-
Tetany
Wikipedia
. ^ Grobin, W (May 14, 1960). "A New Syndrome, Magnesium-Deficiency Tetany" . ... Wikimedia Commons has media related to Tetany (medical sign) . v t e Symptoms and signs relating to movement and gait Gait Gait abnormality CNS Scissor gait Cerebellar ataxia Festinating gait Marche à petit pas Propulsive gait Stomping gait Spastic gait Magnetic gait Truncal ataxia Muscular Myopathic gait Trendelenburg gait Pigeon gait Steppage gait Antalgic gait Coordination Ataxia Cerebellar ataxia Dysmetria Dysdiadochokinesia Pronator drift Dyssynergia Sensory ataxia Asterixis Abnormal movement Athetosis Tremor Fasciculation Fibrillation Posturing Abnormal posturing Opisthotonus Spasm Trismus Cramp Tetany Myokymia Joint locking Paralysis Flaccid paralysis Spastic paraplegia Spastic diplegia Spastic paraplegia Syndromes Monoplegia Diplegia / Paraplegia Hemiplegia Triplegia Tetraplegia / Quadruplegia General causes Upper motor neuron lesion Lower motor neuron lesion Weakness Hemiparesis Other Rachitic rosary Hyperreflexia Clasp-knife response
-
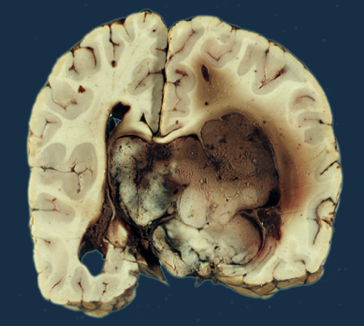
Choroid Plexus Papilloma
Wikipedia
External links [ edit ] Classification D ICD - 10 : C71.5 ICD - 9-CM : 191.5 ICD-O : M9390/1 MeSH : D020288 External resources eMedicine : article/250795 radio/171 Media related to Choroid plexus papilloma at Wikimedia Commons Choroid Plexus Papilloma MRI, CT, and pathology images from MedPix v t e Tumours of the nervous system Endocrine Sellar : Craniopharyngioma Pituicytoma Other: Pinealoma CNS Neuroepithelial ( brain tumors , spinal tumors ) Glioma Astrocyte Astrocytoma Pilocytic astrocytoma Pleomorphic xanthoastrocytoma Subependymal giant cell astrocytoma Fibrillary astrocytoma Anaplastic astrocytoma Glioblastoma multiforme Oligodendrocyte Oligodendroglioma Anaplastic oligodendroglioma Ependyma Ependymoma Subependymoma Choroid plexus Choroid plexus tumor Choroid plexus papilloma Choroid plexus carcinoma Multiple/unknown Oligoastrocytoma Gliomatosis cerebri Gliosarcoma Mature neuron Ganglioneuroma : Ganglioglioma Retinoblastoma Neurocytoma Dysembryoplastic neuroepithelial tumour Lhermitte–Duclos disease PNET Neuroblastoma Esthesioneuroblastoma Ganglioneuroblastoma Medulloblastoma Atypical teratoid rhabdoid tumor Primitive Medulloepithelioma Meninges Meningioma Hemangiopericytoma Hematopoietic Primary central nervous system lymphoma PNS : Nerve sheath tumor Cranial and paraspinal nerves Neurofibroma Neurofibromatosis Neurilemmoma / Schwannoma Acoustic neuroma Malignant peripheral nerve sheath tumor Other WHO classification of the tumors of the central nervous system Note: Not all brain tumors are of nervous tissue, and not all nervous tissue tumors are in the brain (see brain metastasis ). v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosisTP53, MKRN3, KISS1R, KISS1, AMH, DLK1, LEP, ESR1, CPP, SDS, NUCB2, MYC, LIN28B, FOXJ1, KCNK9, VIP, CRP, TNFSF10, CDKN2A, PCGF3, CAT, RASSF1, MCF2L2, ZNF629, NIN, ZNF44, TTR, SHC3, RETN, NPVF, ZNF436, CASP8, ZNF501, PROKR2, ZNF569, ZNF763, BGLAP, TWIST1, CTNNB1, FSHB, LTF, IGF1, IGF1R, IGF2, IGF2R, IGFBP3, IL6, ERBB3, S1PR3, LEPR, LHCGR, DLX5, STC1, CYP19A1, OPRM1, P2RX3, POMC, POU1F1, APC, SHBG, SMARCB1, SOD1, SOX2, RPS27A
-
Hypothalamic Disease
Wikipedia
GHRH stimulates the pituitary gland to secrete growth hormone (GH), which has various effects on body growth and sexual development. [1] [5] Insufficient GH production may cause poor somatic growth, precocious puberty or gonadotropin deficiency, failure to initiate or complete puberty, and is often associated with rapid weight gain, low T 4 , and low levels of sex hormones. [5] Sleep disorders [ edit ] Non-24-hour sleep-wake syndrome , a disabling condition in which one's sleep/wake cycle is longer, or rarely, shorter, than the standard 24 hours, is thought to involve or be caused by, at least in some cases, an abnormal functioning of the suprachiasmatic nucleus (SCN) in the hypothalamus. [10] [11] References [ edit ] ^ a b c d e f Sylvia L., A. (2004). ... External links [ edit ] Classification D ICD - 10 : E23.3 MeSH : D007027 v t e Hypothalamic disease Gonadotropin Kallmann syndrome Adiposogenital dystrophy CRH Tertiary adrenal insufficiency Vasopressin Neurogenic diabetes insipidus General Hypothalamic hamartoma
-
Eustachian Tube Dysfunction
Wikipedia
Disorder of the ear Eustachian tube dysfunction Specialty ENT surgery Symptoms Aural fullness, ears popping, pressure, a feeling the ears are clogged, crackling, ear pain , tinnitus , autophony , muffled hearing [1] Complications Otitis media , cholesteatoma [1] Types Dilatory, baro-challenged induced, patulous [1] Causes Common cold , influenza , allergic rhinitis , sinusitis [1] Differential diagnosis Endolymphatic hydrops , temporomandibular joint dysfunction , superior canal dehiscence syndrome , labyrinthine fistula [1] Eustachian tube dysfunction ( ETD ) is defined as pressure abnormalities in the middle ear which result in symptoms. [2] Contents 1 Signs and symptoms 2 Diagnosis 3 Types 4 Causes 5 Treatment 6 References Signs and symptoms [ edit ] Symptoms include aural fullness, ears popping, a feeling of pressure in the affected ear(s), a feeling that the affected ear(s) is clogged, crackling, ear pain , tinnitus , autophony , and muffled hearing. [1] Diagnosis [ edit ] While Eustachian tube dysfunction can be hard to diagnose, due to the Eustachian tubes and the nasopharynx not being easily visible, usually a tympanometry is indicated, along with findings on an otoscopy . ... ISSN 1531-7129 . v t e Diseases of the outer and middle ear Outer ear Otitis externa Otomycosis Middle ear and mastoid Otitis media Mastoiditis Bezold's abscess Gradenigo's syndrome Tympanosclerosis Cholesteatoma Perforated eardrum Symptoms Ear pain Hearing loss Tests Otoscope pneumatic tympanometry
-
Disorders Of Calcium Metabolism
Wikipedia
See also [ edit ] calcium metabolism Pseudohypoparathyroidism Milk-alkali syndrome References [ edit ] ^ a b c d e f g Murphy, E; Williams (2009). ... Classification D MeSH : D002128 Classification D ICD - 10 : E83.5 ICD - 9-CM : 275.4 MeSH : D002128 v t e Metal deficiency and toxicity disorders Iron excess: Iron overload Hemochromatosis Hemochromatosis/HFE1 Juvenile/HFE2 HFE3 African iron overload/HFE4 Aceruloplasminemia Atransferrinemia Hemosiderosis deficiency: Iron deficiency Copper excess: Copper toxicity Wilson's disease deficiency: Copper deficiency Menkes disease / Occipital horn syndrome Zinc excess: Zinc toxicity deficiency: Acrodermatitis enteropathica Other Inborn errors of metabolism
-
Degenerative Lumbosacral Stenosis
Wikipedia
Degenerative lumbosacral stenosis Other names Cauda equina syndrome Degenerative lumbosacral stenosis ( DLSS ), also known as cauda equina syndrome , is a pathologic degeneration in the lumbosacral disk in dogs; affecting the articulation, nerve progression, tissue and joint connections of the disk. [1] [2] This degeneration causes compressions in soft tissues and nerve root locations in the ultimate caudal area of the medulla , causing neuropathic pain in the lumbar vertebrae . [3] [4] Contents 1 Signs and symptoms 2 Research 3 Diagnosis 4 Treatment 5 References Signs and symptoms [ edit ] DLSS has been found to affect dogs between the ages of 7 and 8, males ranging twice as higher than females in the research area.
-
Spaceflight Osteopenia
Wikipedia
Whether they can provide the same benefits for spaceflight as they do for osteoporosis is not yet known. [4] See also [ edit ] Artificial gravity Effect of spaceflight on the human body Space medicine Space adaptation syndrome Microgravity University Reduced-gravity aircraft Timeline of longest spaceflights References [ edit ] ^ Kelly, Scott (2017). ... Retrieved 2013-02-23 . ^ Ubick, Suzanne; Mud, Mud, Glorious Mud, The Magazine of the California Academy of Sciences, Apr. 3, 2008 v t e Space medicine Main areas Artificial gravity Astronautical hygiene Bioastronautics Neuroscience in space Space exposure Space food Space nursing Space weather Weightlessness Illness and injuries Asthenization Ebullism Illness and injuries during spaceflight Medical treatment during spaceflight Space adaptation syndrome Space and survival Spaceflight osteopenia Organizations Aerospace Medical Association National Space Biomedical Research Institute Rubicon Foundation Space Nursing Society Other topics Adverse health effects from lunar dust exposure Cardiac rhythm problems during space flight Central nervous system effects from radiation exposure during spaceflight Effect of spaceflight on the human body Effects of sleep deprivation in space Epidemiology data for low-linear energy transfer radiation Sleep in space Health threat from cosmic rays Intervertebral disc damage and spaceflight List of microorganisms tested in outer space Psychological and sociological effects of spaceflight Radiobiology evidence for protons and HZE nuclei Reduced muscle mass, strength and performance in space Renal stone formation in space Spaceflight radiation carcinogenesis Team composition and cohesion in spaceflight missions Visual impairment due to intracranial pressure
-
Orchitis
Wikipedia
External links [ edit ] Classification D ICD - 10 : N45 ICD - 9-CM : 604 MeSH : D009920 DiseasesDB : 4342 External resources MedlinePlus : 001280 eMedicine : emerg/344 v t e Male diseases of the pelvis and genitals Internal Testicular Orchitis Hydrocele testis Testicular cancer Testicular torsion Male infertility Aspermia Asthenozoospermia Azoospermia Hyperspermia Hypospermia Oligospermia Necrospermia Teratospermia Epididymis Epididymitis Spermatocele Hematocele Prostate Prostatitis Acute prostatitis Chronic bacterial prostatitis Chronic prostatitis/chronic pelvic pain syndrome Asymptomatic inflammatory prostatitis Benign prostatic hyperplasia Prostate cancer Seminal vesicle Seminal vesiculitis External Penis Balanoposthitis / Balanitis Balanitis plasmacellularis Pseudoepitheliomatous keratotic and micaceous balanitis Phimosis Paraphimosis Priapism Sexual dysfunction Erectile dysfunction Peyronie's disease Penile cancer Penile fracture Balanitis xerotica obliterans Other Hematospermia Retrograde ejaculation Postorgasmic illness syndrome
-
Tadpole Pupil
Wikipedia
Other symptoms may include blurred vision, [1] abnormal periocular sensations [1] (unusual feelings around the eyes [4] ), migraines , [5] and feelings of a chilled face. [3] Some patients who demonstrate tadpole pupil symptoms also experienced Horner’s syndrome or Adie’s tonic pupil [5] Tadpole pupil symptoms occur in episodes. ... These tests include pharmacological testing (testing for an effective drug against a specific disease or condition), a complete ocular examination (a test that examines the entire eye), and video pupillography (recording and analysis of spontaneous pupil behavior in darkness). [6] A test for Horner Syndrome is highly recommended to all the patients who have a history of tadpole pupil episodes because studies have linked the two conditions. [7] Treatments [ edit ] Since the condition appears to slowly subside or diminish on its own, [1] there are no specific treatments for this condition available.
-
Perivascular Epithelioid Cell Tumour
Wikipedia
External links [ edit ] Classification D MeSH : D054973 External resources eMedicine : orthoped/377 v t e Connective / soft tissue tumors and sarcomas Not otherwise specified Soft-tissue sarcoma Desmoplastic small-round-cell tumor Connective tissue neoplasm Fibromatous Fibroma / fibrosarcoma : Dermatofibrosarcoma protuberans Desmoplastic fibroma Fibroma / fibromatosis : Aggressive infantile fibromatosis Aponeurotic fibroma Collagenous fibroma Diffuse infantile fibromatosis Familial myxovascular fibromas Fibroma of tendon sheath Fibromatosis colli Infantile digital fibromatosis Juvenile hyaline fibromatosis Plantar fibromatosis Pleomorphic fibroma Oral submucous fibrosis Histiocytoma / histiocytic sarcoma : Benign fibrous histiocytoma Malignant fibrous histiocytoma Atypical fibroxanthoma Solitary fibrous tumor Myxomatous Myxoma / myxosarcoma Cutaneous myxoma Superficial acral fibromyxoma Angiomyxoma Ossifying fibromyxoid tumour Fibroepithelial Brenner tumour Fibroadenoma Phyllodes tumor Synovial -like Synovial sarcoma Clear-cell sarcoma Lipomatous Lipoma / liposarcoma Myelolipoma Myxoid liposarcoma PEComa Angiomyolipoma Chondroid lipoma Intradermal spindle cell lipoma Pleomorphic lipoma Lipoblastomatosis Spindle cell lipoma Hibernoma Myomatous general: Myoma / myosarcoma smooth muscle : Leiomyoma / leiomyosarcoma skeletal muscle : Rhabdomyoma / rhabdomyosarcoma : Embryonal rhabdomyosarcoma Sarcoma botryoides Alveolar rhabdomyosarcoma Leiomyoma Angioleiomyoma Angiolipoleiomyoma Genital leiomyoma Leiomyosarcoma Multiple cutaneous and uterine leiomyomatosis syndrome Multiple cutaneous leiomyoma Neural fibrolipoma Solitary cutaneous leiomyoma STUMP Complex mixed and stromal Adenomyoma Pleomorphic adenoma Mixed Müllerian tumor Mesoblastic nephroma Wilms' tumor Malignant rhabdoid tumour Clear-cell sarcoma of the kidney Hepatoblastoma Pancreatoblastoma Carcinosarcoma Mesothelial Mesothelioma Adenomatoid tumor v t e Tumours of blood vessels Blood vessel Hemangiosarcoma Blue rubber bleb nevus syndrome Hemangioendothelioma Composite Endovascular papillary Epithelioid Kaposiform Infantile Retiform ) Spindle cell Proliferating angioendotheliomatosis Hemangiopericytoma Venous lake Kaposi's sarcoma African cutaneous African lymphadenopathic AIDS-associated Classic Immunosuppression-associated Hemangioblastoma Hemangioma Capillary Cavernous Glomeruloid Microvenular Targeted hemosiderotic Angioma Cherry Seriginosum Spider Tufted Universal angiomatosis Angiokeratoma of Mibelli Angiolipoma Pyogenic granuloma Lymphatic Lymphangioma / lymphangiosarcoma Lymphangioma circumscriptum Acquired progressive lymphangioma PEComa Lymphangioleiomyomatosis Cystic hygroma Multifocal lymphangioendotheliomatosis Lymphangiomatosis Either Angioma / angiosarcoma Angiofibroma
-
Mandibulofacial Dysostosis With Alopecia
Omim
Cushman et al. (2005) noted that this patient exhibited many of the features of Johnson-McMillin syndrome (147770) as well as features not previously reported in that phenotype, including preauricular pits and tags, broad depression at the lateral aspects of the eyes, and abnormal left lower eyelid. ... Zechi-Ceide et al. (2010) concluded that the facial phenotype of this patient was consistent with mandibulofacial dysostosis, and suggested that it could represent a severe form of Johnson-McMillin syndrome. Gordon et al. (2015) studied 3 patients with highly similar facial dysmorphism, including the boy previously reported by Zechi-Ceide et al. (2010), as well as a more mildly affected girl originally described by Cushman et al. (2005).
-
Hyperosmia
Wikipedia
The causes of hyperosmia may be genetic, hormonal, environmental or the result of benzodiazepine withdrawal syndrome . When odorants enter the nasal cavity, they bind to odorant receptors at the base of the olfactory epithelium. ... Treatment [ edit ] Normal olfactory acuity will usually return over time if the cause is environmental, even if it is untreated. [7] [8] The hyperosmic person may need to be removed from strong odorants for a period of time if the sensation becomes unbearable. [8] Before they had been discontinued due to undesirable side effects, butyrophenones or thioridazine hydrochloride , both of which are dopamine antagonists, have been used to treat hyperosmia. [8] See also [ edit ] Phantosmia Hyposmia Multiple chemical sensitivity , a condition that some believe is caused by a very acute sense of smell Olfaction Oliver Sacks Benzodiazepine withdrawal syndrome Parosmia References [ edit ] ^ "hyperosmia" .
-
Mental Retardation, Autosomal Dominant 50
Omim
One of the patients was a 15-year-old boy diagnosed with Asperger syndrome. Two of 4 patients were noted to have motor delay. ... Four patients had cardiac anomalies, one of whom had a complex heterotaxy syndrome. The patients were ascertained through international collaboration of research and clinical groups who shared whole-genome, whole-exome, or candidate gene sequencing results of patients with variable intellectual disability.
-
Lymphocytosis
Wikipedia
External links [ edit ] Classification D ICD - 10 : D72.8 ICD - 9-CM : 288.8 MeSH : D008218 DiseasesDB : 7678 v t e Leukaemias , lymphomas and related disease B cell ( lymphoma , leukemia ) (most CD19 CD20 ) By development/ marker TdT+ ALL ( Precursor B acute lymphoblastic leukemia/lymphoma ) CD5 + naive B cell ( CLL/SLL ) mantle zone ( Mantle cell ) CD22 + Prolymphocytic CD11c+ ( Hairy cell leukemia ) CD79a + germinal center / follicular B cell ( Follicular Burkitt's GCB DLBCL Primary cutaneous follicle center lymphoma ) marginal zone / marginal zone B-cell ( Splenic marginal zone MALT Nodal marginal zone Primary cutaneous marginal zone lymphoma ) RS ( CD15 +, CD30 +) Classic Hodgkin lymphoma ( Nodular sclerosis ) CD20+ ( Nodular lymphocyte predominant Hodgkin lymphoma ) PCDs / PP ( CD38 +/ CD138 +) see immunoproliferative immunoglobulin disorders By infection KSHV ( Primary effusion ) EBV Lymphomatoid granulomatosis Post-transplant lymphoproliferative disorder Classic Hodgkin lymphoma Burkitt's lymphoma HCV Splenic marginal zone lymphoma HIV ( AIDS-related lymphoma ) Helicobacter pylori ( MALT lymphoma ) Cutaneous Diffuse large B-cell lymphoma Intravascular large B-cell lymphoma Primary cutaneous marginal zone lymphoma Primary cutaneous immunocytoma Plasmacytoma Plasmacytosis Primary cutaneous follicle center lymphoma T/NK T cell ( lymphoma , leukemia ) (most CD3 CD4 CD8 ) By development/ marker TdT+ : ALL ( Precursor T acute lymphoblastic leukemia/lymphoma ) prolymphocyte ( Prolymphocytic ) CD30+ ( Anaplastic large-cell lymphoma Lymphomatoid papulosis type A ) Cutaneous MF+variants indolent: Mycosis fungoides Pagetoid reticulosis Granulomatous slack skin aggressive: Sézary disease Adult T-cell leukemia/lymphoma Non-MF CD30 -: Non-mycosis fungoides CD30− cutaneous large T-cell lymphoma Pleomorphic T-cell lymphoma Lymphomatoid papulosis type B CD30 +: CD30+ cutaneous T-cell lymphoma Secondary cutaneous CD30+ large-cell lymphoma Lymphomatoid papulosis type A Other peripheral Hepatosplenic Angioimmunoblastic Enteropathy-associated T-cell lymphoma Peripheral T-cell lymphoma not otherwise specified ( Lennert lymphoma ) Subcutaneous T-cell lymphoma By infection HTLV-1 ( Adult T-cell leukemia/lymphoma ) NK cell / (most CD56 ) Aggressive NK-cell leukemia Blastic NK cell lymphoma T or NK EBV ( Extranodal NK-T-cell lymphoma / Angiocentric lymphoma ) Large granular lymphocytic leukemia Lymphoid+ myeloid Acute biphenotypic leukaemia Lymphocytosis Lymphoproliferative disorders ( X-linked lymphoproliferative disease Autoimmune lymphoproliferative syndrome ) Leukemoid reaction Diffuse infiltrative lymphocytosis syndrome Cutaneous lymphoid hyperplasia Cutaneous lymphoid hyperplasia with bandlike and perivascular patterns with nodular pattern Jessner lymphocytic infiltrate of the skin General Hematological malignancy leukemia Lymphoproliferative disorders Lymphoid leukemiasCARD11, ZAP70, SH2D1A, XIAP, IL7R, ARPC1B, PRKCD, LMNB2, RNASEH2B, NRAS, KRAS, TRBV20OR9-2, IL2, NCAM1, FCGR3B, FCGR3A, IGH, B3GAT1, IGHV3-69-1, CCND1, LOC102723407, LOC102724971, IGHV3OR16-7, CD19, HLA-DRB1, TP53, STAT3, TGFB1, THPO, SLC19A1, TNF, ADA, LAP, TCL1A, PDLIM7, LONP1, TCL1B, RFC1, DLEU1, SLC27A5, NRM, IGHV3-23, IGHV1-2, PARP9, MLSM7, CCL5, MYD88, PTPRC, CBLIF, FAS, AR, BCL2, BCR, CBL, CD5, CD14, CD27, CD28, CD38, CEL, CSF2, FCER2, GNAZ, PIM1, IL5, CXCL8, ITGA4, ITGAE, ITGAM, ITGAX, LAMC2, MDM2, MME, MS, MYC, ANG, SERPINA5, RN7SL263P
-
Spring Viraemia Of Carp
Wikipedia
External links [ edit ] Spring Viraemia of Carp expert reviewed and published by Wikivet, accessed 08/10/2011. v t e Fish diseases and parasites Pathogens Aeromonas salmonicida Nervous necrosis virus Columnaris Enteric redmouth Fin rot Fish dropsy Flavobacterium Hematopoietic necrosis Heterosigma akashiwo Hole in the head Hypodermal and hematopoietic necrosis Infectious pancreatic necrosis Koi herpes virus Mycobacterium marinum Novirhabdovirus Pfiesteria piscicida Photobacterium damselae ssp piscicida Salmon anemia Streptococcus iniae Spring viraemia of carp Taura syndrome UDN VHS White spot Yellowhead Parasites Abergasilus Amoebic gill disease Anisakis Carp lice Ceratomyxa shasta Clinostomum marginatum Dactylogyrus vastator Diphyllobothrium Cymothoa exigua Eustrongylidosis Epizootic ulcerative syndrome Flukes Glugea Gyrodactylus salaris Henneguya zschokkei Ich (freshwater) Ich (marine) Kudoa thyrsites Lernaeocera branchialis Microsporidia Monogenea Myxobolus cerebralis Myxosporea Nanophyetus salmincola Pseudorhabdosynochus spp.
-
Retinal Migraine
Wikipedia
Retinal migraine tends to be more common in: Women People aged under 40 People with a personal or family history of migraines or other headaches People with an underlying disease ( lupus , hardening of the arteries , sickle cell disease , epilepsy , antiphospholipid syndrome , and giant cell arteritis ) [4] Diagnosis [ edit ] The medical exam should rule out any underlying causes, such as blood clot, stroke, pituitary tumor, or detached retina. ... External links [ edit ] Classification D ICD - 10 : G43.81 v t e Headache Primary ICHD 1 Migraine Familial hemiplegic Retinal migraine ICHD 2 Tension Mixed tension migraine ICHD 3 Cluster Chronic paroxysmal hemicrania SUNCT ICHD 4 Hemicrania continua Thunderclap headache Sexual headache New daily persistent headache Hypnic headache Secondary ICHD 5 Migralepsy ICHD 7 Ictal headache Post-dural-puncture headache ICHD 8 Hangover Medication overuse headache ICHD 13 Trigeminal neuralgia Occipital neuralgia External compression headache Cold-stimulus headache Optic neuritis Postherpetic neuralgia Tolosa–Hunt syndrome Other Vascular
-
Normal Weight Obesity
Wikipedia
Contents 1 Definition 2 Prevalence 3 Treatment 4 References Definition [ edit ] Main article: Classification of obesity The term "metabolically obese normal weight" (MONW) refers to people with normal weight and body mass index (BMI), who display some metabolic characteristics which increase the risk of developing metabolic syndrome in the same way as obesity. People with MONW have excess visceral fat, and are predisposed to hyperinsulinemia, insulin-resistance and thus predisposition to type 2 diabetes, hypertriglyceridemia, hypertension and premature coronary heart disease or cardiovascular disease . [1] The BMI does not capture information about percentage body fat (PBF), which is a better predictor of risk due to obesity. [2] [3] [4] [5] Some studies have suggested that the main factor which explains the metabolic abnormalities in MONW individuals is fat distribution. On the basis of these studies, a scoring method has been proposed to identify MONW individuals, based on the presence of associated diseases or biochemical abnormalities related to insulin resistance. [6] Prevalence [ edit ] In 2008, the first prevalence of US adults above 20 years was published, based on the National Health and Nutrition Examination Surveys from 1999-2004, finding that 24% of normal-weight adults were metabolically abnormal; on the other hand 51% of overweight adults and 32% of obese adults were metabolically healthy. [7] An analysis from an earlier NHANES from 1988 to 1994 found people with NWO had a four-fold higher frequency of metabolic syndrome compared with the low body fat group. [8] Treatment [ edit ] As of 2018, optimal treatment is unknown. [9] A 1998 study suggested that energy restriction and weight loss, for example a 4- to 12-week period of diet and exercise was beneficial. [1] A small study of 11 Asians with MONW published June 2018 found that moderate weight loss through dieting reduced their cardiometabolic risk per improved body composition, lipid profile, and insulin sensitivity. [9] References [ edit ] ^ a b Ruderman, N; Chisholm, D; Pi-Sunyer, X; Schneider, S (May 1998).
-
Platelet Glycoprotein Iv Deficiency
Omim
Four members of his family, including a son, also had macrothrombocytopenia without notable bleeding tendency. The Bernard-Soulier syndrome (231200) is another form of familial macrothrombocytopenia, which is caused by a defect in platelet glycoprotein Ib (138720). ... Miyaoka et al. (2001) concluded that CD36 deficiency might be a cause of human insulin resistance syndrome in the Japanese population. Yanai et al. (2007) evaluated the aerobic exercise capacity of 12 women with CD36 deficiency, including 2 with type I and 10 with type II.
-
Histiocytosis
Wikipedia
. ^ Goldberg, J; Nezelof, C (1986), "Lymphohistiocytosis: a multi-factorial syndrome of macrophagic activation clinico-pathological study of 38 cases", Hematol Oncol , 4 (4): 275–289, PMID 3557322 . ^ Egan, Caoimhe; Jaffe, Elaine S. (2018). ... "What is the Histiocyte Society classification of histiocytosis syndromes?" . Medscape . Retrieved 4 December 2020 . ^ Chang, Karen L.; Snyder, David S. (2007). "17.
-
Precursor B-Cell Lymphoblastic Leukemia
Wikipedia
External links [ edit ] Classification D ICD - 10 : C83.5 ICD-O : M9836/3 MeSH : D015452 Precursor B-lymphoblastic leukemia entry in the public domain NCI Dictionary of Cancer Terms v t e Leukaemias , lymphomas and related disease B cell ( lymphoma , leukemia ) (most CD19 CD20 ) By development/ marker TdT+ ALL ( Precursor B acute lymphoblastic leukemia/lymphoma ) CD5 + naive B cell ( CLL/SLL ) mantle zone ( Mantle cell ) CD22 + Prolymphocytic CD11c+ ( Hairy cell leukemia ) CD79a + germinal center / follicular B cell ( Follicular Burkitt's GCB DLBCL Primary cutaneous follicle center lymphoma ) marginal zone / marginal zone B-cell ( Splenic marginal zone MALT Nodal marginal zone Primary cutaneous marginal zone lymphoma ) RS ( CD15 +, CD30 +) Classic Hodgkin lymphoma ( Nodular sclerosis ) CD20+ ( Nodular lymphocyte predominant Hodgkin lymphoma ) PCDs / PP ( CD38 +/ CD138 +) see immunoproliferative immunoglobulin disorders By infection KSHV ( Primary effusion ) EBV Lymphomatoid granulomatosis Post-transplant lymphoproliferative disorder Classic Hodgkin lymphoma Burkitt's lymphoma HCV Splenic marginal zone lymphoma HIV ( AIDS-related lymphoma ) Helicobacter pylori ( MALT lymphoma ) Cutaneous Diffuse large B-cell lymphoma Intravascular large B-cell lymphoma Primary cutaneous marginal zone lymphoma Primary cutaneous immunocytoma Plasmacytoma Plasmacytosis Primary cutaneous follicle center lymphoma T/NK T cell ( lymphoma , leukemia ) (most CD3 CD4 CD8 ) By development/ marker TdT+ : ALL ( Precursor T acute lymphoblastic leukemia/lymphoma ) prolymphocyte ( Prolymphocytic ) CD30+ ( Anaplastic large-cell lymphoma Lymphomatoid papulosis type A ) Cutaneous MF+variants indolent: Mycosis fungoides Pagetoid reticulosis Granulomatous slack skin aggressive: Sézary disease Adult T-cell leukemia/lymphoma Non-MF CD30 -: Non-mycosis fungoides CD30− cutaneous large T-cell lymphoma Pleomorphic T-cell lymphoma Lymphomatoid papulosis type B CD30 +: CD30+ cutaneous T-cell lymphoma Secondary cutaneous CD30+ large-cell lymphoma Lymphomatoid papulosis type A Other peripheral Hepatosplenic Angioimmunoblastic Enteropathy-associated T-cell lymphoma Peripheral T-cell lymphoma not otherwise specified ( Lennert lymphoma ) Subcutaneous T-cell lymphoma By infection HTLV-1 ( Adult T-cell leukemia/lymphoma ) NK cell / (most CD56 ) Aggressive NK-cell leukemia Blastic NK cell lymphoma T or NK EBV ( Extranodal NK-T-cell lymphoma / Angiocentric lymphoma ) Large granular lymphocytic leukemia Lymphoid+ myeloid Acute biphenotypic leukaemia Lymphocytosis Lymphoproliferative disorders ( X-linked lymphoproliferative disease Autoimmune lymphoproliferative syndrome ) Leukemoid reaction Diffuse infiltrative lymphocytosis syndrome Cutaneous lymphoid hyperplasia Cutaneous lymphoid hyperplasia with bandlike and perivascular patterns with nodular pattern Jessner lymphocytic infiltrate of the skin General Hematological malignancy leukemia Lymphoproliferative disorders Lymphoid leukemias This oncology article is a stub .IKZF1, GATA3, TCF3, RUNX1, PAX5, ETV6, CCN2, ATF7IP, DUX4, MGA, CRLF2, STAT3, CDKN2A, PIP4K2A, CD19, PBX1, LHPP, ARID5B, CCDC26, MME, ELK3, ABL1, BCR, BCL2, CD22, PBXIP1, HCFC1R1, NR3C1, TRBV20OR9-2, CDR3, KMT2A, MYC, PIK3CD, PBX3, AKT1, SALL4, PKNOX1, BLNK, SMUG1, IL7, INSR, LINC02605, CD33, CD6, CDKN2B, HOXB4, CD79A, FBLIM1, RTEL1, WNT16, LEF1, CDK2, UHRF1, AFF4, CDKN1B, MAPRE1, MAPRE2, PDLIM5, CSF1R, GSTO1, KLF4, COX7A2L, NRP1, BECN1, KMO, DNMT3A, TAF15, CD79B, ANKS1B, FMN2, ZAP70, ALL1, ANPEP, RASSF10, TARP, MIR203A, MIR152, ZNF384, RASSF6, CBLL2, OPN1SW, GSTO2, TP53INP1, RCSD1, PHF6, BTK, ARHGAP24, MUL1, DCLRE1C, CAPG, CD47, GOPC, PAX8, TPD52, HOXB5, LTA4H, HIF1A, PRKN, ROR1, NCL, HLF, MPO, HOXB@, AFF1, HOXB1, LYL1, AFF3, FLT3, HOXB2, IL15, HOXB3, IL4, IL1B, IL1A, HOXB9, HOXB8, HOXB7, HOXB6, FUT4, PCM1, TPBG, EPHA3, TP73, TP53, THY1, TRGC1, TRG, DNTT, TRA, ENG, TACR1, TAC1, SRC, PIK3CA, SLC22A2, SELE, PTEN, POU2F2, PLA2G4A, EPS15, ETV5, EVPL, FAT1, PIK3CB, PIK3CG