-
Mushroom Poisoning
Wikipedia
Muscarine Potentially deadly Causes SLUDGE syndrome . Found in various mushrooms. Antidote is atropine Monomethylhydrazine (MMH) Deadly Causes brain damage, seizures, gastrointestinal upset, and hemolysis . ... ISBN 978-0-89815-169-5 . ^ Benjamin DR. "Amatoxin syndrome": 198–214. Cite journal requires |journal= ( help ) in: Mushrooms: poisons and panaceas – a handbook for naturalists, mycologists and physicians . ... S2CID 2175833 . ^ Disulfiramlike Mushroom Toxicity at eMedicine ^ "Mushroom Poisoning Syndromes" . NAMA. 2003. Archived from the original on 2008-03-29 . ... External links [ edit ] Classification D ICD - 10 : T62.0 ICD - 9-CM : 988.1 MeSH : D009145 Poisonous American Mushrooms – AmericanMushrooms.com Poisonous mushrooms: microscopic identification in cooked specimens from medical mycologist R.C. Summerbell Mushroom Poisoning Syndromes from the North American Mycological Association Mushroom Poisoning Case Registry (North America) from the North American Mycological Association American Association of Poison Control Centers Provides information on toxicity of mushroom's in your area, symptoms and first aid. ... Fungi . 3 (3): 36–44. v t e Poisoning Toxicity Overdose History of poison Inorganic Metals Toxic metals Beryllium Cadmium Lead Mercury Nickel Silver Thallium Tin Dietary minerals Chromium Cobalt Copper Iron Manganese Zinc Metalloids Arsenic Nonmetals Sulfuric acid Selenium Chlorine Fluoride Organic Phosphorus Pesticides Aluminium phosphide Organophosphates Nitrogen Cyanide Nicotine Nitrogen dioxide poisoning CHO alcohol Ethanol Ethylene glycol Methanol Carbon monoxide Oxygen Toluene Pharmaceutical Drug overdoses Nervous Anticholinesterase Aspirin Barbiturates Benzodiazepines Cocaine Lithium Opioids Paracetamol Tricyclic antidepressants Cardiovascular Digoxin Dipyridamole Vitamin poisoning Vitamin A Vitamin D Vitamin E Megavitamin-B 6 syndrome Biological 1 Fish / seafood Ciguatera Haff disease Ichthyoallyeinotoxism Scombroid Shellfish poisoning Amnesic Diarrhetic Neurotoxic Paralytic Other vertebrates amphibian venom Batrachotoxin Bombesin Bufotenin Physalaemin birds / quail Coturnism snake venom Alpha-Bungarotoxin Ancrod Batroxobin Arthropods Arthropod bites and stings bee sting / bee venom Apamin Melittin scorpion venom Charybdotoxin spider venom Latrotoxin / Latrodectism Loxoscelism tick paralysis Plants / fungi Cinchonism Ergotism Lathyrism Locoism Mushrooms Strychnine 1 including venoms , toxins , foodborne illnesses .
-
Anorexia Nervosa
Wikipedia
It has been documented that some people with celiac disease, irritable bowel syndrome or inflammatory bowel disease who are not conscious about the importance of strictly following their diet, choose to consume their trigger foods to promote weight loss. ... Can be useful in detecting various disorders such as diabetes , an insulinoma , Cushing's Syndrome , hypoglycemia and polycystic ovary syndrome . [103] Serum cholinesterase test: a test of liver enzymes ( acetylcholinesterase and pseudocholinesterase ) useful as a test of liver function and to assess the effects of malnutrition. [104] Liver Function Test : A series of tests used to assess liver function some of the tests are also used in the assessment of malnutrition, protein deficiency , kidney function, bleeding disorders, and Crohn's Disease. [105] Luteinizing hormone (LH) response to gonadotropin-releasing hormone (GnRH): Tests the pituitary glands' response to GnRh, a hormone produced in the hypothalamus. ... Diagnosis can be challenging, risk assessment may not be performed accurately, consent and the need for compulsion may not be assessed appropriately, refeeding syndrome may be missed or poorly treated and the behavioural and family problems in AN may be missed or poorly managed. [132] The MARSIPAN guidelines recommend that medical and psychiatric experts work together in managing severely ill people with AN. [133] Nutrition [ edit ] The rate of refeeding can be difficult to establish, because the fear of refeeding syndrome (RFS) can lead to underfeeding. ... The most common gastrointestinal complications of anorexia nervosa are delayed stomach emptying and constipation , but also include elevated liver function tests , diarrhea , acute pancreatitis , heartburn , difficulty swallowing , and, rarely, superior mesenteric artery syndrome . [145] Delayed stomach emptying, or gastroparesis, often develops following food restriction and weight loss; the most common symptom is bloating with gas and abdominal distension, and often occurs after eating.HTR2A, HTR4, EBF1, NCKIPSD, CADM1, SORCS2, CARMIL1, ASB3, LEP, FOXP1, MGMT, ERLEC1, TAFA2, SOX2-OT, BDNF, SLC6A4, COMT, AGRP, LEPR, OPN1SW, DRD4, DRD2, PYY, GHRL, ADIPOQ, RETN, ESR1, TNF, BEST1, DMD, OXTR, MC4R, SCLY, IFNG, CRH, TPH2, HTR1D, KRT7, TAL1, EPHX2, ESR2, CNR1, UCP3, IGF1, UCP2, POMC, OPRD1, NTRK2, HTR2C, SLC6A2, SLC6A3, CNTN4, MAOA, BED, FGF21, DPP4, MBOAT4, CD38, NUCB2, KCNN3, SMIM20, APOB, PTGS2, BMS1, HDAC4, DNTT, ACACA, SPX, NR3C1, GCG, ZDHHC2, GHSR, RBPJP4, CYP2B6, FTO, IL15, IL6, SPAG9, GRAP2, NR1H3, AIMP2, BAS, ADIPOR2, CARF, CLOCK, PARP9, AKAP6, CGB5, HTR3B, PANK2, ANGPTL6, CEP70, OLIG2, PPIG, GPR55, PDLIM7, ZW10, NT5C1B, MTCO2P12, OR2AG1, POSTN, NBEAL1, RSPO1, ANGPTL4, DLL1, YY1, ANGPTL3, CNTN6, NIPA1, ATP8A2, CNTN5, NPW, SYTL5, POLDIP2, GDF11, SS18L1, RNF19A, NTNG1, CSGALNACT1, TREX1, CGB8, WDHD1, SDS, C1QL1, AHSA1, NPB, PTH, WAS, DBI, ELK3, EPHB1, EPHB2, ETFA, FAAH, MSTN, GFER, GJA1, GPT, GRIA3, GRIN2B, HCRT, HSD11B2, HTC2, HTR3A, DRD3, CYP19A1, IL1B, CYP17A1, AMY1A, AMY1B, AMY1C, ARVCF, CCKAR, CCNE1, CDH9, CGA, CGB3, CPN1, CPN2, CRK, CRYGD, MAPK14, CTBP2, IGFBP1, IL18, VEGFA, PRL, TAS2R38, PTPN11, RAN, S100B, SCD, CX3CL1, SGSH, SHBG, SLC18A1, SNCA, STATH, TACR1, TNXB, UCN, VDR, PSMB6, MAPK1, INHBB, ABCB1, STMN1, LDLR, LTB, LYZ, MC3R, MCL1, MDK, MMP9, COX2, MUC1, NEFL, NNAT, NTRK3, PEPB, PGC, LOC110806262
-
Tooth Decay
Wikipedia
Pronunciation Caries / ˈ k ɛər iː z / Specialty Dentistry Symptoms Pain, tooth loss, difficulty eating [1] [2] Complications Inflammation around the tooth , tooth loss , infection or abscess formation [1] [3] Duration Long term Causes Bacteria producing acid from food debris [4] Risk factors Diet high in simple sugar, diabetes mellitus , Sjögren syndrome , medications that decrease saliva [4] Prevention Low- sugar diet, teeth brushing, fluoride , flossing [2] [5] Medication Paracetamol (acetaminophen), ibuprofen [6] Frequency 3.6 billion (2016) [7] Tooth decay , also known as dental caries or cavities , is the breakdown of teeth due to acids made by bacteria . [6] The cavities may be a number of different colors from yellow to black. [1] Symptoms may include pain and difficulty with eating. [1] [2] Complications may include inflammation of the tissue around the tooth , tooth loss , and infection or abscess formation. [1] [3] The cause of cavities is acid from bacteria dissolving the hard tissues of the teeth ( enamel , dentin and cementum ). [4] The acid is produced by the bacteria when they break down food debris or sugar on the tooth surface. [4] Simple sugars in food are these bacteria's primary energy source and thus a diet high in simple sugar is a risk factor. [4] If mineral breakdown is greater than build up from sources such as saliva , caries results. [4] Risk factors include conditions that result in less saliva such as: diabetes mellitus , Sjögren syndrome and some medications. [4] Medications that decrease saliva production include antihistamines and antidepressants. [4] Dental caries are also associated with poverty, poor cleaning of the mouth , and receding gums resulting in exposure of the roots of the teeth. [6] [8] Prevention of dental caries includes regular cleaning of the teeth, a diet low in sugar, and small amounts of fluoride . [2] [4] Brushing the teeth twice per day and flossing between the teeth once a day is recommended. [4] [6] Fluoride may be acquired from water , salt or toothpaste among other sources. [2] Treating a mother's dental caries may decrease the risk in her children by decreasing the numbers of certain bacteria she may spread to them. [4] Screening can result in earlier detection. [6] Depending on the extent of destruction, various treatments can be used to restore the tooth to proper function or the tooth may be removed . [6] There is no known method to grow back large amounts of tooth. [9] The availability of treatment is often poor in the developing world. [2] Paracetamol (acetaminophen) or ibuprofen may be taken for pain. [6] Worldwide, approximately 3.6 billion people (48% of the population) have dental caries in their permanent teeth as of 2016. [7] The World Health Organization estimates that nearly all adults have dental caries at some point in time. [2] In baby teeth it affects about 620 million people or 9% of the population. [10] They have become more common in both children and adults in recent years. [11] The disease is most common in the developed world due to greater simple sugar consumption and less common in the developing world . [6] Caries is Latin for "rottenness". [3] Contents 1 Signs and symptoms 2 Cause 2.1 Bacteria 2.2 Dietary sugars 2.3 Exposure 2.4 Teeth 2.5 Other factors 3 Pathophysiology 3.1 Enamel 3.2 Dentin 3.2.1 Sclerotic dentin 3.2.2 Tertiary dentin 3.3 Cementum 4 Diagnosis 4.1 Classification 4.2 Early childhood caries 4.3 Rate of progression 4.4 Affected hard tissue 5 Prevention 5.1 Oral hygiene 5.2 Dietary modification 5.3 Other measures 6 Treatment 7 Epidemiology 8 History 8.1 Etymology and usage 9 Society and culture 10 Other animals 11 References 11.1 Cited sources 12 External links Signs and symptoms [ edit ] (A) A small spot of decay visible on the surface of a tooth. ... As a result, medical conditions that reduce the amount of saliva produced by salivary glands , in particular the submandibular gland and parotid gland , are likely to lead to dry mouth and thus to widespread tooth decay. Examples include Sjögren syndrome , diabetes mellitus , diabetes insipidus , and sarcoidosis . [48] Medications, such as antihistamines and antidepressants, can also impair salivary flow.
-
Oxygen Toxicity
Wikipedia
Toxic effects of breathing in oxygen at high concentrations Oxygen toxicity Other names Oxygen toxicity syndrome, oxygen intoxication, oxygen poisoning In 1942–43 the UK Government carried out extensive testing for oxygen toxicity in divers. ... The earliest signs of pulmonary toxicity begin with evidence of tracheobronchitis, or inflammation of the upper airways, after an asymptomatic period between 4 and 22 hours at greater than 95% oxygen, [34] with some studies suggesting symptoms usually begin after approximately 14 hours at this level of oxygen. [35] At partial pressures of oxygen of 2 to 3 bar (200 to 300 kPa)—100% oxygen at 2 to 3 times atmospheric pressure—these symptoms may begin as early as 3 hours after exposure to oxygen. [34] Experiments on rats breathing oxygen at pressures between 1 and 3 bars (100 and 300 kPa) suggest that pulmonary manifestations of oxygen toxicity may not be the same for normobaric conditions as they are for hyperbaric conditions. [36] Evidence of decline in lung function as measured by pulmonary function testing can occur as quickly as 24 hours of continuous exposure to 100% oxygen, [35] with evidence of diffuse alveolar damage and the onset of acute respiratory distress syndrome usually occurring after 48 hours on 100% oxygen. [34] Breathing 100% oxygen also eventually leads to collapse of the alveoli ( atelectasis ), while—at the same partial pressure of oxygen—the presence of significant partial pressures of inert gases, typically nitrogen, will prevent this effect. [37] Preterm newborns are known to be at higher risk for bronchopulmonary dysplasia with extended exposure to high concentrations of oxygen. [38] Other groups at higher risk for oxygen toxicity are patients on mechanical ventilation with exposure to levels of oxygen greater than 50%, and patients exposed to chemicals that increase risk for oxygen toxicity such the chemotherapeutic agent bleomycin . [35] Therefore, current guidelines for patients on mechanical ventilation in intensive care recommends keeping oxygen concentration less than 60%. [34] Likewise, divers who undergo treatment of decompression sickness are at increased risk of oxygen toxicity as treatment entails exposure to long periods of oxygen breathing under hyperbaric conditions, in addition to any oxygen exposure during the dive. [31] Ocular toxicity [ edit ] See also: Retinopathy of prematurity Prolonged exposure to high inspired fractions of oxygen causes damage to the retina . [39] [40] [41] Damage to the developing eye of infants exposed to high oxygen fraction at normal pressure has a different mechanism and effect from the eye damage experienced by adult divers under hyperbaric conditions. [42] [43] Hyperoxia may be a contributing factor for the disorder called retrolental fibroplasia or retinopathy of prematurity (ROP) in infants. [42] [44] In preterm infants, the retina is often not fully vascularised. ... Navy has procedures for completing the decompression stops where a recompression chamber is not immediately available. [89] The occurrence of symptoms of bronchopulmonary dysplasia or acute respiratory distress syndrome is treated by lowering the fraction of oxygen administered, along with a reduction in the periods of exposure and an increase in the break periods where normal air is supplied.
-
Periodontal Disease
Wikipedia
Research has shown that smokers have more bone loss, attachment loss and tooth loss compared to non-smokers. [43] This is likely due to several effects of smoking on the immune response including decreased wound healing, suppression of antibody production, and the reduction of phagocytosis by neutrophils [43] Ehlers–Danlos syndrome and Papillon–Lefèvre syndrome (also known as palmoplantar keratoderma) are also risk factors for periodontitis. ... Several conditions and diseases, including Down syndrome , diabetes, and other diseases that affect one's resistance to infection, also increase susceptibility to periodontitis.CRP, MMP9, FPR1, GGT1, TNF, IL1B, IL10, CD14, MMP2, CCL2, MMP3, HMGB1, MMP13, NTRK1, AGER, VIP, NAMPT, ADRB1, MET, VCAM1, PPARA, LBP, CLDN1, POSTN, CXCL2, PLG, ELANE, GLT6D1, ITGB2, MFSD1, SIGLEC5, CTC1, NOTCH2, COL3A1, LYST, GFI1, USB1, OCRL, MMP8, TNFRSF11B, FGF3, CRACR2A, PARN, MPO, NOP10, MMP1, TENM2, NHP2, RTEL1, IL17A, ICAM1, DKC1, ADGRE1, NKAIN2, CXCL8, WRAP53, SLC35C1, FERMT1, IL1A, IFNG, GORAB, IL6, TINF2, TLR2, C1R, C1S, SRP54, TCIRG1, MCM3AP, TERC, TERT, BIRC5, PTGS2, TNFSF11, LINC02022, AP3B1, TLR4, PKN2-AS1, VDR, DEFB1, VEGFA, IL1RN, TLR9, CDKN2B-AS1, DEFB4B, SOST, TGFB1, DEFB4A, NLRP3, IL4, S100A8, F2RL1, PPARG, DEFB103A, DEFB103B, IL17F, IL13, BTF3P11, IL18, COX2, CASP3, PTX3, CSF1, MAPK1, TIMP3, ESR1, TNFRSF11A, CTLA4, MIR146A, CCR5, CAMP, HSPD1, CASP1, IL22, SERPINF2, FOXP3, HSPA14, BSG, ITGAM, MTCO2P12, SERPINE1, NFKB1, S100A9, HIF1A, OLFM1, HLA-DRB1, NFE2L2, GABPA, NOD2, MYD88, WNT5A, NPY, RNF19A, LEP, POLDIP2, COL25A1, LTA, EDIL3, INPP5D, LTF, MIF, CXCL12, GRAP2, SLC52A1, SOD2, REN, IL2RA, ADAM17, NR1I2, MMP7, PTH, TIMP1, PRTN3, AHSA1, AIMP2, FCGR3A, IL33, CRK, MIR142, MAPK14, ALB, AHR, CTSK, FCGR2B, IL34, COX8A, PCSK9, CD40LG, MIR21, CD36, RUNX2, TRAP, C20orf181, MBL3P, BCL2, CD274, TRBV20OR9-2, MEFV, MBL2, MALAT1, CSF3, CTNNB1, GCFC2, TREM1, ATM, MLKL, CTSS, RTL1, CYP1A1, IFNL1, SYT1, TREM2, STAT1, ADIPOQ, CLU, SIRT1, ANP32B, TNFSF13B, CAT, PTPN2, RARRES2, CALCA, P2RX7, RELA, RNASE3, DKK1, CD68, TMPRSS13, SFRP5, PADI4, CDK9, NFATC1, MUC4, CTSC, SELE, MST1, MSMB, TUG1, SETMAR, MMP12, ODAM, PON1, IL11, THBS1, IGF1, TIMP2, EGF, ELN, TIMP4, LMLN, TLR1, FGD5-AS1, AGT, GIP, SLC52A2, F2R, TNFSF13, WNK1, GORASP1, HGF, ALDH2, GSTM1, FCGR2A, IGFBP5, CXCR4, ATN1, IL6ST, THNSL2, APOE, IL2, APP, PWAR1, ST8SIA4, FOXO1, DNMT1, FN1, FGF2, NR1H4, LINC00687, MIR584, ZBTB18, OIP5-AS1, HAX1, DEFA1B, LRPPRC, BHLHE40, NOD1, CDR1-AS, EBI3, RECK, LOH19CR1, YAP1, DEFB104B, MIR381, CRISP3, EDS8, CDR3, DDX39A, MIR335, ARHGEF5, MAEA, UPK3B, DEFA1A3, MIR4435-2HG, PLPPR4, VAMP8, SDC3, PTGES, SLC33A1, P2RX6, MAFD4, BOP, NRP1, CCRL2, HDAC3, SOCS3, TNFSF12-TNFSF13, HAP1, SELENBP1, HSPB3, TIMELESS, PROM1, ZNF667-AS1, SQSTM1, MAFD6, MIR1226, IL18R1, IL32, MIR543, NCR1, NCR2, ZGLP1, MYMX, SOCS1, CDK5R1, NTN1, TNFSF12, PDLIM7, PGR-AS1, PTCSC3, P2RX5-TAX1BP3, VAMP3, CD163, SOCS6, MRLN, NLRC5, ANGPTL2, MIR27A, DDX53, ZNF513, YOD1, MEG3, CD200R1, DEFB104A, NEK7, IL23R, DRAM1, GHS, LBX2-AS1, ASPN, IL22RA2, NLRP6, FAM20A, COPD, LEPROT, CCHCR1, IFNL3, LINC01566, IL23A, NME8, TLR8, MRGPRX2, UCN3, MIR23A, ACE2, MIXL1, MAP1LC3B, DCSTAMP, PTGES2, DHDDS, ABCC11, EHMT1, DHX40, PANK3, BACH2, IL21, CDCA5, NLRC4, ZNF410, MTG1, SLAMF7, DNER, SFXN1, CHPT1, FAM20C, KCNQ5, SLC50A1, TLR7, BFAR, DCTN4, SLC7A9, CAMTA1, MIR200A, MIR200C, JMJD6, P2RX2, HSPA4L, PARK7, PADI2, ADAMTS7, WDHD1, RIPK3, NLRP10, IL24, FASTK, LILRB1, HPSE, TOB2, NES, PTGES3, KHDRBS1, MIR214, MIR22, MIR182, MIR17, HEY1, NUP62, GPR141, DELEC1, TBX21, SETD2, HPGDS, IL31, GTF2H5, MIR100, MIR125A, IL17C, MIR126, IL37, HAVCR1, MIR132, MIR143, MIR144, MIR148A, MIR155, PART1, QPCT, IL17RA, ACP5, RBP4, TFEB, ENO1, FGF7, FGB, FCN2, FCGR3B, FBN1, PTK2B, FABP4, ETS1, ERCC2, EPO, EPHB2, EPHA3, ENO3, ELAVL1, FOS, S1PR1, ECE1, DSG1, RCAN1, DSC3, DSC1, DMP1, DMD, DLX5, DLD, DEFA4, DEFA1, DECR1, FOLR1, FOSB, DDX39B, CXCL1, IFN1@, IBSP, TNC, HSPB2, HSPB1, HPX, HNRNPL, HMOX1, HLA-B, HDC, HBB, GTF2H1, GSTT1, GRN, GAD1, GPX1, GPT, FFAR1, CXCR3, GLP1R, GIPR, GHRHR, GH1, GEM, GCHFR, GCG, GC, GATA3, DDOST, CYP2E1, CYP1B1, APRT, C5, C3, C1QA, BMP4, BMP2, BMP1, PRDM1, CEACAM1, BGLAP, AZU1, ATF4, AR, AQP3, APOH, CTSG, APOB, XIAP, BIRC3, APEX1, APAF1, ANXA1, ANPEP, ALPP, AKT1, AGTR1, JAG1, ADRB2, ADM, CALR, CASP8, CASP9, CAV1, CSF3R, CSF1R, CRYGD, COL5A1, CMKLR1, CCR6, CCR4, CCR1, CISH, CHGA, CEACAM7, CFTR, CEACAM5, CDKN2B, CDKN2A, LRBA, CD81, CD74, CD69, CD44, CD40, CD38, CD28, CD27, CD1D, CD1A, CBS, IFNB1, IFNGR1, JCHAIN, RXRA, SHBG, SH3BP2, SET, SELP, SELL, CXCL5, CCL25, CCL5, CCL3, S100B, S100A4, S100A2, S100A1, RPS19, PIK3CD, ROS1, RCN1, ADA, RAC2, PTPRA, PTHLH, PROS1, PPP1R1A, PPIA, PLTP, PLEK, PLAU, PIN1, SLC2A1, SLC2A4, SLIT3, SP1, CRSA, IL1R2, BEST1, VEGFC, VAV1, TYRO3, TWIST1, TRAF6, TPM3, TP53, TLR3, TLL1, TH, TGM4, TFRC, PRDX2, TCF12, TCF7L2, TAC1, SYK, ABCC8, SULT1A1, STAT2, SSTR2, SST, SPIB, SPG7, PIK3CG, PIK3CB, IL1R1, JAK1, MFAP1, MAFD2, MAFD1, SMAD6, LPO, LEPR, LDLR, LAD1, KRT19, KRT13, KLRB1, KIR3DL1, KDR, ITGB6, PIK3CA, ITGAL, ITGAE, ISG20, IRF5, IRF4, IL16, IL12RB2, IL12B, IL12A, CXCR2, IL6R, IL5, IL4R, MFGE8, MME, MMP10, MNAT1, PI3, PGF, PF4, PCNA, SERPINB2, PRDX1, P2RY2, P2RY1, P2RX5, P2RX4, P2RX3, P2RX1, OSM, OPRM1, NT5E, NPM1, PNP, NOS3, NOS2, NM, NGF, NFYA, NFKBIL1, GADD45B, MT1A, MSX2, CD200, LOC107984137
-
Porphyria
Wikipedia
For instance, the polyneuropathy of acute porphyria may be mistaken for Guillain–Barré syndrome , and porphyria testing is commonly recommended in those situations. [6] Chronic porphyrias [ edit ] The non-acute porphyrias are X-linked dominant protoporphyria (XLDPP), congenital erythropoietic porphyria (CEP), porphyria cutanea tarda (PCT), and erythropoietic protoporphyria (EPP). ... As a result of feedback, the decreased production of heme leads to increased production of precursors, PBG being one of the first substances in the porphyrin synthesis pathway. [23] In nearly all cases of acute porphyria syndromes, urinary PBG is markedly elevated except for the very rare ALA dehydratase deficiency or in patients with symptoms due to hereditary tyrosinemia type I . [24] In cases of mercury - or arsenic poisoning -induced porphyria, other changes in porphyrin profiles appear, most notably elevations of uroporphyrins I & III, coproporphyrins I & III, and pre-coproporphyrin. [25] Repeat testing during an attack and subsequent attacks may be necessary in order to detect a porphyria, as levels may be normal or near-normal between attacks. ... In the United Kingdom, supplies of NormoSang are kept at two national centers; emergency supply is available from St Thomas's Hospital , London. [27] In the United States, Lundbeck manufactures and supplies Panhematin for infusion. [28] Heme arginate (NormoSang) is used during crises but also in preventive treatment to avoid crises, one treatment every 10 days. [ citation needed ] Any sign of low blood sodium ( hyponatremia ) or weakness should be treated with the addition of hematin, heme arginate, or even tin mesoporphyrin , as these are signs of impending syndrome of inappropriate antidiuretic hormone (SIADH) or peripheral nervous system involvement that may be localized or severe, progressing to bulbar paresis and respiratory paralysis. [ citation needed ] Cimetidine [ edit ] Cimetidine has also been reported to be effective for acute porphyric crisis and possibly effective for long-term prophylaxis. [29] Symptom control [ edit ] Pain is severe, frequently out of proportion to physical signs, and often requires the use of opiates to reduce it to tolerable levels. ... External links [ edit ] Porphyria at Curlie The Drug Database for Acute Porphyria - comprehensive database on drug porphyrinogenicity Orphanet's disease page on Porphyria Classification D ICD - 10 : E80.0 - E80.2 ICD - 9-CM : 277.1 MeSH : D011164 External resources MedlinePlus : 001208 Patient UK : Porphyria Orphanet : 738 v t e Heme metabolism disorders Porphyria , hepatic and erythropoietic ( porphyrin ) early mitochondrial: ALAD porphyria Acute intermittent porphyria cytoplasmic: Gunther disease/congenital erythropoietic porphyria Porphyria cutanea tarda / Hepatoerythropoietic porphyria late mitochondrial: Hereditary coproporphyria Harderoporphyria Variegate porphyria Erythropoietic protoporphyria Hereditary hyperbilirubinemia ( bilirubin ) unconjugated: Gilbert's syndrome Crigler–Najjar syndrome Lucey–Driscoll syndrome conjugated: Dubin–Johnson syndrome nd sheet Rotor syndrome
-
Hydrocephalus
Wikipedia
Focal neurological deficits may also occur, such as abducens nerve palsy and vertical gaze palsy ( Parinaud syndrome due to compression of the quadrigeminal plate , where the neural centers coordinating the conjugated vertical eye movement are located). ... Fluid accumulates in the upper ventricles, causing hydrocephalus. [13] Other causes of congenital hydrocephalus include neural-tube defects, arachnoid cysts , Dandy–Walker syndrome , and Arnold–Chiari malformation . ... Children more commonly live with undeveloped brain tissue and consequential intellectual disabilities and restrictions. [37] Society and culture [ edit ] Name [ edit ] The word hydrocephalus is from the Greek ὕδωρ , hydōr meaning 'water' and κεφαλή , kephalē meaning 'head'. [7] Other names for hydrocephalus include "water on the brain", a historical name, and "water baby syndrome". [1] [38] Awareness campaign [ edit ] Hydrocephalus awareness ribbon September was designated National Hydrocephalus Awareness Month in July 2009 by the U.S. ... Hydrocephalus at Curlie Guidelines for pediatric hydrocephalus v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Congenital malformations and deformations of nervous system Brain Neural tube defect Anencephaly Acephaly Acrania Acalvaria Iniencephaly Encephalocele Chiari malformation Other Microcephaly Congenital hydrocephalus Dandy–Walker syndrome other reduction deformities Holoprosencephaly Lissencephaly Microlissencephaly Pachygyria Hydranencephaly Septo-optic dysplasia Megalencephaly Hemimegalencephaly CNS cyst Porencephaly Schizencephaly Polymicrogyria Bilateral frontoparietal polymicrogyria Spinal cord Neural tube defect Spina bifida Rachischisis Other Currarino syndrome Diastomatomyelia Syringomyelia Authority control GND : 4064743-2 NDL : 00568721HYDIN, CCDC88C, CRPPA, CCND2, TMEM67, CCDC39, FZD3, POMK, EXOC3L2, NMNAT2, THAS, STK36, SIN3A, IFT122, AQP4, CCDC85C, AQP1, NME5, MBOAT7, ADD1, E2F5, CELSR2, ITGB1, KIF27, SOX3, AK8, NME7, L1CAM, HSPD1, AK7, HMGB1, ULK4, BOK, DPCD, PPARA, B3GALNT2, CCNO, DNAAF3, OFD1, AP1S2, POMGNT1, B3GLCT, PTEN, FANCC, CCDC151, FANCB, LRRC6, CEP290, TSC2, GPC4, BUB1B, FGFR2, DNAI1, FLNA, MTOR, COL18A1, B4GALT1, POMT1, SMARCB1, CSF1R, POMGNT2, CRB2, DNAH5, PIK3CA, CC2D2A, TP53, FUZ, CHST3, VANGL1, HDAC6, SLC25A1, SPAG1, TTC25, TBXT, AKT3, SEC24C, TMEM231, MED12, MFN2, WASHC5, CEP104, KIAA0586, SOX9, PTDSS1, RECQL4, FIG4, SOX2, SEC24D, HIRA, TCTN1, TBX15, TYROBP, UFD1, KDM6A, TSC1, VHL, WNT3, XRCC2, ZIC2, ZIC3, ARMC9, B9D2, SF3B4, SHOC2, ROGDI, KMT2D, CNTNAP1, TNFSF11, FRAS1, PTCH2, DNAH11, TNFRSF11A, TCTN2, CSPP1, PALB2, TBX1, ZNHIT3, LARGE1, BICD2, TCIRG1, RFWD3, ARMC4, FANCL, CCDC40, RNF125, DNAAF5, MKS1, NSUN2, AHI1, DLL4, NDUFB11, DNAI2, TREM2, PORCN, SUFU, TMEM138, LMBR1, CEP55, ZMYND10, DNAAF2, FANCM, PIEZO2, DOCK6, ARHGAP31, FAM111A, VANGL2, RPGRIP1, SMOC1, CFAP298, INPP5E, VAC14, FLVCR2, CHD7, SLC29A3, FANCI, TMEM237, MBTPS2, RXYLT1, DNAH1, KIF4A, SIK3, RPGRIP1L, RSPH3, KIAA0556, ZNF423, CILK1, POLR3A, B4GAT1, EBP, ARFGEF2, RNASEH2A, PIBF1, MAD2L2, FKRP, MMACHC, ZBTB20, NME8, B3GAT3, TMEM216, WDPCP, VSX1, SLC25A24, POMT2, GMPPB, GPSM2, SNX10, UBE2T, OSTM1, CCDC22, CPLANE1, FTO, B9D1, SLC17A5, DNAL1, PYCR1, CCL2, GPC3, GFAP, GBA, GAS8, GALC, RSPH9, FGFR3, FGFR1, FKTN, FBN1, FANCG, FANCF, FANCE, FANCD2, FANCA, GAS2L2, JMJD1C, HYLS1, CEP120, ARL13B, RBPJ, DNAAF4, TMEM92, IDUA, IDS, HRAS, BRIP1, HCCS, HBA2, HBA1, GUSB, GP1BB, GNAQ, GLI3, GLI2, SLC13A5, ERF, ERCC5, ERCC4, RSPH4A, COMT, COL4A1, DNAJB13, CLCN7, KIF7, CENPF, CCDC103, BRCA2, BRAF, BRCA1, KIF1A, ARVCF, ARSB, ARL3, MCIDAS, COX7B, CREBBP, DMPK, ERCC3, ERCC2, EOGT, EML1, SUMF1, DPH1, DHCR24, CSF2, DHCR7, RSPO2, DAG1, CTSK, CYP26C1, CTNNB1, ESCO2, HNRNPU, PDGFRB, IFT43, TMEM107, PTCH1, SLX4, MAP2K2, MAP2K1, OGDH, P4HB, PRKAR1A, PPP2R5D, LRRC56, PRDX1, PPP2R1A, PIK3R2, CEP41, CCDC114, PPP1CB, POR, DRC1, PDGFB, PLOD1, PDHA1, RSPH1, CCDC65, PLG, NRAS, NPHP1, NOTCH2, NOTCH1, KIAA1109, KRAS, RREB1, LAMB1, LAMC2, RPGR, LIG4, MC1R, MTM1, MUSK, RAP1B, RAP1A, AMER1, PIH1D3, RAD51C, WDR81, NF1, NF2, RAD51, DNAAF1, TRPV4, NID1, PEX19, CFAP300, IL6, ENOPH1, TGFB1, UGCG, EPO, NAPA, GCLC, TNF, PWAR1, IL24, DNAH3, SLC52A2, MINDY4, NR1I2, SPEF2, PRL, CRP, FOXJ1, IL1B, F2R, CFAP52, DELYQ11, ARHGAP24, TMX2-CTNND1, COMMD3-BMI1, RN7SL263P, SFTPA2, PRDM16, MIR630, SFTPA1, RNF34, SNX27, RSS, MIR146B, SFTA2, ARX, TTC8, EXOSC6, DHDDS, ADAMTS20, ASRGL1, IS1, CCDC28B, ACHE, ISLR2, PAFAH1B1, F5, FOXC1, GH1, GLB1, GLDC, GLP1R, IFNG, IGF1, IGFBP1, IKBKB, IL4, CXCL8, ITPR1, LDLR, MYC, MYH2, NCAM1, NELL1, NEO1, NFIA, NFIB, NFIX, NT5E, F3, EYA1, MARK2, CDH5, AFP, APP, AR, RND3, AVP, BDNF, BMI1, BMP4, CD68, CDC42, CDKN1C, EGF, CETN2, CNR2, COL1A2, KLF6, COX6B1, CTNND1, ECI1, HBEGF, DUSP2, E2F1, NTF3, PAK1, SLC4A10, PAK3, ADCYAP1R1, RUVBL1, PSMG1, TP63, MPDZ, ENDOU, WASF1, DLG5, CD163, SLC9A3R1, SPAG6, TUBB3, NDC80, NES, CORO1A, BBS9, CNTN6, DCDC2, CNTN5, RHOF, CDCA8, CHPT1, ADAMTS9, EOS, WNT1, TP73, RMRP, PAX2, PAX3, PCBD1, PCM1, PIK3CB, PIK3CD, PIK3CG, PKD2, PSEN1, PTPN11, S100A10, TNFRSF1A, S100B, ACSM3, SFTPC, SFTPD, SLC12A2, SLC20A2, SMARCA1, SMARCA4, SMS, TCHH, H3P47
-
Feline Idiopathic Cystitis
Wikipedia
However, UTIs in cats under the age of 10 years old are very rarely encountered and whilst other specific reasons for the inflammation may be identified, in most cases it will not have an known cause and remains idiopathic. [2] [3] In cats over 10 years of age, UTIs are much more common and idiopathic cases are much less frequently observed. [4] On the other hand, FIC does show several similarities to an analogous disease in humans called bladder pain syndrome . [5] [6] Contents 1 Signs and symptoms 1.1 Non-obstructive FIC 1.2 Obstructive FIC (“the blocked cat”) 1.3 Differential diagnosis of obstructive and non-obstructive cases 2 Pathophysiology 3 Non-obstructive episodes of FIC 3.1 Causes 3.2 Treatment of an acute episode 4 Obstructive episodes of FIC (“the blocked cat”) 4.1 Causes 4.1.1 Functional blockage 4.1.2 Mechanical blockage 4.1.3 Interaction between functional and mechanical blockage in FIC 4.1.4 The role of crystals in obstructive FIC 4.2 Treatment of an acute episode 4.3 Secondary bacterial infection (UTI) after an obstructive episode 5 Ongoing management of FIC 5.1 Importance of hydration 5.2 Environmental modification 5.3 Surgical intervention for refractory cases 6 References Signs and symptoms [ edit ] Feline idiopathic cystitis begins as an acute non-obstructive episode and in most cases (around 85%) is self-limiting, resolving itself in around a week. ... He is unwell and his urinary system is not functioning properly, and therefore he may struggle to clear crystals from the bladder as a result of the syndrome. The inflammation, particularly in a full or partial obstructive episode, may encourage urinary retention and incomplete voiding. ... Even after the cat is unblocked, the underlying inflammatory syndrome will continue for some days at home (particularly since the catheter itself will have irritated the urethra).
-
Juvenile Idiopathic Arthritis
Wikipedia
Long term steroid use can cause contribute to the development of cataracts. [6] Macrophage activation syndrome (MAS) is a severe, potentially life-threatening complication that can occur in patients with the Systemic subtype of JIA. ... Patients with Systemic-onset juvenile idiopathic arthritis are at risk of a potentially life-threatening complication called Macrophage activation syndrome .Rheumatoid factor and ANA are generally negative in systemic JIA. [ citation needed ] Enthesitis Related Arthritis [ edit ] This subtype of arthritis is diagnosed by the presence of arthritis and enthesitis, or by the presence of arthritis or enthesitis alone with 2 or more of the following features: (1) Presence or history of sacroiliac joint tenderness and/or inflammatory back pain; (2) Presence of the HLA-B27 antigen; (3) Onset of arthritis in a male over 6 years of age; (4) Acute (symptomatic) anterior uveitis; or (5) a history of Ankylosing spondylitis , enthesitis related arthritis, sacroiliitis with Inflammatory bowel disease , or acute anterior Uveitis in a first-degree relative. ... For the Systemic-onset form of JIA, the differential diagnosis also includes Kawasaki disease and periodic fever syndromes. Rarely, skeletal dysplasias or metabolic diseases, such as Farber disease and forms of Mucopolysaccharidosis , may also mimic JIA, as they may present with joint swelling, joint restriction, stiffness, and pain.
-
Head Injury
Wikipedia
Specific problems after head injury can include [4] [5] [6] Skull fracture Lacerations to the scalp and resulting hemorrhage of the skin Traumatic subdural hematoma, a bleeding below the dura mater which may develop slowly Traumatic extradural, or epidural hematoma, bleeding between the dura mater and the skull Traumatic subarachnoid hemorrhage Cerebral contusion , a bruise of the brain Concussion , a loss of function due to trauma Dementia pugilistica , or "punch-drunk syndrome", caused by repetitive head injuries, for example in boxing or other contact sports A severe injury may lead to a coma or death Shaken baby syndrome – a form of child abuse Concussion [ edit ] Main article: Concussion coup bruise A concussion is a form of a mild traumatic brain injury (TBI). ... In all cases, the patients develop post concussion syndrome , which includes memory problems, dizziness, tiredness, sickness and depression . ... External links [ edit ] Classification D ICD - 10 : S00.0 S09 ICD - 9-CM : 800 - 879 MeSH : D006259 DiseasesDB : 5671 External resources eMedicine : neuro/153 Patient UK : Head injury Brain Injury (journal) Cochrane Injuries Group: systematic reviews on the prevention, treatment and rehabilitation of traumatic injury First aid advice for head injuries from the British Red Cross v t e Nonmusculoskeletal injuries of head ( head injury ) and neck Intracranial see neurotrauma Extracranial/ facial trauma eye : Black eye Eye injury Corneal abrasion ear : Perforated eardrum Either/both Penetrating head injury v t e Trauma Principles Polytrauma Major trauma Traumatology Triage Resuscitation Trauma triad of death Assessment Clinical prediction rules Revised Trauma Score Injury Severity Score Abbreviated Injury Scale NACA score Investigations Diagnostic peritoneal lavage Focused assessment with sonography for trauma Management Principles Advanced trauma life support Trauma surgery Trauma center Trauma team Damage control surgery Early appropriate care Procedures Resuscitative thoracotomy Pathophysiology Injury MSK Bone fracture Joint dislocation Degloving Soft tissue injury Resp Flail chest Pneumothorax Hemothorax Diaphragmatic rupture Pulmonary contusion Cardio Internal bleeding Thoracic aorta injury Cardiac tamponade GI Blunt kidney trauma Ruptured spleen Neuro Penetrating head injury Traumatic brain injury Intracranial hemorrhage Mechanism Blast injury Blunt trauma Burn Penetrating trauma Crush injury Stab wound Ballistic trauma Electrocution Region Abdominal trauma Chest trauma Facial trauma Head injury Spinal cord injury Demographic Geriatric trauma Pediatric trauma Complications Posttraumatic stress disorder Wound healing Acute lung injury Crush syndrome Rhabdomyolysis Compartment syndrome Contracture Volkmann's contracture Embolism air fat Chronic traumatic encephalopathy Subcutaneous emphysema v t e General wounds and injuries Abrasions Abrasion Avulsion Blisters Blood blister Coma blister Delayed blister Edema blister Fracture blister Friction blister Sucking blister Bruises Hematoma / Ecchymosis Battle's sign Raccoon eyes Black eye Subungual hematoma Cullen's sign Grey Turner's sign Retroperitoneal hemorrhage Animal bites Insect bite Spider bite Snakebite Other: Ballistic trauma Stab wound Blunt trauma /superficial/ closed Penetrating trauma / open Aerosol burn Burn / Corrosion / Chemical burn Frostbite Occupational injuries Traumatic amputation By region Hand injury Head injury Chest trauma Abdominal trauma
-
Tension Headache
Wikipedia
External links [ edit ] Classification D ICD - 10 : G44.2 ICD - 9-CM : 307.81 , 339.1 MeSH : D018781 DiseasesDB : 12554 External resources MedlinePlus : 000797 eMedicine : article/1142908 American Council for Headache Education National Headache Foundation World Headache Alliance v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Headache Primary ICHD 1 Migraine Familial hemiplegic Retinal migraine ICHD 2 Tension Mixed tension migraine ICHD 3 Cluster Chronic paroxysmal hemicrania SUNCT ICHD 4 Hemicrania continua Thunderclap headache Sexual headache New daily persistent headache Hypnic headache Secondary ICHD 5 Migralepsy ICHD 7 Ictal headache Post-dural-puncture headache ICHD 8 Hangover Medication overuse headache ICHD 13 Trigeminal neuralgia Occipital neuralgia External compression headache Cold-stimulus headache Optic neuritis Postherpetic neuralgia Tolosa–Hunt syndrome Other Vascular
-
Ectopic Pregnancy
Wikipedia
Intrauterine adhesions (IUA) present in Asherman's syndrome can cause ectopic cervical pregnancy or, if adhesions partially block access to the tubes via the ostia , ectopic tubal pregnancy. [24] [25] [26] Asherman's syndrome usually occurs from intrauterine surgery, most commonly after D&C . [24] Endometrial/pelvic/genital tuberculosis , another cause of Asherman's syndrome, can also lead to ectopic pregnancy as infection may lead to tubal adhesions in addition to intrauterine adhesions. [27] Tubal ligation can predispose to ectopic pregnancy. ... "[Cervical pregnancy in Asherman's syndrome]". Ginekologia Polska . 58 (1): 46–8. ... Association with abortion, pelvic pathology, IUDs and Asherman's syndrome". The Journal of Reproductive Medicine . 30 (1): 25–7.CRISP3, DNAAF2, CFAP298, TTC25, DNAL1, RSPH3, CFAP300, CCDC65, RSPH1, DRC1, CCDC114, LRRC56, CCDC151, DNAAF1, PIH1D3, DNAAF4, RSPH9, GAS2L2, CCDC39, MCIDAS, RSPH4A, DNAAF3, DNAJB13, DNAI2, CCDC103, DNAH5, DNAH1, GAS8, RPGR, SPAG1, OFD1, DNAH11, ARMC4, LRRC6, CCNO, DNAI1, STK36, NME8, ZMYND10, HYDIN, DNAAF5, CCDC40, VEGFA, TRO, MUC1, LIF, HOXA11, CNR1
-
Conversion Disorder
Wikipedia
Usually the physical symptoms of the syndrome affect the senses or movement. ... Treatment [ edit ] There are a number of different treatments available to treat and manage conversion syndrome. Treatments for conversion syndrome include hypnosis, psychotherapy, physical therapy, stress management, and transcranial magnetic stimulation . ... External links [ edit ] Classification D ICD - 10 : F44 ICD - 9-CM : 300.11 MeSH : D003291 DiseasesDB : 1645 External resources MedlinePlus : 000954 eMedicine : emerg/112 med/1150 v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Ichthyosis, Congenital, Autosomal Recessive 1
Omim
ARCI14 (617571) is caused by mutation in the SULT2B1 gene (604125) on chromosome 19q13. Ichthyosis prematurity syndrome (608649) is a self-improving form of ichthyosis that includes respiratory complications at birth and persistent eosinophilia and is caused by mutation in the FATP4 (SLC27A4; 604194) gene. A rare syndromic form of NCIE, Chanarin-Dorfman syndrome (275630), is caused by mutation in the ABHD5 gene (604780). ... Nomenclature Vahlquist (2010) proposed a subclassification of ARCI for the self-improving forms of ichthyosis, including self-healing collodion baby and ichthyosis prematurity syndrome (IPS), to be designated 'pleomorphic ichthyosis' (PI).
-
Frontal Lobe Epilepsy
Wikipedia
People with frontal lobe epilepsy show decreased cognitive capabilities in the following areas: humor appreciation, recognition of emotional expressions, response selection/initiation and inhibition, hyperactivity, conscientiousness, obsession, addictive behavior , motor coordination and planning, attention span, performance speed, continuous performance without intrusion and interference errors, copying and recall, concept formation, anticipatory behavior, memory span , working memory , executive planning, visuo-spatial organization, mental flexibility, conceptual shift, problem solving, programming of complex motor sequences, impulse control , judgment and forecasting of consequences. [9] [23] [24] [25] Physical health and risk of other conditions Patients with epilepsy face a greater risk of accidents, injury and other medical conditions than the general population. [22] A European study showed that people with epilepsy were at greater risk for accidental injuries related to seizures such as concussions, abrasions and wounds and reported more hospitalizations and medical action than the general population. [26] Other studies have shown that people with epilepsy are at a greater risk of seizure related drowning, suffocation, broken bones and burns and more likely to die in a fatal automobile crash. [27] Epilepsy Ontario reports that people with epilepsy are also more likely to have other conditions than the general population such as: 30% of autistic children have epilepsy, 33% of cerebral palsy patients have epilepsy, 15-20% of fragile X syndrome patients have epilepsy, 50% of children with learning disabilities will have some form of epilepsy, 3-10% of patients with Lennox-Gastaut syndrome will have epilepsy, 80% of children with Rett syndrome will have epilepsy and 80% of patients with Tuberous Sclerosis will have epilepsy. [28] Mental and emotional health Epileptic patients are more prone to suffer psychological and social dysfunction than individuals that do not have epilepsy. ... External links [ edit ] Frontal lobe epilepsy on Epilepsy.com Epilepsy Foundation v t e Seizures and epilepsy Basics Seizure types Aura (warning sign) Postictal state Epileptogenesis Neonatal seizure Epilepsy in children Management Anticonvulsants Investigations Electroencephalography Epileptologist Personal issues Epilepsy and driving Epilepsy and employment Seizure types Focal Seizures Simple partial Complex partial Gelastic seizure Epilepsy Temporal lobe epilepsy Frontal lobe epilepsy Rolandic epilepsy Nocturnal epilepsy Panayiotopoulos syndrome Vertiginous epilepsy Generalised Tonic–clonic Absence seizure Atonic seizure Automatism Benign familial neonatal seizures Lennox–Gastaut syndrome Myoclonic astatic epilepsy Epileptic spasms Status epilepticus Epilepsia partialis continua Complex partial status epilepticus Myoclonic epilepsy Progressive myoclonus epilepsy Dentatorubral–pallidoluysian atrophy Unverricht–Lundborg disease MERRF syndrome Lafora disease Juvenile myoclonic epilepsy Non-epileptic seizure Febrile seizure Psychogenic non-epileptic seizure Related disorders Sudden unexpected death in epilepsy Todd's paresis Landau–Kleffner syndrome Epilepsy in animals Organizations Citizens United for Research in Epilepsy (US) Epilepsy Action (UK) Epilepsy Action Australia Epilepsy Foundation (US) Epilepsy Outlook (UK) Epilepsy Research UK Epilepsy Society (UK)
-
Depersonalization-Derealization Disorder
Wikipedia
The project was conducted in the hope that it would stimulate further scientific investigations into depersonalization disorder. [51] Diagnostic and Statistical Manual of Mental Disorders, 5th Edition (DSM-5) [ edit ] In the DSM-5 , the word "derealization" was added to "depersonalization disorder" and renamed "depersonalization/derealization disorder" ("DPDR"). [3] It remains classified as a dissociative disorder . [3] Patients must meet the following criteria to be diagnosed per the DSM-5: [3] Presence of persistent/recurrent episodes of depersonalization/derealization Ability to distinguish between reality and dissociation during an episode (i.e. patient is aware of a perceptual disturbance) Symptoms are severe enough to interfere with social, occupational, or other areas of functioning Symptoms are not due to a substance or medication Symptoms are not due to another psychiatric disorder International Classification of Diseases 11th Revision (ICD-11) [ edit ] The ICD-11 has relisted DPDR as a disorder rather than a syndrome as previously, and has also reclassed it as a dissociative disorder from its previous listing as a neurotic disorder . [4] The description used in the ICD-11 is similar to the criteria found in the DSM-5. ... Symptoms are severe enough to cause distress or impairment in functioning. [52] Differential Diagnoses [ edit ] DPDR differentials include neurologic and psychiatric conditions as well as side effects from illicit substances or medications. [9] [53] Neurologic [ edit ] Seizures Brain tumor Post-concussion syndrome Metabolic abnormalities Migraines Vertigo Meniere's disease Psychiatric [ edit ] Panic attack Phobias PTSD Acute stress syndrome Depression Schizophrenia Borderline personality disorder Other dissociative disorders Intoxication/Withdrawal from Illicit Substances [ edit ] Marijuana Hallucinogens MDMA Ketamine Prevention [ edit ] Depersonalization-derealization disorder may be prevented by connecting children who have been abused with professional mental health help. [54] Some trauma specialists suggest increasing inquiry into information about children's trauma history and exposure to violence, since the majority of people (about 80%) responsible for child maltreatment are children's own parents. [55] Trauma-specific intervention for children may be a useful in preventing future symptoms. [56] Treatment [ edit ] Treatment of DPDR is often difficult and refractory. ... Depersonalization: A New Look at a Neglected Syndrome . Cambridge, UK: Cambridge University Press. p. 120. ... "A case series of 223 patients with depersonalization-derealization syndrome" . BMC Psychiatry . 16 (1): 203. doi : 10.1186/s12888-016-0908-4 . ... External links [ edit ] Depersonalization at Curlie Classification D ICD - 10 : F48.1 ICD - 9-CM : 300.6 MeSH : D003861 v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Meningitis
Wikipedia
Specialty Infectious disease , neurology Symptoms Fever , headache , neck stiffness [1] Complications Deafness , epilepsy , hydrocephalus , cognitive deficits [2] [3] Causes Viral, bacterial, other [4] Diagnostic method Lumbar puncture [1] Differential diagnosis Encephalitis , brain tumor , lupus , Lyme disease , seizures , neuroleptic malignant syndrome , [5] naegleriasis [6] Prevention Vaccination [2] Medication Antibiotics , antivirals , steroids [1] [7] [8] Frequency 10.6 million (2017) [9] Deaths 288,000 (2017) [10] Meningitis is an acute inflammation of the protective membranes covering the brain and spinal cord , known collectively as the meninges . [2] The most common symptoms are fever , headache , and neck stiffness . [1] Other symptoms include confusion or altered consciousness , vomiting, and an inability to tolerate light or loud noises . [1] Young children often exhibit only nonspecific symptoms , such as irritability, drowsiness, or poor feeding. [1] If a rash is present, it may indicate a particular cause of meningitis; for instance, meningitis caused by meningococcal bacteria may be accompanied by a characteristic rash. [2] [3] The inflammation may be caused by infection with bacteria , other microorganisms , or viruses , and less commonly by certain drugs . [4] Meningitis can be life-threatening because of the inflammation's proximity to the brain and spinal cord; therefore, the condition is classified as a medical emergency . [2] [8] A lumbar puncture , in which a needle is inserted into the spinal canal to collect a sample of cerebrospinal fluid (CSF), can diagnose or exclude meningitis. [1] [8] Some forms of meningitis are preventable by immunization with the meningococcal , mumps , pneumococcal , and Hib vaccines . [2] Giving antibiotics to people with significant exposure to certain types of meningitis may also be useful. [1] The first treatment in acute meningitis consists of promptly giving antibiotics and sometimes antiviral drugs . [1] [7] Corticosteroids can also be used to prevent complications from excessive inflammation. [3] [8] Meningitis can lead to serious long-term consequences such as deafness , epilepsy , hydrocephalus , or cognitive deficits , especially if not treated quickly. [2] [3] In 2017, meningitis occurred in about 10.6 million people worldwide. [9] This resulted in 288,000 deaths—down from 464,000 deaths in 1990. [11] [12] With appropriate treatment the risk of death in bacterial meningitis is less than 15%. [1] Outbreaks of bacterial meningitis occur between December and June each year in an area of sub-Saharan Africa known as the meningitis belt . [13] Smaller outbreaks may also occur in other areas of the world. [13] The word meningitis comes from the Greek μῆνιγξ meninx , "membrane", and the medical suffix -itis , "inflammation". [14] [15] Contents 1 Signs and symptoms 1.1 Clinical features 1.2 Early complications 2 Causes 2.1 Bacterial 2.2 Viral 2.3 Fungal 2.4 Parasitic 2.5 Non-infectious 3 Mechanism 4 Diagnosis 4.1 Lumbar puncture 4.2 Postmortem 5 Prevention 5.1 Behavioral 5.2 Vaccination 5.3 Antibiotics 6 Management 6.1 Bacterial meningitis 6.1.1 Antibiotics 6.1.2 Steroids 6.2 Viral meningitis 6.3 Fungal meningitis 7 Prognosis 8 Epidemiology 9 History 10 References 11 External links Signs and symptoms [ edit ] Clinical features [ edit ] Neck stiffness, Texas meningitis epidemic of 1911–12 In adults, the most common symptom of meningitis is a severe headache , occurring in almost 90% of cases of bacterial meningitis, followed by neck stiffness (the inability to flex the neck forward passively due to increased neck muscle tone and stiffness). [16] The classic triad of diagnostic signs consists of neck stiffness , sudden high fever , and altered mental status ; however, all three features are present in only 44–46% of bacterial meningitis cases. [16] [17] If none of the three signs are present, acute meningitis is extremely unlikely. [17] Other signs commonly associated with meningitis include photophobia (intolerance to bright light) and phonophobia (intolerance to loud noises). ... The infection may trigger sepsis , a systemic inflammatory response syndrome of falling blood pressure , fast heart rate , high or abnormally low temperature, and rapid breathing . ... Gangrene of limbs can occur in meningococcal disease. [2] Severe meningococcal and pneumococcal infections may result in hemorrhaging of the adrenal glands , leading to Waterhouse-Friderichsen syndrome , which is often fatal. [22] The brain tissue may swell , pressure inside the skull may increase and the swollen brain may herniate through the skull base.C8B, C8A, CRP, HCN1, HCN2, IL10, PRF1, BTK, TLR4, HLA-B, CYBB, WIPF1, LAMC2, JAK3, FOXP3, IL12A, IGLL1, SH2D1A, IGHM, IGH, ERAP1, HLA-DRB1, HLA-DPB1, HLA-DPA1, NDE1, ICOS, PTPN22, BLNK, TBK1, CXCR4, TLR3, KLRC4, TCF3, STAT4, RAG2, RAG1, PRTN3, PIK3R1, STAG2, NCF4, NCF2, TNFRSF13B, NLRC4, MEFV, LRRC8A, WAS, CR2, CD79B, CTLA4, CSF2, C4A, NLRP3, CCR1, TNFRSF13C, FAS, DNASE1L3, CD79A, IL23R, BCL2, CD19, UBAC2, BCL6, CYBA, C4B, XIAP, IL12A-AS1, CYBC1, NCF1, VANGL1, TNF, IL6, MBL2, MMP9, CADM1, CXCL8, ST11, TLR2, BPI, GAST, NOD2, CXCL11, BDNF, CD248, MYD88, RECQL4, VIM, BATF, EGF, ENOSF1, LINC01672, IL2RG, TGFB1, CXCL10, ICAM1, IL1B, GALNS, TCF12, PAGR1, MECP2, TNFSF10, PER2, CNTNAP1, MARCO, ARTN, RIPK2, SAMM50, NEURL1, IRAK4, CARD9, ARHGEF28, CARD14, DDX56, TLR9, MARCHF9, IL23A, AADAT, SLC46A1, LRG1, MSC, LAMP3, SUMF2, NCOA6, IFNL3, WDHD1, CYCSP51, FST, UBAC1, ABCB6, PARP1, NEU1, HSP90B1, IGFBP2, PRMT1, HLA-G, HLA-A, CFH, GYPC, CXCL1, GDNF, GC, FN1, FCGR3A, FCGR2A, FCGR1A, ESR1, ERBB2, EGFR, CSF3, COX8A, CHI3L1, CDS1, CD47, CAT, CAMP, C4BPA, AQP4, KLK3, APRT, AMBP, IFNG, IL1RN, TIMP1, IL17A, THBS1, PRDX2, STAT3, SLC11A1, CCL8, CCL3, PRNP, PDE7A, SERPINE1, OMP, OGG1, OAS3, OAS2, NTF3, NOS3, AGRP, MPO, MMP12, MMP8, MMP3, CXCL9, MFAP1, MDK, MAPT, LYZ, LSAMP, IL18, LOC108281177
-
Pulmonary Hypertension
Wikipedia
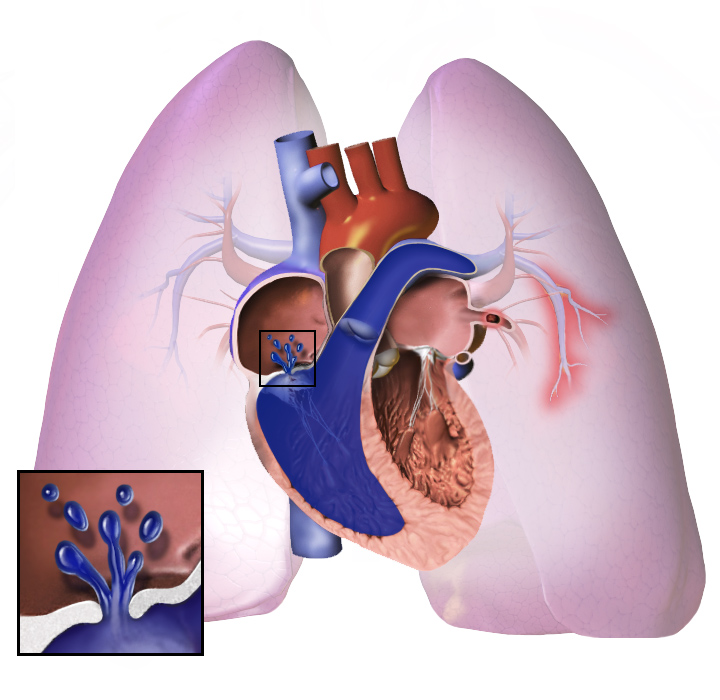
Condition causing increased blood pressure within the arteries of the lungs Pulmonary hypertension Other names Pulmonary arterial hypertension, [1] Ayerza syndrome [2] Pulmonary hypertension Specialty Pulmonology , cardiology Symptoms Chest pain, fatigue [3] Usual onset 20 to 60 years old [4] Duration Long term [1] Causes Unknown [1] Risk factors Family history, pulmonary embolism , HIV/AIDS , sickle cell disease , cocaine use, COPD , sleep apnea , living at high altitudes [5] [4] Diagnostic method Following ruling out other potential causes [1] Treatment Supportive care , various medications, lung transplantation [1] [6] Medication Epoprostenol , treprostinil , iloprost , bosentan , ambrisentan , macitentan , sildenafil [1] Frequency 1,000 new cases a year (US) [2] Pulmonary hypertension ( PH or PHTN ) is a condition of increased blood pressure within the arteries of the lungs . [7] Symptoms include shortness of breath , syncope , tiredness, chest pain, swelling of the legs , and a fast heartbeat . [7] [2] The condition may make it difficult to exercise. [7] Onset is typically gradual. [8] A patient is deemed to have pulmonary hypertension if the pulmonary mean arterial pressure is greater than 25mmHg at rest, or greater than 30mmHg during exercise. [9] The cause is often unknown. [1] Risk factors include a family history, prior blood clots in the lungs , HIV/AIDS , sickle cell disease , cocaine use, chronic obstructive pulmonary disease , sleep apnea , living at high altitudes , and problems with the mitral valve . [5] [4] The underlying mechanism typically involves inflammation and subsequent remodeling of the arteries in the lungs . [5] Diagnosis involves first ruling out other potential causes. [1] There is currently no cure for pulmonary hypertension, although research on a cure is ongoing. [7] Treatment depends on the type of disease. [6] A number of supportive measures such as oxygen therapy , diuretics , and medications to inhibit blood clotting may be used. [1] Medications specifically used to treat pulmonary hypertension include epoprostenol , treprostinil , iloprost , bosentan , ambrisentan , macitentan , and sildenafil . [1] Lung transplantation may be an option in severe cases. [6] While the exact frequency of the condition is unknown, it is estimated that about 1,000 new cases occur a year in the United States. [4] [2] Females are more often affected than males. [2] Onset is typically between 20 and 60 years of age. [4] It was first identified by Ernst von Romberg in 1891. [10] [1] Contents 1 Signs and symptoms 2 Causes 2.1 Classification 2.2 Genetics 3 Pathogenesis 3.1 Molecular pathology 3.1.1 Nitric oxide-soluble guanylate cyclase pathway 3.1.2 Endothelin 3.1.3 Prostacyclin (and thromboxane) 3.1.4 Other pathways 4 Diagnosis 4.1 Physical examination 4.2 Echocardiography 4.3 Exclude other diseases 4.3.1 Ventilation/perfusion scintigraphy 4.4 CT scan 4.5 Right heart catheterization 4.6 Other 5 Treatment 5.1 Vasoactive substances 5.1.1 Prostaglandins 5.1.2 Endothelin receptor antagonists 5.1.3 Phosphodiesterase type 5 inhibitors 5.1.4 Activators of soluble guanylate cyclase 5.2 Surgical 5.3 Monitoring 6 Prognosis 7 Epidemiology 8 Research 9 Notable cases 10 See also 11 References 12 Further reading 13 External links Signs and symptoms [ edit ] The symptoms of pulmonary hypertension include the following: [3] [11] [12] Shortness of breath Fatigue Chest pain Palpitations ( heartbeat rate increased) Right-sided abdominal pain Poor appetite Lightheadedness Fainting Swelling (legs/ankles) Cyanosis Less common signs/symptoms include non-productive cough and exercise-induced nausea and vomiting. [11] Coughing up of blood may occur in some patients, particularly those with specific subtypes of pulmonary hypertension such as heritable pulmonary arterial hypertension, Eisenmenger syndrome and chronic thromboembolic pulmonary hypertension . [13] Pulmonary venous hypertension typically presents with shortness of breath while lying flat or sleeping ( orthopnea or paroxysmal nocturnal dyspnea ), while pulmonary arterial hypertension (PAH) typically does not. [14] Other typical signs of pulmonary hypertension include an accentuated pulmonary component of the second heart sound, a right ventricular third heart sound , and parasternal heave indicating a hypertrophied right ventricle . ... This finding in three or four lobes, in the presence of a dilated pulmonary trunk (≥29 mm), and absence of significant structural lung disease confers a specificity of 100% for pulmonary hypertension. [60] Mural calcification in central pulmonary arteries is most frequently seen in patients with Eisenmenger's syndrome . [60] Right heart catheterization [ edit ] Although pulmonary arterial pressure (PAP) can be estimated on the basis of echocardiography , [61] pressure measurements with a Swan-Ganz catheter inserted through the right side of the heart provide the most definite assessment.[42] Pulmonary hypertension is defined as a mean PAP of at least 20 mm Hg (3300 Pa) at rest, and PAH is defined as precapillary pulmonary hypertension (i.e. mean PAP ≥ 20 mm Hg with pulmonary arterial occlusion pressure [PAOP] ≤ 15 mm Hg and pulmonary vascular resistance [PVR] > 3 Wood Units). [54] PAOP and PVR cannot be measured directly with echocardiography. ... In systemic scleroderma , the incidence has been estimated to be 8 to 12% of all patients; [91] in rheumatoid arthritis it is rare. [92] However, in systemic lupus erythematosus it is 4 to 14%, [93] and in sickle cell disease, it ranges from 20 to 40%. [94] Up to 4% of people who suffer a pulmonary embolism go on to develop chronic thromboembolic disease including pulmonary hypertension. [37] A small percentage of patients with COPD develop pulmonary hypertension with no other disease to explain the high pressure. [95] On the other hand, obesity-hypoventilation syndrome is very commonly associated with right heart failure due to pulmonary hypertension. [96] Research [ edit ] For people that inherited the disease, gene therapy is being studied. [97] Notable cases [ edit ] Elaine Kaufman , American restaurateur [98] Priya Balachandran, TV producer [99] Ina Balin , American Broadway and TV actress [100] Chloe Temtchine , American singer-songwriter [101] [102] Natalie Cole , American singer [103] See also [ edit ] Pulmonary Hypertension Association Cambridge Pulmonary Hypertension Outcome Review (CAMPHOR) References [ edit ] ^ a b c d e f g h i j k "Pulmonary Arterial Hypertension – NORD (National Organization for Rare Disorders)" . ... "Fatal ventricular fibrillation following verapamil in Wolff-Parkinson-White syndrome with atrial fibrillation" . Annals of Emergency Medicine . 14 (2): 159–60. doi : 10.1016/j.jacc.2013.10.025 .NPPB, EDN1, SLC6A4, ACVRL1, NFATC2, EDNRB, CD40LG, ALOX5, HIF1A, KCNA5, NOS3, CCL2, BMPR2, ACE, TGFA, PRKG1, TPH1, MIR204, CBLN2, FOXO1, BRD4, GBA, GDF2, FBLN5, HTR2B, TNF, CCL1, CXCL8, KCNK3, KCNMA1, LEPR, LOX, SLC31A1, SOD2, ABCA3, EIF2AK4, CA9, ATP7A, CALCA, ARG2, NOS2, AGT, CCN2, UTS2, PTGS2, ANGPT1, TNC, MMP1, RHOA, RELA, PTGIS, ATP2A2, SERPINA1, PECAM1, MMP9, MYC, PDGFA, CX3CL1, PDE3A, SERPINE1, ATP5F1A, NPPA, ATP5PF, PDGFB, TAC1, SLC2A4, HDAC5, CAVIN1, HIF3A, MFN1, SMPD3, ALAS1, GPR182, CYSLTR1, ALOX5AP, RAMP2, NAMPT, HYAL2, SMAD7, PDE5A, VIP, VCAM1, ANGPT2, TGFBR2, TGFBR1, BIRC5, TERT, TACR1, TACR2, SMAD9, COL4A1, SMAD6, PDIA3, CAV1, CD40, GATA6, SMAD4, MTOR, CDKN1A, FGFR1, FGF2, ESR2, EPHX2, EPAS1, EGR1, CDKN1B, EDNRA, CLU, ECE1, COL1A1, CYP1A1, CYBB, CYBA, CX3CR1, GJA1, GATA4, IL6, SMAD1, HYAL1, HMOX1, HMGCR, IL13, BDKRB2, BCL2, HMGB1, BCL2L1, HK1, CASR, HDAC1, HAS3, HAS2, HAS1, ID1, PPARG, BMP2, UTS2B, BMPR1B, NOX4, GREM1, BMP7, JUN, ADM, ARG1, ARHGEF6, APOE, F3, PLA2G7, VWF, FGA, VEGFA, TRPC6, TRPC4, TRPC3, HLA-A, SELP, F2
-
Pituitary Tumors
Mayo_clinic
Cushing disease is one cause of Cushing syndrome. Cushing disease symptoms include: Weight gain and fatty tissue deposits around the midsection and upper back. ... Enlargement of and pain in the ovaries caused by a condition called ovarian hyperstimulation syndrome. Symptoms in men may include: Enlarged testicles. ... Carney complex. McCune-Albright syndrome. Complications Pituitary tumors usually don't spread to other parts of the body.GH1, AIP, DRD2, PRL, MEN1, CDKN1B, IGF1, AGTR1, PTTG1, RB1, HNRNPK, IL6ST, POMC, VEGFA, PTTG1IP, FGF2, TP53, CDKN2A, HMGA2, CSH1, CSH2, SOX2, PTGS2, GHR, GH2, MEG3, KDR, PPARG, EGFR, BMP4, CCND1, ASAP2, AKAP4, DLK1, SOCS1, TP63, FZD6, BCL2, CXCR4, VEGFC, VDR, BAX, BRAF, TOP2A, TLR4, TIMP3, KLF10, THRB, TFAP2A, TBXAS1, TAL1, STAT3, CCNB2, ESPL1, SSTR1, SPA17, TMED7-TICAM2, MIR524, MIR146A, TICAM2, LRIG3, CCDC54, HDAC11, ZNF395, STS, WNT4, SCLY, ZNRD2, TMED7, CD274, SNHG1, RAB18, WIF1, GADD45G, NES, DCTN6, SCGB1D2, SCGN, SSTR5, SST, ESR1, CTSB, MMP2, CHGA, MAP2, LEPR, KRT7, KISS1, CREB1, ITGB2, IL10, CTNNB1, IFI27, MPP2, HSD11B2, CTSL, HMGA1, MSH6, GSTP1, GADD45A, DIO1, DIO2, FGFR4, ECT2, MMP9, MSH2, DDR1, PRKAA2, SKP2, SHH, SFRP4, SFRP2, CXCL12, CCNG1, CDH1, PSMD9, CDH13, PRKAB1, PRKAA1, NEUROD1, AHR, PPARA, POU1F1, CDKN1A, PIK3CG, PIK3CD, PIK3CB, PIK3CA, ABCB1, PCNA, H3P23
-
Retinoblastoma
Omim
See also the chromosome 13q14 deletion syndrome (613884) in which retinoblastoma is a feature. ... In a second child, they found retinoblastoma in association with Bloom syndrome (210900), another chromosome breakage syndrome. ... Grace et al. (1971) described a patient with typical 13q- syndrome plus retinoblastoma (613884). The karyotype contained a ring D chromosome. ... Lemieux et al. (1989) suggested that the gain in resolution afforded by immunochemical banding, coupled with electron microscopy, would prove highly useful in detecting small chromosome anomalies in clinical syndromes and neoplasms. Greger et al. (1990) studied a family in which the father and 2 of his children had bilateral retinoblastoma.RB1, MDM4, BCOR, TP53, BRCA2, CHEK2, PIK3CD, CDK4, CDK2, PCNA, PIK3CA, PIK3CB, H3P10, PAX6, TMED7-TICAM2, PSMD9, PTEN, TMED7, CASP3, RBL1, PIK3CG, CDK6, FANCM, CDKN1A, EGFR, ESD, CTNNB1, ESR1, CRX, IFI27, TICAM2, EPCAM, MDM2, TCHP, MYC, CDKN2B, CDKN2A, MYCN, CDKN1B, RBL2, E2F1, BCL2, ZNRD2, VEGFA, NOLC1, DCTN6, PRDM2, AKT1, CCND1, RAB3GAP1, H3P23, MAPK1, E2F3, PRB2, ERBB2, RBBP7, CIB1, FOXM1, TGFB1, RBP3, MTOR, CCNE1, MIR34A, KRAS, HMGB1, ATM, SLC12A9, HIF1A, DDX1, CDK1, GRAP2, KIF14, BDNF, MTDH, RNF19A, AIMP2, HDAC1, MAP2K7, CRK, ABCB1, POLDIP2, AHSA1, PLK1, BRAF, UHRF1, EZH2, MAPK14, TERT, SERPINF1, RBBP4, GRB10, FGF2, MIR17HG, FOXO1, MIR204, RNF40, RB1CC1, NXT1, CXCR4, MIR140, MIR106B, RGCC, HPGDS, S100A4, SAI1, MAPK8, SKP2, STAT3, SYK, TFF1, SUB1, RBBP9, DEK, MMP9, MRPL28, HMGA2, RBM45, IL6, POLD1, ABCG2, CDKN3, CD44, AR, CDKN1C, APC, CHEK1, H3P9, CDH11, CRH, FGFR3, COMMD3-BMI1, MIR183, MIR506, MAPK3, SIRT1, MIR21, SP1, ARR3, MIR215, SMAD2, SMARCA4, SOX2, MIR18A, MIR17, IGF1, H2AX, KLF6, MIR137, INTS6, RAF1, CAV1, RBBP6, BMI1, MIR613, HMGA1, HRAS, TNF, TFRC, CDKN2C, VDR, ACTB, DHFR, MGMT, PROM1, LMNA, E2F4, MTHFR, TSC2, XIST, EPHB2, SNHG16, ZNF266, OAT, OTX2, HOTAIR, ELOF1, MSH2, RUNX2, PTGS2, PTPN14, ODC1, AFAP1-AS1, ATRAID, MKI67, CDH13, CEACAM5, MCL1, BRS3, BRCA1, ACKR3, RCVRN, PSG2, NRAS, CCND2, MEG3, PIK3R1, LAMTOR1, AD12, MIB1, SEMA6A, PPARG, NME1, EAF2, CDC25C, NFKB1, MYBL2, CCNB1, MXI1, MMUT, MTR, CDK5, PDK1, MED4, PPM1D, TYMS, NEK6, UBE2I, APRT, VHL, CXCR6, WT1, LINC02210-CRHR1, MAFK, CLLS2, ADRA2B, PIK3R3, SGSM3, KHSRP, PSMG1, ZNF197, BECN1, ADRA1A, ADCYAP1R1, ADCYAP1, HDAC9, LPAR2, EEF1E1, RECQL4, TNFRSF1B, IL24, PSIP1, RASSF1, RFC1, RHO, SIGLEC7, ROCK1, PRDM1, SH2B1, BGN, SMAD4, BAX, SLC19A1, SMARCA1, SMARCB1, SSTR4, DICER1, SUV39H1, SYP, TAZ, TCF3, ATR, ATF3, H3P12, ASMT, TFF3, CCL2, MCM2, UCA1, IDH1, CEACAM7, IGFBP3, MIR34B, CUX1, IL2RB, CEACAM3, ILK, MIR98, MIR99A, ELN, FOLH1B, KIT, ELF1, EIF4E, EFNA2, IFNB1, MIR22, E2F5, MALAT1, MIR145, GPR42, H1-0, HCLS1, MAD2L1, MIR182, MIR186, FOS, HSPA4, FOLH1, HSP90AA1, FGFR1, CRHR1, FASN, FAP, EDNRA, NEAT1, MIR361, MIR449A, E2F2, CFL1, STMN1, ACVR1C, LGALS3, DNMT1, NEK7, TPPP2, DUSP2, MIR504, MIR485, ELL2, NT5C2, KLRK1, MIR200C, MIR203A, ZHX2, AKAP12, GDF3, KDM4A, MIR503, MIR212, WIF1, CEP57, HDAC4, MIR373, MIR340, FSTL1, MELK, NUP205, USP22, FBXW11, BRD4, MIR382, ATG5, MIR181A2, MIR181C, SH3BP4, MIR376A1, NUP62, CCNDBP1, BAG3, EI24, MIR184, BCAR1, CRB1, ZFPM2, H3P17, MIR188, MIR191, KLRC4-KLRK1, SRGAP2, MIR198, MIR19B1, ZEB2, CDC37, MIR223, TOPBP1, MIR330, MIR93, KHDRBS1, MVP, NUP153, ARID3B, MIR202, NKILA, RN7SL263P, THOC1, MTCO2P12, LOC110806263, UBE2C, ABCB6, MIR338, H3P13, DNM1L, PRMT5, APC2, AKAP8, MIR491, GPC6, ABCC4, CTCF, PANDAR, EBP, MIR34C, MIR221, MPZL2, MIR498, MIR25, COPS5, TMED10, CBX1, MED4-AS1, LYVE1, MIR29A, MIR320A, C1QL1, ZBTB5, SRCAP, MIR497, MIR495, MIR492, PTGES3, POU5F1P3, MIR433, BANCR, CADM1, CYTOR, AIPL1, CEMIP, KIF13A, BCORL1, CADM3, A2ML1, MIR758, EP400, PPM1K, MRTFA, MIR638, FEZF1-AS1, SCYL1, DANCR, CBLL2, TP73-AS1, KIF4A, RASSF6, DDX53, RALGAPB, MIR675, PNPLA2, TIGAR, MIR422A, PCBP4, TBCEL, HOXA11-AS, CADM2, PAG1, H19, PRDM16, SOX17, SMURF2, WNK1, MED23, SCGB3A1, POTEF, MIR655, KRT8P3, WNT3A, DIXDC1, EAF1, AZIN2, LRG1, PCAT4, PRAP1, CDCA7, RGPD2, ARHGAP24, CDT1, DRAM2, COL18A1, ULBP2, E2F8, LIN28A, ZNF329, SLCO6A1, MUL1, CDC73, PIWIL4, SLC25A23, CDKN2B-AS1, MIR665, PGP, LUCAT1, CBR3-AS1, TBPL2, ANAPC2, FAM238C, CD274, THORLNC, CCAT1, LINC01194, ATAD2, GTF2H5, MIRLET7B, MIR106A, MIR598, MIR125A, PDCD4, BBC3, MIR130B, MIR132, TCL6, CYFIP2, LATS2, MIR139, POU5F1P4, SIN3A, MICA, WWTR1, TMX2-CTNND1, KCNIP3, MIR3613, STX17, SOST, TMED10P1, MIR874, MIR365B, ZCCHC2, PGPEP1, TRPM7, OTUD4, RTEL1, LIN9, ARID4B, PIAS4, IL23A, CINP, TRIM59, GADL1, RBMY2DP, ENDO1, NOL7, MIR3163, GSTK1, MZB1, DCTN4, LINC00328, RBMY1D, PHF20L1, IL31, MIR3619, MIR448, AANAT, LIPG, HMGB2, GTF2H1, HDGF, HELLS, HIC1, HLA-A, HLF, HLA-G, HNF4A, GLI3, HOXB5, AGFG2, HSF1, HSPB1, HSPB2, HTR2A, ICAM1, GPI, GLI1, MMP2, FOXO3, F9, PTK2B, FANCB, FGF1, FGF9, FGF13, FGFR2, FOLR1, GLB1, FUT7, GAS6, GATA1, GDF10, GFAP, GHRHR, GJA3, ID2, IDH2, IFNG, LOX, LCP1, LDHA, LEP, LIG4, LMNB1, LMO2, LMO7, LY9, IGF1R, SMAD3, MCM6, MCM7, MEFV, MEN1, MFAP1, MLH1, LASP1, L1CAM, KRT19, KRT8, IGF2, IGF2R, IGFBP2, IL1A, IL1B, IL2, IL3, IL17A, INSM1, IRS1, ANOS1, CD82, KDR, KNG1, KPNA2, F3, EWSR1, EVPL, CCK, FOXL2, CAPN5, CA9, CASP5, CASP8, RUNX3, CBR3, CCND3, CDX1, CCNG1, TNFRSF8, CD40, CDC25A, CDC25B, CDH17, CDK9, BNIP3, BMP4, BCL6, BCL3, ABL1, ACY1, ADRB3, GRK3, JAG1, AGT, ALB, ALK, APEX1, APOC2, APOD, FAS, ASS1, ATRX, BAG1, CDKN2D, CEBPD, MECOM, ELAVL2, DCT, DDIT3, DDX3X, DDX5, DNMT3A, DNMT3B, DUSP1, ELF4, CETN2, ELK3, ENDOG, ENO1, ENO2, EPHB1, ERCC2, ESR2, DCC, DAXX, DAP, DAB1, CGA, CHRM3, CHRM5, CKS1B, CLU, PLK3, COX8A, CLDN7, CREBBP, CRHR2, CRYAB, CSE1L, CSF2, CTNND1, CXADR, MMP1, MMP3, ADIPOQ, TP73, TGFB2, TGFBI, TGFBR2, THBS1, THY1, TIAM1, TIMP1, TPM3, TFF2, TPO, TPT1, TRAF3, TYR, TYRO3, UBC, UBE2B, TG, TFDP1, MMP15, SST, SLPI, SNCG, SOAT1, SOD1, SOX4, ABCA4, SREBF1, STAT1, TFAP2B, STC1, TACR1, TBX1, TBX5, ZEB1, TCF19, TFAP2A, UCN, KDM6A, TRPV1, HSPB3, SUCLA2, CDK5R1, SQSTM1, SLC5A6, CCNA1, PHOX2B, MBD2, TRPA1, VRK1, PRC1, CLDN8, CLDN1, ARHGEF1, EXO1, PIWIL1, TRIP11, NAPG, FADD, TNFSF10, ADAM19, WEE1, WNT1, WNT10B, XPO1, XRCC4, KMT2D, XRS, SLC7A5, COIL, MKKS, CUL2, CASK, STC2, TP63, MBTPS1, SLC6A2, SLC5A5, SRSF3, PDE3B, NOTCH1, NPY, NOVA2, NPM1, NRF1, NTRK1, PRKN, PDGFA, PLAU, SLC26A4, PECAM1, PFDN4, PGF, PI3, PIGF, PLAG1, NOS2, NKTR, NGF, NFE2L1, MPG, MSN, MT1JP, MTAP, COX2, MTTP, MYB, MYCL, MYOD1, NCAM1, NEDD9, NEK2, NEUROG1, NF1, NF2, PLAGL1, PLXNA2, SATB1, BRD2, OPN1LW, REL, REG1A, UPF1, RET, TRIM27, RNASE3, ABCE1, POMC, ROS1, RPE, RPL34, RPS6KB1, RPS27A, RRAS, SAG, RBP2, RBP1, RBMY1A1, RBBP8, PON1, POU5F1, PPARD, PPP1CA, PTPA, PRB1, PRKCB, RELN, PSMD10, PTPN12, PVT1, RAD51, RARA, RASGRF1, KDM5A, SRC