-
Pyaemia
Wikipedia
Diagnosis [ edit ] features of systemic inflammatory response syndrome tachycardia >90beats/min tachypnea >24/min temperature >38 or <36 Treatment [ edit ] Antibiotics are effective.
- Bubo Wikipedia
-
Pseudohallucination
Wikipedia
But "the current understanding of pseudohallucinations is mostly based on the work of Karl Jaspers ". [6] A further distinction is sometimes made between pseudohallucinations and parahallucinations , the latter being a result of damage to the peripheral nervous system . [7] They are considered a possible symptom of conversion disorder in DSM-IV (2000). [8] In DSM-5 (2013), this definition has been removed. [2] Also, pseudohallucinations can occur in people with visual/hearing loss, with the typical such type being Charles Bonnet syndrome . [ citation needed ] See also [ edit ] Anomalous experiences Auditory hallucination Illusion Lucid dream Phosphene References [ edit ] ^ Lavretsky, H. (1998).
-
Alpha-Fetoprotein, Hereditary Persistence Of
Omim
., hepatocellular carcinoma or teratoma) or in pregnant women being screened for neural tube defects or Down syndrome in the fetus. Greenberg et al. (1990) reported a family in which a 33-year-old man, 2 of his sibs, and a daughter showed elevated serum AFP levels.
-
Nodular Melanoma
Wikipedia
External links [ edit ] Classification D ICD - 10 : C43 ( ILDS C43.L10) ICD-O : M8721/3 v t e Skin cancer of nevi and melanomas Melanoma Mucosal melanoma Superficial spreading melanoma Nodular melanoma lentigo Lentigo maligna / Lentigo maligna melanoma Acral lentiginous melanoma Amelanotic melanoma Desmoplastic melanoma Melanoma with features of a Spitz nevus Melanoma with small nevus-like cells Polypoid melanoma Nevoid melanoma Melanocytic tumors of uncertain malignant potential Nevus / melanocytic nevus Nevus of Ito / Nevus of Ota Spitz nevus Pigmented spindle cell nevus Halo nevus Pseudomelanoma Blue nevus of Jadassohn–Tièche Cellular Epithelioid Deep penetrating Amelanotic Malignant Congenital melanocytic nevus ( Giant Medium-sized Small-sized ) Balloon cell nevus Dysplastic nevus / Dysplastic nevus syndrome Acral nevus Becker's nevus Benign melanocytic nevus Nevus spilus
-
Deafness, Autosomal Dominant 10
Omim
Noting that the 3 known EYA4 mutations causing nonsyndromic SNHL are predicted to encode truncated EYA proteins with a deleted Eya domain but an intact variable domain, whereas the EYA4 deletion (603550.0003) causing syndromic hearing loss with dilated cardiomyopathy (CMD1J; 605362) partially truncates the variable domain of the protein as well, Makishima et al. (2007) proposed a correlation between EYA4 mutation position and the presence or absence of DCM.
-
Glomerulocystic Kidney Disease With Hyperuricemia And Isosthenuria
Omim
Hypoplastic GCKD has been identified in some families with mutations in the TCF2 gene (189907) as part of the clinical phenotype of renal cysts and diabetes syndrome (137920). Clinical Features Sharp et al. (1997) reported a 3-generation African American family in which 7 affected individuals out of 20 available for study were identified by renal sonogram or renal histopathology.
-
Glomuvenous Malformation
Orphanet
Differential diagnosis The differential diagnosis should include mucocutaneous venous malformations (VMCMs, which are also commonly seen on mucosal membranes, are lighter purple in color than GMVs, and are compressible and generally not painful on palpation, and caused by inherited TIE2 / TEK mutations) and Blue rubber bleb nevus syndrome (characterized by the association of cutaneous and mucosal venous-like lesions with gastrointestinal lesions, and caused by somatic TIE2 / TEK mutations).
-
Mental Retardation, X-Linked 91
Omim
Clinical Features Gustavson et al. (1984) reported a girl with a developmental history and features typical of Prader-Willi syndrome (PWS; 176270), including muscular hypotonia that was severe in infancy, pronounced early childhood obesity, small hands and feet, shortness of the fifth fingers relative to the other digits, facial changes, and retarded psychomotor development.
- Familial Adenomatous Polyposis Medlineplus
-
Lichen Striatus
Wikipedia
External links [ edit ] Classification D ICD - 10 : L44.2 ICD - 9-CM : 697.8 DiseasesDB : 31402 External resources eMedicine : article/1111723 New England Journal of Medicine - Images of the Week v t e Papulosquamous disorders Psoriasis Pustular Generalized pustular psoriasis ( Impetigo herpetiformis ) Acropustulosis / Pustulosis palmaris et plantaris ( Pustular bacterid ) Annular pustular psoriasis Localized pustular psoriasis Other Guttate psoriasis Psoriatic arthritis Psoriatic erythroderma Drug-induced psoriasis Inverse psoriasis Napkin psoriasis Seborrheic-like psoriasis Parapsoriasis Pityriasis lichenoides ( Pityriasis lichenoides et varioliformis acuta , Pityriasis lichenoides chronica ) Lymphomatoid papulosis Small plaque parapsoriasis ( Digitate dermatosis , Xanthoerythrodermia perstans ) Large plaque parapsoriasis ( Retiform parapsoriasis ) Other pityriasis Pityriasis rosea Pityriasis rubra pilaris Pityriasis rotunda Pityriasis amiantacea Other lichenoid Lichen planus configuration Annular Linear morphology Hypertrophic Atrophic Bullous Ulcerative Actinic Pigmented site Mucosal Nails Peno-ginival Vulvovaginal overlap synromes with lichen sclerosus with lupus erythematosis other: Hepatitis-associated lichen planus Lichen planus pemphigoides Other Lichen nitidus Lichen striatus Lichen ruber moniliformis Gianotti–Crosti syndrome Erythema dyschromicum perstans Idiopathic eruptive macular pigmentation Keratosis lichenoides chronica Kraurosis vulvae Lichen sclerosus Lichenoid dermatitis Lichenoid reaction of graft-versus-host disease This cutaneous condition article is a stub .
-
Classic Congenital Adrenal Hyperplasia Due To 21-Hydroxylase Deficiency
Orphanet
Differential diagnosis Differential diagnoses include other forms of CAH, polycystic ovary syndrome (PCOS, see these terms) or any diseases with androgen excess.CYP21A2, POMC, CYP21A1P, HLA-B, AR, C4B, TNXB, HSD3B2, CYP2B6, GLO1, DKK1, NR3C1, C4B_2, CYP2C19, C4A, CYP17A1, TNFSF11, PRKAR1A, TRIM27, BRD2, SPG7, TNFRSF1B, TNXA, NR1I2, TNFRSF11B, NR1I3, TRIM13, CAPN10, AZF1, CFC1, CXADRP1, CASR, NR3C2, CYP11B1, HLA-A, CYP3A4, FPR2, GH1, GNRH1, GRB7, CYP3A7, CXADR, IRS1, HLA-DOA, ARR3, CRH, HSD17B1, IDS, IGF2, HSD3B1
-
Delirium
Wikipedia
Severe confusion that develops quickly, and often fluctuates in intensity Delirium Other names Acute confusional state Delirium is an acute disturbance of mental abilities Specialty Psychiatry , Geriatrics , Intensive care medicine , Neurology Symptoms agitation , confusion , drowsiness , hallucinations , delusions , memory problems Usual onset Any age, but more often in elderly Duration days to weeks, sometimes months Types Hyperactive, Hypoactive, Mixed state Causes Not well understood Risk factors Infection , chronic health problems, certain medications, neurological problems , sleep deprivation , surgery Differential diagnosis Dementia Treatment Medication, treating underlying cause Medication Haloperidol , Risperidone , Olanzapine , Quetiapine Delirium , also known as acute confusional state , is the organically caused decline from a previous baseline mental functioning that develops over a short period of time, typically hours to days. [1] [2] Delirium is a syndrome encompassing disturbances in attention, consciousness, and cognition. ... Without careful assessment and history, delirium can easily be confused with a number of psychiatric disorders or chronic organic brain syndromes because of many overlapping signs and symptoms in common with dementia , depression , psychosis , etc. [4] Delirium may manifest from a baseline of existing mental illness, baseline intellectual disability, or dementia, without being due to any of these problems. ... One research study has been reported on 7 patients who died during ICU admission. [33] Each case was admitted with a range of primary pathologies, but all had acute respiratory distress syndrome and/or septic shock contributing to the delirium, 6 showed evidence of low brain perfusion and diffuse vascular injury, and 5 showed hippocampal involvement. ... In the only population-based prospective study of delirium, older persons had an eight-fold increase in dementia and faster cognitive decline. [77] The same association is also evident in persons already diagnosed with Alzheimer’s dementia. [81] Recent long-term studies showed that many patients still meet criteria for delirium for a prolonged period after hospital discharge, with up to 21% of patients showing persistent delirium at 6 months post-discharge. [82] Dementia in ICU survivors [ edit ] See also: Post-intensive care syndrome Dementia is supposed to be an entity that continues to decline, such as Alzheimer’s disease. ... PMID 28165616 . ^ Engel GL, Romano J (Fall 2004). "Delirium, a syndrome of cerebral insufficiency. 1959".IL6, APOE, IGF1, SLC6A3, CXCL8, DRD3, IL1RN, DRD2, TH, LIF, SLC25A13, SRPX, DNMT1, NAGS, TRNE, PNN, CALM1, FIG4, CAMKMT, PRDX1, MMACHC, KRIT1, CRP, CALM2, CALM3, ALB, S100B, TNF, LAMC2, BTBD8, BDNF, BCHE, ENO2, CSF2, IL1B, COMT, NEFL, CIT, MTNR1B, CCL2, IL10, ACHE, HCRT, AMBP, IL2, IL17A, PLA2G15, CD2AP, MCF2L, CNOT1, WDHD1, CYP3A4, RRAGA, FGL2, ACSS2, CYP3A5, THOC1, EEF1A2, CCL4L2, ADAMTS2, CD19, PELI1, CCL28, ADIPOQ, CORO7, BCS1L, SARNP, ACCS, PRDM6, NLRP3, GRIN3A, AZGP1, SASS6, NLRP6, CCL4L1, PSS, ABCG2, PER2, IL18, TNFSF14, CXCL10, IL6R, LBP, LEP, LGALS3, LRP2, HTR2C, HTR1A, NPPB, AGT, ABCB1, PIK3CA, PIK3CB, PIK3CD, PIK3CG, NR3C1, S100A12, GRIN2B, GCLC, CCL4, GFAP, SOAT1, TCF21, GABBR1, FCGR3B, TXN, UCHL1, UGCG, FCGR3A, RN7SL263P
-
Adenosine Deaminase 2 Deficiency
Gene_reviews
A multigene panel that includes ADA2 and other genes associated with immune dysregulation, primary immunodeficiency, or autoinflammatory syndromes (see Differential Diagnosis) is most likely to identify a genetic cause at the most reasonable cost while limiting identification of variants of uncertain significance and pathogenic variants in genes that do not explain the underlying phenotype. ... The lymphoproliferative phenotype of DADA2 can include the following: Features mimicking the following disorders: GATA2 deficiency [Hsu et al 2016] Autoimmune lymphoproliferative syndrome (ALPS) [Alsultan et al 2018, Barzaghi et al 2019] Multicentric Castleman disease [Van Nieuwenhove et al 2018] CD3+ CD8+ T-cell large granular lymphocytic (T-LGL) infiltration of the bone marrow (in 2 individuals) [Trotta et al 2018]. ... Vasculitic complications are rare. Autoimmune lymphoproliferative syndrome (ALPS) CASP10 , FAS , FASLG 3 AD AR Lymphadenopathy, splenomegaly, immune-mediated cytopenia 4 ALPS, caused by primary defect in programmed cell death, has more autoimmune features. ... Features of DADA2 not observed are strokes, hematologic disorders, and immune deficiency. Sneddon syndrome characterized by livedo racemosa, Raynaud phenomenon, and noninflammatory thrombotic cerebral vasculopathy. It can be associated with systemic lupus erythematosus and antiphospholipid syndrome (antiphospholipid antibodies are detected in ~50% of affected individuals).
-
Beta-2-Adrenergic Receptor
Omim
Dallongeville et al. (2003) studied the association between the G16R (109690.0001) and Q27E (109690.0002) polymorphisms of the ADRB2 receptor and metabolic syndrome (605552) in 276 male and female patients with metabolic syndrome and 872 controls. Metabolic syndrome was defined according to National Cholesterol Education Program Adult Treatment Panel III guidelines. The G16R (P less than 0.005) and Q27E (P less than 0.04) polymorphisms were associated with metabolic syndrome in men, but not in women. Because both variants were in linkage disequilibrium, a haplotype analysis was performed. There was no evidence of any statistically significant association between ADRB2 haplotypes and metabolic syndrome. Evolution Cagliani et al. (2009) analyzed the recent evolutionary history of the ADRB genes in humans, with particular concern to selective patterns.
-
Frontotemporal Dementia
Omim
In addition to frontotemporal dementia, semantic dementia, and PPA, different clinical syndromes with overlapping features have been described, leading to confusion in the terminology (Tolnay and Probst, 2002). ... Kertesz (2003) suggested the term 'Pick complex' to represent the overlapping syndromes of FTD, primary progressive aphasia (PPA), corticobasal degeneration (CBD), PSP, and FTD with motor neuron disease. ... Personality and behavioral changes, including the Kluever-Bucy syndrome, were the first symptoms in 12 individuals. ... Lesions made of hyperphosphorylated tau similar to those found in AD are present in Down syndrome (190685), Niemann-Pick disease type C (257220), Gerstmann-Straussler-Scheinker disease (137440), prion protein amyloid angiopathy (see 176640), etc. ... Those with the behavioral variant of the disorder were more likely to have a positive family history than those with the language syndromes. Mutations in the MAPT and GRN genes were found in 8.9% and 8.4% of the cohort, respectively.
-
Succinic Semialdehyde Dehydrogenase Deficiency
Wikipedia
NINDS - National Institute of Neurological Disorders and Stroke External links [ edit ] Classification D ICD - 10 : E72.8 OMIM : 271980 MeSH : C535803 C535803, C535803 DiseasesDB : 29825 External resources Orphanet : 22 v t e Inborn error of amino acid metabolism K → acetyl-CoA Lysine /straight chain Glutaric acidemia type 1 type 2 Hyperlysinemia Pipecolic acidemia Saccharopinuria Leucine 3-hydroxy-3-methylglutaryl-CoA lyase deficiency 3-Methylcrotonyl-CoA carboxylase deficiency 3-Methylglutaconic aciduria 1 Isovaleric acidemia Maple syrup urine disease Tryptophan Hypertryptophanemia G G→ pyruvate → citrate Glycine D-Glyceric acidemia Glutathione synthetase deficiency Sarcosinemia Glycine → Creatine : GAMT deficiency Glycine encephalopathy G→ glutamate → α-ketoglutarate Histidine Carnosinemia Histidinemia Urocanic aciduria Proline Hyperprolinemia Prolidase deficiency Glutamate / glutamine SSADHD G→ propionyl-CoA → succinyl-CoA Valine Hypervalinemia Isobutyryl-CoA dehydrogenase deficiency Maple syrup urine disease Isoleucine 2-Methylbutyryl-CoA dehydrogenase deficiency Beta-ketothiolase deficiency Maple syrup urine disease Methionine Cystathioninuria Homocystinuria Hypermethioninemia General BC / OA Methylmalonic acidemia Methylmalonyl-CoA mutase deficiency Propionic acidemia G→ fumarate Phenylalanine / tyrosine Phenylketonuria 6-Pyruvoyltetrahydropterin synthase deficiency Tetrahydrobiopterin deficiency Tyrosinemia Alkaptonuria / Ochronosis Tyrosinemia type I Tyrosinemia type II Tyrosinemia type III / Hawkinsinuria Tyrosine → Melanin Albinism : Ocular albinism ( 1 ) Oculocutaneous albinism ( Hermansky–Pudlak syndrome ) Waardenburg syndrome Tyrosine → Norepinephrine Dopamine beta hydroxylase deficiency reverse: Brunner syndrome G→ oxaloacetate Urea cycle / Hyperammonemia ( arginine aspartate ) Argininemia Argininosuccinic aciduria Carbamoyl phosphate synthetase I deficiency Citrullinemia N-Acetylglutamate synthase deficiency Ornithine transcarbamylase deficiency / translocase deficiency Transport / IE of RTT Solute carrier family : Cystinuria Hartnup disease Iminoglycinuria Lysinuric protein intolerance Fanconi syndrome : Oculocerebrorenal syndrome Cystinosis Other 2-Hydroxyglutaric aciduria Aminoacylase 1 deficiency Ethylmalonic encephalopathy Fumarase deficiency Trimethylaminuria
-
Visual Impairment
Wikipedia
It has been estimated that over half of completely blind people have non-24-hour sleep–wake disorder , a condition in which a person's circadian rhythm , normally slightly longer than 24 hours, is not entrained (synchronized) to the light–dark cycle. [27] [28] Cause [ edit ] The most common causes of visual impairment globally in 2010 were: Refractive error (42%) Cataract (33%) Glaucoma (2%) Age-related macular degeneration (1%) Corneal opacification (1%) Diabetic retinopathy (1%) Childhood blindness Trachoma (1%) Undetermined (18%) [8] The most common causes of blindness worldwide in 2010 were: Cataracts (51%) Glaucoma (8%) Age-related macular degeneration (5%) Corneal opacification (4%) Childhood blindness (4%) Refractive errors (3%) Trachoma (3%) Diabetic retinopathy (1%) Undetermined (21%) [8] About 90% of people who are visually impaired live in the developing world . [5] Age-related macular degeneration, glaucoma, and diabetic retinopathy are the leading causes of blindness in the developed world. [29] Among working-age adults who are newly blind in England and Wales the most common causes in 2010 were: [30] Hereditary retinal disorders (20.2%) Diabetic retinopathy (14.4%) Optic atrophy (14.1%) Glaucoma (5.9%) Congenital abnormalities (5.1%) Disorders of the visual cortex (4.1%) Cerebrovascular disease (3.2%) Degeneration of the macula and posterior pole (3.0%) Myopia (2.8%) Corneal disorders (2.6%) Malignant neoplasms of the brain and nervous system (1.5%) Retinal detachment (1.4%) Cataracts [ edit ] Cataracts are the congenital and pediatric pathology that describes the greying or opacity of the crystalline lens, which is most commonly caused by intrauterine infections, metabolic disorders, and genetically transmitted syndromes. [31] Cataracts are the leading cause of child and adult blindness that doubles in prevalence with every ten years after the age of 40. [32] Consequently, today cataracts are more common among adults than in children. [31] That is, people face higher chances of developing cataracts as they age. ... UV-B rays). [32] Glaucoma [ edit ] Glaucoma is a congenital and pediatric eye disease characterized by increased pressure within the eye or intraocular pressure (IOP). [36] Glaucoma causes visual field loss as well as severs the optic nerve. [37] Early diagnosis and treatment of glaucoma in patients is imperative because glaucoma is triggered by non-specific levels of IOP. [37] Also, another challenge in accurately diagnosing glaucoma is that the disease has four causes: 1) inflammatory ocular hypertension syndrome (IOHS); 2) severe uveitic angle closure; 3) corticosteroid-induced; and 4) a heterogonous mechanism associated with structural change and chronic inflammation. [36] In addition, often pediatric glaucoma differs greatly in cause and management from the glaucoma developed by adults. [38] Currently, the best sign of pediatric glaucoma is an IOP of 21 mm Hg or greater present within a child. [38] One of the most common causes of pediatric glaucoma is cataract removal surgery, which leads to an incidence rate of about 12.2% among infants and 58.7% among 10-year-olds. [38] Infections [ edit ] The burden of onchocerciasis : children leading blind adults in Africa Childhood blindness can be caused by conditions related to pregnancy, such as congenital rubella syndrome and retinopathy of prematurity . ... One such example is Bardet–Biedl syndrome . Poisoning [ edit ] Rarely, blindness is caused by the intake of certain chemicals. ... Other [ edit ] Amblyopia : is a category of vision loss or visual impairment that is caused by factors unrelated to refractive errors or coexisting ocular diseases. [34] Amblyopia is the condition when a child's visual systems fail to mature normally because the child either suffers from a premature birth, measles, congenital rubella syndrome, vitamin A deficiency, or meningitis. [42] If left untreated during childhood, amblyopia is currently incurable in adulthood because surgical treatment effectiveness changes as a child matures. [42] Consequently, amblyopia is the world's leading cause of child monocular vision loss, which is the damage or loss of vision in one eye. [34] In the best case scenario, which is very rare, properly treated amblyopia patients can regain 20/40 acuity. [34] Corneal opacification Degenerative myopia Diabetic retinopathy : is one of the manifestation microvascular complications of diabetes, which is characterized by blindness or reduced acuity.TTPA, TSEN2, ATXN7, TSEN54, TSEN34, CLN6, HK1, WHRN, FOXP1, TBL2, CNNM4, PTPN22, SETBP1, NSMF, MMACHC, NDUFAF3, ABCA1, FSCN2, TUBGCP4, AIPL1, AMACR, LEMD3, ZFYVE26, SF3B1, CRB1, ADNP, SMCHD1, FLRT3, COQ2, PLXND1, GLRX5, NCAPG2, BCOR, AHI1, TRIM44, IL17RD, CNGB3, GTPBP2, NDUFB11, PIGT, PCDH12, TMEM216, SLC45A2, OSTM1, SAR1B, MECR, POLR1D, SOST, POMT2, GMPPA, GMPPB, SNX10, ANKRD11, UBE2T, FLVCR1, RPGRIP1L, SNRNP200, TTLL5, RAB11B, KIAA0586, IFT140, GDF3, GTF2IRD1, POLR1C, PEX16, HS6ST1, RAB28, ZNHIT3, AIMP1, LARGE1, ARNT2, AIFM1, USP8, UNC119, BAZ1B, AP3D1, BCL10, ST3GAL5, SYNJ1, PROM1, FGF17, PLEKHM1, SCO2, RIMS1, CIB2, ATF6, ARSG, EXOSC8, TREX1, PRDM5, CLP1, MALT1, PLK4, POMT1, SLC19A2, MAD2L2, USH1C, YAP1, TUBB4A, TUBB3, SEMA3A, TFG, IKZF1, LAMC3, TCIRG1, COQ7, TSFM, MKS1, RFWD3, FANCL, C12orf65, SFXN4, TWIST2, NUS1, C1QTNF5, SLC52A3, TP53RK, CEP41, CACNA2D4, CDHR1, RFT1, TMEM67, EARS2, TUBGCP6, ALG2, USP45, RAX2, KISS1R, ZNF469, SLX4, HPS3, PHF6, ANTXR1, ISCA2, USH1G, ADGRV1, MFSD8, SDHAF1, GDF6, FEZF1, PCARE, BLOC1S3, RGS9BP, NHLRC1, SUMF1, CCDC141, POC1B, IBA57, MICOS13, ARX, LCA5, VPS13B, C8orf37, CEP120, CKAP2L, B3GALNT2, B3GLCT, PROKR2, DRAM2, CEP78, BRIP1, SUCLA2, WDR45B, CC2D2A, ARID1B, TBC1D24, MCOLN1, SALL4, CYSLTR2, RPGRIP1, CABP4, MFF, INPP5E, ANKH, PROK2, SMG9, SPATA7, MBD5, WDR11, PEX26, OSGEP, CHD7, SLC39A4, POMGNT1, FANCI, FANCM, TRAPPC11, SLC4A11, SRD5A3, PITPNM3, SPRY4, ADAMTS10, COL18A1, SPG11, OPA3, CEP290, PDZD7, CSPP1, PALB2, CARS2, PIEZO2, SLC52A2, FKRP, PCDH15, NMNAT1, SEMA4A, XYLT2, NOD2, CDH23, PRDM16, ELMO2, HESX1, RGS9, PEX11B, CYTB, HBB, HARS1, HADHA, HSD17B10, GUCY2D, GUCA1B, GUCA1A, GTF2I, GSN, GRN, GNAT2, GNAQ, GNA11, GJA1, OPN1MW, GATA2, GABRD, FOXE3, FOXC1, FH, FGFR2, FGFR3, FGFR1, HCCS, HLA-A, HLA-B, LCAT, ATP6, MITF, MC1R, MAB21L1, LTBP2, LSS, LRPAP1, LRP5, LMNB1, LIMK1, LAMP2, HLA-DPA1, KIF11, ANOS1, ITPR1, IMPDH1, IGH, IGBP1, HSPG2, HSD17B4, HLA-DQB1, HLA-DPB1, FGF8, FDXR, FKTN, BRCA2, COL4A1, COL2A1, CNGA3, CLCN7, LYST, CAMK2B, CACNA1F, CA2, CFAP410, BTD, BRCA1, COL17A1, BDNF, KIF1A, RERE, ASPA, PHOX2A, ABCC6, FAS, BIRC3, AIRE, ABCD1, COL7A1, COX7B, EFEMP1, ERCC4, FBN1, FANCG, FANCF, FANCB, FANCE, FANCD2, FANCC, FANCA, ERCC6, ERCC5, ERCC2, CRX, ERCC1, ELN, DUSP6, TIMM8A, DDX3X, DCC, CYP1B1, CTSD, CTLA4, VCAN, COX3, ND1, ABCA4, ND2, TTR, TP53, TK2, TGFBI, TEK, TCOF1, TAT, TACR3, SYT1, SURF1, SRY, SOX10, SOX3, SOX2, SMARCB1, SMARCA4, SKI, SDHD, SDHA, SAG, RPE65, RPGR, RMRP, TYR, USH2A, CLRN1, PLA2G6, ADAM9, GPAA1, TNFSF11, CASK, PDXK, AP3B1, IKBKG, KCNAB2, CNTNAP1, PEX3, BAP1, VHL, TRRAP, ARID1A, NAA10, AAAS, EPM2A, ALMS1, XRCC2, WT1, CLIP2, BEST1, RFC2, REV3L, PRPH2, NDUFB8, OPA1, OCRL, OCA2, GPR143, NTRK2, NRL, NOTCH3, NHS, NF2, NDUFS2, MYOC, PRDX1, MYO7A, TRNS2, TRNL1, TRNK, TRNE, MTTP, ND6, ND5, ND4L, ND4, OTX2, PAX2, OPN1LW, POLA1, RAD51C, RAD51, PEX5, PEX2, PEX19, PRTN3, PRPS1, PRNP, PPP2CA, POLG, PLOD1, PAX6, PEX14, PEX13, PEX12, PEX10, PEX6, PEX1, PEPD, ENPP1, PDE6C, PCYT1A, RNU4ATAC
-
Colony Collapse Disorder
Wikipedia
Aspect of apiculture Honey bees at a hive entrance: one is about to land and another is fanning Colony collapse disorder ( CCD ) is an abnormal phenomenon that occurs when the majority of worker bees in a honey bee colony disappear, leaving behind a queen , plenty of food, and a few nurse bees to care for the remaining immature bees. [1] While such disappearances have occurred sporadically throughout the history of apiculture , and have been known by various names (including disappearing disease , spring dwindle , May disease , autumn collapse , and fall dwindle disease ), [2] the syndrome was renamed colony collapse disorder in late 2006 [3] in conjunction with a drastic rise in reports of disappearances of western honey bee ( Apis mellifera ) colonies in North America. [4] Beekeepers in most European countries have observed a similar phenomenon since 1998, especially in Southern and Western Europe; [5] [6] the Northern Ireland Assembly received reports of a decline greater than 50%. [7] The phenomenon became more global when it affected some Asian and African countries as well. [8] [9] Although the US industry has been declining, worldwide, the bee population has been increasing steadily since 1975, based on honey production. ... Suggested causes include pesticides ; [20] infections with various pathogens , especially those transmitted by Varroa and Acarapis mites ; malnutrition ; genetic factors ; immunodeficiencies ; loss of habitat ; changing beekeeping practices; or a combination of factors. [21] [22] A large amount of speculation has surrounded the contributions of the neonicotinoid family of pesticides to CCD, but many collapsing apiaries show no trace of neonicotinoids. [22] Contents 1 History 2 Signs and symptoms 3 Genetic and physio-pathological predictions 4 Scope and distribution 4.1 United States 4.2 Europe 4.3 Asia 5 Possible causes 5.1 Pesticides 5.1.1 Neonicotinoids 5.1.2 Other 5.2 Pathogens and immunodeficiency theories 5.2.1 Varroa mites 5.2.2 Israeli acute paralysis virus 5.2.3 Nosema 5.3 Viral and fungal combination 5.4 Fungicides 5.5 Antibiotics and miticides 5.5.1 Fluvalinate/coumaphos 5.6 Climate change 5.7 Bee rentals and migratory beekeeping 5.8 Selective commercial breeding and lost genetic diversity in industrial apiculture 5.9 Malnutrition 5.10 Electromagnetic radiation 5.11 Genetically modified crops 6 Management 7 Economic and ecological impact 8 In the media 9 See also 10 References 11 Further reading History [ edit ] Colony collapse disorder is a syndrome defined by a specific set of symptoms which, in the past several decades, has been given many different names (among them "disappearing disease", "spring dwindle", "May disease", "autumn collapse", and "fall dwindle disease"). [2] The cause of these symptoms has never been determined. Only very recently, upon recognition that the syndrome does not seem to be seasonally restricted, and that it may not be a "disease" in the standard sense—that there may not be one specific causative agent or pathogenesis —was the syndrome renamed. [3] Limited occurrences resembling CCD were documented as early as 1869. [23] [24] A well-documented outbreak of colony losses spread from the Isle of Wight to the rest of the UK in 1906. ... However, in late 2006 and early 2007, the rate of attrition was alleged to have reached new proportions, and people began to use the term colony collapse disorder to describe the sudden rash of disappearances (or sometimes spontaneous hive collapse or the Mary Celeste syndrome in the United Kingdom). [4] [32] Losses had remained stable since the 1990s at 17–20% per year, attributable to a variety of factors, such as mites, diseases, and management stress. [33] In the winter of 2004–2005, a spontaneous collapse occurred and was attributed to varroa mites (the "vampire mite" scare), though this was ultimately never confirmed. ... It is conjectured that Dicistroviridae , like the IAPV, cause degradation of the ribosomes , which are responsible for protein production of cells , and that this reduced ribosomal function weakens the bees, making them more vulnerable to factors that might not otherwise be lethal. [47] [149] Nosema [ edit ] Some have suggested the syndrome may be an inability by beekeepers to correctly identify known diseases such as European foulbrood or the microsporidian fungus Nosema apis .
-
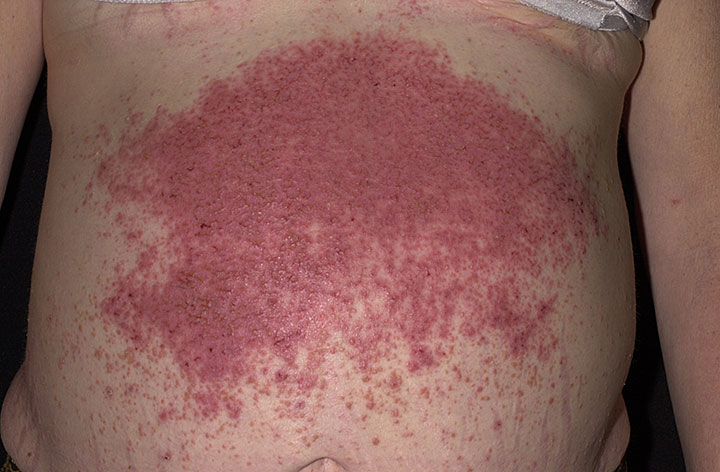
Dermatitis Herpetiformis
Wikipedia
It is an autoimmune disease , however, and thus individuals with DH are more likely to develop other autoimmune conditions such as thyroid disease, insulin-dependent diabetes , lupus erythematosus , Sjögren's syndrome , sarcoidosis , vitiligo , and alopecia areata . [37] There has been an association of non-Hodgkin lymphoma in individuals who have dermatitis herpetiformis, although this risk decreases to less than the population risk with a strict gluten-free diet. [12] [15] [38] Dermatitis herpetiformis does not usually cause complications on its own, without being associated with another condition. ... External links [ edit ] Classification D ICD - 10 : L12.2 , L13 ICD - 10-CM : L13.0 ICD - 9-CM : 694.0 MeSH : D003874 DiseasesDB : 3597 External resources MedlinePlus : 001480 eMedicine : derm/95 Orphanet : 1656 Pictures: DermNet NZ Pictures: The Gastrolab Image Library DermNet immune/dermatitis-herpetiformis Journal of Investigative Dermatology v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Vesiculobullous disease Acantholysis ( epidermis ) Pemphigus Pemphigus vulgaris : Pemphigus vegetans of Hallopeau of Neumann Pemphigus foliaceus : Pemphigus erythematosus Endemic pemphigus Paraneoplastic pemphigus IgA pemphigus Subcorneal pustular Intraepidermal neutrophilic Other Transient acantholytic dermatosis Pemphigoid ( dermis ) IgG : Bullous pemphigoid Cicatricial pemphigoid Localised Gestational pemphigoid Pemphigoid nodularis Epidermolysis bullosa acquisita IgA : Linear IgA bullous dermatosis Childhood Adult Other bullous Dermatitis herpetiformis In diseases classified elsewhere Porphyria cutanea tarda Bullous lupus erythematosus PUVA-induced acrobullous dermatosis v t e Gluten sensitivity Conditions general Wheat allergy Oat sensitivity nervous system GS idiopathic neuropathies digestive system Coeliac disease GSE associated conditions integumentary system Dermatitis herpetiformis Antibodies Anti-gliadin antibodies Anti-transglutaminase antibodies HLA-DQ HLA-DQ2 HLA-DQ8 Other Gluten immunochemistry Gluten-free diet Gluten challenge test List of people diagnosed with coeliac disease