-
Thymic Hypoplasia
Wikipedia
Calcium levels can be used to distinguish between the following two conditions associated with thymic hypoplasia: 22q11.2 deletion syndrome : hypocalcemia Ataxia telangiectasia : normal levels of calcium References [ edit ] External links [ edit ] Classification D ICD - 10 : Q89.2 (note: thymus is classified as endocrine in ICD-10) ICD - 9-CM : 759.2 DiseasesDB : 34516 This article about an endocrine, nutritional, or metabolic disease is a stub . You can help Wikipedia by expanding it . v t e v t e Lymphatic disease : organ and vessel diseases Thymus Abscess Hyperplasia Hypoplasia DiGeorge syndrome Ectopic thymus Thymoma Thymic carcinoma Spleen Asplenia Asplenia with cardiovascular anomalies Accessory spleen Polysplenia Wandering spleen Splenomegaly Banti's syndrome Splenic infarction Splenic tumor Lymph node Lymphadenopathy Generalized lymphadenopathy Castleman's disease Intranodal palisaded myofibroblastoma Kikuchi disease Tonsils see Template:Respiratory pathology Lymphatic vessels Lymphangitis Lymphangiectasia Lymphedema Primary lymphedema Congenital lymphedema Lymphedema praecox Lymphedema tarda Lymphedema–distichiasis syndrome Milroy's disease Secondary lymphedema Bullous lymphedema Factitial lymphedema Postinflammatory lymphedema Postmastectomy lymphangiosarcoma Waldmann disease v t e Lymphoid and complement disorders causing immunodeficiency Primary Antibody / humoral ( B ) Hypogammaglobulinemia X-linked agammaglobulinemia Transient hypogammaglobulinemia of infancy Dysgammaglobulinemia IgA deficiency IgG deficiency IgM deficiency Hyper IgM syndrome ( 1 2 3 4 5 ) Wiskott–Aldrich syndrome Hyper-IgE syndrome Other Common variable immunodeficiency ICF syndrome T cell deficiency ( T ) thymic hypoplasia : hypoparathyroid ( Di George's syndrome ) euparathyroid ( Nezelof syndrome Ataxia–telangiectasia ) peripheral: Purine nucleoside phosphorylase deficiency Hyper IgM syndrome ( 1 ) Severe combined (B+T) x-linked: X-SCID autosomal: Adenosine deaminase deficiency Omenn syndrome ZAP70 deficiency Bare lymphocyte syndrome Acquired HIV/AIDS Leukopenia : Lymphocytopenia Idiopathic CD4+ lymphocytopenia Complement deficiency C1-inhibitor ( Angioedema / Hereditary angioedema ) Complement 2 deficiency / Complement 4 deficiency MBL deficiency Properdin deficiency Complement 3 deficiency Terminal complement pathway deficiency Paroxysmal nocturnal hemoglobinuria Complement receptor deficiency
-
Toriello–carey Syndrome
Wikipedia
(November 2003). "Toriello-Carey syndrome: delineation and review". Am J Med Genet A . 123A (1): 84–90. doi : 10.1002/ajmg.a.20493 . PMID 14556252 . ^ Wegner KJ, Hersh JA (April 2001). "Toriello-Carey syndrome: an additional case and summary of previously reported cases". ... PMID 27510950 . ^ a b "Toriello-Carey syndrome" . Genetic and Rare Diseases Information Center . ... Retrieved 17 December 2020 . ^ "Toriello Carey syndrome" . Orphanet . Retrieved 17 December 2020 . External links [ edit ] Toriello-Carey syndrome on The Monarch Initiative Classification D ICD - 10-CM : Q87.8 OMIM : 217980 MeSH : C563127 External resources GARD : Toriello-Carey syndrome Orphanet : 3338
-
Mirizzi's Syndrome
Wikipedia
Mirizzi's syndrome Specialty Gastroenterology Mirizzi's syndrome is a rare complication in which a gallstone becomes impacted in the cystic duct or neck of the gallbladder causing compression of the common hepatic duct, resulting in obstruction and jaundice. ... Neela Lamki; Bernard D Coombs; Abraham H Dachman; Robert M Krasny; John Karani (eds.). "Mirizzi syndrome" . eMedicine . WebMD . Retrieved 2007-12-09 . ^ Aydin, U., P. ... "Surgical management of Mirizzi syndrome." Turk J Gastroenterol 19(4): 258–263. ... "Combined endoscopic and surgical management of Mirizzi syndrome". Surgical Endoscopy . 13 (6): 618–20. doi : 10.1007/s004649901054 . PMID 10347304 . ^ synd/3587 at Who Named It? ^ Mirizzi PL: Syndrome del conducto hepatico. J Int de Chir 1948; 8: 731–77 External links [ edit ] Classification D ICD - 9-CM : 576.2 MeSH : D057792 DiseasesDB : 33254 External resources eMedicine : radio/451 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Apparent Mineralocorticoid Excess Syndrome
Wikipedia
Apparent mineralocorticoid excess syndrome Other names AME Apparent mineralocorticoid excess syndrome has an autosomal recessive pattern of inheritance Specialty Medical genetics , endocrinology Apparent mineralocorticoid excess is an autosomal recessive [1] disorder causing hypertension (high blood pressure ) and hypokalemia (abnormally low levels of potassium ). ... "Van gen naar ziekte; 'apparent mineralocorticoid excess'-syndroom, een syndroom met ogenschijnlijke overmaat aan mineralocorticoïden" [From gene to disease; 'apparent mineralocorticoid excess' syndrome, a syndrome with an apparent excess of mineral corticoids]. ... "Apparent mineralocorticoid excess syndrome: report of one family with three affected children". ... "Apparent mineralocorticoid excess syndrome: an overview" (PDF) . Arq Bras Endocrinol Metabol . 48 (5): 687–696. doi : 10.1590/S0004-27302004000500015 . ... External links [ edit ] Apparent mineralocorticoid excess at NIH 's Office of Rare Diseases Classification D ICD - 10 : E26.1 OMIM : 218030 MeSH : D043204 DiseasesDB : 12740 External resources Orphanet : 320 v t e Inborn errors of steroid metabolism Mevalonate pathway HMG-CoA lyase deficiency Hyper-IgD syndrome Mevalonate kinase deficiency To cholesterol 7-Dehydrocholesterol path: Hydrops-ectopic calcification-moth-eaten skeletal dysplasia CHILD syndrome Conradi-Hünermann syndrome Lathosterolosis Smith–Lemli–Opitz syndrome desmosterol path: Desmosterolosis Steroids Corticosteroid (including CAH ) aldosterone : Glucocorticoid remediable aldosteronism cortisol / cortisone : CAH 17α-hydroxylase CAH 11β-hydroxylase both: CAH 3β-dehydrogenase CAH 21-hydroxylase Apparent mineralocorticoid excess syndrome/11β-dehydrogenase Sex steroid To androgens 17α-Hydroxylase deficiency 17,20-Lyase deficiency Cytochrome b 5 deficiency 3β-Hydroxysteroid dehydrogenase deficiency 17β-Hydroxysteroid dehydrogenase deficiency 5α-Reductase deficiency Pseudovaginal perineoscrotal hypospadias To estrogens Aromatase deficiency Aromatase excess syndrome Other X-linked ichthyosis Antley–Bixler syndrome v t e Adrenal gland disorder Hyperfunction Aldosterone Hyperaldosteronism Primary aldosteronism Conn syndrome Bartter syndrome Glucocorticoid remediable aldosteronism AME Liddle's syndrome 17α CAH Pseudohypoaldosteronism Cortisol Cushing's syndrome Pseudo-Cushing's syndrome Steroid-induced osteoporosis Sex hormones 21α CAH 11β CAH Hypofunction Aldosterone Hypoaldosteronism 21α CAH 11β CAH Cortisol CAH Lipoid 3β 11β 17α 21α Sex hormones 17α CAH Inborn errors of steroid metabolism Adrenal insufficiency Adrenal crisis Adrenalitis Xanthogranulomatous Addison's disease Waterhouse–Friderichsen syndrome
-
Alveolar Capillary Dysplasia
Wikipedia
External links [ edit ] Medicine portal Classification D ICD - 10 : J84.843 ICD - 9-CM : 516.64 OMIM : 265380 MeSH : C536590 DiseasesDB : 34875 External resources Orphanet : 210122 v t e Genetic disorders relating to deficiencies of transcription factor or coregulators (1) Basic domains 1.2 Feingold syndrome Saethre–Chotzen syndrome 1.3 Tietz syndrome (2) Zinc finger DNA-binding domains 2.1 ( Intracellular receptor ): Thyroid hormone resistance Androgen insensitivity syndrome PAIS MAIS CAIS Kennedy's disease PHA1AD pseudohypoaldosteronism Estrogen insensitivity syndrome X-linked adrenal hypoplasia congenita MODY 1 Familial partial lipodystrophy 3 SF1 XY gonadal dysgenesis 2.2 Barakat syndrome Tricho–rhino–phalangeal syndrome 2.3 Greig cephalopolysyndactyly syndrome / Pallister–Hall syndrome Denys–Drash syndrome Duane-radial ray syndrome MODY 7 MRX 89 Townes–Brocks syndrome Acrocallosal syndrome Myotonic dystrophy 2 2.5 Autoimmune polyendocrine syndrome type 1 (3) Helix-turn-helix domains 3.1 ARX Ohtahara syndrome Lissencephaly X2 MNX1 Currarino syndrome HOXD13 SPD1 synpolydactyly PDX1 MODY 4 LMX1B Nail–patella syndrome MSX1 Tooth and nail syndrome OFC5 PITX2 Axenfeld syndrome 1 POU4F3 DFNA15 POU3F4 DFNX2 ZEB1 Posterior polymorphous corneal dystrophy Fuchs' dystrophy 3 ZEB2 Mowat–Wilson syndrome 3.2 PAX2 Papillorenal syndrome PAX3 Waardenburg syndrome 1&3 PAX4 MODY 9 PAX6 Gillespie syndrome Coloboma of optic nerve PAX8 Congenital hypothyroidism 2 PAX9 STHAG3 3.3 FOXC1 Axenfeld syndrome 3 Iridogoniodysgenesis, dominant type FOXC2 Lymphedema–distichiasis syndrome FOXE1 Bamforth–Lazarus syndrome FOXE3 Anterior segment mesenchymal dysgenesis FOXF1 ACD/MPV FOXI1 Enlarged vestibular aqueduct FOXL2 Premature ovarian failure 3 FOXP3 IPEX 3.5 IRF6 Van der Woude syndrome Popliteal pterygium syndrome (4) β-Scaffold factors with minor groove contacts 4.2 Hyperimmunoglobulin E syndrome 4.3 Holt–Oram syndrome Li–Fraumeni syndrome Ulnar–mammary syndrome 4.7 Campomelic dysplasia MODY 3 MODY 5 SF1 SRY XY gonadal dysgenesis Premature ovarian failure 7 SOX10 Waardenburg syndrome 4c Yemenite deaf-blind hypopigmentation syndrome 4.11 Cleidocranial dysostosis (0) Other transcription factors 0.6 Kabuki syndrome Ungrouped TCF4 Pitt–Hopkins syndrome ZFP57 TNDM1 TP63 Rapp–Hodgkin syndrome / Hay–Wells syndrome / Ectrodactyly–ectodermal dysplasia–cleft syndrome 3 / Limb–mammary syndrome / OFC8 Transcription coregulators Coactivator: CREBBP Rubinstein–Taybi syndrome Corepressor: HR ( Atrichia with papular lesions )
-
Sopite Syndrome
Wikipedia
Sopite syndrome Specialty Neurology The sopite syndrome ( / s oʊ ˈ p aɪ t / ; Latin: sopire, "to lay to rest, to put to sleep") [1] is a neurological disorder that relates symptoms of fatigue , drowsiness , and mood changes to prolonged periods of motion. [2] The sopite syndrome has been attributed to motion-induced drowsiness such as that experienced by a baby when rocked. [1] Researchers Graybiel and Knepton at the Naval Aerospace Medical Research Laboratory first used the term "the sopite syndrome", in 1976, to refer to the sometimes sole manifestation of motion sickness , though other researchers have referred to it as "Sopite syndrome." ... The sopite syndrome may persist even after an individual has adapted to the other symptoms associated with motion-induced sickness. [2] Severity [ edit ] The effects of the sopite syndrome may range from minor physical inconveniences to hazardous conditions. ... However, the sopite syndrome itself does not directly result in death. [4] A subject experiencing the sopite syndrome on a frequent basis may increase the number of hours spent sleeping by fifty percent. ... Also, the length of time exposed to vehicular motion did not appear to affect the occurrence (or lack thereof) or severity of the sopite syndrome. No difference was observed in the incidence of the sopite syndrome for men versus women. [6] The sopite syndrome is likely a cumulative disorder. ... Melatonin may therefore be involved in the drowsy state associated with the sopite syndrome. [8] Noradrenergic pathways [ edit ] The inhibition of noradrenergic pathways has also been associated with symptoms of the sopite syndrome.
-
Guillain-Barre Syndrome
Mayo_clinic
Overview Guillain-Barre (gee-YAH-buh-RAY) syndrome is a rare disorder in which your body's immune system attacks your nerves. ... Although most people recover completely from Guillain-Barre syndrome, some severe cases can be fatal. ... Guillain-Barre syndrome may occur after infection with the COVID-19 virus. ... Sluggish bowel function and urine retention may result from Guillain-Barre syndrome. Blood clots. People who are immobile due to Guillain-Barre syndrome are at risk of developing blood clots. ... Rarely, death may occur from complications such as respiratory distress syndrome and heart attacks. Diagnosis Guillain-Barre syndrome can be difficult to diagnose in its earliest stages.PMP22, CD86, AIRE, TNF, IL17A, CSF2, LAMC2, CD1E, ALB, CD1A, HLA-DQB1, IL1B, CD1C, TLR4, IL10, CD1B, ICAM1, IL23A, ISG20, FCGR2A, CRP, IL4, IL2RA, IL17D, HLA-DRB1, IL6, MAPK1, NFASC, GFAP, ITGAM, COX2, MYDGF, PTGS2, FCGR3A, APOE, IL27, FAS, MTCO2P12, CNTNAP1, YY1, YWHAZ, CXCR4, AIMP2, RETN, SELENBP1, TNFRSF1B, MIR155, GRAP2, GLDN, NOD1, VIM, MIR642B, SIGLEC14, AHSA1, OCLN, TLR2, TH, TGFB1, STAT3, SPP1, SMPD2, CXCL6, CCL2, PTPN11, MIF-AS1, IVNS1ABP, CSGALNACT1, POLDIP2, SMPD3, NS2, IL21, ISYNA1, FOXP3, IL22, ICOS, DLL1, ERVK-6, SIGLEC9, ST6GALNAC4, PTGS1, RNF19A, TUBGCP2, NOD2, SUMF2, FTSJ1, IL33, CADM1, FCRL3, FTSJ3, RBM45, HT, CABIN1, PLB1, YWHAQ, SIGLEC7, NOS2, PSMB6, F2R, HMGB1, HLA-DQB2, HLA-DQA1, HLA-DOA, CXCL2, CXCL1, NR3C1, GOLGA4, GNAO1, GLO1, GJB1, GALE, FOLH1, FCGR3B, ESR1, HPRT1, EPHB2, ENO2, CST3, MAPK14, CRK, COX8A, CNTN1, CDC42, CD59, CD80, CD14, CACNA1A, SERPING1, FASLG, HP, HSPA4, MAP2K7, MMP2, MAPK8, PRKD1, POMC, PLA2G1B, PKD1, PGF, PDCD1, NPPB, NPY, NOS3, NEFL, COX1, MRC1, MMP9, NR3C2, HSPD1, MIF, MBL2, LEP, ITGB2, ITGAL, IRF6, INSRR, CXCL10, IL18, IL12B, IL12A, IL2, IGHG3, IFNG, ERVK-32
-
Alice In Wonderland Syndrome
Wikipedia
ISBN 978-0-19-856837-7 . ^ "Alice and Wonderland Syndrome and Visual Migraines" . ^ "Alice in Wonderland Syndrome | Symptoms & Treatment" . ... "Alice in Wonderland Syndrome: A real life version of Lewis Carroll's novel". ... "Alice in Wonderland Syndrome" . aiws.info . Archived from the original on 2017-09-14 . ... PMID 1390519 . ^ "Alice in Wonderland syndrome". Taber's Cyclopedic Medical Dictionary . ... "Alice in Wonderland Syndrome: A real life version of Lewis Carroll's novel".
-
Epilepsy Syndromes
Wikipedia
People with epilepsy may be classified into different syndromes based on specific clinical features. ... These are associated with frequent seizures that are resistant to treatment and severe cognitive dysfunction, for instance Lennox-Gastaut syndrome and West syndrome . [4] [5] Contents 1 Classification of Epilepsy syndromes 2 Autosomal dominant nocturnal frontal lobe epilepsy 3 Rolandic epilepsy 4 Benign occipital epilepsy of childhood 5 Childhood absence epilepsy 6 Dravet syndrome 7 Epilepsy in females with mental retardation 8 Febrile infection-related epilepsy syndrome 9 Frontal lobe epilepsy 10 Juvenile myoclonic epilepsy 11 Lennox-Gastaut syndrome 12 Ohtahara syndrome 13 Reflex epilepsies 14 Progressive myoclonic epilepsies 15 Rasmussen's encephalitis 16 Temporal lobe epilepsy 17 West syndrome 18 See also 19 References Classification of Epilepsy syndromes [ edit ] Epilepsy syndromes are classified as per the age onset. ... Others are included in symptomatic despite a presumed genetic cause (in at least in some cases), for instance Lennox-Gastaut syndrome . [11] Clinical syndromes in which epilepsy is not the main feature (e.g. ... As in West syndrome, LGS result from idiopathic, symptomatic, or cryptogenic causes, and many patients first have West syndrome . ... Anticonvulsants are usually only partially successful in treatment. Ohtahara syndrome [ edit ] Ohtahara syndrome is a rare but severe epilepsy syndrome usually starting in the first few days or weeks of life.SCN1A, SCN2A, GABRG2, PCDH19, LGI1, GRIN2A, SCN8A, BFIS1, STXBP1, POLG, STX1B, TBC1D24, CNTNAP2, SCN1B, ECT, CHRNA4, GABRA1, KCNQ2, GABRB3, GABRD, ABCB1, ADAM22, CISH, SLC12A5, LRRC4, EJM2, STRADA, PRRT2, CDK9, EFHC1, C1orf52, FCMTE1, PLCB1, F5, PART1, MMP9, MVP, CACNA1H, SLC2A1, BDNF, SCN3A, KCNQ3, MAP6, PSEN1, PRNP, AQP4
-
Gms Syndrome
Wikipedia
GMS syndrome Other names Goniodysgenesis-intellectual disability-short stature syndrome GMS syndrome is a syndrome characterised by goniodysgenesis , intellectual disability , and short stature . [1] References [ edit ] ^ Kupchik GS, Ludman MD, Raab EL, Gilbert F (January 1992). "GMS syndrome: a new dominant condition with goniodysgenesis, mental retardation, and short stature".
-
Al-Raqad Syndrome
Wikipedia
Al-Raqad syndrome Other names ARS Al-Raqad syndrome is a congenital autosomal recessive syndrome discovered by Jordanian physician Mohammad Al-Raqad . It's characterized by: Microcephaly Growth delay Psycho-motor developmental delay Congenital hypotonia . Al-Raqad syndrome is caused by mutation of DCPS gene . [1] References [ edit ] ^ "OMIM Entry - # 616459 - AL-RAQAD SYNDROME; ARS" . www.omim.org .
-
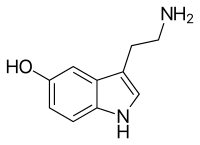
Serotonin Syndrome
Orphanet
Serotoninergic syndrome is characterised by an excess of serotonin in the central nervous system, associated with the use of various agents, including selective serotonin reuptake inhibitors (SSRIs). ... Clinical description Serotoninergic syndrome may result in muscle rigidity, myoclonus, agitation, confusion, hyperthermia, hyperreflexia as well as dysautonomic symptoms, with a risk of shock with low peripheral vascular resistance, seizures, coma, rhabdomyolysis and/or disseminated intravascular coagulation (DIC). Etiology SSRIs and monoamine oxidase inhibitors (MAOIs) may be responsible for this syndrome at toxic but also at therapeutic concentrations. ... Differential diagnosis Differential toxicological diagnoses include neuroleptic malignant syndrome (see this term), adrenergic or anticholinergic syndromes as well as alcohol withdrawal syndrome. ... Cyproheptadine is the specific antidote for serotonin syndrome. Prognosis Prognosis is generally good if adequate supportive treatments are administered.
-
Catastrophic Antiphospholipid Syndrome
Wikipedia
Find sources: "Catastrophic antiphospholipid syndrome" – news · newspapers · books · scholar · JSTOR ( February 2018 ) ( Learn how and when to remove this template message ) Catastrophic antiphospholipid syndrome Other names Catastrophic APS Catastrophic antiphospholipid syndrome ( CAPS ), also known as Asherson's syndrome , is a rare autoimmune disease in which widespread, intravascular clotting causes multi-organ failure. [1] The syndrome is caused by antiphospholipid antibodies that target a group of proteins in the body that are associated with phospholipids . ... The syndrome usually occurs with small vessel thromboses affecting organ systems such as the gastrointestinal tract and manifestations of the acute respiratory distress syndrome (ARDS), a type of systemic inflammatory response syndrome (SIRS). [2] Peripheral thrombosis may be encountered affecting veins and arteries. ... "The Catastrophic Antiphospholipid Syndrome" . Antiphospholipid Antibody Syndrome : 249–262. doi : 10.1007/978-3-319-11044-8_20 . ... S2CID 207211666 . ^ "Asherson's Syndrome" . NORD (National Organization for Rare Disorders) . ... PMID 17223653 . ^ NORD. "Asherson's Syndrome" . National Organization of Rare Disorders .
-
Au-Kline Syndrome
Medlineplus
Au-Kline syndrome is a condition that affects many body systems. ... Some people with Au-Kline syndrome have an abnormal curvature of the spine (scoliosis). ... In people with Au-Kline syndrome, abnormalities in this system can lead to digestive problems, difficulty feeling pain, abnormal sweating, and an inability to adjust to high heat in people with Au-Kline syndrome. Frequency Au-Kline syndrome is a rare condition with an unknown prevalence. At least 25 cases have been diagnosed. Causes Au-Kline syndrome is caused by mutations in the HNRNPK gene.
-
Urethral Syndrome
Wikipedia
Urethral syndrome Specialty Urology Urethral syndrome is characterised by a set of symptoms typically associated with lower urinary tract infection, such as painful urination ( dysuria ) and frequency . ... Some physicians believe that urethral syndrome may be due to a low grade infection of the Skene's glands on the sides and bottom of the urethra . [ citation needed ] The Skene's glands are embryologically related to the prostate gland in the male, thus urethral syndrome may share a comparable cause with chronic prostatitis . [ citation needed ] Possible non-infective causes include hormonal imbalance, [2] [3] trauma, allergies , anatomical features such as diverticula , and post-surgical scarring and adhesions. [1] Diagnosis [ edit ] This section is empty. ... "The urethral syndrome and its management". J. Antimicrob. ... PMID 7928838 . ^ a b c d e Brumfitt W, Hamilton-Miller JM, Gillespie WA (July 1991). "The mysterious "urethral syndrome " " . BMJ . 303 (6793): 1–2. doi : 10.1136/bmj.303.6793.1 . ... PMID 1859947 . ^ a b Terris, Martha K. "Urethral Syndrome" . eMedicine . Retrieved 2008-09-25 .
-
Plica Syndrome
Wikipedia
Unsourced material may be challenged and removed . Find sources: "Plica syndrome" – news · newspapers · books · scholar · JSTOR ( February 2015 ) ( Learn how and when to remove this template message ) Plica syndrome Other names Synovial plica syndrome Specialty Orthopedics Plica syndrome is a condition that occurs when a plica (a vestigial extension of the protective synovial capsule of usually the knee ) becomes irritated, enlarged, or inflamed. [1] Contents 1 Cause 2 Diagnosis 3 Treatment 4 See also 5 References 6 External links Cause [ edit ] This inflammation is typically caused by the plica being caught on the femur , or pinched between the femur and the patella . ... The plica are usually harmless and unobtrusive; plica syndrome only occurs when the synovial capsule becomes irritated, which thickens the plica themselves (making them prone to irritation/inflammation, or being caught on the femur). ... Diagnosis is often complicated by the thin structures of plicae, fenestrated septum or unfenestrated septum all being too fine to resolve well even in MRI. Treatment [ edit ] Plica syndrome treatment focuses on decreasing inflammation of the synovial capsule . ... See also [ edit ] Knee pain Patellofemoral pain syndrome Iliotibial band syndrome References [ edit ] ^ Casadei, Kyle; Kiel, John (2020). "Plica Syndrome" . StatPearls . StatPearls Publishing.
-
Persistent Müllerian Duct Syndrome
Medlineplus
Persistent Müllerian duct syndrome is a disorder of sexual development that affects males. ... This condition, called transverse testicular ectopia, is common in people with persistent Müllerian duct syndrome. Other effects of persistent Müllerian duct syndrome may include the inability to father children (infertility) or blood in the semen (hematospermia). ... Frequency Persistent Müllerian duct syndrome is a rare disorder; however, the prevalence of the condition is unknown. Causes Most people with persistent Müllerian duct syndrome have mutations in the AMH gene or the AMHR2 gene. ... Approximately 45 percent of cases of persistent Müllerian duct syndrome are caused by mutations in the AMH gene and are called persistent Müllerian duct syndrome type 1.
-
Beare–stevenson Cutis Gyrata Syndrome
Wikipedia
Beare–Stevenson cutis gyrata syndrome Other names Cutis gyrata-acanthosis nigricans-craniosynostosis syndrome [1] Diagnostic method identification of the p.Pro250Arg pathogenic variant in FGFR3; the diagnosis of FGFR2-related isolated coronal synostosis is based on identification of a FGFR2 pathogenic variant. ... Any alternative underlying causes are currently unidentified. The syndrome follows an autosomal dominant pattern, meaning that if one of the two available genes carries a mutation the syndrome will result. ... You can help by adding to it . ( April 2017 ) Incidence [ edit ] Beare–Stevenson cutis gyrata syndrome is so rare that a reliable incidence cannot be established as of yet; fewer than 25 patients with the condition have been reported. ... "Orphanet: Cutis gyrata acanthosis nigricans craniosynostosis syndrome" . www.orpha.net . Retrieved 14 March 2019 . ^ http://ghr.nlm.nih.gov/condition/beare-stevenson-cutis-gyrata-syndrome The Genetic Home Reference entry on Beare-Stevenson cutis gyrata syndrome ^ a b Hall BD, Cadle RG, Golabi M, Morris CA, Cohen MM (September 1992). "Beare-Stevenson cutis gyrata syndrome". Am J Med Genet . 44 (1): 82–89. doi : 10.1002/ajmg.1320440120 .
-
Mayer-Rokitansky-Küster-Hauser Syndrome Type 2
Orphanet
Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome type 2, a form of MRKH syndrome (see this term), is characterized by congenital aplasia of the uterus and upper 2/3 of the vagina that is associated with at least one other malformation such as renal, vertebral, or, less commonly, auditory and cardiac defects. The acronym MURCS (MÜllerian duct aplasia, Renal dysplasia, Cervical Somite anomalies) is also used. Epidemiology MRKH syndrome has an estimated worldwide incidence of 1/4500 live female births. The prevalence of MRKH syndrome type 2 is unknown. Clinical description MRKH syndrome type 2 is most often diagnosed in adolescence as the first symptom is most commonly a primary amenorrhea in young women presenting with otherwise normal development of secondary sexual characteristics and normal external genitalia. ... Initially, MRKH syndrome was considered to be of sporadic occurrence, suggesting the involvement of non-genetic or environmental factors. However, no link between an environmental cause and MRKH syndrome has ever been established. It is now clear that MRKH syndrome has a genetic origin, through increasing family descriptions and numerous genetic studies already completed.
-
Progeroid Syndromes
Wikipedia
For aging in general, see Senescence . Progeroid syndromes ( PS ) are a group of rare genetic disorders which mimic physiological aging , making affected individuals appear to be older than they are. [1] [2] The term progeroid syndrome does not necessarily imply progeria ( Hutchinson–Gilford progeria syndrome ), which is a specific type of progeroid syndrome. ... Most known PS are due to genetic mutations that lead to either defects in the DNA repair mechanism or defects in lamin A/C . Examples of PS include Werner syndrome (WS), Bloom syndrome (BS), Rothmund–Thomson syndrome (RTS), Cockayne syndrome (CS), xeroderma pigmentosum (XP), trichothiodystrophy (TTD), combined xeroderma pigmentosum - Cockayne syndrome (XP-CS), restrictive dermopathy (RD), and Hutchinson–Gilford progeria syndrome (HGPS). ... The most widely studied of the progeroid syndromes are Werner syndrome and Hutchinson–Gilford progeria, as they are seen to most resemble natural aging . [3] Contents 1 Defects in DNA repair 1.1 RecQ-associated PS 1.1.1 Werner syndrome 1.1.2 Bloom syndrome 1.2 NER protein-associated PS 1.2.1 Cockayne syndrome 1.2.2 Xeroderma pigmentosum 1.2.3 Trichothiodystrophy 2 Defects in Lamin A/C 2.1 Hutchinson–Gilford progeria syndrome 2.2 Restrictive dermopathy 3 Defects in FBN1 4 A common cause for premature aging 5 Unknown causes 5.1 Wiedemann–Rautenstrauch syndrome 5.1.1 Rothmund–Thomson syndrome 6 Cancer 7 Animal models 8 Other 9 Society and popular culture 9.1 People 9.2 Literature 9.3 Film 10 See also 11 References 12 Further reading 13 External links Defects in DNA repair [ edit ] One of the main causes of progeroid syndromes is genetic mutations , which lead to defects in the cellular processes which repair DNA . ... Hutchinson–Gilford progeria syndrome [ edit ] Girl with HGPS ( left ). ... PMID 16246145 . ^ German, J; Sanz, MM; Ciocci, S; Ye, TZ; Ellis, NA (2007). "Syndrome-causing mutations of the BLM gene in persons in the Bloom's Syndrome Registry".KL, WRN, ERCC6, APP, EXT1, LMNA, BLM, RECQL4, TP53, ZMPSTE24, SIRT1, CISD2, FGF23, HTRA2, ATM, CDKN2A, CSH2, CSH1, IGF1, HSPA9, SPRTN, ARNTL, ANGPTL2, ROBO3, ERCC2, EMD, ELN, TH, DKC1, BUB1B, CYP27A1, ERCC8, SOX2, CDKN1A, VDR, BMI1, SOD1, TUSC2, TOP3A, PPARGC1A, VCP, CFDP1, IKBKG, NCOR2, CLOCK, TP63, ATG5, XPO1, RECQL5, CUL4A, BANF1, SIRT2, TBPL1, ADCYAP1, EXOSC2, TNMD, COMMD3-BMI1, EDS8, COPD, IS1, ASPM, TMEM201, KCNH8, SPNS1, ROPN1L, SMURF2, CHMP1B, KCNH4, WRNIP1, TWNK, NHP2, ENOSF1, TFAM, SIRT6, FOXP3, GEMIN4, A1CF, SENP6, APTX, SCT, TERF2, TERC, GUSB, GLO1, G6PD, FUS, FOXO3, FGF1, EFEMP1, ERCC4, ERCC3, EPHB2, ELK1, EIF4G2, DPP4, CYLD, RUNX2, CAV1, CAT, CASP2, C3, BRCA1, BCL2, ASPA, ASIP, AR, APOE, H1-4, IGFBP3, IL1A, PSMD2, SRF, SOD3, SOD2, SNAI2, SLC3A2, SRSF5, SFRP1, AGTR2, RBBP4, RAD51, PYCR1, MAPK1, IL1B, POLG, PIN1, SERPINE1, NFE2L2, MYOD1, MUC1, MMP9, MECP2, MDM2, LPA, LBR, H3P10