-
Achilles Tendon Rupture
Wikipedia
External links [ edit ] Classification D ICD - 10 : S86.0 ICD - 9-CM : 727.67 External resources eMedicine : sports/1 Image sequence demonstrating Achilles tendinosis and Achilles tendon rupture v t e Soft tissue disorders Capsular joint Synoviopathy Synovitis / Tenosynovitis Calcific tendinitis Stenosing tenosynovitis Trigger finger De Quervain syndrome Transient synovitis Ganglion cyst osteochondromatosis Synovial osteochondromatosis Plica syndrome villonodular synovitis Giant-cell tumor of the tendon sheath Bursopathy Bursitis Olecranon Prepatellar Trochanteric Subacromial Achilles Retrocalcaneal Ischial Iliopsoas Synovial cyst Baker's cyst Calcific bursitis Noncapsular joint Symptoms Ligamentous laxity Hypermobility Enthesopathy / Enthesitis / Tendinopathy upper limb Adhesive capsulitis of shoulder Impingement syndrome Rotator cuff tear Golfer's elbow Tennis elbow lower limb Iliotibial band syndrome Patellar tendinitis Achilles tendinitis Calcaneal spur Metatarsalgia Bone spur other/general: Tendinitis / Tendinosis Nonjoint Fasciopathy Fasciitis : Plantar Nodular Necrotizing Eosinophilic Fibromatosis / contracture Dupuytren's contracture Plantar fibromatosis Aggressive fibromatosis Knuckle pads v t e Dislocations / subluxations , sprains and strains Joints and ligaments Head and neck Dislocation of jaw Whiplash Shoulder and upper arm GH ( Dislocated shoulder ) AC ( Separated shoulder ) ALPSA lesion SLAP tear Bankart lesion Elbow and forearm Pulled elbow Gamekeeper's thumb Hip and thigh Hip dislocation Knee and leg Tear of meniscus Anterior cruciate ligament injury Unhappy triad Patellar dislocation Knee dislocation Ankle and foot Sprained ankle ( High ankle sprain ) Turf toe Muscles and tendons Shoulder and upper arm Rotator cuff tear Hip and thigh Pulled hamstring Knee and leg Patellar tendon rupture Achilles tendon rupture Shin splints
-
Pulmonary Fibrosis
Wikipedia
External links [ edit ] Classification D ICD - 10 : J84.1 ICD - 10-CM : J84.10 ICD - 9-CM : 516.31 MeSH : D011658 External resources Patient UK : Pulmonary fibrosis v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisTGFB1, CCN2, EDN1, IL1B, MMP9, NFE2L2, IL4, CCL2, IL13, TIMP1, AGT, CSF2, HPS1, FAM13A, DSP, AP3B1, ABCA3, FN1, HGF, TNF, IL6, HMGB1, TGFA, STAT3, IGF1, FGF2, CXCL8, MTOR, MMP2, SOD1, CCL11, CCR2, SERPINA1, SPP1, AREG, MIR326, ADIPOQ, HMOX1, STAT6, MIR30A, MECP2, EGF, COL3A1, MIR29C, CAT, SOD3, BMP7, FGF1, ELN, CEBPB, FGF7, CCL5, GREM1, CCL4, CCR3, PARP1, SMAD7, ACTA2, LAMB1, PDGFA, IL1RN, IL5, CSF3, MIR140, MIR125A, CYSLTR2, CEBPA, MIR26B, CMA1, FYN, MIR200C, IL12B, MIR122, MIR345, CALCA, SKIL, MIR10A, PDGFB, PTX3, SERPINE1, MIR101-1, CXCL2, MIR425, MIR378A, CCL3, CFD, EGFR, IL17A, PTGS2, AGER, COL1A1, ACE, PLAU, SMAD4, MMP1, SCGB1A1, IL1A, ELANE, CD36, TGFBR2, COL1A2, PDGFRA, CCL17, CCL22, ANXA1, HSP90AB1, CDH1, HABP2, STAT1, ICAM1, MFN2, CYSLTR1, TERT, B3GAT1, HSPD1, MUC5B, CCR4, BAD, VWF, NKX2-5, CCR8, SFTPC, MUC5AC, CAV1, HPS4, RTEL1, TERC, PARN, IRF5, SFTPA2, SFTPA1, FAM111B, HLA-DRB1, TINF2, DKC1, HLA-DPB1, CTLA4, CFTR, DCTN4, PRTN3, PRKCD, FASLG, FAS, ACTB, BTNL2, HIF1A, IL10, MRPS22, PIK3CD, PIK3CG, PIK3CB, PIK3CA, RNF168, SMAD2, NLRP3, STN1, SP110, BMP15, NHP2, HLA-DPA1, KIAA0319L, DPP9, RCBTB1, SMAD3, NOP10, NR5A1, NUP107, FSHR, THOC2, NOX4, PLEC, PSMC3IP, RASGRP1, ALMS1, ASAH1, POSTN, NKX2-1, CASP10, CLCA4, STX1A, CCR6, ATP11A, SMN2, SMN1, SPIDR, CTNNB1, PTPN22, MIR21, F2R, VEGFA, TP53, LOX, AKT1, GABPA, CXCR4, TLR4, FOSL2, PLG, COPD, ACE2, THY1, ANGPT1, TNC, SIRT3, MMRN1, GLI1, DECR1, BLM, LPAR1, CXCL12, VIM, CEL, FSTL1, LOXL2, SLC27A5, PARP9, PRKAB1, IL33, JAK2, PRKAA1, PRKAA2, TM7SF2, IFNG, MTCO2P12, SIRT1, SFTPD, COX2, LGALS3, MMP12, CCL18, MMP7, REN, S100A4, HSPA4, NR1I2, PTEN, MUC1, MIRLET7D, ZEB1, MIR34A, OGG1, ADAM17, MSC, VTN, CCN4, YY1, PPARG, SPHK1, SEMA7A, NT5E, DNM1L, SMUG1, TOP1, BRD4, SLC52A2, HSPB3, PINK1, TMED7, SPARC, PDGFRB, TGFB3, GDF15, PHEX, MAPK3, KLF4, HSP90AA1, DNER, MAPK14, MARK2, TMED7-TICAM2, F2RL1, TICAM2, BLMH, TSLP, GLB1, PWAR1, GSK3B, FOXO3, EGR1, CD44, DDIT3, DCN, DNMT1, ING4, MAPK1, ELK1, MAPK7, MAPK8, PSMD9, TLR2, LILRB1, PTK2, PTPN11, DCTN6, IL7, TSC1, CXCR6, FOLR2, PDCD1, LCLAT1, ZNRD2, FOXM1, WNT1, SLC52A1, PF4, ATF3, SSRP1, AHSA1, BDNF, STING1, UTRN, SIRT6, TXN, FASN, TWIST1, PTPRC, MIR145, HPGDS, MIR154, CD274, CST3, CHI3L1, NLRP1, CSF1R, CSF1, SLC2A1, CRYAB, CRMP1, SNAI1, CRK, SOAT1, MIR29A, SOD2, CREBBP, MIR29B1, MIR29B2, STAT4, CNR2, LTB4R, DAPK2, SDC2, SDC1, TGFBI, MOK, THBD, PRKN, METAP2, IL37, MIR155, MIR15A, MIR18A, DPP4, CX3CL1, SERPINH1, RIPK3, POLDIP2, RNF19A, TFF1, MIR200B, NUDT21, CDH11, FOS, BACH1, SOCS1, ANXA2, LGALS1, SQSTM1, JAG1, LOXL1, PERCC1, TNFSF14, HDAC4, MARCO, CTHRC1, BECN1, DENR, MIP, RBM45, HAS2, CXCL16, ANPEP, MMP13, ROCK2, LDHA, HSPB1, SETD7, S1PR2, IL9, MAPKAPK2, H3P23, CCN1, MAP1LC3B, IL18, IRAK1, HSPB2, KL, IGFBP3, GRAP2, MCU, IFI27, ITGB6, ADORA2B, LTBP4, ST2, MYD88, MPO, FST, GLI2, GPX4, P2RX7, ANXA5, TSPAN1, YAP1, CBLIF, AIMP2, GLRX, TFEB, GAS6, IL18BP, OSM, NTN1, MIR323A, RAPGEF3, MIR542, MIR1224, CHP1, TMPRSS11D, ABCG2, AIM2, GGPS1, DUSP10, TRIM16, MIR328, MIR96, LINC02605, KLF2, MIR34B, P2RX2, MIR31, MERTK, FBLN5, KAT5, CXCL13, ATG7, SLIT2, H3P11, TRIP10, MIR30D, P2RX5-TAX1BP3, ATG5, MIR541, RAMP2, ATP6AP2, MIR506, PPARGC1A, TNFSF13B, GAB2, MIR5100, MIR486-1, MIR454, MIR455, DNM3OS, CAPN9, FAM72A, NEU3, FAM72B, MIR627, HDAC6, SPATA2, RPL17-C18orf32, JTB, KHDRBS1, PLF, MIR448, PLXNC1, MIR4516, MIR449A, SIRT1-AS, CDR1-AS, PCLAF, ABCG1, H4C15, RGS6, LRPPRC, MIR503, CD226, TMX2-CTNND1, B3GAT3, ATG4B, ACKR3, TRPV4, GER, H4-16, SLCO6A1, ROMO1, TRIB3, PRX, MRTFA, RCN3, RMDN2, ASPRV1, KMT5AP1, PCBP4, TCIM, SULF1, SPHK2, RHOV, TMPRSS4, PARD3, PGAM5, MYDGF, SULF2, HDAC8, PAG1, IL26, MFN1, PRSS55, ZEB1-AS1, RXFP1, FKBP10, SCGB3A2, SMOC2, SPZ1, RETNLB, ING5, CRISPLD2, LOXL3, HAVCR2, CD276, ADAM33, WNT10A, ZC3H12A, GRHL2, NAF1, MMP28, ELOVL6, TRPM8, WNK1, CDCP1, IL25, MUC16, PRRT2, DEPTOR, NREP, SEMA4A, IFIH1, IL17F, UCN3, FBXO32, SYBU, EBF3, ELMOD2, ADGRE2, TBK1, SETD2, IL17B, BBC3, LATS2, FGF21, KISS1R, PHGDH, MIR185, PART1, MIR193A, MIR19A, MIR19B1, MIR205, MIR210, PRDX5, NUP62, MIR221, DDAH1, PIGN, MIR27A, TRAM1, MIR27B, CBX5, HEY1, PPP1R13B, MIR301A, MIR146A, DELEC1, RMDN3, MIR144, SARS2, EGLN1, ROBO4, NPNT, IFNL3, POLE3, LAMA1, PWAR4, GSTK1, SIRT7, GTSE1, MALAT1, FENDRR, SNX9, CSAD, CHST15, CRNKL1, TNFRSF12A, MIR126, MIR130A, MIR130B, MIR139, RMDN1, ADIPOR1, MIR141, MIR142, FOXP3, GORASP1, SFRP4, CRLF1, GRP, FUT8, GAB1, GATA3, GLS, CCR10, CXCR3, GPT, GTF2H1, HPGD, HDAC2, CFHR1, NRG1, HLA-A, HLA-B, HLA-C, HLF, FOSB, FLT3LG, FLT3, FLT1, ESR1, ETS2, F2, F2RL2, F3, F10, FAP, FCGR3A, FCGR3B, FGF13, FGFR2, FGL1, VEGFD, FOXF1, FOXD1, NR4A1, HSPA1A, ERN1, JUNB, ITGAE, ITGAX, ITGB3, EIF6, IVD, JAK1, JUN, JUND, HSPA1B, KCNMB1, LEP, LMNA, LRP6, LTBR, LUM, MARCKS, ITGA9, ISG20, ITGA6, INPP5D, HTR2A, ID1, IFNB1, IGF2, IGFBP2, IGFBP5, IL2, IL2RA, IL4R, IL6ST, IL7R, IL11, IL11RA, IL15, TNFRSF9, FBL, ERBB3, MEN1, CAST, KLF9, TSPO, C3, C3AR1, C5AR1, VPS51, DDR1, CASP1, CDKN2A, RUNX2, RUNX3, CBS, CD28, CD59, ADGRE5, CD151, BSG, BMPR2, BMP3, BGN, ADA, ADAM10, ADM, AEBP1, AGTR1, AIF1, AKT2, ALB, ANGPT2, ANXA11, APOA1, APRT, ARG1, BARD1, BCL2, CDH5, CDKN2B, ERBB2, E2F4, CYP27B1, DES, NQO1, DIO2, DNAH8, ARID3A, E2F1, ECE1, CHAT, ECT2, S1PR3, EFNB2, EPHA2, EIF4E, EP300, STX2, CYP2E1, CYLD, CX3CR1, CTSK, CHIT1, CHRM3, CHRNA4, CLU, ACKR2, CNR1, COL11A2, COX8A, CREB1, ATF2, CRIP1, CRYZ, CSNK1D, CSRP1, CTNND1, MCAM, MFAP1, XPR1, TNFRSF1A, TGFB2, TGFBR1, THAS, THBS1, TIAM1, TIMP3, TLR3, TNNC1, WT1, TPH1, CRISP2, TRPC6, TSC2, TNFSF4, VCAM1, VDR, TMBIM6, PPP1R11, TRBV20OR9-2, TAZ, SHH, SIX1, SKI, SKP2, SNAI2, SNCA, SOX2, SPINT1, SRC, SREBF1, SRF, STC1, STK11, SYT1, TAGLN, TRPV1, XIST, SFRP1, MBD2, AOC3, EIF3A, MBTPS1, TNFSF10, CCN6, CCN5, SGPL1, TRPA1, FOSL1, F2RL3, TM4SF5, SYT7, P2RX6, ATG12, LPAR2, IL1RL1, BHLHE40, ENC1, RASAL1, ULK1, HMGA2, H3-4, H4C9, FZD7, H4C1, H4C4, H4C6, H4C12, H4C11, H4C3, H4C8, H4C2, H4C5, H4C13, H4C14, ACO2, SELPLG, MID1, PAWR, P2RX3, P2RX4, P2RX5, P2RY1, P2RY2, P4HB, FURIN, PCNA, PIP, PDE1A, PDK1, PECAM1, ATP8B1, ABCB1, PHB, SERPINE2, P2RX1, DDR2, NTF3, NOTCH4, MAP3K11, MMP3, MMP10, MMP14, MMP19, MPG, MRC1, MSR1, MST1, NEDD8, NEU1, NFKB1, NINJ1, NM, NOTCH1, PIN1, PLA2G4A, SELE, ROCK1, RASA1, RBP2, OPN1LW, RELA, RGS2, BRD2, RNH1, ROS1, PLAUR, RPL17, S100A6, S100A9, SARS1, SERPINB3, CCL24, SDC4, RARRES2, RAG2, RAF1, RAC2, PLK1, POU2AF1, PPL, PRH1, PRH2, PRKCA, PRKCB, PRKDC, EIF2AK2, PTCH1, PTGER4, PTHLH, PTPN13, PTPRJ, RAC1, H3P10
-
Pelvic Girdle Pain
Wikipedia
It is now referred to as Pregnancy Related Pelvic Girdle Pain that may incorporate the following conditions: Diastasis of the Symphysis Pubis (DSP) Symphysis pubis dysfunction (SPD) Pelvic Joint Syndrome Physiological Pelvic Girdle Relaxation Symptom Giving Pelvic Girdle Relaxation Posterior Pelvic Pain Pelvic Arthropathy Inferior Pubic Shear/ Superior Pubic Shear /Symphyseal Shear Symphysiolysis Osteitis pubis (usually postpartum) Sacroiliitis One-sided Sacroiliac Syndrome /Double Sided Sacroiliac Syndrome Hypermobility "The classification between hormonal and mechanical pelvic girdle instability is no longer used. ... S2CID 12727231 . ^ Symptom-giving p Pelvic Girdle Relaxation of Pregnancy, Postnatal Pelvic Joint Syndrome and Developmental Dysplasia of Hip.
-
Cowpox
Wikipedia
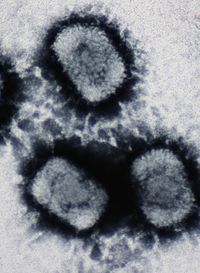
Classification D ICD - 10 : B08.0 ICD - 10-CM : B08.010 ICD - 9-CM : 051.01 MeSH : D015605 SNOMED CT : 70090004 v t e Skin infections , symptoms and signs related to viruses DNA virus Herpesviridae Alpha HSV Herpes simplex Herpetic whitlow Herpes gladiatorum Herpes simplex keratitis Herpetic sycosis Neonatal herpes simplex Herpes genitalis Herpes labialis Eczema herpeticum Herpetiform esophagitis Herpes B virus B virus infection VZV Chickenpox Herpes zoster Herpes zoster oticus Ophthalmic zoster Disseminated herpes zoster Zoster-associated pain Modified varicella-like syndrome Beta Human herpesvirus 6 / Roseolovirus Exanthema subitum Roseola vaccinia Cytomegalic inclusion disease Gamma KSHV Kaposi's sarcoma Poxviridae Ortho Variola Smallpox Alastrim MoxV Monkeypox CPXV Cowpox VV Vaccinia Generalized vaccinia Eczema vaccinatum Progressive vaccinia Buffalopox Para Farmyard pox : Milker's nodule Bovine papular stomatitis Pseudocowpox Orf Sealpox Other Yatapoxvirus : Tanapox Yaba monkey tumor virus MCV Molluscum contagiosum Papillomaviridae HPV Wart / plantar wart Heck's disease Genital wart giant Laryngeal papillomatosis Butcher's wart Bowenoid papulosis Epidermodysplasia verruciformis Verruca plana Pigmented wart Verrucae palmares et plantares BPV Equine sarcoid Parvoviridae Parvovirus B19 Erythema infectiosum Reticulocytopenia Papular purpuric gloves and socks syndrome Polyomaviridae Merkel cell polyomavirus Merkel cell carcinoma RNA virus Paramyxoviridae MeV Measles Togaviridae Rubella virus Rubella Congenital rubella syndrome ("German measles" ) Alphavirus infection Chikungunya fever Picornaviridae CAV Hand, foot, and mouth disease Herpangina FMDV Foot-and-mouth disease Boston exanthem disease Ungrouped Asymmetric periflexural exanthem of childhood Post-vaccination follicular eruption Lipschütz ulcer Eruptive pseudoangiomatosis Viral-associated trichodysplasia Gianotti–Crosti syndrome Taxon identifiers Wikidata : Q12418974 Wikispecies : Cowpox virus EoL : 540225 IRMNG : 11459545 NCBI : 10243
-
Pancreatic Neuroendocrine Tumor
Wikipedia
Up to 60% [ medical citation needed ] of PanNETs are nonsecretory or nonfunctional, in which there is no secretion, or the quantity or type of products, such as pancreatic polypeptide (PPoma), chromogranin A, and neurotensin , do not cause a clinical syndrome although blood levels may be elevated. [10] In total, 85% of PanNETs have an elevated blood marker. [2] Functional tumors are often classified by the hormone most strongly secreted, for example: gastrinoma : the excessive gastrin causes Zollinger–Ellison syndrome (ZES) with peptic ulcers and diarrhea insulinoma : [11] hypoglycemia occurs with concurrent elevations of insulin , proinsulin and C peptide [12] glucagonoma : the symptoms are not all due to glucagon elevations, [12] and include a rash , sore mouth, altered bowel habits, venous thrombosis , and high blood glucose levels [12] VIPoma , producing excessive vasoactive intestinal peptide , which may cause profound chronic w atery d iarrhea and resultant dehydration , h ypokalemia , and a chlorhydria (WDHA or pancreatic cholera syndrome) somatostatinoma : these rare tumors are associated with elevated blood glucose levels, achlorhydria , cholelithiasis , and diarrhea [12] less common types include ACTHoma , CRHoma , calcitoninoma , GHRHoma , GRFoma , and parathyroid hormone–related peptide tumor In these various types of functional tumors, the frequency of malignancy and the survival prognosis have been estimated dissimilarly, but a pertinent accessible summary is available. [13] Diagnosis [ edit ] Because symptoms are non-specific, diagnosis is often delayed. [14] Measurement of hormones including pancreatic polypeptide , gastrin , proinsulin , insulin , glucagon , and vasoactive intestinal peptide can determine if a tumor is causing hypersecretion. [14] [15] Multiphase CT and MRI are the primary modalities for morphologic imaging of PNETs. ... "Inherited pancreatic endocrine tumor syndromes: advances in molecular pathogenesis, diagnosis, management, and controversies" .
-
Prelingual Deafness
Wikipedia
The autosomal dominant hearing loss is when an abnormal gene from one parent is able to cause hearing loss even though the matching gene from the other parent is normal. [9] This can lead to genetic syndromes, such as Down syndrome , Usher syndrome or Waardenburg syndrome , which are concomitant with hearing loss. [10] Acquired hearing loss can be the result of toxicity (drugs given as treatment when in the neonatal intensive care unit) and infections such as meningitis . [11] Treatment [ edit ] Hearing aids and cochlear implants may make the child able to hear sounds in their hearing range—but they don't restore normal hearing.
-
Chancroid
Wikipedia
Use of condom, prophylaxis by azithromycin , syndromic management of genital ulcers, treating patients with reactive syphilis serology are some of the strategies successfully tried in Thailand . [9] Also, treatment of sexual partners is advocated whether they develop symptoms or not as long as there was unprotected sexual intercourse with the patient within 10 days of developing the symptoms. [12] Treatment [ edit ] For the initial stages of the lesion, cleaning with soapy solution is recommended and sitz bath may be beneficial. ... External links [ edit ] Classification D ICD - 10 : A57 ICD - 9-CM : 099.0 MeSH : D002602 DiseasesDB : 5563 External resources MedlinePlus : 000635 eMedicine : emerg/95 v t e Sexually transmitted infections (STI) Bacterial Chancroid ( Haemophilus ducreyi ) Chlamydia , lymphogranuloma venereum ( Chlamydia trachomatis ) Donovanosis ( Klebsiella granulomatis ) Gonorrhea ( Neisseria gonorrhoeae ) Mycoplasma hominis infection ( Mycoplasma hominis ) Syphilis ( Treponema pallidum ) Ureaplasma infection ( Ureaplasma urealyticum ) Protozoal Trichomoniasis ( Trichomonas vaginalis ) Parasitic Crab louse Scabies Viral AIDS ( HIV-1/HIV-2 ) Cancer cervical vulvar penile anal Human papillomavirus (HPV) Genital warts ( condyloma ) Hepatitis B ( Hepatitis B virus ) Herpes simplex HSV-1 & HSV-2 Molluscum contagiosum ( MCV ) General inflammation female Cervicitis Pelvic inflammatory disease (PID) male Epididymitis Prostatitis either Proctitis Urethritis / Non-gonococcal urethritis (NGU) v t e Proteobacteria -associated Gram-negative bacterial infections α Rickettsiales Rickettsiaceae / ( Rickettsioses ) Typhus Rickettsia typhi Murine typhus Rickettsia prowazekii Epidemic typhus , Brill–Zinsser disease , Flying squirrel typhus Spotted fever Tick-borne Rickettsia rickettsii Rocky Mountain spotted fever Rickettsia conorii Boutonneuse fever Rickettsia japonica Japanese spotted fever Rickettsia sibirica North Asian tick typhus Rickettsia australis Queensland tick typhus Rickettsia honei Flinders Island spotted fever Rickettsia africae African tick bite fever Rickettsia parkeri American tick bite fever Rickettsia aeschlimannii Rickettsia aeschlimannii infection Mite-borne Rickettsia akari Rickettsialpox Orientia tsutsugamushi Scrub typhus Flea-borne Rickettsia felis Flea-borne spotted fever Anaplasmataceae Ehrlichiosis : Anaplasma phagocytophilum Human granulocytic anaplasmosis , Anaplasmosis Ehrlichia chaffeensis Human monocytotropic ehrlichiosis Ehrlichia ewingii Ehrlichiosis ewingii infection Rhizobiales Brucellaceae Brucella abortus Brucellosis Bartonellaceae Bartonellosis : Bartonella henselae Cat-scratch disease Bartonella quintana Trench fever Either B. henselae or B. quintana Bacillary angiomatosis Bartonella bacilliformis Carrion's disease , Verruga peruana β Neisseriales M+ Neisseria meningitidis/meningococcus Meningococcal disease , Waterhouse–Friderichsen syndrome , Meningococcal septicaemia M− Neisseria gonorrhoeae/gonococcus Gonorrhea ungrouped: Eikenella corrodens / Kingella kingae HACEK Chromobacterium violaceum Chromobacteriosis infection Burkholderiales Burkholderia pseudomallei Melioidosis Burkholderia mallei Glanders Burkholderia cepacia complex Bordetella pertussis / Bordetella parapertussis Pertussis γ Enterobacteriales ( OX− ) Lac+ Klebsiella pneumoniae Rhinoscleroma , Pneumonia Klebsiella granulomatis Granuloma inguinale Klebsiella oxytoca Escherichia coli : Enterotoxigenic Enteroinvasive Enterohemorrhagic O157:H7 O104:H4 Hemolytic-uremic syndrome Enterobacter aerogenes / Enterobacter cloacae Slow/weak Serratia marcescens Serratia infection Citrobacter koseri / Citrobacter freundii Lac− H2S+ Salmonella enterica Typhoid fever , Paratyphoid fever , Salmonellosis H2S− Shigella dysenteriae / sonnei / flexneri / boydii Shigellosis , Bacillary dysentery Proteus mirabilis / Proteus vulgaris Yersinia pestis Plague / Bubonic plague Yersinia enterocolitica Yersiniosis Yersinia pseudotuberculosis Far East scarlet-like fever Pasteurellales Haemophilus : H. influenzae Haemophilus meningitis Brazilian purpuric fever H. ducreyi Chancroid H. parainfluenzae HACEK Pasteurella multocida Pasteurellosis Actinobacillus Actinobacillosis Aggregatibacter actinomycetemcomitans HACEK Legionellales Legionella pneumophila / Legionella longbeachae Legionnaires' disease Coxiella burnetii Q fever Thiotrichales Francisella tularensis Tularemia Vibrionaceae Vibrio cholerae Cholera Vibrio vulnificus Vibrio parahaemolyticus Vibrio alginolyticus Plesiomonas shigelloides Pseudomonadales Pseudomonas aeruginosa Pseudomonas infection Moraxella catarrhalis Acinetobacter baumannii Xanthomonadaceae Stenotrophomonas maltophilia Cardiobacteriaceae Cardiobacterium hominis HACEK Aeromonadales Aeromonas hydrophila / Aeromonas veronii Aeromonas infection ε Campylobacterales Campylobacter jejuni Campylobacteriosis , Guillain–Barré syndrome Helicobacter pylori Peptic ulcer , MALT lymphoma , Gastric cancer Helicobacter cinaedi Helicobacter cellulitis
-
Methemoglobinemia
Wikipedia
The nitrates can be hazardous to the infants. [22] [23] The link between blue baby syndrome in infants and high nitrate levels is well established for waters exceeding the normal limit of 10 mg/L. [24] [25] However, there is also evidence that breastfeeding is protective in exposed populations. [26] Society and culture [ edit ] Blue Fugates [ edit ] Main article: Blue Fugates The Fugates, a family that lived in the hills of Kentucky, had the hereditary form. ... External links [ edit ] Classification D ICD - 10 : D74 ICD - 9-CM : 289.7 MeSH : D008708 DiseasesDB : 8100 External resources MedlinePlus : 000562 eMedicine : med/1466 emerg/313 ped/1432 v t e Diseases of red blood cells ↑ Polycythemia Polycythemia vera ↓ Anemia Nutritional Micro- : Iron-deficiency anemia Plummer–Vinson syndrome Macro- : Megaloblastic anemia Pernicious anemia Hemolytic (mostly normo- ) Hereditary enzymopathy : Glucose-6-phosphate dehydrogenase deficiency glycolysis pyruvate kinase deficiency triosephosphate isomerase deficiency hexokinase deficiency hemoglobinopathy : Thalassemia alpha beta delta Sickle cell disease / trait Hereditary persistence of fetal hemoglobin membrane : Hereditary spherocytosis Minkowski–Chauffard syndrome Hereditary elliptocytosis Southeast Asian ovalocytosis Hereditary stomatocytosis Acquired AIHA Warm antibody autoimmune hemolytic anemia Cold agglutinin disease Donath–Landsteiner hemolytic anemia Paroxysmal cold hemoglobinuria Mixed autoimmune hemolytic anemia membrane paroxysmal nocturnal hemoglobinuria Microangiopathic hemolytic anemia Thrombotic microangiopathy Hemolytic–uremic syndrome Drug-induced autoimmune Drug-induced nonautoimmune Hemolytic disease of the newborn Aplastic (mostly normo- ) Hereditary : Fanconi anemia Diamond–Blackfan anemia Acquired: Pure red cell aplasia Sideroblastic anemia Myelophthisic Blood tests Mean corpuscular volume normocytic microcytic macrocytic Mean corpuscular hemoglobin concentration normochromic hypochromic Other Methemoglobinemia Sulfhemoglobinemia Reticulocytopenia
-
Urinary Retention
Wikipedia
Specialty Emergency medicine , urology Symptoms Sudden onset : Inability to urinate, low abdominal pain [1] Long term : Frequent urination, loss of bladder control, urinary tract infection [1] Types Acute, chronic [1] Causes Blockage of the urethra, nerve problems, certain medications, weak bladder muscles [1] Diagnostic method Amount of urine in the bladder post urination [1] Treatment Catheter , urethral dilation , urethral stents , surgery [1] Medication Alpha blockers such as terazosin , 5α-reductase inhibitors such as finasteride [1] Frequency 6 per 1,000 per year (males > 40 years old) [1] Urinary retention is an inability to completely empty the bladder . [1] Onset can be sudden or gradual. [1] When of sudden onset, symptoms include an inability to urinate and lower abdominal pain. [1] When of gradual onset, symptoms may include loss of bladder control , mild lower abdominal pain, and a weak urine stream. [1] Those with long-term problems are at risk of urinary tract infections . [1] Causes include blockage of the urethra , nerve problems, certain medications, and weak bladder muscles. [1] Blockage can be caused by benign prostatic hyperplasia (BPH), urethral strictures , bladder stones , a cystocele , constipation , or tumors . [1] Nerve problems can occur from diabetes , trauma, spinal cord problems , stroke , or heavy metal poisoning . [1] Medications that can cause problems include anticholinergics , antihistamines , tricyclic antidepressants , decongestants , cyclobenzaprine , diazepam , NSAIDs , amphetamines , and opioids . [1] Diagnosis is typically based on measuring the amount of urine in the bladder after urinating. [1] Treatment is typically with a catheter either through the urethra or lower abdomen . [1] [2] Other treatments may include medication to decrease the size of the prostate, urethral dilation , a urethral stent , or surgery. [1] Males are more often affected than females. [1] In males over the age of 40 about 6 per 1,000 are affected a year. [1] Among males over 80 this increases 30%. [1] Contents 1 Signs and symptoms 2 Causes 2.1 Bladder 2.2 Prostate 2.3 Postoperative 2.4 Chronic 2.5 Other 3 Diagnosis 4 Complications 5 Treatment 5.1 Medication 5.2 Catheter 5.3 Surgery 5.4 Sitting voiding position 6 Epidemiology 7 References 8 External links Signs and symptoms [ edit ] Onset can be sudden or gradual. [1] When of sudden onset, symptoms include an inability to urinate and lower abdominal pain. [1] When of gradual onset, symptoms may include loss of bladder control , mild lower abdominal pain, and a weak urine stream. [1] Those with long-term problems are at risk of urinary tract infections . [1] Causes [ edit ] Bladder [ edit ] Detrusor sphincter dyssynergia Neurogenic bladder (commonly spinal cord damage, pelvic splanchic nerve damage, cauda equina syndrome, pontine micturition or storage center lesions, demyelinating diseases or Parkinson's disease ) Iatrogenic (caused by medical treatment/procedure) scarring of the bladder neck (commonly from removal of indwelling catheters or cystoscopy operations) Damage to the bladder Prostate [ edit ] Benign prostatic hyperplasia (BPH) Prostate cancer and other pelvic malignancies Prostatitis Penile urethra : Congenital urethral valves Phimosis or pinhole meatus Circumcision Obstruction in the urethra, for example a stricture (usually caused either by injury or STD), a metastasis or a precipitated pseudogout crystal in the urine STD lesions (gonorrhoea causes numerous strictures, leading to a "rosary bead" appearance, whereas chlamydia usually causes a single stricture) Emasculation Postoperative [ edit ] Risk factors include Age: Older people may have degeneration of neural pathways involved with bladder function and it can lead to an increased risk of postoperative urinary retention. [3] The risk of postoperative urinary retention increases up to 2.11 fold for people older than 60 years. [3] Medications: Anticholinergics and medications with anticholinergic properties, alpha-adrenergic agonists , opiates , nonsteroidal anti-inflammatories (NSAIDs), calcium-channel blockers and beta-adrenergic agonists , may increase the risk. [3] Anesthesia: General anesthetics during surgery may cause bladder atony by acting as a smooth muscle relaxant. [3] General anesthetics can directly interfere with autonomic regulation of detrusor tone and predispose people to bladder overdistention and subsequent retention. [3] Spinal anesthesia results in a blockade of the micturition reflex . [3] Spinal anesthesia shows a higher risk of postoperative urinary retention compared to general anesthesia. [3] Benign prostatic hyperplasia : Men with benign prostatic hyperplasia are at an increased risk of acute urinary retention. [3] Surgery related: Operative times longer than 2 hours may lead to an increased risk of postoperative urinary retention 3-fold. [3] Chronic [ edit ] Chronic urinary retention that is due to bladder blockage which can either be as a result of muscle damage or neurological damage. [4] If the retention is due to neurological damage, there is a disconnect between the brain to muscle communication, which can make it impossible to completely empty the bladder. [4] If the retention is due to muscle damage, it is likely that the muscles are not able to contract enough to completely empty the bladder. [4] The most common cause of chronic urinary retention is BPH. [1] BPH is a result of the ongoing process of testosterone being converted to dihydrotestosterone which stimulates prostate growth. [5] Over a person's lifetime, the prostate experiences constant growth due to the conversion of testosterone to dihydrotestosterone. [5] This can cause the prostate to push on the urethra and block it, which can lead to urinary retention. [5] Other [ edit ] Tethered spinal cord syndrome Psychogenic causes (psychosocial stresses, fear associated with urination, paruresis ("shy bladder syndrome")- in extreme cases, urinary retention can result) Consumption of some psychoactive substances , mainly stimulants , such as MDMA and amphetamine . ... In acute cases of urinary retention where associated symptoms in the lumbar spine are present such as pain, numbness (saddle anesthesia), parasthesias, decreased anal sphincter tone, or altered deep tendon reflexes, an MRI of the lumbar spine should be considered to further assess cauda equina syndrome . Complications [ edit ] Play media The urinary bag of a person with post obstructive diuresis Urinary retention often occurs without warning.
-
Exercise-Induced Bronchoconstriction
Wikipedia
Fact sheet: Exercise-induced asthma Classification D ICD - 10 : J45.990 ICD - 9-CM : 493.81 MeSH : D001250 DiseasesDB : 31728 External resources MedlinePlus : 000036 eMedicine : sports/155 v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis
-
Lymphogranuloma Venereum
Wikipedia
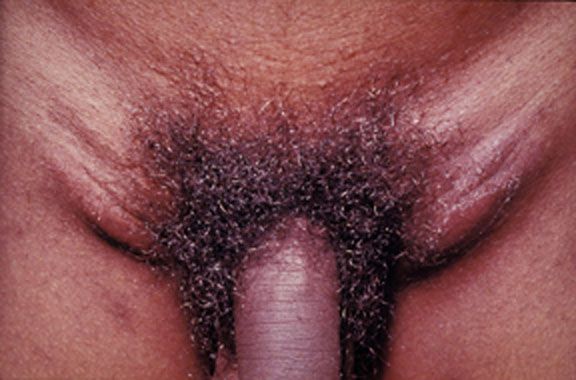
Inoculation at the mucous lining of external sex organs (penis and vagina) can lead to the inguinal syndrome named after the formation of buboes or abscesses in the groin (inguinal) region where draining lymph nodes are located. These signs usually appear from 3 days to a month after exposure. The rectal syndrome (Lymphogranuloma venereum proctitis, or LGVP) arises if the infection takes place via the rectal mucosa (through anal sex) and is mainly characterized by proctocolitis or proctitis symptoms. [12] The pharyngeal syndrome is rare. ... External links [ edit ] Classification D ICD - 10 : A55 ICD - 9-CM : 099.1 MeSH : D008219 DiseasesDB : 29101 External resources MedlinePlus : 000634 eMedicine : emerg/304 med/1356 derm/617 Sexually transmitted infections (BMJ publishing) v t e Sexually transmitted infections (STI) Bacterial Chancroid ( Haemophilus ducreyi ) Chlamydia , lymphogranuloma venereum ( Chlamydia trachomatis ) Donovanosis ( Klebsiella granulomatis ) Gonorrhea ( Neisseria gonorrhoeae ) Mycoplasma hominis infection ( Mycoplasma hominis ) Syphilis ( Treponema pallidum ) Ureaplasma infection ( Ureaplasma urealyticum ) Protozoal Trichomoniasis ( Trichomonas vaginalis ) Parasitic Crab louse Scabies Viral AIDS ( HIV-1/HIV-2 ) Cancer cervical vulvar penile anal Human papillomavirus (HPV) Genital warts ( condyloma ) Hepatitis B ( Hepatitis B virus ) Herpes simplex HSV-1 & HSV-2 Molluscum contagiosum ( MCV ) General inflammation female Cervicitis Pelvic inflammatory disease (PID) male Epididymitis Prostatitis either Proctitis Urethritis / Non-gonococcal urethritis (NGU) v t e Bacterial diseases due to gram negative non- proteobacteria ( BV4 ) Spirochaete Spirochaetaceae Treponema Treponema pallidum Syphilis / bejel Yaws Treponema carateum ( Pinta ) Treponema denticola Borrelia Borrelia burgdorferi / Borrelia afzelii Lyme disease Erythema migrans Neuroborreliosis Borrelia recurrentis ( Louse borne relapsing fever ) Borrelia hermsii / Borrelia duttoni / Borrelia parkeri ( Tick borne relapsing fever ) Leptospiraceae Leptospira Leptospira interrogans ( Leptospirosis ) Chlamydiaceae Chlamydia Chlamydia psittaci ( Psittacosis ) Chlamydia pneumoniae Chlamydia trachomatis Chlamydia Lymphogranuloma venereum Trachoma Bacteroidetes Bacteroides fragilis Tannerella forsythia Capnocytophaga canimorsus Porphyromonas gingivalis Prevotella intermedia Fusobacteria Fusobacterium necrophorum ( Lemierre's syndrome ) Fusobacterium nucleatum Fusobacterium polymorphum Streptobacillus moniliformis ( Rat-bite fever / Haverhill fever )
-
Acute Exacerbation Of Chronic Obstructive Pulmonary Disease
Wikipedia
CS1 maint: archived copy as title ( link ) ^ MORBIDITY & MORTALITY: 2009 CHART BOOK ON CARDIOVASCULAR, LUNG, AND BLOOD DISEASES Archived October 19, 2013, at the Wayback Machine National Heart, Lung, and Blood Institute External links [ edit ] Classification D v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosisCOPD, CRP, IL17A, ACE2, TNF, IFNG, IL1B, IL4, AVP, PIK3CD, CCL2, PIK3CB, PIK3CG, PIK3CA, ORM1, PTPRC, MUC1, RNASE2, RNASE3, TMOD1, SFTPD, TIMP4, LGALS3, EPX, HSPB3, LITAF, C1RL, FSD1, SLC2A10, FSD1L, BANF2, MIR146A, MIR149, MMP12, ALAS2, CXCL10, IL18, ANPEP, APC, SERPING1, C1QC, CA1, CASP1, CD28, TNFSF8, CHGA, COL4A5, DPP4, ELANE, FCGR3A, FCGR3B, MSTN, CXCR3, GRN, HP, HSPB1, HSPB2, IL2, IL6, CXCL8, IL13, ALB, MIR23A
-
Diabetes And Pregnancy
Wikipedia
., oxidative stress , by activating protein kinase C [6] that leads to apoptosis of some cells. [6] A hyperglycemic maternal environment has also been associated with neonates that are at greater risk for development of negative health outcomes such as future obesity, insulin resistance, type 2 diabetes mellitus, and metabolic syndrome. [7] During the first trimester, besides increased birth defect risks, having a miscarriage is also increased due to abnormal development in the early stages of pregnancy. [8] When blood glucose is not controlled, shortly after birth, the infant's lungs may be under developed and can cause respiratory problems. [4] Hypoglycemia can occur after birth if the mother's blood sugar was high close to the time of delivery, which causes the baby to produces extra insulin of its own. ... External links [ edit ] CDC’s National Center on Birth Defects and Developmental Disabilities v t e Pregnancy and childbirth Planning Birth control Natural family planning Pre-conception counseling Conception Assisted reproductive technology Artificial insemination Fertility medication In vitro fertilisation Fertility awareness Unintended pregnancy Testing 3D ultrasound Obstetric ultrasonography Pregnancy test Home testing Prenatal diagnosis Prenatal Anatomy Amniotic fluid Amniotic sac Endometrium Placenta Development Fundal height Gestational age Human embryogenesis Maternal physiological changes Postpartum physiological changes Care Nutrition Environmental toxicants In pregnancy Prenatal Concomitant conditions Drinking Diabetes mellitus Smoking Vaping SLE Sexual activity during pregnancy Procedures Amniocentesis Cardiotocography Chorionic villus sampling Nonstress test Abortion Childbirth Preparation Bradley method Hypnobirthing Lamaze Nesting instinct Roles Doula Birth attendant Men's roles Midwife Obstetrician Perinatal nurse Traditional birth attendant Delivery Bloody show Childbirth positions Home birth Multiple birth Natural childbirth Pelvimetry / Bishop score Cervical dilation Cervical effacement Position Presentation Breech Cephalic Shoulder Rupture of membranes Unassisted childbirth Uterine contraction Water birth Postpartum Maternal Postpartum confinement Sex after pregnancy Psychiatric disorders of childbirth Postpartum physiological changes Roles Doula Health visitor Lactation consultant Monthly nurse Confinement nanny Infant Adaptation to extrauterine life Child care Congenital disorders Obstetric history Gravidity and parity v t e Diabetes Types Type 1 Type 2 LADA Gestational diabetes Diabetes and pregnancy Prediabetes Impaired fasting glucose Impaired glucose tolerance Insulin resistance KPD MODY Neonatal Transient Permanent Type 3c (pancreatogenic) Type 3 Blood tests Blood sugar level Glycosylated hemoglobin Glucose tolerance test Postprandial glucose test Fructosamine Glucose test C-peptide Noninvasive glucose monitor Insulin tolerance test Management Diabetic diet Anti-diabetic drugs Insulin therapy intensive conventional pulsatile Cure Embryonic stem cells Artificial pancreas Other Gastric bypass surgery Complications Diabetic comas Hypoglycemia Ketoacidosis Hyperosmolar hyperglycemic state Diabetic foot ulcer Neuropathic arthropathy Organs in diabetes Blood vessels Muscle Kidney Nerves Retina Heart Diabetic skin disease Diabetic dermopathy Diabetic bulla Diabetic cheiroarthropathy Neuropathic ulcer Hyperglycemia Hypoglycemia Other Glossary of diabetes History of diabetes Notable people with type 1 diabetes v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy CategoryGC, GAPDH, VEGFA, ADM, REN, SLC2A1, IGF2, GH2, PGM1, SLC2A9, SLC2A6, TXNIP, PTH, MIR15B, RARRES2, MIR15A, MIR129-2, SLC2A4, SLC6A4, SLC9A1, ATP6AP2, SIRT1, CCRL2, ADIPOQ, PIK3CD, PPARGC1A, ABCG2, GDF15, ACO1, MTHFR, ABCB1, FGF2, ALX3, APCS, BAX, BCL2, CMKLR1, ABCC2, CSH1, CSH2, EPO, FGF13, PGF, GCK, FOXA2, ICAM1, IGF1, LEP, LEPR, SH2D1A, MBL2, MMP14, DIP
-
Krabbe Disease
Wikipedia
External links [ edit ] GeneReviews/NCBI/NIH/UW entry on Krabbe disease OMIM entries on Krabbe disease Classification D ICD - 10 : E75.2 ICD - 10-CM : E75.23 ICD - 9-CM : 330.0 OMIM : 245200 MeSH : D007965 DiseasesDB : 29468 External resources MedlinePlus : 001198 eMedicine : ped/2892 GeneReviews : Krabbe Disease Orphanet : 487 v t e Lysosomal storage diseases : Inborn errors of lipid metabolism ( Lipid storage disorders ) Sphingolipidoses (to ceramide ) From ganglioside ( gangliosidoses ) Ganglioside : GM1 gangliosidoses GM2 gangliosidoses ( Sandhoff disease Tay–Sachs disease AB variant ) From globoside Globotriaosylceramide : Fabry's disease From sphingomyelin Sphingomyelin : phospholipid: Niemann–Pick disease ( SMPD1-associated type C ) Glucocerebroside : Gaucher's disease From sulfatide ( sulfatidoses leukodystrophy ) Sulfatide : Metachromatic leukodystrophy Multiple sulfatase deficiency Galactocerebroside : Krabbe disease To sphingosine Ceramide : Farber disease NCL Infantile Jansky–Bielschowsky disease Batten disease Other Cerebrotendineous xanthomatosis Cholesteryl ester storage disease ( Lysosomal acid lipase deficiency / Wolman disease ) Sea-blue histiocytosis v t e Multiple sclerosis and other demyelinating diseases of the central nervous system Signs and symptoms Ataxia Depression Diplopia Dysarthria Dysphagia Fatigue Incontinence Nystagmus Optic neuritis Pain Uhthoff's phenomenon Investigations and diagnosis Multiple sclerosis diagnosis McDonald criteria Poser criteria Clinical Clinically isolated syndrome Expanded Disability Status Scale Serological and CSF Oligoclonal bands Radiological Radiologically isolated syndrome Lesional demyelinations of the central nervous system Dawson's fingers Approved [ by whom? ] treatment Management of multiple sclerosis Alemtuzumab Cladribine Dimethyl fumarate Fingolimod Glatiramer acetate Interferon beta-1a Interferon beta-1b Mitoxantrone Natalizumab Ocrelizumab Ozanimod Siponimod Teriflunomide Other treatments Former Daclizumab Multiple sclerosis research Demyleinating diseases Autoimmune Multiple sclerosis Neuromyelitis optica Diffuse myelinoclastic sclerosis Inflammatory Acute disseminated encephalomyelitis MOG antibody disease Balo concentric sclerosis Marburg acute multiple sclerosis Neuromyelitis optica Diffuse myelinoclastic sclerosis Tumefactive multiple sclerosis Experimental autoimmune encephalomyelitis Hereditary Adrenoleukodystrophy Alexander disease Canavan disease Krabbe disease Metachromatic leukodystrophy Pelizaeus–Merzbacher disease Leukoencephalopathy with vanishing white matter Megalencephalic leukoencephalopathy with subcortical cysts CAMFAK syndrome Other Central pontine myelinolysis Marchiafava–Bignami disease Mitochondrial DNA depletion syndrome Other List of multiple sclerosis organizations List of people with multiple sclerosis Multiple sclerosis drug pipeline Pathophysiology
-
Csf Leak (Cerebrospinal Fluid Leak)
Mayo_clinic
Risk factors Risk factors for spinal CSF leaks include: Having a previous surgery or procedure on or around the spine Connective tissue disorders such as Marfan syndrome or Ehlers-Danlos syndrome Risk factors for cranial CSF leaks include: Having a previous surgery on or around the skull Obesity Obstructive sleep apnea Head trauma Tumor at the skull base Abnormalities of the skull base or inner ear Complications Possible complications of a cranial CSF leak that is left untreated include meningitis and air entering the spaces surrounding the brain (tension pneumocephalus).
-
Morning Sickness
Mayo_clinic
Using marijuana may result in a nausea and vomiting syndrome called cannabinoid hyperemesis syndrome.
-
Glycogen Storage Disease Ib
Omim
Kuijpers et al. (2003) studied neutrophils from children with infections (active pneumonia or septicemia) or with other neutropenic syndromes (Shwachman-Diamond syndrome; 260400), but to date had not observed circulating apoptotic neutrophils in these patients.
-
Congenital Disorder Of Glycosylation, Type Ib
Omim
The infants, who died between the ages of 4 and 21 months, also had antithrombin III deficiency (613118), a typical feature of CDG syndromes. Niehues et al. (1998) reported an 11-month-old boy who presented with diarrhea and vomiting. ... Vuillaumier-Barrot et al. (2002) found that the protein-losing enteropathy-hepatic fibrosis syndrome described in the Saguenay-Lac-Saint-Jean region of Quebec, reported by Pelletier et al. (1986), is caused by an arg295-to-his mutation in the MPI gene (R295H; 154550.0005), and is therefore a form of CDG Ib.
-
Muscular Dystrophy-Dystroglycanopathy (Congenital With Mental Retardation), Type B, 1
Omim
They are less severe than muscular dystrophy-dystroglycanopathy with brain and eye anomalies (type A; see MDDGA1, 236670), previously designated Walker-Warburg syndrome (WWS) or muscle-eye-brain disease (MEB), and more severe than limb-girdle muscular dystrophy-dystroglycanopathy (type C; see MDDGC1, 609308). ... All 5 patients had a milder form of Walker-Warburg syndrome, with less severe structural brain abnormalities and absence of severe eye abnormalities, except for myopia in some cases.
-
Fire Breather's Pneumonia
Wikipedia
Severe cases may lead to acute respiratory distress syndrome (ARDS). Causes [ edit ] Fire breather’s pneumonia is caused by the entrance of hydrocarbon fuels into the bronchial tree , usually due to accidental aspiration or inhalation during a fire performance show. ... It may have potential benefit in large (> 30 cc), intentional ingestion of compounds with systemic toxicity. [13] Prognosis after peak symptoms is typically good, with most patients making a full recovery in weeks to months. [4] [5] See also [ edit ] Fire breathing Fire eating Fire dancing Acute respiratory distress syndrome References [ edit ] ^ Karacan O, Yilmaz I, Eyüboğlu FO (2006).