnostic Radiology Interventional radiology Nuclear medicine Pathology Anatomical Clinical pathology Clinical chemistry Cytopathology Medical microbiology Transfusion medicine Other Addiction medicine Adolescent medicine Anesthesiology Dermatology Disaster medicine Diving medicine Emergency medicine Mass gathering medicine Family medicine General practice Hospital medicine Intensive care medicine Medical genetics Narcology Neurology Clinical neurophysiology Occupational medicine Ophthalmology Oral medicine Pain management Palliative care Pediatrics Neonatology Physical medicine and rehabilitation PM&R Preventive medicine Psychiatry Addiction psychiatry Radiation oncology Reproductive medicine Sexual medicine Sleep medicine Sports medicine Transplantation medicine Tropical medicine Travel medicine Venereology Medical education Medical school Bachelor of Medicine, Bachelor of Surgery Bachelor of Medical Sciences Master of Medicine Master of Surgery Doctor of Medicine Doctor of Osteopathic Medicine MD–PhD Related topics Alternative medicine Allied health Dentistry Podiatry Pharmacy Physiotherapy Molecular oncology Nanomedicine Personalized medicine Public health Rural health Therapy Traditional medicine Veterinary medicine Physician Chief physician History of medicine Book Category Commons Wikiproject Portal OutlineALOX15, KITLG, GATA3, HLA-DQA1, PTGER2, DNAH5, HLA-B, ZMYND10, STK11, RSPH9, TAP2, STK36, IL13, CYP2S1, TBX21, NME8, TAP1, DNAI1, GAS8, HYDIN, DNAAF5, FOXP1, IL17A, DNAH1, LRRC6, ARMC4, POSTN, IL1RL1, MUC5AC, TAPBP, IL18R1, DNAH11, OFD1, VEGFA, TGFB1, ECM1, TWIST1, GPX4, CCDC40, CCNO, TNF, MCIDAS, CCDC151, DNAAF1, PIH1D3, DNAAF4, GAS2L2, CCDC39, RSPH4A, CCDC114, DNAAF3, DNAJB13, CCDC103, MIR3936HG, IL4, RPGR, LRRC56, DRC1, MYRF, IL33, CFAP298, SPAG1, BACH2, IL5, DNAI2, TTC25, TMEM258, DNAAF2, DNAL1, RSPH3, CFAP300, CCDC65, SLC22A4, RSPH1, IL25, MMP9, MYDGF, CCL11, TSLP, NR3C1, CSF2, CCL5, PTGS2, IL1B, SCGB1A1, FOXP3, CXCL8, IL6, CFTR, PTGS1, IL10, IFNG, TLR9, IL22, CYSLTR1, CCL2, TNFSF4, MUC8, IL21, CD68, MMP2, COX2, MUC4, ICAM1, MTCO2P12, CCL17, RNASE3, CCL24, TLR4, EGFR, TIMP1, MUC5B, CRLF2, SPP1, BPIFA1, SOCS3, LGALS1, TNFSF13B, MMP1, TP53, S100A8, COX1, ABCB1, HPGDS, SDC1, CASP8, FGF2, HIF1A, F3, SLC26A4, CD1A, CHI3L1, CD69, CD40, CD19, IL17RB, OSM, CYSLTR2, CCL18, IL22RA1, ARG2, CAV1, BCL2, GORASP1, NOX4, RPE65, FOS, WNK1, RELA, ARHGAP24, PTGDS, MAPK1, PLA2G1B, FN1, STAT3, CXCL1, SYT1, MAPK14, CD163, GRAP2, CCL26, TP63, AHSA1, AIMP2, YWHAZ, HSD11B1, VDR, VCAM1, UVRAG, DEFB4A, CKAP4, EGF, SPINK5, TP73, PTGDR2, SIRT1, TLR2, RNF19A, POLDIP2, TGFB2, CCR3, TFF1, NOS2, CRK, IFNA13, PLB1, ADAM10, IDO1, GSTT1, AGER, AHR, HMGB1, MPO, IFNB1, IFNA1, IL1A, SMAD2, ITGAX, HLA-A, DEFB4B, IL9, GSTM1, ANXA1, JUN, CCR4, NRON, PLA2G2D, COX8A, LTB4R, NOX1, POTEM, COL26A1, IL17B, POTEKP, CHIA, AGO2, IL37, PRDX5, ADAMDEC1, CCR1, CD274, CLCN3, IL19, CLCN2, PLA2G2E, CD207, PGA3, KIF3A, SPDEF, NES, MIR4492, CD83, OCLN, COX5A, FHL5, SLC4A8, UBE3C, CPOX, SPAG11B, CLDN7, CLDN4, ACTG1, TRAF3IP2, CPB2, IL17RA, CCL27, C20orf181, SFTPA2, ACTG2, MIR663A, HPSE, SFTPA1, SCGB1C2, SPAG11A, PGA4, CLCA1, ACOT7, CPA3, MIR26B, CHIT1, CLC, BGN, CLEC4C, COL18A1, TRPV3, CASP3, VPS51, C6, SYVN1, KDM2B, ANGPT2, HAVCR2, ORAI1, BSG, BRAF, CXCR5, SLC5A8, ADAM33, SCGB3A1, BAX, MARVELD2, ARSA, IL17F, NOSTRIN, AREG, SCGB3A2, SCGB1C1, LRRK2, BIRC5, RBM45, DCBLD2, SLCO6A1, BPIFB2, ANGPT1, CPA4, ITLN1, MIR21, LYST, MIR19A, SIRT6, IL23A, ADRB2, TREM1, CD40LG, IL31, TNFSF8, SLC52A1, TNFRSF8, AP2A1, GSTK1, CD14, ANG, LTB4R2, CD1C, ACKR3, AICDA, ACTBL2, ALOX5, TRPV4, SERPINH1, AMT, CAT, IFNL1, EBAG9, IFNL2, TAC4, HOXD13, DECR1, CLDN1, NTF3, PGA5, PDGFB, PDE4D, PCNA, SERPINE1, PEBP1, P2RY2, NOTCH1, PIK3CD, NGF, MYD88, MUC6, GSK3B, MUC2, GSTP1, MSX2, GPR17, PLA2G2A, TRPA1, MOK, S100A9, S100A7, RNPEP, FOSB, RNASE2, REG1A, RAG1, PTPRC, PLAT, MTOR, CBLIF, GLRX, PTGDR, MAPK8, PLG, PLAU, MRC1, MNT, GUCA2A, HLA-DRB1, TNFRSF9, IL13RA2, HGF, IL9R, HLA-DQA2, HLA-DRA, IL4R, IL2, GUCA2B, HLA-G, CCN1, IGF1, IFRD1, FOXA2, HYAL1, TNC, HAS3, JUNB, JUND, KIT, MIF, CIITA, GZMB, SCGB2A2, SCGB2A1, MBL2, SMAD3, CD180, LUM, LTC4S, LGALS9, HAS2, LEPR, LEP, LCN2, FOXJ1, CCL3, CCL4, TLR3, EIF4EBP1, TNNC1, TNFRSF1B, TNFRSF1A, ELANE, TM7SF2, EMP1, TLR1, TFAP2A, NKX2-1, CTTN, THBD, TGM2, TGFB3, EPAS1, TFPI, TRAF6, DMBT1, TXN, VIM, NR1I2, CST1, IL1RL2, TNFSF13, TNFRSF25, CTNNB1, SLC4A4, SOCS1, TNFSF11, DCN, PLA2G10, IL1R2, XRCC1, WNT5A, TRPV1, TFF3, TERT, FGF7, SERPINA3, SLC9A2, SLC9A1, SIPA1, SFTPB, SELP, SELE, CXCL12, CCL25, TEAD1, FANCC, CCL22, CCL21, CCL20, FGF1, CCL13, CCL7, SLC9A3, SLC12A4, FABP1, SMARCA4, ERBB4, ERCC2, EREG, ADAM17, ERCC3, STATH, STAT5B, STAT5A, STAT2, STAT1, F2RL1, SPAM1, SOD3, SMN2, SMN1, A2M
-
Lactic Acidosis
Wikipedia
., from decreased blood flow) Type B B1: Underlying diseases (sometimes causing type A) B2: Medication or intoxication B3: Inborn error of metabolism Signs and symptoms [ edit ] Lactic acidosis is commonly found in people who are unwell, such as those with severe heart and/or lung disease, a severe infection with sepsis , the systemic inflammatory response syndrome due to another cause, severe physical trauma , or severe depletion of body fluids . [2] Symptoms in humans include all those of typical metabolic acidosis (nausea, vomiting, generalized muscle weakness, and laboured and deep breathing). [3] Causes [ edit ] The several different causes of lactic acidosis include: [ citation needed ] Genetic conditions Biotinidase deficiency , multiple carboxylase deficiency , or nongenetic deficiencies of biotin Diabetes mellitus and deafness Fructose 1,6-bisphosphatase deficiency Glucose-6-phosphatase deficiency GRACILE syndrome Mitochondrial encephalomyopathy, lactic acidosis, and stroke-like episodes Pyruvate dehydrogenase deficiency Pyruvate carboxylase deficiency Leigh syndrome Drugs Linezolid [4] Paracetamol/acetaminophen poisoning [5] Metformin : this risk is low (less than 10 cases for 100,000 patient years), but the risk of metformin-induced lactic acidosis (MALA) increases in certain situations where both the plasma levels of metformin are increased and lactate clearance is impaired. [6] The older related and now withdrawn drug phenformin carried a much higher risk of lactic acidosis. [7] Isoniazid toxicity Propofol Epinephrine Propylene glycol (D-lactic acidosis) Nucleoside reverse-transcriptase inhibitors Abacavir/dolutegravir/lamivudine [8] Emtricitabine/tenofovir [9] Potassium cyanide ( cyanide poisoning ) Fialuridine [10] Other Thiamine deficiency (especially during TPN) Impaired delivery of oxygen to cells in the tissues (e.g., from impaired blood flow (hypoperfusion)) Bleeding Polymyositis Ethanol toxicity Sepsis Shock Advanced liver disease Diabetic ketoacidosis Excessive exercise ( overtraining ) Regional hypoperfusion (e.g., bowel ischemia or marked cellulitis ) Cancers such as Non-Hodgkin's and Burkitt lymphomas Pheochromocytoma [2] Tumor lysis syndrome [11] D-lactic acidosis due to intestinal bacterial flora production in short gut syndrome Pathophysiology [ edit ] Glucose metabolism begins with glycolysis , in which the molecule is broken down into pyruvate in ten enzymatic steps. ... PMID 7565947 . ^ Darmon, Michael; Malak, Sandra; Guichard, Isabelle; Schlemmer, Benoit (July–September 2008). "Acute tumor lysis syndrome: a comprehensive review" . Revista Brasileira de Terapia Intensiva . 20 (3): 278–285. doi : 10.1590/S0103-507X2008000300011 .PDHA1, TRNL1, DNM1L, RRM2B, ND6, ATAD3A, PLAT, CYTB, ACAD9, MTO1, PDP1, POLG, BCS1L, PC, ISCU, COX1, ND1, ATP5F1E, SCO2, RMND1, TMEM70, COQ9, ND4, KARS1, FBXL4, TRMT10C, NDUFB11, LIPT1, MRPS14, NDUFS4, SLC25A3, EXOSC9, WARS2, SUCLA2, ELAC2, SURF1, TUFM, HADHA, IBA57, SLC37A4, DLD, EARS2, NDUFAF3, MICOS13, NDUFA11, NDUFAF6, NAXE, MLYCD, LARS2, FASTKD2, SFXN4, TANGO2, USP18, TPK1, ETHE1, FARS2, LIAS, NFU1, SLC25A42, NDUFS7, LIPT2, SLC25A13, LRPPRC, TSFM, COA6, BOLA3, PREPL, UQCC3, SUCLG1, PDHX, UQCRFS1, COQ2, MRPS34, COX20, SLC25A19, NDUFAF5, AARS2, LYRM4, COQ8A, TMEM126B, CAMKMT, AGK, TRMU, NUBPL, PUS1, FOXRED1, COA8, TK2, GTPBP3, SERAC1, COX14, LYRM7, ATPAF2, MPC1, NDUFAF2, LARS1, TIMMDC1, TACO1, NDUFAF1, MRPS7, YARS2, MRPS16, PNPLA8, TIMM50, NDUFAF4, PET100, TRNN, TRNS1, NDUFS2, NDUFS1, NDUFB10, NDUFB9, NDUFB3, NDUFA10, NDUFA6, GFER, NDUFA1, TRNW, TRNV, TRNT, TRNS2, TRNQ, NDUFS3, HSD17B10, HADHB, TRNK, TRNH, TRNF, ND5, ND3, HADH, ND2, COX3, COX2, TRNC, MPV17, G6PC, NDUFV1, CYC1, NDUFS6, SLC25A4, ALDOB, ATP5F1D, BCKDHA, SLC3A1, BCKDHB, CA5A, CHAT, COX6B1, SDHA, SCO1, COX8A, COX10, COX15, MIPEP, DBT, PPM1B, DGUOK, PHKG2, DLAT, PHKA2, PDHB, PCK1, PCCB, PCCA, TYMP, FH, NDUFV2, NDUFS8, HSPA5, MB, TFAM, TXNIP, VARS2, CA2, PTGS1, RPS6KA3, ABCB6, MGAM, SRSF2, SI, MEHMO, MAP2K7, SLC5A2, UQCRB, ALDH7A1, ATF4, AQP9, LINC01194, TTR, PTBP1, ARRDC4, MET, GSTZ1, IL10, IL6, MRPS22, SLC47A1, TNF, ZDHHC13, NDUFA5, RNPS1, UQCC2, UQCRQ, OPA1, FBP1, ECHS1, TRS-AGA2-3, ALB
-
Pulmonary Edema
Wikipedia
Acute lung injury and acute respiratory distress syndrome . [9] (ALI-ARDS) cover many of these causes, but they may include: Inhalation of hot or toxic gases Pulmonary contusion , i.e., high-energy trauma (e.g. vehicle accidents) Aspiration , e.g., gastric fluid Reexpansion, i.e. post large volume thoracocentesis , resolution of pneumothorax, post decortication, removal of endobronchial obstruction, effectively a form of negative pressure pulmonary oedema. ... Arteriovenous malformation Hantavirus pulmonary syndrome High altitude pulmonary edema (HAPE) [14] [15] Envenomation , such as with the venom of Atrax robustus [16] Signs and symptoms [ edit ] The most common symptom of pulmonary edema is difficulty breathing , but may include other symptoms such as coughing up blood (classically seen as pink, frothy sputum), excessive sweating , anxiety , and pale skin . ... Classification D ICD - 10 : J81 ICD - 9-CM : 514 518.4 506.1 MeSH : D011654 DiseasesDB : 11017 External resources MedlinePlus : 000140 eMedicine : article/157452 article/300813 , article/360932 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis v t e Disorders of volume state Volume contraction dehydration hypovolemia Hypervolemia Edema Anasarca Cerebral edema Pulmonary edema Angioedema Lymphedema Other Cause of fluid collection Exudate Transudate By site Hydrothorax Ascites Hydrosalpinx Hyperemia Authority control GND : 4134256-2 NDL : 00575969
-
Gingival Enlargement
Wikipedia
Younger Other specialties Endodontology Orthodontology Prosthodontology v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic diseaseKCNK4, AGA, AIMP2, CD96, ABCC9, GTF2IRD1, ADAMTS2, ADAMTS3, ZNHIT3, BAZ1B, CNTNAP1, USP9X, ZBTB16, ABCA5, WNT5A, CLIP2, STAT5B, STAT3, SOS1, SCN8A, SC5D, RMRP, RFC2, RET, EMC1, PIGN, ATP6V1B2, SLC17A5, SH3PXD2B, VPS13B, CCBE1, ANTXR2, PIGS, TBCK, FIP1L1, TBL1XR1, FAT4, NABP1, NXN, TBC1D24, HYMAI, FAM20C, SLC29A3, BCOR, FAM20A, TMCO1, RIN2, OSTM1, TBL2, REST, RARA, PRKAR1A, MGAT2, LIMK1, LBR, KCNJ6, KCNH1, INSR, IDUA, GUSB, GTF2I, GNAQ, GLB1, FZD2, FGFR2, FGF3, ELN, DVL3, DVL1, DHCR7, COL3A1, C1S, C1R, KIF1A, MAN2B1, MMP2, PML, MMP14, PLG, PLAGL1, PIGA, NUMA1, ROR2, NPM1, NFIX, TRNW, TRNS2, TRNS1, TRNQ, TRNL1, TRNH, TRNF, ND6, ND5, ND4, ND1, COX3, COX2, COX1, IRF2BP2
-
Contrast-Induced Nephropathy
Wikipedia
External links [ edit ] Classification D ICD - 10 : N99.0 ICD - 9-CM : 586 v t e Kidney disease Glomerular disease See Template:Glomerular disease Tubules Renal tubular acidosis proximal distal Acute tubular necrosis Genetic Fanconi syndrome Bartter syndrome Gitelman syndrome Liddle's syndrome Interstitium Interstitial nephritis Pyelonephritis Balkan endemic nephropathy Vascular Renal artery stenosis Renal ischemia Hypertensive nephropathy Renovascular hypertension Renal cortical necrosis General syndromes Nephritis Nephrosis Renal failure Acute renal failure Chronic kidney disease Uremia Other Analgesic nephropathy Renal osteodystrophy Nephroptosis Abderhalden–Kaufmann–Lignac syndrome Diabetes insipidus Nephrogenic Renal papilla Renal papillary necrosis Major calyx / pelvis Hydronephrosis Pyonephrosis Reflux nephropathy
-
Pharyngitis
Wikipedia
In one out of 400 untreated cases, Lemierre's syndrome occurs. [19] Diphtheria Diphtheria is a potentially life-threatening upper respiratory infection caused by Corynebacterium diphtheriae , which has been largely eradicated in developed nations since the introduction of childhood vaccination programs, but is still reported in the Third World and increasingly in some areas in Eastern Europe . ... Aspirin may be used in adults, but is not recommended in children due to the risk of Reye syndrome . [28] Steroids (such as dexamethasone ) may be useful for severe pharyngitis. [29] [8] Their general use, however, is poorly supported. [7] Viscous lidocaine relieves pain by numbing the mucous membranes. [30] Antibiotics are useful if a bacterial infection is the cause of the sore throat. [31] [32] For viral infections, antibiotics have no effect. ... External links [ edit ] Classification D ICD - 10 : J02 , J31.2 ICD - 9-CM : 462 , 472.1 MeSH : D010612 DiseasesDB : 24580 External resources MedlinePlus : 000655 eMedicine : emerg/419 Wikimedia Commons has media related to Pharyngitis . v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis v t e Common cold Viruses Adenovirus Coronavirus Enterovirus Rhinovirus Symptoms Cough Fatigue Fever Headache Loss of appetite Malaise Muscle aches Nasal congestion Rhinorrhea Sneezing Sore throat Weakness Complications Acute bronchitis Bronchiolitis Croup Otitis media Pharyngitis Pneumonia Sinusitis Strep throat Drugs Antiviral drugs Pleconaril (experimental)
-
Salivary Gland Tumour
Wikipedia
Atlanta: American Cancer Society. v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease v t e Tumors of lip , oral cavity and pharynx / head and neck cancer Oral cancer Salivary gland malignant epithelial tumors Acinic cell carcinoma Mucoepidermoid carcinoma Adenoid cystic carcinoma Salivary duct carcinoma Epithelial-myoepithelial carcinoma Polymorphous low-grade adenocarcinoma Hyalinizing clear cell carcinoma benign epithelial tumors Pleomorphic adenoma Warthin's tumor ungrouped: Oncocytoma Tongue Leukoplakia Rhabdomyoma Oropharynx External links [ edit ] Salivary gland cancer entry in the public domain NCI Dictionary of Cancer Terms Classification D ICD - 10 : C07 - C08 , D11 ICD - 9-CM : 142 , 210.2 MeSH : D012468 External resources MedlinePlus : 001040 This article incorporates public domain material from the U.S.DAPK1, CTNNB1, JAG1, GINS2, GAS2, GAS6, GUCY1A1, ISYNA1, SOX4, IGFBP2, ITGB4, KRT5, IRX4, KRT15, PCSK1N, ZIM2, MARCKS, RBFOX2, MLC1, SPEN, ESPL1, HOMER3, PDZK1, SERPINF1, PRKD1, TOP2A, PYGB, SOX11, ST3GAL4, DTL, SON, SLC24A3, EN1, EFHD1, BCL11A, AQP1, NETO2, CDH1, ASPM, VCAN, MARK2, CCND1, MIER2, WNT5B, FANCA, FAT1, STAG3L1, PLAG1, MLH1, MSH2, MSH6, ETV6, NTRK3, ERBB2, TP53, BCL2, WWOX, MUC17, STAT3, SOX10, C17orf97, TPM3, CKAP4, UVRAG, CXCR4, TP63, PDLIM7, STAG2, RASSF1, MUC3B, ACKR3, DDX43, KRT20, LEF1, PCNA, SDC1, HIF1A, GAGE5, GAGE4, GAGE1, FOLH1, FHIT, EWSR1, ENG, NQO1, CCR7, CDKN2A, CD6, BRAF, BAX, BAGE, ATF1, ALDH3A1, ALCAM, HGF, KRT7, CCL19, LEP, RPE65, PTGS2, PTEN, PPARG, PIK3CA, PGR, AKT1, NTRK1, NOTCH4, MYB, MUC6, MUC5AC, MUC3A, MDM2, MAGEA3, SMAD4, LGALS3, LINC01194
-
Geographic Tongue
Wikipedia
External links [ edit ] Classification D ICD - 10 : K14.1 ICD - 9-CM : 529.1 MeSH : D005929 External resources MedlinePlus : 001049 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic diseaseTNF, IFNG, IL6, IL1B, MMP9, CXCL9, CXCL10, HLA-C, CXCL8, ANXA1, SPRR2A, TLR1, VEGFA, CDK5R1, CXCL13, DCTN3, CHP1, CCL4, PHB2, LRIT1, IL36RN, HPGDS, IL23A, NUP37, SHCBP1, CDCA5, SLCO6A1, UBXN2B, GSTK1, CXCL11, MNAT1, CCL3, PRH2, CD8B, CRP, DYNC1H1, EGF, EPHA5, FCN2, GCHFR, CXCL1, HLA-A, HLA-B, HNRNPD, IL1A, IL10, IL12A, IL17A, MMP10, CCNH, PAM, PRH1, UPK3B
-
Pulmonary Alveolar Proteinosis
Wikipedia
This has been recognized in the settings of certain cancers (such as myeloid leukemia ), lung infections , or environmental exposure to dusts or chemicals , such as nickel. [3] Although the cause of PAP was not originally understood, a major breakthrough in the understanding of the cause of the disease came by the chance observation that mice bred for experimental study to lack a hematologic growth factor known as granulocyte-macrophage colony stimulating factor (GM-CSF) developed a pulmonary syndrome of abnormal surfactant accumulation resembling human PAP. [4] The implications of this finding are still being explored, but significant progress was reported in February 2007. Researchers in that report discussed the presence of anti- GM-CSF autoantibodies in patients with PAP, and duplicated that syndrome with the infusion of these autoantibodies into mice. [5] Familial or sporadic inactivating mutations in one of the two parental GATA2 genes produces an autosomal dominant disorder termed GATA2 deficiency . ... External links [ edit ] ORPHANET/ The portal for rare diseases and orphan drugs Classification D ICD - 10 : J84.01 ICD - 9-CM : 516.0 OMIM : 610910 MeSH : D011649 DiseasesDB : 29642 External resources MedlinePlus : 000114 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisCSF2RA, CSF2RB, SFTPC, CSF2, ABCA3, SFTPB, MARS1, NPC2, SLC7A7, PPARG, PARP9, CEL, SFTPD, SLC27A5, IL5, BACH2, SLA2, IL3, ABCG1, IL10, SOAT1, ABCA1, VDR, SLC7A6, FCGR2C, IL22, IL17F, PLF, SFTPA1, FARSB, IL17A, OAS1, MUC1, ABL1, ADA, CD36, CD40LG, CEACAM5, CHI3L1, CSF1, CYP27A1, DMBT1, ENO2, FCGR2A, FCGR2B, IFNG, IL1A, IL1B, IL6, ITGAX, CCR2