-
Silent Sinus Syndrome
Wikipedia
Silent sinus syndrome Other names Imploding antrum syndrome Specialty ENT surgery Silent sinus syndrome is a spontaneous, asymptomatic collapse of the maxillary sinus and orbital floor associated with negative sinus pressures. ... References [ edit ] Illner A, Davidson HC, Harnsberger HR, Hoffman J (2002). "The silent sinus syndrome: clinical and radiographic findings". ... Full text Numa WA, Desai U, Gold DR, Heher KL, Annino DJ (2005). "Silent sinus syndrome: a case presentation and comprehensive review of all 84 reported cases". ... "Queen Meresankh III – the oldest case of bilateral Silent Sinus Syndrome (c. 2620/10 - 2570 BC)?". Anthropologie . 56 (2): 103–113. doi : 10.26720/anthro.17.09.25.2 .
-
Uv-Sensitive Syndrome
Wikipedia
UV-sensitive syndrome Other names UVSS This condition is inherited in an autosomal recessive manner. Specialty Dermatology UV-sensitive syndrome is a cutaneous condition inherited in an autosomal recessive fashion, characterized by photosensitivity and solar lentigines . [1] Recent research identified that mutations of the KIAA1530 (UVSSA) gene as cause for the development of UV-sensitive syndrome. [2] Furthermore, this protein was identified as a new player in the Transcription-coupled repair (TC-NER). [2] Contents 1 See also 2 References 3 Further reading 4 External links See also [ edit ] Solar urticaria List of cutaneous conditions Cockayne syndrome Xeroderma pigmentosum Nucleotide excision repair References [ edit ] ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). ... ISBN 978-1-4160-2999-1 . ^ a b Schwertman P., Marteijn JA.; Lagarou A; Dekkers DH; Raams A; van der Hoek AC; Laffeber C; Hoeijmakers JH; Demmers JA; Fousteri M; Vermeulen W (May 2012). "UV-sensitive syndrome protein UVSSA recruits USP7 to regulate transcription-coupled repair". ... Further reading [ edit ] "UV sensitive syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program" . rarediseases.info.nih.gov .
-
Treacher Collins Syndrome 3
Omim
A number sign (#) is used with this entry because Treacher Collins syndrome-3 (TCS3) is caused by compound heterozygous mutation in the POLR1C gene (610060) on chromosome 6p21. Description Treacher Collins syndrome is a disorder of craniofacial development characterized by a combination of bilateral downward slanting of the palpebral fissures, colobomas of the lower eyelids with a paucity of eyelashes medial to the defect, hypoplasia of the facial bones, cleft palate, malformation of the external ears, atresia of the external auditory canals, and bilateral conductive hearing loss (Dauwerse et al., 2011). For additional phenotypic information and a discussion of genetic heterogeneity of Treacher Collins syndrome, see TCS1 (154500). Clinical Features Richieri-Costa et al. (1993) and Splendore et al. (2000) both reported sibs with Treacher Collins syndrome who were born to normal parents. The possibility of either nonpenetrance or germline mosaicism in one of the parents could not be discarded. Inheritance Treacher Collins syndrome-3 is an autosomal recessive disorder (Dauwerse et al., 2011). Molecular Genetics Dauwerse et al. (2011) analyzed the POLR1C gene in 252 individuals with Treacher Collins syndrome and identified 3 patients, including 1 from a family previously studied by Splendore et al. (2000), with compound heterozygous mutations (610060.0001-610060.0005, respectively).
-
Chromosome Abnormality
Wikipedia
Known disorders in humans include Wolf-Hirschhorn syndrome , which is caused by partial deletion of the short arm of chromosome 4; and Jacobsen syndrome , also called the terminal 11q deletion disorder. ... Isochromosome : Formed by the mirror image copy of a chromosome segment including the centromere. Chromosome instability syndromes are a group of disorders characterized by chromosomal instability and breakage. ... "Molecular genetic analysis of Down syndrome" . Human Genetics . 126 (1): 195–214. doi : 10.1007/s00439-009-0696-8 . ISSN 1432-1203 . ^ "Turner Syndrome" . National Institute of Child Health and Human Development . ... External links [ edit ] Chromosome+disorders at the US National Library of Medicine Medical Subject Headings (MeSH) v t e Chromosome abnormalities Autosomal Trisomies /Tetrasomies Down syndrome 21 Edwards syndrome 18 Patau syndrome 13 Trisomy 9 Tetrasomy 9p Warkany syndrome 2 8 Cat eye syndrome / Trisomy 22 22 Trisomy 16 Monosomies / deletions ( 1q21.1 copy number variations / 1q21.1 deletion syndrome / 1q21.1 duplication syndrome / TAR syndrome / 1p36 deletion syndrome ) 1 Wolf–Hirschhorn syndrome 4 Cri du chat syndrome / Chromosome 5q deletion syndrome 5 Williams syndrome 7 Jacobsen syndrome 11 Miller–Dieker syndrome / Smith–Magenis syndrome 17 DiGeorge syndrome 22 22q11.2 distal deletion syndrome 22 22q13 deletion syndrome 22 genomic imprinting Angelman syndrome / Prader–Willi syndrome ( 15 ) Distal 18q- / Proximal 18q- X / Y linked Monosomy Turner syndrome (45,X) Trisomy / tetrasomy , other karyotypes / mosaics Klinefelter syndrome (47,XXY) XXYY syndrome (48,XXYY) XXXY syndrome (48,XXXY) 49,XXXYY 49,XXXXY Triple X syndrome (47,XXX) Tetrasomy X (48,XXXX) 49,XXXXX Jacobs syndrome (47,XYY) 48,XYYY 49,XYYYY 45,X/46,XY 46,XX/46,XY Translocations Leukemia / lymphoma Lymphoid Burkitt's lymphoma t(8 MYC ;14 IGH ) Follicular lymphoma t(14 IGH ;18 BCL2 ) Mantle cell lymphoma / Multiple myeloma t(11 CCND1 :14 IGH ) Anaplastic large-cell lymphoma t(2 ALK ;5 NPM1 ) Acute lymphoblastic leukemia Myeloid Philadelphia chromosome t(9 ABL ; 22 BCR ) Acute myeloblastic leukemia with maturation t(8 RUNX1T1 ;21 RUNX1 ) Acute promyelocytic leukemia t(15 PML ,17 RARA ) Acute megakaryoblastic leukemia t(1 RBM15 ;22 MKL1 ) Other Ewing's sarcoma t(11 FLI1 ; 22 EWS ) Synovial sarcoma t(x SYT ;18 SSX ) Dermatofibrosarcoma protuberans t(17 COL1A1 ;22 PDGFB ) Myxoid liposarcoma t(12 DDIT3 ; 16 FUS ) Desmoplastic small-round-cell tumor t(11 WT1 ; 22 EWS ) Alveolar rhabdomyosarcoma t(2 PAX3 ; 13 FOXO1 ) t (1 PAX7 ; 13 FOXO1 ) Other Fragile X syndrome Uniparental disomy XX male syndrome / 46,XX testicular disorders of sex development Marker chromosome Ring chromosome 6 ; 9 ; 14 ; 15 ; 18 ; 20 ; 21 , 22 v t e Mutation Mechanisms of mutation Insertion Deletion Substitution Transversion Transition Mutation with respect to structure Point mutation Nonsense mutation Missense mutation Conservative mutation Silent mutation Frameshift mutation Dynamic mutation Large-scale mutation Chromosomal translocations Chromosomal inversions Mutation with respect to overall fitness Deleterious mutation Advantageous mutation Neutral mutation Nearly neutral mutation Synonymous mutation Nonsynonymous mutation Authority control GND : 4010163-0 LCCN : sh85025385 NDL : 00570781
-
Clinical Vampirism
Wikipedia
The talk page may contain suggestions. ( March 2016 ) ( Learn how and when to remove this template message ) Vampirism Other names Renfield's syndrome, Renfield syndrome Specialty Psychiatry Clinical vampirism , more commonly known as Renfield's syndrome or Renfield syndrome , is an obsession with drinking blood . ... Origin of Renfield's syndrome [ edit ] The syndrome is named after R. ... Retrieved 10 October 2013 . ^ Noll, Richard (October 2013). "Renfield's Syndrome, or, How I (unintentionally) created a monster" . ... Retrieved 12 July 2012 . ^ "The Renfield Syndrome (2010)" . Archived from the original on 6 April 2012 . ... Waterville, Maine: Five Star. ^ Saare, J.A. "The Renfield Syndrome" . Archived from the original on 12 July 2012 .
-
Keratosis Pilaris
Wikipedia
., atopic dermatitis ), and rarely cancer . [1] Many rarer types of the disorder are part of inherited genetic syndromes. [1] The cause of KP is not completely understood. ... KP subtypes are occasionally part of genetically inherited syndromes associated with intellectual disability , neuro-cardio-facial-cutaneous syndromes , RASopathies , ectodermal dysplasias , and certain myopathies . [1] Diagnosis [ edit ] Physicians can often diagnose KP simply by examining the skin without specialized tests. [4] However, a dermatologist can use dermoscopy to confirm the diagnosis and assess if a person with KP is responding to treatment. [2] Physicians will often consider family history and the presence of symptoms when making the diagnosis. [9] Those with this condition are generally encouraged to contact a physician if the bumps are bothersome and do not improve with over-the-counter lotions. [4] Differential diagnosis [ edit ] Several medications can cause a skin eruption similar to KP. ... Classification D ICD - 9-CM : 757.39 OMIM : 604093 MeSH : C537412 DiseasesDB : 32387 External resources MedlinePlus : 001462 eMedicine : ped/1246 derm/211 The American Academy of Dermatology The American Osteopathic College of Dermatology - Article on keratosis pilaris v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Congenital malformations and deformations of integument / skin disease Genodermatosis Congenital ichthyosis / erythrokeratodermia AD Ichthyosis vulgaris AR Congenital ichthyosiform erythroderma : Epidermolytic hyperkeratosis Lamellar ichthyosis Harlequin-type ichthyosis Netherton syndrome Zunich–Kaye syndrome Sjögren–Larsson syndrome XR X-linked ichthyosis Ungrouped Ichthyosis bullosa of Siemens Ichthyosis follicularis Ichthyosis prematurity syndrome Ichthyosis–sclerosing cholangitis syndrome Nonbullous congenital ichthyosiform erythroderma Ichthyosis linearis circumflexa Ichthyosis hystrix EB and related EBS EBS-K EBS-WC EBS-DM EBS-OG EBS-MD EBS-MP JEB JEB-H Mitis Generalized atrophic JEB-PA DEB DDEB RDEB related: Costello syndrome Kindler syndrome Laryngoonychocutaneous syndrome Skin fragility syndrome Ectodermal dysplasia Naegeli syndrome / Dermatopathia pigmentosa reticularis Hay–Wells syndrome Hypohidrotic ectodermal dysplasia Focal dermal hypoplasia Ellis–van Creveld syndrome Rapp–Hodgkin syndrome / Hay–Wells syndrome Elastic / Connective Ehlers–Danlos syndromes Cutis laxa ( Gerodermia osteodysplastica ) Popliteal pterygium syndrome Pseudoxanthoma elasticum Van der Woude syndrome Hyperkeratosis / keratinopathy PPK diffuse : Diffuse epidermolytic palmoplantar keratoderma Diffuse nonepidermolytic palmoplantar keratoderma Palmoplantar keratoderma of Sybert Meleda disease syndromic connexin Bart–Pumphrey syndrome Clouston's hidrotic ectodermal dysplasia Vohwinkel syndrome Corneodermatoosseous syndrome plakoglobin Naxos syndrome Scleroatrophic syndrome of Huriez Olmsted syndrome Cathepsin C Papillon–Lefèvre syndrome Haim–Munk syndrome Camisa disease focal : Focal palmoplantar keratoderma with oral mucosal hyperkeratosis Focal palmoplantar and gingival keratosis Howel–Evans syndrome Pachyonychia congenita Pachyonychia congenita type I Pachyonychia congenita type II Striate palmoplantar keratoderma Tyrosinemia type II punctate : Acrokeratoelastoidosis of Costa Focal acral hyperkeratosis Keratosis punctata palmaris et plantaris Keratosis punctata of the palmar creases Schöpf–Schulz–Passarge syndrome Porokeratosis plantaris discreta Spiny keratoderma ungrouped: Palmoplantar keratoderma and spastic paraplegia desmoplakin Carvajal syndrome connexin Erythrokeratodermia variabilis HID / KID Other Meleda disease Keratosis pilaris ATP2A2 Darier's disease Dyskeratosis congenita Lelis syndrome Dyskeratosis congenita Keratolytic winter erythema Keratosis follicularis spinulosa decalvans Keratosis linearis with ichthyosis congenita and sclerosing keratoderma syndrome Keratosis pilaris atrophicans faciei Keratosis pilaris Other cadherin EEM syndrome immune system Hereditary lymphedema Mastocytosis / Urticaria pigmentosa Hailey–Hailey see also Template:Congenital malformations and deformations of skin appendages , Template:Phakomatoses , Template:Pigmentation disorders , Template:DNA replication and repair-deficiency disorder Developmental anomalies Midline Dermoid cyst Encephalocele Nasal glioma PHACE association Sinus pericranii Nevus Capillary hemangioma Port-wine stain Nevus flammeus nuchae Other/ungrouped Aplasia cutis congenita Amniotic band syndrome Branchial cyst Cavernous venous malformation Accessory nail of the fifth toe Bronchogenic cyst Congenital cartilaginous rest of the neck Congenital hypertrophy of the lateral fold of the hallux Congenital lip pit Congenital malformations of the dermatoglyphs Congenital preauricular fistula Congenital smooth muscle hamartoma Cystic lymphatic malformation Median raphe cyst Melanotic neuroectodermal tumor of infancy Mongolian spot Nasolacrimal duct cyst Omphalomesenteric duct cyst Poland anomaly Rapidly involuting congenital hemangioma Rosenthal–Kloepfer syndrome Skin dimple Superficial lymphatic malformation Thyroglossal duct cyst Verrucous vascular malformation Birthmark
-
Organic Brain Syndrome
Wikipedia
A more specific medical term for the acute subset of organic brain syndromes is delirium . [6] Thinking, remembering, sleeping, and paying attention can become difficult during alcohol withdrawal, after surgery, or with dementia. [7] Dementia [ edit ] See also: Dementia Dementia or chronic organic brain syndrome is long-term. ... A; Reich, P; Austen, K. F (1986). "Mixed organic brain syndrome as a manifestation of systemic mastocytosis". ... PMID 3749421 . ^ "Organic brain syndrome" . MedlinePlus. ^ Khan A, Joyce P, Jones AV (August 1980). "Benzodiazepine withdrawal syndromes" . N. Z. Med. J . 92 (665): 94–6. ... PMID 2648495 . ^ "Treatment for Organic Mental Disorders" . ^ a b "Organic brain syndrome: MedlinePlus Medical Encyclopedia" .INS, MMP9, HTR7, GRIN1, MMP3, MAPT, LAMP2, IRAK1, IL4, COMT, GRIN2B, GRIN2A, CYP2D6, DBN1, ITIH4, APOE, ERVK-32, ERVK-6, GLS, MAP3K11, CEBPZ, NPS, CXADRP1, SRRM2, SIRT3, TRIM13, SMOX, KCTD7, ADIPOQ, MMP23A, MMP23B, ZNF142, ZFP36, NR1I3, MTDH, MMP21, MAK16, DCLRE1C, SMUG1, ROBO3, DDX58, TPSG1, AUTS2, TP53, RBMS3, TMEM97, TREM2, ACKR3, PNO1, TYRP1, ACHE, TIMP2, STAT1, APCS, APP, AQP4, ARR3, TSPO, CASR, CD14, CEBPB, CPE, CXADR, EPO, FGF2, HLA-C, HMGB1, HMOX1, IFNG, IGF1, IGF2R, IL17A, NFE2L2, NRGN, ADRB1, PTBP1, PLAAT4, CCL2, CCL5, SLC1A2, SLC6A3, SPG7, PRKAR1A
-
Iridocorneal Endothelial Syndrome
Orphanet
Iridocorneal endothelial (ICE) syndrome describes a group of progressive corneal proliferative endotheliopathies comprised of Chandler’s syndrome, Cogan-Reese syndrome and essential iris atrophy (see these terms), affecting mainly young adult females and characterized by iris holes and atrophy, papillary distortion, anterior synechiae, corneal edema and often with secondary glaucoma and corneal decompensation as complications
-
Palmoplantar Keratoderma
Wikipedia
PMID 14945735 . ^ Gach JE, Munro CS, Lane EB, Wilson NJ, Moss C (November 2005). "Two families with Greither's syndrome caused by a keratin 1 mutation". ... "A gene for an autosomal dominant scleroatrophic syndrome predisposing to skin cancer (Huriez syndrome) maps to chromosome 4q23" . ... "A missense mutation in connexin26, D66H, causes mutilating keratoderma with sensorineural deafness (Vohwinkel's syndrome) in three unrelated families" . ... "Exome sequencing reveals mutations in TRPV3 as a cause of Olmsted syndrome" . American Journal of Human Genetics . 90 (3): 558–64. doi : 10.1016/j.ajhg.2012.02.006 . ... PMID 26515860 . ^ Online Mendelian Inheritance in Man (OMIM): 144200 ^ Online Mendelian Inheritance in Man (OMIM): 600962 External links [ edit ] Classification D ICD - 10 : L85.1 - L85.2 , Q82.8 ICD - 9-CM : 701.1 , 757.39 OMIM : 144200 600962 MeSH : D007645 DiseasesDB : 32042 SNOMED CT : 706885006 External resources eMedicine : derm/589 v t e Cutaneous keratosis, ulcer, atrophy, and necrobiosis Epidermal thickening keratoderma : Keratoderma climactericum Paraneoplastic keratoderma Acrokeratosis paraneoplastica of Bazex Aquagenic keratoderma Drug-induced keratoderma psoriasis Keratoderma blennorrhagicum keratosis : Seborrheic keratosis Clonal seborrheic keratosis Common seborrheic keratosis Irritated seborrheic keratosis Seborrheic keratosis with squamous atypia Reticulated seborrheic keratosis Dermatosis papulosa nigra Keratosis punctata of the palmar creases other hyperkeratosis : Acanthosis nigricans Confluent and reticulated papillomatosis Callus Ichthyosis acquisita Arsenical keratosis Chronic scar keratosis Hyperkeratosis lenticularis perstans Hydrocarbon keratosis Hyperkeratosis of the nipple and areola Inverted follicular keratosis Lichenoid keratosis Multiple minute digitate hyperkeratosis PUVA keratosis Reactional keratosis Stucco keratosis Thermal keratosis Viral keratosis Warty dyskeratoma Waxy keratosis of childhood other hypertrophy: Keloid Hypertrophic scar Cutis verticis gyrata Necrobiosis / granuloma Necrobiotic/palisading Granuloma annulare Perforating Generalized Subcutaneous Granuloma annulare in HIV disease Localized granuloma annulare Patch-type granuloma annulare Necrobiosis lipoidica Annular elastolytic giant-cell granuloma Granuloma multiforme Necrobiotic xanthogranuloma Palisaded neutrophilic and granulomatous dermatitis Rheumatoid nodulosis Interstitial granulomatous dermatitis / Interstitial granulomatous drug reaction Foreign body granuloma Beryllium granuloma Mercury granuloma Silica granuloma Silicone granuloma Zirconium granuloma Soot tattoo Tattoo Carbon stain Other/ungrouped eosinophilic dermatosis Granuloma faciale Dermis / localized CTD Cutaneous lupus erythematosus chronic: Discoid Panniculitis subacute : Neonatal ungrouped: Chilblain Lupus erythematosus–lichen planus overlap syndrome Tumid Verrucous Rowell's syndrome Scleroderma / Morphea Localized scleroderma Localized morphea Morphea–lichen sclerosus et atrophicus overlap Generalized morphea Atrophoderma of Pasini and Pierini Pansclerotic morphea Morphea profunda Linear scleroderma Atrophic / atrophoderma Lichen sclerosus Anetoderma Schweninger–Buzzi anetoderma Jadassohn–Pellizzari anetoderma Atrophoderma of Pasini and Pierini Acrodermatitis chronica atrophicans Semicircular lipoatrophy Follicular atrophoderma Linear atrophoderma of Moulin Perforating Kyrle disease Reactive perforating collagenosis Elastosis perforans serpiginosa Perforating folliculitis Acquired perforating dermatosis Skin ulcer Pyoderma gangrenosum Other Calcinosis cutis Sclerodactyly Poikiloderma vasculare atrophicans Ainhum / Pseudo-ainhum v t e Congenital malformations and deformations of integument / skin disease Genodermatosis Congenital ichthyosis / erythrokeratodermia AD Ichthyosis vulgaris AR Congenital ichthyosiform erythroderma : Epidermolytic hyperkeratosis Lamellar ichthyosis Harlequin-type ichthyosis Netherton syndrome Zunich–Kaye syndrome Sjögren–Larsson syndrome XR X-linked ichthyosis Ungrouped Ichthyosis bullosa of Siemens Ichthyosis follicularis Ichthyosis prematurity syndrome Ichthyosis–sclerosing cholangitis syndrome Nonbullous congenital ichthyosiform erythroderma Ichthyosis linearis circumflexa Ichthyosis hystrix EB and related EBS EBS-K EBS-WC EBS-DM EBS-OG EBS-MD EBS-MP JEB JEB-H Mitis Generalized atrophic JEB-PA DEB DDEB RDEB related: Costello syndrome Kindler syndrome Laryngoonychocutaneous syndrome Skin fragility syndrome Ectodermal dysplasia Naegeli syndrome / Dermatopathia pigmentosa reticularis Hay–Wells syndrome Hypohidrotic ectodermal dysplasia Focal dermal hypoplasia Ellis–van Creveld syndrome Rapp–Hodgkin syndrome / Hay–Wells syndrome Elastic / Connective Ehlers–Danlos syndromes Cutis laxa ( Gerodermia osteodysplastica ) Popliteal pterygium syndrome Pseudoxanthoma elasticum Van der Woude syndrome Hyperkeratosis / keratinopathy PPK diffuse : Diffuse epidermolytic palmoplantar keratoderma Diffuse nonepidermolytic palmoplantar keratoderma Palmoplantar keratoderma of Sybert Meleda disease syndromic connexin Bart–Pumphrey syndrome Clouston's hidrotic ectodermal dysplasia Vohwinkel syndrome Corneodermatoosseous syndrome plakoglobin Naxos syndrome Scleroatrophic syndrome of Huriez Olmsted syndrome Cathepsin C Papillon–Lefèvre syndrome Haim–Munk syndrome Camisa disease focal : Focal palmoplantar keratoderma with oral mucosal hyperkeratosis Focal palmoplantar and gingival keratosis Howel–Evans syndrome Pachyonychia congenita Pachyonychia congenita type I Pachyonychia congenita type II Striate palmoplantar keratoderma Tyrosinemia type II punctate : Acrokeratoelastoidosis of Costa Focal acral hyperkeratosis Keratosis punctata palmaris et plantaris Keratosis punctata of the palmar creases Schöpf–Schulz–Passarge syndrome Porokeratosis plantaris discreta Spiny keratoderma ungrouped: Palmoplantar keratoderma and spastic paraplegia desmoplakin Carvajal syndrome connexin Erythrokeratodermia variabilis HID / KID Other Meleda disease Keratosis pilaris ATP2A2 Darier's disease Dyskeratosis congenita Lelis syndrome Dyskeratosis congenita Keratolytic winter erythema Keratosis follicularis spinulosa decalvans Keratosis linearis with ichthyosis congenita and sclerosing keratoderma syndrome Keratosis pilaris atrophicans faciei Keratosis pilaris Other cadherin EEM syndrome immune system Hereditary lymphedema Mastocytosis / Urticaria pigmentosa Hailey–Hailey see also Template:Congenital malformations and deformations of skin appendages , Template:Phakomatoses , Template:Pigmentation disorders , Template:DNA replication and repair-deficiency disorder Developmental anomalies Midline Dermoid cyst Encephalocele Nasal glioma PHACE association Sinus pericranii Nevus Capillary hemangioma Port-wine stain Nevus flammeus nuchae Other/ungrouped Aplasia cutis congenita Amniotic band syndrome Branchial cyst Cavernous venous malformation Accessory nail of the fifth toe Bronchogenic cyst Congenital cartilaginous rest of the neck Congenital hypertrophy of the lateral fold of the hallux Congenital lip pit Congenital malformations of the dermatoglyphs Congenital preauricular fistula Congenital smooth muscle hamartoma Cystic lymphatic malformation Median raphe cyst Melanotic neuroectodermal tumor of infancy Mongolian spot Nasolacrimal duct cyst Omphalomesenteric duct cyst Poland anomaly Rapidly involuting congenital hemangioma Rosenthal–Kloepfer syndrome Skin dimple Superficial lymphatic malformation Thyroglossal duct cyst Verrucous vascular malformation Birthmark
-
Zttk Syndrome
Wikipedia
ZTTK syndrome Other names Z hu- T okita- T akenouchi- K im syndrome ZTTK Syndrome (Zhu-Tokita-Takenouchi-Kim syndrome) is a rare disease caused in humans by a genetic mutation of the SON gene . ... Macrocephaly and brain white matter abnormalities have also been observed. [5] Seizures often develop between the ages of 1 to 6 years old. [3] Physiological [ edit ] Mutations of the SON gene can affect metabolism and mitochondrial function in newborns with ZTTK syndrome. Metabolic screening confirmed mitochondrial dysfunction and O-glycosylation defects in individuals with ZTTK syndrome. [1] Decreased levels of immunoglobulin A and or immunoglobulin G identified in ZTTK syndrome patients resulted in coagulation abnormalities. [2] Genetics [ edit ] ZTTK syndrome is caused by heterozygous mutations in the SON gene. [5] As an autosomal dominant disease, children with parents carrying a SON mutation have a 50% risk of inheriting the mutation. ... For example, FLNA haploinsufficiency observed in individuals with ZTTK syndrome is the main cause of a rare brain disorder, periventricular nodular heterotopia . ... PMID 27545680 . ^ a b "OMIM Entry # 617140 - ZTTK SYNDROME; ZTTKS" . Online Mendelian Inheritance in Man . ... "EstablishingSONin 21q22.11 as a cause a new syndromic form of intellectual disability: Possible contribution to Braddock-Carey syndrome phenotype" .
-
Berk–tabatznik Syndrome
Wikipedia
Berk–Tabatznik syndrome Other names Kyphosis brachyphalangy optic atrophy Berk–Tabatznik syndrome is a medical condition with an unknown cause that shows symptoms of short stature , congenital optic atrophy and brachytelephalangy . This condition is extremely rare with only two cases being found. [1] Contents 1 See also 2 References 3 Further reading 4 External links See also [ edit ] Heart-hand diseases Rare disease References [ edit ] ^ Bissonnette, Bruno; Luginbuehl, Igor; Dalens, Bernard J., eds. (2006). "Berk–Tabatznik Syndrome" . Syndromes: rapid recognition and perioperative implications . ... "Congenital optic atrophy and brachytelephalangy: the Berk–Tabatznik syndrome". American Journal of Medical Genetics . 29 (2): 383–9. doi : 10.1002/ajmg.1320290220 .
-
Pellegrini–stieda Syndrome
Wikipedia
Please help to improve this article by introducing more precise citations. ( September 2009 ) ( Learn how and when to remove this template message ) Pellegrini–Stieda syndrome Pellegrini-Stieda syndrome. Also visible is a fracture of the patella. Pellegrine–Stieda syndrome (also called Stieda disease and Köhler–Pellegrine–Stieda disease) refers to the ossification of the superior part of the medial collateral ligament of the knee. ... "Images in clinical medicine. Pellegrini-Stieda syndrome". The New England Journal of Medicine . 354 (1): e1. doi : 10.1056/NEJMicm040406 . ... Wang, JC; Shapiro, MS (1995). "Pellegrini-Stieda syndrome". American Journal of Orthopedics . 24 (6): 493–7.
-
Biemond Syndrome
Wikipedia
Biemond syndrome Other names Brachydactyly–nystagmus–cerebellar ataxia syndrome Biemond syndrome is a genetic disorder characterised by brachydactyly , nystagmus , strabismus , cerebellar ataxia and intellectual disability. ... Some of the members did not have the full syndrome. [1] Diagnosis [ edit ] This section is empty. ... Retrieved 2019-12-23 . ^ Beighton, Greta (2012-12-06). The Person Behind the Syndrome . Springer Science & Business Media. p. 83.
-
Lennox–gastaut Syndrome
Wikipedia
These diagnoses are: [ citation needed ] Doose syndrome Dravet syndrome pseudo-Lennox Gastaut syndrome ( atypical benign partial epilepsy ) LGS is more easily distinguished from Doose syndrome by seizure type after the syndrome has progressed. ... The Doose syndromes is less likely to have cognitive disabilities. [ citation needed ] The Dravet syndrome has a strong family history of epilepsy, unlike LGS. ... "Lennox–Gastaut syndrome (childhood epileptic encephalopathy)". ... Pg. 51 ^ Ohtahara S, Yamatogi Y, Ohtsukd Y, Oka E, lshida T. Prognosis of West syndrome with special reference to Lennox syndrome: a developmental study. ... Retrieved 2007-09-19 . ^ The Felbamate Study Group In Lennox–Gastaut Syndrome (1993). "Efficacy of felbamate in childhood epileptic encephalopathy (Lennox-Gastaut syndrome).
-
Mitochondrial Dna-Associated Leigh Syndrome And Narp
Gene_reviews
LLS = Leigh-like syndrome; LS = Leigh syndrome 1. Genes are listed alphabetically. 2. ... The heterogeneous clinical presentation that occurs in Leigh syndrome is also present in Leigh-like syndromes. ... Individuals with Leigh syndrome caused by a mtDNA pathogenic variant are often referred to as having "maternally inherited Leigh syndrome" (MILS) [Ciafaloni et al 1993]. Prevalence The following prevalence data are for all Leigh syndrome. In southeastern Australia, Leigh syndrome occurs in 1:77,000 infants, and the combined birth prevalence of Leigh syndrome plus Leigh-like syndrome was 1:40,000 [Rahman et al 1996]. ... NARP is substantially less common than Leigh syndrome. Differential Diagnosis Leigh syndrome and Leigh-like syndrome.
-
Gastrojejunocolic Fistula
Wikipedia
Retrieved 29 July 2010 . v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Chops Syndrome
Medlineplus
CHOPS syndrome is a disorder involving multiple abnormalities that are present from birth (congenital). ... People with CHOPS syndrome have abnormalities of the throat and airways that cause momentary cessation of breathing while asleep (obstructive sleep apnea). ... Frequency CHOPS syndrome is a rare disorder whose prevalence is unknown. Only a few affected individuals have been described in the medical literature. Causes CHOPS syndrome is caused by mutations in the AFF4 gene. ... This dysregulation of transcription leads to problems in the development of multiple organs and tissues, resulting in the signs and symptoms of CHOPS syndrome. Learn more about the gene associated with CHOPS syndrome AFF4 Inheritance Pattern CHOPS syndrome is inherited in an autosomal dominant pattern , which means one copy of the altered gene in each cell is sufficient to cause the disorder.
-
Couvade Syndrome
Wikipedia
The labor pain symptom is commonly known as sympathy pain . Couvade syndrome is not recognized as a real syndrome by many medical professionals. [2] Its source is a matter of debate. ... Retrieved 20 April 2012 . ^ a b Klein, Hilary (1991). "Couvade syndrome: Male counterpart to pregnancy". ... "What can you tell me about Couvade syndrome? Can men really experience sympathetic pregnancy symptoms?" ... H.; Conlon, M. F. (1965). "The Couvade Syndrome". The British Journal of Psychiatry . 111 (470): 57–66. doi : 10.1192/bjp.111.470.57 . ... Bogren, L. Y. (1984). "The couvade syndrome: Background variables". Acta Psychiatrica Scandinavica . 70 (4): 316–20. doi : 10.1111/j.1600-0447.1984.tb01215.x .
-
Arterial Tortuosity Syndrome
Wikipedia
Arterial tortuosity syndrome (ATS) Arterial tortuosity syndrome has an autosomal recessive pattern of inheritance Specialty Cardiology Symptoms Congenital diaphragmatic hernia [1] Causes Mutations in SLC2A10 gene [2] [3] Diagnostic method CT scan, MRI [4] Treatment Possible surgery for aortic aneurysms [5] Arterial tortuosity syndrome is a rare congenital connective tissue condition disorder characterized by elongation and generalized tortuosity of the major arteries including the aorta . [1] [6] It is associated with hyperextensible skin and hypermobility of joints , however symptoms vary depending on the person. ... "arterial tortuosity syndrome" . Genetics Home Reference . Retrieved 2017-03-21 . ^ Morris, Shaine A. (2017-03-23). ... PMID 26398550 . ^ "Arterial tortuosity syndrome - Conditions - GTR - NCBI" . www.ncbi.nlm.nih.gov . ... "Glucose transporter 10 and arterial tortuosity syndrome: the vitamin C connection". FEBS Letters . 584 (14): 2990–2994. doi : 10.1016/j.febslet.2010.06.011 . ... "Clinical utility gene card for: Arterial tortuosity syndrome" . European Journal of Human Genetics . 23 (10): 1432. doi : 10.1038/ejhg.2014.294 .
-
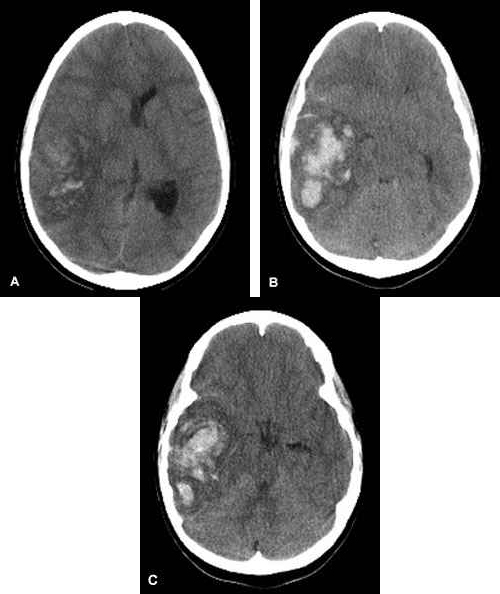
Intraparenchymal Hemorrhage
Wikipedia
Substantial displacement of brain parenchyma may cause elevation of intracranial pressure (ICP) and potentially fatal herniation syndromes . Contents 1 Signs and symptoms 2 Causes 3 Pathophysiology 4 Diagnosis 5 Treatment 6 References 7 External links Signs and symptoms [ edit ] Clinical manifestations of intraparenchymal hemorrhage are determined by the size and location of hemorrhage, but may include the following: [ citation needed ] Hypertension, fever , or cardiac arrhythmias Nuchal rigidity Subhyaloid retinal hemorrhages Altered level of consciousness Anisocoria , nystagmus Focal neurological deficits Putamen - Contralateral hemiparesis , contralateral sensory loss, contralateral conjugate gaze paresis, homonymous hemianopsia , aphasia , neglect, or apraxia Thalamus - Contralateral sensory loss, contralateral hemiparesis, gaze paresis, homonymous hemianopia, miosis , aphasia, or confusion Lobar - Contralateral hemiparesis or sensory loss, contralateral conjugate gaze paresis, homonymous hemianopia, abulia , aphasia, neglect, or apraxia Caudate nucleus - Contralateral hemiparesis, contralateral conjugate gaze paresis, or confusion Brain stem - Tetraparesis , facial weakness, decreased level of consciousness, gaze paresis, ocular bobbing, miosis, or autonomic instability Cerebellum - Ataxia , usually beginning in the trunk, ipsilateral facial weakness, ipsilateral sensory loss, gaze paresis, skew deviation , miosis, or decreased level of consciousness Causes [ edit ] Hypertension Arteriovenous malformation Aneurysm rupture Cerebral amyloid angiopathy Intracranial neoplasm Coagulopathy Hemorrhagic transformation of an ischemic stroke Cerebral venous thrombosis Sympathomimetic drug abuse Moyamoya disease Sickle cell disease Eclampsia or postpartum vasculopathy Infection Vasculitis Neonatal intraventricular hemorrhage Trauma In younger patients, vascular malformations, specifically AVMs and cavernous angiomas are more common causes for hemorrhage. ... References [ edit ] External links [ edit ] Classification D ICD - 10 : I61 .0-4, .6-9 ICD - 9-CM : 431 MeSH : D002543 v t e Cerebrovascular diseases including stroke Ischaemic stroke Brain Anterior cerebral artery syndrome Middle cerebral artery syndrome Posterior cerebral artery syndrome Amaurosis fugax Moyamoya disease Dejerine–Roussy syndrome Watershed stroke Lacunar stroke Brain stem Brainstem stroke syndrome Medulla Medial medullary syndrome Lateral medullary syndrome Pons Medial pontine syndrome / Foville's Lateral pontine syndrome / Millard-Gubler Midbrain Weber's syndrome Benedikt syndrome Claude's syndrome Cerebellum Cerebellar stroke syndrome Extracranial arteries Carotid artery stenosis precerebral Anterior spinal artery syndrome Vertebrobasilar insufficiency Subclavian steal syndrome Classification Brain ischemia Cerebral infarction Classification Transient ischemic attack Total anterior circulation infarct Partial anterior circulation infarct Other CADASIL Binswanger's disease Transient global amnesia Haemorrhagic stroke Extra-axial Epidural Subdural Subarachnoid Cerebral/Intra-axial Intraventricular Brainstem Duret haemorrhages General Intracranial hemorrhage Aneurysm Intracranial aneurysm Charcot–Bouchard aneurysm Other Cerebral vasculitis Cerebral venous sinus thrombosis v t e Neurotrauma Traumatic brain injury Intracranial hemorrhage Intra-axial Intraparenchymal hemorrhage Intraventricular hemorrhage Extra-axial Subdural hematoma Epidural hematoma Subarachnoid hemorrhage Brain herniation Cerebral contusion Cerebral laceration Concussion Post-concussion syndrome Second-impact syndrome Dementia pugilistica Chronic traumatic encephalopathy Diffuse axonal injury Abusive head trauma Penetrating head injury Spinal cord injury Anterior spinal artery syndrome Brown-Séquard syndrome Cauda equina syndrome Central cord syndrome Paraplegia Posterior cord syndrome Spinal cord injury without radiographic abnormality Tetraplegia (Quadriplegia) Peripheral nerves Nerve injury Peripheral nerve injury classification Wallerian degeneration Injury of accessory nerve Brachial plexus injury Traumatic neuroma