-
Lassa Fever
Wikipedia
Viral disease spread by a type of mouse Lassa fever Other names Lassa hemorrhagic fever Community education material for Lassa fever Specialty Infectious disease Symptoms Fever , headaches , bleeding [1] Complications Deafness [1] Usual onset 1–3 weeks following exposure [1] Causes Lassa virus [1] Risk factors Exposure to rodents in West Africa [1] Diagnostic method Laboratory testing [1] Differential diagnosis Ebola , malaria , typhoid fever [1] Treatment Supportive [1] Prognosis 1% risk of death [1] Frequency 400,000 cases per year [2] Deaths 5,000 deaths per year [2] Lassa fever , also known as Lassa hemorrhagic fever ( LHF ), is a type of viral hemorrhagic fever caused by the Lassa virus . [1] Many of those infected by the virus do not develop symptoms. [1] When symptoms occur they typically include fever , weakness, headaches, vomiting , and muscle pains . [1] Less commonly there may be bleeding from the mouth or gastrointestinal tract . [1] The risk of death once infected is about one percent and frequently occurs within two weeks of the onset of symptoms. [1] Of those who survive, about a quarter have hearing loss , which improves within three months in about half of these cases. [1] The disease is usually initially spread to people via contact with the urine or feces of an infected multimammate mouse . [1] Spread can then occur via direct contact between people. [1] Diagnosis based on symptoms is difficult. [1] Confirmation is by laboratory testing to detect the virus's RNA , antibodies for the virus, or the virus itself in cell culture . [1] Other conditions that may present similarly include Ebola , malaria , typhoid fever , and yellow fever . [1] The Lassa virus is a member of the Arenaviridae family of viruses . [1] There is no vaccine . [3] Prevention requires isolating those who are infected and decreasing contact with the mice. [1] Other efforts to control the spread of disease include having a cat to hunt vermin , and storing food in sealed containers. [1] Treatment is directed at addressing dehydration and improving symptoms. [1] The antiviral medication ribavirin has been recommended, [1] but evidence to support its use is weak. [4] Descriptions of the disease date from the 1950s. [1] The virus was first described in 1969 from a case in the town of Lassa, in Borno State , Nigeria . [1] [5] Lassa fever is relatively common in West Africa including the countries of Nigeria , Liberia , Sierra Leone , Guinea , and Ghana . [1] [2] There are about 300,000 to 500,000 cases which result in 5,000 deaths a year. [2] [6] Contents 1 Signs and symptoms 2 Cause 2.1 Virology 2.2 Spread 3 Diagnosis 4 Prevention 4.1 Vaccine 5 Treatment 5.1 Medications 5.2 Pregnancy 6 Prognosis 7 Epidemiology 7.1 Geography 7.2 Nigeria 7.2.1 2018 outbreak 7.2.2 2019 outbreak 7.2.3 2020 outbreak 8 Liberia 9 History 10 Research 11 References 12 External links Signs and symptoms [ edit ] Onset of symptoms is typically 7 to 21 days after exposure. [7] In 80% of those who are infected few or no symptoms occur. [7] [8] These mild symptoms may include fever, tiredness, weakness, and headache. [7] In 20% of people more severe symptoms such as bleeding gums, breathing problems, vomiting, chest pain, or dangerously low blood pressure may occur. [7] Long term complications may include hearing loss . [7] In those who are pregnant , miscarriage may occur in 95%. [7] Lassa fever can be difficult to distinguish clinically from other viral hemorrhagic fevers, such as Ebola virus disease . [1] A combination of pharyngitis , pain behind the sternum , presence of excess protein in the urine and fever can indicate Lassa fever with higher specificity. [9] In cases in which death occurs, this typically occurs within 14 days of onset. [7] About 1% of all Lassa virus infections result in death. [7] Approximately 15%-20% of those who have required hospitalization for Lassa fever die. [7] The risk of death is greater in those who are pregnant. [7] A "Swollen baby syndrome" may occur in newborns, infants and toddlers with pitting edema , abdominal distension and bleeding. [10] Cause [ edit ] Virology [ edit ] A transmission electron micrograph (TEM) of a number of Lassa virus virions adjacent to some cell debris. ... They therefore list it for urgent research and development to develop new diagnostic tests, vaccines, and medicines. [41] [42] In 2007, SIGA Technologies , studied a medication in guinea pig with Lassa fever. [43] Work on a vaccine is continuing, with multiple approaches showing positive results in animal trials. [44] In addition to animal models, Organ-on-a-chip models have been developed to study Lassa hemorrhagic syndrome. These microchips allow for high throughput modelling of hemorrhagic syndrome and candidate drug screening. ... Retrieved 11 September 2017 . ^ Lassa hemorrhagic shock syndrome‐on‐a‐chip External links [ edit ] Viruses portal Echioya, Deborah U.; Hass, Meike; Olshlager, Stephan; Becker-Ziaja, Beate; Chukwu, Christian O. ... Classification D ICD - 10 : A96.2 ICD - 9-CM : 078.8 MeSH : D007835 DiseasesDB : 7272 v t e Zoonotic viral diseases (A80–B34, 042–079 ) Arthropod -borne Mosquito -borne Bunyavirales Arbovirus encephalitides : La Crosse encephalitis LACV Batai virus BATV Bwamba Fever BWAV California encephalitis CEV Jamestown Canyon encephalitis Tete virus Tahyna virus TAHV Viral hemorrhagic fevers : Rift Valley fever RVFV Bunyamwera fever BUNV Ngari virus NRIV Flaviviridae Arbovirus encephalitides : Japanese encephalitis JEV Australian encephalitis MVEV KUNV Saint Louis encephalitis SLEV Usutu virus West Nile fever WNV Viral hemorrhagic fevers : Dengue fever DENV-1-4 Yellow fever YFV Zika fever Zika virus Togaviridae Arbovirus encephalitides : Eastern equine encephalomyelitis EEEV Western equine encephalomyelitis WEEV Venezuelan equine encephalomyelitis VEEV Chikungunya CHIKV O'nyong'nyong fever ONNV Pogosta disease Sindbis virus Ross River fever RRV Semliki Forest virus Reoviridae Banna virus encephalitis Tick -borne Bunyavirales Viral hemorrhagic fevers : Bhanja virus Crimean–Congo hemorrhagic fever (CCHFV) Heartland virus Severe fever with thrombocytopenia syndrome ( Huaiyangshan banyangvirus ) Tete virus Flaviviridae Arbovirus encephalitides : Tick-borne encephalitis TBEV Powassan encephalitis POWV Viral hemorrhagic fevers : Omsk hemorrhagic fever OHFV Kyasanur Forest disease KFDV AHFV Langat virus LGTV Orthomyxoviridae Bourbon virus Reoviridae Colorado tick fever CTFV Kemerovo tickborne viral fever Sandfly -borne Bunyavirales Adria virus (ADRV) Oropouche fever Oropouche virus Pappataci fever Toscana virus Sandfly fever Naples virus Rhabdoviridae Chandipura virus Mammal -borne Rodent -borne Arenaviridae Viral hemorrhagic fevers : Lassa fever LASV Venezuelan hemorrhagic fever GTOV Argentine hemorrhagic fever JUNV Brazilian hemorrhagic fever SABV Bolivian hemorrhagic fever MACV LUJV CHPV Bunyavirales Hemorrhagic fever with renal syndrome DOBV HTNV PUUV SEOV AMRV THAIV Hantavirus pulmonary syndrome ANDV SNV Herpesviridae Murid gammaherpesvirus 4 Bat -borne Filoviridae BDBV SUDV TAFV Marburg virus disease MARV RAVV Rhabdoviridae Rabies ABLV MOKV DUVV LBV CHPV Paramyxoviridae Henipavirus encephalitis HeV NiV Coronaviridae SARS-related coronavirus SARS-CoV MERS-CoV SARS-CoV-2 Primate -borne Herpesviridae Macacine alphaherpesvirus 1 Retroviridae Simian foamy virus HTLV-1 HTLV-2 Poxviridae Tanapox Yaba monkey tumor virus Multiple vectors Rhabdoviridae Rabies RABV Mokola virus Poxviridae Monkeypox
-
Pellagra
Wikipedia
Alterations in protein metabolism may also produce pellagra-like symptoms. An example is carcinoid syndrome , a disease in which neuroendocrine tumors along the GI tract use tryptophan as the source for serotonin production, which limits the available tryptophan for niacin synthesis. In normal patients, only one percent of dietary tryptophan is converted to serotonin; however, in patients with carcinoid syndrome, this value may increase to 70%. Carcinoid syndrome thus may produce niacin deficiency and clinical manifestations of pellagra. ... ISSN 0813-9008 . ^ Frostig J. P., Spies T. D. "The initial syndrome of pellagra and associated deficiency diseases". ... "Studies of tryptophan and albumin metabolism in a patient with carcinoid syndrome, pellagra, and hypoproteinemia" .
-
Sleep Apnea
Wikipedia
Sleep apnea awareness day is April 18 in recognition of Colin Sullivan. [94] See also [ edit ] Medicine portal Congenital central hypoventilation syndrome Modes of mechanical ventilation Periodic breathing Obesity hypoventilation syndrome Respiratory disturbance index (RDI) Upper airway resistance syndrome References [ edit ] ^ a b c d e f g h i j k l m n o p "Sleep Apnea: What Is Sleep Apnea?" ... "Obstructive sleep apnea/hypopnea syndrome". Panminerva Medica . 55 (2): 191–5. ... PMID 15989309 . ^ Morgenthaler TI, Kagramanov V, Hanak V, Decker PA (September 2006). "Complex sleep apnea syndrome: is it a unique clinical syndrome?" ... Sleep Apnea – The Phantom of the Night: Overcome Sleep Apnea Syndrome and Win Your Hidden Struggle to Breathe, Sleep, and Live . ... "[The effect of nocturnal oxygen therapy in patients with sleep apnea syndrome and chronic airflow limitation]".P4HTM, BCHE, S100B, AHDC1, GSN, SYT1, NDN, SRPX2, NPAP1, IPW, LAMB2, LTBP3, RAI1, MAP6, MKRN3-AS1, GNE, AIP, NEFH, GABRG2, HERC2, PRPH, PTCH1, PEX11B, COLQ, USP7, RPS6KA3, MKRN3, TWIST1, TSPYL1, TCF4, SOD1, GRIN2A, CTNNB1, PWAR1, SLC52A2, WDR26, GPR101, COL4A1, COL3A1, SLC52A3, RUNX2, CENPJ, ASXL1, BRAF, FLCN, SNORD115-1, PWRN1, SNORD116-1, GNPTAB, SNRPN, LARP7, FGFR2, DCTN1, MAGEL2, FGFR3, APOE, LEP, HCRT, EPO, FMR1, ACE, CD274, MTPAP, NANS, TUSC2, ASAP1, ASAP2, PHOX2B, PAPOLA, MRPS30, PDAP1, ACP3, SLC2A1, TSPAN31, REG3A, IL6, REN, PTGS2, SPG7, CYP1A2, CSH2, CST3, FTO, LRRC4, CXADR, ENOSF1, CYP2J2, CSH1, DES, CFD, DMD, ZBTB7A, GCG, GLP1R, EHMT1, ERCC8, PPP1R2C, APP, PTLS, AMPD1, APOA2, CXADRP1, NPS, MIR452, HCCAT5, CRP, ARR3, CASR, C1orf52, CD34, NLRP3, HMOX2, REM1, PART1, HSPA9, S100A8, ADIPOQ, PMP22, PRKAR1A, PER3, PSG5, PTEN, ZFP36, SACS, VWF, TRPV1, VEGFA, VCL, SLC6A4, AGT, RECQL4, ADAMTS3, ADAMTS2, CLOCK, NR1I3, NR3C2, MECP2, TRIM13, MXD1, CYSLTR1, CD3EAP, LGALS3, LEPR, IGF1, RRS1, IDS, CDKL5, ZGLP1
-
Thrombosis
Wikipedia
Contents 1 Signs and symptoms 1.1 Venous thrombosis 1.1.1 Deep vein thrombosis 1.1.2 Paget-Schroetter disease 1.1.3 Budd-Chiari syndrome 1.1.4 Portal vein thrombosis 1.1.5 Renal vein thrombosis 1.1.6 Cerebral venous sinus thrombosis 1.1.7 Jugular vein thrombosis 1.1.8 Cavernous sinus thrombosis 1.2 Arterial thrombosis 1.2.1 Stroke 1.2.2 Myocardial infarction 1.3 Limb ischemia 1.3.1 Other sites 2 Causes 3 Mechanism 3.1 Pathogenesis 3.1.1 Hypercoagulability 3.1.2 Endothelial cell injury 3.1.3 Disturbed blood flow 3.2 Pathophysiology 3.2.1 Natural history 3.2.2 Embolization 4 Prevention 5 Treatment 5.1 Anticoagulation 5.2 Thrombolysis 5.3 Surgery 5.4 Endovascular treatment 5.5 Antiplatelet agents 5.6 Targeting ischemia/reperfusion injury 6 See also 7 References 7.1 Bibliography 8 External links Signs and symptoms [ edit ] Thrombosis is generally defined by the type of blood vessel affected (arterial or venous thrombosis) and the precise location of the blood vessel or the organ supplied by it. ... Men are affected more than women. [ citation needed ] Budd-Chiari syndrome [ edit ] Main article: Budd-Chiari syndrome Budd-Chiari syndrome is the blockage of a hepatic vein or of the hepatic part of the inferior vena cava . ... Some people have a higher risk of developing thrombosis and its possible development into thromboembolism. [8] Some of these risk factors are related to inflammation . " Virchow's triad " has been suggested to describe the three factors necessary for the formation of thrombosis: stasis of blood, vessel wall injury, and altered blood coagulation. [9] [10] Some risk factors predispose for venous thrombosis while others increase the risk of arterial thrombosis. [ citation needed ] Risk factors for thrombosis Factor Notes References Previous episodes of thrombosis [9] Vasoconstriction [11] Slow or turbulent blood flow slow flow is modifiable with exercise [11] Stroke [12] Heart failure [12] Sedentary life style modifiable [11] Plaster cast transient [12] Dehydration modifiable [11] Acute respiratory failure [12] Dysrhythmias [11] Shock [11] Obesity modifiable [8] [12] [13] [14] [15] Pregnancy and the post-partum period [8] [14] [15] Varicose veins [12] [14] Surgery [8] [14] Trauma [8] [12] [14] Estrogen-based oral contraceptive discontinuation reduces risk [8] [11] [14] Hormone replacement therapy discontinuation reduces risk [8] Ovarian hyper-stimulation therapy to treat infertility [8] Compression of a vein or artery by abnormality, tumor, hematoma [8] Long surgeries [13] Pacing wires [14] [16] Local vein damage, incompetent valves [11] [14] [15] Central venous catheters [14] Dialysis catheters [14] Repetitive motion injury [14] Immobility modifiable risk [12] [14] Spinal cord injury [14] Age [8] [11] [12] [14] Cancers [14] Sepsis [14] Polycythemia [14] Protein C and/or S deficiency congenital; associated with Warfarin necrosis [14] Antiphospholipid antibody syndrome altered coagulation [14] Factor V Leiden defect altered coagulation [14] Prothrombin G20210A defect altered coagulation [14] Hyperhomocysteinemia altered coagulation [14] Elevated factors II , VIII , IX , XI altered coagulation [14] Antithrombin III deficiency altered coagulation [14] Falls and hip fracture related to immobility [17] Selective estrogen-receptor modulators [8] Erythropoiesis -stimulating agents [8] Acute medical illness [8] Inflammatory bowel disease [8] Nephrotic syndrome [8] Myeloproliferative disorders [8] Paroxysmal nocturnal hemoglobinnuria [8] Thrombophilias [8] Post-menopausal hormone replacement therapy discontinuation reduces risk [8] Right heart failure [15] Venous inflammation/phlebitis when a thrombus forms, it is thrombophlebitis [11] Ambient air pollution thought to be related to inflammation [18] [19] [20] Mechanism [ edit ] Pathogenesis [ edit ] Main article: Virchow's triad The main causes of thrombosis are given in Virchow's triad which lists thrombophilia , endothelial cell injury, and disturbed blood flow . ... Also, atrial fibrillation , causes stagnant blood in the left atrium (LA), or left atrial appendage (LAA), and can lead to a thromboembolism. [22] Cancers or malignancies such as leukemia may cause increased risk of thrombosis by possible activation of the coagulation system by cancer cells or secretion of procoagulant substances ( paraneoplastic syndrome ), by external compression on a blood vessel when a solid tumor is present, or (more rarely) extension into the vasculature (for example, renal cell cancers extending into the renal veins). [22] Also, treatments for cancer (radiation, chemotherapy) often cause additional hypercoagulability. [22] There are scores that correlate different aspects of patient data (comorbidities, vital signs, and others) to risk of thrombosis, such as the POMPE-C, which stratifies risk of mortality due to pulmonary embolism in patients with cancer, who typically have higher rates of thrombosis. [26] Also, there are several predictive scores for thromboembolic events, such as Padua, [27] Khorana, [28] [29] and ThroLy score. [30] Pathophysiology [ edit ] Natural history [ edit ] Fibrinolysis is the physiological breakdown of blood clots by enzymes such as plasmin . ... Thrombosis at Curlie v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension v t e Disorders of bleeding and clotting Coagulation · coagulopathy · Bleeding diathesis Clotting By cause Clotting factors Antithrombin III deficiency Protein C deficiency Activated protein C resistance Protein S deficiency Factor V Leiden Prothrombin G20210A Platelets Sticky platelet syndrome Thrombocytosis Essential thrombocythemia DIC Purpura fulminans Antiphospholipid syndrome Clots Thrombophilia Thrombus Thrombosis Virchow's triad Trousseau sign of malignancy By site Deep vein thrombosis Bancroft's sign Homans sign Lisker's sign Louvel's sign Lowenberg's sign Peabody's sign Pratt's sign Rose's sign Pulmonary embolism Renal vein thrombosis Bleeding By cause Thrombocytopenia Thrombocytopenic purpura : ITP Evans syndrome TM TTP Upshaw–Schulman syndrome Heparin-induced thrombocytopenia May–Hegglin anomaly Platelet function adhesion Bernard–Soulier syndrome aggregation Glanzmann's thrombasthenia platelet storage pool deficiency Hermansky–Pudlak syndrome Gray platelet syndrome Clotting factor Hemophilia A/VIII B/IX C/XI von Willebrand disease Hypoprothrombinemia/II Factor VII deficiency Factor X deficiency Factor XII deficiency Factor XIII deficiency Dysfibrinogenemia Congenital afibrinogenemia Signs and symptoms Bleeding Bruise Hematoma Petechia Purpura Nonthrombocytopenic purpura By site head Epistaxis Hemoptysis Intracranial hemorrhage Hyphema Subconjunctival hemorrhage torso Hemothorax Hemopericardium Pulmonary hematoma abdomen Gastrointestinal bleeding Hemobilia Hemoperitoneum Hematocele Hematosalpinx joint Hemarthrosis Authority control GND : 4059963-2 NDL : 00565646F2, SERPINC1, P2RY12, PLAU, FGA, F5, F3, PROC, VWF, SERPINE1, PROCR, SELP, PLAT, ADAMTS13, PROS1, TNF, PF4, FCGR2A, PTGS2, THBD, VHL, CRP, MERTK, GAS6, GP1BA, PDE3A, P2RY1, AGT, PTGER3, PODXL, HMOX1, TYRO3, KLF4, SIRT1, VKORC1, KLKB1, MAS1, HGF, FUT4, BDKRB2, CD2, CYP2C19, CYP3A5, EPO, F9, F10, FLT3, BCRP3, GUCY1A1, APOH, CD40LG, TBXAS1, C5AR1, PIK3CB, ACE2, JAK2, MTHFR, NOS3, ITGA2, ITGB3, CPB2, VASP, TFPI, F8, P2RX1, MPL, TNFSF14, SCUBE2, CD177, GP6, C1QBP, C4B, IL1B, SCUBE1, TUBB1, IL6, KLF2, MRVI1, CANT1, LPA, DCN, PLA2G6, F11, LEPR, LEP, FGG, PECAM1, FGB, F13A1, PTGS1, ITGA2B, ICAM4, EGR1, SLC19A1, TBXA2R, ANXA5, CD55, ENG
-
Venous Ulcer
Wikipedia
Additional causes include neutrophilic skin conditions such as pyoderma gangrenosum or Sweet's syndrome ; vasculitic processes such as cryoglobulinemia ; calciphylaxis (often seen in people with end-stage kidney disease but may also occur with medications such as warfarin ); cancers such as squamous cell carcinoma ( Marjolin's ulcer ) or myelodysplastic syndrome ; neuropathy (e.g., diabetic peripheral neuropathy ); or atypical infections such as nocardiosis , sporotrichosis , or mycobacterial infections. ... External links [ edit ] Classification D ICD - 10 : I83.0 , I83.2 , L97 ICD - 9-CM : 454.0 MeSH : D014647 DiseasesDB : 29114 External resources MedlinePlus : 000834 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension
-
Panic Attack
Wikipedia
Hyperventilation syndrome can cause respiratory alkalosis and hypocapnia . This syndrome often involves prominent mouth breathing as well. ... "International Expert Consensus Document on Takotsubo Syndrome (Part I): Clinical Characteristics, Diagnostic Criteria, and Pathophysiology" . ... CS1 maint: archived copy as title ( link ) [ full citation needed ] ^ "Hyperventilation Syndrome]" . 28 November 2016. Archived from the original on 13 July 2017 . ... These patients can often be cared for with low-flow oxygen and lots of reassurance ^ Hyperventilation Syndrome – Can I treat hyperventilation syndrome by breathing into a paper bag?ADORA2A, ADRA2A, CCKBR, COMT, INS, DNAJC6, SDHC, SDHD, SNCA, TP53, UCHL1, VHL, SLC25A11, SGCE, KIF1B, PARK7, RET, SPART, CIZ1, HTRA2, VPS13C, SDHAF2, TMEM127, PINK1, KCTD17, LRRK2, SDHA, SDHB, SLC25A42, PODXL, PRKN, MDH2, DLST, DRD2, MAX, TOR1A, FH, CCK, PTK7, HTR1A, KRT7, MAOA, TAL1, SCLY, CYP2D6, COPD, TPH2, AGT, DST, DUSP26, SLC6A1, ACE, DBI, IGFBP2, SLC6A4, SNAP25, LEP, HCRTR1, GLO1
-
Atrial Fibrillation
Wikipedia
Sepsis also increases the risk of developing new-onset atrial fibrillation. [26] [27] Disorders of breathing during sleep, such as obstructive sleep apnea (OSA), are also associated with AF. [28] Obesity is a risk factor for AF. [29] Hyperthyroidism and subclinical hyperthyroidism are associated with AF development. [30] Caffeine consumption does not appear to be associated with AF; [15] [31] excessive alcohol consumption (" binge drinking " or " holiday heart syndrome ") is linked to AF. [32] Low-to-moderate alcohol consumption also appears to be associated with an increased risk of developing atrial fibrillation, although the increase in risk associated with drinking less than two drinks daily appears to be small. [32] [33] Tobacco smoking and secondhand tobacco smoke exposure are associated with an increased risk of developing atrial fibrillation. [7] [34] Long-term endurance exercise that far exceeds the recommended amount of exercise (e.g., long-distance cycling or marathon running) appears to be associated with a modest increase in the risk of atrial fibrillation in middle-aged and elderly people. [19] [35] [36] Genetics [ edit ] A family history of AF may increase the risk of AF. A study of more than 2,200 people found an increased risk factor for AF of 1.85 for those that had at least one parent with AF. [37] [38] [39] Various genetic mutations may be responsible. [40] [41] Four types of genetic disorder are associated with atrial fibrillation: [42] Familial AF as a monogenic disease Familial AF presenting in the setting of another inherited cardiac disease (hypertrophic cardiomyopathy, dilated cardiomyopathy , familial amyloidosis ) Inherited arrhythmic syndromes (congenital long QT syndrome , short QT syndrome , Brugada syndrome ) Non-familial AF associated with genetic backgrounds (polymorphism in the ACE gene) that may predispose to atrial fibrillation Family history in a first degree relative is associated with a 40% increase in risk of AF. ... All atrial remodeling is related to heterogeneous conduction and the formation of re-entrant electric conduction from the pulmonary veins . [43] [54] Other diseases [ edit ] There is a relationship between risk factors such as obesity and hypertension, with the appearance of diseases such as diabetes mellitus and sleep apnea-hypopnea syndrome, specifically, obstructive sleep apnea (OSA). ... Fibrosis is not limited to the muscle mass of the atria and may occur in the sinus node (SA node) and atrioventricular node (AV node), correlating with sick sinus syndrome . Prolonged episodes of atrial fibrillation have been shown to correlate with prolongation of the sinus node recovery time; [21] this suggests that dysfunction of the SA node is progressive with prolonged episodes of atrial fibrillation.KCNH2, KCNN3, CAV1, GJA5, SCN5A, PITX2, ZFHX3, TBX5, HCN4, SCN10A, KCNJ2, NKX2-5, PLN, NEURL1, KCNJ5, TTN, MYH7, SIRT1, SYNE2, CAND2, SOX5, HAND2, PRRX1, AOPEP, TNFSF12, ERBB4, NEBL, RBM20, KCND3, CASQ2, WNT8A, SMAD7, SYNPO2L, ATXN1, RPL3L, GCOM1, RPS2, AGBL4, BEST3, SPATS2L, ARHGAP10, KDM1B, SLC35F1, LRIG1, IGF1R, SLIT3, CDKN1A, CDK6, ARMH3, SLC27A6, ESR2, MYO18B, DGKB, EPHA3, MAPT, NUCKS1, DNAH10, TEX41, GNB4, ZNF462, MYH6, FBRSL1, ACE, PAK2, PTK2, XXYLT1, LRMDA, CASZ1, KCNN2, PKP2, KIF3C, REEP3, PPP2R3A, SLC9B1, MEX3C, TUBA8, FBXO32, LINC01426, CYTH1, UBE4B, MIR1-1HG, VWF, HIP1R, HERC1, WNT3, MYOCD, COG5, TTN-AS1, PHLDB2, PPFIA4, ASAH1, CUL4A, DPF3, LHX3, XPO7, SCMH1, GTF2I, SH3PXD2A, USP3, ZPBP2, USP34, SUN1, THRB, AKAP6, CAMK2D, CEP68, CREB5, GOSR2, GYPC, NAV2, FRMD4B, SSPN, EDN1, KCNA5, NOS3, NPPB, CYP2C19, KCNE2, GATA4, MYOZ1, KCNE5, CAV2, SELE, HTR4, KCNJ8, ABCC9, HSF2, LINC00477, MIR6500, CFL2, OPN1SW, WIPF1, FGF5, PHLDA1, SNRNP27, IRF2BPL, LRRC10, C1orf185, GJA1, MYOT, SGCA, CALU, UST, REEP1, LINC01142, MYPN, MIR30B, SORL1, SOX15, WDR1, MBD5, ARNT2, XPO1, GOPC, DES, HSPG2, PSMB7, NACA, MYO1C, NR3C1, CGA, NPPA, KCNQ1, TFPI, LMNA, IL6R, CACNA1C, ANK2, SMAD3, PPARG, NUP155, MTHFR, GATA5, FAF1, CACNB2, TNFSF12-TNFSF13, CDKN2B-AS1, SNTA1, PRKAG2, IL6, KCNE1, ALPK1, CCDC92, ITPK1, PANCR, TMEM43, LGALS3, RYR2, BSCL2, TCF7L2, TGFB1, SIK3, TNF, TAB2, XK, POLG2, SLC30A3, AGPAT2, ALDH1A2, ZPR1, BAZ1B, FADS2, GDF15, CERT1, PKD2L2, REN, GRHL1, TWNK, LIPC, FADS1, GMCL1, SLC39A8, ABHD17C, SUGP1, CRAMP1, PEX26, RRM2B, ZCCHC8, MAML3, SEMA5B, PLCG1, POLG, SLC25A26, TNNI3K, POLK, FTO, ATP2B1, LINC02269, MYZAP, DCBLD1, SLC25A4, ALB, ANXA4, CEP85L, GCKR, LINC00964, LINC02245, FOS, CELSR2, AGT, HBEGF, DTNA, CAVIN1, LINC01629, CRP, DINOL, PLCXD2, LINC01681, LIPC-AS1, CACNA2D1, LINC02576, DNAH10OS, F10, KCNK3, CYP11B2, CYP2C9, MMP9, VKORC1, F3, TNNI3, SERPINA5, MIR21, TTR, IL1B, CAD, P2RY12, MMP2, SERPINE1, COPD, NR3C2, SMAD2, F2, FSD1, ACE2, DPP4, CREM, ADRB1, AGTR1, FSD1L, ANGPT2, NLRP3, CCL2, TIMP2, TIMP1, IGF1, F2R, FGF23, SELP, VPS51, CCN2, ATP2A2, C20orf181, CST3, KCNE3, MAPK3, THBD, MIR328, ADIPOQ, MIR106B, MYL4, SCN4B, SCN2B, STAT3, DLD, DECR1, PCLAF, SLN, ABCB6, ABCB1, NOC2L, SCN1B, SCN3B, ITGB2, IL10, PCSK9, LAD1, TCFL5, NR1I2, GATA6, BCL2, PLA2G15, NGF, SLC52A2, CD40LG, TNFRSF11B, IL1A, ACSS2, CETP, ACTN2, CYP3A4, MIR150, CAAP1, COL1A1, MIR29A, NLRP6, VEGFA, RAC1, MYBPC3, VCAM1, ACCS, APLNR, CUX2, SIGMAR1, PWAR1, LPA, TRPC3, APLN, CYP4F2, CHI3L1, CXCL12, PRKRA, LYST, BAX, AVP, C1QL1, CALR, WDHD1, TSPAN31, TIMP4, PSMB8, PTH, CALCR, NOX4, ADAMTS13, MINK1, CP, RBBP6, S100B, RNASE1, ROS1, MIR133B, COL4A2, FAS-AS1, SLC30A1, MIR208B, SHBG, MIR499A, SMUG1, PGR-AS1, CD14, CAV3, TAT, ADM, AMACR, CASP8, STK11, KAT2B, TGFBR1, STAR, TH, KCNE4, ST2, SPRY1, CD44, SOD1, ADH1B, RAPGEF3, BDNF, SLC6A3, ACVR1B, SLC5A2, APOE, MIR483, SHOX2, MMRN1, PART1, HIF1A, CRH, PLG, PLAT, MIR155, TRPM7, MIR146A, ZNF415, RETN, OAT, JPH2, NHS, MSR1, GAS5, MAP6, ADGRE4P, KNG1, KCNK1, FCGR3A, FCGR3B, FN1, ITGA2B, INSRR, IL18, CXCL8, GCG, IDE, GRK5, HSPA8, HSPA4, HMOX1, HMGB1, NANS, CHAF1A, MIR223, MAPK9, MIR27B, AHSP, MIR26B, POMC, PON1, HAVCR1, MIR34A, MIR3149, PPARGC1A, MRPS30, FLVCR1, VOPP1, ARID3B, HOTAIRM1, JTB, MFRP, ATG7, TMX2-CTNND1, CAP2, SESN2, JAML, MIR4279, FASTK, UTS2, PAPOLA, POTEKP, EHMT1, SLCO1B3, MIR17HG, IL27, FOLH1B, CRYGEP, WWP1, TRAP, SLC35G1, KCNQ1OT1, LINC00472, PPM1K, STIP1, NPPA-AS1, PRSS21, ECRG4, SPATC1L, RMC1, HOPX, PCAT1, KCNK17, G3BP1, CSAD, GGTLC1, KCNK7, LOC102724197, MIR31, CACNA2D4, NKX2-6, SLCO6A1, MUC16, PRRT2, CERNA3, SIRT1-AS, C1QTNF5, GJC1, KCNK9, TRIM69, EMSLR, TRPM6, NPY4R2, CCDC141, GDF7, ANAPC10, AKR1A1, EBPL, KCNIP2, APBB3, BET1, PDZK1IP1, TICAM1, SESN3, KRT90P, KCNIP1, ATP6AP2, WNT3A, SIRPA, H19, ZGLP1, FILIP1L, HEY2, IL17D, MAP3K7CL, MIR132, SMIM10L2B, PELI1, MIR126, SALL4, GDE1, SLC24A3, LY96, LINC00273, CD2AP, MIR125A, MIR122, MIR10A, NNT, GGTLC5P, ARIH1, SNORD44, KCNK13, MTPAP, TRIM72, MIR206, MIR15B, MIR342, MIR146B, KRT20, FGF21, PRPF31, SH2B1, MIR142, CNTN5, CTNNBL1, KCNQ5, MIR137, POTEM, MIR133A2, MIR106A, NPTXR, MIR20A, MIRLET7B, ASAP1, NIBAN2, AGXT2, TSPAN33, ZHX2, RGPD2, C1QTNF9, PSS, COG2, TUSC2, PDAP1, ACOT7, DESI1, MMP28, TLX1NB, SGSM3, PHB2, GGTLC4P, GSTK1, ISYNA1, GGTLC3, MIR590, MIR92B, CASC15, IL37, PRM3, HAGLR, SNORD118, WWC1, GPD1L, SMIM10L2A, SIL1, GGT2, GREM2, CCR2, SLC22A25, ENHO, ACTBL2, SERPINA3, HDAC5, FGB, FGF13, FGFR4, VEGFD, FKBP1A, FKBP1AP1, FKBP1AP2, FKBP1AP3, FKBP1AP4, FLOT2, FOLH1, GAP43, GC, GCH1, GGCX, GGT1, CBLIF, GJA4, FGF2, FBN1, ELK3, FANCF, EMD, MARK2, ENO2, ENPEP, EPHX2, EPO, ERCC6, ETV1, EZH2, F2RL1, F5, F7, F8, FABP4, FABP3, FANCC, PTK2B, GLA, GLP1R, GLS, GNB3, IFNG, IFNGR2, IGFBP3, IGFBP7, CCN1, IL1RN, IL9, CXCR2, IL16, FOXK2, INCENP, INPP5D, INPPL1, ITGA2, ITGA5, ITGAM, ITPR1, IFNB1, ICAM1, TNC, HLA-C, GNRHR, GPT, GSK3B, GSN, HARS1, HGF, NRG1, HNF4A, HSPD1, AGFG2, HRC, HSD11B1, HSD11B2, HSPA1L, HSPB1, HSPB2, ELN, ELAVL2, SRA1, STS, ATF4, ATM, ATP2A3, ATP7B, BCHE, BCL2A1, HCN2, BMP7, BTF3P11, BTK, SLC25A20, CAPN1, CAPN2, CASP1, CASP3, CASP9, CAT, SERPINC1, RHOA, EGFR, ARAF, ABO, ACP3, ACTG1, ACTG2, ADA, ADAM10, ADCYAP1R1, PLIN2, PARP1, ADRA2C, AFA, AGER, AKT1, ALDH2, ANPEP, APOA1, APP, MS4A1, CD28, CD40, CD68, CTRL, CYBB, CYP1A2, CYP2J2, CYP3A5, DAB2, CD55, DCC, DDT, NQO1, DMD, ATN1, DUSP2, ECT2, EDN2, EDNRB, EFNA5, CTNND1, CTNNB1, CSH2, COL9A1, CES1, CTSC, CHAT, CHGA, CHRM2, CLIC2, COL1A2, COL9A2, CSH1, COL9A3, COMP, KLF6, CPB1, CPM, CRYGC, CSE1L, KCNB1, KCNJ3, KCNJ11, THBS2, THY1, TIMP3, TSPAN8, TP53, TPO, HSP90B1, TRAF2, TRAF6, TRPC1, TSC1, TSC2, TYRP1, UBC, UCHL1, UCP1, VASP, WNT1, THOP1, TGFBI, KCNK2, TFAP2A, SRSF5, SHC1, SLC2A3, SLC6A8, SMPD1, SNAI1, SOAT1, ABCA4, SULT2A1, ETF1P2, TAC1, TACR3, MAP3K7, CNTN2, TBL1X, TRA, TERT, WNT5A, ZAP70, ZNF143, MANF, TIMELESS, WASF1, HSPB3, HGS, SLC28A1, SLC33A1, NOG, SLC9A3R2, KL, FHL5, TBPL1, BCAR1, RGS6, RAPGEF5, SNX17, MVP, CASP8AP2, ASAP2, HDAC3, CES2, CMAHP, PLA2G7, ARHGEF5, NR4A3, MLLT10, CDK2AP1, USP9X, ARID1A, RECK, TNFRSF11A, DOC2A, KCNAB2, LGR5, PSMG1, TNFSF13, TNFSF10, ADAM15, MAP2K4, SCN8A, SCN2A, PDE4D, MPO, MSRA, MT3, MTR, MYD88, NDUFS4, NFATC3, NFATC4, NOS2, NPPC, NPR1, NTF3, NUCB2, OLR1, OSM, PAK1, REG3A, MMP7, MMP3, MMP1, LOXL2, KIT, LBR, LCAT, LEP, LIMK1, LIPE, LOX, LRP5, MME, EPCAM, MCL1, MET, MFAP4, MIF, ATXN3, MLLT6, PCYT1A, PDGFRA, RRAS, PDGFRB, PROC, PSMB10, PSMD4, PTGS2, PTPN11, PTPRC, PTX3, PVR, PVT1, RAF1, RARRES2, RBP4, REG1A, RENBP, RLN2, RPE, RPS27A, MAP2K1, MAPK1, PRKCD, PIK3CG, PDK4, PENK, PEPD, ABCB4, PIK3CA, PIK3CB, PIK3CD, PKD2, PRKCB, PLEC, PPA1, PPBP, PPOX, PPP1R3A, NPY4R, PRKCA, ST13
-
Rickets
Wikipedia
Rickets X-ray of a two-year-old with rickets, with a marked bowing of the femurs and decreased bone density Pronunciation / ˈ r ɪ k ɪ t s / Specialty Pediatrics , rheumatology Symptoms Bowed legs , stunted growth , bone pain, large forehead, trouble sleeping [1] [2] [3] Complications Bone fractures , muscle spasms , abnormally curved spine , intellectual disability [3] Usual onset Childhood [3] Causes Diet without enough vitamin D or calcium , too little sun exposure, exclusive breastfeeding without supplementation, celiac disease , certain genetic conditions [2] [3] [4] Diagnostic method Blood tests , X-rays [2] Differential diagnosis Fanconi syndrome , scurvy , Lowe syndrome , osteomalacia [3] Prevention Vitamin D supplements for exclusively-breastfed babies [5] Treatment Vitamin D and calcium [2] Frequency Relatively common ( Middle East , Africa, Asia) [4] Rickets is a condition that results in weak or soft bones in children. [2] Symptoms include bowed legs , stunted growth , bone pain, large forehead, and trouble sleeping. [2] [3] Complications may include bone fractures , muscle spasms , an abnormally curved spine , or intellectual disability . [2] [3] The most common cause of rickets is a vitamin D deficiency . [2] This can result from eating a diet without enough vitamin D , dark skin, too little sun exposure, exclusive breastfeeding without vitamin D supplementation, celiac disease , and certain genetic conditions . [2] [3] Other factors may include not enough calcium or phosphorus . [4] [5] The underlying mechanism involves insufficient calcification of the growth plate . [6] Diagnosis is generally based on blood tests finding a low calcium , low phosphorus , and a high alkaline phosphatase together with X-rays . [2] Prevention for exclusively breastfed babies is vitamin D supplements. [5] Otherwise, treatment depends on the underlying cause. [2] If due to a lack of vitamin D, treatment is usually with vitamin D and calcium. [2] This generally results in improvements within a few weeks. [2] Bone deformities may also improve over time. [5] Occasionally surgery may be performed to correct bone deformities. [7] [3] Genetic forms of the disease typically require specialized treatment. [5] Rickets occurs relatively commonly in the Middle East , Africa, and Asia. [4] It is generally uncommon in the United States and Europe, except among certain minority groups . [3] [4] It begins in childhood, typically between the ages of 3 and 18 months old. [3] [4] Rates of disease are equal in males and females. [3] Cases of what is believed to have been rickets have been described since the 1st century, [8] and the condition was widespread in the Roman Empire . [9] The disease was common into the 20th century. [8] Early treatments included the use of cod liver oil . [8] Contents 1 Signs and symptoms 2 Cause 2.1 Sunlight 2.2 Evolutionary considerations 3 Diagnosis 3.1 Types 3.2 Differential diagnosis 4 Treatment 4.1 Diet and sunlight 4.2 Supplementation 4.3 Surgery 5 Epidemiology 6 History 6.1 Etymology 7 See also 8 References 9 External links Signs and symptoms [ edit ] Widening of wrist Signs and symptoms of rickets can include bone tenderness, and a susceptibility for bone fractures , particularly greenstick fractures . [10] Early skeletal deformities can arise in infants such as soft, thinned skull bones – a condition known as craniotabes , [11] [12] which is the first sign of rickets; skull bossing may be present and a delayed closure of the fontanelles . ... Therefore, a skeletal survey for rickets can be accomplished with anteroposterior radiographs of the knees, wrists, and ankles. [36] Types [ edit ] Vitamin D-related rickets [37] Vitamin D deficiency Vitamin D-dependent rickets (VDDR) [38] Type 1: insufficiency in actication VDDR1A: 25-Hydroxyvitamin D3 1-alpha-hydroxylase deficiency VDDR1B: CYP2R1 deficiency Type 2: resistance to calcitriol VDDR2A: calcitriol receptor mutation VDDR2B: unknown nuclear ribonucleoprotein interfering with signal transduction Type 3: excessive inactivation ( CYP3A4 mutation, dominant) Hypocalcemia-related rickets Hypocalcemia Chronic kidney failure (CKD-BMD) Hypophosphatemia-related rickets Congenital Vitamin D-resistant rickets [37] Autosomal dominant hypophosphatemic rickets (ADHR) Autosomal recessive hypophosphatemic rickets (ARHR) [39] Hypophosphatemia (typically secondary to malabsorption) Fanconi's syndrome Secondary to other diseases Tumor-induced osteomalacia McCune-Albright syndrome Epidermal nevus syndrome Dent's disease Differential diagnosis [ edit ] Osteochondrodysplasias also known as genetic bone diseases may mimic the clinical picture of rickets in regard to the features of bone deformities. [40] The radiologic picture and the laboratory findings of serum calcium, phosphate and alkaline phosphatase, are important differentiating factors. ... PMID 12897318 . ^ Greek Word Study Tool External links [ edit ] Classification D ICD - 10 : E55 ICD - 9-CM : 268 MeSH : D012279 DiseasesDB : 9351 External resources MedlinePlus : 000344 eMedicine : ped/2014 Patient UK : Rickets Wikimedia Commons has media related to Rickets . v t e Malnutrition Protein-energy malnutrition Kwashiorkor Marasmus Catabolysis Vitamin deficiency B vitamins B 1 Beriberi Wernicke–Korsakoff syndrome Wernicke's encephalopathy Korsakoff's syndrome B 2 Riboflavin deficiency B 3 Pellagra B 6 Pyridoxine deficiency B 7 Biotin deficiency B 9 Folate deficiency B 12 Vitamin B 12 deficiency Other A: Vitamin A deficiency Bitot's spots C: Scurvy D: Vitamin D deficiency Rickets Osteomalacia Harrison's groove E: Vitamin E deficiency K: Vitamin K deficiency Mineral deficiency Sodium Potassium Magnesium Calcium Iron Zinc Manganese Copper Iodine Chromium Molybdenum Selenium Keshan disease Growth Delayed milestone Failure to thrive Short stature Idiopathic General Anorexia Weight loss Cachexia Underweight Authority control NDL : 00567048
-
Leber Optic Atrophy
Omim
Among the Finnish patients, preexcitation syndromes including Wolff-Parkinson-White and Lown-Ganong-Levine are common (Nikoskelainen et al., 1985). ... In studies of 35 Japanese LHON families, Mashima et al. (1996) found that, as in Finnish families, the preexcitation syndromes, Wolff-Parkinson-White syndrome and Lown-Ganong-Levine syndrome, were found relatively commonly, being seen in 5 of 63 individuals (8%) with mtDNA mutations. Nikoskelainen et al. (1985) had found the preexcitation syndrome in 14 of 163 Finns (9%) with mitochondrial DNA mutations. ... In addition to visual loss, each patient developed a complicated neurologic syndrome resembling Leigh syndrome (256000).ND6, ND1, ND4, ND5, ND4L, ATP6, CYTB, COX3, ND2, RPE65, NDUFS2, COX1, IL1B, IL1A, LRAT, CPLX1, OPA1, TBC1D24, PARL, OPA3, CEP290, NDUFA1, CRYZ, FXN, MFN2, PLXNA2, NPTX2, SOD2, RP2, SPG7, RPGR, TAP2, SCN1A, TFPI, TFAM, ABCA4, TK2, TWNK, GGT2, POTEF, GGTLC3, GGTLC5P, SLC26A5, GLIS3, GMCL2, GMCL1, RPGRIP1, ADI1, TP53, NDUFB11, YARS2, GCA, AIPL1, KIF1B, IMMT, OPTN, COX5A, PHLDA2, POLG, RNR2, SERPINA1, PGD, ERG, EPHX1, ENO2, ENDOG, TIMM8A, ACE, CPOX, COX8A, CAT, CASP3, BNIP3L, BNIP3, AR, AQP4, AMD1P2, AMD1, AKR1B1, ESR2, GGT1, GCLC, MAS1, TRNK, TRNF, ACTB, RNR1, MTHFR, COX2, TRNC, MAPT, GRIA1, TACSTD2, KRT10, HLA-B, HLA-A, GSR, GRM2, GRIA2, GGTLC4P
-
X-Linked Severe Combined Immunodeficiency
Gene_reviews
No defect in a known SCID-related gene and 300 to 1500 autologous T cells/μL with impaired function Syndromes with variably affected cellular immunity that may be severe, such as DiGeorge syndrome, CHARGE syndrome, Jacobsen syndrome, RAC2 -dominant interfering variant, DOCK8-deficient hyper IgE syndrome, and cartilage-hair hypoplasia Transient lymphopenia and abnormal TREC screening associated with prematurity (<37 weeks adjusted gestational age). ... Other X-linked immunodeficiencies include X-linked agammaglobulinemia, Wiskott-Aldrich syndrome, X-linked hyper-IgM syndrome, X-linked lymphoproliferative disease, NEMO (X-linked ectodermal dysplasia with varying immunodeficiency) (see Incontinentia Pigmenti), IPEX (autoimmunity, polyendocrinopathy, enteropathy), chronic granulomatous disease (CGD), and properdin deficiency (OMIM 312060).
-
Spinal Muscular Atrophy, X-Linked Infantile
Gene_reviews
Other Autosomal Recessive SMA (non- SMN ) Lethal congenital contracture syndrome (LCCS) is characterized by fetal akinesia sequence leading to multiple joint contractures and death in utero typically before 32 weeks' gestation. ... In addition, congenital myasthenic syndromes are genetic disorders of the neuromuscular junction that may present with arthrogryposis. ... In summary, over the last two decades, knowledge regarding X-linked clinical syndromes in which arthrogryposis is part of the clinical spectrum has grown tremendously. A number of these syndromes have associated hypotonia (for further review, see Hall [2007] and Hall [2010]). Further discussion of these syndromes is beyond the scope of this review.
-
Hospital-Acquired Pneumonia
Wikipedia
External links [ edit ] Hospital-Acquired, Health Care Associated, and Ventilator-Associated Pneumonia from the Cleveland Clinic Cecil Textbook of Medicine v t e Medical harm Concepts Iatrogenesis Medical malpractice Medical error Patient safety Medical debt Unnecessary health care Adverse effect Patient abuse Related concerns Adverse drug reaction Hospital-acquired pneumonia Hospital-acquired infection Iatrogenic anemia Hand washing Records and histories Drug pollution ( List ) v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis v t e Pneumonia Infectious pneumonias Bacterial pneumonia Viral pneumonia Fungal pneumonia Parasitic pneumonia Atypical pneumonia Community-acquired pneumonia Healthcare-associated pneumonia Hospital-acquired pneumonia Ventilator-associated pneumonia Severe acute respiratory syndrome Pneumonias caused by infectious or noninfectious agents Aspiration pneumonia Lipid pneumonia Eosinophilic pneumonia Bronchiolitis obliterans organizing pneumonia Noninfectious pneumonia Chemical pneumonitis Idiopathic pneumonia syndrome
-
Developmental Disability
Wikipedia
The most common developmental disabilities are: Down syndrome is a condition in which people are born with an extra copy of chromosome 21. ... However, if they are born with Down syndrome, they have an extra copy of this chromosome. This extra copy affects the development of the body and brain, causing physical and mental challenges for the individual. Fragile X syndrome (FXS) is thought to cause autism and intellectual disability, usually among boys. ... This, in turn, can be used to calculate a developmental quotient (DQ) as follows: [10] [11] D Q = D e v e l o p m e n t a l a g e C h r o n o l o g i c a l a g e ∗ 100 {\displaystyle DQ={\frac {Developmental\ age}{Chronological\ age}}*100} Associated issues [ edit ] Physical health issues [ edit ] There are many physical health factors associated with developmental disabilities. For some specific syndromes and diagnoses, these are inherent, such as poor heart function in people with Down syndrome. ... George's University of London/Down's Syndrome Association. Archived from the original on 2009-05-04 .
-
Neurofibroma
Wikipedia
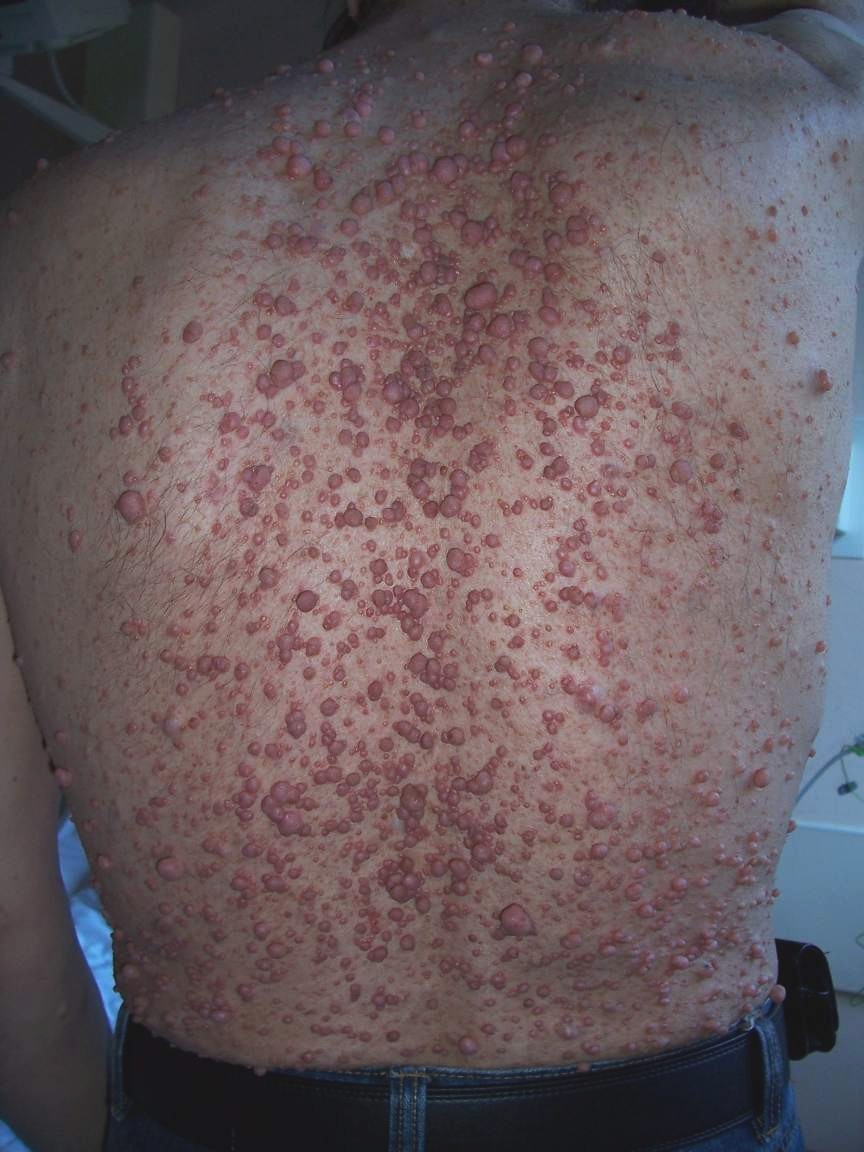
Sirolimus , a compound that inhibits mTOR signalling, is being studied to treat plexiform neurofibromas. [24] [25] The combination of erlotinib with sirolimus was studied to treat low-grade gliomas . [26] Early research has shown potential for using the c-kit tyrosine kinase blocking properties of imatinib to treat plexiform neurofibromas. [27] [28] [29] Peginterferon alfa-2b is being studied to treat plexiform neurofibromas. [30] [31] [32] [33] Sorafenib is being studied for treatment of unresectable plexiform neurofibroma and low-grade astrocytomas . [34] [35] [36] In vitro , tranilast , inhibits growth of neurofibroma cells. [37] Gene therapy for the neurofibromin 1 gene represents the ultimate solution to preventing the cluster of maladies which are enabled by the mutation. [38] [39] As of 2006, therapy for NF1 tumors had not been tested due to the lack of an appropriate NF1 tumor model. [40] See also [ edit ] Malignant peripheral nerve sheath tumor Neurofibromatosis Neurofibromin Genetic disorder Watson syndrome Proteus syndrome RASopathy Palisaded encapsulated neuroma References [ edit ] ^ a b Muir D, Neubauer D, Lim IT, Yachnis AT, Wallace MR (2003). ... PMID 12447105 . v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Tumours of the nervous system Endocrine Sellar : Craniopharyngioma Pituicytoma Other: Pinealoma CNS Neuroepithelial ( brain tumors , spinal tumors ) Glioma Astrocyte Astrocytoma Pilocytic astrocytoma Pleomorphic xanthoastrocytoma Subependymal giant cell astrocytoma Fibrillary astrocytoma Anaplastic astrocytoma Glioblastoma multiforme Oligodendrocyte Oligodendroglioma Anaplastic oligodendroglioma Ependyma Ependymoma Subependymoma Choroid plexus Choroid plexus tumor Choroid plexus papilloma Choroid plexus carcinoma Multiple/unknown Oligoastrocytoma Gliomatosis cerebri Gliosarcoma Mature neuron Ganglioneuroma : Ganglioglioma Retinoblastoma Neurocytoma Dysembryoplastic neuroepithelial tumour Lhermitte–Duclos disease PNET Neuroblastoma Esthesioneuroblastoma Ganglioneuroblastoma Medulloblastoma Atypical teratoid rhabdoid tumor Primitive Medulloepithelioma Meninges Meningioma Hemangiopericytoma Hematopoietic Primary central nervous system lymphoma PNS : Nerve sheath tumor Cranial and paraspinal nerves Neurofibroma Neurofibromatosis Neurilemmoma / Schwannoma Acoustic neuroma Malignant peripheral nerve sheath tumor Other WHO classification of the tumors of the central nervous system Note: Not all brain tumors are of nervous tissue, and not all nervous tissue tumors are in the brain (see brain metastasis ).NF1, SUZ12, KIT, NF2, SPRED1, CDKN2A, PDGFB, TP53, SUFU, SMARCB1, SDHC, SDHB, EGFR, S100B, PDGFRA, S100A1, MDK, NRG1, EGF, SMUG1, VEGFA, FGF2, MDM2, SOX9, PDGFRB, CCND1, FN1, TOP2A, BRAF, CDKN2B-AS1, STAT3, CTNNB1, SST, EED, HMGA2, SYK, CNTN2, FGF23, VDR, TGFA, AURKA, NKX2-1, CXCR4, WT1, TLE1, TGFB1, ALDH1A1, RGS6, SPRY1, H3P23, TMED7-TICAM2, CCR2, MIR339, MIR34A, MIR210, MIR21, MIR10B, TICAM2, GADL1, THSD7A, AZIN2, ARID1B, ADAP2, TMED7, CD274, PDCD4, BRD4, KANK1, SNF8, DCTN6, ZNRD2, CIB1, NES, PTN, SOAT1, DCX, GHSR, GEM, FOLH1, MLANA, EZH2, EVI2B, ERBB2, EPHB2, EFNA3, DUSP5, CSF1, GSTP1, COL3A1, CNP, CDKN2B, CDKN1B, CDK4, CD44, CD38, RUNX1, ATRX, ATM, CXCR3, HGF, SMARCA2, PPARD, CXCL12, CCL2, RASA1, PTPN11, AR, PTEN, PSMD9, MAPK3, MAPK1, PRKAR1A, PMP22, IFI27, PLG, PGR, PDGFA, SERPINE1, NGF, MVD, MMP13, LEP, CXCL10, IFNA2, H3P10
-
Jet Lag
Wikipedia
This article is about the syndrome. For other uses, see Jet lag (disambiguation) . ... External links [ edit ] Classification D ICD - 10 : G47.25 ICD - 9-CM : 307.45 , 780.50 327.35 MeSH : D021081 DiseasesDB : 7045 v t e Sleep and sleep disorders Stages of sleep cycles Rapid eye movement (REM) Non-rapid eye movement Slow-wave Brain waves Alpha wave Beta wave Delta wave Gamma wave K-complex Mu rhythm PGO waves Sensorimotor rhythm Sleep spindle Theta wave Sleep disorders Dyssomnia Excessive daytime sleepiness Hypersomnia Insomnia Kleine–Levin syndrome Narcolepsy Night eating syndrome Nocturia Sleep apnea Catathrenia Central hypoventilation syndrome Obesity hypoventilation syndrome Obstructive sleep apnea Periodic breathing Sleep state misperception Circadian rhythm disorders Advanced sleep phase disorder Cyclic alternating pattern Delayed sleep phase disorder Irregular sleep–wake rhythm Jet lag Non-24-hour sleep–wake disorder Shift work sleep disorder Parasomnia Bruxism Nightmare disorder Night terror Periodic limb movement disorder Rapid eye movement sleep behavior disorder Sleepwalking Somniloquy Benign phenomena Dreams Exploding head syndrome Hypnic jerk Hypnagogia / Sleep onset Hypnopompic state Sleep paralysis Sleep inertia Somnolence Nocturnal clitoral tumescence Nocturnal penile tumescence Nocturnal emission Treatment Sleep diary Sleep hygiene Sleep induction Hypnosis Lullaby Somnology Polysomnography Other Sleep medicine Behavioral sleep medicine Sleep study Daily life Bed Bunk bed Daybed Four-poster bed Futon Hammock Mattress Sleeping bag Bed bug Bedding Bedroom Bedtime Bedtime story Bedtime toy Biphasic and polyphasic sleep Chronotype Dream diary Microsleep Mouth breathing Nap Nightwear Power nap Second wind Siesta Sleep and creativity Sleep and learning Sleep deprivation / Sleep debt Sleeping while on duty Sleepover Snoring
-
Nasopharyngeal Carcinoma
Wikipedia
Undifferentiated cells are cells that do not have their mature features or functions Contents 1 Signs and symptoms 2 Causes 3 Diagnosis 3.1 Classification 3.2 Staging 4 Risk factors 4.1 EBV 4.2 Smoking 5 Treatment 5.1 Radiation therapy 5.2 Chemotherapy 6 Surgery 7 Epidemiology 8 See also 9 References 10 External links Signs and symptoms [ edit ] See also: Trotter's syndrome NPC may present as a lump or a mass on both sides towards the back of the neck. ... Metastatic spread may result in bone pain or organ dysfunction. Rarely, a paraneoplastic syndrome of osteoarthropathy (diseases of joints and bones) may occur with widespread disease. [ citation needed ] Causes [ edit ] NPC is caused by a combination of factors: viral, environmental influences, and heredity. [5] The viral influence is associated with infection with Epstein-Barr virus (EBV). [6] [7] The Epstein-Barr virus is one of the most common viruses. 95% of all people in the U.S. are exposed to this virus by the time they are 30–40 years old. ... External links [ edit ] Classification D ICD - 10 : C11 ICD - 9-CM : 147 OMIM : 161550 MeSH : D009303 DiseasesDB : 8814 External resources eMedicine : ped/1553 Cancer Management Handbook: Head and Neck Tumors Clinically reviewed nasopharyngeal cancer information for patients from Cancer Research UK v t e Cancer involving the respiratory tract Upper RT Nasal cavity Esthesioneuroblastoma Nasopharynx Nasopharyngeal carcinoma Nasopharyngeal angiofibroma Larynx Laryngeal cancer Laryngeal papillomatosis Lower RT Trachea Tracheal tumor Lung Non-small-cell lung carcinoma Squamous-cell carcinoma Adenocarcinoma ( Mucinous cystadenocarcinoma ) Large-cell lung carcinoma Rhabdoid carcinoma Sarcomatoid carcinoma Carcinoid Salivary gland–like carcinoma Adenosquamous carcinoma Papillary adenocarcinoma Giant-cell carcinoma Small-cell carcinoma Combined small-cell carcinoma Non- carcinoma Sarcoma Lymphoma Immature teratoma Melanoma By location Pancoast tumor Solitary pulmonary nodule Central lung Peripheral lung Bronchial leiomyoma Pleura Mesothelioma Malignant solitary fibrous tumor v t e Tumors of lip , oral cavity and pharynx / head and neck cancer Oral cancer Salivary gland malignant epithelial tumors Acinic cell carcinoma Mucoepidermoid carcinoma Adenoid cystic carcinoma Salivary duct carcinoma Epithelial-myoepithelial carcinoma Polymorphous low-grade adenocarcinoma Hyalinizing clear cell carcinoma benign epithelial tumors Pleomorphic adenoma Warthin's tumor ungrouped: Oncocytoma Tongue Leukoplakia Rhabdomyoma Oropharynx v t e Infectious diseases – viral systemic diseases Oncovirus DNA virus HBV Hepatocellular carcinoma HPV Cervical cancer Anal cancer Penile cancer Vulvar cancer Vaginal cancer Oropharyngeal cancer KSHV Kaposi's sarcoma EBV Nasopharyngeal carcinoma Burkitt's lymphoma Hodgkin lymphoma Follicular dendritic cell sarcoma Extranodal NK/T-cell lymphoma, nasal type MCPyV Merkel-cell carcinoma RNA virus HCV Hepatocellular carcinoma Splenic marginal zone lymphoma HTLV-I Adult T-cell leukemia/lymphoma Immune disorders HIV AIDS Central nervous system Encephalitis / meningitis DNA virus Human polyomavirus 2 Progressive multifocal leukoencephalopathy RNA virus MeV Subacute sclerosing panencephalitis LCV Lymphocytic choriomeningitis Arbovirus encephalitis Orthomyxoviridae (probable) Encephalitis lethargica RV Rabies Chandipura vesiculovirus Herpesviral meningitis Ramsay Hunt syndrome type 2 Myelitis Poliovirus Poliomyelitis Post-polio syndrome HTLV-I Tropical spastic paraparesis Eye Cytomegalovirus Cytomegalovirus retinitis HSV Herpes of the eye Cardiovascular CBV Pericarditis Myocarditis Respiratory system / acute viral nasopharyngitis / viral pneumonia DNA virus Epstein–Barr virus EBV infection / Infectious mononucleosis Cytomegalovirus RNA virus IV : Human coronavirus 229E / NL63 / HKU1 / OC43 Common cold MERS coronavirus Middle East respiratory syndrome SARS coronavirus Severe acute respiratory syndrome SARS coronavirus 2 Coronavirus disease 2019 V , Orthomyxoviridae : Influenza virus A / B / C / D Influenza / Avian influenza V, Paramyxoviridae : Human parainfluenza viruses Parainfluenza Human orthopneumovirus hMPV Human digestive system Pharynx / Esophagus MuV Mumps Cytomegalovirus Cytomegalovirus esophagitis Gastroenteritis / diarrhea DNA virus Adenovirus Adenovirus infection RNA virus Rotavirus Norovirus Astrovirus Coronavirus Hepatitis DNA virus HBV ( B ) RNA virus CBV HAV ( A ) HCV ( C ) HDV ( D ) HEV ( E ) HGV ( G ) Pancreatitis CBV Urogenital BK virus MuV Mumps
-
Rhinitis
Wikipedia
Vasomotor rhinitis is now included among these under the more general classification of nonallergic rhinitis. [17] The diagnosis is made upon excluding allergic causes. [18] It is an umbrella term of rhinitis of multiple causes, such as occupational (chemical), smoking, gustatory, hormonal, senile (rhinitis of the elderly), atrophic, medication-induced (including rhinitis medicamentosa), local allergic rhinitis, non-allergic rhinitis with eosinophilia syndrome (NARES) and idiopathic (vasomotor or non-allergic, non-infectious perennial allergic rhinitis (NANIPER), or non-infectious non-allergic rhinitis (NINAR). [19] In vasomotor rhinitis, [20] [21] certain nonspecific stimuli, including changes in environment (temperature, humidity, barometric pressure , or weather), airborne irritants (odors, fumes), dietary factors (spicy food, alcohol), sexual arousal, exercise, [22] and emotional factors trigger rhinitis. [23] There is still much to be learned about this, but it is thought that these non-allergic triggers cause dilation of the blood vessels in the lining of the nose, which results in swelling and drainage. ... "Classification of Nonallergic Rhinitis Syndromes With a Focus on Vasomotor Rhinitis, Proposed to be Known henceforth as Nonallergic Rhinopathy" . ... External links [ edit ] Classification D ICD - 10 : J00 , J30 , J31.0 ICD - 9-CM : 472.0 , 477 OMIM : 607154 MeSH : D012220 DiseasesDB : 26380 External resources MedlinePlus : 000813 eMedicine : ent/194 med/104 , ped/2560 Sinus Infection And Allergic Rhinitis Specialist Library for ENT and Audiology Hay fever resources – online library of high quality research on hay fever and other ENT disorders v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis v t e Decongestants and other nasal preparations ( R01 ) Topical Sympathomimetics , plain Cyclopentamine Ephedrine Epinephrine Fenoxazoline Levomethamphetamine Metizoline Naphazoline Oxymetazoline Phenylephrine Propylhexedrine Tetryzoline Tramazoline Tuaminoheptane Tymazoline Xylometazoline Antiallergic agents, excluding corticosteroids Spaglumic acid histamine antagonists ( Levocabastine Antazoline Thonzylamine ) mast cell stabilizer (some are also antihistamines) ( Cromoglicic acid Nedocromil Azelastine Olopatadine Lodoxamide ) Corticosteroids Beclometasone dipropionate Betamethasone # Budesonide Ciclesonide Dexamethasone Flunisolide Fluticasone ( Fluticasone furoate , Fluticasone propionate ) Mometasone furoate Prednisolone # Tixocortol Triamcinolone Triamcinolone acetonide Other nasal preparations Cafaminol Calcium hexamine thiocyanate Eucalyptus oil Framycetin Hexamidine Hyaluronan Ipratropium bromide Mupirocin Retinol Ritiometan Saline water Combination products Olopatadine/mometasone Systemic use: Sympathomimetics Phenylephrine Phenylpropanolamine Pseudoephedrine ( +loratadine ) # WHO-EM ‡ Withdrawn from market Clinical trials : † Phase III § Never to phase III v t e Allergic conditions Respiratory system Allergic rhinitis (hay fever) Asthma Hypersensitivity pneumonitis Eosinophilic pneumonia Eosinophilic granulomatosis with polyangiitis Allergic bronchopulmonary aspergillosis Farmer's lung Laboratory animal allergy Skin Angioedema Urticaria Atopic dermatitis Allergic contact dermatitis Hypersensitivity vasculitis Blood and immune system Serum sickness Circulatory system Anaphylaxis Digestive system Coeliac disease Eosinophilic gastroenteritis Eosinophilic esophagitis Food allergy Egg allergy Milk intolerance Nervous system Eosinophilic meningitis Genitourinary system Acute interstitial nephritis Other conditions Drug allergy Allergic conjunctivitis Latex allergy Medicine portal
-
Anti-Nmda Receptor Encephalitis
Wikipedia
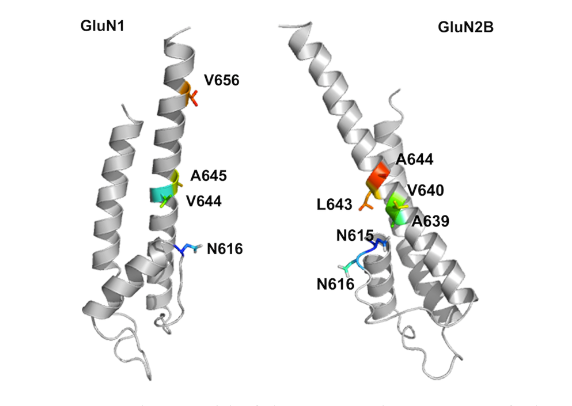
rare disease which results in brain inflammation Anti-NMDA receptor encephalitis Other names NMDA receptor antibody encephalitis, anti-N-methyl-D-aspartate receptor encephalitis, anti-NMDAR encephalitis A schematic diagram of the NMDA receptor Specialty Neurology , psychiatry Symptoms Early : Fever , headache, feeling tired, psychosis , agitated [1] [2] Later : Seizures , decreased breathing , blood pressure and heart rate variability [1] Complications Long term mental or behavioral problems [2] Usual onset Over days to weeks [3] Risk factors Ovarian teratoma , unknown [1] [4] Diagnostic method Specific antibodies in the cerebral spinal fluid [1] Differential diagnosis Viral encephalitis , acute psychosis , neuroleptic malignant syndrome [2] Treatment Immunosuppresive medication , surgery [1] Medication Corticosteroids , intravenous immunoglobulin (IVIG), plasma exchange , azathioprine [2] Prognosis Typically good (with treatment) [1] Frequency Relatively common [2] Deaths ~4% risk of death [2] Anti-NMDA receptor encephalitis is a type of brain inflammation caused by antibodies . [4] Early symptoms may include fever , headache, and feeling tired. [1] [2] This is then typically followed by psychosis which presents with false beliefs (delusions) and seeing or hearing things that others do not see or hear (hallucinations). [1] People are also often agitated or confused. [1] Over time seizures , decreased breathing , and blood pressure and heart rate variability typically occur. [1] About half of cases are associated with tumors , most commonly teratomas of the ovaries . [1] [4] Another established trigger is herpesviral encephalitis , while the cause in others cases is unclear. [1] [4] [5] The underlying mechanism is autoimmune with the primary target the GluN1 subunit of the N-methyl D-aspartate receptors (NMDAR) in the brain. [1] [6] Diagnosis is typically based on finding specific antibodies in the cerebral spinal fluid . [1] MRI of the brain is often normal. [2] Misdiagnosis is common. [6] Treatment is typically with immunosuppresive medication and, if a tumor is present, surgery to remove it. [1] With treatment about 80% of people have a good outcome. [1] Outcomes are better if treatment is begun earlier. [2] Long-term mental or behavioral problems may remain. [2] About 4% of those affected die from the condition. [2] Recurrence occurs in about 10% of people. [1] The estimated number of cases of the disease is 1.5 per million people per year. [5] The condition is relatively common compared to other paraneoplastic disorders . [2] About 80% of those affected are female. [2] It typically occurs in adults younger than 45 years old, but it can occur at any age. [4] [6] The disease was first described by Josep Dalmau in 2007. [1] [7] Contents 1 Signs and symptoms 2 Pathophysiology 2.1 Antibodies 3 Diagnosis 4 Management 5 Prognosis 6 Epidemiology 7 Society and culture 8 See also 9 References 10 External links Signs and symptoms [ edit ] Prior to the development of a symptom complex that is specific to anti-NMDA receptor encephalitis, people may experience prodromal symptoms, including headaches , flu-like illness , or symptoms similar to an upper respiratory infection . ... "Anti-NMDA receptor encephalitis presenting with imaging findings and clinical features mimicking Rasmussen syndrome". Seizure . 20 (3): 266–270. doi : 10.1016/j.seizure.2010.11.013 . ... Columbia University Medical Center. v t e Paraneoplastic syndromes Endocrine Hypercalcaemia SIADH Zollinger–Ellison syndrome Cushing's syndrome Hematological Multicentric reticulohistiocytosis Nonbacterial thrombotic endocarditis Neurological Paraneoplastic cerebellar degeneration Encephalomyelitis Limbic encephalitis Opsoclonus Polymyositis Transverse myelitis Lambert–Eaton myasthenic syndrome Anti-NMDA receptor encephalitis Musculoskeletal Dermatomyositis Hypertrophic osteopathy Mucocutaneous reactive erythema Erythema gyratum repens Necrolytic migratory erythema papulosquamous Acanthosis nigricans Ichthyosis acquisita Acrokeratosis paraneoplastica of Bazex Extramammary Paget's disease Florid cutaneous papillomatosis Leser-Trélat sign Pityriasis rotunda Tripe palms Other Febrile neutrophilic dermatosis Pyoderma gangrenosum Paraneoplastic pemphigus
-
Erethism
Wikipedia
Mercury poisoning, chronic (neurological symptomatology) Elemental mercury Specialty Medical toxicology Erethism , also known as erethism mercurialis , mad hatter disease , or mad hatter syndrome , is a neurological disorder which affects the whole central nervous system, as well as a symptom complex, derived from mercury poisoning . ... Signs and symptoms can include red fingers, red toes, red cheeks, sweating, loss of hearing, bleeding from the ears and mouth, loss of appendages such as teeth, hair, and nails, lack of coordination, poor memory, shyness, insomnia, nervousness, tremors, and dizziness. [10] A survey of exposed U.S. hatters revealed predominantly neurological symptomatology, including intention tremor . [8] After chronic exposure to the mercury vapours, hatters tended to develop characteristic psychological traits, such as pathological shyness and marked irritability (box). [11] Such manifestations among hatters prompted several popular names for erethism, including "mad hatter disease", [9] "mad hatter syndrome", [12] [13] "hatter's shakes" and " Danbury shakes". ... Public Health Service in 1941, the manufacturers voluntarily agreed to adopt a readily available alternative process using hydrogen peroxide . [18] "Mad as a hatter" [ edit ] While the name of Lewis Carroll's Mad Hatter may contain an allusion to the hatters' syndrome, the character itself appears to have been based on an eccentric furniture dealer. Main article: Mad as a hatter Although the expression "mad as a hatter" was associated with the syndrome, [28] the origin of the phrase is uncertain. ... PMC 1550196 . PMID 6418283 . ^ "Mad Hatter syndrome" . Stedman's Medical Dictionary .
-
Obesity
Omim
Autosomal recessive disorders with obesity as a predominant feature include leptin deficiency (614962), leptin receptor deficiency (614963), prohormone convertase-1 deficiency (600955), and proopiomelanocortin deficiency (609734); associated features in these disorders include hypogonadotropic hypogonadism, hypoadrenalism, and short stature. There are also syndromes associated with obesity such as Prader-Willi syndrome (176270), Bardet-Biedl syndrome (BBS; see 209900), and Cohen syndrome (216550), among others. ... Barness et al. (2007) reviewed the genetic, molecular, and environmental aspects of obesity and discussed the myriad associated complications, including hypertension (145500), dyslipidemia, endothelial dysfunction, type 2 diabetes mellitus (125853) and impaired glucose tolerance, acanthosis nigricans (100600), hepatic steatosis, premature puberty (see 176400), hypogonadism and polycystic ovary syndrome, obstructive sleep disorder, orthopedic complications, cholelithiasis, and pseudotumor cerebri (243200). ... Application of this method to liver and adipose gene expression data generated from a segregating mouse population resulted in the identification of a macrophage-enriched metabolic network (MEMN) supported as having a causal relationship with disease traits associated with metabolic syndrome (see 605552). Three genes in this network, lipoprotein lipase (LPL; 609708), lactamase beta (LACTB; 608440), and protein phosphatase 1-like (PPM1L; 611931), were validated as previously unknown obesity genes, strengthening the association between this network and metabolic disease traits.