-
Thyroid Disease
Wikipedia
The main categories are: Thyroiditis : an inflammation of the thyroid gland Hashimoto's thyroiditis / Hashimoto's disease Ord's thyroiditis Postpartum thyroiditis Silent thyroiditis Acute thyroiditis Riedel's thyroiditis (the majority of cases do not affect thyroid function, but approximately 30% of cases lead to hypothyroidism) Iatrogenic hypothyroidism [16] Postoperative hypothyroidism Medication- or radiation-induced hypothyroidism Thyroid hormone resistance Euthyroid sick syndrome Congenital hypothyroidism : a deficiency of thyroid hormone from birth, which untreated can lead to cretinism High function [ edit ] Exophthalmos is the eye bulging that may be seen with Graves Disease, one of the major causes of hyperthyroidism Main article: Hyperthyroidism Hyperthyroidism is a state in which the body is producing too much thyroid hormone. ... Radioiodine scanning and uptake [ edit ] Five scintigrams taken from thyroids with different syndromes: A) normal thyroid, B) Graves disease, diffuse increased uptake in both thyroid lobes, C) Plummer's disease, D) Toxic adenoma, E) Thyroiditis. ... Radioiodine treatment can also cause hypothyroidism (which is sometimes the end goal of treatment) and, although rare, a pain syndrome (due to radiation thyroiditis) . [31] Epidemiology [ edit ] In the United States, autoimmune inflammation is the most common form of thyroid disease while worldwide hypothyroidism and goiter due to dietary iodine deficiency is the most common. [32] [33] Hypothyroidism affects 3-10% percent of adults, with a higher incidence in women and the elderly. [34] [35] [36] An estimated one-third of the world's population currently lives in areas of low dietary iodine levels. ... External links [ edit ] Classification D ICD - 10 : E00-E07, Q89.1-Q89.2 ICD - 9-CM : 240 - 246 , 759.1 - 759.2 MeSH : D013959 SNOMED CT : 14304000 Thyroid disease at Curlie Medline Plus Medical Encyclopedia entry for Thyroid Disease National Institutes of Health v t e Thyroid disease Hypothyroidism Iodine deficiency Cretinism Congenital hypothyroidism Myxedema Myxedema coma Euthyroid sick syndrome Signs and symptoms Queen Anne's sign Woltman sign Thyroid dyshormonogenesis Pickardt syndrome Hyperthyroidism Hyperthyroxinemia Thyroid hormone resistance Familial dysalbuminemic hyperthyroxinemia Hashitoxicosis Thyrotoxicosis factitia Thyroid storm Graves' disease Signs and symptoms Abadie's sign of exophthalmic goiter Boston's sign Dalrymple's sign Stellwag's sign lid lag Griffith's sign Möbius sign Pretibial myxedema Graves' ophthalmopathy Thyroiditis Acute infectious Subacute De Quervain's Subacute lymphocytic Palpation Autoimmune /chronic Hashimoto's Postpartum Riedel's Enlargement Goitre Endemic goitre Toxic nodular goitre Toxic multinodular goiter Thyroid nodule Colloid nodule v t e Congenital endocrine disorders Pituitary Congenital hypopituitarism Thyroid Thyroid disease Persistent thyroglossal duct Thyroglossal cyst Congenital hypothyroidism Thyroid dysgenesis Thyroid dyshormonogenesis Pendred syndrome Parathyroid Congenital absence of parathyroid Adrenal Absent adrenal glandTSHR, CCL2, DIO2, KLF9, GULP1, DIO1, ITGB5, TGOLN2, TBX3, ID2, ZNF676, CNST, ID3, PTEN, TG, CTLA4, SLC5A5, TPO, HT, SLC16A2, BRAF, PTPN22, RET, TNF, FOXP3, CALCA, SLC26A4, IL17A, IL4, IL13, CD40, DICER1, TNFRSF1A, VDR, HLA-DRB1, GH1, VEGFA, PAX8, NCOA4, TNFSF10, SH2B3, NKX2-1, IL6, ZFAT, IGF1, IFNG, VAMAS6, MIR125A, ICAM1, HMGA1, STAT3, ABO, CD52, BCL2, GAD2, CAT, CTSB, GNB3, MED12, IL18RAP, IL18R1, INPP4B, NRP2, SQSTM1, SOCS3, CD83, VAV3, AQP4, RNASET2, SLC19A2, TXNRD2, FASLG, KHDRBS1, IKZF3, TBC1D9, ICOSLG, ATD, BAX, PDE8B, TNFSF4, TLR4, CD47, CD34, TNFRSF1B, TP53, CD14, TRH, UCP2, FOSL1, CAPZB, PTTG1IP, BEST1, XRCC3, XRCC5, TNDM, SMUG1, XIAP, NUP62, TGFB1, AIRE, FCRL3, CYP2R1, RBM45, ALB, CEP128, IL23R, SLC5A8, AHSG, AGA, GLIS3, PARP4, IL27, LINC01193, SERPINA13P, PARP1, MIR34A, MIR499A, MT1IP, PSS, FCRL1, MAGT1, SECISBP2, HSD17B7, HIPK2, DROSHA, CD274, TBX21, NOX4, APC, DCTN4, ALPP, GHRL, SMOC2, DUOX1, BANK1, UACA, CHDH, SELENOS, ZNF395, ALG1, ALPI, THRA, CISH, CXCR3, JUND, IL16, ERBB2, CXCL10, INSL3, IRAK1, DMD, JUN, JUNB, KIT, FOXE1, LGALS1, LGALS3, LRP2, LTA, EPCAM, MBL2, MECP2, CXCL9, IL15, FOXO3, MT1B, GAD1, GPX4, GSTM1, GSTT1, GTF2H1, HFE, HLA-A, LRRC32, IAPP, GABPA, FOLH1, FSHR, IFNA1, IFNA13, FOSB, FOS, IGFBP3, IL1B, IL2RA, MT1A, MT1E, TFPI, SNX2, S100A1, S100B, CTSL, CCL5, CXCL12, SEL1L, SLC2A1, CTAG1B, SPTAN1, CYP1A1, SSTR2, CCR6, STAT4, STATH, TBXT, CCR5, TRA, TERT, RXRB, REN, MT1F, MYO9B, MT1G, MT1H, MT1JP, MT1M, MT1L, MT1X, MTHFR, MTNR1A, NFE2L2, PTGS2, TNFRSF11B, SERPINE1, PDE4D, CYP1A2, ABCB1, PTCH1, ACR, PTGDS, THRA1/BTR
-
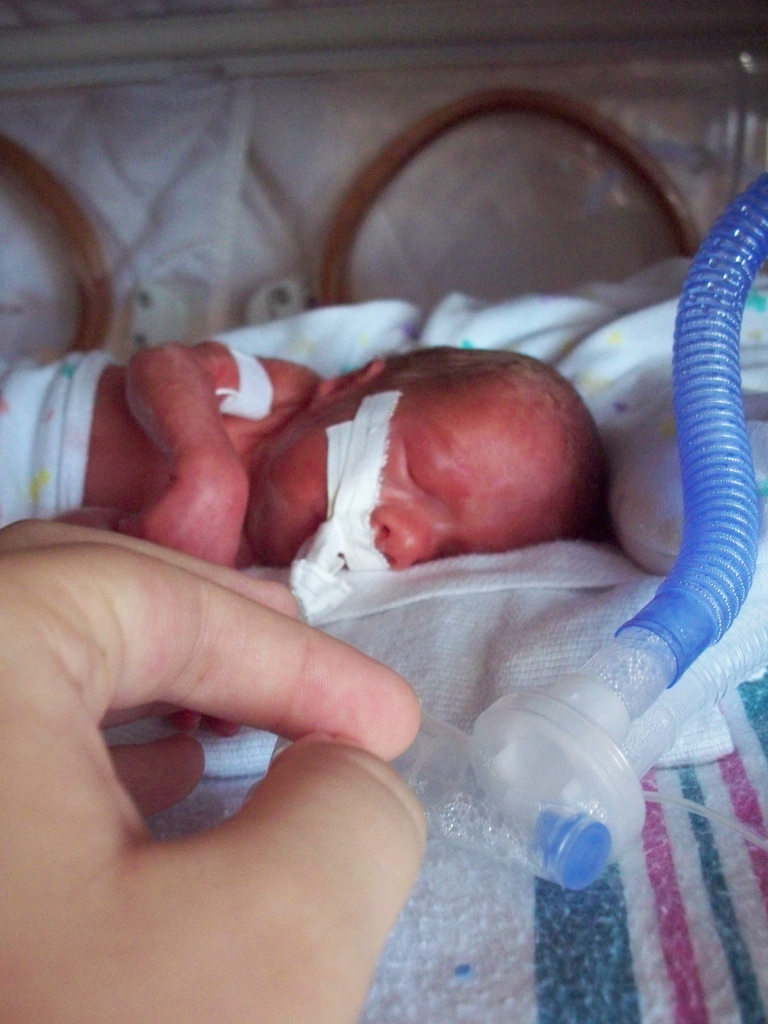
Premature Birth
Mayo_clinic
This is a treatable problem called respiratory distress syndrome. It's common for preterm babies to have pauses in their breathing called apnea. ... Premature infants also are at higher risk of sudden infant death syndrome (SIDS). That's when an infant dies for unclear reasons, often while asleep. ... Depending on your baby's health, the medicines they receive may include: Surfactant, which is used to treat respiratory distress syndrome. Fine-mist or medicines given in a vein to strengthen breathing and heart rate.TNF, IL4, IL6, CAT, OGG1, EDN1, PTGS2, MMP9, SOD2, MBL2, LTF, ADAMTS2, SF3B4, PEX16, KMT2B, TMEM94, FIG4, MED12, ACTA1, ZMPSTE24, KLHL41, WDR4, MAGED2, SLC27A4, NIPBL, COG4, TRIP4, FOXH1, AIMP1, SMC3, SIX3, SLC12A1, TDGF1, TGFB1, TGIF1, TPM3, TSHR, TUB, ZIC2, BSND, LZTR1, SMC1A, LAGE3, FZD4, PEX3, CNTNAP1, DNAH11, PEX11B, SLC17A5, ABCA12, TPRKB, DLL1, TP53RK, ARHGAP31, DOCK6, NLRC4, EEFSEC, IFIH1, WDR73, DISP1, STRADA, TBCK, NLRP3, CDON, KLHL40, ESCO2, ADCY4, HYLS1, COL24A1, EOGT, KIF7, RNU4ATAC, MICOS10-NBL1, ARID1B, PRR12, NUP107, LMOD3, RPS19, ASCC1, WAC, SUFU, NDUFB11, MAGEL2, DLL4, SARS2, TMEM70, BANP, PNPO, SETD5, ASXL2, CHD7, FLVCR2, OSGEP, PEX26, NUP133, HDAC8, SHH, RPL10, LRP5, HOXD13, FLI1, FLNB, MTOR, GAS1, GBA, GLI2, GNAQ, GNAS, HRAS, FGF8, IGHMBP2, RBPJ, ITGB4, KCNJ1, KRAS, LMNA, ALB, MECP2, FGFR1, FBN1, KMT2A, COL1A2, ATP5F1D, BCR, BRAF, CAPN1, CLCN7, CLCNKA, CLCNKB, COL1A1, COL3A1, DYRK1A, COL5A1, COL5A2, COL11A1, CRKL, CYP11A1, DHCR7, DYNC1H1, SLC26A3, MIPEP, SNHG22, ATP6, MAP2K1, PEX10, PEX13, PEX14, ATP8B1, ABCB4, PLEC, PMM2, MAPK1, MAP2K2, PEX1, PTCH1, PTH1R, PTPN11, PEX19, PEX2, PEX5, RAD21, RIT1, PEX6, PEX12, NOTCH2, NODAL, NDUFB3, NEB, NDP, MUSK, MYH7, MYO5B, NBL1, NOTCH1, LTA, SLC23A1, RLN1, CFB, TLR2, TLR4, IL1RN, IL13, IL6R, VEGFA, IL1B, IL1A, PPARG, SLC23A2, NR3C1, GDF15, MTHFR, CXCL5
-
Lactose Intolerance
Wikipedia
Lactose intolerance Other names Lactase deficiency, hypolactasia, alactasia Lactose is made up of two simple sugars Specialty Gastroenterology Symptoms Abdominal pain, bloating , diarrhea , flatulence , nausea [1] Complications Does not cause damage to the GI tract [2] Usual onset 30–120 min after dairy products [1] Causes Decreased ability to digest lactose (genetic, small intestine injury) [1] Diagnostic method Symptoms resolve following eliminating lactose [1] Differential diagnosis Irritable bowel syndrome , celiac disease , inflammatory bowel disease , milk allergy [1] Treatment Decreasing lactose in the diet, lactase supplements , treat the underlying cause [1] Frequency ~65% of people (less common in Europeans) [3] Lactose intolerance is a common condition caused by a decreased ability to digest lactose , a sugar found in dairy products . [1] Those affected vary in the amount of lactose they can tolerate before symptoms develop. [1] Symptoms may include abdominal pain , bloating , diarrhea , gas , and nausea . [1] These symptoms typically start thirty minutes to two hours after eating or drinking milk-based food. [1] Their severity typically depends on the amount a person eats or drinks. [1] Lactose intolerance does not cause damage to the gastrointestinal tract . [2] Lactose intolerance is due to the lack of the enzyme lactase in the small intestines to break lactose down into glucose and galactose . [3] There are four types: primary, secondary, developmental, and congenital. [1] Primary lactose intolerance occurs as the amount of lactase declines as people age. [1] Secondary lactose intolerance is due to injury to the small intestine. Such injury could be the result of infection, celiac disease , inflammatory bowel disease , or other diseases. [1] [4] Developmental lactose intolerance may occur in premature babies and usually improves over a short period of time. [1] Congenital lactose intolerance is an extremely rare genetic disorder in which little or no lactase is made from birth. [1] The onset of primary lactose intolerance, the most common type, is typically in late childhood or early adulthood, [1] but prevalence increases with age. [5] Diagnosis may be confirmed if symptoms resolve following eliminating lactose from the diet. [1] Other supporting tests include a hydrogen breath test and a stool acidity test . [1] Other conditions that may produce similar symptoms include irritable bowel syndrome , celiac disease , and inflammatory bowel disease . [1] Lactose intolerance is different from a milk allergy . [1] Management is typically by decreasing the amount of lactose in the diet, taking lactase supplements , or treating the underlying disease. [1] [6] People are usually able to drink at least one cup of milk per sitting without developing significant symptoms, with greater amounts tolerated if drunk with a meal or throughout the day. [1] [7] Most adults (around 65–70% of the world's population) are lactose intolerant. [5] [8] Other mammals normally lose the ability to digest lactose after weaning and this was the ancestral state of all humans before the recent evolution of lactase persistence , which extends lactose tolerance into adulthood. [9] Lactase persistence evolved in several populations independently, probably as an adaptation to the domestication of dairy animals around 10,000 years ago. [10] [11] Today the prevalence of lactose tolerance varies widely between regions and ethnic groups. [5] It is most common in people of European descent, and to a lesser extent in parts of the Middle East and Africa. [5] [8] Traditional food cultures reflect local variations in tolerance [5] and historically many societies have adapted to low levels of tolerance by making dairy products that contain less lactose than fresh milk. [12] The medicalization of lactose intolerance as a disorder has been attributed to biases in research history (most early studies were conducted amongst populations where tolerance is the norm) [9] as well as the cultural and economic importance of milk in countries such as the United States. [13] Contents 1 Terminology 2 Signs and symptoms 3 Causes 3.1 Primary hypolactasia 3.2 Secondary hypolactasia 3.3 Primary congenital alactasia 4 Diagnosis 4.1 Hydrogen breath test 4.2 Blood test 4.3 Stool acidity test 4.4 Intestinal biopsy 4.5 Stool sugar chromatography 4.6 Genetic diagnostic 5 Management 5.1 Dietary avoidance 5.2 Milk substitutes 5.3 Lactase supplements 5.4 Rehabituation to dairy products 6 Epidemiology 7 History 7.1 History of research 8 Other animals 9 See also 10 References 11 External links Terminology [ edit ] Lactose intolerance primarily refers to a syndrome having one or more symptoms upon the consumption of food substances containing lactose. ... "Celiac disease: an immune dysregulation syndrome". Current Problems in Pediatric and Adolescent Health Care (Review). 44 (11): 324–7. doi : 10.1016/j.cppeds.2014.10.002 . ... External links [ edit ] Classification D ICD - 10 : E73 ICD - 9-CM : 271.3 OMIM : 223100 MeSH : D007787 DiseasesDB : 7238 External resources MedlinePlus : 000276 eMedicine : med/3429 ped/1270 Patient UK : Lactose intolerance Lactose intolerance at Curlie Human Culture, an Evolutionary Force v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum v t e Inborn error of carbohydrate metabolism : monosaccharide metabolism disorders Including glycogen storage diseases (GSD) Sucrose , transport (extracellular) Disaccharide catabolism Congenital alactasia Sucrose intolerance Monosaccharide transport Glucose-galactose malabsorption Inborn errors of renal tubular transport ( Renal g
-
Meningococcal Disease
Wikipedia
Later symptoms include septic shock , purpura , hypotension, cyanosis, petechiae , seizures, anxiety, and multiple organ dysfunction syndrome . Acute respiratory distress syndrome and altered mental status may also occur. ... In 1884, Italian pathologists Ettore Marchiafava and Angelo Celli described intracellular micrococci in cerebrospinal fluid , and in 1887, Anton Wiechselbaum identified the meningococcus (designated as Diplococcus intracellularis meningitidis ) in cerebrospinal fluid and established the connection between the organism and epidemic meningitis. [48] See also [ edit ] Endocarditis Pathogenic bacteria Waterhouse–Friderichsen syndrome African meningitis belt 2009–10 West African meningitis outbreak Meningococcal vaccine Meningitis Vaccine Project References [ edit ] ^ Riedo FX, Plikaytis BD, Broome CV (August 1995). ... External links [ edit ] Classification D ICD - 10 : A39 ICD - 9-CM : 036.9 MeSH : D008589 DiseasesDB : 8847 SNOMED CT : 23511006 External resources MedlinePlus : 000608 DermAtlas -1886809878 v t e Proteobacteria -associated Gram-negative bacterial infections α Rickettsiales Rickettsiaceae / ( Rickettsioses ) Typhus Rickettsia typhi Murine typhus Rickettsia prowazekii Epidemic typhus , Brill–Zinsser disease , Flying squirrel typhus Spotted fever Tick-borne Rickettsia rickettsii Rocky Mountain spotted fever Rickettsia conorii Boutonneuse fever Rickettsia japonica Japanese spotted fever Rickettsia sibirica North Asian tick typhus Rickettsia australis Queensland tick typhus Rickettsia honei Flinders Island spotted fever Rickettsia africae African tick bite fever Rickettsia parkeri American tick bite fever Rickettsia aeschlimannii Rickettsia aeschlimannii infection Mite-borne Rickettsia akari Rickettsialpox Orientia tsutsugamushi Scrub typhus Flea-borne Rickettsia felis Flea-borne spotted fever Anaplasmataceae Ehrlichiosis : Anaplasma phagocytophilum Human granulocytic anaplasmosis , Anaplasmosis Ehrlichia chaffeensis Human monocytotropic ehrlichiosis Ehrlichia ewingii Ehrlichiosis ewingii infection Rhizobiales Brucellaceae Brucella abortus Brucellosis Bartonellaceae Bartonellosis : Bartonella henselae Cat-scratch disease Bartonella quintana Trench fever Either B. henselae or B. quintana Bacillary angiomatosis Bartonella bacilliformis Carrion's disease , Verruga peruana β Neisseriales M+ Neisseria meningitidis/meningococcus Meningococcal disease , Waterhouse–Friderichsen syndrome , Meningococcal septicaemia M− Neisseria gonorrhoeae/gonococcus Gonorrhea ungrouped: Eikenella corrodens / Kingella kingae HACEK Chromobacterium violaceum Chromobacteriosis infection Burkholderiales Burkholderia pseudomallei Melioidosis Burkholderia mallei Glanders Burkholderia cepacia complex Bordetella pertussis / Bordetella parapertussis Pertussis γ Enterobacteriales ( OX− ) Lac+ Klebsiella pneumoniae Rhinoscleroma , Pneumonia Klebsiella granulomatis Granuloma inguinale Klebsiella oxytoca Escherichia coli : Enterotoxigenic Enteroinvasive Enterohemorrhagic O157:H7 O104:H4 Hemolytic-uremic syndrome Enterobacter aerogenes / Enterobacter cloacae Slow/weak Serratia marcescens Serratia infection Citrobacter koseri / Citrobacter freundii Lac− H2S+ Salmonella enterica Typhoid fever , Paratyphoid fever , Salmonellosis H2S− Shigella dysenteriae / sonnei / flexneri / boydii Shigellosis , Bacillary dysentery Proteus mirabilis / Proteus vulgaris Yersinia pestis Plague / Bubonic plague Yersinia enterocolitica Yersiniosis Yersinia pseudotuberculosis Far East scarlet-like fever Pasteurellales Haemophilus : H. influenzae Haemophilus meningitis Brazilian purpuric fever H. ducreyi Chancroid H. parainfluenzae HACEK Pasteurella multocida Pasteurellosis Actinobacillus Actinobacillosis Aggregatibacter actinomycetemcomitans HACEK Legionellales Legionella pneumophila / Legionella longbeachae Legionnaires' disease Coxiella burnetii Q fever Thiotrichales Francisella tularensis Tularemia Vibrionaceae Vibrio cholerae Cholera Vibrio vulnificus Vibrio parahaemolyticus Vibrio alginolyticus Plesiomonas shigelloides Pseudomonadales Pseudomonas aeruginosa Pseudomonas infection Moraxella catarrhalis Acinetobacter baumannii Xanthomonadaceae Stenotrophomonas maltophilia Cardiobacteriaceae Cardiobacterium hominis HACEK Aeromonadales Aeromonas hydrophila / Aeromonas veronii Aeromonas infection ε Campylobacterales Campylobacter jejuni Campylobacteriosis , Guillain–Barré syndrome Helicobacter pylori Peptic ulcer , MALT lymphoma , Gastric cancer Helicobacter cinaedi Helicobacter cellulitisCFHR3, CFH, ACE, CFD, ADAM32, FBXO15, CNTNAP5, ZMIZ1, GRM5, PRDM11, OLA1, ALCAM, NUP62, MYO16, TMPRSS15, IL4I1, CES1, SERPINE1, MBL2, TLR4, TNF, IL10, ST11, IL1A, C7, IL1RN, TLR2, IL1B, CD46, FCGR2C, CFP, ABO, SFTPA2, IL4, FCGR2A, FCGR2B, CPB2, DHPS, DEFA4, C5AR2, BPIFA1, TLR9, ENAH, AP2M1, CD14, SERPING1, C11orf40, CEACAM1, CFB, ADRB1, SFTPA1, DEFB1, CXCL10, EGFR, F3, GAPDH, SLC11A1, SFTPD, CXCL11, RELA, CFHR1, PLG, IGHA1, PC, IL1R1, NMB, MIF, ADD1, ALKBH1
-
Foodborne Illness
Wikipedia
However, in some cases, such as Staphylococcal food poisoning, the onset of illness can be as soon as 30 minutes after ingesting contaminated food. [5] Salmonella Most common bacterial foodborne pathogens are: Campylobacter jejuni which can lead to secondary Guillain–Barré syndrome and periodontitis [6] Clostridium perfringens , the "cafeteria germ" [7] [8] Salmonella spp. – its S. typhimurium infection is caused by consumption of eggs or poultry that are not adequately cooked or by other interactive human-animal pathogens [9] [10] [11] Escherichia coli O157:H7 enterohemorrhagic (EHEC) which can cause hemolytic-uremic syndrome Other common bacterial foodborne pathogens are: [ citation needed ] Bacillus cereus Escherichia coli , other virulence properties , such as enteroinvasive (EIEC), enteropathogenic (EPEC), enterotoxigenic (ETEC), enteroaggregative (EAEC or EAgEC) Listeria monocytogenes Shigella spp. ... Some of the toxins can be present in sorghum, ragi , wheat and tomatoes. [24] [25] [26] Some research has shown that the toxins can be easily cross-contaminated between grain commodities, suggesting that manufacturing and storage of grain commodities is a critical practice. [27] Citrinin Citreoviridin Cyclopiazonic acid Cytochalasins Ergot alkaloids / ergopeptine alkaloids – ergotamine Fumonisins – Crop corn can be easily contaminated by the fungi Fusarium moniliforme , and its fumonisin B1 will cause leukoencephalomalacia (LEM) in horses, pulmonary edema syndrome (PES) in pigs, liver cancer in rats and esophageal cancer in humans. [28] [29] For human and animal health, both the FDA and the EC have regulated the content levels of toxins in food and animal feed. [30] [31] Fusaric acid Fusarochromanone Kojic acid Lolitrem alkaloids Moniliformin 3-Nitropropionic acid Nivalenol Ochratoxins – In Australia, The Limit of Reporting (LOR) level for ochratoxin A (OTA) analyses in 20th Australian Total Diet Survey was 1 µg/kg, [32] whereas the EC restricts the content of OTA to 5 µg/kg in cereal commodities, 3 µg/kg in processed products and 10 µg/kg in dried vine fruits. [33] Oosporeine Patulin – Currently, this toxin has been advisably regulated on fruit products. ... The Sunday Times . ^ "BBC News - Health - Sheriff criticises E. coli butcher" . ^ Cowden JM, Ahmed S, Donaghy M, Riley A (June 2001).
-
Primary Effusion Lymphoma
Wikipedia
New treatment strategies, including those directed at its underlying predisposing diseases, may improve the prognosis of PEL. [9] Contents 1 History 2 Pathophysiology 3 Presentation 4 Diagnosis 5 KSHV/HHV8-negative primary effusion lymphoma 6 Treatment and prognosis 7 See also 8 References 9 External links History [ edit ] PEL was first described in 1989 as a malignant B cell-derived non-Hodgkin lymphoma that developed in three individuals afflicted with HIV/AIDS. [10] In 1995, a group of researchers found DNA sequences that identified KSHV/HHV8 sequences in 8 lymphomas in the malignant cells of patients infected with the HIV; all 8 patients had effusions containing malignant cells in their pleural, pericardial, or peritoneal spaces and had malignant cells in their effusions that evidenced the Epstein-Barr viral genome. [11] Nadir and colleagues termed this syndrome of findings pulmonary effusion lymphoma in 1996. [12] During the years following these initial reports, several cases of PEL were found to be KSHV/HHV8-negative, i.e. occurring in individuals with no evidence of being infected with KSHV/HHV8, or to be manifested by solid tumors that were not associated with effusions, i.e. cases of extracavitary PEL. [13] Pathophysiology [ edit ] PEL develops in patients that have predisposing diseases that reduce the immune systems ability to attack precancerous and cancerous cells. ... term=rituximab&cond=Primary+Effusion+Lymphoma&draw=2&rank=1 External links [ edit ] Classification D ICD-O : M9678/3 MeSH : D054685 DiseasesDB : 33904 SNOMED CT : 713516007 External resources Orphanet : 48686 v t e Leukaemias , lymphomas and related disease B cell ( lymphoma , leukemia ) (most CD19 CD20 ) By development/ marker TdT+ ALL ( Precursor B acute lymphoblastic leukemia/lymphoma ) CD5 + naive B cell ( CLL/SLL ) mantle zone ( Mantle cell ) CD22 + Prolymphocytic CD11c+ ( Hairy cell leukemia ) CD79a + germinal center / follicular B cell ( Follicular Burkitt's GCB DLBCL Primary cutaneous follicle center lymphoma ) marginal zone / marginal zone B-cell ( Splenic marginal zone MALT Nodal marginal zone Primary cutaneous marginal zone lymphoma ) RS ( CD15 +, CD30 +) Classic Hodgkin lymphoma ( Nodular sclerosis ) CD20+ ( Nodular lymphocyte predominant Hodgkin lymphoma ) PCDs / PP ( CD38 +/ CD138 +) see immunoproliferative immunoglobulin disorders By infection KSHV ( Primary effusion ) EBV Lymphomatoid granulomatosis Post-transplant lymphoproliferative disorder Classic Hodgkin lymphoma Burkitt's lymphoma HCV Splenic marginal zone lymphoma HIV ( AIDS-related lymphoma ) Helicobacter pylori ( MALT lymphoma ) Cutaneous Diffuse large B-cell lymphoma Intravascular large B-cell lymphoma Primary cutaneous marginal zone lymphoma Primary cutaneous immunocytoma Plasmacytoma Plasmacytosis Primary cutaneous follicle center lymphoma T/NK T cell ( lymphoma , leukemia ) (most CD3 CD4 CD8 ) By development/ marker TdT+ : ALL ( Precursor T acute lymphoblastic leukemia/lymphoma ) prolymphocyte ( Prolymphocytic ) CD30+ ( Anaplastic large-cell lymphoma Lymphomatoid papulosis type A ) Cutaneous MF+variants indolent: Mycosis fungoides Pagetoid reticulosis Granulomatous slack skin aggressive: Sézary disease Adult T-cell leukemia/lymphoma Non-MF CD30 -: Non-mycosis fungoides CD30− cutaneous large T-cell lymphoma Pleomorphic T-cell lymphoma Lymphomatoid papulosis type B CD30 +: CD30+ cutaneous T-cell lymphoma Secondary cutaneous CD30+ large-cell lymphoma Lymphomatoid papulosis type A Other peripheral Hepatosplenic Angioimmunoblastic Enteropathy-associated T-cell lymphoma Peripheral T-cell lymphoma not otherwise specified ( Lennert lymphoma ) Subcutaneous T-cell lymphoma By infection HTLV-1 ( Adult T-cell leukemia/lymphoma ) NK cell / (most CD56 ) Aggressive NK-cell leukemia Blastic NK cell lymphoma T or NK EBV ( Extranodal NK-T-cell lymphoma / Angiocentric lymphoma ) Large granular lymphocytic leukemia Lymphoid+ myeloid Acute biphenotypic leukaemia Lymphocytosis Lymphoproliferative disorders ( X-linked lymphoproliferative disease Autoimmune lymphoproliferative syndrome ) Leukemoid reaction Diffuse infiltrative lymphocytosis syndrome Cutaneous lymphoid hyperplasia Cutaneous lymphoid hyperplasia with bandlike and perivascular patterns with nodular pattern Jessner lymphocytic infiltrate of the skin General Hematological malignancy leukemia Lymphoproliferative disorders Lymphoid leukemiasIL6, MYC, VEGFA, STAT3, IRF4, CTNNB1, HGF, HIF1A, BCL6, IL10, MET, TNFRSF8, TP53, PRKAA1, POU2F2, NFE2L2, PCNA, NTRK1, NOTCH1, PRKAB1, MDM2, MCL1, ICAM1, ADRA2B, ADRA1A, PTGS2, PDLIM7, VKORC1, ACKR3, SPHK2, CRBN, CXCR6, IKZF1, TRIM28, LPAR2, SDC1, CFLAR, USP7, XBP1P1, XBP1, TNF, SSTR4, GPR42, SLC22A2, PRKAA2, EDNRA, BRS3, PRDM1, CDKN2A, FGF2, BCL2, CDKN1B, CDKN3, F10, ATN1, CASP8, MAPK14, BRAF, EBI3, CIB1, LRPPRC, KAT5, TCL1B, ABCG2, GSK3B, BSG, GRAP2, MSC, CALR, SQSTM1, SPHK1, CASP3, IL18R1, TNFRSF10B, FADD, TCL1A, AIMP2, XRCC5, XPO1, AHSA1, CDC42EP1, MALT1, CNTRL, MTCO2P12, INAFM2, MIR711, AIRN, BMS1P20, PWWP3A, SESN2, FAM107B, AKT1, BIRC5, KRT20, WWOX, OPN1SW, OSGIN1, CD274, BBC3, PABPC1, POLDIP2, RNF19A, CORO1C, SMUG1, BRD4, SIRT1, NLRP1, IKZF3, PSIP1, CAT, XK, VDR, CCK, PAX5, DNASE1, NM, NFKB2, NCAM1, EPHA2, COX2, MNDA, EPHA7, EPHB2, LTA4H, LIF, LGALS1, IRF5, IRAK1, IL13, FHIT, IL6ST, IL6R, FKBP4, IL1B, IGF2R, MTOR, HLA-C, FUS, GABPA, PAEP, DHFR, CLIP2, PLXNB1, CCND2, GTF2H4, UCHL1, TYRO3, TRAF6, MS4A1, CD86, THBS1, TGFBR2, PPP1R11, STAT6, CD47, CDK1, SUMO2, SELPLG, CXCL12, CLIP1, PTPRC, MAPK1, PRKCZ, CCR5, CRK, CTSD, POU2AF1, POMC, H3P42
-
Tubb4a-Related Leukodystrophy
Gene_reviews
SOX 10 -associated leukodystrophy/peripheral and central demyelination, Waardenburg syndrome, and Hirschsprung disease (PCWH) (OMIM 609136) is an autosomal dominant disorder caused by heterozygous pathogenic variants in SOX10 . ... Additional manifestations of PCWH include: Involvement of the peripheral nervous system (sensory loss) Waardenburg syndrome (skin and hair pigmentation changes, heterochromia iridis, and hearing loss) and Hirschsprung disease [Inoue et al 2002, Bondurand et al 2007] Free sialic acid storage disorders are autosomal recessive neurodegenerative disorders caused by biallelic pathogenic variants in SLC17A5 that result in defective sialic acid storage and transport.
-
Spinal And Bulbar Muscular Atrophy
Gene_reviews
This is especially true of the androgen insensitivity signs of testicular atrophy and oligospermia/azoospermia with reduced fertility (see Androgen Insensitivity Syndrome). Males with SBMA may not be able to grow a thick beard and may have difficulty conceiving. ... Non-genetic causes for motor neuron disease include structural lesions (e.g., spinal cord arteriovenous malformations), infections (especially poliomyelitis), toxins (chronic lead poisoning), metabolic problems (thyrotoxicosis), and paraneoplastic syndromes. Individuals with SBMA have been misdiagnosed as having chronic inflammatory neuropathy, metabolic myopathy, polymyositis, and myasthenia gravis.AR, TNF, SOD1, ATXN1, IGFALS, PPARG, IGF1, HTT, HSP90AA1, HSPB8, ATXN3, FRAXE, TNFRSF1A, HSPA4, CRP, MIR298, CASP3, ZEB1, URI1, MAP7, SCN3A, SIX1, SPAG9, HAP1, SQSTM1, KAT2B, BECN1, TGFB1, SMN1, TFEB, SEMA3B, VEGFA, SOD2, SRY, UCP2, STAT1, TBP, VDR, BCAR1, TRIP10, PBK, AD12, CD24, LINC01194, CHCHD10, HES5, CERS6, C9orf72, DNAJB1P1, SYTL1, ZKSCAN3, NLRX1, SEMA6A, PRMT6, STOML1, SUCO, MZB1, DCTN4, FAM135B, POT1, NUP62, HSPH1, CELF2, KHDRBS1, PSME3, WDR1, BAG3, ATXN2, ABCA4, RET, HIF1A, GRM2, GRIA2, GPT, GNA12, GH1, GFRA1, GDNF, KAT2A, GAPDH, GABPA, FRAXA, FXN, FBN1, BPTF, ERBB2, EPHB2, DNMT1, DMPK, CREBBP, COX5B, CEBPD, SEPTIN7, AQP1, AKT1, JAG1, GTF2H1, HSF1, RAN, DNAJB2, PRNP, MAPK1, ADCYAP1, PMP22, SERPINE1, OTX2, NRF1, NFE2L2, NEFL, NEFH, MYO5B, MYH8, MMP2, MAPT, SMAD1, LY6E, LDHA, IRF1, INSR, IL6, IL4, IGF1R, DNAJB1, HSPA5, DNAJA1, LINC01672
-
Slc39a14 Deficiency
Gene_reviews
., pigmentary retinopathy, optic atrophy, oculomotor abnormalities, axonal neuropathy, cognitive decline, seizures) Lacks the T 1 -weighted hyperintensity of the globus pallidus on brain MRI due to Mn deposition PLAN PLA2G6 AR MPAN C19orf12 AR BPAN WDR45 XL FAHN FA2H AR Kufor-Rakeb syndrome ATP13A2 AR CoPAN COASY AR Disorders of copper metabolism Wilson disease ATP7B AR Parkinsonism-dystonia Liver disease, psychiatric symptoms, low serum ceruloplasmin & high non-ceruloplasmin-bound serum copper No Mn deposition on brain MRI Inherited forms of dystonia (see Dystonia Overview) DYT1 early-onset isolated dystonia TOR1A AD Early-onset generalized dystonia No features consistent w/Mn deposition on brain MRI Absent hypermanganesemia KMT2B -related early-onset dystonia KMT2B AD MECR -related childhood-onset dystonia and optic atrophy 3 MECR AR Additional optic atrophy No features consistent w/Mn deposition on brain MRI SLC6A3 -related dopamine transporter deficiency syndrome SLC6A3 AR Parkinsonism-dystonia No features consistent w/Mn deposition on brain MRI Tyrosine hydroxylase-deficient dopa-responsive dystonia TH AR GTP cyclohydrolase 1-deficient dopa-responsive dystonia GCH1 AD Sepiapterin reductase deficiency dopa-responsive dystonia SPR AR Inherited Forms of Parkinson Disease (see Parkinson Disease Overview) Inherited neurodegenerative/metabolic disorders (see Dystonia Overview, Table 4 for hereditary neurodegenerative or metabolic disorders characterized by complex dystonia) Complex dystonia No features consistent w/Mn deposition on brain MRI AD = autosomal dominant; AR = autosomal recessive; BPAN = beta-propeller protein-associated neurodegeneration; CoPAN = COASY protein-associated neurodegeneration; FAHN = fatty acid hydroxylase-associated neurodegeneration.
-
Cardiomyopathy, Familial Hypertrophic, 4
Omim
Kimura et al. (1997) noted that although a locus for 'CMH with WPW' had been mapped to chromosome 7q3 (CMH6; 600858), their findings indicated that more than 1 form of CMH is associated with WPW syndrome. Wang et al. (2013) studied a consanguineous Chinese family in which the 21-year-old proband was referred for cardiac evaluation after the sudden cardiac death of his 23-year-old brother, who had been diagnosed with CMH but was not offered an implantable cardioverter-defibrillator due to the lack of clinical symptoms. ... Kullmann et al. (1993) reported the case of a patient with Holt-Oram syndrome (142900) who had atrial septal defect and developed hypertrophic cardiomyopathy during the first year of life.
-
Tonic-Clonic (Grand Mal) Seizure
Mayo_clinic
Congenital or developmental factors Blood vessels that don't form properly in the brain. Genetic syndromes. Brain tumors. Metabolic issues Very low blood levels of glucose, sodium, calcium or magnesium. Withdrawal syndromes Using or withdrawing from drugs, including alcohol.
-
Epilepsy, Familial Focal, With Variable Foci 1
Omim
Clinical Features Xiong et al. (1999) identified 2 large French Canadian families segregating a familial partial epilepsy syndrome with variable foci characterized by mostly nocturnal seizures arising from frontal, temporal, and occasionally occipital epileptic foci. There was no evidence for structural brain damage or permanent neurologic dysfunction. The syndrome was inherited as an autosomal dominant trait with incomplete penetrance.
-
Leukodystrophy, Demyelinating, Adult-Onset, Autosomal Dominant
Omim
After the fourth episode, progressive neurologic deterioration was observed, including cerebellar ataxia, spastic quadriparesis, and pseudobulbar syndrome. MRI showed progressive cortical and subcortical diffuse white matter abnormalities suggesting cavitating white matter degeneration. ... INHERITANCE - Autosomal dominant HEAD & NECK Eyes - Nystagmus CARDIOVASCULAR Vascular - Orthostatic hypotension due to autonomic dysfunction ABDOMEN Gastrointestinal - Abnormal bowel regulation due to autonomic dysfunction GENITOURINARY External Genitalia (Male) - Impotence due to autonomic dysfunction Bladder - Abnormal bladder regulation due to autonomic dysfunction SKIN, NAILS, & HAIR Skin - Decreased sweating due to autonomic dysfunction NEUROLOGIC Central Nervous System - Cerebellar signs - Cerebellar ataxia - Loss of fine motor skills - Pyramidal signs - Spasticity - Hyperreflexia - Extensor plantar responses - Pseudobulbar syndrome - Autonomic dysfunction - Cognitive impairment (in some patients) - Leukodystrophy, demyelinating - Leukoencephalopathy, diffuse - Demyelination, symmetric - Decreased white matter density - Cavitating white matter degeneration - Atrophy of the corpus callosum - Hypotrophic brainstem - White matter lesions in the brainstem may occur - Neuropathologic findings include leukoencephalopathy, predominantly in the upper corticospinal tract and cerebellar peduncles (initially) - Leukoencephalopathy in the frontal and parietal lobes (later) - Atrophic spinal cord - Oligodendrocytes with foamy cytoplasm - Decreased numbers of astrocytes - Astrocytes show reactive changes - Lack of inflammatory infiltrate - Preservation of U fibers - Sparing of optic tracts Behavioral Psychiatric Manifestations - Personality changes - Depression LABORATORY ABNORMALITIES - Patient cells have increased levels of LMNB1 mRNA and protein MISCELLANEOUS - Onset in the fourth to sixth decades (mean 40 years) - Autonomic dysfunction usually precedes obvious neurologic deterioration - Progressive disorder - Acute neurologic deterioration after viral illness has been reported - Duplication of LMNB1 is sufficient for the disorder, although patients may also have larger duplications - One family with a deletion upstream of the LMNB1 gene did not have autonomic symptoms or cerebellar involvement MOLECULAR BASIS - Caused by duplication of 72 kb of 5q23.2 including at a minimum the lamin B1 gene (LMNB1, 150340.0001 ) ▲ Close
-
Depersonalization
Wikipedia
It is an effect of dissociatives and psychedelics , as well as a possible side effect of caffeine , alcohol , amphetamine , and cannabis . [20] [21] [22] [23] [24] It is a classic withdrawal symptom from many drugs. [25] [26] [27] [28] Benzodiazepine dependence , which can occur with long-term use of benzodiazepines, can induce chronic depersonalization symptomatology and perceptual disturbances in some people, even in those who are taking a stable daily dosage, and it can also become a protracted feature of the benzodiazepine withdrawal syndrome . [29] [30] Lieutenant Colonel Dave Grossman , in his book On Killing , suggests that military training artificially creates depersonalization in soldiers, suppressing empathy and making it easier for them to kill other human beings. [31] Graham Reed (1974) claimed that depersonalization occurs in relation to the experience of falling in love. [32] Depersonalization as a psychobiological mechanism [ edit ] Depersonalization is a classic response to acute trauma , and may be highly prevalent in individuals involved in different traumatic situations including motor vehicle accident , and imprisonment . [3] Psychologically depersonalization can, just like dissociation in general, be considered a type of coping mechanism. ... PMID 9696914 . ^ Ashton, Heather (1991). "Protracted withdrawal syndromes from benzodiazepines". Journal of Substance Abuse Treatment . 8 (1–2): 19–28. doi : 10.1016/0740-5472(91)90023-4 .
-
Discoid Lupus Erythematosus
Wikipedia
External links [ edit ] Classification D ICD - 10 : L93.0 ( ILDS L93.020) ICD - 9-CM : 695.4 MeSH : D008179 DiseasesDB : 29595 External resources Orphanet : 90281 Wikimedia Commons has media related to Discoid lupus erythematosus . v t e Cutaneous keratosis, ulcer, atrophy, and necrobiosis Epidermal thickening keratoderma : Keratoderma climactericum Paraneoplastic keratoderma Acrokeratosis paraneoplastica of Bazex Aquagenic keratoderma Drug-induced keratoderma psoriasis Keratoderma blennorrhagicum keratosis : Seborrheic keratosis Clonal seborrheic keratosis Common seborrheic keratosis Irritated seborrheic keratosis Seborrheic keratosis with squamous atypia Reticulated seborrheic keratosis Dermatosis papulosa nigra Keratosis punctata of the palmar creases other hyperkeratosis : Acanthosis nigricans Confluent and reticulated papillomatosis Callus Ichthyosis acquisita Arsenical keratosis Chronic scar keratosis Hyperkeratosis lenticularis perstans Hydrocarbon keratosis Hyperkeratosis of the nipple and areola Inverted follicular keratosis Lichenoid keratosis Multiple minute digitate hyperkeratosis PUVA keratosis Reactional keratosis Stucco keratosis Thermal keratosis Viral keratosis Warty dyskeratoma Waxy keratosis of childhood other hypertrophy: Keloid Hypertrophic scar Cutis verticis gyrata Necrobiosis / granuloma Necrobiotic/palisading Granuloma annulare Perforating Generalized Subcutaneous Granuloma annulare in HIV disease Localized granuloma annulare Patch-type granuloma annulare Necrobiosis lipoidica Annular elastolytic giant-cell granuloma Granuloma multiforme Necrobiotic xanthogranuloma Palisaded neutrophilic and granulomatous dermatitis Rheumatoid nodulosis Interstitial granulomatous dermatitis / Interstitial granulomatous drug reaction Foreign body granuloma Beryllium granuloma Mercury granuloma Silica granuloma Silicone granuloma Zirconium granuloma Soot tattoo Tattoo Carbon stain Other/ungrouped eosinophilic dermatosis Granuloma faciale Dermis / localized CTD Cutaneous lupus erythematosus chronic: Discoid Panniculitis subacute : Neonatal ungrouped: Chilblain Lupus erythematosus–lichen planus overlap syndrome Tumid Verrucous Rowell's syndrome Scleroderma / Morphea Localized scleroderma Localized morphea Morphea–lichen sclerosus et atrophicus overlap Generalized morphea Atrophoderma of Pasini and Pierini Pansclerotic morphea Morphea profunda Linear scleroderma Atrophic / atrophoderma Lichen sclerosus Anetoderma Schweninger–Buzzi anetoderma Jadassohn–Pellizzari anetoderma Atrophoderma of Pasini and Pierini Acrodermatitis chronica atrophicans Semicircular lipoatrophy Follicular atrophoderma Linear atrophoderma of Moulin Perforating Kyrle disease Reactive perforating collagenosis Elastosis perforans serpiginosa Perforating folliculitis Acquired perforating dermatosis Skin ulcer Pyoderma gangrenosum Other Calcinosis cutis Sclerodactyly Poikiloderma vasculare atrophicans Ainhum / Pseudo-ainhumCYBB, CR2, C2, C5, TSPYL2, SPP1, C1QA, STAT4, IRAK1, NCF2, IL10, IL6, IL2, C1R, TLR9, IL21, TNF, IFNA1, CD40LG, FCGR2B, TRIM21, DNMT1, CYBA, IL17A, IFNA13, IRF5, TLR7, NCF1, CD70, TNFSF13B, TLR5, IL1B, MTOR, ITGAM, TREX1, RO60, ESR1, BTK, IFNG, FLI1, MAPK1, IL22, TRBV20OR9-2, CTLA4, HLA-DRB1, CD28, TP53BP1, BLK, ITGAL, RAB4A, IFIH1, FCGR3A, CCL2, FOXP3, MBL2, EZH2, RNPC3, EPHB2, ICOS, PRL, ACE, CRP, TLR4, PBX1, STAT1, MECP2, AIM2, PTPN22, IL4, FCGR3B, IL2RA, KIR3DL2, C3, CD44, TGFB1, ITGB2, F11R, BTG3, DECR1, BANK1, IFN1@, IRF7, HDAC6, IFI16, HRES1, ISG20, MYDGF, IGHG3, CXCL12, FLII, RFX1, MAVS, F5, IL18, KIR3DL1, FCGR2A, CBLIF, GEM, CXCL10, F3, CASP1, STAT3, MIR31, CALR, CAMK4, CREM, BCR, MIR21, VEGFA, APOH, MIR146A, TNFRSF17, TLR8, AR, FASLG, CXADRP1, ARR3, BCL2, CXCR5, IL17D, PRDM1, TRIM13, KIR2DS1, IL1A, TREM1, IFNAR1, MIR155, CASR, TLR2, MIR148A, IRAK4, MIR663A, ANXA6, SLEB4, P2RX7, PDCD1, NOS3, CXCR4, SIRT1, ACTB, MYD88, MTHFR, PPARD, PADI4, PTPA, ADAM10, MMP9, PRKAR1A, CXCL13, CD274, VCAM1, PRKCB, SH2D1A, LGALS9, LGALS3, LEP, IL21R, TNFSF4, TRPM2, MIR125A, CXADR, NR1I3, CD40, XRCC6, CD69, CD72, APOL1, VSIR, NEAT1, HMGB1, CDR1, SYK, IL27, IL34, SSB, ETS1, EMB, SRCIN1, FAM167A, RBM45, UBASH3B, SLAMF1, EGFR, MBD2, TNFSF13, SLAMF6, CTNNB1, SPG7, GATA3, KRT20, CXCR3, IGAN1, REN, RPS19, CD38, CD19, TGFB3, STING1, MS4A1, HDAC9, AHSA1, FCGR2C, IER3, SPATA2, SH2B2, ATG12, DCTN6, EIF2AK3, TNFSF12, TNFSF9, AIMP2, TNFSF15, C1QL1, HNRNPDL, LILRB4, MBTPS1, LILRA3, H4C5, CORO1A, PADI2, H4C13, PSME3, PROCR, XPR1, DGAT1, H4C11, H4C12, TRIM38, NR0B2, MAEA, H4C6, ZNRD2, H4C3, OASL, H4C8, ATG5, H4C2, H4C1, MACROH2A1, BECN1, GRAP2, CD163, H4C14, ANP32B, H4C9, KLK4, TAM, TNIP1, H4C4, NAT2, SYNPO, DNER, VGLL3, GSTK1, TICAM2, H3C15, RSPO1, IFNL3, SGMS1, TIGIT, CENPV, BTLA, IL23R, DOCK11, SLCO6A1, H3C14, H4-16, CTHRC1, TNFRSF13C, CGAS, NLRP3, IL17F, PRRT2, LBX1-AS1, MIR142, MIR145, MIR633, LOC102723971, ERVW-4, ERVK-20, KLRC4-KLRK1, RPL17-C18orf32, TMED7-TICAM2, H3C9P, SIGLEC14, CCR2, H3C13, MIR150, MIR485, H4C15, WG, TNFSF12-TNFSF13, MIR17HG, MIR29B2, MIR29B1, MIR23B, MIR224, ORMDL3, IL33, KLRK1, ELOF1, CD244, IL23A, NT5C3A, TMED7, DUOX2, CD209, ERVW-1, TBX21, PDCD4, PHGDH, POLDIP2, RNF19A, CABIN1, TNFRSF13B, BRD4, NBEAL2, KDM6B, ZNF423, DKK1, ATF6, PLA2R1, DUOX1, RIPK4, VIP, HIVEP3, LBH, CD276, VTCN1, WNK1, IL25, GORASP1, ERVK-6, BACH2, RFH1, HAMP, LARP6, PHRF1, MRTFA, SCYL1, SLC12A9, BDH2, SPHK2, IFNK, APOM, CHST12, VWF, PTPRC, VIM, DUSP4, F10, F2, ERN1, ERBB2, EPO, EPHX2, ELF1, EIF4EBP1, EGR2, EFNA2, TSC22D3, FCER1G, ATN1, ARID3A, DNMT3B, DNMT3A, DNASE1, DLAT, CX3CR1, CTBP2, CSF3R, CSF1, F12, FCN2, EZR, HIF1A, IFNAR2, IFI27, HSPG2, HSPA5, HSPA4, HNRNPC, HMGN2, HLA-H, HLA-DQA1, HLA-C, HGF, FOXC1, CFHR1, CFH, H1-0, GSTP1, GRIN2A, GRN, GPER1, GPI, GFI1, IFI6, MAPK14, CRK, CRH, KLK3, CAMP, C4B, C1QC, TSPO, BST2, BGN, ATF3, SERPINC1, ABCC6, FAS, APOE, CREBBP, ANXA2, AMELX, ABCD1, ALB, AKT1, AGER, PARP1, ADD2, ACP5, ACR, CAST, CASP6, CASP8, CASP9, COX8A, CCR5, CHRM3, AKR1C4, CD52, CDKN1A, CDH13, CDK1, CD48, ENTPD1, CD36, CD80, CD8B, CD247, CD3G, CD2, CD1D, CD1A, CBL, RUNX1T1, CAT, IFNB1, IFNR, IL1RN, RPL17, SH3BP2, SRSF1, SELP, SDC2, CX3CL1, CCL14, CCL3L1, SERPINB3, S100B, RPS6, TRIM27, PRKCD, RELB, RELA, PTX3, ABCA1, PTPN11, PTPN6, PTGS2, PTGS1, PSMD9, MASP1, SLC4A1, SIGLEC1, SNCA, SNRNP70, VDR, UMOD, TYK2, TRPC6, TRAF6, TRAF2, HSP90B1, TPO, TP53, TNFRSF1B, TNFAIP3, TIMP3, THAS, TG, ZEB1, ADAM17, SYT1, SUV39H1, SRI, SNRPB, SNRPA, MAP2K1, PRKCA, IL7R, LCT, MMP11, MMP2, AFF1, CIITA, MFGE8, CD46, MCL1, CD180, LY6E, LDLR, LCN2, SRGN, LBR, LAG3, KIR2DL4, KIF5A, ITGAX, ITGAE, IRF6, TNFRSF9, IL16, IL15, MNAT1, MPL, MPO, MRC1, PPARG, PON1, SERPINA1, PGK1, PF4, PECAM1, PDE7A, PCNA, PC, PAK3, OCA2, NT5E, PNP, NOTCH1, NHS, NFKB1, NF1, NEDD9, NCL, COX1, MSH5, H3P23
-
Lymphangiomatosis
Wikipedia
"Thoracic Lymphangiomas, Lymphangiectasis, Lymphangiomatosis, and Lymphatic Dysplasia Syndrome". Am. J. Respir. Crit. Care Med . 161 (3): 1037–1046. doi : 10.1164/ajrccm.161.3.9904056 . ... CS1 maint: multiple names: authors list ( link ) External Resources [ edit ] Lymphangiomatosis & Gorham's Disease Alliance (LGDA) is a 501(c)(3) organization incorporated in the United States and serving patients and families around the world: www.lgdalliance.org International LGDA Registry for Lymphatic Malformations is a patient outreach and research development project of the LGDA: www.lgdaregistry.org v t e Tumours of blood vessels Blood vessel Hemangiosarcoma Blue rubber bleb nevus syndrome Hemangioendothelioma Composite Endovascular papillary Epithelioid Kaposiform Infantile Retiform ) Spindle cell Proliferating angioendotheliomatosis Hemangiopericytoma Venous lake Kaposi's sarcoma African cutaneous African lymphadenopathic AIDS-associated Classic Immunosuppression-associated Hemangioblastoma Hemangioma Capillary Cavernous Glomeruloid Microvenular Targeted hemosiderotic Angioma Cherry Seriginosum Spider Tufted Universal angiomatosis Angiokeratoma of Mibelli Angiolipoma Pyogenic granuloma Lymphatic Lymphangioma / lymphangiosarcoma Lymphangioma circumscriptum Acquired progressive lymphangioma PEComa Lymphangioleiomyomatosis Cystic hygroma Multifocal lymphangioendotheliomatosis Lymphangiomatosis Either Angioma / angiosarcoma Angiofibroma
-
Religious Delusion
Wikipedia
In 2011, a team of psychiatrists , behavioral psychologists , neurologists and neuropsychiatrists from the Harvard Medical School published a research which suggested the development of a new diagnostic category of psychiatric disorders related to religious delusion and hyperreligiosity . [25] They compared the thought and behavior of the most important figures in the Bible ( Abraham , Moses , Jesus Christ and Paul ) [25] with patients affected by mental disorders related to the psychotic spectrum using different clusters of disorders and diagnostic criteria ( DSM-IV-TR ), [25] and concluded that these Biblical figures "may have had psychotic symptoms that contributed inspiration for their revelations", [25] such as schizophrenia , schizoaffective disorder , manic depression , delusional disorder , delusions of grandeur , auditory - visual hallucinations , paranoia , Geschwind syndrome (Paul especially) and abnormal experiences associated with temporal lobe epilepsy (TLE). [25] In 1998–2000 Pole Leszek Nowak (born 1962) [26] from Poznań authored a study in which, based on his own history of religious delusions of mission and overvalued ideas, and information communicated in the Gospels, made an attempt at reconstructing Jesus′ psyche [27] with the view of Jesus as apocalyptic prophet . [28] He does so in chapters containing, in sequence, an analysis of character traits of the ″savior of mankind″, a description of the possible course of events from the period of Jesus' public activity, a naturalistic explanation of miracles. ... These auditory experiences are classified by psychiatry as command hallucination . [34] Persons acting to commit murder are reported as hearing voices of religious beings such as God , [35] [36] [37] [38] [39] [40] [41] [42] angels , [43] or the Devil . [44] Professor Thomas Szasz critiques the concept of religious auditory hallucination: those who hear the voice of God talking to them are experiencing schizophrenia, while those who talk to God but hear no response are simply praying . [45] See also [ edit ] Jerusalem syndrome Messiah complex Religion and schizophrenia The God Delusion Creationism References [ edit ] ^ a b c Freud, Sigmund (1939).
-
Abortion In West Virginia
Wikipedia
The law required the licensed medical professionals, the only ones allowed to perform abortions, read a counselling script to women seeking an abortion. [16] Some states, such as Alaska, Mississippi, West Virginia, Texas, and Kansas, have passed laws requiring abortion providers to warn patients of a link between abortion and breast cancer, and to issue other scientifically unsupported warnings. [17] [18] The state was one of 23 states in 2007 to have a detailed abortion-specific informed consent requirement. [19] The informed consent materials in South Dakota, Texas, Utah and West Virginia given to women seeking abortions include counseling materials that say women who have abortions may have suicidal thoughts or they may experience "postabortion traumatic stress syndrome." The latter syndrome is not recognized by American Psychological Association or the American Psychiatric Association. [20] In March 2015, after overriding a veto from the Governor, the West Virginia legislature passed a bill banning abortion after week 20. [21] [22] In 2017, the West Virginia legislature passed a law trying to make it more difficult for minors to get an abortion.
-
Illusory Palinopsia
Wikipedia
Multiple types of illusory palinopsia often co-exist in a patient and occur with other diffuse, persistent illusory symptoms such as halos around objects , dysmetropsia ( micropsia , macropsia , pelopsia , or teleopsia ), Alice in Wonderland Syndrome , visual snow , and oscillopsia . ... "Reversible palinopsia and the Alice in Wonderland syndrome associated with topiramate use in migraineurs".
-
Patellar Dislocation
Wikipedia
In some cases, the injured ligaments involved in patellar dislocation do not allow the leg to flex almost at all. [2] Risk factors [ edit ] A predisposing factor is tightness in the tensor fasciae latae muscle and iliotibial tract in combination with a quadriceps imbalance between the vastus lateralis and vastus medialis muscles can play a large role, found, mainly, in women with higher level the physical activity. [7] Moreover, women with patellofemoral pain may show increased Q-angle compared with women without patellofemoral pain. [ citation needed ] Another cause of patellar symptoms is lateral patellar compression syndrome , which can be caused from lack of balance or inflammation in the joints. [8] The pathophysiology of the kneecap is complex, and deals with the osseous soft tissue or abnormalities within the patellofemoral groove. ... Doctors generally only recommend surgery when other structures in the knee have sustained severe damage, or specifically when there is: [20] Concurrent osteochondral injury Continued gross instability Palpable disruption of the medial patellofemoral ligament and the vastus medialis obliquus High-level athletic demands coupled with mechanical risk factors and an initial injury mechanism not related to contact Supplements like glucosamine and NSAIDs can be used to minimize bothersome symptoms. [14] Rehabilitation [ edit ] An effective rehabilitation program reduces the chances of re-injury and of other knee-related problems such as patellofemoral pain syndrome and osteoarthritis . Most patella dislocations are initially immobilized for the first 2–3 weeks to allow the stretched structures to heal.