-
Acral Nevus
Wikipedia
External links [ edit ] Classification D ICD - 10 : D22.9 v t e Skin cancer of nevi and melanomas Melanoma Mucosal melanoma Superficial spreading melanoma Nodular melanoma lentigo Lentigo maligna / Lentigo maligna melanoma Acral lentiginous melanoma Amelanotic melanoma Desmoplastic melanoma Melanoma with features of a Spitz nevus Melanoma with small nevus-like cells Polypoid melanoma Nevoid melanoma Melanocytic tumors of uncertain malignant potential Nevus / melanocytic nevus Nevus of Ito / Nevus of Ota Spitz nevus Pigmented spindle cell nevus Halo nevus Pseudomelanoma Blue nevus of Jadassohn–Tièche Cellular Epithelioid Deep penetrating Amelanotic Malignant Congenital melanocytic nevus ( Giant Medium-sized Small-sized ) Balloon cell nevus Dysplastic nevus / Dysplastic nevus syndrome Acral nevus Becker's nevus Benign melanocytic nevus Nevus spilus This cutaneous condition article is a stub .
- Waxy Flexibility Wikipedia
-
Superficial Spreading Melanoma
Wikipedia
External links [ edit ] Classification D ICD - 10 : C43 ( ILDS C43.L20) ICD-O : M8743/3 Fact File from the Royal College of Pathologists of Australasia (pdf) v t e Skin cancer of nevi and melanomas Melanoma Mucosal melanoma Superficial spreading melanoma Nodular melanoma lentigo Lentigo maligna / Lentigo maligna melanoma Acral lentiginous melanoma Amelanotic melanoma Desmoplastic melanoma Melanoma with features of a Spitz nevus Melanoma with small nevus-like cells Polypoid melanoma Nevoid melanoma Melanocytic tumors of uncertain malignant potential Nevus / melanocytic nevus Nevus of Ito / Nevus of Ota Spitz nevus Pigmented spindle cell nevus Halo nevus Pseudomelanoma Blue nevus of Jadassohn–Tièche Cellular Epithelioid Deep penetrating Amelanotic Malignant Congenital melanocytic nevus ( Giant Medium-sized Small-sized ) Balloon cell nevus Dysplastic nevus / Dysplastic nevus syndrome Acral nevus Becker's nevus Benign melanocytic nevus Nevus spilus
- Lipodystrophy, Familial Partial, Type 1 Omim
- Hemochromatosis Type 4 Orphanet
-
Spinal Muscular Atrophy
Gene_reviews
Disorders to Consider in the Differential Diagnosis of Spinal Muscular Atrophy (SMA) View in own window Age of Onset Disorder Gene(s) or Region MOI Clinical Features of Differential Diagnosis Disorder Overlapping w/SMA Distinguishing from SMA Congenital to <6 mos X-linked infantile SMA UBA1 XL Hypotonia, weakness, areflexia Multiple congenital contractures, intrauterine fractures SMARD1 1 (OMIM 604320) IGHMBP2 AR Weakness, respiratory failure, hypo- or areflexia Distal predominant weakness, diaphragmatic paralysis GARS1 -related infantile-onset SMA 2 (OMIM 619042) GARS1 AD Hypotonia, weakness, areflexia Diaphragmatic paralysis, sensory involvement Prader-Willi syndrome 15q11.2-q13 3 See footnote 3. Hypotonia, feeding difficulties Poor respiratory effort is rare. Myotonic dystrophy type 1 DMPK AD Hypotonia, muscle weakness Marked facial weakness Congenital muscular dystrophy Many genes AR AD Hypotonia, muscle weakness CNS, eye involvement, possible increased tone Zellweger spectrum disorder PEX family of genes AR Hypotonia Hepatosplenomegaly, CNS Congenital myasthenic syndromes CHAT CHRNE COLQ DOK7 GFPT1 RAPSN 4 AR AD Hypotonia Ophthalmoplegia, ptosis, episodic respiratory failure Pompe disease GAA AR Hypotonia Cardiomegaly Other: congenital myopathies, 5 metabolic/mitochondrial myopathies, 6 peripheral neuropathies 7 >6 mos Botulism NA NA Proximal muscle weakness, decreased reflexes Prominent cranial nerve palsies, acute onset Later childhood Guillain-Barré syndrome NA Muscle weakness Subacute onset, sensory involvement Duchenne muscular dystrophy DMD XL Muscle weakness, motor regression Serum creatine kinase concentration 10-20x > normal Hexosaminidase A deficiency (juvenile, chronic, & adult-onset variants) HEXA AR Lower motor neuron disease Slow progression, progressive dystonia, spinocerebellar degeneration, cognitive/psychiatric involvement Fazio-Londe syndrome (See Riboflavin Transporter Deficiency Neuronopathy.) ... CMT2D and dSMA-V are characterized by adolescent or early-adult onset of unique patterns of motor and sensory manifestations with age of onset ranging from eight to 36 years. 3. Prader-Willi syndrome (PWS) is caused by an absence of expression of imprinted genes in the paternally derived PWS / Angelman syndrome region (15q11.2-q13) of chromosome 15 by one of several genetic mechanisms (paternal deletion, maternal uniparental disomy 15, and rarely an imprinting defect). ... The most commonly associated genes include those listed in the table (see Congenital Myasthenic Syndromes). 5. Congenital myopathies: see X-Linked Centronuclear Myopathy 6.SMN1, SMN2, TRPV4, ASCC1, ATAD3A, DYNC1H1, BICD2, VRK1, UBA1, ASAH1, IGHMBP2, TRIP4, VAPB, EXOSC8, SIGMAR1, TK2, CHCHD10, DNAJB2, SNURF, NAIP, FBXO38, KCNK9, DYSF, PLS3, SNRPN, TBCE, PLEKHG5, LSM2, MAP1B, STMN1, ATP7A, CNTNAP1, GEMIN2, SOD1, IGFALS, ACTB, FUS, TP53, BCL2, SERF1A, ZPR1, IGF1, NCALD, KHDRBS1, SLC9A3R2, GUSBP1, GUSBP3, GTF2H2, MSTN, SCAF11, SYNCRIP, DDX20, ZEB2, SCO2, GUSBP14, DMD, IFI44, H3P33, SERF1B, CARM1, TMEM41B, NEFL, AR, WDR77, HDAC9, TARDBP, COPA, EXOSC3, DCPS, VIM, RPL3, CORO1C, LMNA, PART1, MUC1, HTRA2, LIX1, PTEN, DROSHA, RNPC3, SLCO2A1, CHODL, CARD16, SNCA, SLC25A21, NRXN2, TIA1, CHP1, PLA1A, SLC7A10, AAVS1, ALB, CDK5, DES, CTNNB1, MAPK14, AKT1, GJB1, ETFA, GTF2H1, GARS1, ACVR2B, MORC2, ITGA11, COMP, SETX, KIF1B, NCDN, CREM, CRK, CREB1, IGF2, CD2AP, NUP62, CNTN1, RNF19A, POLDIP2, EIF3K, SGSM3, CHML, KLF15, CD47, GEMIN4, HAPLN1, CSF2, STRAP, HNRNPR, CLOCK, MAD2L1BP, NCOR2, EEF1D, HDAC4, TYMP, SLC23A2, DPP4, ABCB6, RBM7, POP7, GUSBP15, DNM1, SMNDC1, PRMT5, FST, CCN2, AHSA1, CTF1, CELF2, PPARGC1A, CD36, CD40, LEF1, DCTN4, GRAP2, ANXA1, FBXO32, ANG, ALPP, C9orf72, CYP4V2, HCN1, ALPI, GTF2H5, MIR146A, MIR206, MIR223, MIR23A, MIR335, MIR375, MIR431, OCLNP1, HNRNPA1P10, POTEF, AGRP, ADRB2, RNU4ATAC, RNU6ATAC, OCLN, UPK3B, CDCA5, SLC25A46, STARD13, KIDINS220, CAT, CASP8, POP5, VPS54, ARID4B, GEMIN8, WRAP53, CASP3, CANX, CALR, BMP4, CIP2A, APOE, BICD1, ARHGAP22, HCN2, GORASP1, WNK1, BCL2L1, GEMIN6, ATP6V1B2, CCDC8, ARSF, MAGT1, NR1D1, EPHA4, ELAVL4, EMX1, NOS2, OXA1L, PAX3, PAX7, PFN1, PGK1, HTT, PML, PPARG, MAPK1, MAPK10, PSMD4, GTF2H4, PTGS2, PVALB, RAB1A, RELA, RNASE4, BRD2, GTF2H3, RPL9, RPS6KB2, RYR1, S100A1, S100A10, NOS1, NFKB1, HDAC2, MBP, IAPP, IL1B, IL6, IL12A, KIT, LAMC2, HSPG2, LBR, LGALS3, HOXA5, HNRNPA1, MDM2, NEFH, MDM4, MECP2, RAB8A, MAP3K10, MNAT1, NRG1, MYH7, MYOG, HEXA, NCL, NEDD8, S100B, ATXN2, CCL2, KHSRP, BEST1, GAPDH, ZAP70, AIMP2, SPPM, CDK2AP1, COIL, KDSR, FUT1, FOXO1, FCN2, BECN1, UCHL1, SOCS2, CDK5R1, ARHGEF7, SQSTM1, BCL10, ERCC3, ARTN, ERCC2, ERBB4, KLF4, IGF1R, VDAC2, GART, CCL18, STAT5A, CCL21, XCL1, SRSF1, TRA2B, SLC1A3, GSK3B, GRIN2A, GM2A, ACHE, SPP1, SRF, STAT5B, TTN, STATH, SYT1, TBCD, GFAP, PPP1R11, TFRC, GCHFR, GCG, TNF, GATA6, TRH, H3P40
-
Aneurysm
Wikipedia
Renal (kidney) aneurysm [ edit ] Flank pain and tenderness Hypertension Haematuria Signs of hypovolemic shock Risk factors [ edit ] Risk factors for an aneurysm include diabetes , obesity , hypertension , tobacco use , alcoholism , high cholesterol, copper deficiency , increasing age, and tertiary syphilis infection. [17] : 602 Connective tissue disorders such as Loeys-Dietz syndrome, Marfan syndrome, and certain forms of Ehlers-Danlos syndrome are also associated with aneurysms. Aneurysms, dissections, and ruptures in individuals under 40 years of age are a major diagnostic criteria of the vascular form of Ehlers-Danlos syndrome (vEDS). [19] Specific infective causes associated with aneurysm include: Advanced syphilis infection resulting in syphilitic aortitis and an aortic aneurysm Tuberculosis , causing Rasmussen's aneurysms Brain infections , causing infectious intracranial aneurysms A minority of aneurysms are associated with genetic factors. ... "A Cough Deteriorating Gross Hematuria: A Clinical Sign of a Forthcoming Life-Threatening Rupture of an Intraparenchymal Aneurysm of Renal Artery (Wunderlich's Syndrome)" . Case Reports in Vascular Medicine . 2013 : 452317. doi : 10.1155/2013/452317 . ... Introduction to Neurogenic Communication Disorders . p. 93. ^ Byers PH. Vascular Ehlers-Danlos Syndrome. 1999 Sep 2 [Updated 2019 Feb 21]. ... @neurIST – Integrated Biomedical Informatics for the Management of Cerebral Aneurysms Brain aneurysm and percent packing calculator Classification D ICD - 10 : I72 ICD - 9-CM : 442 MeSH : D000783 DiseasesDB : 15088 External resources MedlinePlus : 001122 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension v t e Cerebrovascular diseases including stroke Ischaemic stroke Brain Anterior cerebral artery syndrome Middle cerebral artery syndrome Posterior cerebral artery syndrome Amaurosis fugax Moyamoya disease Dejerine–Roussy syndrome Watershed stroke Lacunar stroke Brain stem Brainstem stroke syndrome Medulla Medial medullary syndrome Lateral medullary syndrome Pons Medial pontine syndrome / Foville's Lateral pontine syndrome / Millard-Gubler Midbrain Weber's syndrome Benedikt syndrome Claude's syndrome Cerebellum Cerebellar stroke syndrome Extracranial arteries Carotid artery stenosis precerebral Anterior spinal artery syndrome Vertebrobasilar insufficiency Subclavian steal syndrome Classification Brain ischemia Cerebral infarction Classification Transient ischemic attack Total anterior circulation infarct Partial anterior circulation infarct Other CADASIL Binswanger's disease Transient global amnesia Haemorrhagic stroke Extra-axial Epidural Subdural Subarachnoid Cerebral/Intra-axial Intraventricular Brainstem Duret haemorrhages General Intracranial hemorrhage Aneurysm Intracranial aneurysm Charcot–Bouchard aneurysm Other Cerebral vasculitis Cerebral venous sinus thrombosis Authority control BNE : XX555959 BNF : cb11981676n (data) GND : 4131419-0 LCCN : sh85004986 NDL : 00561683
-
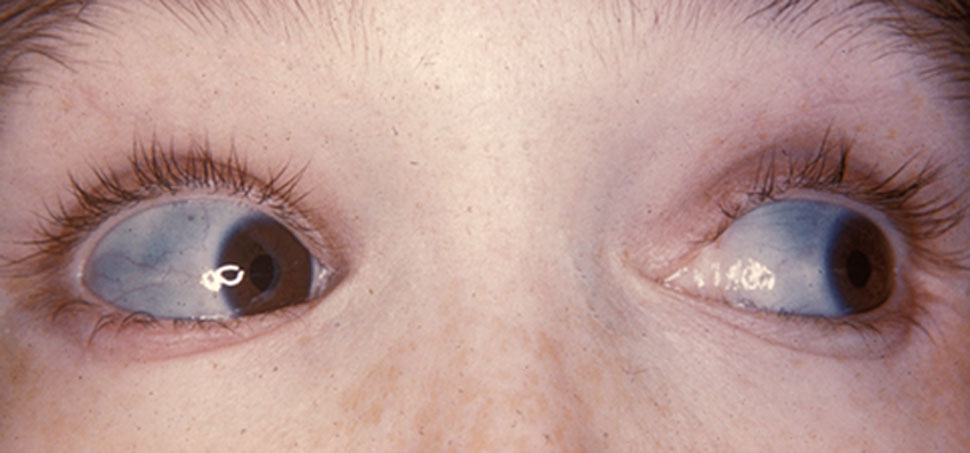
Osteogenesis Imperfecta
Wikipedia
These mutations can also cause autosomal recessive Bruck syndrome which is similar to OI. Type XII [ edit ] OI caused by a frameshift mutation in SP7. ... These factors include; intracellular stress, abnormal tissue mineralization, abnormal cell to cell interactions, abnormal cell-matrix interactions, a compromised cell matrix structure, and disturbances between non-collagenous proteins and collagen. [39] Previous research lead to the belief that OI was an autosomal dominant disorder with few other variations in genomes. [40] However, In the past several years, there has been the identification of autosomal recessive forms of the disorder. [41] Recessive forms of OI relate heavily to defects in the collagen chaperones responsible for production of pro-collagen and the assembly of the related proteins. [42] Examples of collagen chaperones that are defective in OI patients include chaperone HSP47 ( Cole-Carpenter syndrome ) and FKBP65. [43] Mutations in these chaperones result in an improper folding pattern in the collagen 1 proteins which causes the recessive form of the disorder. [43] There are three significant types of OI that are a result of mutations in the collagen prolyl 3-hydroxylation complex (components CRTAP, P3H1, and CyPB). [43] These components are responsible for the modification of collagen a1(l)Pro986. [43] Mutations in other genes such as SP7, SERPINF1, TMEM38B and BMP1 can also lead to irregularly formed proteins and enzymes that result in the recessive form of Osteogenesis Imperfecta. [43] There are now links to defects in other proteins caused by genetic mutations ranging in function from structural proteins to enzymatic proteins. [40] A link between proteins such as pigment epithelium-derived factor (PEDF) and bone-restricted interferon-induced transmembrane protein (BRIL) are causes for type V and VI Osteogenesis Imperfecta. [44] Defects in these proteins lead to defective bone mineralization which aids in the formation of the brittle bone symptom of Osteogenesis Imperfecta. [44] Additionally, mutations in the COL1A1 and COL1A2 genes can result in signal disruptions of the extracellular matrix signaling that is present within the collagen proteins, causing worsened symptoms of the disorder. [45] A single point mutation in the untranslated 5' region of the IFITM5 gene was recently discovered and linked directly to OI type V. [46] Another single point mutation in the region that codes for collagen proteins on the IFITM5 gene was also found to be present in patients with substantially more severe versions of OI than just type V. [46] Osteogenesis imperfecta has also been seen as an X-linked related genetic disorder in some rare cases but continues to be a primarily heterozygous dominant disorder. [47] Pathophysiology [ edit ] People with OI are born with defective connective tissue, or without the ability to make it, usually because of a deficiency of Type-I collagen . [48] This deficiency arises from an amino acid substitution of glycine to bulkier amino acids in the collagen triple helix structure. ... Other differential diagnoses include rickets , osteomalacia , and other rare skeletal syndromes. Treatment [ edit ] There is no cure. [4] Maintaining a healthy lifestyle by exercising and avoiding smoking can help prevent fractures. ... Among some of the most common alternatives are Ekman-Lobstein syndrome, Vrolik syndrome, and the colloquial glass-bone disease. ... Osteogenesis Imperfecta Overview NIH Osteoporosis and Related Bone Diseases ~ National Resource Center v t e Diseases of collagen , laminin and other scleroproteins Collagen disease COL1 : Osteogenesis imperfecta Ehlers–Danlos syndrome, types 1, 2, 7 COL2 : Hypochondrogenesis Achondrogenesis type 2 Stickler syndrome Marshall syndrome Spondyloepiphyseal dysplasia congenita Spondyloepimetaphyseal dysplasia, Strudwick type Kniest dysplasia (see also C2/11 ) COL3 : Ehlers–Danlos syndrome, types 3 & 4 Sack–Barabas syndrome COL4 : Alport syndrome COL5 : Ehlers–Danlos syndrome, types 1 & 2 COL6 : Bethlem myopathy Ullrich congenital muscular dystrophy COL7 : Epidermolysis bullosa dystrophica Recessive dystrophic epidermolysis bullosa Bart syndrome Transient bullous dermolysis of the newborn COL8: Fuchs' dystrophy 1 COL9: Multiple epiphyseal dysplasia 2, 3, 6 COL10: Schmid metaphyseal chondrodysplasia COL11: Weissenbacher–Zweymüller syndrome Otospondylomegaepiphyseal dysplasia (see also C2/11 ) COL17: Bullous pemphigoid COL18: Knobloch syndrome Laminin Junctional epidermolysis bullosa Laryngoonychocutaneous syndrome Other Congenital stromal corneal dystrophy Raine syndrome Urbach–Wiethe disease TECTA DFNA8/12, DFNB21 see also fibrous proteins v t e Osteochondrodysplasia Osteodysplasia/ / osteodystrophy Diaphysis Camurati–Engelmann disease Metaphysis Metaphyseal dysplasia Jansen's metaphyseal chondrodysplasia Schmid metaphyseal chondrodysplasia Epiphysis Spondyloepiphyseal dysplasia congenita Multiple epiphyseal dysplasia Otospondylomegaepiphyseal dysplasia Osteosclerosis Raine syndrome Osteopoikilosis Osteopetrosis Other/ungrouped FLNB Boomerang dysplasia Opsismodysplasia Polyostotic fibrous dysplasia McCune–Albright syndrome Chondrodysplasia / chondrodystrophy (including dwarfism ) Osteochondroma osteochondromatosis Hereditary multiple exostoses Chondroma / enchondroma enchondromatosis Ollier disease Maffucci syndrome Growth factor receptor FGFR2 : Antley–Bixler syndrome FGFR3 : Achondroplasia Hypochondroplasia Thanatophoric dysplasia COL2A1 collagen disease Achondrogenesis type 2 Hypochondrogenesis SLC26A2 sulfation defect Achondrogenesis type 1B Autosomal recessive multiple epiphyseal dysplasia Atelosteogenesis, type II Diastrophic dysplasia Chondrodysplasia punctata Rhizomelic chondrodysplasia punctata Conradi–Hünermann syndrome Other dwarfism Fibrochondrogenesis Short rib – polydactyly syndrome Majewski's polydactyly syndrome Léri–Weill dyschondrosteosisCOL1A1, COL1A2, SERPINF1, CRTAP, P3H1, SPARC, WNT1, TMEM38B, PLOD2, P4HB, MESD, PPIB, SERPINH1, TENT5A, TAPT1, SMPD3, SMAD4, SUCO, CREB3L1, FKBP10, BMP1, IFITM5, SOST, PPP1R2C, BGLAP, DMD, BEST1, GH1, ACVR2B, SEC24D, PNPLA2, FGFR3, AGA2, PLS3, COX8A, DCN, LRP5, TLL1, PDIA2, GPATCH8, RER, WWTR1, MTCO2P12, PADI1, EFEMP2, PLA1A, MBTPS2, GPR180, NBAS, MED18, LINC01672, TRAP, MIR29B2, MIR29B1, MIR145, SP7, ACTB, EIF2AK3, TNC, ALPL, BAAT, BGN, TSPO, KRIT1, CD38, CD44, CHRM3, COL3A1, COL5A1, CSF2, DLX3, FN1, MSTN, IGF1, TNFSF11, LAMC2, LOX, LRP6, COX2, PPP1CB, PTH, PTGS2, RNASE1, SRSF2, SLC6A2, TNXB, TSC1, TSHR, CXCR4, LOC107984355
-
Poor Ovarian Reserve
Wikipedia
Genetic factors, such as fragile x syndrome. Approximately 20–28% of women with an FMR1 premutation (55–200 CGG repeats) experience fragile x primary ovarian insufficiency (POI) and another 23% experience early menopause (i.e., menopause before the age of forty five). [9] Autoimmune disorders . ... "Laparoscopic surgery in polycystic ovary syndrome: reproductive and metabolic effects". ... "Pharmacological options in resistant ovary syndrome and premature ovarian failure". ... PMID 16080236 . v t e Female diseases of the pelvis and genitals Internal Adnexa Ovary Endometriosis of ovary Female infertility Anovulation Poor ovarian reserve Mittelschmerz Oophoritis Ovarian apoplexy Ovarian cyst Corpus luteum cyst Follicular cyst of ovary Theca lutein cyst Ovarian hyperstimulation syndrome Ovarian torsion Fallopian tube Female infertility Fallopian tube obstruction Hematosalpinx Hydrosalpinx Salpingitis Uterus Endometrium Asherman's syndrome Dysfunctional uterine bleeding Endometrial hyperplasia Endometrial polyp Endometriosis Endometritis Menstruation Flow Amenorrhoea Hypomenorrhea Oligomenorrhea Pain Dysmenorrhea PMS Timing Menometrorrhagia Menorrhagia Metrorrhagia Female infertility Recurrent miscarriage Myometrium Adenomyosis Parametrium Parametritis Cervix Cervical dysplasia Cervical incompetence Cervical polyp Cervicitis Female infertility Cervical stenosis Nabothian cyst General Hematometra / Pyometra Retroverted uterus Vagina Hematocolpos / Hydrocolpos Leukorrhea / Vaginal discharge Vaginitis Atrophic vaginitis Bacterial vaginosis Candidal vulvovaginitis Hydrocolpos Sexual dysfunction Dyspareunia Hypoactive sexual desire disorder Sexual arousal disorder Vaginismus Urogenital fistulas Ureterovaginal Vesicovaginal Obstetric fistula Rectovaginal fistula Prolapse Cystocele Enterocele Rectocele Sigmoidocele Urethrocele Vaginal bleeding Postcoital bleeding Other / general Pelvic congestion syndrome Pelvic inflammatory disease External Vulva Bartholin's cyst Kraurosis vulvae Vestibular papillomatosis Vulvitis Vulvodynia Clitoral hood or clitoris Persistent genital arousal disorder
-
Epstein–barr Virus-Associated Lymphoproliferative Diseases
Wikipedia
Non-LPD that have significant percentages of cases associated with EBV infection (see Epstein–Barr virus infection ) include the immune disorders of multiple sclerosis and systemic lupus erythematosus ; [2] malignancies such as stomach cancers , [3] soft tissue sarcomas , leiomyosarcoma , and undifferentiated nasopharyngeal cancer ; [4] the childhood disorders of Alice in Wonderland syndrome ; [5] and acute cerebellar ataxia . [6] About 95% of the world's population is infected with EBV. ... Short-term courses of corticosteroid drugs are often prescribed for patients afflicted with airways obstruction, autoimmune reactions (e.g. autoimmune anemia or thrombocytopenia ), or other complications of the disease. [17] Treatment of these and the severest IM cases generally use regimens directed at the specific features of each type of complication. [10] Epstein–Barr virus-related hemophagocytic lymphohistiocytosis [ edit ] Main article: Hemophagocytic lymphohistiocytosis Main article: Macrophage activation syndrome Hemophagocytic lymphohistiocytosis (HLH) is a rare disorder characterized by a systemic inflammatory or, in extreme cases, overwhelming cytokine storm condition. ... Malignant disorders associated with secondary HLH include T-cell lymphoma , B-cell lymphoma , acute lymphocytic leukemia , acute myeloid leukemia , and the myelodysplastic syndrome . Non-malignant disorders associated with secondary HLH include: autoimmune disorders such as juvenile idiopathic arthritis , juvenile Kawasaki disease , systemic lupus erythematosus , the juvenile onset and adult onset forms of Still's disease , and rheumatoid arthritis ; [18] immunodeficiency disorders such as severe combined immunodeficiency , DiGeorge syndrome , Wiskott–Aldrich syndrome , ataxia telangiectasia , and dyskeratosis congenita ); [19] and infections caused by EBV, cytomegalovirus , HIV/AIDS , bacteria , protozoa , and fungi . ... This regimen is currently recommended, particularly for primary HLH in young children, as induction therapy for EBV+ HLH except in patients with the macrophage activation syndrome where pulse methylprednisolone is the preferred treatment. ... The lesions often center around and evidence destruction of small blood vessels but, paradoxically, do not contain well‑formed granulomas . [36] Only the lymphoid B cells in the lesions are EBV+; these cells express LMP1 and EBNA2 viral proteins and therefore carry EBV in its latency III phase. [1] Individuals with the disease may be immune deficient due to subtle reductions in their immune function [1] or, based on individual case reports , immunodeficiency diseases such as HIV/AIDS , common variable immunodeficiency , X-linked agammaglobulinemia , hypogammaglobulinemia , sarcoidosis , [37] methotrexate -treated rheumatoid arthritis , or the Wiskott–Aldrich syndrome . [36] They may also have, again based on case reports, a history of inflammatory/autoimmune diseases such as chronic hepatitis , ulcerative colitis , retroperitoneal fibrosis , or primary biliary cholangitis . [37] EBV+ LG may progress to or become complicated by the non-malignant skin disease, lymphomatoid papulosis , or a second lymphoid malignancy such as Hodgkin lymphoma, mycosis fungoides , CD30+ anaplastic large cell lymphoma , follicular lymphoma , chronic lymphocytic leukemia , or diffuse large B cell lymphoma. [38] EBV+ LG appears in part due to the virus causing its infected B cell to release chemokines which attract, and thereby stimulate T cells to injure tissues, particularly blood vessels.
-
Acute Inhalation Injury
Wikipedia
Contents 1 Causes 1.1 Smoke inhalation 1.2 Chlorine 1.3 Phosgene 1.4 Ammonia 1.5 Mustard gas 1.6 Chloramine 1.7 Methyl isocyanate 2 Pathophysiology 2.1 Acute lung injury 2.2 Acute respiratory distress syndrome 3 Treatment strategies 4 Preclinical development of pulmonary protective strategies 4.1 In vitro 4.2 In vivo 5 References Causes [ edit ] Smoke inhalation [ edit ] Smoke inhalation injury, either by itself but more so in the presence of body surface burn, can result in severe lung-induced morbidity and mortality. [3] The most common cause of death in burn centers is now respiratory failure. ... Extensive microvascular thrombosis may lead to pulmonary hypertension, myocardial dysfunction and systemic hypotension. Acute respiratory distress syndrome [ edit ] Clinically, the most serious and immediate complication is acute respiratory distress syndrome (ARDS), which usually occurs within 24 h. [31] [32] [33] Those with significant lower airway involvement may develop bacterial infection. ... Pulm Pharmacol Ther. 20:112-7. ^ Luh SP, Chiang CH. (2007) Acute lung injury/acute respiratory distress syndrome (ALI/ARDS): the mechanism, present strategies and future perspectives of therapies. ... Ann N Y Acad Sci. 1024:24-53. ^ Morrison RJ, Bidani A. (2002) Acute respiratory distress syndrome epidemiology and pathophysiology. ... Qual Life Res. 19:1467-76. ^ Matthay MA, Zemans RL. (2011) The acute respiratory distress syndrome: pathogenesis and treatment. Annu Rev Pathol. 6:147-63. ^ [2] ^ Johnson ER, Matthay MA. (2010) Acute lung injury: epidemiology, pathogenesis, and treatment, J Aerosol Med Pulm Drug Deliv. 23:243-52. ^ [3] ^ Meesun, Vera (June 2014).
-
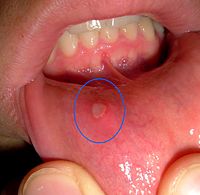
Mouth Ulcer
Wikipedia
Hematological causes include anemia , hematinic deficiencies, neutropenia , hypereosinophilic syndrome , leukemia , myelodysplastic syndromes , other white cell dyscrasias , and gammopathies . ... Dermatological causes include chronic ulcerative stomatitis , erythema multiforme (Stevens-Johnson syndrome), angina bullosa haemorrhagica and lichen planus . Other examples of systemic disease capable of causing mouth ulcers include lupus erythematosus , Sweet syndrome , reactive arthritis , Behçet syndrome , granulomatosis with polyangiitis , periarteritis nodosa , giant cell arteritis , diabetes , glucagonoma , sarcoidosis and periodic fever, aphthous stomatitis, pharyngitis and adenitis . [5] The conditions eosinophilic ulcer and necrotizing sialometaplasia may present as oral ulceration. ... "Clinical Immunology Review Series: an approach to the patient with recurrent orogenital ulceration, including Behçet's syndrome" . Clinical and Experimental Immunology . 156 (1): 1–11. doi : 10.1111/j.1365-2249.2008.03857.x . ... External links [ edit ] Classification D ICD - 10 : K12 ICD - 9-CM : 528.9 MeSH : D019226 DiseasesDB : 22751 SNOMED CT : 26284000 External resources MedlinePlus : 001448 Learning materials related to Oral ulceration at Wikiversity Mouth ulcer at Curlie v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic diseaseEDN1, LEP, STAT4, IL10, TAP2, CRLF1, IL19, CRB1, TRIM31, EHMT2, IKZF1, TCIRG1, MAPKAPK2, FAS, KLRC4, IL20, TNXB, TNFAIP3, TLR4, TAP1, SRP54, SPP1, C1QA, SCHIP1, ERAP1, PTPRC, PSORS1C2, IL12A-AS1, MUC22, ARL17B, IQCJ-SCHIP1, SPATA48, LINC01100, GIMAP6, UBAC2, NSMCE2, PSORS1C1, LZTFL1, IL23R, SLC46A1, ZNRD1ASP, GSDMD, GTDC1, DCLRE1C, NOD2, IFT80, PGPEP1, RELA, RREB1, PSMB9, IL12RB1, IL7R, IFNGR1, HLA-J, HLA-DQA2, HLA-DPB1, HLA-DPA1, HLA-B, HLA-A, GFI1, SLC37A4, ELANE, CYP21A2, CCR1, CDSN, CAT, C4A, C1R, IL12A, IRF8, IRAK1, LTF, PPP5C, PDE4D, NOTCH4, NFKB1, MEFV, LYZ, LINC02009, CRP, TNF, VEGFA, IL2, CSF3, ENO1, ITGAM, IL2RA, NGF, SOCS3, MIR223, MTHFR, PLAAT4, FCGR2A, RNPC3, SOCS1, GEM, ISG20, HGF, KIR3DL1, IFIH1, LGALS1, IL21, TPMT, GYPA
-
Giardiasis
Wikipedia
The evidence for comparing metronidazole to other alternatives such as mebendazole, tinidazole or nitazoxanide was felt to be of very low quality. [47] While tinidazole has side effects and efficacy similar to those of metronidazole, it is administered with a single dose. [20] Resistance has been seen clinically to both nitroimidazoles and albendazole, but not nitazoxanide, though nitazoxanide resistance has been induced in research laboratories. [21] [49] The exact mechanism of resistance to all of these medications is not well understood. [49] In the case of nitroimidazole-resistant strains of Giardia , other drugs are available which have showed efficacy in treatment including quinacrine , nitazoxanide, bacitracin zinc , furazolidone and paromomycin . [20] Mepacrine may also be used for refractory cases. [21] Probiotics, when given in combination with the standard treatment, has been shown to assist with clearance of Giardia . [50] During pregnancy, paromomycin is the preferred treatment drug because of its poor intestinal absorption, resulting in less exposure to the fetus. [51] Alternatively, metronidazole can be used after the first trimester as there has been wide experience in its use for trichomonas in pregnancy. [52] [53] Prognosis [ edit ] In people with a properly functioning immune system, infection may resolve without medication. [5] A small portion, however, develop a chronic infection. [5] People with an impaired immune system are at higher risk of chronic infection. [5] Medication is an effective cure for nearly all people although there is growing drug-resistance. [1] [54] [21] Children with chronic giardiasis are at risk for failure to thrive as well as more long-lasting sequelae such as growth stunting. [55] Up to half of infected people develop a temporary lactose intolerance leading symptoms that may mimic a chronic infection. [1] Some people experience post-infectious irritable bowel syndrome after the infection has cleared. [5] Giardiasis has also been implicated in the development of food allergies . [5] This is thought to be due to its effect on intestinal permeability. [5] Epidemiology [ edit ] Rates of giardiasis in 2005 in the United States In some developing countries Giardia is present in 30% of the population. [16] In the United States it is estimated that it is present in 3–7% of the population. [16] The number of reported cases in the United States in 2018 was 15,584. [56] All states that classify giardiasis as a notifiable disease had cases of giardiasis. [56] The states of Illinois, Kentucky, Mississippi, North Carolina, Oklahoma, Tennessee, Texas, and Vermont did not notify the Center for Disease Control regarding cases in 2018. [56] The states with the highest number of cases in 2018 were California, New York, Florida, and Wisconsin. [56] There are seasonal trends associated with giardiasis. [57] July, August, and September are the months with the highest incidence of giardiasis in the United States. [58] In the ECDC's (European Centre for Disease Prevention Control) annual epidemiological report containing 2014 data, 17,278 confirmed giardiasis cases were reported by 23 of the 31 countries that are members of the EU/EEA. [59] Germany reported the highest number at 4,011 cases. [59] Following Germany, the UK reported 3,628 confirmed giardiasis cases. Together, this accounts for 44% of total reported cases. [59] Research [ edit ] Some intestinal parasitic infections may play a role in irritable bowel syndrome [60] and other long-term sequelae such as chronic fatigue syndrome. [61] [62] The mechanism of transformation from cyst to trophozoites has not been characterized [6] but may be helpful in developing drug targets for treatment-resistant Giardia . ... Retrieved 30 November 2017 . ^ Stark D, van Hal S, Marriott D, Ellis J, Harkness J (January 2007). "Irritable bowel syndrome: a review on the role of intestinal protozoa and the importance of their detection and diagnosis". ... PMID 17070814 . ^ Hanevik K, Wensaas KA, Rortveit G, Eide GE, Mørch K, Langeland N (November 2014). "Irritable bowel syndrome and chronic fatigue 6 years after giardia infection: a controlled prospective cohort study" . ... PMID 25115874 . ^ Quote: "for unclear reasons, chronic sequelae, including post-infectious irritable bowel syndrome, chronic fatigue [..], malnutrition [..], cognitive impairment [..], and extra-intestinal manifestations (such as food allergy, urticaria, reactive arthritis, and inflammatory ocular manifestations), can develop and possibly persist beyond detectable parasite shedding".TPI1, GLUD1, H6PD, UGDH, CRYL1, NLRP3, GPR162, RNF19A, TLR2, PARP9, HSP90B2P, IL23A, UPP1, AIMP2, GRAP2, POLDIP2, SF3B4, TUBA1B, SNAP25, AHSA1, CCL27, SLC27A5, PRDX5, TGFB1, ACTB, AGL, STX2, AKT1, CACNA1B, CEL, CELP, CRK, MAPK14, CTSB, EGF, EPHB2, HPRT1, MAPK1, HSP90AA1, IFNG, CXCL8, IL17A, IVD, MBL2, MPO, PLG, PTPA, RAD52
-
Gluten-Sensitive Enteropathy–associated Conditions
Wikipedia
PMID 643295 . ^ Mauro A, Orsi L, Mortara P, Costa P, Schiffer D (1991). "Cerebellar syndrome in adult celiac disease with vitamin E deficiency". ... S2CID 10964149 . ^ Van Dyk D, Inbal A, Kraus L, Grifel B, Ravid M (1981). "The watery diarrhea syndrome with hypercalcemia--a symptomatic response to phosphate buffer". ... "Celiac disease presenting as the Paterson-Brown Kelly (Plummer-Vinson) syndrome". Am. J. Gastroenterol . 94 (2): 527–529. ... PMID 10521982 . ^ Popadić S, Nikolić M, Gajić-Veljić M, Bonaci-Nikolić B (2006). "Rothmund-Thomson syndrome. The first case with plantar keratoderma and the second with coeliac disease". ... "Predictors of Clinical Response to Gluten-Free Diet in Patients Diagnosed With Diarrhea-Predominant Irritable Bowel Syndrome". Clinical Gastroenterology and Hepatology . 5 (7): 844–850. doi : 10.1016/j.cgh.2007.03.021 .
-
Retrograde Amnesia
Wikipedia
RA can also progress and further deteriorate memory recollection, as in the case of Korsakoff syndrome and Alzheimer's disease , due to the ongoing nature of the damage caused by the illnesses. ... It may even be that in some cases both conscious feigning and unconscious processes are at play. [ citation needed ] Traumatic brain injury (TBI) or post-traumatic amnesia [ edit ] Traumatic brain injury (TBI), also known as post-traumatic amnesia, occurs from an external force that causes structural damage to the brain, such as a sharp blow to the head, a diffuse axonal injury , [12] or childhood brain damage (e.g., shaken baby syndrome ). [12] In cases of sudden rapid acceleration, the brain continues moving around in the skull, harming brain tissue as it hits internal protrusions. [13] TBI varies according to impact of external forces, location of structural damage, and severity of damage ranging from mild to severe. [5] [12] [13] Retrograde amnesia can be one of the many consequences of brain injury but it is important to note that it is not always the outcome of TBI. ... Someone with this might withdraw from the environment that they are placed in because they no longer know how to handle the cognitive resources. [20] Nutritional deficiency [ edit ] RA has been found among alcohol-dependent patients who suffer from Korsakoff's syndrome . [21] Korsakoff's syndrome patients suffer from retrograde amnesia due to a thiamine deficiency (lack of vitamin B1). [22] Also, chronic alcohol use disorders are associated with a decrease in the volume of the left and right hippocampus. [21] These patients' regular diet consists mostly of hard alcohol intake, which lacks the necessary nutrients for healthy development and maintenance. [22] Therefore, after a prolonged time consuming primarily alcohol, these people undergo memory difficulties and ultimately suffer from RA. ... Right medial thalamic lesion causes isolated retrograde amnesia, Neuropsychologia , 39 , 1037-1046. ^ Lucchelli, F.; Muggia, S.; Spinnler, H. (1998). "The Syndrome of Pure Retrograde Amnesia" . Cognitive Neuropsychiatry . 3 : 91–118 . ... J., & Mair, R. G. (1990). The Korsakoff syndrome: A neurochemical perspective, Trends in Neurosciences , 13(8), 340-344. ^ Fujii, T., Yamadori, A., Endo, K., Suzuki, K., & Fukatsu, R. (1999).
-
Endometriosis
Wikipedia
Specialty Gynecology Symptoms Pelvic pain , infertility [1] Usual onset 30–40 years old [2] [3] Duration Long term [1] Causes Unknown [1] Risk factors Family history [2] Diagnostic method Based on symptoms, medical imaging , tissue biopsy [2] Differential diagnosis Pelvic inflammatory disease , irritable bowel syndrome , interstitial cystitis , fibromyalgia [1] Prevention Combined birth control pills , exercise, avoiding alcohol and caffeine [2] Treatment NSAIDs , continuous birth control pills, intrauterine device with progestogen , surgery [2] Frequency 10.8 million (2015) [4] Deaths ~100 (0.0 to 0.1 per 100,000, 2015) [4] [5] Endometriosis is a condition in which cells similar to those in the endometrium , the layer of tissue that normally covers the inside of the uterus , grow outside the uterus. [6] [7] Most often this is on the ovaries , fallopian tubes , and tissue around the uterus and ovaries; however, in rare cases it may also occur in other parts of the body. [2] The main symptoms are pelvic pain and infertility . [1] Nearly half of those affected have chronic pelvic pain , while in 70% pain occurs during menstruation . [1] Pain during sexual intercourse is also common. [1] Infertility occurs in up to half of affected individuals. [1] Less common symptoms include urinary or bowel symptoms. [1] About 25% of individuals have no symptoms and 85% of those seen with infertility in a tertiary center have no pain. [1] [8] Endometriosis can have both social and psychological effects. [9] The cause is not entirely clear. [10] Risk factors include having a family history of the condition. [2] The areas of endometriosis bleed each month (menstrual period), resulting in inflammation and scarring. [1] [2] The growths due to endometriosis are not cancer . [2] Diagnosis is usually based on symptoms in combination with medical imaging ; [2] however, biopsy is the surest method of diagnosis. [2] Other causes of similar symptoms include pelvic inflammatory disease , irritable bowel syndrome , interstitial cystitis , and fibromyalgia . [1] Endometriosis is commonly misdiagnosed, and women are often incorrectly told their symptoms are trivial or normal. [9] Tentative evidence suggests that the use of combined oral contraceptives reduces the risk of endometriosis. [2] [11] Exercise and avoiding large amounts of alcohol may also be preventive. [2] There is no cure for endometriosis, but a number of treatments may improve symptoms. [1] This may include pain medication , hormonal treatments or surgery. [2] The recommended pain medication is usually a non-steroidal anti-inflammatory drug (NSAID), such as naproxen . [2] Taking the active component of the birth control pill continuously or using an intrauterine device with progestogen may also be useful. [2] Gonadotropin-releasing hormone agonist (GnRH agonist) may improve the ability of those who are infertile to get pregnant. [2] Surgical removal of endometriosis may be used to treat those whose symptoms are not manageable with other treatments. [2] One estimate is that 10.8 million people are affected globally as of 2015 [update] . [4] Other sources estimate 6 to 10% of the general female population [1] and 2 to 11% of asymptomatic women [10] are affected. ... Manifestations of this include coughing up blood , a collapsed lung , or bleeding into the pleural space . [10] [30] Stress may be a cause or a consequence of endometriosis. [31] Complications [ edit ] Complications of endometriosis include internal scarring, adhesions , pelvic cysts, chocolate cysts of ovaries , ruptured cysts, and bowel and ureter obstruction resulting from pelvic adhesions. [32] Endometriosis-associated infertility can be related to scar formation and anatomical distortions due to the endometriosis. [2] Ovarian endometriosis may complicate pregnancy by decidualization , abscess and/or rupture. [33] Thoracic endometriosis can be associated with recurrent thoracic endometriosis syndrome at times of a menstrual period that includes catamenial pneumothorax in 73% of women, catamenial hemothorax in 14%, catamenial hemoptysis in 7%, and pulmonary nodules in 6%. [34] [35] A 20-year study of 12,000 women with endometriosis found that individuals under 40 who are diagnosed with endometriosis are 3 times more likely to have heart problems than their healthy peers. [36] [37] It results in few deaths with unadjusted and age-standardized death rates of 0.1 and 0.0 per 100,000. [4] Risk factors [ edit ] Genetics [ edit ] Endometriosis is a heritable condition that is influenced by both genetic and environmental factors. [38] Children or siblings of people with endometriosis are at higher risk of developing endometriosis themselves; low progesterone levels may be genetic, and may contribute to a hormone imbalance. [39] There is an approximate six-fold increased incidence in individuals with an affected first-degree relative. [40] It has been proposed that endometriosis results from a series of multiple hits within target genes, in a mechanism similar to the development of cancer. [38] In this case, the initial mutation may be either somatic or heritable. [38] Individual genomic changes (found by genotyping including genome-wide association studies ) that have been associated with endometriosis include: [41] [42] [43] Chromosome Gene/Region of Mutation Gene Product Function 1 WNT4 Wingless-type MMTV integration site family member 4 Vital for development of the female reproductive organs 2 GREB1 /FN1 Growth regulation by estrogen in breast cancer 1/Fibronectin 1 Early response gene in the estrogen regulation pathway/Cell adhesion and migration processes 6 ID4 Inhibitor of DNA binding 4 Ovarian oncogene, biological function unknown 7 7p15.2 Transcription factors Influence transcriptional regulation of uterine development 9 CDKN2BAS Cyclin-dependent kinase inhibitor 2B antisense RNA Regulation of tumour suppressor genes 10 10q26 12 VEZT Vezatin, an adherens junction transmembrane protein Tumor suppressor gene 19 MUC16 (CA-125) Mucin 16, cell surface associated Form protective mucous barriers There are many findings of altered gene expression and epigenetics , but both of these can also be a secondary result of, for example, environmental factors and altered metabolism. ... Diaphragmatic endometriosis is rare, almost always on the right hemidiaphragm, and may inflict the cyclic pain of the right scapula (shoulder) or cervical area (neck) during a menstrual period. [81] Pulmonary endometriosis can be associated with a thoracic endometriosis syndrome that can include catamenial (occurs during menstruation) pneumothorax seen in 73% of women with the syndrome, catamenial hemothorax in 14%, catamenial hemoptysis in 7%, and pulmonary nodules in 6%. [35] Diagnosis [ edit ] Laparoscopic image of endometriotic lesions in the Pouch of Douglas and on the right sacrouterine ligament . ... Laparoscopy , a surgical procedure where a camera is used to look inside the abdominal cavity, is the only way to accurately diagnose the extent and severity of pelvic/abdominal endometriosis. [85] Laparoscopy is not an applicable test for extrapelvic sites such as umbilicus, hernia sacs, abdominal wall, lung, or kidneys. [85] Reviews in 2019 and 2020 concluded that 1) with advances in imaging, endometriosis diagnosis should no longer be considered synonymous with immediate laparoscopy for diagnosis, and 2) endometriosis should be classified a syndrome that requires confirmation of visible lesions seen at laparoscopy in addition to characteristic symptoms. [86] [87] Laparoscopy permits lesion visualization unless the lesion is visible externally (e.g., an endometriotic nodule in the vagina) or is extra-abdominal. [85] If the growths (lesions) are not visible, a biopsy must be taken to determine the diagnosis. [82] Surgery for diagnoses also allows for surgical treatment of endometriosis at the same time.KRAS, CYP19A1, PGR, IL10, PTGS2, HDAC2, CCL11, GREB1, CDKN2B-AS1, ESR2, NR5A1, HSD17B1, IGF1, EGFR, HSD17B2, PRL, IGFBP1, IL15, SST, IL1R1, MIR21, AKR1C3, ARNT, TGFB2, PTGER4, IDO1, KLF9, FOS, PAPPA, NR3C1, NCOA1, ABCC4, NR2F2, NR4A1, RXFP1, LTF, TAGLN, KLF13, PLA2G2A, CXCL9, MTA1, MTA2, DICER1, ENPP1, CXCL14, NR3C2, ACTA2, TXNIP, PAX2, CXCL13, OLFM4, AKR1B1, TNC, HDAC1, ITGB1, HLA-DPB1, AKR1C1, AKR1C2, CCL1, RASGRP1, RGS4, CNR1, SLC16A6, CCNE2, NR2C2, MED14, NR2C1, PLXNC1, COPS2, MED17, SRD5A1, TOB1, TNF, NCOR1, CYP26A1, HS3ST3B1, NR1D2, MED16, DDX5, ABCC9, UST, RORB, CD55, SLC1A1, THRA, SRD5A2, TRH, NR2F6, PTGER2, CYB5A, FBLN1, FBN1, VEGFA, PRLR, HBEGF, VCAN, MED1, RARB, FKBP5, SPARCL1, DIO2, STC2, CFD, DUSP1, CCL22, FMO2, SUCLG2, NRP1, CPM, SELENOP, CLDN1, PTGFR, ELAVL1, MYLIP, ANKRD1, MED4, ITGA2, FAM180A, RASL11A, IL7R, SLC40A1, HERC5, CNIH3, BMP7, IMPA2, ERRFI1, MAOA, NTRK3, TACSTD2, SULF2, ANKH, AREG, ANO4, LAMB1, NDNF, ARHGAP28, LRRK2, DCSTAMP, OSR2, SCGB3A1, MAOB, ITGB8, SLC7A8, SMPDL3A, DKK1, BRD8, NCOA6, CD226, MMP2, C1R, NEDD4L, MMP9, IFNGR1, IGFBP6, ITGB3BP, DEPP1, LMOD1, METTL7A, GPX3, ABI3BP, SLC20A1, IFIT1, RBPJ, NEFM, IHH, CCL5, BCL2, KDR, SERPINF1, BIRC5, EGR1, HDAC3, RUNX1, LYN, VAV1, ESR1, BAX, WNT4, SELL, NFKBIA, BCL2L1, VEZT, BSG, FN1, CDC42, IL33, IGF1R, CCDC170, SYNE1, MAP3K4, PIK3CB, MME, PDE1C, GRIN2D, PIK3CA, IL1A, MEIS1, ICAM1, IL1B, PIK3CD, INHBA, IL6, PIK3CG, CXCL8, GSTM1, GSTT1, CCL2, HOXA10, MAPK1, PTEN, COX2, CYP17A1, COMT, CTNNB1, OR9Q1, LAMC3, CYP2B6, COL12A1, CYP1A1, RFLNA, SKAP1, ARID1A, CDC73, BEND5, CALHM3, MUC16, FOXP2, AGBL4, NAALADL2, CYP21A2, TP53, AKT1, CACNA1A, MTCO2P12, ARID3B, SYNJ2, LINC00861, C2, FGD6, TGFB1, CAPN14, GPNMB, THOC6, HSD17B7, HGF, ARTN, HIF1A, PPP1R2C, CXCR4, SERPINE1, AGRP, MIF, CXCL12, BDNF, CDH1, GALT, GSTM2, BRD2, STAT3, IFNG, MIR451A, IL1R2, BECN1, FSHR, EPHB2, HPGDS, IL4, MALAT1, TLR4, HP, PAEP, AMH, MAPK3, MMP1, STS, LEP, GSTP1, IL18, IL37, GPER1, MMP3, CD44, TAC1, FGF2, CYP2C19, KLF11, PPARG, HLA-DRB1, FCRL3, ANGPT2, VDR, HOXA11, VCAM1, UCN, CRK, RAF1, TNFRSF1B, MIRLET7B, S100A6, IL1RN, TIMP1, MIR145, MIR20A, MAPK14, AIMP2, CRH, NOTCH1, EGF, RNF19A, POLDIP2, PTPN22, AHSA1, CCR1, FOXP3, NOS3, SPP1, GRAP2, CDKN1B, POU5F1, SULT1E1, DHRS11, HNF1B, POU5F1P4, POU5F1P3, TERT, THBS1, MIR210, KLRK1, MIR17, MMP7, PLAU, MRC1, SLCO6A1, XRCC1, TIMP2, GSTK1, HSD17B13, PTGES, AHRR, IL13, FST, IL16, IL17A, NGF, HPSE, OGG1, MUC1, NAT2, BRCA2, GNRHR, CSF1, EZH2, CDKN2A, CRP, HLA-G, BRAF, BRCA1, HMGB1, DRD2, GC, AGTR1, NME1, AHR, SIRT1, GATA6, TNFRSF11B, PCNA, NFKB1, H3P10, GHRH, MPO, MTOR, MMP14, MIR126, CRHR1, MIR141, CREB1, MDK, SMAD3, LGALS3, LEPR, FSHB, CCN2, PGF, FOXO1, TACR1, CCND1, VPS11, STAR, ATM, ACKR3, SOD2, AR, TNFRSF1A, CCL25, ACE, FASLG, TWIST1, RNASE3, REN, CYP1B1, CTLA4, EZR, F3, MAPK8, ANXA1, PPARA, FGFR2, CCR9, PLG, CD36, ZEB1, ISG20, ITGAV, POSTN, ACTB, IL1RAP, CXCL10, KLRC4-KLRK1, CCN1, CD68, CFL1, CIB1, YAP1, ITGAM, SEMA6A, CSF2, HMGA1, ENPP3, CAPN7, CCR2, LINC00261, EMX2, SLC2A4, SKP2, FPR2, HMGA2, CKS1BP7, FPR1, FLT1, TIMP3, DNMT3A, HSD11B2, LINC00339, OPRM1, TCF21, P2RX3, THY1, NUP62, RELA, SLIT3, NTF4, SERPINB2, PAK1, CSF3, NTRK2, RMDN2, IL23A, IL7, FKBP4, FOXM1, PROK1, CDKN1A, DCTN4, APEX1, IL2RA, WNT7A, RMDN1, MANEA, PDCD4, CXCL5, IL2RB, VIM, EPO, TSLP, VEGFC, HSH2D, CCL21, HSPA4, MAP2K7, SRA1, CSF1R, ANXA2, MIR342, SEMA3C, TLR2, HOXA13, PAX8, ANG, PON1, CEBPA, C3, FGF1, ANGPT1, RB1, RNU1-1, USF2, ENO1, XRCC4, FGA, SOD1, PPIG, EMSLR, LTA, ERBB2, CD274, GTF2H1, SQSTM1, SMAD2, CDH3, MIR200C, STC1, ZHX2, NR1I2, STAT6, RNU1-4, MIR191, KIR2DS5, MIR183, CCNE1, IL22, USP10, LPA, AIF1, SYBU, ADIPOQ, RMDN3, S100B, PPARGC1A, CCR5, CKS1B, IL32, COL18A1, MIR31, FAS, ERVW-1, LHCGR, LIF, DUSP2, MIR29C, MS4A1, STIP1, KIR2DS1, CDK6, TNFSF10, LGR5, SOX9, MUC2, MUC4, AGT, SOX2, NCAM1, GH1, AGTR2, ACP1, ITGB3, IGFBP3, AHSG, NOS1, NOS2, MIR33B, CXCR2, MST1R, MST1, BCL6, MSI1, MIR143, MLH1, SSTR1, CXCR3, CXCR1, RETN, KHDRBS1, GLI1, ABCB6, DNMT3B, CRHR2, LINC02210-CRHR1, SRC, CD47, KRT20, GJA1, MSH2, MBL3P, BMP4, TMED7, HSPA14, SLC52A1, PAK4, CDC6, BNC2, RBFOX1, UGT1A1, DLL4, NOD1, ROBO4, RHOF, UGT2B28, TREM2, IL17D, BMPR1B, VTA1, NRN1, NDRG1, BRS3, CHD5, TBX21, SERPINH1, NUP210, PLCB1, CTCF, CXCR6, ASTN2, CD40LG, PDLIM5, DNMT3L, RUNX3, CAT, CD48, CASR, CASP3, HEY1, PLXND1, CCNB1, KIFAP3, CD14, PHB2, ENTPD1, SCN11A, GALNT6, AKAP13, NUDT6, CD19, UTS2, CD86, MMP24, DCTN6, LILRB1, TNFSF13B, SRRM2, CD74, AGR2, FOXP1, TMOD3, BTF3P11, MYL9, BTG1, REM1, CCDC22, BTK, CDK1, CD79A, RBMS3, TNFRSF21, TSPO, INTU, CACYBP, SERPING1, FAM215A, CARM1, FOXD3, GREM1, C5, ZNRD2, NECTIN3, C9, CA2, CALCA, CALD1, FJX1, CADM1, SH3BP4, DAPK2, LPAR3, CRISPLD2, ATAD3A, MIR205, MIR181C, MIR182, MIR195, MIR196A2, PARP1, MIR200A, MIR200B, MIR204, ADM, MIR33A, ADAR, MIR214, MIR216A, MIR22, MIR23B, MIR27B, MIR30A, MIR30C1, ADRA1A, MIR154, MIR148A, ADRA2B, IL27, CADM2, ALB, NCR3, CPP, TICAM2, USP17L2, TBPL2, HES5, MIRLET7D, MIR100, MIR106A, MIR10B, MIR122, MIR132, MIR139, MIR142, MIR30C2, MIR34A, VPS53, MIR3613, RGPD2, ACTN4, MIR543, MR1P1, DEFB4B, MIR1185-1, TMED7-TICAM2, MIR2861, LINC01541, MIR34B, LINC01672, MIR4634, PCAT1, PGR-AS1, LOC110386951, LOC110806263, LINC02605, H3P23, MIR629, MIR449B, MIR542, ACTN1, CCDC144NL-AS1, ADA, MIR135B, MIR370, MIR196B, MIR375, MIR378A, MIR381, H4C15, MIR363, ACVR2B, MIR488, MIR146B, MIR520G, MIR503, MIR483, ACVR1B, HOXA11-AS, ALOX15, TET3, STN1, RHOC, ARG1, ULBP3, NAA16, AQP9, AQP5, AQP2, NANOG, AQP1, ARX, RNF34, SPHKAP, TET1, ULBP2, SLC38A1, NECTIN4, CAB39L, MAP1LC3B, WNK1, GORASP1, ATG3, DCLRE1C, QRSL1, B2M, ST6GALNAC1, TRERF1, AXL, MYDGF, LTB4R2, PNO1, SALL4, ARSD, CXCL16, IL21, RHOG, AFAP1, SLC22A23, SRR, SMOC2, TMPRSS13, MAGT1, NLRC5, ANK1, H4-16, RBM45, SGPP2, CD200R1, ZFP42, AMHR2, DOCK11, MUC17, SIRPA, ALPP, IL34, ALPI, PDIK1L, GPBAR1, CCDC80, TTC39B, ZNF366, CYP2R1, ANTXR2, LOXL4, CTHRC1, CARD11, MAK16, KISS1R, AFAP1-AS1, APOE, GFM1, WNT3A, LMLN, UCN2, APOA2, CREB3L1, BIRC3, IGSF8, BIRC2, SFXN1, PRRT2, UCN3, LILRB2, IFNA13, EIF1, PDGFA, P2RX5, P2RY6, GATA3, GATA2, GALNT3, GABPA, PDCD1, NR5A2, PDGFRA, POLD1, PDGFRB, PF4, PF4V1, PHB, SERPINA1, FOXO3, PLCB4, PLK1, OXTR, CLDN11, GATM, NTF3, CD200, MSMB, GHRHR, MYB, MYC, NFE2L2, GDNF, MSTN, NGFR, NHS, NINJ1, GBA, NOTCH4, NPTX2, NRAS, YBX1, NT5E, PNN, POLE, MMP13, RBP1, PTPRC, PTPRD, PVR, NECTIN1, EXTL3, RARRES1, RARRES2, RASA1, ETS1, FGF9, ACACA, ROCK1, ESRRB, ROS1, RXRA, S100A1, S100A4, ERCC6, PTN, F2, F2R, F2RL1, PPP2R1A, PPP5C, PPT1, PRELP, PRKCA, PRKCB, FEN1, MAP2K1, FCGR3B, FCGR3A, HTRA1, PSEN1, PSMD2, PSMD9, PSMD10, PTBP1, FANCD2, MNAT1, MMP12, TSHZ1, JUN, HNF4A, FOXA2, INHA, INSR, EIF3E, ITGA5, HLA-DQB1, JAK1, CD82, KLRC1, KCNQ1, KCNQ2, HLA-C, KIR2DL1, KIR2DL3, KIR2DL4, KIR3DL1, KIR3DL2, ILK, HOXB4, HPGD, HPRT1, IFNA1, IGFBP7, IFI27, CFI, ID2, IAPP, HTC2, HSPD1, IL2, HSD17B3, HSD3B2, IL9, HSD3B1, IL11, IL12B, IL12RB1, AGFG2, KISS1, KNG1, GJB2, MECP2, SMAD4, MSH6, GSK3B, MAP2, MAS1, MAT2A, MBL2, MDM2, PDIA3, HLA-B, CXCL1, MET, KITLG, GRB2, GPX4, GPR42, GNRH1, GLI3, EPCAM, SH2D1A, H2AX, HAS1, L1CAM, HK1, LAMC2, STMN1, LBR, HCK, LGALS1, LGALS4, LGALS9, LHB, LIMK1, LIPC, LIPE, LMNB1, LOX, LOXL1, CYP4F3, SAG, SRL, ERCC2, DENR, H4C3, H4C8, H4C2, H4C5, H4C13, H4C14, BCAR3, NR0B2, CSE1L, IER3, CRMP1, IRS2, PEA15, HYAL2, TNFRSF6B, IL18R1, CRABP2, CLDN7, H4C11, H4C12, H4C6, H4C4, VWF, WT1, XBP1, CTH, XRCC3, YWHAZ, ZFP36, ZNF217, ZP3, CSK, BAG6, MIA, H3-4, H4C9, AXIN1, FZD7, H4C1, PROM1, CLDN3, ERCC1, BMS1, GDF3, CLOCK, RGS6, IPO13, CETP, SEMA3E, HDAC9, RASSF2, CDX1, BCL10, PDCD6, BCL2L11, CDKN3, DNM1L, KIF20A, CDK4, HNRNPA3P1, CDH15, BCAR1, CFTR, CHRM3, TECR, CLDN4, CPB2, COL1A1, LTB4R, CCR8, EBAG9, LPAR2, SLC33A1, CCR7, S1PR2, CLCN3, CD163, SLIT2, LIPG, CHUK, HAND2, CHST3, VTN, TRPV1, VIP, SRY, SMARCC1, SNAI1, SNCG, FSCN1, SOX15, EIF4EBP1, MEGF8, EDNRA, EDN1, CX3CR1, SSTR4, S1PR1, STAT4, DUSP6, STX5, SULT1A1, SULT2A1, SYP, SMARCA1, SNAI2, SLPI, ELAVL2, EPOR, CCL14, CCL16, CCL17, CCL19, CX3CL1, SDC1, SDC4, EPHB4, SELE, EPHA3, SFRP1, SFRP2, SHC1, SLC2A1, SLC2A3, SLC6A4, SYT1, ADAM17, DPYSL2, DLX3, DEFB4A, DECR1, TNS1, TPM3, TPT1, DCN, DAPK1, CYP11A1, TRO, TRPC6, TXN, TYK2, TYROBP, UCHL1, CYP3A4, UTRN, CYP1A2, CLDN5, TLR3, TCF3, TIMP4, TDGF1, TEK, TERF1, DPP6, DPP4, TFDP1, TFF3, DOK1, TGFB1I1, TGFB3, LEFTY2, TGFBI, TGFBR1, DNMT1, KLF10, SARDH, DLX5, UTF1
-
Acne
Wikipedia
These gene candidates include certain variations in tumor necrosis factor-alpha (TNF-alpha) , IL-1 alpha , and CYP1A1 genes, among others. [19] The 308 G/A single nucleotide polymorphism variation in the gene for TNF is associated with an increased risk for acne. [40] Acne can be a feature of rare genetic disorders such as Apert's syndrome . [15] Severe acne may be associated with XYY syndrome . [41] Hormones [ edit ] Hormonal activity, such as occurs during menstrual cycles and puberty , may contribute to the formation of acne. ... High levels of growth hormone (GH) and insulin-like growth factor 1 (IGF-1) are also associated with worsened acne. [42] Both androgens and IGF-1 seem to be essential for acne to occur, as acne does not develop in individuals with complete androgen insensitivity syndrome (CAIS) or Laron syndrome (insensitivity to GH, resulting in very low IGF-1 levels). [43] [44] Medical conditions that commonly cause a high-androgen state, such as polycystic ovary syndrome , congenital adrenal hyperplasia , and androgen-secreting tumors , can cause acne in affected individuals. [45] [46] Conversely, people who lack androgenic hormones or are insensitive to the effects of androgens rarely have acne. [45] Pregnancy can increase androgen levels, and consequently, oily sebum synthesis. [46] [47] Acne can be a side effect of testosterone replacement therapy or anabolic steroid use. [1] [48] Over-the-counter bodybuilding and dietary supplements often contain illegally added anabolic steroids. [1] [49] Infections [ edit ] The anaerobic bacterial species Cutibacterium acnes (formerly Propionibacterium acnes ) contributes to the development of acne, but its exact role is not well understood. [2] There are specific sub-strains of C. acnes associated with normal skin and others with moderate or severe inflammatory acne. [50] It is unclear whether these undesirable strains evolve on-site or are acquired, or possibly both depending on the person. ... Infection with the parasitic mite Demodex is associated with the development of acne. [30] [51] It is unclear whether eradication of the mite improves acne. [51] Diet [ edit ] High- glycemic-load diets have been found to have different degrees of effect on acne severity. [7] [52] [53] Multiple randomized controlled trials and nonrandomized studies have found a lower-glycemic-load diet to be effective in reducing acne. [52] There is weak observational evidence suggesting that dairy milk consumption is positively associated with a higher frequency and severity of acne. [51] [54] [52] [55] [56] Milk contains whey protein and hormones such as bovine IGF-1 and precursors of dihydrotestosterone. [52] Studies suggest these components promote the effects of insulin and IGF-1 and thereby increase the production of androgen hormones, sebum, and promote the formation of comedones. [52] Available evidence does not support a link between eating chocolate or salt and acne severity. [54] [55] Few studies have examined the relationship between obesity and acne. [2] Vitamin B 12 may trigger skin outbreaks similar to acne (acneiform eruptions), or worsen existing acne when taken in doses exceeding the recommended daily intake . [57] Eating greasy foods does not increase acne nor make it worse. [58] [59] Stress [ edit ] There are few high-quality studies to demonstrate that stress causes or worsens acne. [60] Despite being controversial, some research indicates that increased acne severity is associated with high stress levels in certain contexts, such as hormonal changes seen in premenstrual syndrome . [61] [62] Other [ edit ] Mechanical obstruction of skin follicles with helmets or chinstraps can worsen pre-existing acne. [63] Several medications can also worsen pre-existing acne.
-
Von Willebrand Disease
Wikipedia
In this case, the function of VWF is not inhibited, but the VWF-antibody complex is rapidly cleared from the circulation. [ medical citation needed ] A form of VWD occurs in patients with aortic valve stenosis , leading to gastrointestinal bleeding ( Heyde's syndrome ). This form of acquired VWD may be more prevalent than is presently thought. ... PMID 8052974 . ^ Oxford Handbook of Clinical Haematology, Chapter 11 ^ Vincentelli A, Susen S, Le Tourneau T, Six I, Fabre O, Juthier F, Bauters A, Decoene C, Goudemand J, Prat A, Jude B (July 2003). "Acquired von Willebrand syndrome in aortic stenosis". The New England Journal of Medicine . 349 (4): 343–9. doi : 10.1056/NEJMoa022831 . PMID 12878741 . ^ Uriel N, Pak SW, Jorde UP, Jude B, Susen S, Vincentelli A, Ennezat PV, Cappleman S, Naka Y, Mancini D (October 2010). "Acquired von Willebrand syndrome after continuous-flow mechanical device support contributes to a high prevalence of bleeding during long-term support and at the time of transplantation" . ... PMID 10444294 . ^ Beighton, Peter; Beighton, Greta (2012). The Man Behind the Syndrome . Springer Science+Business Media. p. 187. ... Classification D ICD - 10 : D68.0 ICD - 9-CM : 286.4 OMIM : 193400 MeSH : D014842 DiseasesDB : 14007 External resources MedlinePlus : 000544 eMedicine : ped/2419 GeneReviews : von Willebrand Disease v t e Disorders of bleeding and clotting Coagulation · coagulopathy · Bleeding diathesis Clotting By cause Clotting factors Antithrombin III deficiency Protein C deficiency Activated protein C resistance Protein S deficiency Factor V Leiden Prothrombin G20210A Platelets Sticky platelet syndrome Thrombocytosis Essential thrombocythemia DIC Purpura fulminans Antiphospholipid syndrome Clots Thrombophilia Thrombus Thrombosis Virchow's triad Trousseau sign of malignancy By site Deep vein thrombosis Bancroft's sign Homans sign Lisker's sign Louvel's sign Lowenberg's sign Peabody's sign Pratt's sign Rose's sign Pulmonary embolism Renal vein thrombosis Bleeding By cause Thrombocytopenia Thrombocytopenic purpura : ITP Evans syndrome TM TTP Upshaw–Schulman syndrome Heparin-induced thrombocytopenia May–Hegglin anomaly Platelet function adhesion Bernard–Soulier syndrome aggregation Glanzmann's thrombasthenia platelet storage pool deficiency Hermansky–Pudlak syndrome Gray platelet syndrome Clotting factor Hemophilia A/VIII B/IX C/XI von Willebrand disease Hypoprothrombinemia/II Factor VII deficiency Factor X deficiency Factor XII deficiency Factor XIII deficiency Dysfibrinogenemia Congenital afibrinogenemia Signs and symptoms Bleeding Bruise Hematoma Petechia Purpura Nonthrombocytopenic purpura By site head Epistaxis Hemoptysis Intracranial hemorrhage Hyphema Subconjunctival hemorrhage torso Hemothorax Hemopericardium Pulmonary hematoma abdomen Gastrointestinal bleeding Hemobilia Hemoperitoneum Hematocele Hematosalpinx joint HemarthrosisVWF, P2RY12, F8, COX8A, ADAMTS13, GP1BA, F9, AK3, ABO, IL11, F11, ACTB, VWA8, ITIH1, TLR5, ITIH5, ANGPT2, POU2F3, CHRD, ALKBH1, CLEC4M, C20orf181, MUC5B, ATP6V0A2, SMPX, RABGEF1, CRISPLD2, SEC1P, PRB2, GP6, BMPER, TERF2IP, FAM20C, STXBP5, ANTXR1, ANO2, RAP1A, THPO, PDIA3, AGT, AVP, CANX, CD40, CLCA1, CSHL1, COCH, EPHA3, F2, F3, IFNA2, THBS1, RBPJ, ITGA2, ITGA2B, LRPAP1, MTHFR, CCN3, SERPINE1, PLG, POMC, SET, BOP
-
Plasma Cell Dyscrasias
Wikipedia
This form of MGRS is usually associated with other syndromes like glomerulopathy associated with a monoclonal immunoglobulin or C4 dense deposit disease associated with a monoclonal immunoglobulin. Diagnosis depends or identifying these other syndromes and the identification of complement components on kidney biopsy. ... Amyloidosis [ edit ] Main article: Amyloidosis Main article: Light chain deposition disease Amyloidosis is a general term for a protein misfolding syndrome that involves the deposition of a low molecular weight beta-pleated sheet -containing protein in extracellular tissues. ... The hematological response to chemotherapy of the AH and AHL renal amyloidosis patients was comparable to those with renal AL amyloidosis. [24] POEMS syndrome [ edit ] Main article: POEMS syndrome Main article: Castleman's disease POEMS syndrome (also known as Crow–Fukase syndrome, Takatsuki disease, or PEP syndrome) is a rare and complex medical syndrome that involves a combination of syndrome-defining signs and symptoms due to the dysfunction of multiple organs. The syndrome is associated with a plasma cell dyscrasia in almost 100% of cases, pathological overexpression of certain cytokines in >95% of cases, and the lymphoproliferative disorder termed Castleman's disease in ~15% of cases.
-
Basal-Cell Carcinoma
Wikipedia
Basal-cell carcinomas can often come in association with other lesions of the skin, such as actinic keratosis , seborrheic keratosis , squamous cell carcinoma . [15] In a small proportion of cases, basal-cell carcinoma also develops as a result of basal-cell nevus syndrome , or Gorlin Syndrome, which is also characterized by keratocystic odontogenic tumors of the jaw, palmar or plantar (sole of the foot) pits, calcification of the falx cerebri (in the center line of the brain) and rib abnormalities. The cause of this syndrome is a mutation in the PTCH1 tumor suppressor gene located in chromosome 9q22.3, which inhibits the hedgehog signaling pathway . ... Radiation therapy may be contraindicated for treatment of nevoid basal-cell carcinoma syndrome . A 2008 study reported that radiation therapy is appropriate for primary BCCs and recurrent BCCs, but not for BCCs that have recurred following previous radiation treatment. [44] Photodynamic therapy [ edit ] Photodynamic therapy (PDT) is a new modality for treatment of basal-cell carcinoma, which is administrated by application of photosensitizers to the target area. ... The development of multiple basal-cell cancer at an early age could be indicative of nevoid basal-cell carcinoma syndrome , also known as Gorlin Syndrome. [57] Notes [ edit ] ^ Desmoplastic tricoepithelioma is particularly similar to basal-cell carcinoma. ... "Nevoid Basal Cell Carcinoma (Gorlin) Syndrome". Neurocutaneous Disorders Phakomatoses and Hamartoneoplastic Syndromes . pp. 669–94. doi : 10.1007/978-3-211-69500-5_45 .