-
Acute Pancreatitis
Wikipedia
The inflammatory response leads to the secondary manifestations of pancreatitis: hypovolemia from capillary permeability, acute respiratory distress syndrome, disseminated intravascular coagulations, renal failure, cardiovascular failure, and gastrointestinal hemorrhage. ... In 5 percent cases, it may result in ARDS (acute respiratory distress syndrome), DIC (disseminated intravascular coagulation) Acute pancreatitis can be further divided into mild and severe pancreatitis. ... Necrosis will be followed by a systemic inflammatory response syndrome (SIRS) and will determine the immediate clinical course. ... BUN >25 mg/dL (8.9 mmol/L) Abnormal mental status with a Glasgow coma score <15 Evidence of SIRS (systemic inflammatory response syndrome) Patient age >60 years old Imaging study reveals pleural effusion Patients with a score of zero had a mortality of less than one percent, whereas patients with a score of five had a mortality rate of 22 percent. ... 2013/137/6/1210/114397 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum PneumoperitoneumLEP, SERPINA1, REG3A, BIRC5, MTNR1B, CX3CL1, KIT, APOE, LMNA, CXCL8, IL10, PRSS1, BSCL2, CFTR, NSMCE2, BTBD8, MPO, CRP, AGPAT2, IL6, NLRP3, HMGCL, HMGB1, TNF, SPINK1, IL1B, TLR4, DPP4, ALB, CCL2, MAPK14, STAT3, PRSS2, GABPA, NFE2L2, AHSA1, PIK3CG, CRK, AKT1, MAPK1, AIMP2, CD14, LPL, GRAP2, HMOX1, RNF19A, ACE, POLDIP2, PIK3CD, PIK3CA, DSPP, TRAF3, PIK3CB, CALCA, JAK2, SH2D1A, CCK, APCS, IL1A, SST, MIR216A, GSTT1, GLP1R, GCG, GORASP1, MTAP, RIPK3, ELANE, WNK1, TLR9, CTRC, IL1RN, HSPA1B, SYT1, TGFB1, REN, PTX3, PTGS2, ACTB, ASPG, MAPK8, KMO, RELA, TAC1, MIR155, DECR1, IFNG, VEGFA, CLDN2, S100A9, TP53, SOCS3, SQSTM1, SETMAR, IFNA1, TLR3, HSPA2, RIPK1, HSPA4, ICAM1, TLR2, NOS2, KL, IL17A, NUP62, LILRB1, P2RX7, FGL2, PROCR, HSPA1A, PON1, MMP9, PPARGC1A, MEFV, MDK, CNPY2, PPID, PRKCD, LPA, LCN2, MPRIP, PTHLH, SIRT1, KHDRBS1, PYY, IFNA13, DCTN4, ANGPT1, CARD9, PTK2B, APOB, F2, MORC4, EHMT1, MIR551B, ASRGL1, TP53INP1, NQO1, APOA5, CASP9, CTNNB1, MLKL, CST3, CSF3, RTL1, GOLGA6A, GPIHBP1, ANGPT2, ERN1, CD34, GOT2, AGT, AGER, GTF2H1, RCBTB1, GPT, ALDH2, GSTM1, CBSL, VIP, MIR148A, OCLN, ADIPOQ, STING1, MIR141, AIM2, MIR127, GDF15, MIR122, IP6K1, NR1H4, ARFRP1, PPIF, VCAM1, MIR21, MTCO2P12, VDR, MAGI2, MALAT1, SRA1, LOC102724197, PLA2G7, MIR27A, BECN1, TFEB, MFT2, CD24, ZGLP1, CCR2, MANF, CXCR4, KMT2D, GALR3, SOCS1, TRPV1, RAMP1, RAB7A, DEFB4B, RIPK2, MIR542, GALR2, DEFB104B, MIR375, HSPB3, MIR339, CDKL2, PIM3, MIR34A, MIR29A, PIAS3, GADL1, RETN, ADM2, RAB21, TNIP2, TAB2, LMF1, TNMD, CELA3B, SMUG1, IL21, CXCL16, AKR1B10, SPHK2, FGF21, PARD3, BET1, SLC17A5, CCDC91, INTU, TREM1, SGSM3, UQCRFS1, GHRL, CD274, ERO1A, MBL3P, GAL, SARAF, ISYNA1, NINL, ADAMTS13, CPTP, VMP1, AKR1A1, RAB7B, OR10A4, TLR6, KLF2, RACK1, MARCHF2, GPRC6A, YAP1, MARVELD2, OLFM1, ATG7, GPBAR1, TICAM1, DEFB104A, NIBAN1, HPSE, B3GALT5-AS1, AZIN2, DNER, GGTLC1, IL33, UCN2, HAVCR2, RALBP1, SPINK5, COL25A1, UROD, ACR, UMOD, CTSG, ESR1, ERBB4, ERBB2, STX2, EPHB2, EPHB1, ENPEP, ELK3, EGR1, EGFR, EGF, DUSP1, RCAN1, DEFB4A, DEFB1, DDIT3, CYP24A1, ESR2, ETV5, F3, GH1, HGF, GSTP1, GSR, CXCL2, CXCL1, GP2, GLI2, GFER, F5, FUT2, FN1, FOXF1, FGFR1, FCGR3B, FCGR3A, FABP2, CYLD, CTSB, UCP2, CTH, SERPINC1, ARRB2, ARRB1, AQP5, FAS, APOC3, APOC2, AQP8, APOA1, XIAP, ANXA3, ANXA2, AHSG, AHCY, CRISP1, ADH5, ADH1C, RERE, AVP, BCL2, CD19, CRH, CLDN4, CPB2, CPB1, CNR2, LTB4R, CEL, CBS, BCL3, RUNX3, CAT, CASR, CASP1, CAPN1, SERPING1, BTC, HIF1A, HRG, HSF1, HSPB1, CCL3, SCT, S100A12, ROS1, RBP4, RARRES2, MOK, RAC1, PTPRC, PTH, PTEN, PSMC1, PRSS3, PROC, MAP2K3, PRKD1, PPY, CXCL12, SELE, SFTPD, PPP1R11, TYMS, TNFAIP6, TNFAIP3, TM7SF2, THPO, TFRC, TFAM, TCF3, SLC2A1, STIM1, SSRP1, SOX9, SOD1, SNTB1, SNAP25, SLC6A2, PTPA, PPIA, PNLIPRP2, IL13, KRT5, KNG1, KDR, ITPR3, ITPR1, ISG20, IL18, IL12B, LTA, IL7R, IL4, IL2RA, IFNB1, IFIT1, IAPP, HSPB2, LGALS3, SMAD2, PNLIP, NPPA, PLG, PLA2G2A, PDCD1, PAK1, SERPINE1, PAEP, NTS, NPY, SMAD7, NFKBIA, MYO9B, COX2, MMP2, MLN, MIF, MBL2, H3P45
-
Toothache
Wikipedia
It normally starts two to four days after the extraction, and may last 10–40 days. [14] [26] : 122 [27] : 216–217 [29] Healing is delayed, and it is treated with local anesthetic dressings, which are typically required for five to seven days. [27] : 216–217 There is some evidence that chlorhexidine mouthwash used prior to extractions prevents alveolar osteitis. [29] Combined pulpal-periodontal [ edit ] Dental trauma and cracked tooth syndrome [ edit ] Crown-root fracture with pulp involvement (left). ... Various conditions may involve the alveolar bone, and cause non-odontogenic toothache, such as Burkitt's lymphoma , [38] : 340 infarcts in the jaws caused by sickle cell disease , [40] : 214 and osteomyelitis . [41] : 497 Various conditions of the trigeminal nerve can masquerade as toothache, including trigeminal zoster (maxillary or mandibular division), [40] : 487 trigeminal neuralgia , [36] cluster headache , [36] and trigeminal neuropathies . [36] Very rarely, a brain tumor might cause toothache. [35] : 80,81 Another chronic facial pain syndrome which can mimic toothache is temporomandibular disorder (temporomandibular joint pain-dysfunction syndrome), [36] which is very common. ... Dental pain can simulate virtually any facial pain syndrome. [44] However, the vast majority of toothache is caused by dental, rather than non-dental, sources. [10] : 40 Consequently, the saying " horses, not zebras " has been applied to the differential diagnosis of orofacial pain. ... For example, a pulpal abscess (which is typically severe, spontaneous and localized) can cause periapical periodontitis (which results in pain on biting). Cracked tooth syndrome may also cause a combination of symptoms. ... Assessment of biting on individual teeth (which sometimes helps to localize the problem) or the separate cusps (may help to detect cracked cusp syndrome). Less commonly used tests might include trans-illumination (to detect congestion of the maxillary sinus or to highlight a crack in a tooth), dyes (to help visualize a crack), a test cavity, selective anaesthesia and laser doppler flowmetry .
-
Pseudobulbar Affect
Wikipedia
., nitrous oxide and insecticides ), fou rire prodromique , and Angelman syndrome . It is hypothesized that these primary neurologic injuries and diseases affect chemical signaling in the brain, which in turn disrupts the neurologic pathways that control emotional expression. [20] [21] [22] Stroke [ edit ] PBA is one of the most frequently reported post-stroke behavioral syndromes , with a range of reported prevalence rates from 28% to 52%. [23] [24] [25] The higher prevalence rates tend to be reported in stroke patients who are older or who have a history of prior stroke. [26] [27] The relationship between post-stroke depression and PBA is complicated, because the depressive syndrome also occurs with high frequency in stroke survivors. Post-stroke patients with PBA are more depressed than post-stroke patients without PBA, and the presence of a depressive syndrome may exacerbate the weeping side of PBA symptoms. [23] [28] Multiple sclerosis [ edit ] Recent studies suggest that approximately 10% of patients with multiple sclerosis (MS) will experience at least one episode of emotional lability. [29] [30] PBA is generally associated with later stages of the disease (chronic progressive phase). [25] PBA in MS patients is associated with more severe intellectual deterioration, physical disability, and neurological disability. [31] Amyotrophic lateral sclerosis [ edit ] A study designed specifically to survey for prevalence found that 49% of patients with amyotrophic lateral sclerosis (ALS) also had PBA. [9] PBA does not appear to be associated with duration of ALS. [32] [33] It is a symptom of ALS that many patients are unaware of and do not receive information about from their physician. [34] Traumatic brain injury [ edit ] One study of 301 consecutive cases in a clinic setting reported a 5% prevalence. ... It is therefore critical for families and caregivers to recognize the pathological nature of PBA and the reassurance that this is an involuntary syndrome that is manageable. Traditionally, antidepressants such as sertraline , [38] fluoxetine , [39] citalopram , [40] nortriptyline [41] and amitriptyline [42] have been prescribed with some efficacy. ... "Often overlooked neuropsychiatric syndromes in Parkinson's disease" . British Journal of Medical Practitioners . 6 (1).
-
Pericoronitis
Wikipedia
Classification D ICD - 10 : K05.2 (acute), K05.3 (chronic) ICD - 9-CM : 523.3 MeSH : D010497 DiseasesDB : 9827 SNOMED CT : 22240003 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Cat Health
Wikipedia
Found in Persians and Himalayans . Flat-chested kitten syndrome Skin disorders [ edit ] Further information: Cat skin disorders Skin disorders are among the most common health problems in cats and have many causes. ... Feline asthma Flat-chested kitten syndrome Feline hepatic lipidosis also known as Feline Fatty Liver Syndrome, is one of the most common forms of liver disease of cats. [5] The disease begins when the cat stops eating from a loss of appetite, forcing the liver to convert body fat into usable energy. Feline lower urinary tract disease is a term that is used to cover many problems of the feline urinary tract , including stones and cystitis . The term feline urologic syndrome is an older term which is still sometimes used for this condition. ... These are people "with immature or weakened immune systems" (infants, the elderly, people undergoing cancer therapy, and individuals with acquired immunodeficiency syndrome). Some common and preventable forms of zoonosis [6] are as follows: Toxoplasmosis Giardia Cat-scratch disease Rabies Ringworm Preventive medicine [ edit ] Vaccinations [ edit ] Main article: Feline vaccination Vaccinations are an important preventive animal health measure. ... Non-therapeutic surgical procedures [ edit ] Spaying and neutering Onychectomy (declawing) Dangers in urban environment [ edit ] High–rise syndrome Vehicles Toxic substances [ edit ] The ASPCA lists some common sources of toxins [16] that pets encounter, including: plants, [17] human medications and cosmetics, [18] cleaning products, [19] and even foods. [20] Some houseplants are harmful to cats.
-
Neurogenic Claudication
Wikipedia
Differential diagnosis Vascular claudication , trochanteric bursitis , piriformis syndrome , muscle pain , vertebral compression fracture , compartment sydnrome , peripheral neuropathy , Lumbar radicular syndrome (lumbar radiculopathy) and pain in other spinal structures: hip , myofascia , sacroiliac joint Treatment Physical therapy, medications, surgery Medication Non-steroidal anti-inflammatory drugs , prostaglandin-based drugs , gabapentin , methylcobalamin , epidural injections , lidocaine and steroids Neurogenic claudication ( NC ), also known as pseudoclaudication , is the most common symptom of lumbar spinal stenosis (LSS) and describes intermittent leg pain from impingement of the nerves emanating from the spinal cord . [1] [2] Neurogenic means that the problem originates within the nervous system . ... These conditions contribute to the potential narrowing of the spinal cord, increasing pressure and inducing damage on the spinal nerve roots, thus, causing paing, tingling or weakness in the lower body. [5] Risk factors for LSS include: [16] [15] Age Degenerative changes of the spine Obesity Family history of spinal stenosis Tobacco use Occupation involving repetitive mechanical stress on the spine Past deformities or injuries to the spine Diagnosis and Evaluation [ edit ] MRI of the lumbar spine showing spinal stenosis Neurogenic claudication is one subtype of the clinical syndrome of lumbar spinal stenosis (LSS). [9] No gold standard diagnostic criteria currently exist, but evaluation and diagnosis is generally based on the patient history, physical exam, and medical imaging . [1] The accuracy of a diagnosis of NC increases with each additional suggestive clinical finding. ... The differential diagnosis for NC includes: [9] Vascular claudication Lumbosacral radicular pain secondary to lumbar disc herniation Referred pain from spinal structures, hip or sacroiliac joint, myofascia , or viscera Trochanteric bursitis Piriformis syndrome Muscle pain Vertebral compression fracture Compartment syndrome Peripheral neuropathy Neurogenic vs vascular claudication [ edit ] Neurogenic vs Vascular Claudication [2] [10] [4] Clinical feature Neurogenic Vascular Pain worse with Standing, walking Walking Pain relieved by Spinal flexion , sitting Standing Timing of relief Within minutes Immediately Location Above the knees Below the knees Radiation of pain Extends down legs Extends up legs Quality of pain Sharp Cramping, dull Back pain Common Sometimes Peripheral pulses Present May be absent Both neurogenic claudication and vascular claudication manifest as leg pain with walking, but several key features help distinguish between these conditions. [7] In contrast to NC , vascular claudication does not vary with changes in posture. [9] Patients with vascular claudication may experience relief with standing, which may provoke symptoms in NC . ... Over time, untreated NC and LSS can lead to chronic pain and muscle weakness. [13] In severe cases, caudea equina syndrome can develop, disrupting sensory and motor function in the lower body and bladder. [15] Consequently, disability in the lower extremities may develop over time in individuals with untreated NC and LSS . [15] Whilst some patients may recover and improve their NC condition over time, without the help of medical treatment or interventions, this is only prevalent in individuals with light or very mild symptoms of NC . ... "Does this older adult with lower extremity pain have the clinical syndrome of lumbar spinal stenosis?" . JAMA . 304 (23): 2628–36. doi : 10.1001/jama.2010.1833 .
-
Flat-Chested Kitten Syndrome
Wikipedia
Flat-chested kitten syndrome ( FCKS ) is a disorder in cats wherein kittens develop a compression of the thorax (chest/ribcage) caused by lung collapse. ... Hyaline membrane disease is a type of respiratory distress syndrome of the newborn in which there is formation of a hyaline -like membrane lining the terminal respiratory passages, and this may also be a (rarer) cause of FCKS. ... The kitten was wrapped in a 'corset' for about 2 weeks. It is now a healthy adult. The syndrome is life-threatening in a significant number of cases (possibly around 40%) mainly due to a lack of understanding of the underlying cause of the condition, failure to treat colic (leading to slow starvation) and insufficient sources of information in veterinary literature. ... Burmese Cat Club Newsletter 1980, downloadable pdf files accessible from this page ^ Edinburgh FAB resident, Royal Dick Veterinary Hospital: Report in FAB Journal (1993), vol. 31 (1) 71-72 ^ particularly B A Hills: The role of lung surfactant, British Journal of Anaesthesia 1990, 65, 13-29 ^ Information regarding splinting of FCKS kittens ^ Although corsets can be improvised easily from e.g. plastic drinks bottles etc., one breeder has marketed a 'corset' design that she found successful with her kittens www.fck-flat-korsett.de ^ Information about kitten milk and other supplements further down the page External links [ edit ] Vetstream article on FCKS in journal Felis ISSN 2398-2950 Flat-Chested Kitten Syndrome Marine Minnaert: Étude rétrospective de la cage thoracique plate chez le chat : caractéristiques épidémiologiques et cliniques, pronostic et aspects génétiques , PhD thesis (2014) pdf International Cat Care website; based on Sturgess 1997, which is out of date and incorrect in many particulars Sturgess C P, Waters L, Gruffydd-Jones T J et al (1997) Investigation of the association between whole blood and tissue taurine levels and the development of thoracic deformities in neonatal Burmese kittens.
-
Dentin Hypersensitivity
Wikipedia
External links [ edit ] Classification D ICD - 10 : K03.8 MeSH : D003807 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
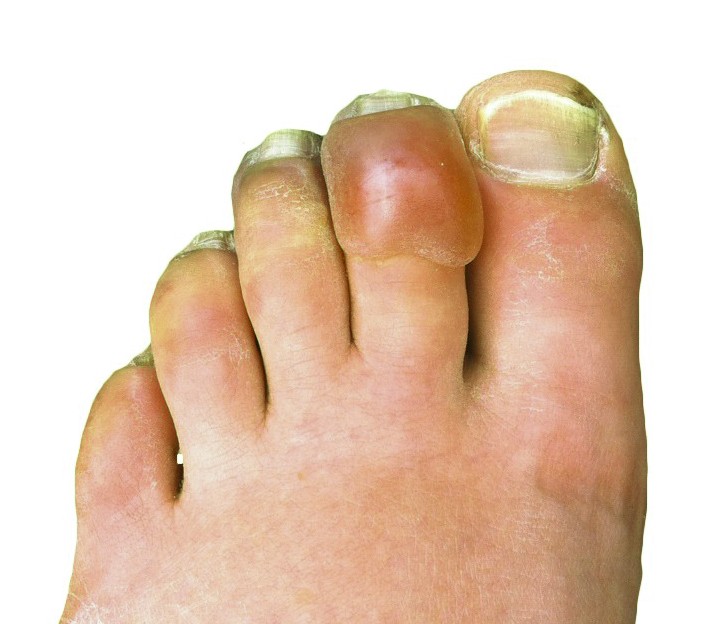
Frostbite
Wikipedia
Frostbite Other names Frostnip Frostbitten toes two to three days after mountain climbing Specialty Dermatology Emergency medicine , orthopedics Symptoms Numbness, feeling cold, clumsy, pale color [1] Complications Hypothermia , compartment syndrome [2] [1] Types Superficial, deep [2] Causes Temperatures below freezing [1] Risk factors Alcohol , smoking, mental health problems , certain medications, prior cold injury [1] Diagnostic method Based on symptoms [3] Differential diagnosis Frostnip, pernio , trench foot [4] Prevention Avoid cold, wear proper clothing, maintain hydration and nutrition, stay active without becoming exhausted [2] Treatment Rewarming, medication, surgery [2] Medication Ibuprofen , tetanus vaccine , iloprost , thrombolytics [1] Frequency Unknown [5] Frostbite occurs when exposure to low temperatures causes freezing of the skin or other tissues. [1] The initial symptom is typically numbness. [1] This may be followed by clumsiness with a white or bluish color to the skin. [1] Swelling or blistering may occur following treatment. [1] The hands, feet, and face are most commonly affected. [4] Complications may include hypothermia or compartment syndrome . [2] [1] People who are exposed to low temperatures for prolonged periods, such as winter sports enthusiasts, military personnel, and homeless individuals, are at greatest risk. [6] [1] Other risk factors include drinking alcohol , smoking, mental health problems , certain medications, and prior injuries due to cold. [1] The underlying mechanism involves injury from ice crystals and blood clots in small blood vessels following thawing. [1] Diagnosis is based on symptoms. [3] Severity may be divided into superficial (1st and 2nd degree) or deep (3rd and 4th degree). [2] A bone scan or MRI may help in determining the extent of injury. [1] Prevention is through wearing proper clothing, maintaining hydration and nutrition, avoiding low temperatures, and staying active without becoming exhausted. [2] Treatment is by rewarming. [2] This should be done only when refreezing is not a concern. [1] Rubbing or applying snow to the affected part is not recommended. [2] The use of ibuprofen and tetanus toxoid is typically recommended. [1] For severe injuries iloprost or thrombolytics may be used. [1] Surgery is sometimes necessary. [1] Amputation, however, should generally be delayed for a few months to allow determination of the extent of injury. [2] The number of cases of frostbite is unknown. [5] Rates may be as high as 40% a year among those who mountaineer . [1] The most common age group affected is those 30 to 50 years old. [4] Evidence of frostbite occurring in people dates back 5,000 years. [1] Frostbite has also played an important role in a number of military conflicts. [1] The first formal description of the condition was in 1813 by Dominique Jean Larrey , a physician in Napoleon 's army, during its invasion of Russia . [1] Contents 1 Signs and symptoms 1.1 First degree 1.2 Second degree 1.3 Third degree 1.4 Fourth degree 2 Causes 2.1 Risk factors 3 Mechanism 3.1 Freezing 3.2 Rewarming 3.3 Non-freezing cold injury 3.4 Pathophysiology 4 Diagnosis 5 Prevention 6 Treatment 6.1 Rewarming 6.2 Medications 6.3 Surgery 7 Prognosis 7.1 Grades 8 Epidemiology 9 History 10 Society and culture 11 Research directions 12 References 13 External links Signs and symptoms [ edit ] Frostbite Areas that are usually affected include cheeks, ears, nose and fingers and toes. ... Debridement or amputation of necrotic tissue is usually delayed unless there is gangrene or systemic infection ( sepsis ). [6] This has led to the adage "Frozen in January, amputate in July". [20] If symptoms of compartment syndrome develop, fasciotomy can be done to attempt to preserve blood flow. [6] Prognosis [ edit ] 3 weeks after initial frostbite Tissue loss and autoamputation are potential consequences of frostbite. ... Mayo Clinic Definition v t e General wounds and injuries Abrasions Abrasion Avulsion Blisters Blood blister Coma blister Delayed blister Edema blister Fracture blister Friction blister Sucking blister Bruises Hematoma / Ecchymosis Battle's sign Raccoon eyes Black eye Subungual hematoma Cullen's sign Grey Turner's sign Retroperitoneal hemorrhage Animal bites Insect bite Spider bite Snakebite Other: Ballistic trauma Stab wound Blunt trauma /superficial/ closed Penetrating trauma / open Aerosol burn Burn / Corrosion / Chemical burn Frostbite Occupational injuries Traumatic amputation By region Hand injury Head injury Chest trauma Abdominal trauma v t e Consequences of external causes Temperature Elevated Hyperthermia Heat syncope Reduced Hypothermia Immersion foot syndromes Trench foot Tropical immersion foot Warm water immersion foot Chilblains Frostbite Aerosol burn Cold intolerance Acrocyanosis Erythrocyanosis crurum Radiation Radiation poisoning Radiation burn Chronic radiation keratosis Eosinophilic, polymorphic, and pruritic eruption associated with radiotherapy Radiation acne Radiation-induced cancer Radiation recall reaction Radiation-induced erythema multiforme Radiation-induced hypertrophic scar Radiation-induced keloid Radiation-induced morphea Air Hypoxia / Asphyxia Barotrauma Aerosinusitis Decompression sickness High altitude Altitude sickness Chronic mountain sickness Death zone HAPE HACE Food Starvation Maltreatment Physical abuse Sexual abuse Psychological abuse Travel Motion sickness Seasickness Airsickness Space adaptation syndrome Adverse effect Hypersensitivity Anaphylaxis Angioedema Allergy Arthus reaction Adverse drug reaction Other Electrical injury Drowning Lightning injuries Ungrouped skin conditions resulting from physical factors Dermatosis neglecta Pinch mark Pseudoverrucous papules and nodules Sclerosing lymphangitis Tropical anhidrotic asthenia UV-sensitive syndrome environmental skin conditions Electrical burn frictional/traumatic/sports Black heel and palm Equestrian perniosis Jogger's nipple Pulling boat hands Runner's rump Surfer's knots Tennis toe Vibration white finger Weathering nodule of ear Wrestler's ear Coral cut Painful fat herniation Uranium dermatosis iv use Skin pop scar Skin track Slap mark Pseudoacanthosis nigricans Narcotic dermopathy
-
Rectal Prolapse
Wikipedia
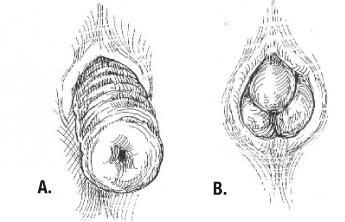
Contents 1 Classification 2 Diagnosis 2.1 History 2.2 Physical examination 2.3 Proctoscopy/sigmoidoscopy/colonoscopy 2.4 Videodefecography 2.5 Colonic transit studies 2.6 Anorectal manometry 2.7 Anal electromyography/Pudendal nerve testing 3 Complete rectal prolapse 3.1 Signs and symptoms 3.2 Cause 3.3 Treatment 3.3.1 Conservative 3.3.2 Surgical 3.3.2.1 Abdominal procedures 3.3.2.2 Perineal procedures 4 Internal rectal intussusception 4.1 Symptoms 4.2 Cause 4.3 Comorbidities and complications 4.4 Diagnosis 4.5 Treatment 4.5.1 laparoscopic ventral (mesh) rectopexy (LVR) 4.5.2 Stapled trans-anal rectal resection (STARR) 5 Mucosal prolapse 5.1 Symptoms 5.2 Cause 5.3 Diagnosis 5.4 Treatment 6 Solitary rectal ulcer syndrome and colitis cystica profunda 6.1 Symptoms 6.2 Prevalence 6.3 Cause 6.4 Complications 6.5 Diagnosis and investigations 6.6 Treatment 7 Mucosal prolapse syndrome 8 Pornography 9 Terminology 10 See also 11 References 12 External links Classification [ edit ] A . ... SRUS can be considered a consequence of internal intussusception, which can be demonstrated in 94% of cases. Mucosal prolapse syndrome (MPS) is recognized by some. It includes solitary rectal ulcer syndrome, rectal prolapse, proctitis cystica profunda, and inflammatory polyps. [16] [17] It is classified as a chronic benign inflammatory disorder. ... In mucosal prolapse, these folds are radially. [9] The folds in mucosal prolapse are usually associated with internal hemorrhoids. [20] Treatment [ edit ] EUA (examination under anesthesia) of anorectum and banding of the mucosa with rubber bands. Solitary rectal ulcer syndrome and colitis cystica profunda [ edit ] Solitary rectal ulcer syndrome (SRUS, SRU), is a disorder of the rectum and anal canal , caused by straining and increased pressure during defecation . ... Improvement with surgery is about 55-60%. [85] Ulceration may persist even when symptoms resolve. [86] Mucosal prolapse syndrome [ edit ] A group of conditions known as Mucosal prolapse syndrome (MPS) has now been recognized. ... "The clinical, endoscopic and histological spectrum of the solitary rectal ulcer syndrome: a single-center experience of 116 cases" .BMPR1A, RFC2, NSUN2, BCOR, MLXIPL, TBL2, TAB2, GTF2IRD1, BAZ1B, LTBP4, NAA10, CLIP2, CFTR, TGFB1, STK11, RPS6KA3, CCBE1, ELN, FCGR2A, GTF2I, LIMK1, LIG4, PTEN, REG1A, GAB2, BPIFA2, RAPH1, MRTFA, EPHB2, CRIM1, GPR4, FBLN5, RIDA, IL10, TCL1B, MMP1, TCL1A, MSMB, TNXB, TNXA, PLAU, MAPK1, STXBP3, PSPN, PSPH, TIMP1
-
Dysgeusia
Wikipedia
"Drug points: Dysgeusia and burning mouth syndrome by eprosartan" . BMJ . 325 (7375): 1277. doi : 10.1136/bmj.325.7375.1277 . ... Mann, MD, “Management of Smell and Taste Problems,” Cleveland Clinic Journal of Medicine Apr. 2002: 334. ^ Giuseppe Lauria, Alessandra Majorana, Monica borgna, Raffaella Lombardi, Paola Penza, Alessandro padovani, and Pierluigi Sapelli, “Trigeminal small-fiber sensory neuropathy causes burning mouth syndrome,” Pain 11 Mar. 2005: 332, 336. ^ Brand JG (October 2000). ... "Abnormalities of the blink reflex in burning mouth syndrome". Pain . 73 (3): 455–60. doi : 10.1016/S0304-3959(97)00140-1 . ... "Idiopathic hypogeusia with dysgeusia, hyposmia, and dysosmia. A new syndrome". JAMA . 217 (4): 434–40. doi : 10.1001/jama.1971.03190040028006 . ... PMID 19408460 . ^ a b c d Bromley, Steven M., "Smell and Taste Disorders: A Primary Care Approach," American Family Physician 15 Jan. 2000, 23 Oct. 2009 < http://www.aafp.org/afp/20000115/427.html > ^ a b c d Castells, Xavier, et al., "Drug Points: Dysgeusia and Burning Mouth Syndrome by Eprosartan," British Medical Journal , 30 Nov. 2002: 1277. ^ a b c d e f Sadasivam B, Jhaj R (February 2007).
-
Childhood Schizophrenia
Wikipedia
Unspecified psychoses with origin specific to childhood (code 299.9) in the International Classification of Diseases 9th revision (ICD-9) includes "child psychosis NOS", "schizophrenia, childhood type NOS" and "schizophrenic syndrome of childhood NOS". [15] "Childhood type schizophrenia" available in the Soviet adapted version of the ICD-9 (code 299.91) and the Russian adapted version of the 10th revision ICD-10 (code F20.8xx3). [16] Signs and symptoms [ edit ] Main article: Schizophrenia See also: Basic symptoms of schizophrenia Schizophrenia is a mental disorder that is expressed in abnormal mental functions and disturbed behavior. ... Several environmental factors , including perinatal complications and prenatal maternal infections could cause schizophrenia. [9] These factors in a greater severity or frequency could result in an earlier onset of schizophrenia. [9] Maybe a genetic predisposition is an important factor too, familial illness reported for childhood-onset schizophrenic patients. [20] Genetic [ edit ] There is "considerable overlap" in the genetics of childhood-onset and adult-onset schizophrenia, but in childhood-onset schizophrenia there is a higher number of "rare allelic variants". [21] An important gene for adolescent-onset schizophrenia is the catechol-O-methyltransferase gene , a gene that regulates dopamine . [22] Children with schizophrenia have an increase in genetic deletions or duplication mutations [ citation needed ] and some have a specific mutation called 22q11 deletion syndrome , which accounts for up to 2% of cases. [23] [24] Neuroanatomical [ edit ] Neuroimaging studies have found differences between the medicated brains of individuals with schizophrenia and neurotypical brains, though research does not know the cause of the difference. [25] In childhood-onset schizophrenia, there appears to be a faster loss of cerebral grey matter during adolescence. [25] [26] Studies have reported that adverse childhood experiences (ACEs) are the most preventable cause of the development of psychiatric disorders such as schizophrenia. ... He called the condition "dementia praecocissima" (Latin, "very premature madness"), by analogy to the term then used for schizophrenia, " dementia praecox " (Latin, "premature madness). [52] Sante de Sanctis characterized the condition by the presence of catatonia. [53] Philip Bromberg thinks that "dementia praecocissima" is in some cases indistinguishable from childhood schizophrenia, and Leo Kanner believed that "dementia praecocissima" encompassed a number of pathological conditions. [53] Theodor Heller discovered a new syndrome dementia infantilis (Latin, "infantile madness") in 1909 which was named Heller syndrome . [54] In ICD-11 Heller syndrome is classed as an autism spectrum subtype. [55] Also in 1909, Julius Raecke reported on ten cases of catatonia in children at the Psychiatric and Neurological Hospital of Kiel University , where he worked. ... PMID 24639636 . ^ Squarcione C, Torti MC, Di Fabio F, Biondi M (2013). "22q11 deletion syndrome: a review of the neuropsychiatric features and their neurobiological basis" . ... PMID 24102356 . v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Apathy
Wikipedia
Pathological apathy, characterised by extreme forms of apathy, is now known to occur in many different brain disorders, [2] including neurodegenerative conditions often associated with dementia such as Alzheimer's disease , [3] and psychiatric disorders such as schizophrenia . [4] Although many patients with pathological apathy also suffer from depression, several studies have shown that the two syndromes are dissociable: apathy can occur independently of depression and vice versa. [2] Contents 1 Etymology 2 History and other views 2.1 Technology 2.2 Social origin 2.3 In the school system 2.4 Bystander 2.5 Communication 3 Measurement of Apathy 3.1 Apathy Evaluation Scale 3.2 Apathy Motivation Index 3.3 Dimensional Apathy Scale 4 Medical aspects | Pathological apathy 4.1 Depression 4.2 Alzheimer's disease 4.3 Anxiety 4.4 Other 5 See also 6 Notes 7 References 8 External links Etymology [ edit ] Although the word apathy was first used in 1594 [5] and is derived from the Greek ἀπάθεια ( apatheia ), from ἀπάθης ( apathēs , "without feeling" from a- ("without, not") and pathos ("emotion")), [6] it is important not to confuse the two terms. ... In a Journal of Neuropsychiatry and Clinical Neurosciences article from 1991, Robert Marin, MD, claimed that pathological apathy occurs due to brain damage or neuropsychiatric illnesses such as Alzheimer's, Parkinson's, or Huntington's disease, stroke. Marin argues that apathy is a syndrome associated with many different brain disorders. [22] This has now been shown to be the case across a range of neurological and psychiatric conditions. [2] A review article by Robert van Reekum, MD, et al. from the University of Toronto in the Journal of Neuropsychiatry (2005) claimed that an obvious relationship between depression and apathy exists in some populations. [23] However, although many patients with depression suffer from apathy, several studies have shown that apathy can occur independently of depression, and vice versa. [2] Apathy can be associated with depression, a manifestation of negative disorders in schizophrenia, or a symptom of various somatic and neurological disorders. [24] [2] Alzheimer's disease [ edit ] Depending upon how it has been measured, apathy affects 19–88% percent of individuals with Alzheimer's disease (mean prevalence of 49% across different studies). [3] It is a neuropsychiatric symptom associated with functional impairment. ... It is also known to be a distinct psychiatric syndrome [ citation needed ] that is associated with many conditions, some of which are: CADASIL syndrome , depression , Alzheimer's disease , Chagas disease , Creutzfeldt–Jakob disease , dementia (and dementias such as Alzheimer's disease, vascular dementia, and frontotemporal dementia), Korsakoff's syndrome , excessive vitamin D , hypothyroidism , hyperthyroidism , general fatigue, Huntington's disease , Pick's disease , progressive supranuclear palsy (PSP), brain damage , schizophrenia , schizoid personality disorder , bipolar disorder , [ citation needed ] autism spectrum disorders, ADHD , and others. ... Solmitz Apathy – McMan's Depression and Bipolar Web, by John McManamy v t e Emotions ( list ) Emotions Acceptance Adoration Aesthetic emotions Affection Agitation Agony Amusement Anger Angst Anguish Annoyance Anticipation Anxiety Apathy Arousal Attraction Awe Boredom Calmness Compassion Confidence Contempt Contentment Courage Cruelty Curiosity Defeat Depression Desire Despair Disappointment Disgust Distrust Ecstasy Embarrassment Vicarious Empathy Enthrallment Enthusiasm Envy Euphoria Excitement Fear Flow (psychology) Frustration Gratification Gratitude Greed Grief Guilt Happiness Hatred Hiraeth Homesickness Hope Horror Hostility Humiliation Hygge Hysteria Indulgence Infatuation Insecurity Inspiration Interest Irritation Isolation Jealousy Joy Kindness Loneliness Longing Love Limerence Lust Mono no aware Neglect Nostalgia Outrage Panic Passion Pity Self-pity Pleasure Pride Grandiosity Hubris Insult Vanity Rage Regret Social connection Rejection Remorse Resentment Sadness Melancholy Saudade Schadenfreude Sehnsucht Self-confidence Sentimentality Shame Shock Shyness Sorrow Spite Stress Suffering Surprise Sympathy Tenseness Trust Wonder Worry World views Cynicism Defeatism Nihilism Optimism Pessimism Reclusion Weltschmerz Related Affect consciousness in education measures in psychology Affective computing forecasting neuroscience science spectrum Affectivity positive negative Appeal to emotion Emotion and art and memory and music and sex classification evolution expressed functional accounts group homeostatic perception recognition in conversation in animals regulation interpersonal work Emotional aperture bias blackmail competence conflict contagion detachment dysregulation eating exhaustion expression intelligence and bullying intimacy isolation lability labor lateralization literacy prosody reasoning responsivity security selection symbiosis well-being Emotionality bounded Emotions and culture in decision-making in the workplace in virtual communication history moral self-conscious social social sharing sociology Feeling Gender and emotional expression Group affective tone Interactions between the emotional and executive brain systems Meta-emotion Pathognomy Pathos Social emotional development Stoic passions Theory affect appraisal discrete emotion somatic marker constructed emotion v t e Narcissism Types Collective Egomania Flying monkeys Healthy Malignant Narcissistic personality disorder Spiritual Workplace Characteristics Betrayal Boasting Egocentrism Egotism Empathy (lack of) Envy Entitlement (exaggerated sense of) Fantasy Grandiosity Hubris Magical thinking Manipulative Narcissistic abuse Narcissistic elation Narcissistic rage and narcissistic injury Narcissistic mortification Narcissistic supply Narcissistic withdrawal Perfectionism Self-esteem Self-righteousness Shamelessness Superficial charm Superiority complex True self and false self Vanity Defences Denial Idealization and devaluation Distortion Projection Splitting Cultural phenomena Control freak Don Juanism Dorian Gray syndrome My way or the highway Selfie Related articles Codependency Counterdependency Dark triad Ego ideal "Egomania" (film) Egotheism Empire-building God complex History of narcissism Messiah complex Micromanagement Narcissism of small differences Narcissistic leadership Narcissistic parent Narcissistic Personality Inventory Narcissus (mythology) On Narcissism Sam Vaknin Self-love Self-serving bias Spoiled child The Culture of Narcissism Workplace bullyingGRN, TBK1, MAPT, ACAT1, DNAJC6, TARDBP, ATP13A2, DNAJC13, PARK7, SQSTM1, CHMP2B, VCP, UCHL1, SPAST, SNCA, PSEN1, ATXN10, GIGYF2, PRKAR1B, COQ2, HTRA2, TREM2, TMEM106B, VPS13C, VPS35, JPH3, PINK1, EHMT1, LRRK2, HGSNAT, C9orf72, TMEM240, CHCHD10, PRNP, SMARCB1, PODXL, CACNA1A, FUS, DNMT1, GBA, PDGFB, DCTN1, GM2A, HEXA, CSF1R, HLA-DQB1, HMGCL, EIF4G1, PRKN, APOE, MCIDAS, ACHE, CSF2, SLC6A4, LAMC2, TLE5, SLC6A3, COMT, DRD1, USH1G, AR, BDNF, PRX, DRD3, CRP, PRND, DRD4, CFLAR, SGCA, MSN, SOD1, MC4R, LIPA, TRPV1, IGFALS, ENPEP, ADAMTS2, RAPGEF4, MAPK8IP3, HCRT, SMUG1, TPSG1, NPS
-
Sarcoma
Wikipedia
Previous exposure to ionizing radiation (such as prior radiation therapy) is one such risk factor. [2] Exposure to alkylating agents, such as those found in certain cancer chemotherapeutic medicines , also increases the risk of bone sarcoma. [3] Certain inherited genetic syndromes, including Li-Fraumeni syndrome , heritable RB1 gene mutations, and Paget's disease of bone , are associated with an increased risk of developing bone sarcomas. [2] Most soft tissue sarcomas arise from what doctors call "sporadic" (or random) genetic mutations within an affected person's cells. [3] Nevertheless, there are certain risk factors associated with an increased risk of developing soft tissue sarcoma. Previous exposure to ionizing radiation is one such risk factor. [2] Exposure to vinyl chloride (e.g., such as the fumes encountered in the production of Polyvinyl chloride (PVC)), Arsenic and Thorotrast all are associated with an increased risk of angiosarcoma. [2] [3] Lymphedema, such as that resulting from certain types of breast cancer treatment, also is a risk factor for development of angiosarcoma. [3] As with bone sarcomas, certain inherited genetic syndromes also are associated with an increased risk of developing soft tissue sarcoma, including Li-Fraumeni syndrome , familial adenomatous polyposis , neurofibromatosis type 1 , and heritable RB1 gene mutations. [3] Kaposi's sarcoma is caused by Kaposi's sarcoma-associated herpesvirus (HHV-8). ... Sarcoma Help from the Liddy Shriver Sarcoma Initiative Classification D ICD-O : M8800/3 MeSH : D012509 SNOMED CT : 424413001 v t e Connective / soft tissue tumors and sarcomas Not otherwise specified Soft-tissue sarcoma Desmoplastic small-round-cell tumor Connective tissue neoplasm Fibromatous Fibroma / fibrosarcoma : Dermatofibrosarcoma protuberans Desmoplastic fibroma Fibroma / fibromatosis : Aggressive infantile fibromatosis Aponeurotic fibroma Collagenous fibroma Diffuse infantile fibromatosis Familial myxovascular fibromas Fibroma of tendon sheath Fibromatosis colli Infantile digital fibromatosis Juvenile hyaline fibromatosis Plantar fibromatosis Pleomorphic fibroma Oral submucous fibrosis Histiocytoma / histiocytic sarcoma : Benign fibrous histiocytoma Malignant fibrous histiocytoma Atypical fibroxanthoma Solitary fibrous tumor Myxomatous Myxoma / myxosarcoma Cutaneous myxoma Superficial acral fibromyxoma Angiomyxoma Ossifying fibromyxoid tumour Fibroepithelial Brenner tumour Fibroadenoma Phyllodes tumor Synovial -like Synovial sarcoma Clear-cell sarcoma Lipomatous Lipoma / liposarcoma Myelolipoma Myxoid liposarcoma PEComa Angiomyolipoma Chondroid lipoma Intradermal spindle cell lipoma Pleomorphic lipoma Lipoblastomatosis Spindle cell lipoma Hibernoma Myomatous general: Myoma / myosarcoma smooth muscle : Leiomyoma / leiomyosarcoma skeletal muscle : Rhabdomyoma / rhabdomyosarcoma : Embryonal rhabdomyosarcoma Sarcoma botryoides Alveolar rhabdomyosarcoma Leiomyoma Angioleiomyoma Angiolipoleiomyoma Genital leiomyoma Leiomyosarcoma Multiple cutaneous and uterine leiomyomatosis syndrome Multiple cutaneous leiomyoma Neural fibrolipoma Solitary cutaneous leiomyoma STUMP Complex mixed and stromal Adenomyoma Pleomorphic adenoma Mixed Müllerian tumor Mesoblastic nephroma Wilms' tumor Malignant rhabdoid tumour Clear-cell sarcoma of the kidney Hepatoblastoma Pancreatoblastoma Carcinosarcoma Mesothelial Mesothelioma Adenomatoid tumor v t e Tumours of bone and cartilage Diaphysis Multiple myeloma Epithelia Adamantinoma Primitive neuroectodermal tumor Ewing family Ewing's sarcoma Metaphysis Osteoblast Osteoid osteoma Osteoblastoma Osteoma / osteosarcoma Chondroblast Chondroma / ecchondroma / enchondroma Enchondromatosis Extraskeletal chondroma Chondrosarcoma Mesenchymal chondrosarcoma Myxoid chondrosarcoma Osteochondroma Osteochondromatosis Chondromyxoid fibroma Fibrous Ossifying fibroma Fibrosarcoma Epiphysis Chondroblast Chondroblastoma Myeloid Giant-cell tumor of bone Other Notochord Chordoma v t e Tumours of blood vessels Blood vessel Hemangiosarcoma Blue rubber bleb nevus syndrome Hemangioendothelioma Composite Endovascular papillary Epithelioid Kaposiform Infantile Retiform ) Spindle cell Proliferating angioendotheliomatosis Hemangiopericytoma Venous lake Kaposi's sarcoma African cutaneous African lymphadenopathic AIDS-associated Classic Immunosuppression-associated Hemangioblastoma Hemangioma Capillary Cavernous Glomeruloid Microvenular Targeted hemosiderotic Angioma Cherry Seriginosum Spider Tufted Universal angiomatosis Angiokeratoma of Mibelli Angiolipoma Pyogenic granuloma Lymphatic Lymphangioma / lymphangiosarcoma Lymphangioma circumscriptum Acquired progressive lymphangioma PEComa Lymphangioleiomyomatosis Cystic hygroma Multifocal lymphangioendotheliomatosis Lymphangiomatosis Either Angioma / angiosarcoma Angiofibroma Authority control BNE : XX526877 BNF : cb11982790q (data) GND : 4179127-7 LCCN : sh85117504
-
Dementia
Wikipedia
Regions showing loss of volume include the frontal, temporal, and parietal lobes, the cerebellum, thalamus, and hippocampus. [55] This loss can be more notable, with greater cognitive impairments seen in those aged 65 years and older. [55] Other conditions [ edit ] Chronic inflammatory conditions that may affect the brain and cognition include Behçet's disease , multiple sclerosis , sarcoidosis , Sjögren's syndrome , systemic lupus erythematosus , celiac disease , and non-celiac gluten sensitivity . [56] [57] These types of dementias can rapidly progress, but usually have a good response to early treatment. ... For example, a proportion of patients with Parkinson's disease develop dementia, though widely varying figures are quoted for this proportion. [61] When dementia occurs in Parkinson's disease, the underlying cause may be dementia with Lewy bodies or Alzheimer's disease , or both. [62] Cognitive impairment also occurs in the Parkinson-plus syndromes of progressive supranuclear palsy and corticobasal degeneration (and the same underlying pathology may cause the clinical syndromes of frontotemporal lobar degeneration ). ... Limbic-predominant age-related TDP-43 encephalopathy (LATE) is a type of dementia that primarily affects people in their 80s or 90s and in which TDP-43 protein deposits in the limbic portion of the brain. [63] Aside from those mentioned above, heritable conditions that can cause dementia (alongside other symptoms) include: [64] Dentatorubral-pallidoluysian atrophy Epilepsy Fatal familial insomnia Fragile X-associated tremor/ataxia syndrome Glutaric aciduria type 1 Various leukodystrophies Maple syrup urine disease Niemann–Pick disease type C Neuronal ceroid lipofuscinosis Neuroacanthocytosis Organic acidemias Sanfilippo syndrome type B Spinocerebellar ataxia type 2 Urea cycle disorders Slowly progressive [ edit ] Dementia that begins gradually and worsens over several years is usually caused by neurodegenerative disease —that is, by conditions that affect only or primarily brain neurons and cause gradual but irreversible loss of function. ... Frontotemporal lobar degeneration and Huntington's disease account for most of the remaining cases. [68] Vascular dementia also occurs, but this in turn may be due to underlying conditions (including antiphospholipid syndrome , CADASIL , MELAS , homocystinuria , moyamoya , and Binswanger's disease ). ... Certain animals may also be regarded as “unclean” or “dangerous” by some cultural groups. [140] Medications [ edit ] Donepezil No medications have been shown to prevent or cure dementia. [142] Medications may be used to treat the behavioural and cognitive symptoms, but have no effect on the underlying disease process. [12] [143] Acetylcholinesterase inhibitors , such as donepezil , may be useful for Alzheimer disease [144] and dementia in Parkinson's, DLB, or vascular dementia. [143] The quality of the evidence is poor [145] and the benefit is small. [9] No difference has been shown between the agents in this family. [16] In a minority of people side effects include a slow heart rate and fainting . [146] Rivastigmine is recommended for treating symptoms in Parkinson's disease dementia. [147] Before prescribing antipsychotic medication in the elderly, an assessment for an underlying cause of the behavior is needed. [148] Severe and life-threatening reactions occur in almost half of people with DLB, [51] [149] and can be fatal after a single dose. [150] People with Lewy body dementias who take neuroleptics are at risk for neuroleptic malignant syndrome, a life-threatening illness. [151] Extreme caution is required in the use of antipsychotic medication in people with DLB because of their sensitivity to these agents. [50] Antipsychotic drugs are used to treat dementia only if non-drug therapies have not worked, and the person's actions threaten themselves or others. [152] [153] [14] [154] Aggressive behavior changes are sometimes the result of other solvable problems, that could make treatment with antipsychotics unnecessary. [152] Because people with dementia can be aggressive, resistant to their treatment, and otherwise disruptive, sometimes antipsychotic drugs are considered as a therapy in response. [152] These drugs have risky adverse effects, including increasing the person's chance of stroke and death. [152] Given these adverse events and small benefit antipsychotics are avoided whenever possible. [137] Generally, stopping antipsychotics for people with dementia does not cause problems, even in those who have been on them a long time. [155] N-methyl-D-aspartate (NMDA) receptor blockers such as memantine may be of benefit but the evidence is less conclusive than for AChEIs. [156] Due to their differing mechanisms of action memantine and acetylcholinesterase inhibitors can be used in combination however the benefit is slight. [157] [158] While depression is frequently associated with dementia, selective serotonin reuptake inhibitors (SSRIs) do not appear to affect outcomes. [159] [160] The SSRIs sertraline and citalopram have been demonstrated to reduce symptoms of agitation, compared to placebo. [161] The use of medications to alleviate sleep disturbances that people with dementia often experience has not been well researched, even for medications that are commonly prescribed. [162] In 2012 the American Geriatrics Society recommended that benzodiazepines such as diazepam , and non-benzodiazepine hypnotics , be avoided for people with dementia due to the risks of increased cognitive impairment and falls. [163] Additionally, little evidence supports the effectiveness of benzodiazepines in this population. [162] [164] No clear evidence shows that melatonin or ramelteon improves sleep for people with dementia due to Alzheimer's, [162] but it is used to treat REM sleep behavior disorder in dementia with Lewy bodies. [51] Limited evidence suggests that a low dose of trazodone may improve sleep, however more research is needed. [162] No solid evidence indicates that folate or vitamin B12 improves outcomes in those with cognitive problems. [165] Statins have no benefit in dementia. [166] Medications for other health conditions may need to be managed differently for a person who has a dementia diagnosis.TREM2, APP, MAPT, PRNP, NOTCH3, GRN, PSEN2, CST3, DNMT1, CP, HTRA1, FUS, TYROBP, SLC6A3, CSF1R, COL4A1, SLC9A8, C9orf72, ITM2B, APOE, LRRK2, SNCA, PSEN1, VCP, CHMP2B, ATP13A2, SNCB, FMR1, SPAST, GBA, PINK1, SERPINI1, TTR, NOS3, TBP, TMEM106B, ARSA, ATXN2, JPH3, OPA1, SNCAIP, WDR45, ABCD1, NPC2, C19orf12, TRPM7, COX2, SPG21, NPC1, IRF6, NAGLU, AARS2, CLN6, DCTN1, CISD2, MECP2, PPP2R2B, HTT, CERS1, EIF4G1, SDHB, ATN1, ATP7B, EPM2A, HFE, CTSF, MPO, ATXN3, DNAJC5, SMOX, RNF216, GBE1, FTL, ATP6, AMN, VPS13C, APTX, LAMC2, PANK2, GLUD2, IGFALS, VPS35, GM2A, ROGDI, TWNK, HEXA, PRDM8, IL6, HLA-DQB1, IRF2BPL, IL1B, GBA2, TRNC, ADA2, COX1, SDHD, BACE1, PSAP, SMUG1, ATP6V0A2, NECTIN2, ALDH18A1, TARDBP, DNAJC13, ATXN8OS, SDHA, SLC2A3, ATXN10, TREX1, SOD1, PNPLA6, TUBB4A, TNF, DNM1L, MATR3, WFS1, CUBN, XPR1, FBXO7, POLG, COX3, TRNS2, CYTB, ND1, ND5, ND6, TRNE, TRNF, TRNK, TRNL1, TRNQ, TRNS1, TRNV, MMACHC, TRNW, NDP, NEFL, MBTPS2, NR4A2, RRM2B, PRDX1, PDGFB, PLAU, GIGYF2, OSBPL1A, A2M, TYMP, ASAH1, PRICKLE1, ACE, KCTD7, ACHE, MCIDAS, TIMM8A, CRP, BDNF, CYP27A1, DGUOK, SCARB2, CSF2, CSTB, SLC13A5, ATP6V1A, CDR1, ATP6V1E1, ADH1C, ERCC8, SDHAF1, CLN3, ESR1, BCHE, NHLRC1, CHI3L1, COMT, CLU, IGF1, IL1A, SERPINA3, MTHFR, PAEP, RUNX1T1, PON1, ITIH4, NHS, LEP, AKR1C4, UBQLN2, CCL2, ALB, DYRK1A, SLC6A4, CIT, DPP4, IDE, ABCB6, COPD, NRGN, GFAP, ADIPOQ, SORL1, SIRT1, AGER, CHRNA4, ST3GAL4, CHRNA7, SQSTM1, BCL2, APOC1, AGPS, TSHZ1, TGFB1, SCD, MCF2L, LRP2, ADAMTS2, CHAT, PRKN, CYP19A1, NDUFAB1, CETP, ALDH2, TOMM40, CYP2D6, BPIFA4P, FASTK, NGF, MME, MOK, IAPP, IGF1R, DHDDS, SERPINA1, HTR6, STH, ICAM1, S100B, VCAM1, APOA1, WWC1, IL10, SUCLA2, IL1RN, PLA2G7, CPAT1, MIR132, ATM, CCL4, PPARG, CXCL12, PART1, ERVW-1, ATP2B3, EBP, RELN, OPN1SW, REN, SEC14L2, MIR659, TGDS, TXNIP, RAB3A, NF1, APOB, MIR155, AKT1, PDC, SLC18A3, SERPINE1, PAFAH1B1, PDYN, SNAP25, SNCG, CHCHD10, SLC1A3, ABCB1, SLC1A2, NOS2, SHBG, SGCA, SFTPC, PIN1, PARK7, STAR, EDAR, REM1, TBK1, MMP9, SLC30A6, CHRFAM7A, TPI1, GAP43, USO1, GCG, IL18, TRPM2, PLA2G6, SPG11, GLS, SLC17A7, DBN1, ASXL1, PICALM, AKAP6, ACTB, AGTR1, GDF15, HTR2A, ERVK-6, HSD11B1, DRD3, YWHAE, DLG4, ERVK-32, SIGMAR1, INSRR, TIMP1, MTOR, FLNB, MMP2, ESR2, MFGE8, THBS1, TET2, NXF1, TAS2R62P, MAOA, SF3B1, KL, SPTLC1, EPO, ERVK-20, ABCA1, LPA, ABCA7, JAG1, MMP3, CCL4L2, LGI1, AD10, H6PD, H3P28, TRIM2, ASTN2, FAM72A, ATG5, UBR4, TAOK2, FHL5, NCSTN, GRAP2, LIPG, PHLPP1, CYTIP, FPGT-TNNI3K, NBEAL2, RABEPK, MCI2, AD16, MIR2113, LANCL1, ADAMTS13, CNMD, SDS, EBNA1BP2, SPON1, CFDP1, OLFM1, PPARGC1A, NES, FAS-AS1, CRTAP, RIDA, WDHD1, SIRT2, WIF1, ABCG1, FASTKD2, ACOT7, MTCO2P12, RAPGEF5, AD17, PGR-AS1, RBM8A, ZGLP1, CCS, AD11, GNE, WASF2, ERVK-18, MPZL2, LRRC37A, SLCO6A1, FAM72B, ACE2, ANKK1, PCSK9, KIDINS220, PLEKHG5, AICDA, MCOLN1, TIGAR, SLC17A6, PDXP, ACKR3, CHPT1, MRGPRX1, FMN2, RETN, ASAH2, USE1, MBD5, ATF7IP, ADI1, SLC52A1, MARCHF1, HCCAT5, INTS11, DYM, ARHGEF2, ARMH1, NANOS3, ACTBL2, PWAR4, HAMP, LGR6, CABIN1, CLSTN2, MRGPRX3, ESCO1, CSMD2, NLRP3, TMEM54, ATPAF2, GPR151, SHANK3, BPIFA2, CACUL1, COL25A1, TOM1L2, PPP1R2C, NAA50, OXER1, RIN3, EHMT1, DHX40, PTCRA, FTO, UBE2Z, WNK1, GPRC6A, CSMD1, CIAO3, HHIP, ROBO3, FNDC5, ABCG4, GSTK1, SERPINA13P, DNAJC10, CCL4L1, CYFIP2, SLC17A5, SEZ6L2, HSPB8, FBXW8, PTPN22, VN1R17P, LRP10, GPR166P, PLF, SH2B1, MIR384, BACE2, BDNF-AS, PRDX5, TPSG1, MIR193B, GCA, BRI3, QPCT, NPS, POTEM, LOC643387, CD2AP, KLHDC2, DDX58, PADI4, LPAR3, LINC00273, GLS2, POTEKP, SIT1, MIR21, MIRLET7B, MIR106B, MIR107, MIR125A, POLE3, INPP5K, WWOX, UBR5, PLA1A, MIR181C, MIR195, MIR206, CHCHD2, SAR1B, HPGDS, TNNI3K, GEMIN4, MIR210, IL22, DELEC1, NOX4, MIR212, MIR223, KCNIP3, CD274, MIR29A, MRGPRX4, PYCARD, SLC33A1, CCL21, HGS, HHEX, GHR, CBLIF, GCLC, GLP1R, GLRA2, GPR39, GRK5, GPX1, GPX4, GRIN2B, NR3C1, GSK3B, GYPC, HARS1, HDAC2, GH1, GDNF, GDF1, PTK2B, EIF4G2, ELF3, EPHX2, F2RL1, F11, FANCD2, FANCB, GAPDH, FDXR, FOXO3, FLT1, FN1, FOLH1, G6PD, HGF, HLA-C, LRPAP1, HMGB1, IL12B, IL13, IL15, IL17A, CXCL10, INPP5D, INSR, IRS1, ITGB2, KNG1, LAD1, RPSA, LIMK1, LMNA, LPL, IL12A, IL9, CXCL8, IDH2, HMOX1, HP, HSF1, HSPG2, HTR1A, IDH1, IFNG, IL7, IGF2, IGFBP2, IGFBP3, IKBKB, IL4, IL6R, EGFR, EEF1A2, EDN1, ECE1, BAX, BCL2A1, DST, BRCA1, BRCA2, TSPO, SERPING1, CA11, CASP1, CASP2, CASP6, CAV1, CBS, CCT, CD4, BACH1, ATR, ATP7A, AGT, ACTG1, ACTG2, ACY1, ADA, ADAM10, ADSL, AGTR2, APOC3, AHR, AKR1B1, ALK, BIN1, ANGPT1, ANXA1, CD14, CD38, CDKN1A, DIH1, CSF3, CSPG4, CTSB, CTSD, CUX1, DAG1, DLD, CREB1, SARDH, DPP6, DRD2, DSC3, DSPP, E2F1, CRYGD, CPE, CDR2, CHD2, CEACAM5, CEBPB, CECR, CGA, CEACAM3, CEACAM7, CHIT1, COL4A2, CHM, CHRM1, CHRNB2, TPP1, CCR5, CNR1, LRP5, LY6E, F2RL3, TLR2, SST, ST13, STAT1, STC1, STXBP3, SULT1A1, SYP, TAC1, TBCA, TCEA1, TFAM, TFPI, TGFB2, THOP1, TIMP2, SREBF1, SPP1, SORD, SELP, CCL3, CCL11, NAT2, CX3CL1, SEL1L, SELE, SET, SOD2, SFPQ, SRSF5, SLC5A2, SMARCA1, SMPD1, SNTA1, TIMP4, TLR4, MAP2, CLDN5, TFEB, NTT, NUP214, FGF23, CNSN, COLQ, FZD4, SRPX, BHLHE40, STK16, TP63, FADD, NR1I2, SYNJ1, WASF1, DEK, CXCR4, LRP8, TYRP1, TNNI3, TP53, TPO, HSP90B2P, TSC2, TYMS, UBB, VWF, UBE2H, UCHL1, UGCG, NR1H2, UROD, VLDLR, ATXN1, RPL29, BRD2, REG1A, NTRK2, NTS, OXT, P2RY11, P4HB, PEBP1, REG3A, PAWR, SERPINA5, PDE9A, SLC26A4, PENK, PER1, PFN1, PGF, NPTX2, NOTCH4, NOS1, MTR, SMCP, MDM2, MDM4, MEF2C, MSD, MSMB, MYLK, NINJ2, NDUFS3, NFIA, NFATC3, NFIB, NFIC, NFIX, PIK3CA, PIK3CB, PIK3CD, PTGS2, KLK10, PSG2, PSMD2, PSMD7, PSPH, PTH, PTHLH, PSPN, PTK2, PZP, RAP1GDS1, PLAAT4, RBP4, RCN1, KLK7, MAPK3, PIK3CG, PNN, PITX2, PITX3, PKNOX1, PLAUR, PLD1, PLP1, POLE, MAPK1, PON2, PPARA, PPP3CA, PREP, PRKAR1B, PRKCB, H3P11
-
Peripheral Neuropathy
Wikipedia
The most common cause of mononeuropathy is physical compression of the nerve, known as compression neuropathy . Carpal tunnel syndrome and axillary nerve palsy are examples. ... Causes of neuritis include: Physical injury Infection Diphtheria Herpes zoster (shingles) Leprosy Lyme disease Chemical injury such as chemotherapy Radiation therapy Types of neuritis include: Brachial neuritis Cranial neuritis such as Bell's palsy Optic neuritis Vestibular neuritis Wartenberg's migratory sensory neuropathy Underlying conditions including: : Alcoholism Autoimmune disease, especially multiple sclerosis and Guillain–Barré syndrome Beriberi ( vitamin B1 deficiency) Cancer Celiac disease [24] Non-celiac gluten sensitivity [7] Diabetes mellitus ( Diabetic neuropathy ) Hypothyroidism Porphyria Vitamin B12 deficiency Vitamin B6 excess [25] Signs and symptoms [ edit ] Those with diseases or dysfunctions of their nerves may present with problems in any of the normal nerve functions. ... Peripheral neuropathies also may result from long term (more than 21 days) treatment with linezolid. [ medical citation needed ] Adverse effects of fluoroquinolones : irreversible neuropathy is a serious adverse reaction of fluoroquinolone drugs [35] Inflammatory diseases: Guillain–Barré syndrome , [31] systemic lupus erythematosus , leprosy , multiple sclerosis , [31] Sjögren's syndrome , Babesiosis , Lyme disease , [31] vasculitis , [31] sarcoidosis , [36] Vitamin deficiency states: Vitamin B 12 (Methylcobalamin), [31] vitamin A , vitamin E , vitamin B 1 (thiamin) Physical trauma: compression , automobile accident, sports injury, sports pinching, cutting, projectile injuries (for example, gunshot wound), strokes including prolonged occlusion of blood flow, electric discharge, including lightning strikes [ medical citation needed ] Effect of chemotherapy – see Chemotherapy-induced peripheral neuropathy [31] Exposure to Agent Orange [37] Others: electric shock , HIV , [31] [38] malignant disease, radiation , shingles , MGUS ( Monoclonal gammopathy of undetermined significance ). [39] Diagnosis [ edit ] Peripheral neuropathy may first be considered when an individual reports symptoms of numbness, tingling, and pain in feet. ... During physical examination , specifically a neurological examination , those with generalized peripheral neuropathies most commonly have distal sensory or motor and sensory loss, although those with a pathology (problem) of the nerves may be perfectly normal; may show proximal weakness, as in some inflammatory neuropathies, such as Guillain–Barré syndrome ; or may show focal sensory disturbance or weakness, such as in mononeuropathies. ... Also, the authors state, "we did not identify any study comparing acupuncture with treatment as usual." [100] A 2018 Cochrane review on acupuncture and related interventions for the treatment of carpal tunnel syndrome concluded that, "Acupuncture and laser acupuncture may have little or no effect in the short term on symptoms of carpal tunnel syndrome (CTS) in comparison with placebo or sham acupuncture."ARTN, TLR3, LTC4S, NEFL, PMP2, LMNA, TYMP, NGLY1, CHRNG, COX6A1, IARS2, SPTLC3, ATAD3A, GJB1, QRICH1, BRAF, PEX5, PMP22, KIF1A, DNAJB5, TPI1, TTR, ABCC6, PEX11B, MFN2, HSPB1, CEP72, TNF, GJB3, NFE2L2, SARM1, ABCB1, PRNP, LY6E, AIFM1, SPTLC1, DNM2, TRPV4, MPZ, TRPV1, BDNF, ATXN2, SACS, IL10, VEGFA, FIG4, APOE, GABPA, FXN, YARS1, HMGB1, POLG, HARS1, APTX, GPT, PLP1, PRPS1, NGF, KIF1B, CYP3A5, MMP9, MTM1, SLC12A6, HDAC6, PIK3CA, ATXN3, LITAF, ACTG1, AKR1A1, SIGMAR1, HFE, HGF, HSPB8, IFNG, NAMPT, SETX, AFP, IGF1, ARHGEF10, LAMC2, IL6, AIRE, PIK3CB, AKR1B1, KIF5A, ITIH4, SBF2, S100B, PIK3CD, CSF2, PRKCB, KMT2D, PIK3CG, EGFR, PRRT2, MAPK14, ACE, ST3GAL4, REEP1, MTMR2, MYH14, CYP2C8, SPG11, REN, PRKCA, GSTP1, NDRG1, PMM2, ZBTB17, GARS1, GFER, SLC22A4, CAV3, GFAP, ABCG1, AIMP2, TP53, TSFM, RAB7A, NR1I2, EIF2B5, TFG, TUBB3, XPA, HSPB3, TYMS, SCO2, LRIG2, TRPA1, SPTLC2, MYOT, GRAP2, VCP, CST7, ELP1, DCLRE1A, CUL4B, MAD2L1BP, FHL5, SERPINA3, SEMA4D, EHMT1, CYP2U1, SCA18, C12orf65, SLC25A46, DGAT2, TUBB1, SH3TC2, NIPA1, WNK1, EBF2, INF2, VSIR, PRX, EP400, FGD4, CPT1C, MFF, MIR29A, ZGLP1, SPG36, D2HGDH, POTEM, MIR381, POTEKP, MIR146A, TCHHL1, GSTK1, ACTBL2, LAMA1, EPGN, NRG4, SLCO6A1, SCYL1, SEPTIN3, FBLN5, RPIA, HARS2, TRIM2, AGTPBP1, RHOBTB2, MCF2L2, NMNAT2, RAB3GAP1, THBD, ACOT7, IMMT, SEPTIN9, RAI1, AVIL, AHSA1, FBXO7, POLDIP2, NLRP2, PTRH2, MEG3, SLC47A1, ANO10, KRT20, GDAP1, TREM2, CRBN, KIFBP, ATL1, DHH, SOX8, CD274, DBNL, FGF21, RNF19A, MAPK1, THAS, PTK2B, GHSR, GCG, FOLR1, FGF14, FGF2, FAP, FAAH, DES, F2RL1, EPO, ENO2, CTTN, EGR2, DYNC1I1, GLA, GLP1R, PRLHR, GPX1, GRIN1, GRIN2A, GRIN2B, CXCL1, GSK3B, GSTM1, GSTT1, HADHA, HINT1, HMBS, HSPB2, IFRD1, IGFALS, DLG4, DDIT3, IL1B, FAS, CD86, MS4A1, CCNH, CAPG, BMP7, ARSA, ANK1, DAG1, ALOX15, ABCD1, ALB, AGRP, ACTG2, ACTB, TNFRSF8, CD59, LTB4R, CNR2, CRK, CRP, CSF1R, CSF3, CST3, CCN2, CTLA4, CTNNB1, CTSS, CX3CR1, CYP2E1, CYP3A4, CYP17A1, IGHMBP2, IL1RN, TGFB1, PRTN3, SBF1, RARRES2, PTPN13, PTK2, PTEN, PSMB1, PRPH, OPA1, AARS1, POU3F1, ABCB4, PGR, PDK3, PRKN, ATXN1, ATXN7, SCN2A, SCN4A, SCN9A, CCL4, SLC22A5, SOD1, SOX10, SOX11, SPAST, SPR, STK11, SURF1, TACR1, TCF4, TCN2, P2RX3, NOTCH1, IL2, KDR, SMAD3, LYZ, LRP1, LEP, LDLR, LAMA2, KARS1, NOS1, INS, CXCR2, IL9, CXCR1, CXCL8, IL4, MAG, MAP1B, MAP4, MAPT, MPO, MPV17, ATP6, CYTB, MTHFR, ND2, ND5, MTR, MYD88, MYO5A, NAIP, NCAM1, NGFR, GJE1
-
Crohn's Disease
Wikipedia
This same gene may reduce innate and adaptive immunity in gastrointestinal tissue and impair the ability to resist infection by the MAP bacterium. [93] Macrophages that ingest the MAP bacterium are associated with high production of TNF-α . [94] [95] Other studies have linked specific strains of enteroadherent E. coli to the disease. [96] Adherent-invasive Escherichia coli (AIEC), are more common in people with CD, [97] [98] [96] have the ability to make strong biofilms compared to non-AIEC strains correlating with high adhesion and invasion indices [99] [100] of neutrophils and the ability to block autophagy at the autolysosomal step, which allows for intracellular survival of the bacteria and induction of inflammation. [101] Inflammation drives the proliferation of AIEC and dysbiosis in the ileum, irrespective of genotype. [102] AIEC strains replicate extensively inside macrophages inducing the secretion of very large amounts of TNF-α. [103] Mouse studies have suggested some symptoms of Crohn's disease, ulcerative colitis, and irritable bowel syndrome have the same underlying cause. Biopsy samples taken from the colons of all three patient groups were found to produce elevated levels of a serine protease . [104] Experimental introduction of the serine protease into mice has been found to produce widespread pain associated with irritable bowel syndrome, as well as colitis, which is associated with all three diseases. [105] Regional and temporal variations in those illnesses follow those associated with infection with the protozoan Blastocystis . [106] The "cold-chain" hypothesis is that psychrotrophic bacteria such as Yersinia and Listeria species contribute to the disease. ... In some cases, however, it may not be possible to tell the difference, in which case the disease is classified as indeterminate colitis. [1] [25] [26] Diagnostic findings Crohn's disease Ulcerative colitis Terminal ileum involvement Commonly Seldom Colon involvement Usually Always Rectum involvement Seldom Usually (95%) [65] Involvement around the anus Common [21] Seldom Bile duct involvement No increase in rate of primary sclerosing cholangitis Higher rate [152] Distribution of disease Patchy areas of inflammation (skip lesions) Continuous area of inflammation [65] Endoscopy Deep geographic and serpiginous (snake-like) ulcers Continuous ulcer Depth of inflammation May be transmural, deep into tissues [21] [153] Shallow, mucosal Stenosis Common Seldom Granulomas on biopsy May have non- necrotizing non-peri- intestinal crypt granulomas [21] [154] [155] Non-peri- intestinal crypt granulomas not seen [156] Differential diagnosis [ edit ] Other conditions with similar symptoms as Crohn's disease includes intestinal tuberculosis , Behçet's disease , ulcerative colitis , nonsteroidal anti-inflammatory drug enteropathy, irritable bowel syndrome and celiac disease . [4] Irritable bowel syndrome is excluded when there are inflammatory changes. [4] Celiac disease cannot be excluded if specific antibodies ( anti-transglutaminase antibodies ) are negative, [157] [158] nor in absence of intestinal villi atrophy. [159] [160] Management [ edit ] Main article: Management of Crohn's disease Management Crohn's disease Ulcerative colitis Mesalazine Less useful [161] More useful [161] Antibiotics Effective in long-term [162] Generally not useful [163] Surgery Often returns following removal of affected part Usually cured by removal of colon There is no cure for Crohn's disease and remission may not be possible or prolonged if achieved. ... Based on the score, treatment plans can be designed to give the patient the best chance of managing recurrence of the disease. [182] Short bowel syndrome (SBS, also short gut syndrome or simply short gut) is caused by the surgical removal of part of the small intestine. It usually develops in those patients who have had half or more of their small intestines removed. [183] Diarrhea is the main symptom, but others may include weight loss, cramping, bloating, and heartburn . Short bowel syndrome is treated with changes in diet, intravenous feeding, vitamin and mineral supplements, and treatment with medications.TNF, IL10, NR1H4, NCF4, CRP, NOD2, FUT2, HLA-DRB1, MST1, PPARG, NLRP3, ERAP2, MTHFR, BACH2, PPARA, CCL2, PTPN2, ATG16L1, LEP, TLR9, SLC11A1, TCF7, TLR4, TYK2, VTN, ADIPOQ, SMAD3, PHOX2B, TAGAP, GPBAR1, IRGM, FAM92B, DNMT3A, FPR2, CCNY, DENND1B, NKX2-3, FN1, IL23R, IGF1, IL2RA, IL6, IFNG, IL12B, PTGS2, MADCAM1, TNFRSF1A, EFS, TNFRSF1B, PIKFYVE, DEFB4B, LYZ, DEFB4A, DEFB103A, XPR1, FGF19, DEFB103B, TRIM22, SOCS3, FFAR4, CCR9, ACAD8, IL22, PLB1, BRAF, STAT4, NR0B2, YWHAZ, CHUK, CCN2, DEFA5, DEFB1, FGF7, GH1, GUCA2A, GUCA2B, GUCY2C, HPS1, CXCL8, INPP5D, KRAS, MLH1, COX2, NFKBIA, NRAS, PLA2G1B, PTPN11, CCL25, STAT3, CEACAM4, MAP3K7, TGFB1, TGFB2, NR2C2, TTR, MTCO2P12
-
Multiple Acyl-Coa Dehydrogenase Deficiency
Gene_reviews
In those who survive the neonatal period, recurrent metabolic decompensation resembling Reye syndrome and the development of hypertrophic cardiomyopathy can occur. ... Those who do survive usually die later in infancy either due to hypertrophic cardiomyopathy or recurrence of metabolic decompensation resembling Reye syndrome. Late Onset (Type III) This is the most common presentation. ... Rapidly progressive proximal myopathy and respiratory failure may mimic Guillain-Barre syndrome (GBS) [Hong et al 2018]. It is important to consider MADD in such scenarios, as early initiation of treatment with riboflavin may lead to complete resolution of symptoms in individuals with MADD. ... Individuals with MADD are at risk of developing rhabdomyolysis, which may manifest during the acute episode of metabolic decompensation [Prasad & Hussain 2015]. Bent spine syndrome characterized by progressive forward flexion of the trunk caused by selective involvement of paravertebral muscles has also been reported [Peng et al 2015]. ... SLC52A1 Transient MADD-like illness in neonates (OMIM 615026) AD Neonatal presentation w/poor feeding, lethargy, hypotonia, hypoglycemia, & hyperammonemia similar to neonatal-onset MADD 2 Biochemical profile similar to MADD Transient presentation & dramatic improvement w/riboflavin supplementation May be secondary to maternal heterozygous pathogenic variant → maternal riboflavin deficiency & secondary neonatal riboflavin deficiency 3 SLC52A2 SLC52A3 Brown-Vialetto-Van Laere syndrome (See Riboflavin Transporter Deficiency Neuronopathy.)
-
Spinal Disc Herniation
Wikipedia
This disorder is called cauda equina syndrome . Other complications include chronic pain . ... A 2006 review of published research states that spinal manipulation "is likely to be safe when used by appropriately-trained practitioners", [50] and research currently suggests that spinal manipulation is safe for the treatment of disc-related pain. [51] Contraindicated [ edit ] Spinal manipulation is contraindicated for disc herniations when there are progressive neurological deficits such as with cauda equina syndrome. [52] A review of non-surgical spinal decompression found shortcomings in most published studies and concluded that there was only "very limited evidence in the scientific literature to support the effectiveness of non-surgical spinal decompression therapy". [53] Its use and marketing have been very controversial. [54] Surgery [ edit ] Surgery may be useful when a herniated disc is causing significant pain radiating into the leg, significant leg weakness, bladder problems, or loss of bowel control. [55] Discectomy (the partial removal of a disc that is causing leg pain) can provide pain relief sooner than non-surgical treatments. Small endoscopic discectomy (called nano-endoscopic discectomy ) is non-invasive and does not cause failed back syndrome . [56] Invasive microdiscectomy with a one-inch skin opening has not been shown to result in a significantly different outcome from larger-opening discectomy with respect to pain. [55] It might however have less risk of infection. [57] Failed back syndrome is a significant, potentially disabling, result that can arise following invasive spine surgery to treat disc herniation. Smaller spine procedures such as endoscopic transforaminal lumbar discectomy cannot cause failed back syndrome, because no bone is removed. [58] The presence of cauda equina syndrome (in which there is incontinence, weakness, and genital numbness) is considered a medical emergency requiring immediate attention and possibly surgical decompression. ... Spinal disc herniation at Curlie v t e Spinal disease Deforming Spinal curvature Kyphosis Lordosis Scoliosis Other Scheuermann's disease Torticollis Spondylopathy inflammatory Spondylitis Ankylosing spondylitis Sacroiliitis Discitis Spondylodiscitis Pott disease non inflammatory Spondylosis Spondylolysis Spondylolisthesis Retrolisthesis Spinal stenosis Facet syndrome Back pain Neck pain Upper back pain Low back pain Coccydynia Sciatica Radiculopathy Intervertebral disc disorder Schmorl's nodes Degenerative disc disease Spinal disc herniation Facet joint arthrosis Authority control GND : 4143993-4 NDL : 01038021
-
Atrioventricular Canal Defect
Mayo_clinic
Experts aren't sure of the cause. Having Down syndrome might increase the risk. How the heart works To understand congenital heart defects, it may be helpful to know how the heart typically works. ... It's associated with many genetic syndromes. For instance, children with Down syndrome often have heart problems present at birth.GATA4, GATA6, GJA1, CRELD1, TBX5, DHCR7, NR2F2, PTPN11, EVC, EVC2, CFC1, RAF1, MAP3K7, ACVR2B, ZIC3, DYNC2LI1, LONP1, WASHC5, CCDC22, NEK1, KAT6B, FANCB, GLI3, GLI1, FLNA, FOXF1, MMP21, BRAF, CEP120, NKX2-5, CHD7, HEY2, BMPR1A, AVSD1, EGF, FOXP1, MKS1, CHDH, TAMM41, SHF, ACVR1, AUTS2, IFT27, IFT88, VEGFA, TBX1, SLC19A1, NFATC1, MTR, MDM4, IL1B, GDF1, FOXF2, ACE, NEXMIF