-
X-Linked Alport Syndrome-Diffuse Leiomyomatosis
Orphanet
A rare renal disease characterized by the association of X-linked Alport syndrome (glomerular nephropathy, sensorineural deafness and ocular anomalies) and benign proliferation of visceral smooth muscle cells along the gastrointestinal, respiratory, and female genital tracts and clinically manifests with dysphagia, dyspnea, cough, stridor, postprandial vomiting, retrosternal or epigastric pain, recurrent pneumonia, and clitoral hypertrophy in females. Epidemiology Prevalence of X-linked Alport syndrome-diffuse leiomyomatosis (XLAS-DL) is unknown. ... Diagnostic methods X-linked Alport syndrome is suspected on clinical presentation and family history of hematuria, deafness and/or renal impairment, and is confirmed by genetic analysis of COL4 genes. ... Differential diagnosis The differential diagnosis regarding the combination of glomerular disease with deafness includes Fechtner syndrome, Epstein syndrome, MELAS and May-Hegglin thrombocytopenia.
-
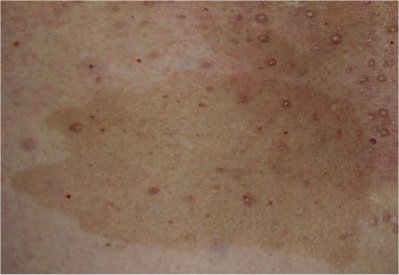
Neurofibromatosis Type 1
Orphanet
Familial spinal and segmental forms of NF1 have been described. Watson syndrome forms part of the NF1 spectrum. Neurofibromatosis-Noonan syndrome is a variant of NF1 in 99% of cases (see these terms). ... Molecular genetic testing can be requested but is mostly not needed. Differential diagnosis Legius syndrome (see this term) is often clinically indistinguishable from NF1 and is seen in about 2% of people fulfilling NF1 diagnostic criteria. There are however a small number of individuals with NF1 who like Legius syndrome patients do not develop non-pigmentary manifestations. Constitutional mismatch repair deficiency syndrome should be considered. Other differential diagnoses include McCune-Albright syndrome, Noonan syndrome with lentigines and Proteus syndrome.NF1, SPRED1, NF2, RASA1, CDKN2A, TP53, PTPN11, KIT, BRAF, RET, RGS6, PDGFRA, SDHD, MRC1, EGFR, VHL, PIK3CA, MAP2K7, SDHB, HRAS, MTOR, SUZ12, PTEN, SMUG1, GH1, MLH1, PIK3CG, PIK3CD, PIK3CB, ERBB2, PAK1, NRAS, EVI2A, APRT, MFAP1, KRAS, MSH6, EPHB2, OMG, DPYSL2, MSH2, GFAP, NGFR, MAPK1, BLVRB, THRA, ALK, S100B, IDH1, CXCL12, ATRX, HOXB2, CCND1, MDK, HGF, HOXB@, HOXB1, HOXB3, VCP, HOXB4, HOXB5, HOXB6, HOXB7, HOXB8, HOXB9, NGF, S100A1, RUNX1, TNFRSF11B, PMS2, EGF, BTF3P11, SPP1, CD38, NME1, CCL5, SDHC, TGFB1, SST, STAT3, PGR, LRRC37B, SOX9, CDKN2B-AS1, IDH2, UTP6, TPT1, MEN1, PACC1, KITLG, CD274, SGSM3, RNMT, MPZ, HTC2, TNF, EED, CXCR4, NFIC, NFIX, SMARCB1, H3P10, BMP2, CDC42, APOBEC1, EVI2B, BRCA1, ATM, FGFR1, BCL2, EPAS1, CRYBA1, HSF1, CTNNB1, BRCA2, PROM1, HSD17B6, IQGAP1, CCN5, AR, WASF1, PICALM, LRRC37A, SNAP91, OLIG2, SPRY1, MRVI1, CITED2, CIB1, CELF1, ALDH1L1, IKBKG, TNC, KMT2D, TOP2A, TFPI, TG, CAMP, CALM3, THY1, TIA1, TIAL1, CALM2, TNXB, TOP1, CALM1, FGF23, TSC2, TTN, TYK2, USF1, VARS1, VDR, VEGFB, BMPR1A, ZMYM2, IMMT, METAP2, TLK2, SDS, LRRC37A3, RNF135, FHDC1, DNER, AMPD1, ESCO1, NMS, RSS, AKT1, THSD7A, HSR, MEX3D, ATAD5, MIR10B, MIR125A, MIR204, NF1P2, LRRC37A2, KIR2DL5B, MIR641, ADM, DUX4, NF1P1, DHDDS, TBL1XR1, TCP1, LRRC37A4P, RASSF1, ZHX2, CIC, SHROOM2, APP, PRPF31, CNNM4, HIPK2, APOB, BCL11A, CRTAC1, KMT2C, BIRC5, FBXW7, ADAP2, ANPEP, CHPT1, KIR2DL5A, RPTOR, KIAA1549, RNF213, LSM2, TERT, CD14, CNTN2, CCN3, G6PD, FOLH1, MYH2, FN1, FMR1, NFIA, NFIB, FOXG1, FH, FAP, ETV5, TBX1, NTRK3, ESR1, EREG, SERPINE1, ERBB4, PAX6, PAX7, EPHB1, PGD, PGF, GC, MMP13, GDNF, MGMT, GSTP1, IGF1R, CCN1, CXCL10, JAK2, GRN, GNRH1, LBR, LIF, MXD1, SMAD1, SMAD4, MAF, MAGEB2, MATN2, MCAM, GNA12, MDM2, GLI1, GHSR, GHR, ENO2, ADCY8, ELK3, RPS6KB1, CREB1, SCN5A, CRABP2, CGA, CFTR, CEL, CEBPD, SH3BP2, SKI, SLC6A2, SLC6A4, SMARCA2, CDKN1B, SMS, SORD, SOS1, CDK4, SOX10, SRY, CD19, AURKA, RYR1, RPS6KA1, EIF4EBP1, RHEB, PKD1, PLG, SERPINF2, PMP22, DUSP6, PNMT, POMC, PTPA, PRKAR1A, DUSP1, MAPK3, MAPK8, SARDH, PTCH1, DIAPH2, PTN, DACH1, PTPRC, RAF1, RASA2, CSF3, ASIC2
-
Cerebral Vasculitis
Wikipedia
External links [ edit ] Classification D ICD - 10 : I67.7 ICD - 9-CM : 437.4 MeSH : D020293 SNOMED CT : 427020007 v t e Cerebrovascular diseases including stroke Ischaemic stroke Brain Anterior cerebral artery syndrome Middle cerebral artery syndrome Posterior cerebral artery syndrome Amaurosis fugax Moyamoya disease Dejerine–Roussy syndrome Watershed stroke Lacunar stroke Brain stem Brainstem stroke syndrome Medulla Medial medullary syndrome Lateral medullary syndrome Pons Medial pontine syndrome / Foville's Lateral pontine syndrome / Millard-Gubler Midbrain Weber's syndrome Benedikt syndrome Claude's syndrome Cerebellum Cerebellar stroke syndrome Extracranial arteries Carotid artery stenosis precerebral Anterior spinal artery syndrome Vertebrobasilar insufficiency Subclavian steal syndrome Classification Brain ischemia Cerebral infarction Classification Transient ischemic attack Total anterior circulation infarct Partial anterior circulation infarct Other CADASIL Binswanger's disease Transient global amnesia Haemorrhagic stroke Extra-axial Epidural Subdural Subarachnoid Cerebral/Intra-axial Intraventricular Brainstem Duret haemorrhages General Intracranial hemorrhage Aneurysm Intracranial aneurysm Charcot–Bouchard aneurysm Other Cerebral vasculitis Cerebral venous sinus thrombosis
-
Dicentric Chromosome
Wikipedia
Tailed nuclei are signatures of radiation exposure in human tissue, microbiota , and aquatic invertebrates from the wake of recent nuclear disasters. [5] Additionally, they are used as potential biomarkers to screen for certain genetic syndromes present in human populations. [3] Pseudodicentric chromosomes Dicentric chromosomes may lead to pseudodicentric mutations, in which one of the centromeres on the chromosome becomes inactivated. [1] This can have severe clinical consequences for patients, as observed in severe progressive neurological and intellectual disorders [11] such as Kabuki syndrome , a pediatric congenital disorder. [3] Kabuki syndrome is one of the most widely studied syndromes that involve the pseudodicentric chromosome. [3] Other characterized syndromes have also been linked to pseudodicentric chromosomes, such as Edwards syndrome , [12] a trisomy of chromosome 18, and Turner syndrome , [13] a loss (or partial loss) of the X chromosome. Pseudodicentric chromosomes alone do not define these syndromes, because the contribution of other chromosomal abnormalities are also considered, such as the presence of isochromosomes in Turner patients. [13] See also [ edit ] Chromosomal inversion Telomeres Cytogenetics Nuclear radiation Intellectual disorders References [ edit ] ^ a b c d e f Nussbaum, Robert; McInnes, Roderick; Willard, Huntington; Hamosh, Ada (2007). ... ISBN 9780073525266 . ^ a b c d e Lynch, Sally; et al. (1995). "Kabuki syndrome-like features in monozygotic twin boys with a pseudodicentric chromosome 13" . ... PMID 2685311 . ^ Gravholt, Claus Højbjerg; Bugge, Merete; Strømkjær, Helle; Caprani, Monna; Henriques, Ulrik; Petersen, Michael B.; Brandt, Carsten A. (1997-07-01). "A patient with Edwards syndrome caused by a rare pseudodicentric chromosome 18 of paternal origin". ... "Microsatellite analysis in Turner syndrome: Parental origin of X chromosomes and possible mechanism of formation of abnormal chromosomes".
-
T Cell Deficiency
Wikipedia
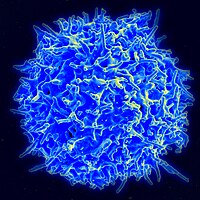
T cell deficiency Human T Cell Specialty Immunology Symptoms Eczematous [1] Types Primary or Secondary [2] Diagnostic method Delayed hypersensitivity skin test, T cell count [1] [3] [4] Treatment Bone marrow transplant, Immunoglobulin replacement [1] [2] T cell deficiency is a deficiency of T cells , caused by decreased function of individual T cells, it causes an immunodeficiency of cell-mediated immunity . [1] T cells normal function is to help with the human body's immunity, they are one of the two primary types of lymphocytes(the other being B cells ). [ medical citation needed ] Contents 1 Symptoms and signs 2 Mechanism 2.1 Pathogens of concern 3 Diagnosis 3.1 Types 3.1.1 Primary or secondary 3.1.1.1 Complete or partial deficiency 4 Treatment 4.1 Epidemiology 5 See also 6 References 7 Further reading 8 External links Symptoms and signs [ edit ] Presentations differ among causes, but T cell insufficiency generally manifests as unusually severe common viral infections ( respiratory syncytial virus , rotavirus ), diarrhea , and eczematous or erythrodermatous rashes. [1] Failure to thrive and cachexia are later signs of a T-cell deficiency. [1] Mechanism [ edit ] In terms of the normal mechanism of T cell we find that it is a type of white blood cell that has an important role in immunity, and is made from thymocytes [5] One sees in the partial disorder of T cells that happen due to cell signaling defects, are usually caused by hypomorphic gene defects [6] Generally, (micro)deletion of 22Q11.2 is the most often seen. [7] Pathogens of concern [ edit ] Further information: Intracellular pathogen The main pathogens of concern in T cell deficiencies are intracellular pathogens , including Herpes simplex virus , Mycobacterium and Listeria . [8] Also, intracellular fungal infections are also more common and severe in T cell deficiencies. [8] Other intracellular pathogens of major concern in T cell deficiency are: Mycobacterium avium intracellulare [9] Salmonella species [9] Rhodococcus equi [9] Pneumocystis jirovecii [9] Toxoplasma gondii [9] Cryptosporidium parvum [9] Leishmania species [9] Herpesviridae ( herpes simplex , cytomegalovirus and varicella zoster ) [9] Cryptococcus neoformans [9] Histoplasma capsulatum [9] Diagnosis [ edit ] The diagnosis of T cell deficiency can be ascertained in those individuals with this condition via the following: [1] [4] [3] Delayed hypersensitivity skin test T cell count Detection via culture(infection) Types [ edit ] Primary or secondary [ edit ] Primary (or hereditary) immunodeficiencies of T cells include some that cause complete insufficiency of T cells, such as severe combined immunodeficiency (SCID), Omenn syndrome , and Cartilage–hair hypoplasia . [1] Lymphoma Secondary causes are more common than primary ones. [9] Secondary (or acquired) causes are mainly: [9] AIDS Cancer chemotherapy Lymphoma Glucocorticoid therapy Complete or partial deficiency [ edit ] Complete insufficiency of T cell function can result from hereditary conditions (also called primary conditions) such as severe combined immunodeficiency (SCID), Omenn syndrome , and cartilage–hair hypoplasia . [1] Partial insufficiencies of T cell function include acquired immune deficiency syndrome (AIDS), and hereditary conditions such as DiGeorge syndrome (DGS), chromosomal breakage syndromes (CBSs), and B-cell and T-cell combined disorders such as ataxia-telangiectasia (AT) and Wiskott–Aldrich syndrome (WAS). [1] Treatment [ edit ] Harvested bone marrow in preparation for transplant In terms of the management of T cell deficiency for those individuals with this condition the following can be applied: [2] [1] Killed vaccines should be used(not live vaccines in T cell deficiency) Bone marrow transplant Immunoglobulin replacement Antiviral therapy Supplemental nutrition Epidemiology [ edit ] In the U.S. this defect occurs in about 1 in 70,000, with the majority of cases presenting in early life. [1] Furthermore, SCID has an incidence of approximately 1 in 66,000 in California [10] See also [ edit ] B cell deficiency References [ edit ] ^ a b c d e f g h i j k l Medscape > T-cell Disorders . ... External links [ edit ] Pubmed Classification D ICD - 10 : D84.8 , ICD - 9-CM : 279.3 Scholia has a topic profile for T cell deficiency . v t e Lymphoid and complement disorders causing immunodeficiency Primary Antibody / humoral ( B ) Hypogammaglobulinemia X-linked agammaglobulinemia Transient hypogammaglobulinemia of infancy Dysgammaglobulinemia IgA deficiency IgG deficiency IgM deficiency Hyper IgM syndrome ( 1 2 3 4 5 ) Wiskott–Aldrich syndrome Hyper-IgE syndrome Other Common variable immunodeficiency ICF syndrome T cell deficiency ( T ) thymic hypoplasia : hypoparathyroid ( Di George's syndrome ) euparathyroid ( Nezelof syndrome Ataxia–telangiectasia ) peripheral: Purine nucleoside phosphorylase deficiency Hyper IgM syndrome ( 1 ) Severe combined (B+T) x-linked: X-SCID autosomal: Adenosine deaminase deficiency Omenn syndrome ZAP70 deficiency Bare lymphocyte syndrome Acquired HIV/AIDS Leukopenia : Lymphocytopenia Idiopathic CD4+ lymphocytopenia Complement deficiency C1-inhibitor ( Angioedema / Hereditary angioedema ) Complement 2 deficiency / Complement 4 deficiency MBL deficiency Properdin deficiency Complement 3 deficiency Terminal complement pathway deficiency Paroxysmal nocturnal hemoglobinuria Complement receptor deficiency v t e Medicine Specialties and subspecialties Surgery Cardiac surgery Cardiothoracic surgery Colorectal surgery Eye surgery General surgery Neurosurgery Oral and maxillofacial surgery Orthopedic surgery Hand surgery Otolaryngology ENT Pediatric surgery Plastic surgery Reproductive surgery Surgical oncology Transplant surgery Trauma surgery Urology Andrology Vascular surgery Internal medicine Allergy / Immunology Angiology Cardiology Endocrinology Gastroenterology Hepatology Geriatrics Hematology Hospital medicine Infectious disease Nephrology Oncology Pulmonology Rheumatology Obstetrics and gynaecology Gynaecology Gynecologic oncology Maternal–fetal medicine Obstetrics Reproductive endocrinology and infertility Urogynecology Diagnostic Radiology Interventional radiology Nuclear medicine Pathology Anatomical Clinical pathology Clinical chemistry Cytopathology Medical microbiology Transfusion medicine Other Addiction medicine Adolescent medicine Anesthesiology Dermatology Disaster medicine Diving medicine Emergency medicine Mass gathering medicine Family medicine General practice Hospital medicine Intensive care medicine Medical genetics Narcology Neurology Clinical neurophysiology Occupational medicine Ophthalmology Oral medicine Pain management Palliative care Pediatrics Neonatology Physical medicine and rehabilitation PM&R Preventive medicine Psychiatry Addiction psychiatry Radiation oncology Reproductive medicine Sexual medicine Sleep medicine Sports medicine Transplantation medicine Tropical medicine Travel medicine Venereology Medical education Medical school Bachelor of Medicine, Bachelor of Surgery Bachelor of Medical Sciences Master of Medicine Master of Surgery Doctor of Medicine Doctor of Osteopathic Medicine MD–PhD Related topics Alternative medicine Allied health Dentistry Podiatry Pharmacy Physiotherapy Molecular oncology Nanomedicine Personalized medicine Public health Rural health Therapy Traditional medicine Veterinary medicine Physician Chief physician History of medicine Book Category Commons Wikiproject Portal Outline
-
Sundowning
Wikipedia
For other uses, see Sundowning (disambiguation) . Sundowning , or sundown syndrome , [1] is a neurological phenomenon associated with increased confusion and restlessness in patients with delirium or some form of dementia . Most commonly associated with Alzheimer's disease , but also found in those with other forms of dementia, the term "sundowning" was coined due to the timing of the patient's confusion. For patients with sundowning syndrome, a multitude of behavioral problems begin to occur in the evening or while the sun is setting. [2] [3] [4] Sundowning seems to occur more frequently during the middle stages of Alzheimer's disease and mixed dementia. ... International Journal of Geriatric Psychiatry . 25 (12): 1201–08. doi : 10.1002/gps.2454 . ^ "Il demente e la sindrome del tramonto" [The demented and the sunset syndrome]. anzianievita.it (in Italian). ... Web. 14 May 2012. http://www.webmd.com/alzheimers/guide/sundowning-causes-symptoms-treatments ^ Khachiyants N, Trinkle D, Son SJ, Kim KY (2011). "Sundown syndrome in persons with dementia: an update" . ... www.universiteitvannederland.nl . v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Ménétrier's Disease
Wikipedia
Diffuse or patchy glandular atrophy, evident as hypoplasia of parietal and chief cells, is typical. [4] Although ICD-10 classifies it under "Other gastritis" ( K29.6 ), and the lamina propria may contain mild chronic inflammatory infiltrate, Ménétrier disease is not considered a form of gastritis. [3] It is rather considered as one of the two most well understood hypertrophic gastropathies; the other being Zollinger–Ellison syndrome . [4] Diagnosis [ edit ] CT abdomen, coronal section, showing characteristic large rugal folds in the stomach. ... Other possible causes (eg differential diagnosis) of large folds within the stomach include: Zollinger-Ellison syndrome, cancer , infection ( cytomegalovirus /CMV, histoplasmosis , syphilis ), and infiltrative disorders such as sarcoidosis . [3] Treatment [ edit ] Cetuximab is the first-line therapy for Ménétrier disease. [2] Cetuximab is a monoclonal antibody against epidermal growth factor receptor (EGFR), and has been shown to be effective in treating Ménétrier disease. [6] Several medications have been used in the treatment of the condition, with variable efficacy. ... External links [ edit ] Classification D ICD - 10 : K29.6 ICD - 9-CM : 535.2 OMIM : 137280 MeSH : D005758 DiseasesDB : 8001 External resources Orphanet : 2494 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Microdontia
Wikipedia
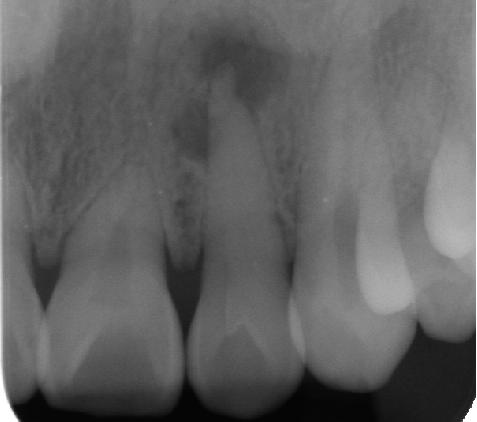
A single tooth is smaller than normal. [3] Localized microdontia is far more common than generalized microdontia, [2] and is often associated with hypodontia (reduced number of teeth). [1] The most commonly involved tooth in localized microdontia is the maxillary lateral incisor, which may also be shaped like an inverted cone (a "peg lateral"). [3] Peg laterals typically occur on both sides, [2] and have short roots. [2] Inheritance may be involved, [2] and the frequency of microdontia in the upper laterals is just under 1%. [1] The second most commonly involved tooth is the maxillary third molars, [3] and after this supernumerary teeth . [3] Causes [ edit ] There are many potential factors involved. [4] Congenital hypopituitarism [1] Ectodermal dysplasia [1] Down syndrome [1] Ionizing radiation to the jaws during tooth development ( odontogenesis ) [1] Chemotherapy during tooth development [4] Marshall syndrome [4] Rieger syndrome [4] Focal dermal hypoplasia [4] Silver-Russell syndrome [4] Williams syndrome [4] Gorlin-Chaudhry-Moss syndrome [4] Coffin–Siris syndrome [4] Salamon syndrome [4] Cleft lip and palate [4] Others include trichorhinopharyngeal, odontotrichomelic, neuroectodermal and dermo-odontodysplasia syndromes. [4] Treatment [ edit ] Unerupted microdonts may require surgical removal to prevent the formation of cysts . [2] Erupted microdonts, peg laterals especially, may cause cosmetic concern. ... External links [ edit ] Classification D ICD - 10 : K00.2 ICD - 9-CM : 520.2 DiseasesDB : 35076 v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic diseaseFGF3, WNT10B, PAX9, TRPS1, WNT10A, TBL2, B3GAT3, WHRN, ATP6V0A2, KAT6B, PLXND1, CHSY1, EDAR, WDR4, SEC23A, IFT140, SMARCAL1, GTF2IRD1, PIGL, CHST3, EIF2AK3, RECQL4, BAZ1B, TP63, AXIN2, KMT2D, PCGF2, SLC25A24, KDM6A, MLXIPL, CLIP2, UBR1, CKAP2L, DNAJC21, EVC2, EDARADD, TWIST2, IFT43, UBE3B, ADGRV1, PDZD7, EFL1, BCL11B, EDA2R, WDR19, WDR35, ARID1B, MCOLN1, CCDC47, IFT122, NHP2, NOP10, DYNC2LI1, SBDS, IFT52, HEPHL1, AMELX, EVC, LIMK1, IRF6, IDUA, GTF2I, GLI1, GJA1, GHR, FOXC1, FGFR1, EYA1, ELN, LTBP3, EDA, DLX3, COL5A2, COL5A1, COL3A1, COL1A1, CDH3, CACNA1C, C1S, C1R, USH2A, LRP6, MSX1, MYO7A, SUMO1, TGFA, TFAP2A, SRP54, SIX1, RFC2, REV3L, DPF2, RBBP8, RAP1B, RAP1A, NECTIN1, PRKD1, PITX2, PIK3R1, PIGA, PCNT, P4HB, ORC1, SMOC2, TBX1, GREM2, TFAP2B, LAMA2, ABCA4
-
Unibrow
Wikipedia
A unibrow is a recognized feature of Cornelia De Lange syndrome , a genetic disorder whose main features include moderate to severe learning difficulties, limb abnormalities such as oligodactyly (fewer than normal fingers or toes) and phocomelia (malformed limbs), and facial abnormalities including a long philtrum (the slight depression/line between the nose and mouth). Other medical conditions associated with a unibrow include: Waardenburg syndrome ; Patau syndrome ; Smith-Lemli-Opitz syndrome ; Sanfilippo syndrome ; 3p deletion syndrome ; [16] Chromosome Deletion Dillan 4p Syndrome ( Wolf–Hirschhorn syndrome ); Gorlin syndrome (Basal Cell Nevus Syndrome); Cornelia de Lange Syndrome Frontometaphyseal dysplasia ; ATRX syndrome ; Chromosome 9q34 Microdeletion Syndrome or Kleefstra syndrome . ... Retrieved 2018-08-27 . ^ "Chromosome 3p- syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program" . rarediseases.info.nih.gov .ASXL3, ATP6V1B2, LEMD3, WNT4, NANS, WAC, CDON, KCNK4, SLC25A24, ANKRD11, ZBTB20, KIFBP, SETBP1, NIPBL, PIGN, NSUN2, ABCA5, PACS2, PHF8, IQSEC2, DHX30, CHSY1, ERLIN2, IL1RAPL1, POLR3A, RAI1, DEAF1, TMCO1, PHIP, ABCC9, SETD5, ASXL1, ARX, FREM1, KCTD7, HGSNAT, UQCC2, UTP23, TRAPPC9, GPR101, TTI2, EHMT1, ROGDI, THOC6, VPS33A, XYLT1, KNL1, CCDC47, KLHL7, HDAC8, MBD5, PACS1, TRMT1, CWF19L1, CERT1, GNE, BMP2, GJB2, KMT2A, MITF, MEFV, MAB21L1, KIT, KCNH1, IGF1R, HSPA9, HNRNPU, GRIN2B, GNS, FLII, NFIX, FHL1, FGFR2, FGFR1, FGF3, BPTF, EDNRB, EDN3, CSNK2A1, CREBBP, CDH11, CDC42, NAGLU, NOTCH2, RUSC2, TRIO, TMEM94, SMC3, AIP, EED, CDK10, CUL4B, SMC1A, HMGA2, ZNF711, ZIC2, UBE2A, TALDO1, PAX3, TAF6, TAF1, SOX10, SMS, SNAI2, SGSH, RAD21, NECTIN1, PSMD12, PPP2R1A, PMM2, EBF3
-
Macroglossia
Wikipedia
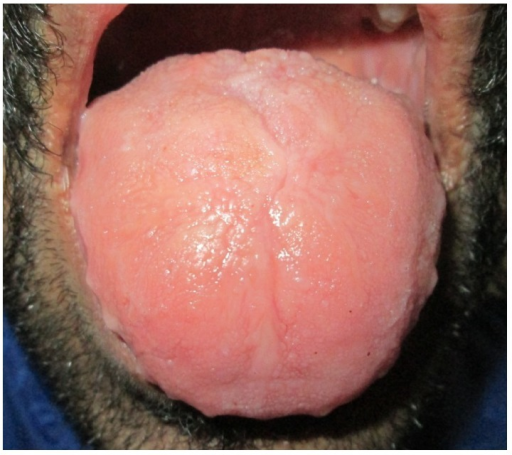
Apparent macroglossia can also occur in Down syndrome . [8] The tongue has a papillary, fissured surface. [3] Macroglossia may be a sign of hypothyroid disorders . Other causes include mucopolysaccharidosis , [9] neurofibromatosis , [3] multiple endocrine neoplasia type 2B, [3] myxedema , [3] acromegaly , [3] angioedema , [3] tumors (e.g. carcinoma ), [3] Glycogen storage disease type 2, [10] Simpson-Golabi-Behmel syndrome , [5] [11] Triploid Syndrome , [ medical citation needed ] trisomy 4p , [ medical citation needed ] fucosidosis , [ medical citation needed ] alpha-mannosidosis , [12] Klippel-Trenaunay-Weber syndrome , [5] cardiofaciocutaneous syndrome , [5] Ras pathway disorders, [5] transient neonatal diabetes , [5] and lingual thyroid . [13] Diagnosis [ edit ] Macroglossia is usually diagnosed clinically. [4] Sleep endoscopy and imaging may be used for assessment of obstructive sleep apnea. [2] The initial evaluation of all patients with macroglossia may involve abdominal ultrasound and molecular studies for Beckwith–Wiedemann syndrome. [5] Classification [ edit ] The ICD-10 lists macroglossia under "other congenital malformations of the digestive system". ... "Treatment of macroglossia in a child with Beckwith–Wiedemann syndrome". Journal of Oral and Maxillofacial Surgery . 58 (9): 1058–61. doi : 10.1053/joms.2000.8753 . ... "Relative rather than absolute macroglossia in patients with Down syndrome: implications for treatment of obstructive sleep apnea". ... S2CID 22012119 . ^ "Mucopolysaccharidosis type I" . ^ http://moon.ouhsc.edu/kfung/jty1/neurohelp/ZNN0IE23.htm ^ "Omim - Simpson-Golabi-Behmel Syndrome, Type 1; Sgbs1 - Omim - Ncbi" . ^ "Omim - Mannosidosis, Alpha B, Lysosomal; Mansa - Omim - Ncbi" . ^ Cawson, R.H19-ICR, MED13L, CDKN1C, LARGE1, SETBP1, ERLIN2, KCNQ1OT1, TRAF3IP2, POMT1, SEC23B, PQBP1, ABCC9, ZBTB24, IFT140, GTF2IRD1, FIBP, GMPPB, AIP, BAZ1B, CUL4B, ARID1A, PAX8, WNT5A, CLIP2, UBE3A, TSHR, TSHB, TRHR, TBL2, POMT2, NKX2-1, EHMT1, KLLN, CRPPA, DUOXA2, IYD, PIGW, H19, FDX2, PIGS, POMK, CDCA7, GPR101, SNIP1, DUOX2, GNPTAB, FKRP, FTO, ALG8, VPS33A, HYMAI, CCDC47, INPP5E, TRMU, POMGNT1, RNF125, TPO, ACTB, AGA, FOXE1, IGF2, IDUA, IDS, HRAS, HEXB, HELLS, GTF2I, GPC3, GATA1, GAA, FUCA1, FOXG1, THRA, GPC4, ELN, DVL3, DVL1, DNMT3B, NKX2-5, ATRX, ATP6V1B2, ARSB, AMPD2, AKT1, KCNH1, KCNQ1, LAMA2, LIMK1, TG, SMARCB1, SMARCA4, SLC5A5, SGCG, SDHD, SDHC, SDHB, RFC2, PTEN, PSMB8, MAP2K1, POU1F1, PLAGL1, PIK3CA, PIK3C2A, PEX1, SLC26A4, ROR2, TRNW, TRNE, MAN2B1, THRB, SPRY2, CTSC, NT5E, HTC2
-
Saddle Nose
Wikipedia
. ^ Saddle Nose Rhinoplasty at eMedicine External links [ edit ] Classification D ICD - 10 : A50.5, M95.0, Q67.4 ICD - 9-CM : 090.5 , 754.0 DiseasesDB : 11755 v t e Proteobacteria -associated Gram-negative bacterial infections α Rickettsiales Rickettsiaceae / ( Rickettsioses ) Typhus Rickettsia typhi Murine typhus Rickettsia prowazekii Epidemic typhus , Brill–Zinsser disease , Flying squirrel typhus Spotted fever Tick-borne Rickettsia rickettsii Rocky Mountain spotted fever Rickettsia conorii Boutonneuse fever Rickettsia japonica Japanese spotted fever Rickettsia sibirica North Asian tick typhus Rickettsia australis Queensland tick typhus Rickettsia honei Flinders Island spotted fever Rickettsia africae African tick bite fever Rickettsia parkeri American tick bite fever Rickettsia aeschlimannii Rickettsia aeschlimannii infection Mite-borne Rickettsia akari Rickettsialpox Orientia tsutsugamushi Scrub typhus Flea-borne Rickettsia felis Flea-borne spotted fever Anaplasmataceae Ehrlichiosis : Anaplasma phagocytophilum Human granulocytic anaplasmosis , Anaplasmosis Ehrlichia chaffeensis Human monocytotropic ehrlichiosis Ehrlichia ewingii Ehrlichiosis ewingii infection Rhizobiales Brucellaceae Brucella abortus Brucellosis Bartonellaceae Bartonellosis : Bartonella henselae Cat-scratch disease Bartonella quintana Trench fever Either B. henselae or B. quintana Bacillary angiomatosis Bartonella bacilliformis Carrion's disease , Verruga peruana β Neisseriales M+ Neisseria meningitidis/meningococcus Meningococcal disease , Waterhouse–Friderichsen syndrome , Meningococcal septicaemia M− Neisseria gonorrhoeae/gonococcus Gonorrhea ungrouped: Eikenella corrodens / Kingella kingae HACEK Chromobacterium violaceum Chromobacteriosis infection Burkholderiales Burkholderia pseudomallei Melioidosis Burkholderia mallei Glanders Burkholderia cepacia complex Bordetella pertussis / Bordetella parapertussis Pertussis γ Enterobacteriales ( OX− ) Lac+ Klebsiella pneumoniae Rhinoscleroma , Pneumonia Klebsiella granulomatis Granuloma inguinale Klebsiella oxytoca Escherichia coli : Enterotoxigenic Enteroinvasive Enterohemorrhagic O157:H7 O104:H4 Hemolytic-uremic syndrome Enterobacter aerogenes / Enterobacter cloacae Slow/weak Serratia marcescens Serratia infection Citrobacter koseri / Citrobacter freundii Lac− H2S+ Salmonella enterica Typhoid fever , Paratyphoid fever , Salmonellosis H2S− Shigella dysenteriae / sonnei / flexneri / boydii Shigellosis , Bacillary dysentery Proteus mirabilis / Proteus vulgaris Yersinia pestis Plague / Bubonic plague Yersinia enterocolitica Yersiniosis Yersinia pseudotuberculosis Far East scarlet-like fever Pasteurellales Haemophilus : H. influenzae Haemophilus meningitis Brazilian purpuric fever H. ducreyi Chancroid H. parainfluenzae HACEK Pasteurella multocida Pasteurellosis Actinobacillus Actinobacillosis Aggregatibacter actinomycetemcomitans HACEK Legionellales Legionella pneumophila / Legionella longbeachae Legionnaires' disease Coxiella burnetii Q fever Thiotrichales Francisella tularensis Tularemia Vibrionaceae Vibrio cholerae Cholera Vibrio vulnificus Vibrio parahaemolyticus Vibrio alginolyticus Plesiomonas shigelloides Pseudomonadales Pseudomonas aeruginosa Pseudomonas infection Moraxella catarrhalis Acinetobacter baumannii Xanthomonadaceae Stenotrophomonas maltophilia Cardiobacteriaceae Cardiobacterium hominis HACEK Aeromonadales Aeromonas hydrophila / Aeromonas veronii Aeromonas infection ε Campylobacterales Campylobacter jejuni Campylobacteriosis , Guillain–Barré syndrome Helicobacter pylori Peptic ulcer , MALT lymphoma , Gastric cancer Helicobacter cinaedi Helicobacter cellulitis v t e Diseases of joints General Arthritis Monoarthritis Oligoarthritis Polyarthritis Symptoms Joint pain Joint stiffness Inflammatory Infectious Septic arthritis Tuberculosis arthritis Crystal Chondrocalcinosis CPPD (Psudogout) Gout Seronegative Reactive arthritis Psoriatic arthritis Ankylosing spondylitis Other Juvenile idiopathic arthritis Rheumatoid arthritis Felty's syndrome Palindromic rheumatism Adult-onset Still's disease Noninflammatory Hemarthrosis Osteoarthritis Heberden's node Bouchard's nodes Osteophyte v t e Congenital malformations and deformations of musculoskeletal system / musculoskeletal abnormality Appendicular limb / dysmelia Arms clavicle / shoulder Cleidocranial dysostosis Sprengel's deformity Wallis–Zieff–Goldblatt syndrome hand deformity Madelung's deformity Clinodactyly Oligodactyly Polydactyly Leg hip Hip dislocation / Hip dysplasia Upington disease Coxa valga Coxa vara knee Genu valgum Genu varum Genu recurvatum Discoid meniscus Congenital patellar dislocation Congenital knee dislocation foot deformity varus Club foot Pigeon toe valgus Flat feet Pes cavus Rocker bottom foot Hammer toe Either / both fingers and toes Polydactyly / Syndactyly Webbed toes Arachnodactyly Cenani–Lenz syndactylism Ectrodactyly Brachydactyly Stub thumb reduction deficits / limb Acheiropodia Ectromelia Phocomelia Amelia Hemimelia multiple joints Arthrogryposis Larsen syndrome RAPADILINO syndrome Axial Skull and face Craniosynostosis Scaphocephaly Oxycephaly Trigonocephaly Craniofacial dysostosis Crouzon syndrome Hypertelorism Hallermann–Streiff syndrome Treacher Collins syndrome other Macrocephaly Platybasia Craniodiaphyseal dysplasia Dolichocephaly Greig cephalopolysyndactyly syndrome Plagiocephaly Saddle nose Vertebral column Spinal curvature Scoliosis Klippel–Feil syndrome Spondylolisthesis Spina bifida occulta Sacralization Thoracic skeleton ribs : Cervical Bifid sternum : Pectus excavatum Pectus carinatum This article about a disease of musculoskeletal and connective tissue is a stub .
-
Dejerine–sottas Disease
Wikipedia
Dejerine–Sottas syndrome Other names Dejerine–Sottas syndrome Specialty Neurology Dejerine–Sottas disease , also known as, Dejerine–Sottas neuropathy , progressive hypertrophic interstitial polyneuropathy of childhood and onion bulb neuropathy [1] (and, hereditary motor and sensory polyneuropathy type III and Charcot–Marie–Tooth disease type 3 ), is a hereditary neurological disorder characterised by damage to the peripheral nerves and resulting progressive muscle wasting. ... S2CID 2512684 . ^ Roa BB, Dyck PJ, Marks HG, Chance PF, Lupski JR (November 1993). "Dejerine-Sottas syndrome associated with point mutation in the peripheral myelin protein 22 (PMP22) gene". ... External links [ edit ] Classification D ICD - 10 : G60.0 ICD - 9-CM : 356.0 OMIM : 145900 MeSH : D015417 DiseasesDB : 5821 v t e Diseases relating to the peripheral nervous system Mononeuropathy Arm median nerve Carpal tunnel syndrome Ape hand deformity ulnar nerve Ulnar nerve entrapment Froment's sign Ulnar tunnel syndrome Ulnar claw radial nerve Radial neuropathy Wrist drop Cheiralgia paresthetica long thoracic nerve Winged scapula Backpack palsy Leg lateral cutaneous nerve of thigh Meralgia paraesthetica tibial nerve Tarsal tunnel syndrome plantar nerve Morton's neuroma superior gluteal nerve Trendelenburg's sign sciatic nerve Piriformis syndrome Cranial nerves See Template:Cranial nerve disease Polyneuropathy and Polyradiculoneuropathy HMSN Charcot–Marie–Tooth disease Dejerine–Sottas disease Refsum's disease Hereditary spastic paraplegia Hereditary neuropathy with liability to pressure palsy Familial amyloid neuropathy Autoimmune and demyelinating disease Guillain–Barré syndrome Chronic inflammatory demyelinating polyneuropathy Radiculopathy and plexopathy Brachial plexus injury Thoracic outlet syndrome Phantom limb Other Alcoholic polyneuropathy Other General Complex regional pain syndrome Mononeuritis multiplex Peripheral neuropathy Neuralgia Nerve compression syndrome v t e Cell membrane protein disorders (other than Cell surface receptor , enzymes , and cytoskeleton ) Arrestin Oguchi disease 1 Myelin Pelizaeus–Merzbacher disease Dejerine–Sottas disease Charcot–Marie–Tooth disease 1B, 2J Pulmonary surfactant Surfactant metabolism dysfunction 1, 2 Cell adhesion molecule IgSF CAM : OFC7 Cadherin : DSG1 Striate palmoplantar keratoderma 1 DSG2 Arrhythmogenic right ventricular dysplasia 10 DSG4 LAH1 DSC2 Arrhythmogenic right ventricular dysplasia 11 Integrin : cell surface receptor deficiencies Tetraspanin TSPAN7 X-Linked mental retardation 58 TSPAN12 Familial exudative vitreoretinopathy 5 Other KIND1 Kindler syndrome HFE HFE hereditary haemochromatosis DYSF Distal muscular dystrophy Limb-girdle muscular dystrophy 2B See also other cell membrane proteinsPMP22, MPZ, EGR2, PRX, GJB1, AMACR, RFC1, KIF1B, NEFL, COX6A1, MTMR2, GARS1, FIG4, MFN2, SLC12A6, NDRG1, DYNC1H1, GDAP1, DHTKD1, SH3TC2, SBF2, LRSAM1, LMNA, FGD4, COL2A1, TNF, RNMT, IL10, IL6, MPO, IL1B, IL17A, PTGS2, MAD2L1BP, IFNG, HLA-A, PLCE1, CCL2, GABPA, NR0B1, NFE2L2, PLAU, TLR2, COX2, TAP1, GORASP1, WNK1, NLRP3, SYT1, RBM45, RELA, OCLN, S100A9, MTCO2P12, CBLIF, BCL2, HLA-DRB1, CTNNB1, CASP3, CXCL1, CBFA2T3, FGL2, DSTN, RIPK3, DUSP10, HP, RUNX1, HPSE, SIRT1, ZNF281, SEC14L2, RUNX2, NOX1, LPIN1, IGF2BP1, NOX4, IVNS1ABP, NXF1, TLR6, ENTPD1, TNFSF15, CD68, CDH1, CHRM3, SCAF11, CLDN2, CMA1, PILRA, IL23A, ANGPTL4, CAT, LINC02210-CRHR1, RAB4B-EGLN2, ANGPT2, MIR146B, MIR155, IMMP1L, ARG1, ARNTL, IL17F, EGLN2, BCL3, KLF5, HM13, ZBP1, TSPO, TRPM8, C3, IL25, VPS51, TPSB2, CALCA, MRTFA, MYDGF, CASP1, CLDN4, NR1I2, USO1, SOCS1, MMP10, ESR1, PLCB4, PTK2B, ABCB1, NTRK1, NFKBIA, FCGR3A, FLNB, MUC2, GAS6, MT1A, GPR4, MMP9, NR4A1, MMP3, MICB, MEFV, CYP4F3, GPX2, ITGA1, IDO1, IL18, IL12B, HGF, HLA-B, IL1RN, MAPK3, MAPK8, EGFR, AKT1, SLC7A5, VEGFA, VDR, UCP2, TTR, TPSAB1, CLDN3, TLR4, CRH, TJP1, TAP2, CRHR1, STAT3, SOX9, HLTF, SLC22A4, SLC3A2, CCL11, CUX1, S100A12, CYBB, S100A8, DECR1, NQO1, PXMP2, PTPN11
-
Aortic Arch Interruption, Facial Palsy, And Retinal Coloboma
Omim
Levin et al. (1973) described monozygotic female twins with a syndrome of hypoplasia or interruption of the transverse aortic arch, facial weakness involving particularly the depressor anguli oris, and bilateral retinal coloboma. Marden and Venters (1966) described macular coloboma and coarctation of the aorta in a single patient who also had the linear nevus sebaceous syndrome. Whether this is a genuine syndrome and, if so, whether it is mendelian is not clear. ... Autosomal dominant Neuro - Facial weakness, esp. depressor anguli oris Skin - Linear nevus sebaceous syndrome ▲ Close
- Chromosome 3p- Syndrome Gard
-
Xy Type Gonadal Dysgenesis-Associated Anomalies Syndrome
Orphanet
Gonadal dysgenesis with multiple anomalies is an association syndrome described only once in two sisters aged 1 1/2 and 8 1/2 years.
-
Primary Microcephaly-Epilepsy-Permanent Neonatal Diabetes Syndrome
Orphanet
Primary microcephaly-epilepsy-permanent neonatal diabetes syndrome is a rare, genetic, neurologic disease characterized by congenital microcephaly, severe, early-onset epileptic encephalopathy (manifesting as intractable, myoclonic and/or tonic-clonic seizures), permanent, neonatal, insulin-dependent diabetes mellitus, and severe global developmental delay.
-
Kyphoscoliotic Ehlers-Danlos Syndrome Due To Fkbp22 Deficiency
Orphanet
A rare subtype of kyphoscoliotic Ehlers-Danlos syndrome characterized by congenital muscle hypotonia, congenital or early-onset kyphoscoliosis (progressive or non-progressive), and generalized joint hypermobility with dislocations/subluxations (in particular of the shoulders, hips, and knees).
-
Non-Acquired Combined Pituitary Hormone Deficiency-Sensorineural Hearing Loss-Spine Abnormalities Syndrome
Orphanet
Non-acquired combined pituitary hormone deficiency-sensorineural hearing loss-spine abnormalities syndrome is a rare, genetic, non-acquired, combined pituitary hormone deficiency disorder characterized by panhypopituitarism (with or without ACTH deficiency) associated with spine abnormalities, including frequent rigid cervical spine and short neck with limited rotation, and variable degrees of sensorineural hearing loss.
-
Primary Hypergonadotropic Hypogonadism-Partial Alopecia Syndrome
Orphanet
This syndrome is characterized by primary hypergonadotropic hypogonadism and partial alopecia.
-
Marfanoid Habitus-Inguinal Hernia-Advanced Bone Age Syndrome
Orphanet
Marfanoid habitus-inguinal hernia-advanced bone age syndrome is a very rare developmental defect with connective tissue involvement disorder characterized by tall stature, inguinal hernia, facial dysmorphism (including a long, triangular face, prominent forehead, telecanthus, downslanting palpebral fissures, bilateral ptosis, everted lower eyelids, large ears, long nose, full, everted vermilions, narrow and high arched palate, dental crowding), and radiologic evidence of advanced bone age.