-
Neutropenia, Severe Congenital, 4, Autosomal Recessive
Omim
A number sign (#) is used with this entry because severe congenital neutropenia-4 (SCN4) and Dursun syndrome are both caused by homozygous mutation in the G6PC3 gene (611045) on chromosome 17q21. ... Clinical Features Boztug et al. (2009) reported an extended consanguineous kindred from Aramean, Turkey, in which 4 children had a syndrome comprising severe congenital neutropenia, cardiac abnormalities, and a prominent superficial venous pattern. ... Mapping By linkage analysis of 2 consanguineous Turkish families with syndromic congenital neutropenia, Boztug et al. (2009) found linkage to a region on chromosome 17q21 (maximum 2-pedigree multipoint lod score of 5.74 at markers D17S932, D17S950, and D17S806). ... In 2 sibs with SCN4 and multiple clinical abnormalities, McDermott et al. (2010) identified a homozygous mutation in the G6PC3 gene (611045.0007). Dursun Syndrome In 1 of the Turkish children with Dursun syndrome (Dursun et al., 2009), Banka et al. (2010) identified a homozygous mutation in the G6PC3 gene (M116V; 611045.0006). ... The findings suggested that Dursun syndrome can be considered a subset of SCN4.
-
Beta-Propeller Protein-Associated Neurodegeneration
Gene_reviews
Seizure types including generalized (absence, tonic, atonic, tonic-clonic and myoclonic), focal with impaired consciousness, and epileptic spasms, as well as epileptic syndromes (West syndrome and Lennox-Gastaut syndrome) can be seen. ... Clinical Findings Seizures characterized by the following: Features Onset in early childhood Development of multiple seizure types Seizures worse in early childhood, lessening with age Types Generalized (absence, tonic, atonic, tonic-clonic and myoclonic) Focal seizures with impaired consciousness Epileptic spasms Syndromes West syndrome Lennox-Gastaut syndrome Early-onset epilepsy with intellectual disability Developmental delay / intellectual disability (with minimal or absent expressive language) that is relatively stable in childhood, followed by progressive loss of cognitive function beginning in adolescence or early adulthood Progressive parkinsonism and dystonia , beginning in adolescence or early adulthood Abnormal behaviors that overlap with Rett syndrome, including stereotypic hand movements, bruxism when awake, and abnormal sleep patterns MRI Findings Nonspecific hypomyelination and thin corpus callosum are seen in early childhood [Rathore et al 2014; Khalifa & Naffaa 2015; Hogarth, unpublished data] and evolve to highly specific signal abnormalities in later childhood, adolescence, or early adulthood: T 2 -weighted or iron-sensitive sequences reveal hypointense signal in the substantia nigra and globus pallidus (Figure 1). ... Some also have limited purposeful hand use (reminiscent of Rett syndrome) that can contribute to functional impairments such as difficulty with dressing and use of utensils. ... Abnormal behaviors that overlap with Rett syndrome include lack of purposeful hand movements, stereotypic hand movements such as repetitive midline hand-wringing, bruxism when awake, abnormal sleep patterns, features of autism spectrum disorder, and diminished response to pain [Haack et al 2012, Hayflick et al 2013, Ohba et al 2014, Khalifa & Naffaa 2015]. ... The differential diagnosis at this stage is therefore broad, and includes Rett syndrome, Angelman syndrome, alpha-fucosidosis, and the epileptic encephalopathies of infancy and childhood: Dravet syndrome (see SCN1A Seizure Disorders) West syndrome Lennox-Gastaut syndrome Epilepsy with electrical status during slow-wave sleep Gelastic epilepsy Kozhevnikov-Rasmussen syndrome Landau-Kleffner syndrome Early-infantile epileptic encephalopathy (See Epileptic encephalopathy, early infantile: OMIM Phenotypic Series to view genes associated with this phenotype in OMIM.)
-
Female Infertility
Wikipedia
Chromosomal abnormalities causing female infertility include Turner syndrome . Oocyte donation is an alternative for patients with Turner syndrome. [34] Some of these gene or chromosome abnormalities cause intersex conditions , such as androgen insensitivity syndrome . ... Many genetic defects (as also detailed previously) also disturb ovarian function. Polycystic ovary syndrome (also see infertility in polycystic ovary syndrome ) Anovulation . ... Uterine factors [ edit ] Uterine malformations [45] Uterine fibroids Asherman's syndrome [46] Implantation failure without any known primary cause. ... "Mayer-Rokitansky-Kuster-Hauser syndrome: recent clinical and genetic findings". ... "Hysteroscopic treatment of Asherman's syndrome". Reprod. Biomed. Online . 4 (Suppl 3): 46–51. doi : 10.1016/s1472-6483(12)60116-3 .
-
Nemaline Myopathy
Wikipedia
External links [ edit ] GeneReview/NCBI/NIH/UW entry on Nemaline Myo\ Classification D ICD - 10 : G71.2 ICD - 9-CM : 359.0 OMIM : 161800 256030 605355 609284 MeSH : D017696 DiseasesDB : 31991 External resources eMedicine : neuro/76 neuro/230 GeneReviews : Nemaline myopathy Orphanet : 607 v t e Muscular dystrophy Types Congenital Dystrophinopathy Becker's Duchenne Distal Emery-Dreifuss Facioscapulohumeral Limb-girdle muscular dystrophy Calpainopathy Myotonic Oculopharyngeal National/International Organizations Muscular Dystrophy Association (USA) Muscular Dystrophy Canada Myotonic Dystrophy Foundation Muskelsvindfonden (Denmark) National/International Events MDA Muscle Walk (USA) Labor Day Telethon (defunct; USA/Canada) Décrypthon (France) Grøn Koncert (Denmark) Clinical trials Stamulumab (MYO-029) Category v t e Diseases of muscle , neuromuscular junction , and neuromuscular disease Neuromuscular- junction disease autoimmune Myasthenia gravis Lambert–Eaton myasthenic syndrome Neuromyotonia Myopathy Muscular dystrophy ( DAPC ) AD Limb-girdle muscular dystrophy 1 Oculopharyngeal Facioscapulohumeral Myotonic Distal (most) AR Calpainopathy Limb-girdle muscular dystrophy 2 Congenital Fukuyama Ullrich Walker–Warburg XR dystrophin Becker's Duchenne Emery–Dreifuss Other structural collagen disease Bethlem myopathy PTP disease X-linked MTM adaptor protein disease BIN1-linked centronuclear myopathy cytoskeleton disease Nemaline myopathy Zaspopathy Channelopathy Myotonia Myotonia congenita Thomsen disease Neuromyotonia / Isaacs syndrome Paramyotonia congenita Periodic paralysis Hypokalemic Thyrotoxic Hyperkalemic Other Central core disease Mitochondrial myopathy MELAS MERRF KSS PEO General Inflammatory myopathy Congenital myopathy v t e Cytoskeletal defects Microfilaments Myofilament Actin Hypertrophic cardiomyopathy 11 Dilated cardiomyopathy 1AA DFNA20 Nemaline myopathy 3 Myosin Elejalde syndrome Hypertrophic cardiomyopathy 1, 8, 10 Usher syndrome 1B Freeman–Sheldon syndrome DFN A3, 4, 11, 17, 22; B2, 30, 37, 48 May–Hegglin anomaly Troponin Hypertrophic cardiomyopathy 7, 2 Nemaline myopathy 4, 5 Tropomyosin Hypertrophic cardiomyopathy 3 Nemaline myopathy 1 Titin Hypertrophic cardiomyopathy 9 Other Fibrillin Marfan syndrome Weill–Marchesani syndrome Filamin FG syndrome 2 Boomerang dysplasia Larsen syndrome Terminal osseous dysplasia with pigmentary defects IF 1/2 Keratinopathy ( keratosis , keratoderma , hyperkeratosis ): KRT1 Striate palmoplantar keratoderma 3 Epidermolytic hyperkeratosis IHCM KRT2E ( Ichthyosis bullosa of Siemens ) KRT3 ( Meesmann juvenile epithelial corneal dystrophy ) KRT4 ( White sponge nevus ) KRT5 ( Epidermolysis bullosa simplex ) KRT8 ( Familial cirrhosis ) KRT10 ( Epidermolytic hyperkeratosis ) KRT12 ( Meesmann juvenile epithelial corneal dystrophy ) KRT13 ( White sponge nevus ) KRT14 ( Epidermolysis bullosa simplex ) KRT17 ( Steatocystoma multiplex ) KRT18 ( Familial cirrhosis ) KRT81 / KRT83 / KRT86 ( Monilethrix ) Naegeli–Franceschetti–Jadassohn syndrome Reticular pigmented anomaly of the flexures 3 Desmin : Desmin-related myofibrillar myopathy Dilated cardiomyopathy 1I GFAP : Alexander disease Peripherin : Amyotrophic lateral sclerosis 4 Neurofilament : Parkinson's disease Charcot–Marie–Tooth disease 1F, 2E Amyotrophic lateral sclerosis 5 Laminopathy : LMNA Mandibuloacral dysplasia Dunnigan Familial partial lipodystrophy Emery–Dreifuss muscular dystrophy 2 Limb-girdle muscular dystrophy 1B Charcot–Marie–Tooth disease 2B1 LMNB Barraquer–Simons syndrome LEMD3 Buschke–Ollendorff syndrome Osteopoikilosis LBR Pelger–Huet anomaly Hydrops-ectopic calcification-moth-eaten skeletal dysplasia Microtubules Kinesin Charcot–Marie–Tooth disease 2A Hereditary spastic paraplegia 10 Dynein Primary ciliary dyskinesia Short rib-polydactyly syndrome 3 Asphyxiating thoracic dysplasia 3 Other Tauopathy Cavernous venous malformation Membrane Spectrin : Spinocerebellar ataxia 5 Hereditary spherocytosis 2, 3 Hereditary elliptocytosis 2, 3 Ankyrin : Long QT syndrome 4 Hereditary spherocytosis 1 Catenin APC Gardner's syndrome Familial adenomatous polyposis plakoglobin ( Naxos syndrome ) GAN ( Giant axonal neuropathy ) Other desmoplakin : Striate palmoplantar keratoderma 2 Carvajal syndrome Arrhythmogenic right ventricular dysplasia 8 plectin : Epidermolysis bullosa simplex with muscular dystrophy Epidermolysis bullosa simplex of Ogna plakophilin : Skin fragility syndrome Arrhythmogenic right ventricular dysplasia 9 centrosome : PCNT ( Microcephalic osteodysplastic primordial dwarfism type II ) Related topics: Cytoskeletal proteinsTNNT1, NEB, TPM3, TPM2, ACTA1, KLHL41, KLHL9, NEFL, SRPK3, POMGNT1, FKTN, CHKB, B4GAT1, ITGA7, LMNA, POMT1, FKRP, LARGE1, CFL2, RIF1, ACTB, TPM1, KLHL40, LMOD3, RYR1, KBTBD13, MSTN, ACTC1, HTC2, CUL3, DES, C16orf82, ACTA2, MYO18B, MYPN, MCOLN1, ACTN1, UCP3, EMD, EIF3K, HK1, GJB6, MYH7, NRAP, MYOT, TNNT3, ACHE
-
Fetal Alcohol Spectrum Disorder
Wikipedia
Fetal alcohol spectrum disorders Other names Foetal alcohol spectrum disorders Baby with fetal alcohol syndrome, showing some of the characteristic facial features Specialty Psychiatry , pediatrics , toxicology Symptoms Abnormal appearance, short height, low body weight, small head size , poor coordination, behavior problems, learning problems [1] [2] Complications Babies : Miscarriage , stillbirth Adults : Alcoholism , substance use disorder , substance abuse Duration Long term [1] [3] Types Fetal alcohol syndrome, Partial fetal alcohol syndrome, Alcohol-related neurodevelopmental disorder, Static Encephalopathy, Alcohol-related birth defects [1] Causes Drinking alcohol during pregnancy [1] Diagnostic method Based on symptoms [1] Prevention Avoiding drinking alcohol during pregnancy [4] Treatment Parent-child interaction therapy , efforts to modify child behavior, possibly medications [5] Prognosis Moderate. ... This complicates diagnosis and treatment of the syndrome. [27] As a result, diagnosis of the severity of FASD relies on protocols of observation of the child's physiology and behavior rather than maternal self-reporting. ... While the four diagnostic systems essentially agree on criteria for fetal alcohol syndrome (FAS), there are still differences when full criteria for FAS are not met. ... While other FASD conditions may not yet be included as an ICD or DSM-IV-TR diagnosis, they nonetheless pose significant impairment in functional behavior because of underlying brain damage. Fetal alcohol syndrome [ edit ] The following criteria must be fully met for an FAS diagnosis: [2] [19] [24] [27] Growth deficiency: Prenatal or postnatal height or weight (or both) at or below the 10th percentile [25] FAS facial features: All three FAS facial features present [33] Central nervous system damage: Clinically significant structural neurological, or functional impairment Prenatal alcohol exposure: Confirmed or Unknown prenatal alcohol exposure Fetal alcohol syndrome (FAS) is the first diagnosable condition of FASD that was discovered. ... However, the Ten Brain Domains are easily incorporated into any of the four diagnostic systems' CNS damage criteria, as the framework only proposes the domains, rather than the cut-off criteria for FASD. [63] Differential diagnosis [ edit ] The CDC reviewed nine syndromes that have overlapping features with FAS; however, none of these syndromes include all three FAS facial features, and none are the result of prenatal alcohol exposure: [27] Aarskog syndrome Williams syndrome Noonan syndrome Dubowitz syndrome Brachman-DeLange syndrome Toluene syndrome Fetal hydantoin syndrome Fetal valproate syndrome Maternal PKU fetal effects Other disorders that have similar symptoms may include: [64] Attention deficit hyperactive disorder Autism spectrum disorder Reactive attachment disorder Oppositional defiant disorder Sensory integration dysfunction Bipolar disorder Depression Asperger's syndrome Prevention [ edit ] See also: Alcohol and pregnancy The only certain way to prevent FAS is to avoid drinking alcohol during pregnancy. [55] [65] In the United States, the Surgeon General recommended in 1981, and again in 2005, that women abstain from alcohol use while pregnant or while planning a pregnancy, the latter to avoid damage even in the earliest stages (even weeks) of a pregnancy, as the woman may not be aware that she has conceived . [18] The Centers for Disease Control and the American College of Obstetricians and Gynecologists also recommend no alcohol during pregnancy. [62] In the United States, federal legislation has required that warning labels be placed on all alcoholic beverage containers since 1988 under the Alcoholic Beverage Labeling Act .
-
Isolated Cytochrome C Oxidase Deficiency
Orphanet
A rare mitochondrial oxidative phosphorylation disorder characterized by a highly variable clinical phenotype, including a benign infantile mitochondrial type affecting mainly the skeletal muscle, a lethal infantile mitochondrial myopathy linked to severe metabolic acidosis and mitochondrial dysfunction in skeletal muscle and often also in heart, Leigh syndrome, which causes severe, early-onset, progressive, and fatal encephalopathy, and French-Canadian type Leigh syndrome, which affects mostly the skeletal muscle, but also brain and liver.COX10, SCO1, COX8A, COA8, COX20, COX14, COX6B1, COX2, COX1, PET100, FASTKD2, SCO2, TACO1, SURF1, COA3, TRNN, COX3, COX5A, MTCO2P12, COX15, COA5, PET117, TRNS1, NDUFA4, TRNL1, KLC1, HNRNPU, CPOX, COA6, LRPPRC, GFM2, MRRF, COX6A2, GAA, COA7, PINK1, MRPL44, COX7A1, COX4I1, COX4I2, CEP89, COX16, COX6A1, OTOA, COX18, COX19, ETHE1, PLCE1, SIRT1, OPA1, PTGS1, PTGS2, HADHA, SOD1, STXBP1, GBE1, UCN, CHKB, CCS, COX17, FARS2, EHHADH, SIRT4, SIRT3, SLC25A20
-
Muscular Dystrophy, Congenital, With Cerebellar Atrophy
Omim
In addition, they referred to 4 earlier reports of sporadic cases with isolated cerebellar atrophy with features of the Dandy-Walker syndrome in the presence of congenital myopathy. ... The authors believed the disorder could be differentiated from the dystroglycanopathies Fukuyama congenital muscular dystrophy (253800), Walker-Warburg syndrome, and muscle-eye-brain disease (see, e.g., 236670).
-
Aichmophobia
Wikipedia
Not to be confused with similar condition ( Avoidance behavior ) the Visual looming syndrome , where the patient does not fear sharp items, but feels pain or discomfort at gazing upon sharp objects nearby. See also [ edit ] Psychosocial treatment of needle phobia in children Visual looming syndrome References [ edit ] ^ "Aichmophobia" .
-
Sternum, Premature Obliteration Of Sutures Of
Omim
This sternal deformity is characteristic of Noonan syndrome (163950). It was also seen in brothers with multiple osteochondritis dissecans (165800), originally reported by Hanley et al. (1967) and considered by later writers, probably correctly, to have had Aarskog syndrome (305400).
-
Renal Oncocytoma
Gard
The exact underlying cause of most isolated (single tumor affecting one kidney) renal oncocytomas is unknown; however, multiple and bilateral (affecting both kidneys) renal oncocytomas sometimes occur in people with certain genetic syndromes such as tuberous sclerosis complex and Birt-Hogg-Dube syndrome .
-
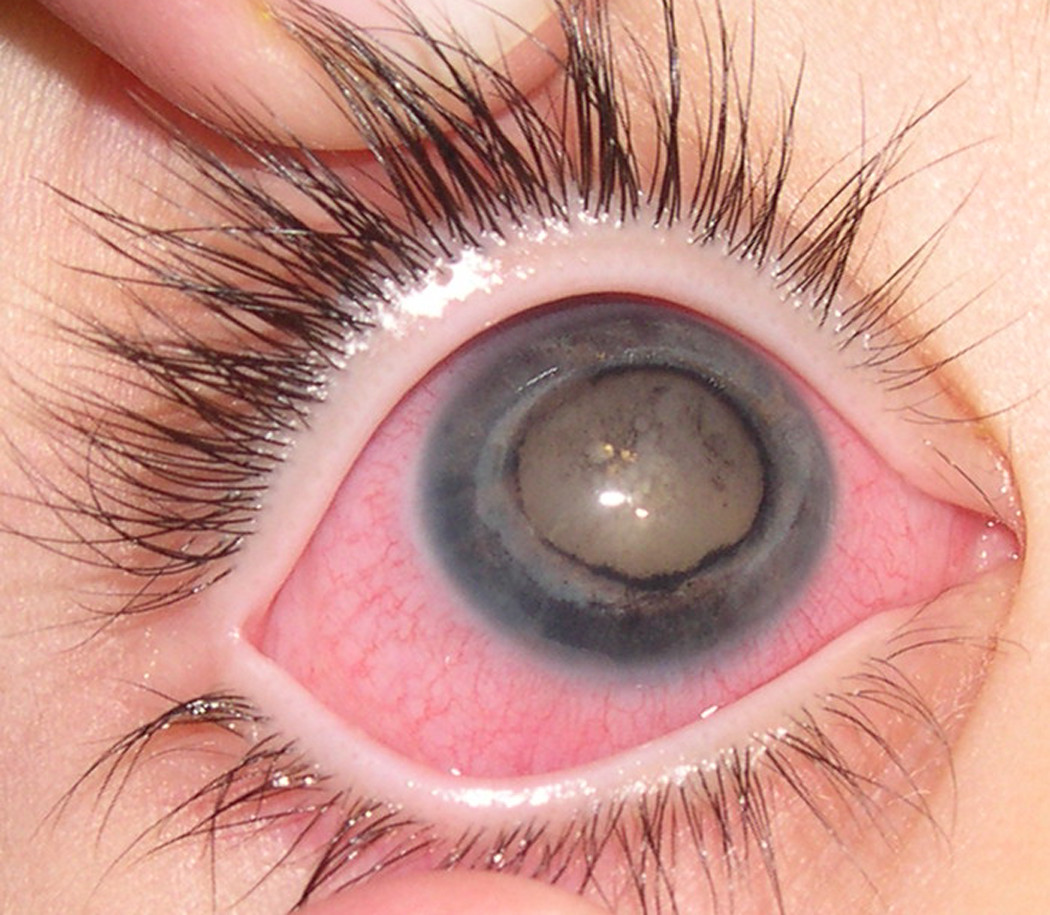
Red Eye (Medicine)
Wikipedia
Although harmless, it can occasionally become inflamed. dry eye syndrome – caused by either decreased tear production or increased tear film evaporation which may lead to irritation and redness [8] acute glaucoma, angle closure type airborne contaminants or irritants tiredness drug use including cannabis [9] episcleritis [10] – most often a mild, inflammatory disorder of the 'white' of the eye unassociated with eye complications in contrast to scleritis, and responding to topical medications such as anti-inflammatory drops. ... Classification D ICD - 10 : H57.9 ICD - 9-CM : 379.93 DiseasesDB : 18665 v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
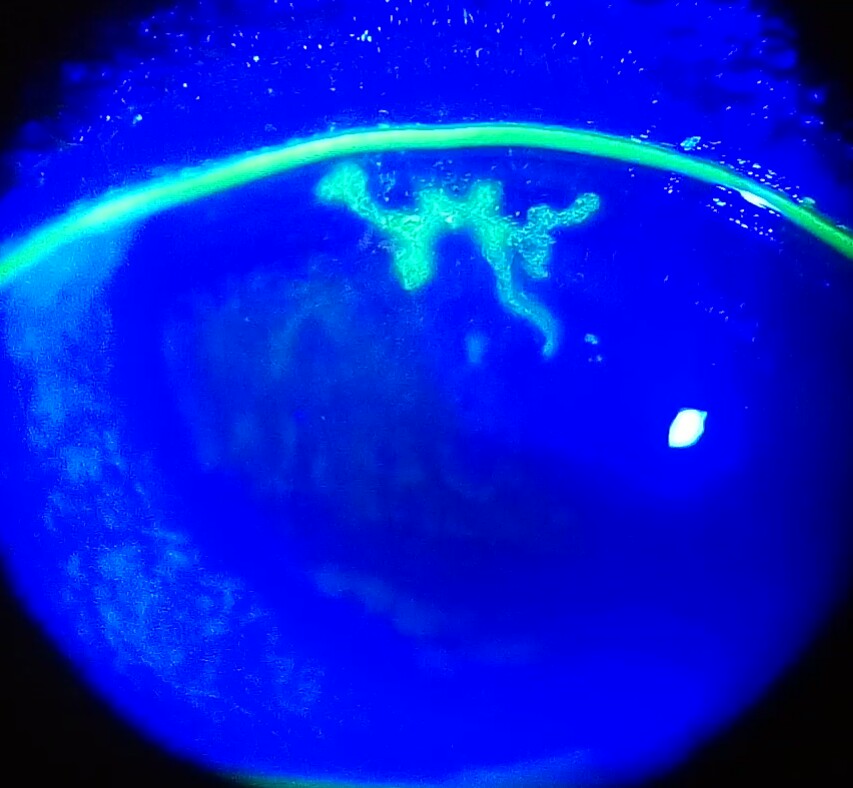
Herpes Simplex Keratitis
Wikipedia
Ganciclovir and brivudine treatments were found to be equally as effective as acyclovir in a systematic review. [8] Valacyclovir , a pro-drug of acyclovir likely to be just as effective for ocular disease, can cause thrombotic thrombocytopenic purpura / Hemolytic-uremic syndrome in severely immunocompromised patients such as those with AIDS ; thus, it must be used with caution if the immune status is unknown. ... External links [ edit ] Classification D ICD - 10 : B00.52 ICD - 9-CM : 54.43 MeSH : D016849 v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
Florid Cutaneous Papillomatosis
Wikipedia
Please help improve it to make it understandable to non-experts , without removing the technical details. ( April 2018 ) ( Learn how and when to remove this template message ) Florid cutaneous papillomatosis Other names Schwartz–Burgess syndrome Specialty Dermatology Florid cutaneous papillomatosis (FCP), is an obligate paraneoplastic syndrome . ... It has since been called Schwartz–Burgess syndrome. [15] [16] Society and culture [ edit ] Patients may have their unaesthetic appearance resulting in isolation from their community , feeling or being unwelcome in public places. [17] References [ edit ] ^ a b c Mansouri, P.; et al. (1999). ... External links [ edit ] Florid cutaneous papillomatosis at eMedicine Classification D DiseasesDB : 34696 External resources eMedicine : derm/917 v t e Dermatitis and eczema Atopic dermatitis Besnier's prurigo Seborrheic dermatitis Pityriasis simplex capillitii Cradle cap Contact dermatitis ( allergic , irritant ) plants: Urushiol-induced contact dermatitis African blackwood dermatitis Tulip fingers other: Abietic acid dermatitis Diaper rash Airbag dermatitis Baboon syndrome Contact stomatitis Protein contact dermatitis Eczema Autoimmune estrogen dermatitis Autoimmune progesterone dermatitis Breast eczema Ear eczema Eyelid dermatitis Topical steroid addiction Hand eczema Chronic vesiculobullous hand eczema Hyperkeratotic hand dermatitis Autosensitization dermatitis / Id reaction Candidid Dermatophytid Molluscum dermatitis Circumostomy eczema Dyshidrosis Juvenile plantar dermatosis Nummular eczema Nutritional deficiency eczema Sulzberger–Garbe syndrome Xerotic eczema Pruritus / Itch / Prurigo Lichen simplex chronicus / Prurigo nodularis by location: Pruritus ani Pruritus scroti Pruritus vulvae Scalp pruritus Drug-induced pruritus Hydroxyethyl starch-induced pruritus Senile pruritus Aquagenic pruritus Aquadynia Adult blaschkitis due to liver disease Biliary pruritus Cholestatic pruritus Prion pruritus Prurigo pigmentosa Prurigo simplex Puncta pruritica Uremic pruritus Other substances taken internally: Bromoderma Fixed drug reaction Nummular dermatitis Pityriasis alba Papuloerythroderma of Ofuji v t e Symptoms and signs relating to skin and subcutaneous tissue Disturbances of skin sensation Hypoesthesia Paresthesia Formication Hyperesthesia Hypoalgesia Hyperalgesia Circulation Cyanosis Pallor Livedo Livedo reticularis Flushing Petechia Blanching Edema Peripheral edema Anasarca Other Rash Desquamation Induration Diaphoresis Mass Neck mass Skin Asboe-Hansen sign Auspitz's sign Borsari's sign Braverman's sign Crowe sign Dennie–Morgan fold Darier's sign Fitzpatrick's sign Florid cutaneous papillomatosis Gottron's sign Hutchinson's sign Janeway lesion Kerr's sign Koebner's phenomenon Koplik's spots Leser-Trelat sign Nikolsky's sign Pastia's sign Russell's sign Wickham striae Wolf's isotopic response Munro's microabscess Nails Aldrich-Mees' lines Beau's lines Muehrcke's lines Terry's nails v t e Paraneoplastic syndromes Endocrine Hypercalcaemia SIADH Zollinger–Ellison syndrome Cushing's syndrome Hematological Multicentric reticulohistiocytosis Nonbacterial thrombotic endocarditis Neurological Paraneoplastic cerebellar degeneration Encephalomyelitis Limbic encephalitis Opsoclonus Polymyositis Transverse myelitis Lambert–Eaton myasthenic syndrome Anti-NMDA receptor encephalitis Musculoskeletal Dermatomyositis Hypertrophic osteopathy Mucocutaneous reactive erythema Erythema gyratum repens Necrolytic migratory erythema papulosquamous Acanthosis nigricans Ichthyosis acquisita Acrokeratosis paraneoplastica of Bazex Extramammary Paget's disease Florid cutaneous papillomatosis Leser-Trélat sign Pityriasis rotunda Tripe palms Other Febrile neutrophilic dermatosis Pyoderma gangrenosum Paraneoplastic pemphigus
-
Coats' Disease
Wikipedia
. ^ Statland JM1, Sacconi S, Farmakidis C, Donlin-Smith CM, Chung M, Tawil R. Coats syndrome in facioscapulohumeral dystrophy type 1: frequency and D4Z4 contraction size. ... External links [ edit ] Classification D ICD - 10 : H35.0 ICD - 9-CM : 362.12 OMIM : 300216 MeSH : D058456 DiseasesDB : 31162 External resources Orphanet : 190 GeneReviews/NIH/NCBI/UW entry on NDP-Related Retinopathies http://www.orpha.net/data/patho/GB/uk-Coats.pdf v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
Second-Degree Atrioventricular Block
Wikipedia
External links [ edit ] Classification D ICD - 10 : I44.1 ICD - 9-CM : 426.12 , 426.13 DiseasesDB : 10477 External resources eMedicine : emerg/234 v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever
-
Steroid Dementia Syndrome
Wikipedia
Steroid dementia syndrome Specialty Neurology/psychiatry Steroid dementia syndrome describes the signs and symptoms of hippocampal and prefrontal cortical dysfunction, such as deficits in memory, attention, and executive function, induced by glucocorticoids . [1] Dementia-like symptoms have been found in some individuals who have been exposed to glucocorticoid medication, often dispensed in the form of asthma, arthritis, and anti-inflammatory steroid medications. The condition reverses, but not always completely, within months after steroid treatment is stopped. [2] The term "steroid dementia" was coined by Varney et al. (1984) in reference to the effects of long-term glucocorticoid use in 1,500 patients. [3] While the condition generally falls under the classification of Cushing's syndrome , the term "steroid dementia syndrome" is particularly useful because it recognizes both the cause of the syndrome and the specific effects of glucocorticoids on cognitive function. Further, the more precise terminology clearly distinguishes the condition from full-blown Cushing's syndrome, which is extremely broad regarding the causes (endogenous or exogenous, pituitary or adrenal) and the multitude of symptoms (ranging from skin disorders to osteoporosis), and from hypercortisolemia, which identifies neither the source nor the symptoms of excess circulatory cortisol. ... Testing after 14 months showed a large jump in Full Scale IQ from 87 to 124, but mild dysfunction in executive function, memory, attentional control, and verbal/nonverbal memory remained. [13] References [ edit ] ^ a b c Wolkowitz, Owen M.; Lupien, Sonia J.; Bigler, Erin D. (2007). "The 'Steroid Dementia Syndrome': A Possible Model of Human Glucocorticoid Neurotoxicity". ... PMID 3527687 . ^ Wolkowitz, Owen M.; Lupien, Sonia J.; Bigler, Erin; Levin, R Bronson; Canick, Jonathan (1 December 2004). "The "Steroid Dementia Syndrome": An Unrecognized Complication of Glucocorticoid Treatment".
-
Pulp Stone
Wikipedia
It is presumed that epithelial remnants are able to induce adjacent mesenchymal stem cells to differentiate into odontoblasts. [7] Associations [ edit ] A pilot study was done with patients with cardiovascular disease (CVD) and it shows increased incidence of pulp stones in teeth with patients with CVD compared to healthy patients without CVD. [8] There are also researchers which suggest the link between pulpal calcification and carotid artery calcification, despite not having a strong proof on this correlation. [5] Besides cardiovascular disease, other disease such as end stage renal disease , Marfan syndrome , Ehlers-Danlos syndrome , Calcinosis universalis , tumoral calcinosis are also discovered to be in association with pulpal calcifications. [9] Several genetic diseases such as dentin dysplasia and dentinogenesis imperfecta are also accompanied by pulpal calcifications and hence, Marfan syndrome was suspected to be in association with pulp stones due to abnormal dentin formation, leading to the increased frequency of pulpal calcifications in these individuals. [9] Another theory suggests that individuals with Marfan syndrome have connective tissue dysplasia or vascular defects which in the case of tooth pulp, endothelial rupture of the pulp arterioles will lead to hemorrhagic areas in the pulp. ... "Prevalence of pulp calcifications in patients with Marfan syndrome". Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics . 106 (6): e56–61. doi : 10.1016/j.tripleo.2008.06.029 . ... S2CID 4873355 . v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Hypertensive Kidney Disease
Wikipedia
External links [ edit ] Classification D ICD - 10 : I12 ICD - 9-CM : 403 MeSH : D009400 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension v t e Kidney disease Glomerular disease See Template:Glomerular disease Tubules Renal tubular acidosis proximal distal Acute tubular necrosis Genetic Fanconi syndrome Bartter syndrome Gitelman syndrome Liddle's syndrome Interstitium Interstitial nephritis Pyelonephritis Balkan endemic nephropathy Vascular Renal artery stenosis Renal ischemia Hypertensive nephropathy Renovascular hypertension Renal cortical necrosis General syndromes Nephritis Nephrosis Renal failure Acute renal failure Chronic kidney disease Uremia Other Analgesic nephropathy Renal osteodystrophy Nephroptosis Abderhalden–Kaufmann–Lignac syndrome Diabetes insipidus Nephrogenic Renal papilla Renal papillary necrosis Major calyx / pelvis Hydronephrosis Pyonephrosis Reflux nephropathy
-
Phantom Limb
Wikipedia
"Phantom limb syndrome: A review" (PDF) . MEJ Anesth . 19 (2): 345–55. ... "Consciousness and body image: lessons from phantom limbs, Capgras syndrome and pain asymbolia" . Philosophical Transactions of the Royal Society of London. ... -W.; Evers, S.; Gerding, H. (2003). "Phantom eye syndrome: Its prevalence, phenomenology, and putative mechanisms" . ... M.; Gennari-Filho, H.; dos Santos, D. M. (2014). "Phantom eye syndrome: A review of the literature" . ... External links [ edit ] Classification D ICD - 10 : G54.6 - G54.7 ICD - 9-CM : 353.6 MeSH : D010591 DiseasesDB : 29431 Phantom limb syndrome: A review M.E.J. ANESTH 19 (2), 2007
-
Deafness, X-Linked 3
Omim
History and physical examinations revealed no stigmata of syndromic hearing loss. Funduscopic examination was normal. ... One family with congenital sensorineural deafness with X-linked inheritance (304500), studied by Reardon et al. (1991), did not show linkage to Xq13-q21.1 and did not show the temporal bone changes of the gusher-deafness syndrome. Thus, this may represent the same entity as that in the family reported by Lalwani et al. (1994). ... Mutations in 'unconventional' myosin-7 (MYO7A; 276903) have been demonstrated in Usher syndrome (hearing loss and retinitis pigmentosa), as well as in nonsyndromic deafness.