-
Concussion
Wikipedia
Specialty Emergency medicine , neurology Symptoms Headache , trouble with thinking, memory or concentration, nausea, blurry vision , sleep disturbances, mood changes [1] Complications Chronic traumatic encephalopathy , Parkinson's disease , depression , post-concussion syndrome Duration Up to 4 weeks [2] Causes Motor vehicle collisions , falls , sports injuries , bicycle accidents [3] [4] Risk factors Drinking alcohol , playing contact sports such as American football , previous history of concussion [5] Diagnostic method Based on symptoms [6] Prevention Helmets when bicycling or motorbiking [3] Treatment Physical and cognitive rest for a day or two with a gradual return to activities [7] [2] Medication Paracetamol (acetaminophen), NSAIDs [2] Frequency 6 per 1,000 people a year [3] Concussion , also known as mild traumatic brain injury ( mTBI ), is a head injury that temporarily affects brain functioning . [8] Symptoms may include loss of consciousness (LOC); memory loss; headaches ; difficulty with thinking, concentration or balance; nausea; blurred vision ; sleep disturbances; and mood changes . [1] Any of these symptoms may begin immediately, or appear days after the injury. [1] Concussion should be suspected if a person indirectly or directly hits their head and experiences any of the symptoms of concussion. [9] It is not unusual for symptoms to last 2 weeks in adults and 4 weeks in children. [10] [2] Fewer than 10% of sports-related concussions among children are associated with loss of consciousness. [11] Common causes include motor vehicle collisions , falls , sports injuries , and bicycle accidents . [3] [4] Risk factors include drinking alcohol and a prior history of concussion. [10] [5] The mechanism of injury involves either a direct blow to the head or forces elsewhere on the body that are transmitted to the head. [10] This is believed to result in neuron dysfunction, as there are increased glucose requirements, but not enough blood supply. [2] A full differential diagnosis by a physician or nurse practitioner is required to rule out life threatening head injuries, injuries to the cervical spine, and neurological conditions. [6] [12] Glasgow coma scale score 13 to 15, loss of consciousness for less than 30 minutes, and memory loss for less than 24 hours may be used to rule out moderate or severe traumatic brain injuries . [6] Diagnostic imaging such as a CT scan or an MRI may also be required to rule out severe head injuries. [12] Routine imaging is not required to diagnose concussion. [13] Prevention of concussions includes the use of a helmet when bicycling or motorbiking . [3] Treatment includes physical and cognitive rest for 1–2 days, with a gradual step-wise return to activities, school, and work. [7] [2] [14] Prolonged periods of rest may slow recovery and result in greater depression and anxiety. [2] Paracetamol (acetaminophen) or NSAIDs may be recommended to help with a headache. [2] Physiotherapy may be useful for persistent balance problems; cognitive behavioral therapy may be useful for mood changes. [2] Evidence to support the use of hyperbaric oxygen therapy and chiropractic therapy is lacking. [2] Worldwide, concussions are estimated to affect more than 3.5 per 1,000 people a year. [15] Concussions are classified as mild traumatic brain injuries and are the most common type of TBIs. [3] [15] Males and young adults are most commonly affected. [3] [15] Outcomes are generally good. [16] Another concussion before the symptoms of a prior concussion have resolved is associated with worse outcomes. [17] [18] Repeated concussions may also increase the risk in later life of chronic traumatic encephalopathy , Parkinson's disease and depression . [19] Play media Video explanation of concussions in children [20] Contents 1 Signs and symptoms 1.1 Physical 1.2 Cognitive and emotional 2 Mechanism 2.1 Forces 2.2 Pathophysiology 3 Diagnosis 3.1 Classification 4 Prevention 5 Treatment 5.1 Rest and return to physical and cognitive activity 5.2 Return-to-school 5.3 Return-to-sport 5.4 Medications 5.5 Return to work 6 Prognosis 6.1 Pediatric concussion 6.2 People aged 65+ with concussion 6.3 Repeat concussion 6.4 Post-concussion syndrome 6.5 Cumulative effects 6.6 Second-impact syndrome 7 Epidemiology 7.1 Age 7.2 Sports 7.3 Workplace 8 History 9 Society and culture 9.1 Costs 9.2 Terminology 10 Research 10.1 Grading systems 11 See also 12 References 13 External links Signs and symptoms Concussions symptoms vary between people and include physical, cognitive, and emotional symptoms. [9] Symptoms may appear immediately or be delayed. [9] Up to one-third of people with concussion experience prolonged or persistent concussion symptoms, also known as post concussion syndrome , which is defined as concussion symptoms lasting for 4-weeks or longer in children/adolescents and symptoms lasting for more than 14 days in an adult. [12] [10] The severity of the initial symptoms is the strongest predictor of recovery time in adults. [10] Physical Headaches are the most common mTBI symptom. [21] Others include dizziness, vomiting, nausea, lack of motor coordination , difficulty balancing , [21] or other problems with movement or sensation. ... It is also a negative process if smaller impacts cause the same symptom severity. [93] Repeated concussions may increase a person's risk in later life for dementia, Parkinson's disease, and depression. [19] Post-concussion syndrome Main article: Post-concussion syndrome In post-concussion syndrome, symptoms do not resolve for weeks, months, or years after a concussion, and may occasionally be permanent. [112] About 10% to 20% of people have post-concussion syndrome for more than a month. [109] Symptoms may include headaches, dizziness, fatigue, anxiety , memory and attention problems, sleep problems, and irritability. [113] Rest, a previously recommended recovery technique, has limited effectiveness. [114] A recommended treatment in both children and adults with symptoms beyond 4 weeks involves an active rehabilitation program with reintroduction of non-contact aerobic activity. [115] Progressive physical exercise has been shown to reduce long-term post-concussive symptoms. [110] Symptoms usually go away on their own within months [87] but may last for years. [116] [117] The question of whether the syndrome is due to structural damage or other factors such as psychological ones, or a combination of these, has long been the subject of debate. [74] Cumulative effects As of 1999, cumulative effects of concussions were poorly understood, especially the effects on children. ... The condition was previously referred to as " dementia pugilistica ", or "punch drunk" syndrome, as it was first noted in boxers. The disease can lead to cognitive and physical handicaps such as parkinsonism , speech and memory problems, slowed mental processing, tremor, depression, and inappropriate behavior. [120] It shares features with Alzheimer's disease. [121] Second-impact syndrome Main article: Second-impact syndrome Second-impact syndrome, in which the brain swells dangerously after a minor blow, may occur in very rare cases. [ citation needed ] The condition may develop in people who receive second blow days or weeks after an initial concussion before its symptoms have gone away. [22] No one is certain of the cause of this often fatal complication, but it is commonly thought that the swelling occurs because the brain's arterioles lose the ability to regulate their diameter, causing a loss of control over cerebral blood flow. [65] As the brain swells , intracranial pressure rapidly rises. [58] The brain can herniate , and the brain stem can fail within five minutes. [22] Except in boxing, all cases have occurred in athletes under age 20. [48] Due to the very small number of documented cases, the diagnosis is controversial, and doubt exists about its validity. [122] A 2010 Pediatrics review article stated that there is debate whether the brain swelling is due to two separate hits or to just one hit, but in either case, catastrophic football head injuries are three times more likely in high school athletes than in college athletes. [11] Epidemiology Annual incidence of MTBI by age group in Canada [123] Most cases of traumatic brain injury are concussions. ... PMID 9701095 . ^ a b c d e f g Bowen AP (June 2003). "Second impact syndrome: a rare, catastrophic, preventable complication of concussion in young athletes".
-
Abortion In The Republic Of Ireland
Wikipedia
The High Court ruled on 9 May 2007 that she could not lawfully be prevented from travelling even though she was a ward of the state . [59] Amanda Mellet became pregnant in 2011; however, the foetus was suffering from Edwards syndrome , a fatal condition. She was unable to have an abortion in Ireland and had to travel to the UK. In 2016, she took a case to the United Nations Human Rights Committee , and in Mellet v Ireland it found that Ireland's abortion law violated the United Nations International Covenant on Civil and Political Rights and called for the law's reform. [60] The Irish government paid her €30,000 in compensation. [61] [22] In a case in 2010, the government of Ireland denied Siobhán Whelan an abortion despite being diagnosed with fatal foetal syndrome; she had to travel from Ireland to the UK to terminate her pregnancy. ... Mistaken cases of fatal foetal conditions [ edit ] In March 2019, a woman in Dublin was told her baby was likely to have Edwards syndrome , considered a fatal foetal condition, following a positive non-invasive prenatal test (NIPT) and a positive chorionic villus sampling (CVS) diagnostic test, the mother opted for an amniocentesis which was clear. She went on to give birth to a healthy baby without the condition. [69] In 2019, a woman attending the National Maternity Hospital was also given a diagnosis of Edwards syndrome. An abortion was carried out after 15 weeks. Following the abortion, genetic tests proved negative for Edwards syndrome, leaving the parents devastated and demanding an external investigation, which the hospital agreed to. [70] Pilots pressurised into having abortions [ edit ] According to the Irish Air Line Pilots' Association (IALPA), some female pilots of Irish registered airlines are under pressure to have an abortion if they become pregnant. [71] The issue was highlighted as many Irish-registered airlines use pilots hired under bogus self-employed contracts.
-
Sleepwalking
Wikipedia
There are varying degrees of amnesia associated with sleepwalking, ranging from no memory at all, vague memories or a narrative. [9] Associated disorders [ edit ] In the study "Sleepwalking and Sleep Terrors in Prepubertal Children" [10] it was found that, if a child had another sleep disorder – such as restless leg syndrome (RLS) or sleep-disorder breathing (SDB) – there was a greater chance of sleepwalking. ... Furthermore, the disappearance of the parasomnias after the treatment of the SDB or RLS periodic limb movement syndrome suggests that the latter may trigger the former. ... One study suggests higher levels of dissociation in adult sleepwalkers, since test subjects scored unusually high on the hysteria portion of the "Crown-Crisp Experiential Index". [12] Another suggested that "A higher incidence [of sleepwalking events] has been reported in patients with schizophrenia , hysteria and anxiety neuroses ". [13] Also, patients with migraine headaches or Tourette syndrome are 4–6 times more likely to sleepwalk. ... "Somnambulism in Children with Tourette Syndrome". Developmental Medicine & Child Neurology . 26 (4): 457–460. doi : 10.1111/j.1469-8749.1984.tb04471.x . ... External links [ edit ] Classification D ICD - 10 : F51.3 MeSH : D013009 DiseasesDB : 36323 SNOMED CT : 80495009 External resources MedlinePlus : 000808 eMedicine : article/1188854 Media related to Sleepwalking at Wikimedia Commons v t e Sleep and sleep disorders Stages of sleep cycles Rapid eye movement (REM) Non-rapid eye movement Slow-wave Brain waves Alpha wave Beta wave Delta wave Gamma wave K-complex Mu rhythm PGO waves Sensorimotor rhythm Sleep spindle Theta wave Sleep disorders Dyssomnia Excessive daytime sleepiness Hypersomnia Insomnia Kleine–Levin syndrome Narcolepsy Night eating syndrome Nocturia Sleep apnea Catathrenia Central hypoventilation syndrome Obesity hypoventilation syndrome Obstructive sleep apnea Periodic breathing Sleep state misperception Circadian rhythm disorders Advanced sleep phase disorder Cyclic alternating pattern Delayed sleep phase disorder Irregular sleep–wake rhythm Jet lag Non-24-hour sleep–wake disorder Shift work sleep disorder Parasomnia Bruxism Nightmare disorder Night terror Periodic limb movement disorder Rapid eye movement sleep behavior disorder Sleepwalking Somniloquy Benign phenomena Dreams Exploding head syndrome Hypnic jerk Hypnagogia / Sleep onset Hypnopompic state Sleep paralysis Sleep inertia Somnolence Nocturnal clitoral tumescence Nocturnal penile tumescence Nocturnal emission Treatment Sleep diary Sleep hygiene Sleep induction Hypnosis Lullaby Somnology Polysomnography Other Sleep medicine Behavioral sleep medicine Sleep study Daily life Bed Bunk bed Daybed Four-poster bed Futon Hammock Mattress Sleeping bag Bed bug Bedding Bedroom Bedtime Bedtime story Bedtime toy Biphasic and polyphasic sleep Chronotype Dream diary Microsleep Mouth breathing Nap Nightwear Power nap Second wind Siesta Sleep and creativity Sleep and learning Sleep deprivation / Sleep debt Sleeping while on duty Sleepover Snoring Authority control GND : 4179666-4
-
Sluggish Cognitive Tempo
Wikipedia
Particular type of attention disorder Sluggish cognitive tempo Specialty Psychology Sluggish cognitive tempo ( SCT ) is a syndrome related to attention deficit hyperactivity disorder (ADHD) but distinct from it. ... Examples might be conditions like depersonalization disorder , dysthymia , thyroid problems , [25] absence seizures , Bipolar II disorder , Kleine–Levin syndrome , forms of autism or schizoid personality disorder . [31] However, the prevalence of SCT in these clinical populations has yet to be empirically and systematically investigated. ... However, he does not further describe any symptoms of the disorder, making this an early but certainly non-specific reference to an SCT-like syndrome. [40] [8] One example from fictional literature is Heinrich Hoffmann 's character of "Johnny Head-in-Air" ( Hanns Guck-in-die-Luft ), in Struwwelpeter (1845). ... "Behavioural Assessment of the Dysexecutive Syndrome (BADS)" (PDF) . Journal of Occupational Psychology, Employment and Disability . 5 (2): 33–37. ... "Sluggish Cognitive Tempo: The Promise and Problems of Measuring Syndromes in the Attention Spectrum". In McBurnett, Keith; Pfiffner, Linda (eds.).
-
Aphthous Stomatitis
Wikipedia
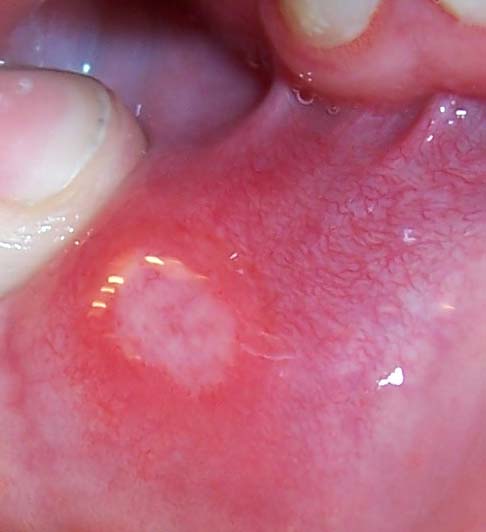
HIV/AIDS Inflammatory bowel disease MAGIC syndrome PFAPA syndrome Reactive arthritis Sweet's syndrome Ulcus vulvae acutum Main article: Oral ulceration Aphthous-like ulceration may occur in association with several systemic disorders (see table). ... Resolution of the systemic condition often leads to decreased frequency and severity of the oral ulceration. [5] Behçet's disease is a triad of mouth ulcers, genital ulcers and anterior uveitis . [7] The main feature of Behçet's disease is aphthous-like ulceration, but this is usually more severe than seen in aphthous stomatitis without a systemic cause, and typically resembles major or herpetiforme ulceration or both. [6] [14] Aphthous-like ulceration is the first sign of the disease in 25–75% of cases. [5] Behçet's is more common in individuals whose ethnic origin is from regions along the Silk Road (between the Mediterranean and the Far East ). [15] It tends to be rare in other countries such as the United States and the United Kingdom. [7] MAGIC syndrome is a possible variant of Behçet's disease, and is associated with aphthous-like ulceration. The name stands for "mouth and genital ulcers with inflamed cartilage" ( relapsing polychondritis ). [8] PFAPA syndrome is a rare condition that tends to occur in children. [8] The name stands for "periodic fever , aphthae, pharyngitis (sore throat) and cervical adenitis " (inflammation of the lymph nodes in the neck). ... Synonyms for major RAS include Sutton's ulcers (named after Richard Lightburn Sutton ), Sutton's disease, [30] Sutton's syndrome and pariadenitis mucosa necrotica recurrens. [2] [8] Synonyms for aphthous stomatitis as a whole include (recurrent) oral aphthae, (recurrent) aphthous ulceration and (oral) aphthosis. [5] [13] In traditional Chinese medicine , claimed treatments for aphthae focus on clearing heat and nourishing Yin . [31] Rembrandt Gentle White toothpaste did not contain sodium lauryl sulfate, and was specifically marketed as being for the benefit of "canker sore sufferers". ... PMID 17850936 . ^ Dalvi SR, Yildirim R, Yazici Y (December 2012). "Behcet's Syndrome". Drugs . 72 (17): 2223–41. doi : 10.2165/11641370-000000000-00000 .
-
Silent Stroke
Wikipedia
Increased levels of CRP as measured by a CRP test or the more sensitive high serum CRP (hsCRP) test and elevated levels of I6 as measured by an IL6 ELISA are markers for the increased risk of silent stroke. [27] Diabetes mellitus : untreated or improperly managed diabetes mellitus is associated with an increased risk for silent stroke. [28] Hypertension : which affects up to 50 million people in the United States alone is the major treatable risk factor associated with silent strokes. [29] Homocysteine : elevated levels of total homocysteine (tHcy) an amino acid are an independent risk factor for silent stroke, even in healthy middle-aged adults. [30] [31] [32] Metabolic syndrome (MetS):Metabolic syndrome is a name for a group of risk factors that occur together and increase the risk for coronary artery disease, stroke, and type 2 diabetes. A higher number of these MetS risk factors the greater the chance of having a silent stroke. [33] [34] Polycystic ovary syndrome (PCOS): is associated with double the risk for arterial disease including silent stroke independent of the subjects Body mass index (BMI). [35] Sleep apnea : encompasses a heterogeneous group of sleep-related breathing disorders in which there is repeated intermittent episodes of breathing cessation or hypopnea , when breathing is shallower or slower than normal. [36] Sleep apnea is a common finding in stroke patients but recent research suggests that it is even more prevalent in silent stroke and chronic microvascular changes in the brain. ... PMID 11340219 . ^ Bokura, H; Yamaguchi, S; Iijima, K; Nagai, A; Oguro, H (2008). "Metabolic syndrome is associated with silent ischemic brain lesions" . ... "Significant association of metabolic syndrome with silent brain infarction in elderly people".
-
Functional Hypothalamic Amenorrhea
Wikipedia
Functional hypothalamic amenorrhea Other names Functional hypothalamic amenorrhoea, juvenile hypothalamosis syndrome Specialty Gynaecology , Endocrinology Functional hypothalamic amenorrhea (FHA) is a form of amenorrhea and chronic anovulation [1] and is one of the most common types of secondary amenorrhea . [2] It is classified as hypogonadotropic hypogonadism . [3] It was previously known as "juvenile hypothalamosis syndrome," prior to the discovery that sexually mature females are equally affected. [4] FHA has multiple risk factors, with links to stress-related, weight-related, and exercise-related factors. ... When diagnosing individuals with FHA it is important to do so while taking prior menstrual disorders into consideration. [16] Patients with a history of, or who currently have, FHA, who become pregnant, require extra care and monitoring during pregnancy to avoid the increased risks of inadequate weight gain, intrauterine fetal growth restrictions , miscarriage , and/or preterm labor . [3] Bone [ edit ] Decreased fat tissue mass and imbalances between bodyweight, fat tissue mass, and lean body mass has been linked to reduced BMD in FHA patients; however, absolute bone strength has not always been found to be affected. [3] The majority of people reach their peak bone mass (PBM) around 30 years of age, however, 40-50% of that mass is formed during puberty. [3] When FHA occurs in adolescence, inability to reach PBM becomes a primary concern, as 40-60% of factors contributing to PBM are of hormonal and nutritional influence. [3] Estrogens , androgens , GH , and IGF-1 are the main determinants of PBM formation. [3] In women, estrogens are the main component in proper bone formation . [3] Through the stimulation of growth factors such as transforming growth factor beta (TGF-B) , bone morphogenetic protein 6 (6-BMP-6) , and IGF-1 and inhibition of receptor activator of nuclear factor kappa-B ligand (RANKL) , estrogen tends to suppress bone resorption and activate bone formation and remodeling units. [3] Because FHA causes hypoestrogenism , women with FHA may lack age-appropriate bone density [5] and have an increased risk of skeletal fragility, stress fractures , osteopenia , and osteoporosis . [3] The profile of low serum IGF-1 , low serum insulin , and high serum cortisol also contribute to low BMD . 8 Adiponectin has also been found to regulate the activity of osteoblasts and osteoclasts , possibly providing a link between the abnormal concentrations found in FHA patients with altered bone metabolism. [8] Additionally, women with FHA may have improper diets or malnutrition , leading to low calcium and vitamin D intake , and may have a tendency to overexercise, which further increases the risk for osteopenia . [3] This improper dieting and tendency to overexercise, leading to low bone density, is also seen in RED-S . [17] Unlike in males diagnosed with RED-S , females are at an increased risk for the consequences of decreased bone density , since females have a PBM 25-30% lower than males. [3] Although this decreased bone density is also seen in anorexia nervosa , the severity of peak bone density loss is less in FHA patients. [3] Cardiovascular [ edit ] Cardiovascular disease (CVD) is the leading cause of death in women in developed countries, and it is well studied that hypoestrogenism has many regulatory functions in the cardiovascular system . [3] Estradiol ( E2 ), an estrogen steroid hormone and the major female sex hormone , has a cardio-protective effect. [3] As such, hypoestrogenism caused by FHA causes significant impairment in the endothelial and vascular function, NO bioactivity, autonomic function, the renin-angiotensin system , and lipid profiles. [3] [13] It has been hypothesized that premenopausal hypoestrogenemia caused by ovarian disruption, including that induced by FHA, increases the risk for the premature acquisition and accelerated development of atherosclerosis in these patients. [10] In hypoestrogenic women with FHA, measures of flow-mediated dilation (FMD) indicate that the positive effects on endothelial function typically conferred by exercise are not realized, but possibly reversed. [10] It has been suggested that long term estrogen deficiency may alter vasculature structure and responsiveness, as an impaired response to exogenous NO by arterial smooth muscle has been demonstrated in patients with FHA. [10] Although hypoestrogenism is the main cause of impaired cardiovascular health in FHA, patients also suffer from metabolic disturbances and an overall negative energy balance that further increases the risk of CVD . [3] Women with FHA caused by exercised-induced factors tend to have a higher lipid profile. [18] As is expected from the presence of heightened levels of superoxides and decreased NO bioavailability in women with FHA, it has been found that LDLc is mildly elevated at rest in these women, and it is more susceptible to oxidation after intense exercise; these levels inversely relate to brachial artery FMD in the same population. [10] While it is not known if reported endothelial dysfunction is caused by LDLc oxidation in these women, the positive relationship between LDLc and atherosclerosis risk are well documented. [10] A relationship has been studied with FHA and diabetes mellitus , [3] with women who have both FHA and diabetes mellitus having a higher risk for CVD than women who have only diabetes mellitus . [13] Studies indicate that the loss of endogenous estrogens through hypothalamic suppression may worsen an already-existing hyperglycemia , further antagonizing estrogen -mediated NO release and compounding the risk for vascular dysfunction in patients with both FHA and diabetes mellitus . [10] [13] Neurological [ edit ] High levels of cortisol caused by FHA is seen not just in peripheral tissues, but also in the cerebrospinal fluid (CSF) , where it is unbound and therefore more biologically available. [5] FHA accelerates the onset of aging syndromes, such as osteoporosis and vaginal atrophy . [3] [4] Because of the high levels of cortisol in the CSF , it is suggested that the chronic stress that causes FHA may alter not just the endocrinological secretory patterns , but also the neurological secretory patterns. This altering can impact brain health, and can lead to an increased risk in neurological aging syndromes, such as dementia and Alzheimer's Disease (AD) . [5] The low levels of estrogen seen in FHA may also contribute to the increased neurodegenerative risk. [5] Microglia are the main immune cells of the central nervous system (CNS) and protect the brain Estrogen is a significant regulator of microglia , and limits the inflammation that occurs when the brain is stressed (e.g. due to bacteria, viruses, hypoxia ). [5] In FHA, the lack of adequate estrogen levels, combined with the chronic stress that caused FHA, promotes a neuroinflammatory state that can cause impaired neuron formation and neuronal stem cell survival, and promote neurodegenerative diseases . [5] However, more research is needed to find a direct link between FHA and its long term effects on neurological health. ... At present, it is unknown if the positive effects of HDLc are able to counteract the effects of elevated LDLc in this population. [10] Another juxtaposition is found in the fact that rather than improving BMD , as is expected by exercise, patients with EAA commonly display osteopenia . [3] If exercise contributes to a negative energy balance, either through excess activity or inadequate caloric intake, stress and skeletal fractures, as well as premature bone loss, becomes a significant risk. [3] Some studies suggest female athletes with FHA may also be affected by hyperandrogenism in addition to hypoestrogenism , and it is the hyperandrogenism (as seen in polycystic ovary syndrome ) that causes the menstrual irregularity, rather than chronic low energy availability and low estrogen levels. [6] While this population may also suffer from higher fasting glucose and blood pressure, less stress fractures and higher BMDs have been observed in patients whose FHA may be due to hyperandrogenemia . [6] However, although further studies and analysis is needed in this area, these findings may imply that LH/FSH ratios could be used as a future biomarker of metabolic and skeletal health in amenorrheic female athletes. [6] Genetic predisposition [ edit ] Idiopathic hypogonadotropic hypogonadism (IHH) , otherwise known as congenital GnRH deficiency, has a known genetic basis. ... The combination of these factors could help explain why populations whose conditions have been triggered by low weight or excess exercise are not only more prone to display elevated serum ghrelin levels, but also commonly engage in abnormal eating behaviors. [8] Ghrelin not only reduces fat utilization and stimulates appetite, but increased ghrelin is linked to alterations in GnRH and LH pulsatility, which can ultimately inhibit the HPO axis . [3] [8] Its elevation in women with FHA may account for the inability of some patients who have returned to a healthy weight to return to regular menses. [3] Conversely, leptin is reduced in patients with FHA and this may suppress GnRH through a kisspeptin -mediated pathway. [3] [12] Leptin and adiponectin are secreted by adipocytes and are directly related to FFM, with the former being directly related and the latter being inversely related. [8] Leptin coordinates metabolic and hormonal signals with reproductive function, and decreased levels of leptin have been shown to decrease LH pulsatile frequency. [11] As leptin mainly decreases feeding behavior, negative energy states have been linked to decreased leptin levels when fat mass is at critically low levels. [11] Thus, hypoleptinemia is often representative of the chronic negative energy balance associated with FHA, and this trend holds true when compared to age-, weight-, and body fat-matched eumenorrheic controls [3] [11] Further, the arcuate nucleus of the hypothalamus, which is known for its regulation of food intake, is considered to be the most concentrated source of both leptin and GnRH receptors in the brain. [11] While GnRH receptors in the hypothalamus do not contain receptors for leptin , a positive correlation has been shown to exist between leptin receptor mRNA and the kisspeptin -expressing cells which are known to stimulate GnRH release. [11] Diagnosis [ edit ] Females who have menstrual cycles lasting longer than 45 days and/or amenorrhea for three or more months should be evaluated for FHA. [9] Differentiating FHA from the irregular menstrual patterns seen in adolescents during the initial years after menarche due to immaturity of the HPO axis can be challenging. [4] [9] However, studies have shown that even during this period, the length of a menstrual cycle does not exceed 45 days. [4] [9] Furthermore, healthy girls with normal BMI (18.5–25 kg/m 2 ) should develop regular menstrual cycles (every 28 +/- 3–5 days) within 1–2 years after menarche . [4] [9] FHA is a diagnosis of exclusion , because the diagnosis can only be made when menstruation has ceased in that absence of organic or anatomic pathology, [4] [3] [11] [9] and thus the evaluation should be used to rule out organic causes of amenorrhea (e.g., pregnancy , thyroid disorders , inflammatory bowel disease , etc.) [4] [9] Endocrinologic etiologies of the thyroid , pituitary , and adrenal glands , ovarian failure , and hyperandrogenism including polycystic ovarian syndrome (PCOS) must be excluded before a diagnosis of FHA can be given. [1] A GnRH stimulation or challenge test should be used to identify FHA as the cause hypogonadotropic hypogonadism in women presenting with symptoms, as hypothalamic dysfunction due to delayed-onset puberty or other pituitary disease will not respond to exogenous GnRH . [4] [3] Hypothalamic disorders are differentiated when GnRH administration results in abnormal increases of gonadotropins . [4] Combined pituitary and hypothalamic impairment is differentiated when there is a decreased or absent response to GnRH secretion; as a result, it impossible to determine if the observed low levels of FSH/LH are due to hypothalamic or pituitary dysfunction, and pulsatile GnRH administration with cyclomate is required to diagnose this distinction (pulsatile LH-RH challenge). [4] Evaluation for FHA may include a thorough history and physical exam, laboratory testing, and imaging if appropriate.
-
Hemolytic Disease Of The Newborn (Anti-Kell)
Wikipedia
External links [ edit ] Classification D ICD - 10 : P55.8 ICD - 9-CM : 773.2 v t e Conditions originating in the perinatal period / fetal disease Maternal factors complicating pregnancy, labour or delivery placenta Placenta praevia Placental insufficiency Twin-to-twin transfusion syndrome chorion / amnion Chorioamnionitis umbilical cord Umbilical cord prolapse Nuchal cord Single umbilical artery presentation Breech birth Asynclitism Shoulder presentation Growth Small for gestational age / Large for gestational age Preterm birth / Postterm pregnancy Intrauterine growth restriction Birth trauma scalp Cephalohematoma Chignon Caput succedaneum Subgaleal hemorrhage Brachial plexus injury Erb's palsy Klumpke paralysis Affected systems Respiratory Intrauterine hypoxia Infant respiratory distress syndrome Transient tachypnea of the newborn Meconium aspiration syndrome Pleural disease Pneumothorax Pneumomediastinum Wilson–Mikity syndrome Bronchopulmonary dysplasia Cardiovascular Pneumopericardium Persistent fetal circulation Bleeding and hematologic disease Vitamin K deficiency bleeding HDN ABO Anti-Kell Rh c Rh D Rh E Hydrops fetalis Hyperbilirubinemia Kernicterus Neonatal jaundice Velamentous cord insertion Intraventricular hemorrhage Germinal matrix hemorrhage Anemia of prematurity Gastrointestinal Ileus Necrotizing enterocolitis Meconium peritonitis Integument and thermoregulation Erythema toxicum Sclerema neonatorum Nervous system Perinatal asphyxia Periventricular leukomalacia Musculoskeletal Gray baby syndrome muscle tone Congenital hypertonia Congenital hypotonia Infections Vertically transmitted infection Neonatal infection rubella herpes simplex mycoplasma hominis ureaplasma urealyticum Omphalitis Neonatal sepsis Group B streptococcal infection Neonatal conjunctivitis Other Miscarriage Perinatal mortality Stillbirth Infant mortality Neonatal withdrawal
-
Delayed Sleep Phase Disorder
Wikipedia
(July 1981). "Delayed sleep phase syndrome. A chronobiological disorder with sleep-onset insomnia". ... "A prospective study of delayed sleep phase syndrome in patients with severe resistant obsessive-compulsive disorder" . ... "A length polymorphism in the circadian clock gene Per3 is linked to delayed sleep phase syndrome and extreme diurnal preference" . ... "Posttraumatic delayed sleep phase syndrome". Neurology . 54 (1): 250–2. doi : 10.1212/wnl.54.1.250 . ... "Phase-dependent treatment of delayed sleep phase syndrome with melatonin" . Sleep . 28 (10): 1271–8. doi : 10.1093/sleep/28.10.1271 .
-
Mold Health Issues
Wikipedia
According to the Institute of Medicine, there is a significant association between dampness in the home and wheeze, cough, and upper respiratory symptoms. [17] A later analysis determined that 30% to 50% of asthma-related health outcomes are associated with not only mold, but also dampness in buildings. [17] Another health effect associated with dampness and mold is Sick Building Syndrome (SBS), which is defined by manifestations of symptomatic illness as a result of poor indoor air quality and pollutant exposures. [17] Signs of potentially illness-causing buildings include condensation on the windows, high humidity in the bathrooms, a moldy odor, or water leakage. [18] While there is a proven correlation between mold exposure and the development of upper and lower respiratory syndromes, there are still fewer incidences of negative health effects than one might expect. [19] Barbeau and colleagues suggested that studies do not show a greater impact from mold exposure for several reasons: 1) the types of health effects are not severe and are therefore not caught; 2) people whose homes have flooded find alternative housing to prevent exposure; 3) self-selection, the healthier people participated in mold clean-up and were less likely to get sick; 4) exposures were time-limited as result of remediation efforts and; 5) the lack of access to health care post-flooding may result in fewer illnesses being discovered and reported for their association with mold. [19] There are also certain notable scientific limitations in studying the exposure effects of dampness and molds on individuals because there are currently no known biomarkers that can prove that a person was exclusively exposed to molds. [20] Thus, it is currently impossible to prove correlation between mold exposure and symptoms. [20] Mold-associated conditions [ edit ] Health problems associated with high levels of airborne mold spores include [21] [ unreliable medical source? ... In 1927, Ismailson, a Soviet scientist, noted a form of mycotoxicosis in employees in a binder twine factory. [50] In the 1940s, "Stachybotryotoxicosis" was identified in Ukraine as a new disease in humans in close contact with moldy hay, including inhalation of the associated dust, which caused, among other symptoms, a "haemorrhagic exúdate". [51] Following cases of pulmonary hemorrhage in infants in Cleveland , Ohio in 1993–94, several related studies suggested a causal relationship between exposure to S. chartarum and the disease. [52] [53] [54] [55] [56] [57] An anonymous panel from within the CDC revisited the cases and argued that the link was not proven. [58] [59] [60] Subsequent studies with mice and rats exposed to S. chartarum and associated mycotoxins showed that pulmonary hemorrhage could occur, suggesting the link is plausible. [61] [62] [63] The American Academy of Pediatrics also found the link plausible, [64] and subsequent analysis and case studies with humans have further noted the association. [65] [66] [67] As well, a 1987 report by the United States Army Medical Research Institute of Infectious Diseases suggested that the effects of "trichothecene mycotoxins are more than 10 times greater via inhalation than via intravenous exposure." [68] [69] The presumed mechanism of action is that Stachybotrys produces a compound, stachylysin, which is a hemolysin that disintegrates (lyses) red blood cells. [70] [71] [72] Innate immune activation [ edit ] The health hazards produced by mold have been associated with sick building syndrome (SBS), but previously, controversy existed around whether studies had sufficiently demonstrated that indoor exposures to these common organisms posed a significant threat. [4] In 1986, a study noted an airborne outbreak of toxicosis from trichothecenes associated with Stachybotrys atra in a Chicago house affecting a family including their maid; symptoms included diarrhea, headaches, fatigue, dermatitis, malaise, and severe leg pains, which resolved following remediation of the mold contamination. [73] This study drew attention to how mycotoxins in indoor environments might impact health. ... Eiser, professor emeritus of medicine at Drexel University College of Medicine , has suggested that environmental factors such as dampness and mold may be a contributing factor for why Finland has the highest death rate from dementia in the world. [134] The WHO estimates the prevalence of significant dampness and mold in buildings to be at least 20%, while other estimates of US homes suggest a prevalence as high as 47%. [135] [136] Sleeping disorders are also associated with exposure to dampness and mold, consistent with the decrease in α-melanocyte stimulating hormone (α-MSH) associated with this syndrome. [137] Patients may also present with psychological symptoms given the neuroinflammatory markers and growth factors involved. [138] [139] [140] [141] Exposure sources and prevention [ edit ] The primary sources of mold exposure are from the indoor air in buildings with substantial mold growth and the ingestion of food with mold growths. ... Afterwards, she fell ill with neurological symptoms, environmental sensitivity, and fatigue, and was eventually diagnosed with chronic inflammatory response syndrome (CIRS) (see Innate immune activation ). [173] [174] This led to a federal inquiry into biotoxin-related illnesses in 2018. [175] [176] It is currently unclear if the Department of Health have made any changes to the Australian healthcare system in response to the Inquiry and subsequent report. [177] [178] But the Australian Government formally responded to the recommendations made by the inquiry in March 2020, [179] and the National Construction Code was updated in 2019 to implement higher standards regarding condensation management in building design. [180] [181] [182] As of 2020, the US Centers for Disease Control and Prevention (CDC) are yet to acknowledge or warn the public of the multi-system, chronic inflammatory, and innate immune system effects that can occur from exposure to dampness, mold, and water-damaged buildings. [183] Today, the US Food and Drug Administration and the agriculture industry closely monitor mold and mycotoxin levels in grains and foodstuffs to keep the contamination of animal feed and human food supplies below specific levels. ... "Neurologic and neuropsychiatric syndrome features of mold and mycotoxin exposure".
-
Rotator Cuff Tear
Wikipedia
Those most prone to failed rotator cuff syndrome are people 65 years of age or older; and those with large, sustained tears. ... Another potential contributing cause is impingement syndrome , the most common non-sports related injury and which occurs when the tendons of the rotator cuff muscles become irritated and inflamed while passing through the subacromial space beneath the acromion . ... Repetitive impingement can inflame the tendons and bursa, resulting in the syndrome. [26] [27] Extrinsic factors [ edit ] A flattened or hooked acromion can predispose a shoulder to rotator cuff impingement and tearing. ... Those who report such symptoms frequently are diagnosed with failed rotator cuff syndrome. There is no irrefutable evidence that rotator cuff surgery benefits more than non-surgical management [55] and a percentage of individuals never regain full range of motion after surgery. [80] Arthroscopic procedures produce "satisfactory results" more than 90 percent of the time. ... "Diagnostic accuracy of clinical tests for the different degrees of subacromial impingement syndrome" . The Journal of Bone and Joint Surgery.
-
Shoulder Problem
Wikipedia
Other regions within the body (such as gallbladder , liver , or heart disease , or disease of the cervical spine of the neck) also may generate pain that the brain may interpret as arising from the shoulder. [1] Contents 1 Shoulder structures and functions 2 Diagnosis 2.1 Medical history and physical exam 2.2 Diagnostic tests 3 Dislocation 3.1 Description 3.2 Signs and diagnosis 3.3 Treatment 4 Separation 4.1 Description 4.2 Signs and diagnosis 4.3 Treatment 5 Sternoclavicular separation 5.1 Description 5.2 Signs and diagnosis 5.3 Treatment 6 Tendinitis, bursitis, impingement syndrome, and rotator cuff tears 6.1 Description 6.2 Signs 6.3 Diagnosis 6.4 Treatment 6.5 Rotator cuff tear 7 SLAP tear (lesion) 7.1 Symptoms 7.2 Diagnosis 7.3 Treatment 7.4 Recovery 8 Frozen shoulder (adhesive capsulitis) 9 Fracture 9.1 Description 9.2 Signs and diagnosis 9.3 Treatment 10 Arthritis of the shoulder (glenohumeral joint) 10.1 Description 10.2 Signs and diagnosis 10.3 Treatment 11 Arthritis or osteolysis of the AC (acromioclavicular) joint 11.1 Description 11.2 Signs and diagnosis 11.3 Treatment 12 Treatment 13 References 14 External links Shoulder structures and functions [ edit ] The shoulder joint is composed of three bones: the clavicle (collarbone), the scapula (shoulder blade), and the humerus (upper arm bone) (see diagram). ... In severe cases, surgery may be advised. [ citation needed ] Tendinitis, bursitis, impingement syndrome, and rotator cuff tears [ edit ] Main article: Rotator cuff Description [ edit ] These conditions are closely related and may occur alone or in combination. ... Squeezing of the rotator cuff is called impingement syndrome. [ citation needed ] An inflamed bursa is called bursitis . Tendinitis and impingement syndrome are often accompanied by inflammation of the bursa sacs that protect the shoulder. ... Ultrasound scans are frequently used to confirm a suspected tendinitis or bursitis as well as rule out a tear in the rotator cuff muscles. Impingement syndrome may be confirmed when injection of a small amount of anesthetic (lidocaine hydrochloride) into the space under the acromion relieves pain. [ citation needed ] Treatment [ edit ] Anti-inflammatory medicines such as aspirin , naproxen or ibuprofen among others can be taken to help with pain.
-
Femoroacetabular Impingement
Wikipedia
Femoroacetabular impingement Other names Hip impingement syndrome , Play media The three recognized types of femoroacetabular impingement. ... The diagnosis is often made in conjunction with a labral tear. [26] Differential Diagnosis [9] [ edit ] Piriformis syndrome or strain Labral tear without FAI Adductor muscle strain Sciatica Athletic pubalgia Gluteus medius / minimus or illiopsoas tendinopathy Stress fracture Femoral head osteonecrosis Other impingements , including anterior inferior iliac spine , ischiofemoral and iliopsoas Loose body in the joint (intra-articular body) Prevention [ edit ] Prevention is currently being investigated. [27] The goal of prevention would be to avoid joint damage and premature hip osteoarthritis. [27] Studies are examining the effectiveness of screening adolescents in school and targeting at-risk individuals for education, physical therapy and decreasing participation in possibly harmful activities/sports as referenced in the epidemiology section. [27] Treatment [ edit ] Treatment of FAI can be divided into those that are non-operative (conservative) and operative. ... PMID 25308887 . ^ Dooley PJ (January 2008). "Femoroacetabular impingement syndrome: Nonarthritic hip pain in young adults" . ... "Lower limb biomechanics in femoroacetabular impingement syndrome: a systematic review and meta-analysis". ... "What treatment options exist for patients with femoroacetabular impingement syndrome but without surgical indication?".
-
Scarlet Fever
Wikipedia
Persons present with what is called acute nephritic syndrome , in which they have high blood pressure, swelling, and urinary abnormalities. ... However, these children tend to be younger than 5 years old, their fever lasts longer (at least five days), and they have additional clinical criteria (including signs such as conjunctival redness and cracked lips), which can help distinguish this from scarlet fever. [29] Toxic shock syndrome : Both streptococcal and staphylococcal bacteria can cause this syndrome. ... It can be distinguished from scarlet fever by low blood pressure, lack of sandpaper texture for the rash, and multi-organ system involvement. [30] Staphylococcal scalded skin syndrome : This is a disease that occurs primarily in young children due to a toxin-producing strain of the bacteria Staphylococcus aureus . ... However, in 1979, Keith Powell identified it as in fact the same illness as the form of scarlet fever which is caused by staphylococcal exotoxin and is known as staphylococcal scalded skin syndrome . [47] [48] [49] [50] Scarlet fever serum from horses' blood was used in the treatment of children beginning in 1900 and reduced mortality rates significantly. ... PMID 367152 . ^ Melish, ME; Glasgow, LA (June 1971). "Staphylococcal scalded skin syndrome: the expanded clinical syndrome" .
-
Insomnia
Wikipedia
Inability to fall or stay asleep Insomnia Other names Sleeplessness, trouble sleeping A drawing of someone with insomnia from the 14th century Pronunciation / ɪ n ˈ s ɒ m n i ə / [1] Specialty Psychiatry , sleep medicine Symptoms Trouble sleeping , daytime sleepiness, low energy, irritability, depressed mood [1] Complications Motor vehicle collisions [1] Causes Unknown, psychological stress , chronic pain , heart failure , hyperthyroidism , heartburn , restless leg syndrome , others [2] Diagnostic method Based on symptoms, sleep study [3] Differential diagnosis Delayed sleep phase disorder , restless leg syndrome , sleep apnea , psychiatric disorder [4] Treatment Sleep hygiene , cognitive behavioral therapy , sleeping pills [5] [6] [7] Frequency ~20% [8] [9] [10] Insomnia , also known as sleeplessness , is a sleep disorder in which people have trouble sleeping . [1] They may have difficulty falling asleep, or staying asleep as long as desired. [9] [11] Insomnia is typically followed by daytime sleepiness, low energy, irritability , and a depressed mood . [1] It may result in an increased risk of motor vehicle collisions , as well as problems focusing and learning. [1] Insomnia can be short term, lasting for days or weeks, or long term, lasting more than a month. [1] Insomnia can occur independently or as a result of another problem. [2] Conditions that can result in insomnia include psychological stress , chronic pain , heart failure , hyperthyroidism , heartburn , restless leg syndrome , menopause , certain medications, and drugs such as caffeine , nicotine , and alcohol . [2] [8] Other risk factors include working night shifts and sleep apnea . [9] Diagnosis is based on sleep habits and an examination to look for underlying causes. [3] A sleep study may be done to look for underlying sleep disorders. [3] Screening may be done with two questions: "do you experience difficulty sleeping?" ... Nocturnal polyuria , excessive nighttime urination, can be very disturbing to sleep. [22] Subjectivity [ edit ] Main article: Sleep state misperception Some cases of insomnia are not really insomnia in the traditional sense, because people experiencing sleep state misperception often sleep for a normal amount of time. [23] The problem is that, despite sleeping for multiple hours each night and typically not experiencing significant daytime sleepiness or other symptoms of sleep loss, they do not feel like they have slept very much, if at all. [23] Because their perception of their sleep is incomplete, they incorrectly believe it takes them an abnormally long time to fall asleep , and they underestimate how long they remain asleep. [23] Causes [ edit ] Symptoms of insomnia can be caused by or be associated with: Sleep breathing disorders, such as sleep apnea or upper airway resistance syndrome [24] Use of psychoactive drugs (such as stimulants ), including certain medications , herbs , caffeine , nicotine , cocaine , amphetamines , methylphenidate , aripiprazole , MDMA , modafinil , or excessive alcohol intake [25] Use of or withdrawal from alcohol and other sedatives, such as anti-anxiety and sleep drugs like benzodiazepines [25] Use of or withdrawal from pain-relievers such as opioids [25] Heart disease [26] Restless legs syndrome , which can cause sleep onset insomnia due to the discomforting sensations felt and the need to move the legs or other body parts to relieve these sensations [27] Periodic limb movement disorder (PLMD), which occurs during sleep and can cause arousals of which the sleeper is unaware [28] Pain : [29] an injury or condition that causes pain can preclude an individual from finding a comfortable position in which to fall asleep, and can also cause awakening. ... While addiction does not seem to be an issue with this class of drugs, they can induce dependence and rebound effects upon abrupt cessation of use. [ citation needed ] However, people whose insomnia is caused by restless legs syndrome may have worsened symptoms with antihistamines. [107] Melatonin [ edit ] The evidence for melatonin in treating insomnia is generally poor. [108] There is low quality evidence that it may speed the onset of sleep by 6 minutes. [108] Ramelteon , a melatonin receptor agonist , does not appear to speed the onset of sleep or the amount of sleep a person gets. [108] Most melatonin drugs have not been tested for longitudinal side effects. [109] Prolonged-release melatonin may improve quality of sleep in older people with minimal side effects. [110] [111] Studies have also shown that children who are on the Autism spectrum or have learning disabilities, Attention-Deficit Hyperactivity Disorder (ADHD) or related neurological diseases can benefit from the use of melatonin. ... Elderly people are more sensitive to these side-effects. [127] Some benzodiazepines have demonstrated effectiveness in sleep maintenance in the short term but in the longer term benzodiazepines can lead to tolerance , physical dependence , benzodiazepine withdrawal syndrome upon discontinuation, and long-term worsening of sleep, especially after consistent usage over long periods of time. ... Retrieved 11 July 2013 . ^ "Restless Legs Syndrome/Periodic Limb Movement Disorder" .MEIS1, ADORA2A, LMX1B, GABRB3, HCRT, PRNP, TUBB3, TBL2, GTF2I, GTF2IRD1, HLA-DQB1, HLA-DRB1, HMBS, PINK1, LIMK1, DNAJC6, MEN1, VPS13C, HTRA2, PRKN, CLIP2, SIN3A, PODXL, SLC25A13, ZNF365, QARS1, RFC2, PARK7, SLC12A3, SNCA, FARS2, UCHL1, LRRK2, BAZ1B, CPOX, ELN, DCTN1, CRY1, CLCNKB, UNC80, NAGS, CLOCK, CRP, OPN1SW, SLC6A4, BDNF, REM1, ACTG2, POTEM, POTEKP, COPD, ACOT7, ACTG1, ACTBL2, FHL5, GAD1, SERPINA3, SLC17A5, MDD1, HTR2A, PSG5, VIP, SDHD, IL6, PER3, CELIAC6, RLS1, MIR182, CD200R1, GSC, TPPP, FREM3, UTS2, PPARGC1A, CTCF, IGSF6, SEMA4D, MARCHF11, EBPL, UBE2Z, ABCB6, RLS3, PCSK9, PPP2R3C, MIR146A, MOCOS, MSTO1, ARSI, TMED9, SIAE, GAL, PYCARD, ADIPOQ, CHDH, CENPJ, FBXO3, PPARGC1B, PART1, DDAH1, USE1, DDAH2, PLEKHM2, NDUFS7, ZC4H2, GTF2H5, IS1, STAC, PKD2L1, ELK3, LEPR, LCN2, IL1B, IARS1, HRES1, HCRTR2, HCRTR1, GSR, GSK3B, PRLHR, FSHMD1A, FLT4, FLNA, ERCC2, DRD2, MAP6, CYP19A1, CYP3A4, CYP2C9, CYP2B6, CASP9, STS, ARNTL, AR, AMT, AMPD1, ALB, AHR, JAG1, ADRA2A, MXD1, SMCP, WASF1, ROM1, TIMELESS, PER2, CDK5R1, TP63, MADD, TAM, PAX8, TST, TPO, TPH1, TNF, STAR, ACHE, CCL11, PSMD9, MET, PRL, POMC, PIGR, PDC, PAX6, PAEP, OPRM1, OPRK1, OAT, NDUFS4, MTNR1B, MTNR1A, MPST, MAP3K10, OCLN
-
Tonsillitis
Wikipedia
Rarely, the infection may spread beyond the tonsil resulting in inflammation and infection of the internal jugular vein giving rise to a spreading infectious thrombophlebitis ( Lemierre's syndrome ). [ citation needed ] In strep throat , diseases like post-streptococcal glomerulonephritis [ non-primary source needed ] [40] can occur. ... Classification D ICD - 10 : J03 , J35.0 ICD - 9-CM : 463 MeSH : D014069 DiseasesDB : 13165 External resources MedlinePlus : 001043 eMedicine : article/871977 Patient UK : Tonsillitis v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis Authority control NDL : 00563120GALNS, PAGR1, GAST, MBL3P, VDR, IFNG, IL1B, MBL2, DEFB1, RXRB, TRBV20OR9-2, S100A7, CCL20, CCL24, SKP1, SOD2, BCL2, TNFSF13, TLR4, PRCP, PDLIM7, ANP32B, CCL27, PART1, TLR9, AICDA, RNASE2, LTF, MTHFR, CCNB1, CDKN2A, EGFR, FANCD2, FCN2, GEM, GPX1, HIF1A, HLA-B, HLA-C, IGHG3, IL6, CXCL8, IL10, KIR2DS1, KIR3DL1, KIR3DL2, LTA, FDCSP
-
Binge Drinking
Wikipedia
Approximately 40% of alcoholics report heavy drinking during adolescence. [31] Repeated episodes of excessive drinking, especially at an early age, are thought to cause a profound increase in the risk of developing an alcohol-related disorder (ICD-10, harmful use/dependence syndrome). Heavy drinking is also closely associated with depression . ... A particular study conducted by the National Longitudinal Survey of Youth found that harmful drinking during adolescent years was significantly associated with the continuance of dangerous levels of alcohol consumption into adulthood years. [37] [38] Binge drinking is a way for young adolescents to rely alcohol as a way to cope with certain stress or depression. [39] Central nervous system [ edit ] See also: Alcohol withdrawal syndrome § Kindling , and Kindling (substance withdrawal) Heavy binge drinkers tend to have delayed auditory and verbal memory and deficits in executive planning function and episodic memory, which are similar to deficits seen in Korsakoff's syndrome . ... Alcohol has definite long-term adverse effects on the fetus, in particular impaired attentional skills and may lead to psychiatric disorders when the child grows up. [44] In a 2005 study in the US, approximately one in five non-pregnant women binge-drank and one in 25 pregnant women binge-drank. [6] Binge drinking during pregnancy is associated with fetal alcohol syndrome , alcohol-related birth defects as well as alcohol-related neurodevelopmental disorders. ... "Recognition and prevention of fetal alcohol syndrome". Obstet Gynecol . 106 (5 Pt 1): 1059–64. ... "Estimating the prevalence of fetal alcohol syndrome. A summary" . Alcohol Res Health . 25 (3): 159–67.
-
Laminitis
Wikipedia
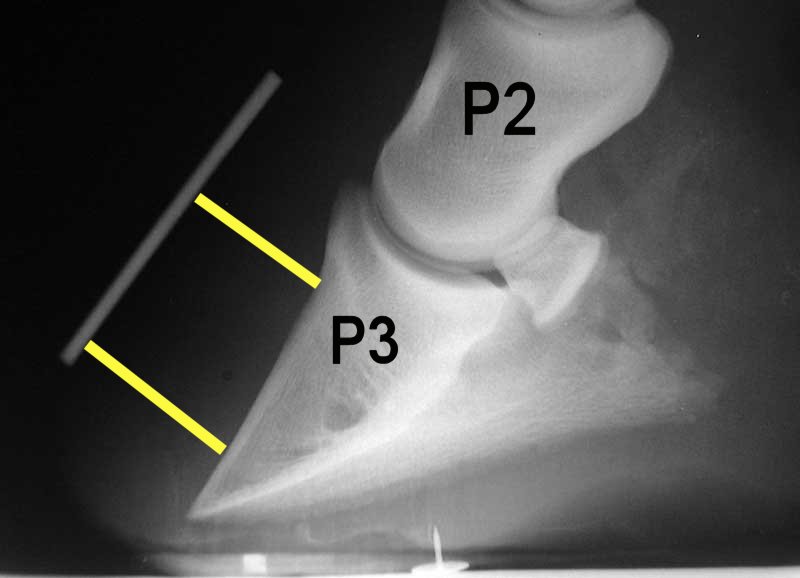
Endocrinopathy Endocrinopathy is usually the result of improper insulin regulation, and is most commonly seen with pituitary pars intermedia dysfunction (also called equine Cushing's syndrome) and equine metabolic syndrome (EMS), [4] as well as obesity and glucocorticoid administration. [5] In cases of EMS, most episodes occur in the spring when the grass is lush. [4] Trauma Mechanical laminitis starts when the hoof wall is pulled away from the bone or lost, as a result of external influences. ... Insulin-resistant horses with laminitis must be removed from all green grass and be fed only hay tested for nonstructural carbohydrates (sugar, starch and fructan) and found to be below 11% on a dry-matter basis. See also: Equine metabolic syndrome Vasoactive amines [ edit ] The inflammatory molecule histamine has also been hypothesized as a causative agent of laminitis. [8] [9] However, contradictory evidence indicates the role of histamine in laminitis has not been conclusively established. [10] Mechanical separation [ edit ] See also: § Mechanical laminitis Commonly known as road founder , mechanical separation occurs when horses with long toes are worked extensively on hard ground. ... However, the continual shifting of weight required to balance in a moving vehicle may enhance blood circulation, so some horsemen recommend trailering as an initial step in rehabilitation of a horse after long confinement. [ citation needed ] Laminitis has been observed following an equine standing in extreme conditions of cold, especially in deep snow. [ citation needed ] Laminitis has also followed prolonged heating such as may be experienced from prolonged contact with extremely hot soil or from incorrectly applied hot-shoeing. [ citation needed ] Complex causes [ edit ] Pituitary pars intermedia dysfunction , or Cushing's disease, is common in older horses and ponies and causes an increased predisposition to laminitis. Equine metabolic syndrome is a subject of much new research and is increasingly believed to have a major role in laminitis. ... It has some similarities to type II diabetes in humans. In this syndrome, peripheral fat cells synthesise adipokines which are analogous to cortisol, resulting in Cushings-like symptoms. ... With modern therapies, most laminitics will be able to bear a rider or completely recover, if treated quickly, and if the laminitis was not severe or complicated (e.g. by equine metabolic syndrome or Cushing's disease ). Even in these cases, a clinical cure can often be achieved.
-
Kmt2b-Related Dystonia
Gene_reviews
Disorders Associated with Complex Early-Onset Generalized Dystonia to Consider in the Differential Diagnosis of KMT2B -Related Dystonia View in own window Disorder Gene(s) MOI Additional Overlapping Clinical Features Distinguishing Features of Differential Diagnosis Disorder Clinical MRI Laboratory Findings Inherited forms of dystonia 1 DYT-TOR1A (DYT1) TOR1A AD Isolated dystonia w/less prominent cervical/cranial/bulbar features early in disease course DYT-THAP1 (DYT6) THAP1 AD Early craniofacial involvement & laryngeal dystonia Isolated dystonia w/older average age of onset DYT-PRKRA (DYT16) PRKRA AR Mild parkinsonism Early-onset NBIA disorders 2 PKAN PANK2 AR Parkinsonism Spasticity Eye movement abnormalities Optic atrophy Axonal neuropathy Seizures Characteristic T 2 -weighted hypointensity in globus pallidus & substantia nigra PLAN PLA2G6 AR MPAN C19orf12 AR BPAN WDR45 XL FAHN FA2H AR Kufor-Rakeb syndrome ATP13A2 AR CoPAN COASY AR Disorders of heavy metal metabolism Wilson disease ATP7B AR Psychiatric comorbidities Tremor Liver disease Kayser-Fleischer corneal ring Face-of-the-giant-panda sign ↓ serum ceruloplasmin ↑ serum non-ceruloplasmin-bound copper SLC39A14 deficiency SLC39A14 AR Parkinsonism Spasticity Dysarthria Bulbar dysfunction T 1 -weighted hyperintensities & T 2 -weighted hypointensities in basal ganglia & anterior pituitary gland, cerebellum, dorsal pons, spinal cord Hypermanganesemia Dystonia/parkinsonism, hypermanganesemia, polycythemia, and chronic liver disease SLC30A10 AR Parkinsonism Liver disease T 1 -weighted hyperintensities in basal ganglia Hypermanganesemia Polycythemia Neurotransmitter disorders Sepiapterin reductase deficiency SPR AR Hypotonia Progressive parkinsonism-dystonia Eye movement disorder Delayed motor milestones Reduced tracer uptake on DaTSCAN images (DTDS) CSF neurotransmitter abnormalities GTPCH1 deficiency (OMIM 233910) GCH1 AR Tyrosine hydroxylase deficiency TH AR Aromatic L-amino acid decarboxylase deficiency (OMIM 608643) DDC AR Brain serotonin-dopamine deficiency [Rilstone et al 2013] SLC18A2 AR SLC6A3 -related dopamine transporter deficiency syndrome SLC6A3 AR Mitochondrial disorders Mitochondrial cytopathies See footnote 3 AD AR Mat Multisystemic involvement Commonly shows "Leigh" radiologic appearance of T 2 -weighted hyperintensities in basal ganglia / brain stem / medulla Leukodystrophy ↑ lactate, pyruvate Metabolic acidosis POLG -related disorders POLG AR Other inherited metabolic disorders Alpha-fucosidosis (OMIM 230000) FUCA1 AR ID Dementia Delayed motor skills Dysostosis multiplex Seizures Spasticity Angiokeratomas Distinct facial features Glutaric acidemia type 1 (OMIM 231670) GCDH AR Encephalopathic crisis associated w/infections/fever (between 6-18 mos) Macrocephaly Frontotemporal atrophy Widening of sylvian fissures T 2 -weighted hyperintensities in basal ganglia ↑ urinary 3-OH-glutaric acid Glutaryl carnitine Methylmalonic acidemia, late-onset (See Isolated Methylmalonic Acidemia.) MCEE MMAA MMAB MMADHC MUT AR Hypotonia; psychiatric symptoms Failure to thrive Renal syndromes ID Metabolic stroke-like events ↑ plasma & urine MMA w/normal B 12 , tHcy, & methionine levels ↑ propionylcarnitine (C3) Hyperammonemia Lactic acidosis Propionic acidemia, late-onset PCCA PCCB AR Failure to thrive DD ID Gastrointestinal symptoms ↑ propionylcarnitine (C3) in plasma, ↑ 3-hydroxypropionate in urine, hyperammonemia, lactic acidosis Niemann-Pick disease type C NPC1 NPC2 AR Spasticity Hepatomegaly/ splenomegaly Supranuclear gaze palsy Cataplexy Seizures Psychiatric comorbidities ↑ oxysterol levels GM1 gangliosidosis, type III (See GLB1 -Related Disorders.) GLB1 AR Extrapyramidal signs Skeletal abnormalities Cardiomyopathy Lesch-Nyhan syndrome HPRT1 XL Pyramidal signs Self-mutilation Hyperuricemia Other monogenic disorders with prominent dystonia phenotype ADCY5 -related movement disorder ADCY5 AD Hypotonia Chorea Orolingual dyskinesia Myoclonus Spasticity Episodic exacerbations of movement disorder Rapid-onset dystonia-parkinsonism (See ATP1A3 -Related Neurologic Disorders.) ... DNAJC6 FBX07 PARK7 (DJ1) PINK1 PRKN (PARK2) AR Young-onset dystonia-parkinsonism (DYT16) [Camargos et al 2008] PRKRA AR TUBB4A -related leukodystrophy (H-ABC) TUBB4A AD ID Motor delay Spasticity Hypomyelinating leukodystrophy Cerebellar & basal ganglia atrophy Deafness-dystonia-optic neuronopathy syndrome TIMM8A XL Pyruvate carboxylase deficiency PC AR AD = autosomal dominant; AR = autosomal recessive; DD = developmental delay; ID = intellectual disability; Mat = maternal inheritance; MOI = mode of inheritance; XL = X-linked 1.
-
Niemann-Pick Disease Type C
Gene_reviews
These include juvenile dystonic idiocy, juvenile dystonic lipidosis, juvenile NPC, neurovisceral lipidosis with vertical supranuclear gaze palsy, Neville-lake disease, sea-blue histiocytosis, lactosylceramidosis, and DAF ( d owngaze paralysis, a taxia, f oam cells) syndrome. The term Niemann-Pick disease type D describes a genetic isolate from Nova Scotia that is biochemically and clinically indistinguishable from NPC and that also results from biallelic pathogenic variants in NPC1 . ... Niemann-Pick disease type B AR Later onset & milder in manifestations than NPD-A; hepatosplenomegaly w/progressive hypersplenism & stable liver dysfunction AR = autosomal recessive; MOI = mode of inheritance; NPD-A = Niemann-Pick disease type A Childhood presentations include acquired conditions such as pineal region or midbrain tumors causing dorsal midbrain syndrome, hydrocephalus, attention-deficit disorder, learning disabilities, absence seizures, other dementing illnesses, pseudodementia (depressive disorder), HIV encephalopathy, sleep disorders, and syncope. Hereditary disorders to consider include subacute necrotizing encephalomyelopathy (see Mitochondrial DNA-Associated Leigh Syndrome and NARP and Nuclear Gene-Encoded Leigh Syndrome Spectrum Overview), mitochondrial disorders, hereditary dystonias, and the conditions summarized in Table 4. ... CHMP2B -FTD, GRN -FTD, C9orf72 amyotrophic lateral sclerosis and FTD), and Steele-Richardson-Olzewski syndrome (also known as progressive supranuclear palsy; see OMIM 601104) Late-onset lysosomal storage diseases Syphilis and HIV dementia Primary psychiatric illnesses Management Clinical management guidelines for Niemann-Pick C (NPC) have been published [Geberhiwot et al 2018] (full text).NPC1, LIPA, NPC2, PDLIM7, APP, SMPD1, PSMB9, ABCA1, RASSF1, CDKN2A, TNF, CHIT1, LINC01193, ERCC2, FCER2, IFNG, LAMP1, LDLR, CD274, MAPT, VEGFA, BACE1, PTCH1, CCL2, SOX2, TP53, ERCC1, H3P10, ATM, CKS1B, SRRM2, APOE, POSTN, APOD, WIF1, CUL9, NBEAL2, SIRT1, TARDBP, SEZ6L, SCO2, ARL2BP, DDX58, APC, TRIM29, DKK3, PDCD4, TMEM97, ANXA6, HDAC6, RAB9A, ATP7B, CD163, TRAF1, UBE2N, UGCG, VHL, VIM, VIP, ZNF154, BSND, ARID1A, ULK1, NR0B2, BECN1, CDK5R1, PER2, ST3GAL5, SPHK1, ARF6, FOXP3, ZMYND10, GDE1, MIR185, NEGR1, NPCA1, H19, STPG4, CELIAC2, ANXA1, MIR10B, MIR130A, MIR203A, RTRAF, MIR31, POU5F1P3, POU5F1P4, UCA1, MIR663A, APOBEC3A_B, UPK3B, CNE-2, NPB, APOBEC3A, ARHGAP42, CKS1BP7, NLK, OTUD4, NLRP2, LPAR5, GBA2, OVOL2, NEUROG2, ROBO3, GORASP1, WNK1, SPNS1, HAVCR2, FATE1, SCGB3A1, CDCA5, SEZ6, OSCP1, TP73, B2M, CP, CD58, GCHFR, GFAP, HCRT, HDAC2, HLA-A, HOXC6, HSPB1, HSP90AA1, IGFBP6, XRCC6, IL1A, IL1B, IL12A, IL17A, JAK2, JUN, JUNB, JUND, GBA, FOSB, THBS1, EGR1, CPT1A, CRP, CTLA4, CTNNB1, DAP, DAPK1, TYMP, S1PR3, EPHA2, FOS, EIF4E, CDKN2B, CDK5, FASN, CDH1, FCN2, FGF2, FOXM1, CD40, SCARB1, LGALS9, SLC6A8, RBM3, RELA, REST, SATB1, BSG, ALB, CCL18, SFRP1, SLPI, CCK, BMP2, BCL2, STAR, STAT3, SYT1, TRBV20OR9-2, TERT, TGFBR1, PLAAT4, PVALB, PTPN12, PTPN6, CAV1, MGMT, MLH1, MMP1, MNAT1, MYC, NBN, CASP8, OSM, OTC, PAK1, ABCB1, PIK3CA, POU5F1, CALR, CALCR, PTK2, CCL5