-
Toxic Encephalopathy
Wikipedia
PMID 10210698 External links [ edit ] NINDS Encephalopathy Information Page Encephalopathy Causes, Symptoms, Diagnosis and Treatment by MedicineNet v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis
-
Selenium Deficiency
Wikipedia
ISBN 978-0-911910-50-6 . [ page needed ] External links [ edit ] Classification D ICD - 10 : E59 ICD - 9-CM : 269.3 DiseasesDB : 11941 v t e Malnutrition Protein-energy malnutrition Kwashiorkor Marasmus Catabolysis Vitamin deficiency B vitamins B 1 Beriberi Wernicke–Korsakoff syndrome Wernicke's encephalopathy Korsakoff's syndrome B 2 Riboflavin deficiency B 3 Pellagra B 6 Pyridoxine deficiency B 7 Biotin deficiency B 9 Folate deficiency B 12 Vitamin B 12 deficiency Other A: Vitamin A deficiency Bitot's spots C: Scurvy D: Vitamin D deficiency Rickets Osteomalacia Harrison's groove E: Vitamin E deficiency K: Vitamin K deficiency Mineral deficiency Sodium Potassium Magnesium Calcium Iron Zinc Manganese Copper Iodine Chromium Molybdenum Selenium Keshan disease Growth Delayed milestone Failure to thrive Short stature Idiopathic General Anorexia Weight loss Cachexia UnderweightALB, SELENOP, BCL2, SELENOH, NOS3, DRD4, CXCL8, SELENOT, GPX1, SLC6A4, TXN, STAT3, TLR2, TNF, TNFRSF1B, VTA1, TXNRD1, GPR132, SECISBP2, OSR1, SELENOV, MIR128-1, MIR155, MIR33A, SOD1, PTGS2, SELENOW, MAPK8, BGN, CASP3, CASP9, COMT, DCN, ACE, MEGF8, FKBP4, GPX3, GPX4, ICAM1, IL1A, IL1B, IL6, PDCD1, LOC110806262
-
Encopresis
Wikipedia
External links [ edit ] Classification D ICD - 10 : R15 F98.1 ICD - 9-CM : 307.7 , 787.6 MeSH : D004688 DiseasesDB : 4221 External resources MedlinePlus : 001570 eMedicine : ped/670 v t e Symptoms and signs relating to the human digestive system or abdomen Gastrointestinal tract Nausea Vomiting Heartburn Aerophagia Pagophagia Dysphagia oropharyngeal esophageal Odynophagia Bad breath Xerostomia Hypersalivation Burping Wet burp Goodsall's rule Chilaiditi syndrome Dance's sign Aaron's sign Arapov's sign Markle sign McBurney's point Sherren's triangle Radiologic signs : Hampton's line Klemm's sign Accessory liver : Councilman body Mallory body biliary: Boas' sign Courvoisier's law Charcot's cholangitis triad / Reynolds' pentad cholecystitis ( Murphy's sign Lépine's sign Mirizzi's syndrome ) Nardi test Defecation Flatulence Fecal incontinence Encopresis Fecal occult blood Rectal tenesmus Constipation Obstructed defecation Diarrhea Rectal discharge Psoas sign Obturator sign Rovsing's sign Hamburger sign Heel tap sign Aure-Rozanova's sign Dunphy sign Alder's sign Lockwood's sign Rosenstein's sign Abdomen Pain Abdominal pain Acute abdomen Colic Baby colic Abdominal guarding Blumberg sign Distension Abdominal distension Bloating Ascites Tympanites Shifting dullness Ascites Fluid wave test Masses Abdominal mass Hepatosplenomegaly Hepatomegaly Splenomegaly Other Jaundice Mallet-Guy sign Puddle sign Ballance's sign Aortic insufficiency Castell's sign Kehr's sign Cullen's sign Grey Turner's sign Hernia Howship–Romberg sign Hannington-Kiff sign Other Cupola sign Fothergill's sign Carnett's sign Sister Mary Joseph nodule
-
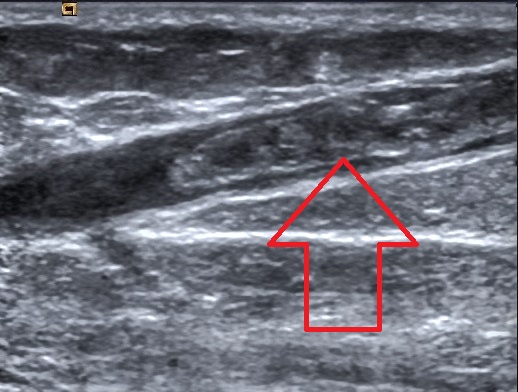
Superficial Vein Thrombosis
Wikipedia
Fixed compression bandages, adhesive short stretch bandages, and graduated elastic compression stockings have all be used in the treatment of SVTs. [1] The benefit of compression stockings is unclear, though they are frequently used. [3] Physical activity [ edit ] Inactivity is contraindicated in the aftermath of an SVT. [1] Uninterrupted periods of sitting or standing may cause the SVT to elongate from its point of origin, increasing the risk for complications and clinical worsening. [1] Medications [ edit ] Medications used for the treatment of SVT include anticoagulants , NSAIDs (except aspirin ), antibiotics , and corticosteroids . [1] Anticoagulants [ edit ] SVTs that occur within the great saphenous vein within 3 cm of the saphenofemoral junction are considered to be equivalent in risk to DVTs. [3] These high risk SVTs are treated identically with therapeutic anticoagulation. [3] Anticoagulation is also used for intermediate risk SVTs that are greater than 3 cm from the saphenofemoral junction or are greater than 4–5 cm in length. [3] Anticoagulation for high risk SVTs includes the use of vitamin K antagonists or novel oral anticoagulants (NOACs) for 3 months. [3] Anticoagulation for intermediate risk SVTs includes fondaparinux 2.5 mg daily for 45 days or the use of intermediate to therapeutic dose low molecular weight heparin for 4–6 weeks. [3] NSAIDs [ edit ] NSAIDs (non-steroidal anti-inflammatory drugs) can be used in both oral or topical formulations for the relief of SVT symptoms. [3] The British Committee for Standards in Haematology guidelines recommend the use of NSAIDs for low-risk SVTs (thrombus <4–5 cm in length, no additional risk factors for thromboembolic events). [3] NSAIDs are used for treatment durations of 8–12 days. [3] Other [ edit ] Antibiotics are used in the treatment of septic SVT . [1] Corticosteroids are used for the treatment of SVTs in the setting of vasculitic and autoimmune syndromes. [1] Surgery [ edit ] Surgical interventions are used for both symptomatic relief of the SVT as well as for preventing the development of more serious complications (e.g. pulmonary embolism). [3] Surgical interventions include ligation of the saphenofemoral junction, ligation and stripping of the affected veins, and local thrombectomy . [3] Because of the risk of symptomatic pulmonary embolism with surgery itself, surgical interventions are not recommended for the treatment of lower limb SVTs by the 2012 American College of Chest Physicians guidelines and the 2012 British Committee for Standards in Haematology guidelines. [3] The use of surgery for the treatment of SVT is controversial. [6] Prognosis [ edit ] SVT is often a mild, self-resolving medical condition. [1] The inflammatory reaction may last up to 2–3 weeks, with possible recanalization of the thrombosed vein occurring in 6–8 weeks. [1] The superficial vein may continue to be hyperpigmented for several months following the initial event. [1] Epidemiology [ edit ] In a French population, SVT occurred in 0.64 per 1000 persons per year. [3] History [ edit ] SVTs have been historically considered to be benign diseases, for which treatment was limited to conservative measures. [6] However, an increased awareness of the potential risks of SVTs developing into more serious complications has prompted more research into the diagnosis, classification, and treatment of SVTs. [6] Research [ edit ] A Cochrane review recommends that future research investigate the utility of oral, topical, and surgical treatments for preventing the progression of SVTs and the development of thromboembolic complications. [7] [8] Footnotes [ edit ] ^ Migratory thrombophlebitis (recurrent SVT) and cancer are the hallmarks of Trousseau syndrome . [2] References [ edit ] ^ a b c d e f g h i j k l m n o p q r s t u v Kalodiki, E; Stvrtinova, V; Allegra, C; Andreozzi, GM; Antignani, P-L; Avram, R; Brkljacic, B; Cadariou, F; Dzsinich, C; Fareed, J; Gaspar, L; Geroulakos, G; Jawien, A; Kozak, M; Lattimer, CR; Minar, E; Partsch, H; Passariello, F; Patel, M; Pecsvarady, Z; Poredos, P; Roztocil, K; Scuderi, A; Sparovec, M; Szostek, M; Skorski, M (2012).
-
Acute Limb Ischaemia
Wikipedia
Most cases involve people with atherosclerosis problems. [7] Symptoms of acute limb ischaemia include: Pain Pallor (pale appearance of the limb) Paresthesias (abnormal sensations in the limb) Perishingly cold Pulselessness Paralysis These symptoms are called "the six P's'"; [8] [9] [10] they are commonly mis-attributed to compartment syndrome. One more symptom would be the development of gangrene. ... Early detection and steps towards fixing the problem with limb-sparing techniques can salvage the limb. Compartment syndrome can occur because of acute limb ischaemia because of the biotoxins that accumulate distal to the occlusion resulting in edema . [1] Treatment [ edit ] Surgery [ edit ] The primary intervention in acute limb ischaemia is emergency embolectomy using a Fogarty Catheter , providing the limb is still viable within the 4-6h timeframe. [11] Other options include a vascular bypass to route blood flow around the clot. [12] Angiograph before and after thrombolytic treatment of acute limb ischemia.
-
Rheumatoid Lung Disease
Wikipedia
From most to lest common: Pleural involvement ( pleurisy , effusions) Pulmonary parenchymal nodules , more common in men than in women [3] Rheumatoid-associated interstitial lung disease Bronchiolitis obliterans organizing pneumonia Obliterative bronchiolitis (obstructive lung disease/bronchiectasis) Rheumatoid-associated pulmonary hypertension Pulmonary vasculitis /arteritis Shrinking lung syndrome Miscellaneous: MTX, cricoarytenoid arthritis , infection , cancer Causes [ edit ] The exact cause of rheumatoid lung disease is unknown. ... Bronchoscopic, video-assisted, or open lung biopsy allows the histological characterization of pulmonary lesions, which can distinguish rheumatoid lung disease from other interstitial lung diseases. [6] The following tests may also show signs of rheumatoid lung disease: [7] Chest x-ray may show: pleural effusion lower zone predominant reticular or reticulonodular pattern volume loss in advanced disease skeletal changes, e.g. erosion of clavicles, glenohumeral erosive arthropathy, superior rib notching Chest CT or HRCT features include: pleural thickening or effusion interstitial fibrosis bronchiectasis bronchiolitis obliterans large rheumatoid nodules single or multiple tend to be based peripherally may cavitate (necrobiotic lung nodules) cavitation of a peripheral nodule can lead to pneumothorax or haemopneumothorax. follicular bronchiolitis small centrilobular nodules or tree-in-bud rare Caplan syndrome Echocardiogram (may show pulmonary hypertension ) Lung biopsy (bronchoscopic, video-assisted, or open), which may show pulmonary lesions Lung function tests Needle inserted into the fluid around the lung ( thoracentesis ) Blood tests for rheumatoid arthritis Treatment [ edit ] Many people with this condition have no symptoms.
-
Methanol Toxicity
Wikipedia
Methanol toxicity Other names Methanol poisoning Molecular structure of methanol Specialty Emergency medicine Symptoms Decreased level of consciousness , poor coordination, vomiting , abdominal pain , specific smell on the breath [1] [2] Complications Blindness , kidney failure [1] Causes Methanol (such as found in windshield washer fluid ) [1] [2] Diagnostic method Blood acidosis , increased osmol gap , methanol blood level [1] [2] Differential diagnosis Infections , exposure to other toxic alcohols , serotonin syndrome , diabetic ketoacidosis [2] Treatment Antidote , hemodialysis [2] Medication Fomepizole , ethanol [2] Prognosis Good with early treatment [1] Frequency 1,700 cases per year (US) [3] Methanol toxicity is poisoning from methanol , characteristically via ingestion. [1] Symptoms may include a decreased level of consciousness , poor or no coordination, vomiting , abdominal pain , and a specific smell on the breath. [1] [2] Decreased vision may start as early as twelve hours after exposure. [2] Long-term outcomes may include blindness and kidney failure . [1] Toxicity and death may occur even after drinking a small amount. [1] Methanol poisoning most commonly occurs following the drinking of windshield washer fluid . [2] This may be accidental or as part of an attempted suicide . [1] Toxicity may also rarely occur through extensive skin exposure or breathing in fumes. [1] When methanol is broken down by the body it results in formaldehyde , formic acid , and formate which cause much of the toxicity. [2] The diagnosis may be suspected when there is acidosis or an increased osmol gap and confirmed by directly measuring blood levels. [1] [2] Other conditions that can produce similar symptoms include infections , exposure to other toxic alcohols , serotonin syndrome , and diabetic ketoacidosis . [2] Early treatment increases the chance of a good outcome. [2] Treatment consists of stabilizing the person, followed by the use of an antidote . [2] The preferred antidote is fomepizole , with ethanol used if this is not available. [2] Hemodialysis may also be used in those where there is organ damage or a high degree of acidosis . [2] Other treatments may include sodium bicarbonate , folate , and thiamine . [2] Outbreaks of methanol ingestion have occurred due to contamination of drinking alcohol . [2] This is more common in the developing world . [2] In 2013 more than 1700 cases occurred in the United States. [3] Those affected are usually adult and male. [3] Toxicity to methanol has been described as early as 1856. [4] Contents 1 Signs and symptoms 2 Cause 3 Mechanism 4 Treatment 5 History 6 See also 7 References 8 External links Signs and symptoms [ edit ] The initial symptoms of methanol intoxication include central nervous system depression , headache, dizziness, nausea, lack of coordination, and confusion.
-
Osteomyelitis Of The Jaws
Wikipedia
Headache or facial pain, as in the descriptive former term "neuralgia-inducing" (cavitational osteonecrosis). Fibromyalgia . Chronic fatigue syndrome . Swelling. External swelling is initially due to inflammatory edema with accompanying erythema (redness), heat and tenderness, and then later may be due to sub-periosteal pus accumulation. ... Specific examples include familial hypercoagulation, diabetes , autoimmune diseases , Agranulocytosis , leukemia , severe anemia , syphilis , chemotherapy , corticosteroid therapy, sickle cell disease , acquired immunodeficiency syndrome , old age, malnutrition , smoking and alcohol consumption, radiotherapy , osteoporosis , Paget's disease of bone , fibrous dysplasia , bone malignancy and causes of bone necrosis such as Bismuth , Mercury or arsenic .
-
Cerebrospinal Fluid Leak
Wikipedia
Spontaneous CSF leaks are associated with heritable connective tissue disorders including Marfan syndrome and Ehlers–Danlos syndromes . [7] Contents 1 Signs and symptoms 2 Causes 3 Diagnosis 4 Treatment 5 References 6 External links Signs and symptoms [ edit ] The most common symptom of a CSF leak is a fast-onset, extremely painful orthostatic headache or thunderclap headache . [8] A spinal leak may cause spontaneous intracranial hypotension (low CSF pressure) because the body cannot replenish the CSF fast enough to keep pace with the leak.
-
Acute Infectious Thyroiditis
Wikipedia
External links [ edit ] Classification D ICD - 10 : E06.0 ICD - 9-CM : 245.0 MeSH : D013969 DiseasesDB : 34307 v t e Thyroid disease Hypothyroidism Iodine deficiency Cretinism Congenital hypothyroidism Myxedema Myxedema coma Euthyroid sick syndrome Signs and symptoms Queen Anne's sign Woltman sign Thyroid dyshormonogenesis Pickardt syndrome Hyperthyroidism Hyperthyroxinemia Thyroid hormone resistance Familial dysalbuminemic hyperthyroxinemia Hashitoxicosis Thyrotoxicosis factitia Thyroid storm Graves' disease Signs and symptoms Abadie's sign of exophthalmic goiter Boston's sign Dalrymple's sign Stellwag's sign lid lag Griffith's sign Möbius sign Pretibial myxedema Graves' ophthalmopathy Thyroiditis Acute infectious Subacute De Quervain's Subacute lymphocytic Palpation Autoimmune /chronic Hashimoto's Postpartum Riedel's Enlargement Goitre Endemic goitre Toxic nodular goitre Toxic multinodular goiter Thyroid nodule Colloid nodule
-
Muscular Dystrophy, Limb-Girdle, Autosomal Recessive 18
Omim
The patients presented at birth or in early infancy with alacrima, and 3 had onset later in infancy of achalasia, features reminiscent of the triple A syndrome (AAAS; 231550), although none had adrenal insufficiency. ... Koehler et al. (2017) noted that alacrima and achalasia are thought to be due to neural degeneration, but concluded that the phenotype in these patients was consistent with expansion of LGMD2S myopathy rather than a new form of AAA syndrome. Fee et al. (2017) reported a brother and sister, born of unrelated parents, with LGMD2S.
-
Myositis Ossificans
Wikipedia
Myositis ossificans progressiva Fibrodysplasia ossificans progressiva Specialty Rheumatology Myositis ossificans comprises two syndromes characterized by heterotopic ossification (calcification) of muscle. ... PMID 11341414 . [ permanent dead link ] External links [ edit ] Radiograph showing myositis ossificans Classification D ICD - 10 : M61.1 OMIM : 135100 MeSH : D009221 External resources Orphanet : 337 v t e Symptoms and conditions relating to muscle Pain Myalgia Fibromyalgia Acute Delayed onset Inflammation Myositis Pyomyositis Destruction Muscle weakness Rhabdomyolysis Muscle atrophy / Amyotrophy Other Myositis ossificans Fibrodysplasia ossificans progressiva Compartment syndrome Anterior Diastasis of muscle Diastasis recti Muscle spasm
-
Steatosis
Wikipedia
Common causes are tetracyclines , acute fatty liver of pregnancy, Reye's syndrome , and hepatitis C . Histology [ edit ] Histologically , steatosis is physically apparent as lipid within membrane bound liposomes of parenchymal cells. [2] When this tissue is fixed and stained to be better viewed under a microscope, the lipid is usually dissolved by the solvents used to prepare the sample. ... PMID 17242448 . ^ Ahmed MH, Byrne CD (September 2010). "Obstructive sleep apnea syndrome and fatty liver: association or causal link?"
-
Meesmann Corneal Dystrophy
Wikipedia
Meesmann Corneal Dystrophy Other names Meesmann Epithelial Corneal Dystrophy Meesmann-Wilke Syndrome Multiple opaque spots in the corneal epithelium Specialty Ophthalmology Symptoms Anterior corneal intraepithelial microcysts, Corneal erosions, Photophobia, Lacrimation, Intermittent visual, acuity loss (rarely seriously impaired), Nonprogressive corneal dystrophy, Fine punctate corneal opacities, Episodic foreign body sensation, Increased tear production, eye stinging, Blepharospasm Usual onset Infancy or Young Childhood Duration Lifelong Types Meesmann corneal dystrophy 1, Meesmann corneal dystrophy 2 Diagnostic method Slit Lamp Biomicroscopy Treatment Eye drops, Corneal Surgery Meesmann corneal dystrophy (MECD) is a rare hereditary autosomal dominant disease that is characterized as a type of corneal dystrophy and a keratin disease . ... A heterozygous mutation in either of these genes will lead to a single phenotype. [1] [2] Many with Meesmann corneal dystrophy are asymptomatic or experience mild symptoms. [3] Autosomal Dominant Inheritance Pattern It is named after the German ophthalmologist Alois Meesmann (1888-1969). [4] [5] It is often considered as the "Meesmann-Wilke syndrome", after the joint contribution of Meesmann and Wilke in 1939. [4] [6] Research was later contributed by Stocker and Holt in 1954 through 1955 who found a variant of Meesmann corneal dystrophy called "Stocker-Holt Dystrophy". [3] Contents 1 Clinical Features and Symptoms 2 Diagnosis 3 Treatment 4 Genetics 5 See also 6 References 7 External links Clinical Features and Symptoms [ edit ] Anterior corneal intraepithelial microcysts Corneal erosions Photophobia Lacrimation Intermittent visual acuity loss (rarely seriously impaired) Nonprogressive corneal dystrophy Fine punctate corneal opacities Episodic foreign body sensation Increased tear production Eye stinging Blepharospasm Meesmann corneal dystrophy is a non-inflammatory condition that effects the restricted region of the cornea epithelium which is the outermost layer. [2] Onset of symptoms begin during infancy or early childhood but may not become noticeable or problematic for many years. [3] [7] [8] Diagnosis [ edit ] Patients with Meesmann corneal dystrophy may remain asymptomatic or experience mild symptoms.
-
Generalized Arterial Calcification Of Infancy
Gene_reviews
Differential Diagnosis Disorders with Vascular Calcification Singleton-Merten syndrome (OMIM 182250 and 616298) is an autosomal dominant disorder caused by pathogenic variants in IFIH1 or DDX58. ... Unlike generalized arterial calcification of infancy (GACI), aortic calcification in Singleton-Merten syndrome starts later in life (age range at diagnosis: 6-39 years). ... Compared with GACI, metastatic calcification exhibits a different distribution of extravascular calcification, and the microscopic vascular changes occur in the media with little intimal proliferation. Twin-twin transfusion syndrome (TTTS) and twin reversed arterial perfusion (TRAP) sequence Increased echogenicity due to calcification has been described in the wall of the pulmonary trunk, proximal branch pulmonary arteries [Saxena & Soni 2003, Bassil Eter et al 2009], and ascending aorta in the recipient twin of TTTS [Saxena & Soni 2003]. ... In fact, a child with a clinical diagnosis of pediatric FMD was eventually found to have ENPP1 deficiency [Ferreira et al 2020]; thus, other individuals with pediatric FMD could benefit from molecular genetic testing of ENPP1 . Grange syndrome (OMIM 602531) is an autosomal recessive disorder caused by pathogenic variants in YY1AP1 . This extremely rare syndrome is characterized by diffuse vascular stenoses with intimal thickening [Weymann et al 2001] in a distribution pattern resembling fibromuscular dysplasia, brachysyndactyly, and osteopenia with increased bone fragility [Grange et al 1998, Volonghi et al 2012].
-
Foxp2-Related Speech And Language Disorders
Gene_reviews
Methylation testing for maternal uniparental disomy (UPD) of chromosome 7 should be considered in individuals with verbal dyspraxia and features suggestive of Silver-Russell syndrome, since UPD accounted for about 12% of cases in one study [Feuk et al 2006]. ... Disorders to Consider in the Differential Diagnosis of FOXP2 -Related Speech and Language Disorders View in own window Disease Name Gene or Critical Region MOI CAS Clinical Features of the Differential Diagnosis Disorder Overlapping (in addition to CAS) Distinguishing 16p11.2 microdeletion AUTS14 AD 1, 2 + ID, ASD, DD Expressive language skills more severely impaired than receptive language Epilepsy or recurrent seizures Dysmorphic features (e.g., low-set ears, partial syndactyly) 7q11.23 duplication syndrome WBSCR AD + 3 DD Appropriate nonverbal pragmatic abilities in socially comfortable situations Oral apraxia Phonologic disorder Expressive language disorder Hypotonia Dysmorphic features (brachycephaly, broad forehead, straight eyebrows, broad nasal tip, low insertion of the columella, short philtrum, thin upper lip, minor ear anomalies, facial asymmetry) Social anxiety Developmental coordination disorder In some: Macrocephaly Visually detectable MRI abnormalities (e.g., vermis hypoplastic, ventriculomegaly, vermis hypoplasia) Signs of cerebellar dysfunction KANSL1 -related intellectual disability syndrome KANSL1 AD 1 + Early oral motor & feeding difficulties DD Oral dyspraxia Expressive language abilities better than receptive language Literacy problems ID Hypotonia Dysmorphic features (elongated face, bulbous nasal tip) Seizures Visual &/or hearing deficits Heart problems GRIN2A -related disorders 4 OMIM GRIN2A AD ± Oral dyspraxia Dysarthria Aphasia Epilepsy Worster-Drought syndrome 5 OMIM AD – Cerebral palsy 6 Oral dyspraxia Dysarthria Mild fine & gross movement difficulties Epilepsy Moderate learning difficulties Club feet Restricted joint movement Floating-Harbor syndrome 7 SRCAP AD 1 + 7 Dysarthria Hypernasality Severe expressive & receptive language & literacy impairment Short stature Delayed bone age Characteristic facies Aggression in childhood Galactosemia 8 GALT AR + 9 Expressive/receptive language impairment Typical or borderline-low IQ to more severe IQ depending on type of galactosemia 10 Dysarthria Movement coordination disorder, primarily affecting balance & manual dexterity Voice dysfunction Liver function issues AD = autosomal dominant; AR = autosomal recessive; ASD = autism spectrum disorder; CAS = childhood apraxia of speech; DD = developmental delay; ID = intellectual disability; MOI = mode of inheritance 1. ... Velleman & Mervis [2011] 4. Landau Kleffner syndrome and epilepsy-aphasia syndromes 5.
-
Charcot-Marie-Tooth Disease, Demyelinating, Type 1a
Omim
Since both of these disorders map to the pericentric region of chromosome 17, they investigated whether this might be a contiguous gene syndrome. In both patients, however, the CMT1A was inherited from the father, who did not have NF1. ... In addition, all 11 individuals had sleep apnea syndrome with a mean apnea-hypopnea index of 46.6 per hour (28.5) of sleep (normal value less than 15 per hour). The remaining 3 family members were free from neuropathy and sleep apnea syndrome. Sleep apnea and neuropathy severity were highly correlated; the compound muscle action potential amplitude of the median nerve was inversely correlated with the apnea-hypopnea index. ... Dematteis et al. (2001) concluded that sleep apnea syndrome is related to a pharyngeal neuropathy. ... Manifestations of both the duplication and the monosomy were present; however, the overall development was better than that previously reported in either syndrome. The patient's motor development was significantly more impaired than cognitive development, and signs of a peripheral neuropathy were found and attributed to duplication of 17p.
-
Frontotemporal Dementia And/or Amyotrophic Lateral Sclerosis 1
Omim
One patient had apraxia and parkinsonism, consistent with a corticobasal syndrome. Age at onset ranged from 35 to 57 years, with a mean of 45.7, and the mean disease duration was 5.4 years. ... Ten patients had a diagnosis of FTD or FTD-ALS, 1 had ALS, and 3 had atypical diagnoses, including olivopontocerebellar degeneration, corticobasal syndrome, and atypical Parkinson syndrome with FTD-ALS. ... These patients were classified as having an 'HD phenocopy' syndrome. Of these 10 patients, 70% had a positive family history for a neurodegenerative disease. ... Hensman Moss et al. (2014) concluded that a C9ORF72 repeat expansion is the most common genetic cause of HD phenocopy syndrome in European populations, and that screening for this expansion should be included in an algorithm for the workup of HD.
-
Igg4-Related Disease
Wikipedia
Branches of the aorta (including coronary , [35] renal or iliac arteries) IgG4-related periarteritis [42] Pericardium IgG4-related pericarditis Mediastinum IgG4-related mediastinitis Fibrosing mediastinitis , chronic sclerosing mediastinitis Retroperitoneum IgG4-related retroperitoneal fibrosis Retroperitoneal fibrosis , Albarran -Ormond syndrome, Ormond 's disease, perirenal fasciitis, Gerota 's fasciitis/syndrome, periureteritis fibrosa, sclerosing lipogranuloma, sclerosing retroperitoneal granuloma, non-specific retroperitoneal inflammation, sclerosing retroperitonitis, retroperitoneal vasculitis with perivascular fibrosis. [43] Mesentery IgG4-related mesenteritis (subtypes are: mesenteric panniculitis , mesenteric lipodystrophy and retractile mesenteritis) [43] Sclerosing mesenteritis , systemic nodular panniculitis, liposclerosis mesenteritis, mesenteric Weber–Christian disease , mesenteric lipogranuloma, xanthogranulomatous mesenteritis. [43] Breast IgG4-related mastitis Sclerosing mastitis Genitourinary Kidney IgG4-related kidney disease (IgG4-RKD) : IgG4-related tubulointerstitial nephritis (IgG4-TIN), membranous glomerulonephritis secondary to IgG4-related disease, IgG4-related renal pyelitis ( renal pelvis ) Idiopathic tubulointerstitial nephritis Prostate IgG4-related prostatitis Vas deferens IgG4-related perivasal fibrosis [30] [44] Chronic orchialgia Scrotum IgG4-related paratesticular pseudotumor, [33] [45] IgG4-related epididymo-orchitis [33] Paratesticular fibrous pseudotumor, inflammatory pseudotumor of the spermatic cord , pseudosarcomatous myofibroblastic proliferations of the spermatic cord, proliferative funiculitis, chronic proliferative periorchitis, fibromatous periorchitis, nodular periorchitis, reactive periorchitis, fibrous mesothelioma [46] Other Lymph nodes IgG4-related lymphadenopathy Skin IgG4-related skin disease Angiolymphoid hyperplasia with eosinophilia , [47] cutaneous pseudolymphoma [48] Nerve IgG4-related perineural disease [33] [49] This is not a complete list, as IgG4-RD can involve any site in the body. ... A 2011 study estimated the incidence of IgG4-RD in Japan at 2.8–10.8/million population, with a median age of onset of 58 years. [66] Nomenclature [ edit ] Names previously used for IgG4-RD: IgG4-related systemic disease (IgG4-RSD) IgG4-related sclerosing disease IgG4-related systemic sclerosing disease IgG4-related autoimmune disease IgG4-associated multifocal systemic fibrosis IgG4-associated disease IgG4 syndrome Hyper-IgG4 disease Systemic IgG4-related plasmacytic syndrome IgG4-positive multiorgan lymphoproliferative syndrome Prior to 2011, IgG4-RD used to get mentioned in the medical literature under various different names. [2] [66] At the 2011 International Symposium on IgG4-Related Diseases , the consensus name of IgG4-related disease was endorsed for the condition. [2] This name had already been agreed upon as a consensus name among Japanese investigators, [2] [3] notably choosing not to use the term ' systemic ' as that might lead to malignant tumours in other organs getting incorrectly diagnosed as being just another manifestation of the IgG4-related condition. [66] However, some experts at the international symposium did express reservations about naming the disease after IgG4 , as its role in pathogenesis is questionable and the use of serum IgG4 concentrations as a biomarker is unreliable. [2] An expanded term, 'Immunoglobulin G4-related disease', has sometimes been used also. [67] However, this term was never referenced in the 2012 recommendations for nomenclature, [2] and its use would appear to be erroneous. ... "IgG4-related disease of the paratestis in a patient with Wells syndrome: a case report" . Diagnostic Pathology . 9 : 225. doi : 10.1186/s13000-014-0225-5 .
-
Long-Term Effects Of Alcohol
Wikipedia
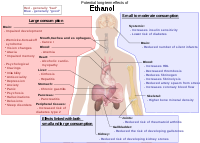
The elderly are the most sensitive to the toxic effects of alcohol on the brain. [100] There is some inconclusive evidence that small amounts of alcohol taken in earlier adult life is protective in later life against cognitive decline and dementia. [101] However, a study concluded, "Our findings suggest that, despite previous suggestions, moderate alcohol consumption does not protect older people from cognitive decline." [102] Wernicke–Korsakoff syndrome is a manifestation of thiamine deficiency, usually as a secondary effect of alcohol abuse. [103] The syndrome is a combined manifestation of two eponymous disorders, Korsakoff's Psychosis and Wernicke's encephalopathy . ... It was noted that every individual has an individual sensitivity level to alcohol or sedative hypnotic drugs and what one person can tolerate without ill health another will suffer very ill health and that even moderate drinking can cause rebound anxiety syndromes and sleep disorders. A person who is suffering the toxic effects of alcohol will not benefit from other therapies or medications as they do not address the root cause of the symptoms. [128] Addiction to alcohol, as with any drug of abuse tested so far, has been correlated with an enduring reduction in the expression of GLT1 ( EAAT2 ) in the nucleus accumbens and is implicated in the drug-seeking behavior expressed nearly universally across all documented addiction syndromes. ... Alcohol use increases the risk of chronic gastritis (stomach inflammation); [1] [132] it is one cause of cirrhosis , hepatitis , and pancreatitis in both its chronic and acute forms. Metabolic syndrome [ edit ] A national survey (NHANES) conducted in the U.S. concluded, "Mild to moderate alcohol consumption is associated with a lower prevalence of the metabolic syndrome , with a favorable influence on lipids, waist circumference, and fasting insulin. This association was strongest among whites and among beer and wine drinkers." [133] Similarly, a national survey conducted in Korea reported a J-curve association between alcohol intake and metabolic syndrome: "The results of the present study suggest that the metabolic syndrome is negatively associated with light alcohol consumption (1–15 g alcohol/d) in Korean adults," but risk increased at higher alcohol consumption. [134] Gallbladder effects [ edit ] Research has found that drinking reduces the risk of developing gallstones . ... This Cr-PdG adduct "is likely to play a central role in the mechanism of alcoholic beverage related carcinogenesis." [195] Alcohol's effect on the fetus [ edit ] Main article: fetal alcohol spectrum disorder Fetal alcohol syndrome or FAS is a birth defect that occurs in the offspring of women who drink alcohol during pregnancy.