-
Inborn Errors Of Metabolism
Wikipedia
Many others do not fall into these categories. [ citation needed ] Disorders of carbohydrate metabolism glycogen storage disease G6PD deficiency [4] Disorders of amino acid metabolism [5] phenylketonuria maple syrup urine disease glutaric acidemia type 1 Urea Cycle Disorder or Urea Cycle Defects Carbamoyl phosphate synthetase I deficiency Disorders of organic acid metabolism ( organic acidurias ) alkaptonuria 2-hydroxyglutaric acidurias Disorders of fatty acid oxidation and mitochondrial metabolism Medium-chain acyl-coenzyme A dehydrogenase deficiency (MCADD) Disorders of porphyrin metabolism acute intermittent porphyria Disorders of purine or pyrimidine metabolism Lesch–Nyhan syndrome Disorders of steroid metabolism lipoid congenital adrenal hyperplasia congenital adrenal hyperplasia Disorders of mitochondrial function Kearns–Sayre syndrome Disorders of peroxisomal function Zellweger syndrome Lysosomal storage disorders [6] Gaucher's disease Niemann–Pick disease Signs and symptoms [ edit ] Because of the enormous number of these diseases the wide range of systems affected badly, nearly every "presenting complaint" to a healthcare provider may have a congenital metabolic disease as a possible cause, especially in childhood and adolescence. ... External links [ edit ] Classification D ICD - 10 : E70 - E90 ICD - 9-CM : 270 - 279 MeSH : D008661 External resources MedlinePlus : 002438 eMedicine : emerg/768 article/804757 National Institutes of Health offers the office of rare diseases , home reference , medlineplus and health information . v t e Inborn error of carbohydrate metabolism : monosaccharide metabolism disorders Including glycogen storage diseases (GSD) Sucrose , transport (extracellular) Disaccharide catabolism Congenital alactasia Sucrose intolerance Monosaccharide transport Glucose-galactose malabsorption Inborn errors of renal tubular transport ( Renal glycosuria ) Fructose malabsorption Hexose → glucose Monosaccharide catabolism Fructose : Essential fructosuria Fructose intolerance Galactose / galactosemia : GALK deficiency GALT deficiency / GALE deficiency Glucose ⇄ glycogen Glycogenesis GSD type 0 (glycogen synthase deficiency) GSD type IV (Andersen's disease, branching enzyme deficiency) Adult polyglucosan body disease (APBD) Glycogenolysis Extralysosomal: GSD type III (Cori's disease, debranching enzyme deficiency) GSD type VI (Hers' disease, liver glycogen phosphorylase deficiency) GSD type V (McArdle's disease, myophosphorylase deficiency) GSD type IX (phosphorylase kinase deficiency) Lysosomal ( LSD ): GSD type II (Pompe's disease, glucosidase deficiency) Glucose ⇄ CAC Glycolysis MODY 2 / HHF3 GSD type VII (Tarui's disease, phosphofructokinase deficiency) Triosephosphate isomerase deficiency Pyruvate kinase deficiency Gluconeogenesis PCD Fructose bisphosphatase deficiency GSD type I (von Gierke's disease, glucose 6-phosphatase deficiency) Pentose phosphate pathway Glucose-6-phosphate dehydrogenase deficiency Transaldolase deficiency 6-phosphogluconate dehydrogenase deficiency Other Hyperoxaluria Primary hyperoxaluria Pentosuria Aldolase A deficiency v t e Inborn error of amino acid metabolism K → acetyl-CoA Lysine /straight chain Glutaric acidemia type 1 type 2 Hyperlysinemia Pipecolic acidemia Saccharopinuria Leucine 3-hydroxy-3-methylglutaryl-CoA lyase deficiency 3-Methylcrotonyl-CoA carboxylase deficiency 3-Methylglutaconic aciduria 1 Isovaleric acidemia Maple syrup urine disease Tryptophan Hypertryptophanemia G G→ pyruvate → citrate Glycine D-Glyceric acidemia Glutathione synthetase deficiency Sarcosinemia Glycine → Creatine : GAMT deficiency Glycine encephalopathy G→ glutamate → α-ketoglutarate Histidine Carnosinemia Histidinemia Urocanic aciduria Proline Hyperprolinemia Prolidase deficiency Glutamate / glutamine SSADHD G→ propionyl-CoA → succinyl-CoA Valine Hypervalinemia Isobutyryl-CoA dehydrogenase deficiency Maple syrup urine disease Isoleucine 2-Methylbutyryl-CoA dehydrogenase deficiency Beta-ketothiolase deficiency Maple syrup urine disease Methionine Cystathioninuria Homocystinuria Hypermethioninemia General BC / OA Methylmalonic acidemia Methylmalonyl-CoA mutase deficiency Propionic acidemia G→ fumarate Phenylalanine / tyrosine Phenylketonuria 6-Pyruvoyltetrahydropterin synthase deficiency Tetrahydrobiopterin deficiency Tyrosinemia Alkaptonuria / Ochronosis Tyrosinemia type I Tyrosinemia type II Tyrosinemia type III / Hawkinsinuria Tyrosine → Melanin Albinism : Ocular albinism ( 1 ) Oculocutaneous albinism ( Hermansky–Pudlak syndrome ) Waardenburg syndrome Tyrosine → Norepinephrine Dopamine beta hydroxylase deficiency reverse: Brunner syndrome G→ oxaloacetate Urea cycle / Hyperammonemia ( arginine aspartate ) Argininemia Argininosuccinic aciduria Carbamoyl phosphate synthetase I deficiency Citrullinemia N-Acetylglutamate synthase deficiency Ornithine transcarbamylase deficiency / translocase deficiency Transport / IE of RTT Solute carrier family : Cystinuria Hartnup disease Iminoglycinuria Lysinuric protein intolerance Fanconi syndrome : Oculocerebrorenal syndrome Cystinosis Other 2-Hydroxyglutaric aciduria Aminoacylase 1 deficiency Ethylmalonic encephalopathy Fumarase deficiency Trimethylaminuria v t e Inborn error of lipid metabolism : fatty-acid metabolism disorders Synthesis Biotinidase deficiency (BTD) Degradation Acyl transport Carnitine CPT1 CPT2 CDSP CACTD Adrenoleukodystrophy (ALD) Beta oxidation General Acyl CoA dehydrogenase Short-chain SCADD Medium-chain MCADD Long-chain 3-hydroxy LCHAD Very long-chain VLCADD Mitochondrial trifunctional protein deficiency (MTPD): Acute fatty liver of pregnancy Unsaturated 2,4 Dienoyl-CoA reductase deficiency (DECRD) Odd chain Propionic acidemia (PCC deficiency) Other 3-hydroxyacyl-coenzyme A dehydrogenase deficiency (HADHD) Glutaric acidemia type 2 (MADD) To acetyl-CoA Malonic aciduria (MCD) Aldehyde Sjögren–Larsson syndrome (SLS) v t e Inborn error of lipid metabolism : dyslipidemia Hyperlipidemia Hypercholesterolemia / Hypertriglyceridemia Lipoprotein lipase deficiency/Type Ia Familial apoprotein CII deficiency/Type Ib Familial hypercholesterolemia/Type IIa Combined hyperlipidemia/Type IIb Familial dysbetalipoproteinemia/Type III Familial hypertriglyceridemia/Type IV Xanthoma/Xanthomatosis Hypolipoproteinemia Hypoalphalipoproteinemia/HDL Lecithin cholesterol acyltransferase deficiency Tangier disease Hypobetalipoproteinemia/LDL Abetalipoproteinemia Apolipoprotein B deficiency Chylomicron retention disease Lipodystrophy Barraquer–Simons syndrome Other Lipomatosis Adiposis dolorosa Lipoid proteinosis APOA1 familial renal amyloidosis v t e Heme metabolism disorders Porphyria , hepatic and erythropoietic ( porphyrin ) early mitochondrial: ALAD porphyria Acute intermittent porphyria cytoplasmic: Gunther disease/congenital erythropoietic porphyria Porphyria cutanea tarda / Hepatoerythropoietic porphyria late mitochondrial: Hereditary coproporphyria Harderoporphyria Variegate porphyria Erythropoietic protoporphyria Hereditary hyperbilirubinemia ( bilirubin ) unconjugated: Gilbert's syndrome Crigler–Najjar syndrome Lucey–Driscoll syndrome conjugated: Dubin–Johnson syndrome nd sheet Rotor syndrome v t e Inborn error of purine–pyrimidine metabolism Purine metabolism Anabolism Adenylosuccinate lyase deficiency Adenosine Monophosphate Deaminase Deficiency type 1 Nucleotide salvage Lesch–Nyhan syndrome / Hyperuricemia Adenine phosphoribosyltransferase deficiency Catabolism Adenosine deaminase deficiency Purine nucleoside phosphorylase deficiency Xanthinuria Gout Mitochondrial neurogastrointestinal encephalopathy syndrome Pyrimidine metabolism Anabolism Orotic aciduria Miller syndrome Catabolism Dihydropyrimidine dehydrogenase deficiency v t e Inborn errors of steroid metabolism Mevalonate pathway HMG-CoA lyase deficiency Hyper-IgD syndrome Mevalonate kinase deficiency To cholesterol 7-Dehydrocholesterol path: Hydrops-ectopic calcification-moth-eaten skeletal dysplasia CHILD syndrome Conradi-Hünermann syndrome Lathosterolosis Smith–Lemli–Opitz syndrome desmosterol path: Desmosterolosis Steroids Corticosteroid (including CAH ) aldosterone : Glucocorticoid remediable aldosteronism cortisol / cortisone : CAH 17α-hydroxylase CAH 11β-hydroxylase both: CAH 3β-dehydrogenase CAH 21-hydroxylase Apparent mineralocorticoid excess syndrome/11β-dehydrogenase Sex steroid To androgens 17α-Hydroxylase deficiency 17,20-Lyase deficiency Cytochrome b 5 deficiency 3β-Hydroxysteroid dehydrogenase deficiency 17β-Hydroxysteroid dehydrogenase deficiency 5α-Reductase deficiency Pseudovaginal perineoscrotal hypospadias To estrogens Aromatase deficiency Aromatase excess syndrome Other X-linked ichthyosis Antley–Bixler syndrome v t e Metabolic disorders of vitamins , coenzymes, and cofactors B7 Biotin / MCD Biotinidase deficiency Holocarboxylase synthetase deficiency Other B B5 ( Pantothenate kinase-associated neurodegeneration ) B12 ( Methylmalonic acidemia ) Other vitamin Familial isolated vitamin E deficiency Nonvitamin cofactor Tetrahydrobiopterin deficiency Molybdenum cofactor deficiency Metabolism portalMMUT, ITPA, ABCD4, DIO1, DHFR, MYO5B, LEPR, CES1, LDHB, PLA2G4A, SLC2A1, SERPINA7, TPI1, PLA2G7, SELENBP1, ADAMTSL2, AGXT2, MOCS2, PAH, ALPL, CBS, CBSL, STS, OTC, GALT, HGD, GLA, GCDH, ACADM, CYP27A1, ECHS1, ACY1, UROS, RPS27, DMGDH, TTK, SERPINA1, CA2, MLYCD, ADSL, IDUA, HMBS, HPRT1, ASS1, GALE, G6PD, MPEG1, ACAT1, AGXT, SCO2, SLC28A1, SLC25A13, FGF21, SGPL1, PPIG, TNKS, ARG1, KIFBP, ZNF185, HIBCH, GALK1, GNMT, LYPD4, LINC01672, ALG11, SUMF1, H19, ACSF3, MMAA, NAGS, SLC46A1, HTRA2, FLAD1, PANK2, SLC5A7, COQ9, HAO1, EIM, LIPT1, HAO2, TAT, ASNS, HEXA, MRC1, TYMP, FAH, LCAT, FXN, FUT1, HEXB, HADHA, TKT, HSD17B10, GPD1, GLS, GLB1, GK, GH1, SLC37A4, MTHFD1, MTHFR, MUC1, DPYD, TCN2, ASPA, TAZ, SUOX, SMPD1, SLC10A1, ATP7B, PSD, PRL, PMM2, PDHA1, SLC25A20, CHKB, NPC1, MVK, OAT
-
Parental Alienation Syndrome
Wikipedia
"Knowledge and Attitudes About the Parental Alienation Syndrome: A Survey of Custody Evaluators". ... "What is it that's being called Parental Alienation Syndrome". In Caplan PJ; Cosgrove L (eds.). ... Adult children of parental alienation syndrome: breaking the ties that bind . ... "A Critical Analysis of Parental Alienation Syndrome and Its Admissibility in the Family Court". ... "What is it that's being called Parental Alienation Syndrome". In Caplan PJ; Cosgrove L (eds.).
-
Pseudoxanthoma Elasticum
Wikipedia
Pseudoxanthoma elasticum Other names Grönblad–Strandberg syndrome; [1] Groenblad-Strandberg syndrome Pseudoxanthoma elasticum of the posterior lateral neck. ... This is the main source of circulating pyrophosphate (PPi), and individuals affected by PXE have strongly reduced plasma PPi levels, explaining their mineralization disorder. [19] One study suggested that mutations causing total absence of an ABCC6 protein caused a more severe disease, [20] but this could not be confirmed in a subsequent case series. [21] Given the variations in age of onset and severity it is likely that other unknown risk factors (genetic, environmental, and lifestyle) may be involved. [3] Premature atherosclerosis is also associated with mutations in the ABCC6 gene, even in those without PXE. [22] A syndrome almost indistinguishable from hereditary PXE has been described in patients with hemoglobinopathies ( sickle-cell disease and thalassemia ) through a poorly understood mechanism. [3] In addition, there appears to be another PXE-like syndrome with a similar phenotype but as a result of problems with another gene, gamma-glutamyl carboxylase . [23] Mutations in ABCC6 can also cause generalized arterial calcification of infancy. [24] In some cases of PXE, mutations in ABCC6 cannot be found, and other genes such as ENPP1 may be implicated [25] Pathophysiology [ edit ] In PXE, there is mineralization (accumulation of calcium and other minerals) and fragmentation of the elastin -containing fibers in connective tissue , but primarily in the midlaminar layer of the dermis, Bruch's membrane and the midsized arteries . [26] Recent studies have confirmed that PXE is a metabolic disease, and that its features arise because metabolites of vitamin K cannot reach peripheral tissues. [27] Low levels of PPi cause mineralization in peripheral tissues. [19] Diagnosis [ edit ] Histopathology of pseudoxanthoma elasticum: Fragmentation and calcification of middermal elastic fibers on Alizarin Red staining. [28] The diagnostic criteria for PXE are the typical skin biopsy appearance and the presence of angioid streaks in the retina. ... Diagnostic histopathological changes in lesional skin: Calcified elastic fibers in the mid and lower dermis, confirmed by positive calcium stain Differential diagnosis [ edit ] The differential diagnosis PXE-like papillary dermal elastolysis : Small flesh-colored papules in the neck region. [28] Histopathology of PXE-like papillary dermal elastolysis: Loss of elastic fibers in the papillary dermis and abnormal pattern in the reticular dermis (arrow) [28] Pseudoxanthoma elasticum versus histopathological differential diagnoses on light microscopy (LM) and electron microscopy (EM) [28] Pseudoxanthoma elasticum LM: Mid-dermal calcification and fragmentation of elastic fibers EM: Mineralization in elastic fiber core PXE-like disease with coagulation deficiency LM: Middermal calcification and fragmentation of elastic fibers EM: Mineralization in elastic fiber periphery Hemoglobinopathies LM: Middermal calcification and fragmentation of elastic fibers EM: Mineralization in elastic fiber core PXE-like papillary dermal elastolysis LM: Selective elastic tissue elimination in the papillary dermis and presence of melanophages White fibrous papulosis of the neck LM: Dermal fibrosis in papillary and mid-reticular dermis Late-onset focal dermal elastosis EM: Decrease of elastic fibers; fragmentation of remaining fibers LM: Accumulation of elastic fibers in mid- and reticular dermis without fragmentation or calcification Perforating calcific elastosis LM: Middermal calcification and degeneration of elastic fibers with transepidermal elimination Buschke-Ollendorff syndrome LM: Increased amount of hypertrophic elastic fibers in dermis EM: Altered translucent elastic fibers Elastosis perforans serpiginosa LM: Transepidermal or perifollicular perforating canals Papular elastorrhexis LM: Thickening of collagen bundles next to loss and fragmentation of elastic fibers Upper dermal elastolysis LM: Complete loss of elastic fibers in the upper dermis Middermal elastolysis LM: Complete absence of elastic fibers in the middermis Linear focal elastosis LM: Massive basophilic fibers; clumping of elastic fibers in papillary dermis Elastoderma LM: Increased, intertwining thin elastic fibers in papillary and upper reticular dermis Calcinosis cutis LM: Deposits of calcium in the dermis Treatment [ edit ] There is no confirmed treatment that directly interferes with the disease process. [5] [6] Cosmetic surgery to remove excessive skin has been used to improve aesthetic appearance in PXE patients [5] but because of the non-life-threatening nature of these symptoms, should be used with caution. [6] One of the most critical symptom of PXE is choroidal neovascularization which can lead to deterioration of central vision. ... The disease occurs in all ethnicities, but Afrikaners are more likely to have PXE as a result of a founder effect (i.e., higher prevalence in the small group of people from whom Afrikaners descend). [36] History [ edit ] The first description of PXE that distinguished it from other xanthoma conditions was by Dr Ferdinand-Jean Darrier in 1896. [37] The eponym "Grönblad-Strandberg syndrome" is used in older literature, after two physicians who made further discoveries in the disease manifestations. [38] PXE has the distinction of being the only disease for which a layperson is the discover of the mutated gene. ... External links [ edit ] PXE international Classification D ICD - 10 : Q82.8 ( ILDS Q82.81) ICD - 9-CM : 757.39 OMIM : 264800 MeSH : D011561 DiseasesDB : 10876 External resources eMedicine : derm/359 oph/475 Patient UK : Pseudoxanthoma elasticum pxe at NIH / UW GeneTests Pseudoxanthoma elasticum at NLM Genetics Home Reference v t e Congenital malformations and deformations of integument / skin disease Genodermatosis Congenital ichthyosis / erythrokeratodermia AD Ichthyosis vulgaris AR Congenital ichthyosiform erythroderma : Epidermolytic hyperkeratosis Lamellar ichthyosis Harlequin-type ichthyosis Netherton syndrome Zunich–Kaye syndrome Sjögren–Larsson syndrome XR X-linked ichthyosis Ungrouped Ichthyosis bullosa of Siemens Ichthyosis follicularis Ichthyosis prematurity syndrome Ichthyosis–sclerosing cholangitis syndrome Nonbullous congenital ichthyosiform erythroderma Ichthyosis linearis circumflexa Ichthyosis hystrix EB and related EBS EBS-K EBS-WC EBS-DM EBS-OG EBS-MD EBS-MP JEB JEB-H Mitis Generalized atrophic JEB-PA DEB DDEB RDEB related: Costello syndrome Kindler syndrome Laryngoonychocutaneous syndrome Skin fragility syndrome Ectodermal dysplasia Naegeli syndrome / Dermatopathia pigmentosa reticularis Hay–Wells syndrome Hypohidrotic ectodermal dysplasia Focal dermal hypoplasia Ellis–van Creveld syndrome Rapp–Hodgkin syndrome / Hay–Wells syndrome Elastic / Connective Ehlers–Danlos syndromes Cutis laxa ( Gerodermia osteodysplastica ) Popliteal pterygium syndrome Pseudoxanthoma elasticum Van der Woude syndrome Hyperkeratosis / keratinopathy PPK diffuse : Diffuse epidermolytic palmoplantar keratoderma Diffuse nonepidermolytic palmoplantar keratoderma Palmoplantar keratoderma of Sybert Meleda disease syndromic connexin Bart–Pumphrey syndrome Clouston's hidrotic ectodermal dysplasia Vohwinkel syndrome Corneodermatoosseous syndrome plakoglobin Naxos syndrome Scleroatrophic syndrome of Huriez Olmsted syndrome Cathepsin C Papillon–Lefèvre syndrome Haim–Munk syndrome Camisa disease focal : Focal palmoplantar keratoderma with oral mucosal hyperkeratosis Focal palmoplantar and gingival keratosis Howel–Evans syndrome Pachyonychia congenita Pachyonychia congenita type I Pachyonychia congenita type II Striate palmoplantar keratoderma Tyrosinemia type II punctate : Acrokeratoelastoidosis of Costa Focal acral hyperkeratosis Keratosis punctata palmaris et plantaris Keratosis punctata of the palmar creases Schöpf–Schulz–Passarge syndrome Porokeratosis plantaris discreta Spiny keratoderma ungrouped: Palmoplantar keratoderma and spastic paraplegia desmoplakin Carvajal syndrome connexin Erythrokeratodermia variabilis HID / KID Other Meleda disease Keratosis pilaris ATP2A2 Darier's disease Dyskeratosis congenita Lelis syndrome Dyskeratosis congenita Keratolytic winter erythema Keratosis follicularis spinulosa decalvans Keratosis linearis with ichthyosis congenita and sclerosing keratoderma syndrome Keratosis pilaris atrophicans faciei Keratosis pilaris Other cadherin EEM syndrome immune system Hereditary lymphedema Mastocytosis / Urticaria pigmentosa Hailey–Hailey see also Template:Congenital malformations and deformations of skin appendages , Template:Phakomatoses , Template:Pigmentation disorders , Template:DNA replication and repair-deficiency disorder Developmental anomalies Midline Dermoid cyst Encephalocele Nasal glioma PHACE association Sinus pericranii Nevus Capillary hemangioma Port-wine stain Nevus flammeus nuchae Other/ungrouped Aplasia cutis congenita Amniotic band syndrome Branchial cyst Cavernous venous malformation Accessory nail of the fifth toe Bronchogenic cyst Congenital cartilaginous rest of the neck Congenital hypertrophy of the lateral fold of the hallux Congenital lip pit Congenital malformations of the dermatoglyphs Congenital preauricular fistula Congenital smooth muscle hamartoma Cystic lymphatic malformation Median raphe cyst Melanotic neuroectodermal tumor of infancy Mongolian spot Nasolacrimal duct cyst Omphalomesenteric duct cyst Poland anomaly Rapidly involuting congenital hemangioma Rosenthal–Kloepfer syndrome Skin dimple Superficial lymphatic malformation Thyroglossal duct cyst Verrucous vascular malformation Birthmark v t e Genetic disorder , membrane: ABC-transporter disorders ABCA ABCA1 ( Tangier disease ) ABCA3 ( Surfactant metabolism dysfunction 3 ) ABCA4 ( Stargardt disease 1 , Retinitis pigmentosa 19 ) ABCA12 ( Harlequin-type ichthyosis , Lamellar ichthyosis 2 ) ABCB ABCB4 ( Progressive familial intrahepatic cholestasis 3 ) ABCB7 ( ASAT ) ABCB11 ( Progressive familial intrahepatic cholestasis 2 ) ABCC ABCC2 ( Dubin–Johnson syndrome ) ABCC6 ( Pseudoxanthoma elasticum ) ABCC7 ( Cystic fibrosis ) ABCC8 ( HHF1 , TNDM2 ) ABCC9 ( Dilated cardiomyopathy 1O ) ABCD ABCD1 ( Adrenoleukodystrophy , Adrenomyeloneuropathy ) ABCG ABCG5 ( Sitosterolemia ) ABCG8 ( Gallbladder disease 4, Sitosterolemia ) see also ABC transporters
-
Polydactyly
Wikipedia
Ulnar polydactyly is also often part of a syndrome. [11] In patients with African ancestry ulnar polydactyly mostly occurs isolated, whereas the presentation in Caucasians is often associated with a syndrome, [8] though in a retrospective review, only 4 of 37 cases of ulnar polydactyly in Caucasians were syndromic. [12] In almost 14% of all patients, this type of polydactyly is hereditary. ... Ulnar polydactyly occurs as an isolated congenital condition, but can also be part of a syndrome. The syndromes which occur with ulnar polydactyly are: Trisomy 13 , Greig cephalopolysyndactyly syndrome , Meckel syndrome , Ellis–van Creveld syndrome , McKusick–Kaufman syndrome , Down syndrome , Bardet–Biedl syndrome , Smith–Lemli–Opitz syndrome [11] [25] Radial polydactyly [ edit ] Type VII of radial polydactyly is associated with several syndromes: Holt–Oram syndrome , Fanconi anemia (aplastic anemia by the age of 6), Townes–Brocks syndrome , and Greig cephalopolysyndactyly (also known to occur with ulnar polydactyly). [15] Central polydactyly [ edit ] The syndromes associated with central polydactyly are: Bardet–Biedl syndrome , [26] Meckel syndrome , [27] Pallister–Hall syndrome , [28] Legius syndrome , [29] Holt–Oram syndrome . [30] Also, central polydactyly can be associated with syndactyly and cleft hand . [17] [18] Other syndromes including polydactyly include acrocallosal syndrome , basal cell nevus syndrome , Biemond syndrome , ectrodactyly-ectodermal dysplasias-cleft lip/palate syndrome , mirror hand deformity , Mohr syndrome , oral-facial-digital syndrome , Rubinstein-Taybi syndrome , short rib polydactyly , and VATER association . [31] It can also occur with a triphalangeal thumb . ... PMID 2304571 . ^ Kumar S, Mahajan BB, Mittal J (2012). "Bardet-Biedl syndrome: a rare case report from North India" . ... PMID 22346195 . ^ Biesecker LG (1993). Pallister-Hall Syndrome . ^ Denayer E, Chmara M (2011). "Legius syndrome in fourteen families" . Hum. Mutat . 32 (1): 1985–98. doi : 10.1002/humu.21404 .FAM92A, GLI3, CCND2, TCTN2, ZBTB16, GLI1, CPLANE1, IQCE, BBS12, SUFU, NCAPG2, IFT57, WDR60, WDR35, CC2D2A, LMBR1, TMEM237, TMEM231, CSPP1, NKX2-5, B9D2, ARL6, UQCC2, IFT43, CTU2, NKX2-6, CRB2, CEP120, IFT81, INTU, TCTN3, RBM10, GPC4, GATA6, GPC3, HNRNPK, PIK3R2, TULP1, USP9X, TBX1, OFD1, KIAA0586, C2CD3, CILK1, KIAA0753, KIF7, RANGAP1, DDX59, AGO2, HTC2, MKKS, EVC2, HOXA@, TBX3, GLI2, C8orf37, CCN6, KIAA0825, VSX1, ZNF141, HPD
-
Vaginal Anomalies
Wikipedia
Defects that prevent menstrual flow become obvious when amenorrhea occurs. [ citation needed ] Syndromes [ edit ] Syndromes may take longer to identify since they are rare and often involve errors in metabolism. ... These include Fraser syndrome , WNT4 deficiency , and Bardet-Biedl syndrome, [38] [60] [47] [55] Isolated incidents of vaginal anomalies can occur with no apparent cause and in other instances these anomalies are part of a syndrome or cluster of other abnormalities. ... PMID 7996504 . ^ a b Slavotinek AM, Tifft CJ (September 2002). "Fraser syndrome and cryptophthalmos: review of the diagnostic criteria and evidence for phenotypic modules in complex malformation syndromes" . ... Retrieved 2018-01-22 . ^ François J (1965). "Syndrome malformatif avec cryptophtalmie". ... CS1 maint: DOI inactive as of January 2021 ( link ) ^ McKusick-Kaufman syndrome at Who Named It? ^ Slavotinek AM, "McKusick-Kaufam Syndrome" , GeneReviews , 1993-2015 ^ Mandava A, Prabhakar RR, Smitha S (April 2012).
-
Exfoliation Syndrome
Omim
A number sign (#) is used with this entry because of evidence that susceptibility to the exfoliation syndrome (XFS) is conferred by variation in the LOXL1 gene (153456) on chromosome 15q24. Description Exfoliation syndrome (XFS) is a common age-related disorder of the extracellular matrix that is frequently associated with severe chronic secondary open-angle glaucoma and cataract. ... Clinical Features Forsius (1981) considered the exfoliation syndrome to be a disorder of the suspensory ligament. ... Yuksel et al. (2001) described the ocular hemodynamics in pseudoexfoliation syndrome and pseudoexfoliation glaucoma. ... Hewitt et al. (2008) noted that their Caucasian population had a 9-fold lower lifetime incidence of pseudoexfoliation syndrome compared to the Nordic populations studied by Thorleifsson et al. (2007) despite having similar allelic architecture at the LOXL1 locus, and suggested that genetic or environmental factors independent of LOXL1 strongly influence the phenotypic expression of the syndrome.LOXL1, CACNA1A, POMP, TLCD5, RBMS3, AGPAT1, LYST, LOXL1-AS1, LTBP2, TBC1D21, PML, CLU, ELN, TNF, MTHFR, CNTNAP2, CXCL8, APOE, MMP9, EGF, MGST1, TLR4, PLXNA2, CXCL11, IGF1, SOD2, CCN2, HPGDS, ABCA1, TXNRD2, FBLN5, DPM2, WNT5A, UBB, ATG5, XPO5, CMPK1, MARCHF1, MIR3161, MIR1304, GGTLC4P, GGT2, GGTLC3, MIR630, GGTLC5P, MIR302D, GSTK1, CCDC167, SLCO6A1, COL18A1, OPA3, SEMA6A, TGFB1, ATG2B, ATG16L1, TGM2, PTEN, SOX2, IL6, GSTT1, GSTP1, GSTM1, GLS, GGT1, GC, FOXC1, CRYBB2, CRP, CPE, CHI3L1, SERPINC1, ABCC6, ALDH1A1, AHSG, TNC, KNG1, CCL16, LOX, CCL2, RBP3, PEX19, PTGS2, ACTB, PSMA5, PON1, PHEX, PCNA, PAK3, MTHFD1, COX2, MMP3, MMP2, MMP1, MTCO2P12
-
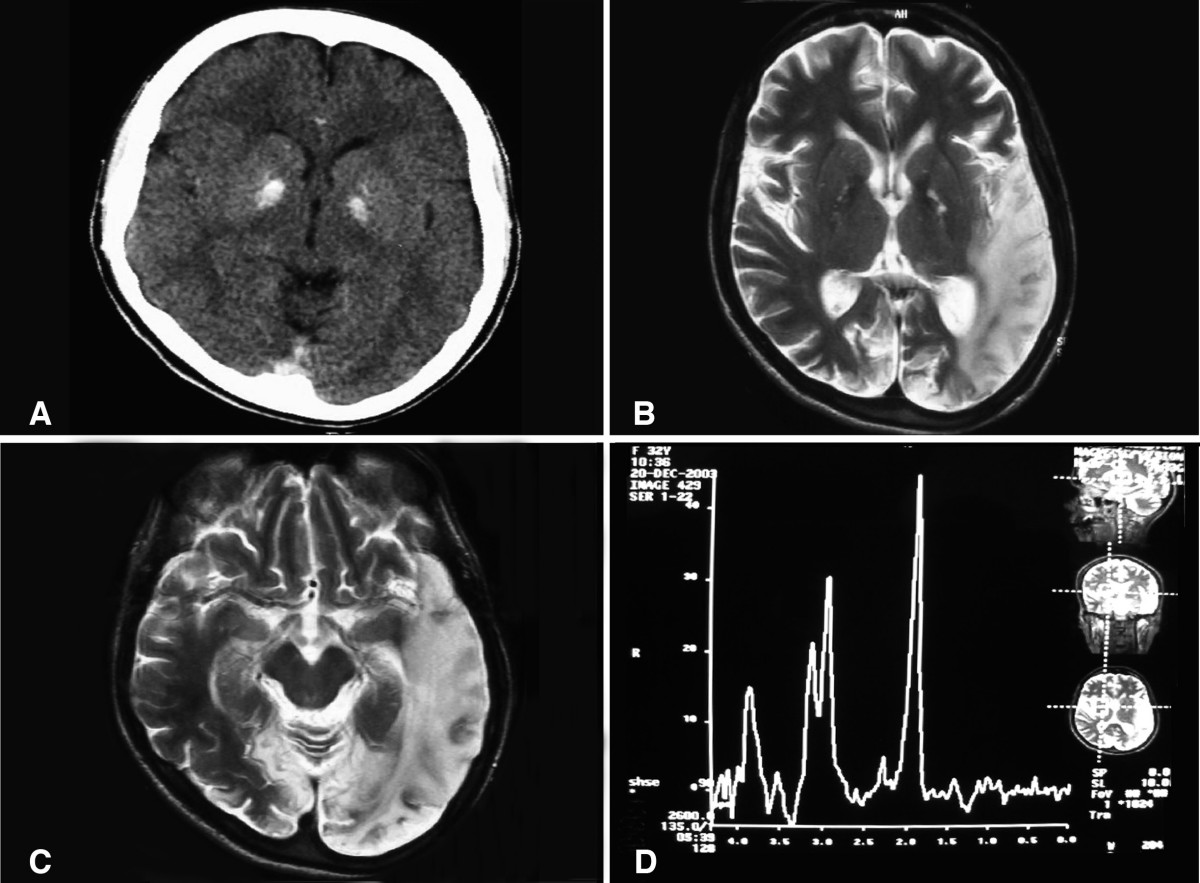
Mitochondrial Myopathy, Encephalopathy, Lactic Acidosis, And Stroke-Like Episodes
Omim
Other mitochondrial encephalomyopathies include Leigh syndrome (LS; 256000), Kearns-Sayre syndrome (KSS; 530000), MERRF syndrome (545000), and Leber optic atrophy (535000). ... Latkany et al. (1999) reported the ocular findings in 4 family members with MELAS syndrome caused by the 3243A-G MTTL1 mutation (590050.0001). ... Bataillard et al. (2001) reported an atypical case of MELAS syndrome associated with a 4332G-A mutation in the MTTQ gene (590030.0003). ... The authors emphasized the genetic heterogeneity of the MELAS syndrome. In several affected members of 3-generation Sardinian kindred with a maternally inherited syndrome characterized by features of both MERRF and MELAS, Zeviani et al. (1993) identified a mutation in the MTTK gene (590060.0002). ... The clinical picture was consistent with MELAS syndrome. At age 25 years, he developed myoclonus and ataxia, suggesting MERRF syndrome.ND5, ND1, ND6, TRNS1, TRNW, TRNF, TRNQ, COX1, COX2, COX3, TRNL1, ND4, TRNS2, TRNK, TRNH, TRNC, TRNV, CYTB, SOD2, SOD1, IL1B, IL1A, ATP6, TRNA, TRNE, TRNL2, TRNI, TRNP, TRNN, NDUFS1, POLG, NPTX2, COX5A, TWNK, MTCO2P12, CPOX, COX8A, RNR2, TRMU, TOMM20, PPARGC1A, SDS, FASTKD2, P2RX2, PRPF6, FGF21, MRM2, SLC25A4, TNFSF10, COQ8A, RARS2, MAPKAP1, GFM2, OR10T2, GLIS3, MIR27B, LINC01672, ASNS, TPO, MTERF1, NDUFV1, ND3, ATXN3, MTOR, ACTB, FH, SARDH, DDIT3, NDUFA1, PNP, RNR1, COL4A1, PRSS1, SDHB, CALB1, RERE, SORD, TFAM, TG, ABL2
-
Epidural Hematoma
Wikipedia
External links [ edit ] Classification D ICD - 10 : I62.1 , S06.4 ICD - 9-CM : 432.0 MeSH : D006407 DiseasesDB : 4353 External resources MedlinePlus : 001412 eMedicine : emerg/167 med/2898 neuro/574 Patient UK : Epidural hematoma MedPix: Epidural hematoma https://web.archive.org/web/20140820073507/http://radiopaedia.org/cases/epidural-hematoma v t e Nonmusculoskeletal injuries of head ( head injury ) and neck Intracranial see neurotrauma Extracranial/ facial trauma eye : Black eye Eye injury Corneal abrasion ear : Perforated eardrum Either/both Penetrating head injury v t e Neurotrauma Traumatic brain injury Intracranial hemorrhage Intra-axial Intraparenchymal hemorrhage Intraventricular hemorrhage Extra-axial Subdural hematoma Epidural hematoma Subarachnoid hemorrhage Brain herniation Cerebral contusion Cerebral laceration Concussion Post-concussion syndrome Second-impact syndrome Dementia pugilistica Chronic traumatic encephalopathy Diffuse axonal injury Abusive head trauma Penetrating head injury Spinal cord injury Anterior spinal artery syndrome Brown-Séquard syndrome Cauda equina syndrome Central cord syndrome Paraplegia Posterior cord syndrome Spinal cord injury without radiographic abnormality Tetraplegia (Quadriplegia) Peripheral nerves Nerve injury Peripheral nerve injury classification Wallerian degeneration Injury of accessory nerve Brachial plexus injury Traumatic neuroma v t e Cerebrovascular diseases including stroke Ischaemic stroke Brain Anterior cerebral artery syndrome Middle cerebral artery syndrome Posterior cerebral artery syndrome Amaurosis fugax Moyamoya disease Dejerine–Roussy syndrome Watershed stroke Lacunar stroke Brain stem Brainstem stroke syndrome Medulla Medial medullary syndrome Lateral medullary syndrome Pons Medial pontine syndrome / Foville's Lateral pontine syndrome / Millard-Gubler Midbrain Weber's syndrome Benedikt syndrome Claude's syndrome Cerebellum Cerebellar stroke syndrome Extracranial arteries Carotid artery stenosis precerebral Anterior spinal artery syndrome Vertebrobasilar insufficiency Subclavian steal syndrome Classification Brain ischemia Cerebral infarction Classification Transient ischemic attack Total anterior circulation infarct Partial anterior circulation infarct Other CADASIL Binswanger's disease Transient global amnesia Haemorrhagic stroke Extra-axial Epidural Subdural Subarachnoid Cerebral/Intra-axial Intraventricular Brainstem Duret haemorrhages General Intracranial hemorrhage Aneurysm Intracranial aneurysm Charcot–Bouchard aneurysm Other Cerebral vasculitis Cerebral venous sinus thrombosis
-
Chemotherapy-Induced Acral Erythema
Wikipedia
Hand-foot syndrome is also rarely seen in sickle-cell disease . ... PMID 9329890 . ^ https://dermnetnz.org/topics/hand-foot-syndrome/ ^ Apisarnthanarax N, Duvic MM (2003). ... American Association for Cancer Research. ^ https://dermnetnz.org/topics/hand-foot-syndrome/ ^ Lacouture ME, Reilly LM, Gerami P, Guitart J (2008). ... "Pegylated liposomal doxorubicin-associated hand-foot syndrome: recommendations of an international panel of experts". ... "Topical henna for capecitabine induced hand-foot syndrome". Investigational New Drugs . 26 (2): 189–192. doi : 10.1007/s10637-007-9082-3 .
-
Antley-Bixler Syndrome With Genital Anomalies And Disordered Steroidogenesis
Omim
A number sign (#) is used with this entry because of evidence that Antley-Bixler syndrome with disordered steroidogenesis (ABS1) is caused by homozygous or compound heterozygous mutation in the gene encoding cytochrome P450 oxidoreductase (POR; 124015) on chromosome 7q11. A form of Antley-Bixler syndrome with normal steroidogenesis (ABS2; 207410) is a distinct disorder caused by mutation in the FGFR2 gene (176943). Congenital adrenal hyperplasia without Antley-Bixler skeletal anomalies can also result from POR mutations (613571). Description The Antley-Bixler syndrome (ABS) is an exceptionally rare craniosynostosis syndrome characterized by radiohumeral synostosis present from the perinatal period. ... Reardon et al. (2000) was impressed with the occurrence of genital abnormalities in patients, especially females, who had been diagnosed as having Antley-Bixler syndrome. They reported abnormalities of steroid biogenesis in 7 of 16 patients with an Antley-Bixler phenotype. ... Molecular Genetics In individuals with disordered steroidogenesis with bony features of Antley-Bixler syndrome, including the patient reported by Kelley et al. (2002), Fluck et al. (2004) demonstrated mutations in the POR gene (e.g., 124015.0001).
-
Upper Motor Neuron Syndrome
Wikipedia
Upper motor neuron syndrome ( UMNS ) is the motor control changes that can occur in skeletal muscle after an upper motor neuron lesion . ... In neuroanatomical circles, it is often joked, for example, that hemisection of the cervical spinal cord leads to an "upper lower motor neuron syndrome and a lower upper motor neuron syndrome". ... Improved understanding of the multiple features of the upper motor neuron syndrome supports more rigorous assessment, and improved treatment planning. Contents 1 Presentation 2 Diagnosis 3 Treatment 4 See also 5 References Presentation [ edit ] The upper motor neuron syndrome signs are seen in conditions where motor areas in the brain and/or spinal cord are damaged or fail to develop normally. ... While multiple muscles in a limb are usually affected in the Upper Motor Neuron Syndrome, there is usually an imbalance of muscle activity (muscle tone), such that there is a stronger pull on one side of a joint, such as into elbow flexion.
-
Paget–schroetter Disease
Wikipedia
It may develop as a sequela of thoracic outlet syndrome . It is differentiated from secondary causes of upper extremity thrombosis caused by intravascular catheters . [4] Paget–Schroetter syndrome was described once for a viola player who suddenly increased practice time 10-fold, creating enough repetitive pressure against the brachiocephalic and external jugular veins to cause thrombosis. [6] Symptoms may include sudden onset of pain, warmth, redness, blueness and swelling in the arm. ... "Venous obstruction in the upper extremity; Paget-Schroetter's syndrome; a review of 320 cases". Surgery, Gynecology & Obstetrics . 88 (2): 89–127. ... "Venous obstruction in the upper extremity; Paget–Schroetter's syndrome; a review of 320 cases". Surg Gynecol Obstet . 88 (2): 89–127. ... PMID 21410116 . ^ Reina, Nick J.; Honet, Joseph C.; Brown, William; Beitman, Max; Chodoroff, Gary (1988). "Paget-Schroetter syndrome in a viola player". Medical Problems of Performing Artists . 3 (1): 24. ^ Di Nisio, M.; Van Sluis, G. ... "Venous thoracic outlet compression and the Paget-Schroetter syndrome: a review and recommendations for management".
-
Hyperdontia
Wikipedia
Find sources: "Hyperdontia" – news · newspapers · books · scholar · JSTOR ( March 2020 ) ( Learn how and when to remove this template message ) Hyperdontia (Supernumerary Teeth) Supernumerary teeth in the premaxillary area Pronunciation hi-pur-don-ti-ia Specialty Dentistry Symptoms the supernumerary teeth coming out from the gum or in the mouth Complications the supernumerary teeth growing into the gum Duration after dental surgery Types 5 Causes Gardner's syndrome , Ehlers-Danlos syndrome , Cleft palate , Cleidocranial dysplasia and DNA disorder Risk factors supernumerary teeth causing problems in the dental arch Differential diagnosis Hypodontia Prevention n/a Treatment dental surgery Hyperdontia is the condition of having supernumerary teeth , or teeth that appear in addition to the regular number of teeth (32 in the average adult). ... While a single excess tooth is relatively common, multiple hyperdontia is rare in people with no other associated diseases or syndromes. [4] Many supernumerary teeth never erupt, but they may delay eruption of nearby teeth or cause other dental or orthodontic problems. [5] [6] Molar -type extra teeth are the most common type. ... Related conditions [ edit ] Hyperdontia is seen in a number of disorders, including Gardner's syndrome and cleidocranial dysostosis , where multiple supernumerary teeth are seen that are usually impacted. [ citation needed ] Other associated conditions are: Cleidocranial dysplasia , Ehlers–Danlos syndrome Type III, Ellis–van Creveld syndrome , Gardner's syndrome , Goldenhar syndrome , Hallermann–Streiff syndrome , Orofaciodigital syndrome type I, Incontinentia pigmenti , Marfan syndrome , Nance–Horan syndrome , and Tricho-rhino-phalangeal syndrome Type 1 . ... However, this approximation varies in terms of location, other associating syndromes that may be present, and the ethnicity of the individual.
-
Isolated 17,20-Lyase Deficiency
Wikipedia
. ^ a b c Miller WL (January 2012). "The syndrome of 17,20 lyase deficiency" . The Journal of Clinical Endocrinology and Metabolism . 97 (1): 59–67. doi : 10.1210/jc.2011-2161 . ... External links [ edit ] Classification D ICD - 10 : E29.1 OMIM : 202110 MeSH : C567076 External resources Orphanet : 90796 v t e Adrenal gland disorder Hyperfunction Aldosterone Hyperaldosteronism Primary aldosteronism Conn syndrome Bartter syndrome Glucocorticoid remediable aldosteronism AME Liddle's syndrome 17α CAH Pseudohypoaldosteronism Cortisol Cushing's syndrome Pseudo-Cushing's syndrome Steroid-induced osteoporosis Sex hormones 21α CAH 11β CAH Hypofunction Aldosterone Hypoaldosteronism 21α CAH 11β CAH Cortisol CAH Lipoid 3β 11β 17α 21α Sex hormones 17α CAH Inborn errors of steroid metabolism Adrenal insufficiency Adrenal crisis Adrenalitis Xanthogranulomatous Addison's disease Waterhouse–Friderichsen syndrome v t e Inborn errors of steroid metabolism Mevalonate pathway HMG-CoA lyase deficiency Hyper-IgD syndrome Mevalonate kinase deficiency To cholesterol 7-Dehydrocholesterol path: Hydrops-ectopic calcification-moth-eaten skeletal dysplasia CHILD syndrome Conradi-Hünermann syndrome Lathosterolosis Smith–Lemli–Opitz syndrome desmosterol path: Desmosterolosis Steroids Corticosteroid (including CAH ) aldosterone : Glucocorticoid remediable aldosteronism cortisol / cortisone : CAH 17α-hydroxylase CAH 11β-hydroxylase both: CAH 3β-dehydrogenase CAH 21-hydroxylase Apparent mineralocorticoid excess syndrome/11β-dehydrogenase Sex steroid To androgens 17α-Hydroxylase deficiency 17,20-Lyase deficiency Cytochrome b 5 deficiency 3β-Hydroxysteroid dehydrogenase deficiency 17β-Hydroxysteroid dehydrogenase deficiency 5α-Reductase deficiency Pseudovaginal perineoscrotal hypospadias To estrogens Aromatase deficiency Aromatase excess syndrome Other X-linked ichthyosis Antley–Bixler syndrome
-
Queen Bee Syndrome
Wikipedia
Queen bee syndrome was first defined by G.L. Staines, T.E. ... There are also doubts as to whether Queen Bee Syndrome is still in effect in academia. [13] Queen Bee Syndrome was first widely discussed 15 years ago so it seems fair to question whether it is still an issue that women face in the workplace and academia. ... "The underrepresentation of women in science: differential commitment or the queen bee syndrome?" (PDF) . British Journal of Social Psychology . 43 (September): 313–338. doi : 10.1348/0144666042037999 . ... But I think also she did suffer, as her critics say, from what they call the queen bee syndrome: she thought, 'I can do it, why can't others? ... (November 1997). "Homophily or the Queen Bee Syndrome: Female Evaluation of Female Leadership" .
-
Remitting Seronegative Symmetrical Synovitis With Pitting Edema
Wikipedia
"RS3PE syndrome: an overview". Clin. Exp. Rheumatol . 18 (4 Suppl 20): S53–55. PMID 10948764 . ^ Queiro R (March 2004). "RS3PE syndrome: a clinical and immunogenetical study". ... "Acute onset polyarthritis in older people: Is it RS3PE syndrome?" . Cases J . 1 (1): 132. doi : 10.1186/1757-1626-1-132 . ... "Remitting seronegative symmetrical synovitis with pitting edema syndrome: followup for neoplasia" . J. Rheumatol . 32 (9): 1760–61. ... "Remitting seronegative symmetrical synovitis with pitting edema (RS3PE) syndrome: ultrasonography as a diagnostic tool".
-
Upper Airway Resistance Syndrome
Wikipedia
Upper airway resistance syndrome Other names UARS, Non-hypoxic sleep-disordered breathing Upper airway resistance syndrome is a sleep disorder characterized by the narrowing of the airway that can cause disruptions to sleep. [1] [2] The symptoms include unrefreshing sleep, fatigue or sleepiness, chronic insomnia , orthostatic intolerance , and difficulty concentrating. ... "Treatment of upper airway resistance syndrome in adults: Where do we stand?". ... New York: Inform Healthcare. pp. 339–347. ^ Guilleminault, C., & Chowdhuri, S. (2000). Upper Airway Resistance Syndrome Is a Distinct Syndrome. American Journal of Respiratory and Critical Care Medicine, 161(5), 1412–1413. https://doi.org/10.1164/ajrccm.161.5.16158a ^ Garcha, Puneet S.; Aboussouan, Loutfi S.; Minai, Omar (January 2013). ... Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects. ... "The upper airway resistance syndrome". Chest . 115 (4): 1127–39. doi :10.1378/chest.115.4.1127. ^ Guilleminault, Christian and Khramtsov, Andrei.
-
Otoonychoperoneal Syndrome
Omim
Bessieres-Grattagliano et al. (2004) noted that hypoplastic ears and nails and shoulder anomalies with straight claviculae and/or acromioclavicular fusion appeared to be the most consistent features of the syndrome and suggested renaming the entity otoonychoacromioclavicular syndrome. Inheritance Devriendt et al. (1998) suggested autosomal recessive inheritance of the otoonychoperoneal syndrome. INHERITANCE - Autosomal recessive HEAD & NECK Ears - Large ears - Low-set ears - Posteriorly rotated ears - Unfolded helix - Prominent superior crus of antihelix - Hypoplastic lobe CHEST Ribs Sternum Clavicles & Scapulae - Straight clavicles (in some patients) - Malformation of the joint between the clavicle and scapula (in some patients) GENITOURINARY External Genitalia (Male) - Hypospadias (in 1 patient) SKELETAL Skull - Dolichocephaly Pelvis - Contracture of hips Limbs - Fibular aplasia/hypoplasia - Contracture of knees and ankles Hands - Immobility of some interphalangeal joints Feet - Pes calcaneovalgus SKIN, NAILS, & HAIR Nails - Partial nail aplasia ▲ Close
-
Contractures, Pterygia, And Variable Skeletal Fusions Syndrome 1b
Omim
A number sign (#) is used with this entry because of evidence that contractures, pterygia, and variable skeletal fusions syndrome-1B (CPSKF1B) is caused by compound heterozygous mutation in the MYH3 gene (160720) on chromosome 17p13. Description Contractures, pterygia, and variable skeletal fusions syndrome-1B (CPSKF1B) is characterized by contractures of proximal and distal joints, pterygia involving the neck, elbows, fingers, and/or knees, and variable vertebral, carpal, and tarsal fusions. ... An autosomal dominant form of contractures, pterygia, and variable skeletal fusions syndrome (CPSKF1A; 178110) is caused by heterozygous mutation in the MYH3 gene.
-
Myoclonus And Ataxia
Omim
Berkovic et al. (1986) concluded that the Ramsay Hunt syndrome 'does not represent a specific disease, and its use should now be abandoned.' Berkovic et al. (1987) described 11 cases previously diagnosed as having the Ramsay Hunt syndrome (among more than 70 patients with progressive myoclonus epilepsy). ... From a study 'supported by a traveling grant from the University of Navarra and under the inspiration of the products of that region,' Marsden and Obeso (1989), 2 neurologists specializing particularly in movement disorders, argued for the usefulness of the designation 'Ramsay Hunt syndrome.' They concluded that many patients with progressive myoclonus and ataxia have no tonic-chronic seizures, although most have abnormal EEGs. Andermann et al. (1989) again argued that the Ramsay Hunt syndrome is no longer a useful diagnostic category. Harding (1989) took a middle-of-the-road position, insisting that 'the concept of the Ramsay Hunt syndrome is clinically useful as long as those using it remember that it is a syndrome, not a disease.'