-
Alcoholic Polyneuropathy
Wikipedia
This ataxia may be caused by cerebellar degeneration, sensory ataxia, or distal muscle weakness. [4] Over time, alcoholic polyneuropathy may also cause difficulty swallowing ( dysphagia ), speech impairment ( disarthria ), muscle spasms , and muscle atrophy . [5] In addition to alcoholic polyneuropathy, the individual may also show other related disorders such as Wernicke–Korsakoff syndrome and cerebellar degeneration that result from alcoholism-related nutritional disorders. [2] Causes [ edit ] The general cause of this disease is prolonged and heavy consumption of alcohol accompanied by a nutritional deficiency. ... When alcoholics have sensorimotor polyneuropathy as well as a nutritional deficiency, a diagnosis of alcoholic polyneuropathy is often reached. [2] [10] To confirm the diagnosis, a physician must rule out other causes of similar clinical syndromes. Other neuropathies can be differentiated on the basis of typical clinical or laboratory features. [10] Differential diagnoses to alcoholic polyneuropathy include amyotrophic lateral sclerosis , beriberi , Charcot-Marie-Tooth disease , diabetic lumbosacral plexopathy , Guillain Barre Syndrome, diabetic neuropathy , mononeuritis multiplex and post-polio syndrome . [3] To clarify the diagnosis, medical workup most commonly involves laboratory tests, though, in some cases, imaging , nerve conduction studies , electromyography , and vibrometer testing may also be used. [3] A number of tests may be used to rule out other causes of peripheral neuropathy. ... External links [ edit ] Classification D ICD - 10 : G62.1 ICD - 9-CM : 357.5 MeSH : D020269 DiseasesDB : 9850 External resources MedlinePlus : 000714 eMedicine : article/315159 v t e Diseases relating to the peripheral nervous system Mononeuropathy Arm median nerve Carpal tunnel syndrome Ape hand deformity ulnar nerve Ulnar nerve entrapment Froment's sign Ulnar tunnel syndrome Ulnar claw radial nerve Radial neuropathy Wrist drop Cheiralgia paresthetica long thoracic nerve Winged scapula Backpack palsy Leg lateral cutaneous nerve of thigh Meralgia paraesthetica tibial nerve Tarsal tunnel syndrome plantar nerve Morton's neuroma superior gluteal nerve Trendelenburg's sign sciatic nerve Piriformis syndrome Cranial nerves See Template:Cranial nerve disease Polyneuropathy and Polyradiculoneuropathy HMSN Charcot–Marie–Tooth disease Dejerine–Sottas disease Refsum's disease Hereditary spastic paraplegia Hereditary neuropathy with liability to pressure palsy Familial amyloid neuropathy Autoimmune and demyelinating disease Guillain–Barré syndrome Chronic inflammatory demyelinating polyneuropathy Radiculopathy and plexopathy Brachial plexus injury Thoracic outlet syndrome Phantom limb Other Alcoholic polyneuropathy Other General Complex regional pain syndrome Mononeuritis multiplex Peripheral neuropathy Neuralgia Nerve compression syndrome v t e Psychoactive substance-related disorder General SID Substance intoxication / Drug overdose Substance-induced psychosis Withdrawal : Craving Neonatal withdrawal Post-acute-withdrawal syndrome (PAWS) SUD Substance abuse / Substance-related disorders Physical dependence / Psychological dependence / Substance dependence Combined substance use SUD Polysubstance dependence SID Combined drug intoxication (CDI) Alcohol SID Cardiovascular diseases Alcoholic cardiomyopathy Alcohol flush reaction (AFR) Gastrointestinal diseases Alcoholic liver disease (ALD): Alcoholic hepatitis Auto-brewery syndrome (ABS) Endocrine diseases Alcoholic ketoacidosis (AKA) Nervous system diseases Alcohol-related dementia (ARD) Alcohol intoxication Hangover Neurological disorders Alcoholic hallucinosis Alcoholic polyneuropathy Alcohol-related brain damage Alcohol withdrawal syndrome (AWS): Alcoholic hallucinosis Delirium tremens (DTs) Fetal alcohol spectrum disorder (FASD) Fetal alcohol syndrome (FAS) Korsakoff syndrome Positional alcohol nystagmus (PAN) Wernicke–Korsakoff syndrome (WKS, Korsakoff psychosis) Wernicke encephalopathy (WE) Respiratory tract diseases Alcohol-induced respiratory reactions Alcoholic lung disease SUD Alcoholism (alcohol use disorder (AUD)) Binge drinking Caffeine SID Caffeine-induced anxiety disorder Caffeine-induced sleep disorder Caffeinism SUD Caffeine dependence Cannabis SID Cannabis arteritis Cannabinoid hyperemesis syndrome (CHS) SUD Amotivational syndrome Cannabis use disorder (CUD) Synthetic cannabinoid use disorder Cocaine SID Cocaine intoxication Prenatal cocaine exposure (PCE) SUD Cocaine dependence Hallucinogen SID Acute intoxication from hallucinogens (bad trip) Hallucinogen persisting perception disorder (HPPD) Nicotine SID Nicotine poisoning Nicotine withdrawal SUD Nicotine dependence Opioids SID Opioid overdose SUD Opioid use disorder (OUD) Sedative / hypnotic SID Kindling (sedative–hypnotic withdrawal) benzodiazepine : SID Benzodiazepine overdose Benzodiazepine withdrawal SUD Benzodiazepine use disorder (BUD) Benzodiazepine dependence barbiturate : SID Barbiturate overdose SUD Barbiturate dependence Stimulants SID Stimulant psychosis amphetamine : SUD Amphetamine dependence Volatile solvent SID Sudden sniffing death syndrome (SSDS) Toluene toxicity SUD Inhalant abuse
-
Raynaud Syndrome
Wikipedia
This may be the case in the CREST syndrome , of which Raynaud's is a part. ... Anti-centromere antibodies are common in limited systemic sclerosis (CREST syndrome). Nail fold vasculature ( capillaroscopy ) can be examined under a microscope . ... Alternative medicine [ edit ] Evidence does not support the use of alternative medicine, including acupuncture and laser therapy . [3] Prognosis [ edit ] The prognosis of primary Raynaud syndrome is often very favorable, with no mortality and little morbidity. ... "Association between treatment with central nervous system stimulants and Raynaud's syndrome in children: A retrospective case–control study of rheumatology patients" . ... Cite journal requires |journal= ( help ) External links [ edit ] Classification D ICD - 10 : I73.0 ICD - 9-CM : 443.0 OMIM : 179600 MeSH : D011928 DiseasesDB : 25933 External resources MedlinePlus : 000412 eMedicine : med/1993 Patient UK : Raynaud syndrome Wikimedia Commons has media related to Raynaud's phenomenon .GSTM1, GSTT1, IFNA2, GUCY1A1, IRAK1, AGXT, SLC12A3, SPP1, STAT4, ADAR, TREX1, SAMHD1, COQ2, ADA2, RNF125, IFIH1, RNASEH2B, RNASEH2A, LBR, RNASEH2C, COL4A1, C1QA, C1R, CLCNKB, CRP, TNF, RNPC3, PDE5A, EDN1, CALCA, VWF, F8, TRPM8, SLC29A3, HIF1A, VEGFA, CALCB, CDH5, CDH11, BTG3, HLA-DPB1, TRPA1, TNFRSF14, ANXA5, HMOX1, HTR1B, HLA-DRB1, ESR1, IL6, EGF, KRT10, NOS1, PTGIR, PTX3, S100A12, SAFB, CXCL6, SDHC, ACE, SPARC, GAD1, SSB, GSTM2
-
Sydenham's Chorea
Wikipedia
PANDAS presents with tics and/or a psychological component (e.g., OCD) and occurs much earlier, days to weeks after GABHS infection rather than 6–9 months later. [6] It may be confused with other conditions such as lupus and Tourette syndrome . [ citation needed ] Movements cease during sleep, and the disease usually resolves after several months. ... Other disorders that may be accompanied by chorea include abetalipoproteinemia , ataxia–telangiectasia , biotin-thiamine-responsive basal ganglia disease, Fahr disease , familial dyskinesia–facial myokymia (Bird–Raskind syndrome) due to an ADCY5 gene mutation, glutaric aciduria , Lesch–Nyhan syndrome , mitochondrial disorders , Wilson disease , hyperthyroidism , lupus erythematosus , pregnancy ( chorea gravidarum ), and side effects of certain anticonvulsants or psychotropic agents. [ citation needed ] Causes [ edit ] A major manifestation of acute rheumatic fever, Sydenham's chorea is a result of an autoimmune response that occurs following infection by group A β-hemolytic streptococci [7] that destroys cells in the corpus striatum of the basal ganglia . [4] [7] [8] Molecular mimicry to streptococcal antigens leading to an autoantibody production against the basal ganglia has long been thought to be the main mechanism by which chorea occurs in this condition. ... The association of chorea with rheumatism was first reported in 1802, and confirmed in the following decades by several French and English authors. [14] The inclusion of chorea under the rheumatic umbrella helped discriminate Sydenham's chorea from other "choreic" syndromes. The incidence of acute rheumatic fever and rheumatic heart disease is not declining. Recent figures quote the incidence of Acute Rheumatic Fever as 0.6–0.7/1,000 population in the United States and Japan compared with 15–21/1,000 population in Asia and Africa. [15] The prevalence of Acute Rheumatic Fever and Sydenham's Chorea has declined progressively in developed countries over the last decades. [16] [17] Physicians working in early children's hospitals recognised new clinical syndromes through the definition of "typical clinical cases". ... External links [ edit ] Classification D ICD - 10 : I02 ICD - 9-CM : 392 MeSH : D002819 DiseasesDB : 29245 SNOMED CT : 46826000 External resources MedlinePlus : 001358 Patient UK : Sydenham's chorea v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever v t e Firmicutes (low- G+C ) Infectious diseases Bacterial diseases : G+ Bacilli Lactobacillales ( Cat- ) Streptococcus α optochin susceptible S. pneumoniae Pneumococcal infection optochin resistant Viridans streptococci : S. mitis S. mutans S. oralis S. sanguinis S. sobrinus S. anginosus group β A bacitracin susceptible: S. pyogenes Group A streptococcal infection Streptococcal pharyngitis Scarlet fever Erysipelas Rheumatic fever B bacitracin resistant, CAMP test +: S. agalactiae Group B streptococcal infection ungrouped Streptococcus iniae Cutaneous Streptococcus iniae infection γ D BEA +: Streptococcus bovis Enterococcus BEA +: Enterococcus faecalis Urinary tract infection Enterococcus faecium Bacillales ( Cat+ ) Staphylococcus Cg+ S. aureus Staphylococcal scalded skin syndrome Toxic shock syndrome MRSA Cg- novobiocin susceptible S. epidermidis novobiocin resistant S. saprophyticus Bacillus Bacillus anthracis Anthrax Bacillus cereus Food poisoning Listeria Listeria monocytogenes Listeriosis Clostridia Clostridium ( spore -forming) motile: Clostridium difficile Pseudomembranous colitis Clostridium botulinum Botulism Clostridium tetani Tetanus nonmotile: Clostridium perfringens Gas gangrene Clostridial necrotizing enteritis Finegoldia (non-spore forming) Finegoldia magna Mollicutes Mycoplasmataceae Ureaplasma urealyticum Ureaplasma infection Mycoplasma genitalium Mycoplasma pneumoniae Mycoplasma pneumonia Anaeroplasmatales Erysipelothrix rhusiopathiae Erysipeloid
-
Microlissencephaly
Wikipedia
Specialty Neurology Types Norman-Roberts syndrome , Barth syndrome , MLIS3, MLIS4 Causes Genetic Microlissencephaly ( MLIS ) is a rare congenital brain disorder that combines severe microcephaly (small head) with lissencephaly (smooth brain surface due to absent sulci and gyri ). ... Patients may also have dysmorphic craniofacial features, abnormal genitalia, and arthrogryposis . [8] [15] [16] Microlissencephaly may arise as a part of Baraitser-Winter syndrome which comprises also ptosis , coloboma , hearing loss and learning disability. [17] Moreover, it is the distinct developmental brain abnormality in "microcephalic osteodysplastic primordial dwarfism " (MOPD1). [18] Microlissencephaly may be accompanied by micromelia as in Basel-Vanagaite-Sirota syndrome ( a.k.a. ... The classification divided those patients into ten groups in which MSGP represented the first four groups, microlissencephaly referred to the groups from 5-8 and polymicrogyria in the last two groups. [37] In Dobyns-Barkovich classification, Dobyns-Barkovich type 6 is equivalent to Norman-Roberts syndrome (MLIS1) while Dobyns-Barkovich type 8 corresponds to Barth microlissencephaly syndrome (MLIS2). [37] [38] Differential diagnosis [ edit ] Microlissencephaly is considered a more severe form than microcephaly with simplified gyral pattern. ... "Profound microcephaly, primordial dwarfism with developmental brain malformations: A new syndrome". American Journal of Medical Genetics Part A . 158A (8): 1823–1831. doi : 10.1002/ajmg.a.35480 . ... "Tubulinopathies and Their Brain Malformation Syndromes: Every TUB on Its Own Bottom" .
-
Paronychia
Wikipedia
Retrieved 2006-07-12 . v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Bacterial skin disease Gram +ve Firmicutes Staphylococcus Staphylococcal scalded skin syndrome Impetigo Toxic shock syndrome Streptococcus Impetigo Cutaneous group B streptococcal infection Streptococcal intertrigo Cutaneous Streptococcus iniae infection Erysipelas / Chronic recurrent erysipelas Scarlet fever Corynebacterium Erythrasma Listeriosis Clostridium Gas gangrene Dermatitis gangrenosa Mycoplasma Erysipeloid of Rosenbach Actinobacteria Mycobacterium-related: Aquarium granuloma Borderline lepromatous leprosy Borderline leprosy Borderline tuberculoid leprosy Buruli ulcer Erythema induratum Histoid leprosy Lepromatous leprosy Leprosy Lichen scrofulosorum Lupus vulgaris Miliary tuberculosis Mycobacterium avium-intracellulare complex infection Mycobacterium haemophilum infection Mycobacterium kansasii infection Papulonecrotic tuberculid Primary inoculation tuberculosis Rapid growing mycobacterium infection Scrofuloderma Tuberculosis cutis orificialis Tuberculosis verrucosa cutis Tuberculous cellulitis Tuberculous gumma Tuberculoid leprosy Cutaneous actinomycosis Nocardiosis Cutaneous diphtheria infection Arcanobacterium haemolyticum infection Group JK corynebacterium sepsis Gram -ve Proteobacteria α: Endemic typhus Epidemic typhus Scrub typhus North Asian tick typhus Queensland tick typhus Flying squirrel typhus Trench fever Bacillary angiomatosis African tick bite fever American tick bite fever Rickettsia aeschlimannii infection Rickettsialpox Rocky Mountain spotted fever Human granulocytotropic anaplasmosis Human monocytotropic ehrlichiosis Flea-borne spotted fever Japanese spotted fever Mediterranean spotted fever Flinders Island spotted fever Verruga peruana Brill–Zinsser disease Brucellosis Cat-scratch disease Oroya fever Ehrlichiosis ewingii infection β: Gonococcemia / Gonorrhea / Primary gonococcal dermatitis Melioidosis Cutaneous Pasteurella hemolytica infection Meningococcemia Glanders Chromobacteriosis infection γ: Pasteurellosis Tularemia Vibrio vulnificus Rhinoscleroma Haemophilus influenzae cellulitis Pseudomonal pyoderma / Pseudomonas hot-foot syndrome / Hot tub folliculitis / Ecthyma gangrenosum / Green nail syndrome Q fever Salmonellosis Shigellosis Plague Granuloma inguinale Chancroid Aeromonas infection ε: Helicobacter cellulitis Other Syphilid Syphilis Chancre Yaws Pinta Bejel Chlamydia infection Leptospirosis Rat-bite fever Lyme disease Lymphogranuloma venereum Unspecified pathogen Abscess Periapical abscess Boil/furuncle Hospital furunculosis Carbuncle Cellulitis Paronychia / Pyogenic paronychia Perianal cellulitis Acute lymphadenitis Pilonidal cyst Pyoderma Folliculitis Superficial pustular folliculitis Sycosis vulgaris Pimple Ecthyma Pitted keratolysis Trichomycosis axillaris Necrotizing fascitis Gangrene Chronic undermining burrowing ulcers Fournier gangrene Elephantiasis nostras Blistering distal dactylitis Botryomycosis Malakoplakia Gram-negative folliculitis Gram-negative toe web infection Pyomyositis Blastomycosis-like pyoderma Bullous impetigo Chronic lymphangitis Recurrent toxin-mediated perineal erythema Tick-borne lymphadenopathy Tropical ulcer v t e Disorders of skin appendages Nail thickness: Onychogryphosis Onychauxis color: Beau's lines Yellow nail syndrome Leukonychia Azure lunula shape: Koilonychia Nail clubbing behavior: Onychotillomania Onychophagia other: Ingrown nail Anonychia ungrouped: Paronychia Acute Chronic Chevron nail Congenital onychodysplasia of the index fingers Green nails Half and half nails Hangnail Hapalonychia Hook nail Ingrown nail Lichen planus of the nails Longitudinal erythronychia Malalignment of the nail plate Median nail dystrophy Mees' lines Melanonychia Muehrcke's lines Nail–patella syndrome Onychoatrophy Onycholysis Onychomadesis Onychomatricoma Onychomycosis Onychophosis Onychoptosis defluvium Onychorrhexis Onychoschizia Platonychia Pincer nails Plummer's nail Psoriatic nails Pterygium inversum unguis Pterygium unguis Purpura of the nail bed Racquet nail Red lunulae Shell nail syndrome Splinter hemorrhage Spotted lunulae Staining of the nail plate Stippled nails Subungual hematoma Terry's nails Twenty-nail dystrophy Hair Hair loss / Baldness noncicatricial alopecia : Alopecia areata totalis universalis Ophiasis Androgenic alopecia (male-pattern baldness) Hypotrichosis Telogen effluvium Traction alopecia Lichen planopilaris Trichorrhexis nodosa Alopecia neoplastica Anagen effluvium Alopecia mucinosa cicatricial alopecia : Pseudopelade of Brocq Central centrifugal cicatricial alopecia Pressure alopecia Traumatic alopecia Tumor alopecia Hot comb alopecia Perifolliculitis capitis abscedens et suffodiens Graham-Little syndrome Folliculitis decalvans ungrouped: Triangular alopecia Frontal fibrosing alopecia Marie Unna hereditary hypotrichosis Hypertrichosis Hirsutism Acquired localised generalised patterned Congenital generalised localised X-linked Prepubertal Acneiform eruption Acne Acne vulgaris Acne conglobata Acne miliaris necrotica Tropical acne Infantile acne / Neonatal acne Excoriated acne Acne fulminans Acne medicamentosa (e.g., steroid acne ) Halogen acne Iododerma Bromoderma Chloracne Oil acne Tar acne Acne cosmetica Occupational acne Acne aestivalis Acne keloidalis nuchae Acne mechanica Acne with facial edema Pomade acne Acne necrotica Blackhead Lupus miliaris disseminatus faciei Rosacea Perioral dermatitis Granulomatous perioral dermatitis Phymatous rosacea Rhinophyma Blepharophyma Gnathophyma Metophyma Otophyma Papulopustular rosacea Lupoid rosacea Erythrotelangiectatic rosacea Glandular rosacea Gram-negative rosacea Steroid rosacea Ocular rosacea Persistent edema of rosacea Rosacea conglobata variants Periorificial dermatitis Pyoderma faciale Ungrouped Granulomatous facial dermatitis Idiopathic facial aseptic granuloma Periorbital dermatitis SAPHO syndrome Follicular cysts " Sebaceous cyst " Epidermoid cyst Trichilemmal cyst Steatocystoma simplex multiplex Milia Inflammation Folliculitis Folliculitis nares perforans Tufted folliculitis Pseudofolliculitis barbae Hidradenitis Hidradenitis suppurativa Recurrent palmoplantar hidradenitis Neutrophilic eccrine hidradenitis Ungrouped Acrokeratosis paraneoplastica of Bazex Acroosteolysis Bubble hair deformity Disseminate and recurrent infundibulofolliculitis Erosive pustular dermatitis of the scalp Erythromelanosis follicularis faciei et colli Hair casts Hair follicle nevus Intermittent hair–follicle dystrophy Keratosis pilaris atropicans Kinking hair Koenen's tumor Lichen planopilaris Lichen spinulosus Loose anagen syndrome Menkes kinky hair syndrome Monilethrix Parakeratosis pustulosa Pili ( Pili annulati Pili bifurcati Pili multigemini Pili pseudoannulati Pili torti ) Pityriasis amiantacea Plica neuropathica Poliosis Rubinstein–Taybi syndrome Setleis syndrome Traumatic anserine folliculosis Trichomegaly Trichomycosis axillaris Trichorrhexis ( Trichorrhexis invaginata Trichorrhexis nodosa ) Trichostasis spinulosa Uncombable hair syndrome Wooly hair nevus Sweat glands Eccrine Miliaria Colloid milium Miliaria crystalline Miliaria profunda Miliaria pustulosa Miliaria rubra Occlusion miliaria Postmiliarial hypohidrosis Granulosis rubra nasi Ross’ syndrome Anhidrosis Hyperhidrosis Generalized Gustatory Palmoplantar Apocrine Body odor Chromhidrosis Fox–Fordyce disease Sebaceous Sebaceous hyperplasia
-
Reactive Arthritis
Wikipedia
The arthritis often is coupled with other characteristic symptoms; this was previously referred to as Reiter's syndrome, Reiter's disease or Reiter's arthritis. ... The classical presentation of the syndrome starts with urinary symptoms such as burning pain on urination ( dysuria ) or an increased frequency of urination. ... Ocular involvement (mild bilateral conjunctivitis) occurs in about 50% of men with urogenital reactive arthritis syndrome and about 75% of men with enteric reactive arthritis syndrome. ... Tests for C-reactive protein and erythrocyte sedimentation rate are non-specific tests that can be done to corroborate the diagnosis of the syndrome. A blood test for the genetic marker HLA-B27 may also be performed. ... Retrieved January 24, 2017 . ^ Mayo Staff (March 5, 2011). "Reactive Arthritis (Reiter's Syndrome)" . Mayo Clinic . Retrieved May 16, 2011 . ^ H.HLA-B, IFNG, TRBV20OR9-2, IL17A, TNF, TAP2, HSPD1, HLA-DRB1, TRB, TLR4, CCR5, SLC11A1, CRP, RBM45, IL10, TP53, CDR3, TLR2, USO1, MARCO, PDLIM7, RPL23, BCL2, NCR2, NXF1, HPLH1, TRBV16, TRBV7-9, TRBC1, HSPA14, IL23A, KIR2DL5A, TET1, PCBD2, CTHRC1, SEC14L2, CCL21, TAP1, SOD2, COMP, CRYGD, CYP1A1, FHL1, FLNB, FN1, GLI2, CFH, HLA-C, HRAS, HSPA1L, IL2RA, IL4, CXCL8, IL18, ISG20, KIR2DL1, KIR2DL2, KIR2DS1, MARK1, MMP3, PTGS2, CXCL5, KIR2DL5B
-
Cerebellar Cognitive Affective Syndrome
Wikipedia
Cognitive and affective symptoms of cerebellum damage Cerebellar cognitive affective syndrome Other names Schmahmann's syndrome Specialty Neurology Cerebellar cognitive affective syndrome ( CCAS ), also called Schmahmann's syndrome [1] is a condition that follows from lesions (damage) to the cerebellum of the brain. ... Underdiagnosis may reflect lack of familiarity of this syndrome in the scientific and medical community. ... References [ edit ] ^ Manto M, Mariën P. Schmahmann’s syndrome - identification of the third cornerstone of clinical ataxiology. ... The cerebellar cognitive affective syndrome. Brain , 121 , 561-579. ^ a b c d e f g Levisohn, L., Cronin-Golomb, A. & Schmahmann, J. ... The cerebellar cognitive affective syndrome: Clinical correlations of the dysmetria of thought hypothesis.
-
Hirsutism
Wikipedia
Ovarian cysts such as in polycystic ovary syndrome (PCOS), the most common cause in women. [9] Ovarian tumors such as granulosa tumors , thecomas , Sertoli–Leydig cell tumors (androblastomas), and gynandroblastomas , as well as ovarian cancer . ... Diagnosis of patients with even mild hirsutism should include assessment of ovulation and ovarian ultrasound , due to the high prevalence of polycystic ovary syndrome (PCOS) , as well as 17α-hydroxyprogesterone (because of the possibility of finding nonclassic 21-hydroxylase deficiency [15] ). ... See also [ edit ] Ferriman-Gallwey score Petrus Gonsalvus Androgenic hair Pubic hair Hypertrichosis Hair removal Laser hair removal Bearded lady Trichophilia Polycystic ovary syndrome (PCOS) References [ edit ] ^ a b c Barrionuevo, P; Nabhan, M; Altayar, O; Wang, Z; Erwin, PJ; Asi, N; Martin, KA; Murad, MH (1 April 2018). ... S2CID 34029116 . ^ a b c d Unluhizarci K, Kaltsas G, Kelestimur F (2012). "Non polycystic ovary syndrome-related endocrine disorders associated with hirsutism". ... "High prevalence of polycystic ovary syndrome in women with mild hirsutism and no other significant clinical symptoms" (PDF) .POMC, ARSB, OFD1, BSCL2, NIPBL, ABCA5, ADNP, DHX30, POLR3A, SRCAP, AGPAT2, LRPPRC, ABCC9, H6PD, ADAMTS2, PLAA, BMP15, SMC3, USP8, PAPSS2, AIP, SETD2, WAC, NANS, NKX6-2, SOX2-OT, ASXL1, ARX, CEP120, CCBE1, HGSNAT, WDR81, LMNB2, UBA5, WNT4, CCDC28B, VPS33A, BCL11B, XYLT1, SHROOM4, HDAC8, FRMD4A, RIN2, CACNA1G, SMC1A, BBS1, FLNA, KCNH1, IDUA, HSD3B2, GUSB, NR3C1, GNS, FUCA1, FSHR, FGFR2, LMNA, ERCC6, EP300, DDX3X, CYP11B1, CREBBP, CDK5, CAV1, BCL2, LIMS1, MAB21L1, KMT2D, SMARCA4, AIMP2, KDM6A, UBE2A, TBX15, TBCD, TAF6, SMARCD2, SMARCB1, SGSH, KMT2A, PRKAR1A, PRKACA, PPARG, POR, NOTCH2, NAGLU, MMP14, MMP2, NPHP3-ACAD11
-
Repetitive Strain Injury
Wikipedia
Repetitive strain injury Other names Cumulative trauma disorders, repetitive stress injuries, repetitive motion injuries or disorders, occupational or sports overuse syndromes Poor ergonomic techniques by computer users is one of many causes of repetitive strain injury Specialty Sports medicine , Performing Arts Medicine , orthopedics Symptoms Sore wrists, aching, pulsing pain, tingling, extremity weakness Complications Torn ligaments Causes Repetitive actions, poor technique Risk factors Sedentary lifestyle, smoking, alcohol consumption Prevention Proper technique, regular rests, regular exercise A repetitive strain injury ( RSI ) is an injury to part of the musculoskeletal or nervous system caused by repetitive use, vibrations, compression or long periods in a fixed position. [1] Other common names include repetitive stress disorders, cumulative trauma disorders (CTDs), and overuse syndrome. [2] Contents 1 Signs and symptoms 1.1 Definition 2 Risk factors 2.1 Occupational risk factors 2.2 Psychosocial factors 2.3 Non-occupational factors 3 Diagnosis 4 Treatment 5 History 6 Society 7 See also 8 Notes 9 External links Signs and symptoms [ edit ] Some examples of symptoms experienced by patients with RSI are aching, pulsing pain, tingling and extremity weakness, initially presenting with intermittent discomfort and then with a higher degree of frequency. [3] Definition [ edit ] Repetitive strain injury (RSI) and associative trauma orders are umbrella terms used to refer to several discrete conditions that can be associated with repetitive tasks, forceful exertions, vibrations, mechanical compression, sustained or awkward positions, or repetitive eccentric contractions . [1] [4] [5] The exact terminology is controversial, but the terms now used by the United States Department of Labor and the National Institute of Occupational Safety and Health (NIOSH) are musculoskeletal disorders (MSDs) and work-related muscular skeletal disorders (WMDs). [2] Examples of conditions that may sometimes be attributed to such causes include tendinosis (or less often tendinitis ), carpal tunnel syndrome , cubital tunnel syndrome , De Quervain syndrome , thoracic outlet syndrome , intersection syndrome , golfer's elbow (medial epicondylitis), tennis elbow (lateral epicondylitis), trigger finger (so-called stenosing tenosynovitis), radial tunnel syndrome , ulnar tunnel syndrome , and focal dystonia . [1] [5] [6] A general worldwide increase since the 1970s in RSIs of the arms, hands, neck, and shoulder has been attributed to the widespread use in the workplace of keyboard entry devices, such as typewriters and computers, which require long periods of repetitive motions in a fixed posture. [7] Extreme temperatures have also been reported as risk factor for RSI. [8] Risk factors [ edit ] Occupational risk factors [ edit ] Workers in certain fields are at risk of repetitive strains. ... Pain related to RSI may evolve into chronic pain syndrome particularly for workers who do not have supports from co-workers and supervisors. [13] Non-occupational factors [ edit ] Age and gender are important risk factors for RSIs. ... These include effort-based tests such as grip and pinch strength, diagnostic tests such as Finkelstein's test for De Quervain's tendinitis , Phalen's contortion , Tinel's percussion for carpal tunnel syndrome, and nerve conduction velocity tests that show nerve compression in the wrist. ... In 1700, the Italian physician Bernardino Ramazzini first described RSI in more than 20 categories of industrial workers in Italy, including musicians and clerks. [22] Carpal tunnel syndrome was first identified by the British surgeon James Paget in 1854. [23] The April 1875 issue of The Graphic describes "telegraphic paralysis." [24] The Swiss surgeon Fritz de Quervain first identified De Quervain’s tendinitis in Swiss factory workers in 1895. [25] The French neurologist Jules Tinel (1879–1952) developed his percussion test for compression of the median nerve in 1900. [26] [27] [28] The American surgeon George Phalen improved the understanding of the aetiology of carpal tunnel syndrome with his clinical experience of several hundred patients during the 1950s and 1960s. [29] Society [ edit ] Specific sources of discomfort have been popularly referred to by terms such as Blackberry thumb , PlayStation thumb, [30] Rubik's wrist or "cuber's thumb", [31] stylus finger, [32] and raver's wrist, [33] and Emacs pinky. [34] See also [ edit ] Ergonomic keyboard List of repetitive strain injury software Maltron Microsoft ergonomic keyboards Notes [ edit ] ^ a b c "Public Employees Occupational Safety and Health Program of the New Jersey Department of Health and Senior Services" (PDF) . ... PMID 7266622 . ^ "5 Modern Technology Strain Injuries | Carpal Tunnel Syndrome" . Ctsplace.com. 30 December 2012 .
-
Cold Urticaria
Wikipedia
"Mutation of a new gene encoding a putative pyrin-like protein causes familial cold autoinflammatory syndrome and Muckle-Wells syndrome" . Nat. ... "Familial cold autoinflammatory syndrome" . U.S. National Library of Medicine . ... "Familial Cold Auto-inflammatory Syndrome (FCAS): Fact Sheet" . Regeneron Pharmaceuticals. ... "Familial cold auto-inflammatory syndrome (FCAS): characterization of symptomatology and impact on patients' lives". ... "Anakinra prevents symptoms of familial cold autoinflammatory syndrome and Raynaud's disease" . The Journal of Rheumatology .
-
Alcoholic Hepatitis
Wikipedia
Prednisolone gave a small reduction in mortality at 28 days but this did not reach significance, and there were no improvements in outcomes at 90 days or 1 year. [3] IV N-acetylcysteine: When used in conjunction with corticosteroids, improves survival at 28 days by decreasing rates of infection and hepatorenal syndrome. [3] Liver Transplantation: Early liver transplantation is ideal and helps to save lives. [14] However, patients must remain abstinent from alcohol for 6 months prior to transplantation, but the ethics and science behind this are controversial. [14] See also [ edit ] AST/ALT ratio Lille Model Steatohepatitis References [ edit ] ^ "Alcoholic liver disease: MedlinePlus Medical Encyclopedia" . medlineplus.gov . ... "Liver Disease in Heavy Drinkers With and Without Alcohol Withdrawal Syndrome". Alcoholism: Clinical & Experimental Research . 28 (1): 131–136. doi : 10.1097/01.ALC.0000106301.39746.EB . ... External links [ edit ] Classification D ICD - 10 : K70.1 ICD - 9-CM : 571.1 MeSH : D006519 External resources MedlinePlus : 000281 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum v t e Alcohol and health Alcohol use Alcohol-related crimes Drunk drivers Alcohol-related traffic crashes in the United States Driving under the influence (DUI) Drunk driving in the United States Public intoxication Rum-running Adulterated moonshine / Denatured alcohol List of methanol poisoning incidents Alcoholism Alcohol and Native Americans Alcoholism in adolescence Alcoholism in family systems Collaborative Study on the Genetics of Alcoholism College student alcoholism Disease theory of alcoholism High-functioning alcoholic (HFA) Seeing pink elephants Chemistry Beer chemistry Congener Alcohol congener analysis Ethanol Blood alcohol content Breathalyzer Fusel alcohol Wine chemistry Effects Short-term effects of alcohol consumption Long-term effects of alcohol On memory Subjective response to alcohol Interactions Aging Brain Cancer breast cancer Cortisol Pregnancy Sleep Tolerance / intolerance Weight Beverage-specific Beer: Potomania Red wine: Red wine headache Social issues Alcohol advertising on college campuses Sex Alcohol myopia Alcohol abuse among college students Binge drinking Epidemiology Blackout (alcohol-related amnesia) Blackout Wednesday Drinking game list pregaming Drinking in public Drunk dialing Drunk walking Drunkorexia Dry drunk French paradox Hair of the dog Nightcap Pantsdrunk Passive drinking Binge drinking devices Beer bong Yard of ale Routes of administration Alcohol enema Alcohol inhalation Sconcing Surrogate alcohol Related issues Balconing Suicide History Dionysian Mysteries Dipsomania Gin Craze List of deaths through alcohol Rum ration Speakeasy General Beer day Drinking culture Apéritif and digestif Hangover remedies Health effects of wine Wine and food matching Long-distance race involving alcohol List of countries by alcohol consumption per capita Alcohol consumption by youth in the United States Nip joint Alcohol control Alcohol law Administrative license suspension (ALS) Alcohol packaging warning messages Drunk driving law by country DWI court Field sobriety testing Hip flask defence Ignition interlock device Legal drinking age Age controversy in US Underage drinking in US List of alcohol laws of US Alcohol prohibition List of countries with alcohol prohibition Neo-prohibitionism Temperance movement Sobriety Alcohol detoxification Alcohol-free zone Dry campus United States open-container laws Designated driver Alcohol rehabilitation Drunk tank Managed alcohol program Non-alcoholic drink List of cocktails List of mixed drinks Spritzer Malt drinks Teetotalism Temperance bar Twelve-step groups Al-Anon/Alateen Alcoholics Anonymous (AA): Adult Children of Alcoholics (ACA) Alcohol limitation 0-0-1-3 Alcohol education Alcohol server training FRAMES Dry January Foundation for Advancing Alcohol Responsibility Campaigns Get Your Sexy Back Liquor license Low-alcohol drinks Fermented tea Low-alcohol beer Low-alcoholic malt drinks Small beer Measurement Alcoholic spirits measure Standard drink Recommended maximum intake of alcoholic beverages Addiction medicine Disulfiram-like drugs : disulfiram , calcium carbimide , cyanamide . Sulfonic acids : Acamprosate Religion and alcohol Christian views on alcohol alcohol in the Bible Islam and alcohol History Bratt System Related Index of alcohol-related articles Austrian syndrome Ban on caffeinated alcoholic beverages Brief intervention Gateway drug effect Last call Mood disorder Non-alcoholic fatty liver disease Self-medication Spins Sober companion Sober living houses Sobering center Town drunk CategoryTNF, CXCL8, CCL5, STS, SULT1E1, DDC, CSF3, TLR4, ALB, CCL2, PNPLA3, IL22, ACKR3, CXCR2, ITGB2, PIK3CD, SIRT1, PIK3CA, PIK3CB, PIK3CG, CCL4, SYK, IL1A, ACTB, IL17A, BRCA1, FOXO1, SQSTM1, MIR21, MIR29C, MIR30E, KHDRBS1, MRPL28, UBD, EBI3, FGF19, CCL4L2, MIR34A, MIR483, SUB1, POTEF, IL18R1, TFEB, CXCR4, UCP2, LINC01093, TP53, TNFRSF1A, MTCO2P12, MIR192, HCAR2, TICAM1, TLR9, TRIM69, NOSTRIN, CCL4L1, GSDMD, WNK1, UFSP1, GORASP1, CIDEC, MIRLET7B, MIR132, TLR3, NUP62, UFM1, SIRT6, MIR141, UFC1, TNFRSF12A, TLR7, DCTN4, MIR148A, NXT1, SLC17A5, MIR182, CXCL11, TLR2, TGFB1, IL1RN, IL1B, IFNA13, IFNA1, ICAM1, HNF4A, HLA-B, HGF, GTF2H1, GCG, GC, GAPDH, ECE1, DNMT3B, DNMT1, CYP7A1, CSF3R, CDKN2B, CDK1, CD74, CD69, CD14, CAV1, ATF3, APOA1, IL6, IL10, IRF3, PRNP, TCF4, ADAM17, SYT1, SPP1, SMPD1, TRA2B, AGA, CCL3, S100A4, RELA, PTX3, PPARG, IRF7, PMCH, NM, NAIP, MYD88, MYC, COX2, MMP7, MIP, MIF, EPCAM, ITPR3, H3P9
-
I-Cell Disease
Wikipedia
Contents 1 Signs and symptoms 2 Pathophysiology 3 Diagnosis 4 Treatment 5 References 6 External links Signs and symptoms [ edit ] Mucolipidosis II (ML II) is a particularly severe form of ML that has a significant resemblance to another mucopolysaccharidosis called Hurler syndrome . Generally only laboratory testing can distinguish the two as the presentation is so similar, with high plasma concentrations of lysosomal enzymes, often fatal in childhood. [4] Typically, by the age of 6 months, failure to thrive and developmental delays are obvious signs of this disorder. ... These young patients are often plagued by recurrent respiratory tract infections, including pneumonia , otitis media (middle ear infections), bronchitis and carpal tunnel syndrome . Children with ML II generally die before their seventh year of life, often as a result of congestive heart failure or recurrent respiratory tract infections. ... It can be associated with N-acetylglucosamine-1-phosphate transferase (GNPTA). [6] In a case report, I-cell disease was complicated by severe dilative cardiomyopathy (DCM). [7] Though rare, a deficiency of phosphodiesterase which would cleave GlcNAc from the mannose-6-phosphate tag will also cause I-cell disease. [5] The presence of lipids, glycosaminoglycans (GAG's) and carbohydrates in the blood provide for the distinguishing characteristic to separate I-cell from Hurler Syndrome . In Hurler's, only glycosaminoglycans would be present. ... External links [ edit ] Classification D ICD - 10 : E77.0 ICD - 9-CM : 272.7 OMIM : 252500 MeSH : D009081 DiseasesDB : 29175 External resources eMedicine : ped/1150 GeneReviews : Mucolipidosis II mucolipidoses at NINDS — article derived from detail sheet available here I cell disease at NIH 's Office of Rare Diseases GeneReview/NIH/UW entry on Mucolipidosis II v t e Lysosomal storage diseases : Inborn errors of carbohydrate metabolism ( Glycoproteinoses ) Anabolism Dolichol kinase deficiency Congenital disorder of glycosylation Post-translational modification of lysosomal enzymes Mucolipidosis : I-cell disease (ML II) Pseudo-Hurler polydystrophy (ML III) Catabolism Aspartylglucosaminuria Fucosidosis mannosidosis Alpha-mannosidosis Beta-mannosidosis Sialidosis Schindler disease Other solute carrier family ( Salla disease ) Galactosialidosis v t e Disorders of translation and posttranslational modification Translation Ribosome : Diamond–Blackfan anemia FMR1 Fragile X syndrome Fragile X-associated tremor/ataxia syndrome Premature ovarian failure 1 Initiation factor : Leukoencephalopathy with vanishing white matter snRNP : Retinitis pigmentosa 33 Posttranslational modification Protein folding Alzheimer's disease Huntington's disease Creutzfeldt–Jakob disease chaperonins: 3-Methylglutaconic aciduria 5 Protein targeting I-cell disease Ubiquitin E1 : X-linked spinal muscular atrophy 2 E3 : Johanson–Blizzard syndrome Von Hippel–Lindau disease 3-M syndrome Angelman syndrome Deubiquitinating enzyme : Machado–Joseph disease Aneurysmal bone cyst Multiple familial trichoepithelioma 1 SUMO OFC10 Other Multiple sulfatase deficiency Hyperproinsulinemia Ehlers–Danlos syndrome 6
-
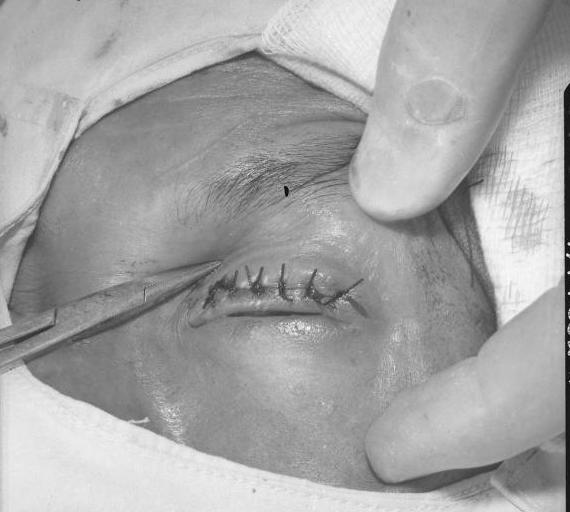
Entropion
Wikipedia
External links [ edit ] Classification D ICD - 10 : H02.0 , Q10.2 ICD - 9-CM : 374.0 MeSH : D004774 DiseasesDB : 29643 External resources MedlinePlus : 001008 eMedicine : oph/212 Humans Medline Plus - Entropion v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis v t e Congenital malformations and deformations of eyes Adnexa Eyelid Ptosis Ectropion Entropion Distichia Blepharophimosis Ablepharon Marcus Gunn phenomenon Lacrimal apparatus Congenital lacrimal duct obstruction Globe Entire eye Anophthalmia ( Cystic eyeball , Cryptophthalmos ) Microphthalmia Lens Ectopia lentis Aphakia Iris Aniridia Anterior segment Axenfeld–Rieger syndrome Cornea Keratoglobus Megalocornea Other Buphthalmos Coloboma ( Coloboma of optic nerve ) Hydrophthalmos Norrie disease
-
Exanthem
Wikipedia
It was described in 1900 and is postulated to be related to the bacterium Staphylococcus aureus . [9] In 1979 and 2001 a possible "seventh diease" was postulated following reports of a condition in Japan also referred to as acute febrile infantile mucocutaneous lymph node syndrome (MCLS). [11] Many other common viruses apart from the ones mentioned above can also produce an exanthem as part of their presentation, though they are not considered part of the classic numbered list: Varicella zoster virus ( chickenpox or shingles ) Mumps rhinovirus (the common cold) unilateral laterothoracic exanthem of childhood Some types of viral haemorrhagic fever are also known to produce a systemic rash of this kind during the progression of the disease. ... ISSN 1756-1833 . ^ https://www.cdc.gov/mmwr/pdf/r/rr5504.pdf External links [ edit ] Classification D ICD - 10 : A38 , B05 - B09 ICD - 9-CM : 034 , 055 - 057 , 782.1 MeSH : D005076 DiseasesDB : 25831 Overview at About.com Definition at MedTerms Differential diagnosis Dermatology Quiz Includes photo, diagnosis, and treatment of unilateral laterothoracic exanthem (ULE). v t e Numbered Diseases of Childhood Diseases First Disease (Measles) Second Disease (Scarlet Fever) Third Disease (Rubella) Fourth Disease (Dukes' Disease) Fifth Disease (Erythema Infectiosum) Sixth Disease (Roseola) v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Skin infections , symptoms and signs related to viruses DNA virus Herpesviridae Alpha HSV Herpes simplex Herpetic whitlow Herpes gladiatorum Herpes simplex keratitis Herpetic sycosis Neonatal herpes simplex Herpes genitalis Herpes labialis Eczema herpeticum Herpetiform esophagitis Herpes B virus B virus infection VZV Chickenpox Herpes zoster Herpes zoster oticus Ophthalmic zoster Disseminated herpes zoster Zoster-associated pain Modified varicella-like syndrome Beta Human herpesvirus 6 / Roseolovirus Exanthema subitum Roseola vaccinia Cytomegalic inclusion disease Gamma KSHV Kaposi's sarcoma Poxviridae Ortho Variola Smallpox Alastrim MoxV Monkeypox CPXV Cowpox VV Vaccinia Generalized vaccinia Eczema vaccinatum Progressive vaccinia Buffalopox Para Farmyard pox : Milker's nodule Bovine papular stomatitis Pseudocowpox Orf Sealpox Other Yatapoxvirus : Tanapox Yaba monkey tumor virus MCV Molluscum contagiosum Papillomaviridae HPV Wart / plantar wart Heck's disease Genital wart giant Laryngeal papillomatosis Butcher's wart Bowenoid papulosis Epidermodysplasia verruciformis Verruca plana Pigmented wart Verrucae palmares et plantares BPV Equine sarcoid Parvoviridae Parvovirus B19 Erythema infectiosum Reticulocytopenia Papular purpuric gloves and socks syndrome Polyomaviridae Merkel cell polyomavirus Merkel cell carcinoma RNA virus Paramyxoviridae MeV Measles Togaviridae Rubella virus Rubella Congenital rubella syndrome ("German measles" ) Alphavirus infection Chikungunya fever Picornaviridae CAV Hand, foot, and mouth disease Herpangina FMDV Foot-and-mouth disease Boston exanthem disease Ungrouped Asymmetric periflexural exanthem of childhood Post-vaccination follicular eruption Lipschütz ulcer Eruptive pseudoangiomatosis Viral-associated trichodysplasia Gianotti–Crosti syndromeHLA-B, MVK, C1QA, IL1RN, NOD2, GJA1, NLRP3, HLA-DRB1, CTLA4, PIK3R1, APOA1, SDHB, KRT5, TRPS1, KDSR, FGA, FBN1, NAXD, MEFV, EGFR, ERCC5, ERCC4, ERCC3, ERCC2, TNFRSF1B, TNFRSF1A, ENPP1, LBR, GJB3, GLUL, IL17RA, IGLL1, IGHM, PTPN22, IL6, RFXANK, CIITA, IKBKG, BLNK, SPINK5, POMP, ZAP70, HLCS, HLA-DPB1, HLA-DPA1, DNASE1L3, PDGFRA, LMBRD1, SMARCAD1, LRRC8A, MIF, CD28, RFX5, GJB4, BTK, BTD, RFXAP, KIT, LACC1, B2M, TEK, TCF3, ABCC6, SLC6A19, STAT3, SDHA, AK2, SDHC, RAG2, IL2RG, IL17F, LYZ, NLRC4, PRTN3, DCLRE1C, CLEC7A, PSMB4, PSMB8, PSMB9, COX4I2, IL17RC, TRAF3IP2, JAK3, CD79B, CD79A, NLRP12, RAG1, TP53, GPT, HLA-A, PTH1R, RUNX2, EGF, IFNG, NAT2, PIK3CA, CCR4, PTHLH, BRAF, TNFRSF11A, TNFSF11, PTH, PAEP, CD274, KRAS, IL5, CARD14, FAM20A, CSF3, GH1, HPGDS, TNFRSF8, AREG, ADNP, SYP, TSLP, TRIM21, SST, STAT1, SPRTN, TNF, CDAGS, HAVCR2, TGFB1, IL33, MIR126, MUC16, MIR31, MIR146A, TGFA, IL21, TIRAP, RBM45, UNC13D, IFIH1, ASPN, ENOSF1, ODAM, PGRMC1, GNLY, MRPL28, SUB1, SAE1, ADAMTS1, SDS, SATB2, RECQL4, DIRAS3, NAE1, IL1RL2, SMUG1, ABCB11, NXT1, SMN2, IL22, SIRT6, ARID4B, XRCC1, UBASH3A, TPI1, CCL27, SOD1, A1BG, SMN1, SMARCB1, CYBB, CYP2C9, CYP2E1, CYP27B1, NQO1, DLX4, DMP1, DSG1, EEC1, EIF4EBP1, ENO1, EREG, ESAT, GATA1, GNRH1, HMGB1, HSPA8, IAPP, IDH1, CTSK, CSTA, MAPK14, SERPING1, ACTB, AKT1, ALPP, AMBN, AR, RHOH, BCL6, BST2, CASP3, CRYZ, CD1A, CD34, CD44, CD68, CDKN2B, CFTR, CKB, CPA1, IDH2, IFNA1, IFNA13, PTEN, TNFRSF11B, PDCD1, CFP, ABCB1, PHB, PIK3CB, PIK3CD, PIK3CG, PTGS2, NPHS1, PLAAT4, SERPINB4, CCL11, CCL17, CCL22, SDHD, SLC1A3, SLC22A1, OPA1, NM, CCN1, LDHB, IL1B, IL2, IL4, CXCL8, IL9, IL10, IL17A, CXCL10, LGALS3, MTRR, LGALS9, LHCGR, ADAM11, MECP2, KMT2A, MMP2, MMP9, MPO, H3P9
-
Premature Atrial Contraction
Wikipedia
External links [ edit ] Classification D ICD - 10 : I49.1 ICD - 9-CM : 427.61 MeSH : D018880 v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic feverSCN5A, GJA5, CTNNB1, APC, MUTYH, TP53, KCNE2, TTN, KRAS, GSTP1, DCC, BRCA2, BRCA1, CDH1, TNKS, PIK3CD, PIK3CB, MGMT, MLH1, CXCL8, MYC, PIK3CA, MCC, PIK3CG, CDKN2A, MIR135B, RASSF1, FAP, AFAP1, HNF4A, IL10, IL15, CXCR4, MAPRE1, LEF1, ARHGEF4, REEP5, FOXO1, PTGS2, APC2, ACTB, H3P10, DNMT1, F2R, GAST, SPEN, OLFM4, NES, KIF3A, APP, WIF1, APOH, PPRC1, ARSA, MKRN1, IL17RA, CHD5, SND1, SLC25A24, IL22, YAP1, ABCB6, AKT1, BCL2L11, CCND1, SMAD5-AS1, KLF4, CCN5, TNFSF9, BCL2, DEGS1, LGR5, AXIN2, MIA, PLA2G7, BLM, USP7, ANXA5, NLK, UBR5, GRK3, MIR155, MIR205, MIR21, MIR27A, MIR31, MIR34A, MIR375, XPO1, MIR582, CEMP1, CD24, LINC01133, MIA-RAB4B, SNORD138, MIR126, MIR106A, FMN1, CISD3, HCA1, C9orf72, PPM1L, IL33, VANGL1, PALB2, CDC73, ANAPC1, RHBDF1, AFP, IL21, PRX, PACC1, BRAF, CAV1, TRPV1, MSH2, MDM2, MET, DLD, CYP2A7, NR3C2, MRC1, MSH3, SERPINE1, MSI1, MUC1, CTBP1, CSF2, ODC1, OGG1, DMBT1, SMAD4, LAMA3, IRF1, ILK, TNFRSF9, EGFR, EMP2, ERBB4, IL6, IFNA13, IFNA1, ESR1, HDAC2, H2AX, GLI3, GLI1, PAFAH1B1, ABCB1, FEN1, STAT1, CCL2, CCL21, CXCL12, SGK1, SOAT1, SOX9, TCF4, CCR7, TCF7L2, PPP1R11, TFAM, TGFB2, TNF, CBR1, CD44, RET, RAC1, CD74, PTEN, PTCH1, ACTC1, PROS1, PROC, PPARG, PPARD, POLB, PLK1, PLG, CDKN2D, CEACAM5, CHEK1, PSMD10
-
Pulseless Electrical Activity
Wikipedia
External links [ edit ] Classification D ICD - 10 : I46.9 ICD - 9-CM : 427.9 DiseasesDB : 4166 External resources eMedicine : med/2963 v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever
-
Wrist Drop
Wikipedia
Nerve entrapment most frequently occurs at the wrist (carpal tunnel syndrome) and elbow (ulnar nerve entrapment). ... CS1 maint: multiple names: authors list ( link ) v t e Acquired musculoskeletal deformities Upper limb shoulder Winged scapula Adhesive capsulitis Rotator cuff tear Subacromial bursitis elbow Cubitus valgus Cubitus varus hand deformity Wrist drop Boutonniere deformity Swan neck deformity Mallet finger Lower limb hip Protrusio acetabuli Coxa valga Coxa vara leg Unequal leg length patella Luxating patella Chondromalacia patellae Patella baja Patella alta foot deformity Bunion/hallux valgus Hallux varus Hallux rigidus Hammer toe Foot drop Flat feet Club foot knee Genu recurvatum Head Cauliflower ear General terms Valgus deformity / Varus deformity Joint stiffness Ligamentous laxity v t e Diseases relating to the peripheral nervous system Mononeuropathy Arm median nerve Carpal tunnel syndrome Ape hand deformity ulnar nerve Ulnar nerve entrapment Froment's sign Ulnar tunnel syndrome Ulnar claw radial nerve Radial neuropathy Wrist drop Cheiralgia paresthetica long thoracic nerve Winged scapula Backpack palsy Leg lateral cutaneous nerve of thigh Meralgia paraesthetica tibial nerve Tarsal tunnel syndrome plantar nerve Morton's neuroma superior gluteal nerve Trendelenburg's sign sciatic nerve Piriformis syndrome Cranial nerves See Template:Cranial nerve disease Polyneuropathy and Polyradiculoneuropathy HMSN Charcot–Marie–Tooth disease Dejerine–Sottas disease Refsum's disease Hereditary spastic paraplegia Hereditary neuropathy with liability to pressure palsy Familial amyloid neuropathy Autoimmune and demyelinating disease Guillain–Barré syndrome Chronic inflammatory demyelinating polyneuropathy Radiculopathy and plexopathy Brachial plexus injury Thoracic outlet syndrome Phantom limb Other Alcoholic polyneuropathy Other General Complex regional pain syndrome Mononeuritis multiplex Peripheral neuropathy Neuralgia Nerve compression syndrome
-
Hemoglobin Lepore Syndrome
Wikipedia
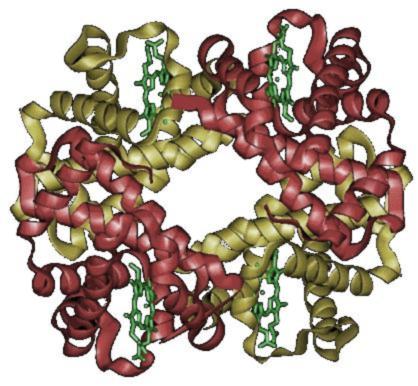
Hemoglobin Lepore syndrome Other names Hb Lepore syndrome A crossover between the delta and beta globin gene loci results in the mutation which causes the Hb Lepore trait . Hemoglobin Lepore syndrome is typically an asymptomatic hemoglobinopathy , which is caused by an autosomal recessive genetic mutation . ... Despite not causing identifiable symptoms a silent stroke still causes damage to the brain, and places the patient at increased risk for both transient ischemic attack and major stroke in the future. [6] Cause [ edit ] Sickle cell-Hb Lepore Boston syndrome is a type of sickle cell disease (HbS) that differs from homozygous sickle cell disease where both parents carry sickle hemoglobin. In this variant one parent has the sickle cell hemoglobin the second parent has Hb Lepore Boston, the only one of the three variants described in association with HbS. [7] Diagnosis [ edit ] The diagnosis of Hb Lepore syndrome may be performed antenatally or postnatally via the use of a variety of tests Complete blood count (CBC) Cation Exchange High-performance liquid chromatography (CE-HPLC): a chromatographic technique used to separate and quantify various normal and abnormal hemoglobin components in blood. [8] Hemoglobin electrophoresis DNA analysis [9] Treatment [ edit ] Homozygous Hb Lepore [ edit ] Those homozygous (Hb LeporeLepore; a very rare situation) or compound heterozygous (Hb Lepore-Β-thalassaemia) might suffer from a severe anaemia. ... PMID 20453400 . ^ Stevens MC, Lehmann H, Mason KP (January 1982). "Sickle cell-Hb Lepore Boston syndrome. Uncommon differential diagnosis to homozygous sickle cell disease".
-
Polyhydramnios
Wikipedia
In a multiple gestation pregnancy, the cause of polyhydramnios usually is twin-to-twin transfusion syndrome . Maternal causes include cardiac problems, kidney problems, and maternal diabetes mellitus , which causes fetal hyperglycemia and resulting polyuria (fetal urine is a major source of amniotic fluid). ... This results in the stomach protrusion up into the thoracic cavity, and the fetus is unable to swallow sufficient amounts of amniotic fluid. fetal renal disorders that result in increased urine production during pregnancy, such as in antenatal Bartter syndrome . [7] Molecular diagnosis is available for these conditions. [8] neurological abnormalities such as anencephaly , which impair the swallowing reflex. ... If the rostral neuropore fails to close there will be no neural mechanism for swallowing. chromosomal abnormalities such as Down syndrome and Edwards syndrome , which is itself often associated with gastrointestinal abnormalities. ... "An improved terminology and classification of Bartter-like syndromes". Nat Clin Pract Nephrol . 4 (10): 560–7. doi : 10.1038/ncpneph0912 . ... S2CID 205340294 . ^ "Hereditary disease: Bartter syndrome" . Moldiag.de . Retrieved 2012-09-28 . ^ Piantelli G, Bedocchi L, Cavicchioni O, et al. (2004).IGF2, MAGEL2, MAMLD1, CD96, ZMPSTE24, TRAIP, KLHL41, SPINT2, EBP, MAGED2, SLC35D1, BICD2, KAT6B, PIGN, LMOD1, SIN3A, PHGDH, NPHP3, BBS9, PSAT1, ASCC1, DYNC2LI1, MAP3K20, PRMT7, TMCO1, MAFB, ACTA1, KIAA0586, PHOX2B, UFD1, WNT3, YWHAE, BSND, SHOC2, LZTR1, CNTNAP1, CDK13, TP63, DPM2, BUB3, PIEZO1, HACD1, TRIP13, TRIP11, EFTUD2, LONP1, ADAMTS3, SEC24C, TTC37, CEP57, SEMA3E, FIG4, WDR60, TPM3, HYLS1, SYT2, DIS3L2, KLHL40, AMER1, B3GLCT, CEP120, ESCO2, ASXL1, IBA57, TAPT1, JMJD1C, SLC25A26, NALCN, TSEN54, DOK7, CRB2, RSPO2, GLDN, KIF7, AGRN, KBTBD13, TMEM151B, WDR81, STRADA, TRPV6, TBC1D24, CHD7, FLVCR2, VAC14, KLHL7, SMG9, LMOD3, SELENON, ADGRG6, TTC7A, GATAD2B, KIDINS220, PIGY, AARS2, WDR35, SLC5A7, SOX17, MTMR14, ALG8, ALG12, PALB2, PLVAP, MYPN, HIRA, TPM2, ACTG2, FUT8, SLC26A2, EP300, ERBB3, ERF, FANCB, GPC4, FGFR3, FOXF1, FOXE1, FLNB, GBA, DNM2, GBE1, GPC3, GLE1, GP1BB, HBA1, HBA2, HIC1, HOXD13, HRAS, HSD17B4, SLC26A3, DMPK, INPPL1, CHAT, ALPL, BIN1, AQP2, ARVCF, ASCL1, AVPR2, BRAF, BUB1, BUB1B, CFL2, CHRNA1, DHCR7, CHRND, CHRNG, CLCN7, CLCNKA, CLCNKB, CNTN1, COL2A1, COL13A1, COMT, CREBBP, HSPG2, ITGA6, TBCD, RYR1, PMM2, PRRX1, PTH1R, NECTIN1, RAF1, RAPSN, RET, RIT1, RPL11, RREB1, SLC9A3, PAFAH1B1, SLC12A1, SLC18A3, SLC25A1, SNAP25, SNRPB, SOS1, SOX9, ABCC8, VAMP1, TBX1, PLEC, OTX2, IRF6, MUSK, ITGA7, ITGB4, KCNJ1, KCNJ6, KCNQ1, KRAS, LBR, LMNA, MSX1, MTM1, MYCN, NUP88, MYF6, MYH3, MYH11, MYL2, MYLK, MYO9A, MYOD1, NEB, NOTCH2, NRAS, ZBTB42
-
Lymphoproliferative Disorders
Wikipedia
Contents 1 Lymphoproliferative disorders (examples) 2 Types 2.1 X-linked Lymphoproliferative disorder 2.2 Autoimmune lymphoproliferative disorder 2.3 Other inherited causes 2.4 Acquired causes 2.5 Iatrogenic causes 3 See also 4 References 5 External links Lymphoproliferative disorders (examples) [ edit ] Follicular lymphoma chronic lymphocytic leukemia acute lymphoblastic leukemia hairy cell leukemia Hemophagocytic lymphohistiocytosis (HLH) B-cell lymphomas T-cell lymphomas multiple myeloma Waldenström's macroglobulinemia Wiskott–Aldrich syndrome Langerhans cell histiocytosis (LCH) Lymphocyte-variant hypereosinophilia Pityriasis Lichenoides (PL, PLC, PLVA) post-transplant lymphoproliferative disorder autoimmune lymphoproliferative syndrome (ALPS) "Lymphoid interstitial pneumonia" [1] Epstein–Barr virus-associated lymphoproliferative diseases Castleman disease X-linked lymphoproliferative disease Types [ edit ] Lymphoproliferative disorders are a set of disorders characterized by the abnormal proliferation of lymphocytes into a monoclonal lymphocytosis . ... Autoimmune lymphoproliferative disorder [ edit ] Main article: Autoimmune lymphoproliferative syndrome Some children with autoimmune lymphoproliferative disorders are heterozygous for a mutation in the gene that codes for the Fas receptor , which is located on the long arm of chromosome 10 at position 24.1, denoted 10q24.1. [3] This gene is member 6 of the TNF-receptor superfamily (TNFRSF6). ... The engagement of Fas by Fas receptor results in apoptosis of the cell and is important for eliminating T cells that are repeatedly stimulated by antigens. [4] As a result of the mutation in the Fas receptor gene, there is no recognition of Fas by Fas receptor , leading to a primitive population of T cells that proliferates in an uncontrolled manner. [2] Other inherited causes [ edit ] Boys with X-linked immunodeficiency syndrome are at a higher risk of mortality associated with Epstein–Barr virus infections, and are predisposed to develop a lymphoproliferative disorder or lymphoma. ... Some disorders that predispose a person to lymphoproliferative disorders are severe combined immunodeficiency (SCID), Chédiak–Higashi syndrome , Wiskott–Aldrich syndrome (an X-linked recessive disorder), and ataxia–telangiectasia . ... In most reported cases, these cause B cell lymphoproliferative disorders; however, some T cell variations have been described. [2] The T cell variations are usually caused by the prolonged use of T cell suppressant drugs, such as sirolimus , tacrolimus , or ciclosporin . [2] The Epstein-Barr virus , which infects >90% of the world population, is also a common cause of these disorders, being responsible for a wide range of non-malignant, pre-malignant, and malignant Epstein-Barr virus-associated lymphoproliferative diseases . [5] See also [ edit ] Evans syndrome Leukaemia Lymphoma Lymphocytosis Myeloma Myeloproliferative disease References [ edit ] ^ "Idiopathic Interstitial Pneumonias: Interstitial Lung Diseases: Merck Manual Professional" .SH2D1A, IFNG, XIAP, IL17A, CASP8, ZAP70, IL2RG, KRT20, IL6, CD70, TRBV20OR9-2, MCM4, CCND1, BCL2, TNFRSF8, KRAS, MS4A1, PDLIM7, PLAA, NRAS, TP53, TNF, MYD88, RAPH1, ACSBG1, ALK, FAS, IGH, ATM, BCL6, IL10, STAT3, CD274, IL2, CTLA4, ITK, JAK2, BCL3, ADA, MME, SOAT1, IRF4, SMUG1, SPN, NCAM1, MYOD1, HSP90AA1, ABL1, MIR155, BRAF, FASLG, CD200, CBL, MIR223, MYC, MTX1, MTHFR, EBI3, PDCD1LG2, SERPING1, CXCL13, EBP, KLRB1, PRAME, IBTK, LAT, CD44, NPM1, TCL1B, IGHV4-34, S100A1, UBE2B, STIM1, SDC1, TCL1A, SATB1, S100B, IL18R1, PDCD1, BCR, MIR17HG, PIK3CG, PIK3CD, PIK3CB, PIK3CA, CD81, TNFSF13B, IL4, HLA-DRB1, DNMT1, FCER2, GATA3, RTEL1, IL13, CDK6, TNFRSF13C, COIL, DCLRE1C, ERVK-6, SOCS1, TNFSF10, STIM2, CD84, ARHGEF7, SOCS3, WDR48, CBFA2T2, MSC, AICDA, DUSP22, ASAH2, PPP1R12C, SGSM3, PARP9, ABCG2, USP9Y, ARHGAP24, FOXP1, KMT2D, LOC102724971, TP73, TRAF1, TRAF3, TSC1, LOC102723407, TYK2, ASRGL1, VIPR1, XIST, WLS, ERVK-20, XRCC5, KIR2DS2, IGKV1-5, YY1, TARP, CXCR4, MARCKSL1, TNFAIP3, FOXP3, HDAC9, IGK, CCL27, SLC27A5, MIR146A, RASSF1, DLL1, CHEK2, TBC1D9, MIR142, PPP1R13B, MLYCD, IGHV1-2, SLC35B2, CIZ1, CLEC4D, KLHDC8B, FAAP24, ACAD8, IGHV3-41, IGHV3-52, MCU, FBXO11, PWWP3A, IGKV2-29, ERVW-1, CHRDL1, HDAC6, ICOS, MIR26B, CARD11, PDCD4, BCL2L11, ORAI1, MIR150, ABCB6, RASGRP1, IGKV3-15, IGKV3-20, IKZF1, MIR17, BATF, IGLV3-21, KNTC1, PLK1, TIA1, DIH1, ATN1, EPO, ERBB2, ETV6, FCGR3A, FCGR3B, FGR, FH, FOXO3, MTOR, GEM, CCR10, CXCR3, GZMH, HBZ, HLA-A, HLA-B, HLA-G, HTC2, ICAM1, IRF8, IGKV@, IL1R1, IL2RA, IL2RB, DLX2, DAPK1, IL7, NKX2-5, ADAM10, ADK, ABCD1, ANPEP, BAK1, PRDM1, CBLB, CD5, CD5L, CD14, CD19, CD22, CD27, CD28, CD38, CD40LG, CD69, CDK2, CDKN1B, CDKN2A, CDKN3, CD52, CEL, CCR3, CCR4, IL5, IL12A, TGFB1, PAX7, ABCB1, PIK3R1, PIK3R2, PKM, POU2AF1, EIF2AK2, PSMB6, PTPRC, RAG1, PLAAT4, CCL17, CCL21, CCL22, XCL1, SLAMF1, SLC11A1, FSCN1, SPP1, SYK, TAC1, CNTN2, TRA, TRG, TRGC1, TERT, PECAM1, ORC4, IL15, NOTCH4, IL18, ISG20, ITGA4, ITGAE, JAK3, KIR2DL1, KIR2DL2, KIR2DL3, KIR2DS1, KIR2DS3, KIR3DL1, KIT, KLRD1, LBR, LCK, LGALS1, LIG4, LMO2, MET, MOS, MRC1, ABCC1, MSH2, MUC1, NFKB1, LINC02605