-
Susto
Wikipedia
It is described by Razzouk et al. as a condition of being frightened and "chronic somatic suffering stemming from emotional trauma or from witnessing traumatic experiences lived by others". [1] Susto is classified as a culture-bound syndrome , [2] a symptom that occurs and is recognized within an ethnic group. [3] Contents 1 Symptoms 2 Treatment 3 Classification 4 See also 5 References 6 Further reading Symptoms [ edit ] Among the indigenous peoples of Latin America , in which this illness is most common, susto may be conceptualized as a case of spirit attack. [4] Symptoms of susto are thought to include nervousness, anorexia , insomnia, listlessness, fever, depression, and diarrhea. [1] Treatment [ edit ] The treatment used among the indigenous people was all natural. ... "The contribution of Latin American and Caribbean countries on culture bound syndromes studies for the ICD-10 revision: key findings from a work in progress" . ... "Coraje, nervios, andsusto: Culture-bound syndromes and mental health among Mexican migrants in the United States". ... S2CID 57602592 . ^ Griffith, Laura (2014-02-21), "Culture-Bound Syndrome", The Wiley Blackwell Encyclopedia of Health, Illness, Behavior, and Society , John Wiley & Sons, Ltd, pp. 354–356, doi : 10.1002/9781118410868.wbehibs189 , ISBN 9781118410868 ^ Castillo, Richard (1997). ... Retrieved 6 March 2013 . v t e Superstition Main topics Amulet Evil eye Luck Omen Talismans Myth and ritual Lists List of superstitions List of lucky symbols List of bad luck signs Sailors' superstitions Theatrical superstitions Africa Buda Gris-gris Sampy Sleeping child Americas Ascalapha odorata Carranca Cooties Curupira Djucu Fortune cookie Groundhog Day I'noGo tied Oscar love curse Susto White lighter myth Witch window Asia Superstition in India Superstition in Pakistan Japanese superstitions Bhoot (ghost) Chhaupadi Churel Ghosts in Bengali culture Jackal's horn Kuai Kuai culture Muhurta Navaratna Nazar battu Pichal Peri Puppy pregnancy syndrome Akabeko Kanai Anzen Maneki-neko Okiagari-koboshi Omamori Fan death Agimat Arbularyo Barang Kulam Lihi Pagtatawas Pasma Usog Kuman Thong Palad khik Takrut Nang Kwak White elephant Curse of 39 Jin Chan Numbers in Chinese culture Superstitions of Malaysian Chinese Europe August curse Barbary macaques in Gibraltar Bayern-luck Blarney Stone Cimaruta Cornicello The Goodman's Croft Himmelsbrief Icelandic magical staves In bocca al lupo Kitchen witch Klabautermann Mooncalf Nazar Need-fire Painted pebbles Powder of sympathy Rabbit rabbit rabbit Ravens of the Tower of London Russian traditions and superstitions Spilling water for luck The Scottish Play Troll cross Tycho Brahe days Witch post Wolfssegen General 11:11 4 ( Four-leaf clover , Tetraphobia ) 7 ( Seventh son of a seventh son ) 8 9 13 ( Friday the 13th , The Thirteen Club , Thirteenth floor , Triskaidekaphobia ) 108 111 666 ( Number of the Beast ) Ace of spades Auspicious wedding dates Baseball superstition Beginner's luck Black cat Bread and butter Break a leg Chain letter Cramp-ring Curse Davy Jones' Locker Dead man's hand End-of-the-day betting effect Fear of frogs Fear of ghosts First-foot Flying Dutchman Four Eleven Forty Four Gambler's conceit Good luck charm Human sacrifice Jinx Knocking on wood Law of contagion Literomancy Lock of hair Maternal impression Miasma theory Nelson Numismatic charm Penny Rabbit's foot Rainmaking Ship sponsor Shoes on a table Sign of the horns Something old Spilling salt Statue rubbing Three on a match Threshold Toi toi toi 27 Club Wishing well Witch ball Witching hour Related Apotropaic magic Astrology and science Coincidence Debunker Divination Folk religion Fortune-telling Magic and religion Magical thinking Numerology Perceptions of religious imagery in natural phenomena Post hoc ergo propter hoc Traditional medicine Urban legend Jew Muslim
-
Arteriovenous Fistula
Wikipedia
External links [ edit ] Classification D ICD - 10 : I28.0 , I77.0 ICD - 9-CM : 414.19 , 417.0 , 447.0 , 747.3 MeSH : D001164 DiseasesDB : 32435 SNOMED CT : 439470001 External resources eMedicine : med/169 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotensionACE, VEGFA, NOS3, MMP2, MMP9, COL1A1, TIMP4, ANGPT2, ARRB1, ARRB2, DES, ACKR1, RASA1, ALB, HMOX1, PTH, EFNB2, AGTR1, IL6, PTEN, CCL2, TGFB1, AGT, EPO, ATM, VDR, TP53, TNF, AKT1, TIMP2, TGFBR1, STAT3, WNT1, SPP1, BAX, S100A4, REN, BCL2, PTX3, AHSG, FGF23, ESR1, RXFP1, TEX46, MIR21, MIR155, PTCRA, RIOX2, RIOX1, NAAA, IER3, ERAL1, ATP6V0A2, WDHD1, PROCR, LRPPRC, SLC33A1, BMP7, CAV1, PROC, CS, IL6ST, CRP, RBPJ, IGF1R, IGF1, ID2, GSTA4, SERPINE1, GLP1R, ELN, F11, F5, F2R, F2, ITGA2B, LGALS3, LIMS1, LMO7, LRP1, CD180, MMP1, CREM, MMP3, CD44, MNT, MTHFR, NDUFS4, NF1, NM, CD38, NOTCH4, PGR-AS1
-
Arteriolosclerosis
Wikipedia
External links [ edit ] Classification D MeSH : D050379 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension
-
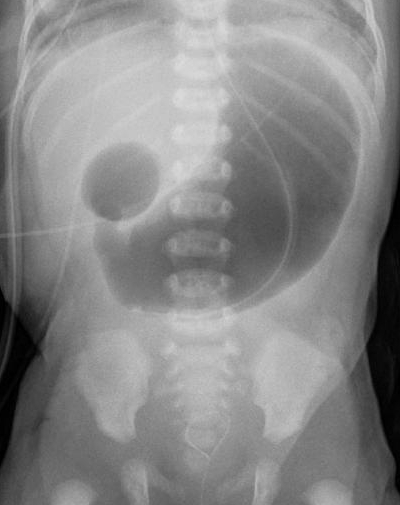
Duodenal Atresia
Wikipedia
Contents 1 Presentation 1.1 Complications 1.2 Associated conditions 2 Diagnosis 2.1 Physical examination 3 Treatment 4 Epidemiology 5 References 6 External links Presentation [ edit ] Complications [ edit ] Prognosis is usually very good, although complications are more likely to occur when there are serious congenital anomalies. [1] Late complications may occur in about 12 percent of patients with duodenal atresia, and the mortality rate for these complications is 6 percent. [2] Associated conditions [ edit ] Approximately 20–40 percent of all infants with duodenal atresia have Down syndrome and 50% have a congenital cardiac anomaly. [3] Approximately 8% of infants with Down syndrome have duodenal atresia. [4] Diagnosis [ edit ] The diagnosis of duodenal atresia is usually confirmed by radiography . ... External links [ edit ] Classification D ICD - 10 : Q41.0 ICD - 9-CM : 751.1 OMIM : 223400 MeSH : C535720 DiseasesDB : 31514 External resources MedlinePlus : 001131 eMedicine : ped/2776 radio/223 v t e Congenital malformations and deformations of digestive system Upper GI tract Tongue , mouth and pharynx Cleft lip and palate Van der Woude syndrome tongue Ankyloglossia Macroglossia Hypoglossia Esophagus EA/TEF Esophageal atresia: types A, B, C, and D Tracheoesophageal fistula: types B, C, D and E esophageal rings Esophageal web (upper) Schatzki ring (lower) Stomach Pyloric stenosis Hiatus hernia Lower GI tract Intestines Intestinal atresia Duodenal atresia Meckel's diverticulum Hirschsprung's disease Intestinal malrotation Dolichocolon Enteric duplication cyst Rectum / anal canal Imperforate anus Rectovestibular fistula Persistent cloaca Rectal atresia Accessory Pancreas Annular pancreas Accessory pancreas Johanson–Blizzard syndrome Pancreas divisum Bile duct Choledochal cysts Caroli disease Biliary atresia Liver Alagille syndrome Polycystic liver disease
-
Hyperlysinemia
Wikipedia
External links [ edit ] Classification D ICD - 10 : E72.3 ICD - 9-CM : 270.7 OMIM : 238700 MeSH : D020167 DiseasesDB : 33215 v t e Inborn error of amino acid metabolism K → acetyl-CoA Lysine /straight chain Glutaric acidemia type 1 type 2 Hyperlysinemia Pipecolic acidemia Saccharopinuria Leucine 3-hydroxy-3-methylglutaryl-CoA lyase deficiency 3-Methylcrotonyl-CoA carboxylase deficiency 3-Methylglutaconic aciduria 1 Isovaleric acidemia Maple syrup urine disease Tryptophan Hypertryptophanemia G G→ pyruvate → citrate Glycine D-Glyceric acidemia Glutathione synthetase deficiency Sarcosinemia Glycine → Creatine : GAMT deficiency Glycine encephalopathy G→ glutamate → α-ketoglutarate Histidine Carnosinemia Histidinemia Urocanic aciduria Proline Hyperprolinemia Prolidase deficiency Glutamate / glutamine SSADHD G→ propionyl-CoA → succinyl-CoA Valine Hypervalinemia Isobutyryl-CoA dehydrogenase deficiency Maple syrup urine disease Isoleucine 2-Methylbutyryl-CoA dehydrogenase deficiency Beta-ketothiolase deficiency Maple syrup urine disease Methionine Cystathioninuria Homocystinuria Hypermethioninemia General BC / OA Methylmalonic acidemia Methylmalonyl-CoA mutase deficiency Propionic acidemia G→ fumarate Phenylalanine / tyrosine Phenylketonuria 6-Pyruvoyltetrahydropterin synthase deficiency Tetrahydrobiopterin deficiency Tyrosinemia Alkaptonuria / Ochronosis Tyrosinemia type I Tyrosinemia type II Tyrosinemia type III / Hawkinsinuria Tyrosine → Melanin Albinism : Ocular albinism ( 1 ) Oculocutaneous albinism ( Hermansky–Pudlak syndrome ) Waardenburg syndrome Tyrosine → Norepinephrine Dopamine beta hydroxylase deficiency reverse: Brunner syndrome G→ oxaloacetate Urea cycle / Hyperammonemia ( arginine aspartate ) Argininemia Argininosuccinic aciduria Carbamoyl phosphate synthetase I deficiency Citrullinemia N-Acetylglutamate synthase deficiency Ornithine transcarbamylase deficiency / translocase deficiency Transport / IE of RTT Solute carrier family : Cystinuria Hartnup disease Iminoglycinuria Lysinuric protein intolerance Fanconi syndrome : Oculocerebrorenal syndrome Cystinosis Other 2-Hydroxyglutaric aciduria Aminoacylase 1 deficiency Ethylmalonic encephalopathy Fumarase deficiency Trimethylaminuria This genetic disorder article is a stub .
-
Exostosis
Wikipedia
External links [ edit ] Classification D ICD - 9-CM : 726.91 MeSH : D005096 DiseasesDB : 18621 External resources Patient UK : Exostosis The Ear and Balance Center , The Sonos Group MHE Research Foundation (Multiple Hereditary Exostoses) v t e Diseases of joints General Arthritis Monoarthritis Oligoarthritis Polyarthritis Symptoms Joint pain Joint stiffness Inflammatory Infectious Septic arthritis Tuberculosis arthritis Crystal Chondrocalcinosis CPPD (Psudogout) Gout Seronegative Reactive arthritis Psoriatic arthritis Ankylosing spondylitis Other Juvenile idiopathic arthritis Rheumatoid arthritis Felty's syndrome Palindromic rheumatism Adult-onset Still's disease Noninflammatory Hemarthrosis Osteoarthritis Heberden's node Bouchard's nodes Osteophyte v t e Bone and joint disease Bone Inflammation endocrine : Osteitis fibrosa cystica Brown tumor infection : Osteomyelitis Sequestrum Involucrum Sesamoiditis Brodie abscess Periostitis Vertebral osteomyelitis Metabolic Bone density Osteoporosis Juvenile Osteopenia Osteomalacia Paget's disease of bone Hypophosphatasia Bone resorption Osteolysis Hajdu–Cheney syndrome Ainhum Gorham's disease Other Ischaemia Avascular necrosis Osteonecrosis of the jaw Complex regional pain syndrome Hypertrophic pulmonary osteoarthropathy Nonossifying fibroma Pseudarthrosis Stress fracture Fibrous dysplasia Monostotic Polyostotic Skeletal fluorosis bone cyst Aneurysmal bone cyst Hyperostosis Infantile cortical hyperostosis Osteosclerosis Melorheostosis Pycnodysostosis Joint Chondritis Relapsing polychondritis Other Tietze's syndrome Combined Osteochondritis Osteochondritis dissecans Child leg: hip Legg–Calvé–Perthes syndrome tibia Osgood–Schlatter disease Blount's disease foot Köhler disease Sever's disease spine Scheuermann's_disease arm: wrist Kienböck's disease elbow Panner disease
-
Megavitamin-B6 Syndrome
Wikipedia
A syndrome marked by sensory neuropathy induced from acute overdose, or chronic supplementation, of vitamin b6 Megavitamin-B 6 syndrome Other names Vitamin B 6 Excess, Hypervitaminosis B 6 , Vitamin B 6 Toxicity [1] [2] Specialty Neurology , toxicology Symptoms Peripheral sensory neuropathy Usual onset Gradual onset with slow progression, in the usual case of chronic vitamin B 6 supplementation. [3] Duration Usually, but not always, resolves within 6 months from cessasation of vitamin B 6 . [4] Causes Chronic vitamin B 6 supplementation, or acute parenteral or oral over‐dosages of vitamin B 6 . [5] [4] [6] [7] [8] Risk factors Impaired kidney function, parenteral nutrition [9] Diagnostic method Serum testing for elevated levels of vitamin B 6 , testing of tendon reflexes , nerve conduction studies and electrodiagnostic testing. [10] [11] Differential diagnosis Progressive mixed sensory or sensorimotor polyneuropathy of undetermined etiology. [12] [13] Treatment Cessation of vitamin B 6 supplementation. [14] Prognosis Symptom progression for 2-6 weeks following cessation of vitamin B 6 , followed by gradual improvement. [14] [4] [15] [16] Megavitamin-B 6 syndrome is a collection of symptoms that can result from chronic supplementation, or acute overdose, of vitamin B 6 . [4] [6] [5] While it is also known as hypervitaminosis B 6 , vitamin B 6 toxicity and vitamin B 6 excess , megavitamin-b6 syndrome is the name used in the ICD-10 . [17] [1] [2] [a] Contents 1 Signs and symptoms 2 Cause 2.1 Potential mechanisms 3 Tolerable upper limits 3.1 Exceptions 4 Diagnosis 4.1 Classification 5 Treatment 6 Prognosis 7 See also 8 Notes 9 References 10 Further reading 11 External links Signs and symptoms [ edit ] The predominant symptom is peripheral sensory neuropathy [23] [4] [6] [24] that is experienced as numbness, pins-and-needles and burning sensations ( paresthesia ) in a patient's limbs on both sides of their body. [14] [4] [13] [15] Patients may experience unsteadiness of gait, incoordination ( ataxia ), [15] [25] [4] [26] involuntary muscle movements ( choreoathetosis ) [10] the sensation of an electric zap in their bodies ( Lhermitte's sign ), [15] a heightened sensitivity to sense stimuli including photosensitivity ( hyperesthesia ), [4] [25] impaired skin sensation ( hypoesthesia ), [27] [14] numbness around the mouth, [27] [3] and gastrointestinal symptoms such as nausea and heartburn . [25] [28] The ability to sense vibrations and to sense one's position are diminished to a greater degree than pain or temperature. [27] [3] Skin lesions have also been reported. [25] [26] [29] [28] Megavitamin-B 6 syndrome may also contribute to burning mouth syndrome . [30] [31] Potential psychiatric symptoms range from anxiety , depression , agitation , and cognitive deficits to psychosis . [32] Symptom severity appears to be dose-dependent (higher doses cause more severe symptoms) [25] and the duration of supplementation with vitamin B 6 before onset of systems appears to be inversely proportional to the amount taken daily (the smaller the daily dosage, the longer it will take for symptoms to develop). [15] [4] [10] [12] [7] It is also possible that some individuals are more susceptible to the toxic effects of vitamin B 6 than others. [4] Megavitamin-B 6 syndrome has been reported in doses as low as 24 mg/day. [33] Symptoms may also be dependent on the form of vitamin B 6 taken in supplements. [24] [34] It has been proposed that vitamin B 6 in supplements should be in pyridoxal or pyridoxal phosphate form rather than pyridoxine as these are thought to reduce the likelihood of toxicity. [24] [35] A tissue culture study, however, showed that all B 6 vitamers that could be converted into active coenzymes (pyridoxal, pyridoxine and pyridoxamine ) were neurotoxic at similar concentrations . [19] [36] Consuming high amounts of vitamin B 6 from food has not been reported to cause adverse effects. [25] [29] [37] Early diagnosis and cessation of vitamin B 6 supplementation can reduce the morbidity of the syndrome. [25] [12] Cause [ edit ] There is a longstanding common misconception that because vitamin B 6 is water-soluble it is therefore harmless. [19] [38] [27] While vitamin B 6 is water-soluble, it has a half-life of 25–33 days and accumulates in the body where it is stored in muscle , plasma , the liver , red blood cells and bound to proteins in tissues. [38] [37] [39] Potential mechanisms [ edit ] The common supplemental form of vitamin B 6 , pyridoxine, is similar to pyridine which can be neurotoxic. ... This is known as coasting and is encountered in other toxic neuropathies. [14] [4] [15] [16] A vitamin B 6 substance dependency may exist in daily dosages of 200 mg or more, making a drug withdrawal effect possible when discontinued. [27] See also [ edit ] B vitamins Dietary Reference Intake Dietary supplement Hypervitaminosis Hypervitaminosis A Hypervitaminosis D Megavitamin therapy Overnutrition Peripheral nervous system Regulation of alternative medicine Notes [ edit ] ^ While megavitamin-B 6 syndrome, hypervitaminosis B 6 , vitamin B 6 toxicity and vitamin B 6 excess are officially recognized, terms for this in literate vary. ... "Role of vitamin B 6 in idiopathic burning mouth syndrome: some clinical observations" (PDF) . ... Further reading [ edit ] A chapter with a story about a woman experiencing a severe case of Megavitamin-B6 syndrome titled "The Disembodied Lady" appears in Chapter 3 of The Man Who Mistook His Wife for a Hat : Oliver Sacks; Oliver W. ... An ethnographic study of an online support group for megavitamin B 6 syndrome appears in: Laura D. Russell (16 December 2019).
-
Rubella
Wikipedia
Rubella can cause congenital rubella syndrome in the newborn, this being the most severe sequela of rubella. ... "Control of rubella and congenital rubella syndrome (CRS) in developing countries, Part 2: Vaccination against rubella" . ... "Elimination of rubella and congenital rubella syndrome—United States, 1969–2004" . MMWR Morb. ... "Optical complications in congenital rubella syndrome". Optometry . 73 (7): 418–24. PMID 12365660 . ^ Freij BJ, South MA, Sever JL (1988). "Maternal rubella and the congenital rubella syndrome". Clin Perinatol . 15 (2): 247–57. doi : 10.1016/S0095-5108(18)30710-3 .MRC1, MFSD6, EBI3, IL10RB, IL18R1, IL6, LAMP3, IL12B, LSAMP, ABL1, CHAF1A, PDR, ELP1, TWIST1, TNF, TFRC, CTR9, RAB3GAP2, IFNG, CIP2A, ANPEP, ERVK-6, CANX, CCDC8, PIK3R4, ERVW-1, CDK5R1, UPK3B, TNFRSF1A, TPO, ERVK-20, WT1, MIR206, LINC01194, CDCA5, PER2, ARID2, CIAO3, BTN3A3, ARFGEF1, BTN2A1, DDX58, SMOC1, TGM1, HPGDS, TLR4, SPINT1, TG, HLA-A, IL4R, IL2RA, IL2, IFNAR1, HLA-DRB5, HLA-DPB1, HDC, IL10, GCHFR, FCN2, CUX1, CD9, ANXA1, ALB, IL7R, IL12A, AURKA, OAS1, ST14, ABO, CCL14, SAG, RIT1, OPN1LW, NDUFS4, LTA, MUC1, MTX1, MS, MOG, MNAT1, MB, ERVK-32
-
Genetic Prion Disease
Gene_reviews
The three major phenotypes of genetic prion disease are genetic Creutzfeldt-Jakob disease (gCJD), fatal familial insomnia (FFI), and Gerstmann-Sträussler-Scheinker (GSS) syndrome. Although these phenotypes display overlapping clinical and pathologic features, recognition of these phenotypes can be useful when providing affected individuals and their families with information about the expected clinical course. ... The disease course ranges from a few months in gCJD and FFI to a few (up to 4, and in rare cases up to 10) years in GSS syndrome. Diagnosis/testing. The diagnosis of genetic prion disease is established in a proband with suggestive findings and a heterozygous PRNP pathogenic variant identified by molecular genetic testing. ... The disease course ranges from a few months in gCJD and FFI to a few (up to 4, and in rare cases up to 10) years in GSS syndrome. Table 2 provides information on the frequency of neurologic features in the most frequent genetic prion disease phenotypes that emerge during the disease course. ... Gerstmann-Sträussler-Scheinker (GSS) Syndrome The typical clinical manifestations are a rapidly progressive cerebellar syndrome with ataxia at onset followed by cognitive decline and other neurologic signs within a few weeks, or at most a few months. ... Tesar et al [2019], who used cluster analysis to address the clinical heterogeneity of GSS syndrome, reported the following four clinical phenotypes: Typical GSS syndrome with early ataxia, late dementia, and long disease duration (up to 4 years) GSS syndrome beginning with areflexia and paresthesias, and later ataxia and dementia Pure dementia GSS syndrome with early onset (age 35 years) with predominant dementia and late ataxia Creutzfeldt-Jakob disease-like GSS syndrome with dementia and ataxia at onset and rapid disease progression Genotype-Phenotype Correlations Although some PRNP pathogenic variants are associated with specific neuropathologic phenotypes (see Table 2), evidence also suggests that heterozygotes for the same variant in the same family may develop distinct clinicopathologic phenotypes [Cracco et al 2018].
-
Nfia-Related Disorder
Gene_reviews
Because individuals with such rearrangements (sometimes termed the chromosome 1p32-p31 deletion syndrome) have additional features, they are not the focus of this GeneReview and are described in Genetically Related Disorders. ... Nomenclature Early reports that identified deletions affecting NFIA referred to the phenotypic presentation as "chromosome 1p32-p31 deletion syndrome" or "chromosome 1p31 deletion." ... Acquired macrocephaly w/impaired intellectual development (OMIM 618286) NFIB AD Macrocephaly DD Minor dysmorphic features Brain malformations incl dysgenesis of corpus callosum Neurodevelopmental phenotypes No urinary tract defects (in affected individuals reported to date) Malan syndrome 2 (OMIM 614753) NFIX AD Macrocephaly Ventriculomegaly DD Brain malformations incl hypoplasia of corpus callosum Individuals w/Malan syndrome generally have an overgrowth phenotype. ... Because Sotos syndrome and Malan syndrome have overlapping features, Sotos syndrome is sometimes referred to as Sotos syndrome 1. 2. Malan syndrome is also referred to as Sotos syndrome 2.
-
Atp7a-Related Copper Transport Disorders
Gene_reviews
Summary Clinical characteristics. Menkes disease, occipital horn syndrome (OHS), and ATP7A -related distal motor neuropathy (DMN) are disorders of copper transport caused by pathogenic variants in ATP7A (encoding a copper-transporting ATPase). ... Serum Copper and Serum Ceruloplasmin Concentration in Males with Menkes Disease, Occipital Horn Syndrome, and ATP7A -Related Distal Motor Neuropathy View in own window Serum Concentration Menkes Disease 1 OHS ATP7A -Related DMN Normal Copper 0-55 µg/dL 40-80 µg/dL 80-100 µg/dL 70-150 µg/dL; (birth - 6 mos: 20-70 µg/dL) Ceruloplasmin 10-160 mg/L 110-240 mg/L 240-310 mg/L 200-450 mg/L; (birth - 6 mos: 50-220 mg/L) DMN = distal motor neuropathy; OHS = occipital horn syndrome 1. ... Pili torti are present. Occipital horn syndrome (OHS; X-linked cutis laxa). Intelligence is normal or slightly reduced. ... Nomenclature Menkes disease is also known as Menkes kinky hair syndrome or trichopoliodystrophy. Occipital horn syndrome was formerly known as X-linked cutis laxa. ... The differential diagnosis includes other infantile-onset neurodevelopmental syndromes: Biotinidase deficiency Organic acidurias Aminoacidurias Mitochondrial myopathies (See Mitochondrial Disorders Overview.)
-
Mog Antibody Disease
Wikipedia
PMID 26185777 . ^ Narayan, Ram N; Wang, Cynthia; Sguigna, Peter; Husari, Khalil; Greenberg, Benjamin (2019). "Atypical Anti-MOG syndrome with aseptic meningoencephalitis and pseudotumor cerebri-like presentations". ... "The clinical spectrum and incidence of anti-MOG-associated acquired demyelinating syndromes in children and adults" . Multiple Sclerosis Journal . 26 (7): 806–814. doi : 10.1177/1352458519845112 . ... "MOG-IgG in NMO and related disorders: a multicenter study of 50 patients. Part 1: Frequency, syndrome specificity, influence of disease activity, long-term course, association with AQP4-IgG, and origin" . ... PMID 27458601 . v t e Multiple sclerosis and other demyelinating diseases of the central nervous system Signs and symptoms Ataxia Depression Diplopia Dysarthria Dysphagia Fatigue Incontinence Nystagmus Optic neuritis Pain Uhthoff's phenomenon Investigations and diagnosis Multiple sclerosis diagnosis McDonald criteria Poser criteria Clinical Clinically isolated syndrome Expanded Disability Status Scale Serological and CSF Oligoclonal bands Radiological Radiologically isolated syndrome Lesional demyelinations of the central nervous system Dawson's fingers Approved [ by whom? ] treatment Management of multiple sclerosis Alemtuzumab Cladribine Dimethyl fumarate Fingolimod Glatiramer acetate Interferon beta-1a Interferon beta-1b Mitoxantrone Natalizumab Ocrelizumab Ozanimod Siponimod Teriflunomide Other treatments Former Daclizumab Multiple sclerosis research Demyleinating diseases Autoimmune Multiple sclerosis Neuromyelitis optica Diffuse myelinoclastic sclerosis Inflammatory Acute disseminated encephalomyelitis MOG antibody disease Balo concentric sclerosis Marburg acute multiple sclerosis Neuromyelitis optica Diffuse myelinoclastic sclerosis Tumefactive multiple sclerosis Experimental autoimmune encephalomyelitis Hereditary Adrenoleukodystrophy Alexander disease Canavan disease Krabbe disease Metachromatic leukodystrophy Pelizaeus–Merzbacher disease Leukoencephalopathy with vanishing white matter Megalencephalic leukoencephalopathy with subcortical cysts CAMFAK syndrome Other Central pontine myelinolysis Marchiafava–Bignami disease Mitochondrial DNA depletion syndrome Other List of multiple sclerosis organizations List of people with multiple sclerosis Multiple sclerosis drug pipeline Pathophysiology v t e Hypersensitivity and autoimmune diseases Type I / allergy / atopy ( IgE ) Foreign Atopic eczema Allergic urticaria Allergic rhinitis (Hay fever) Allergic asthma Anaphylaxis Food allergy common allergies include: Milk Egg Peanut Tree nut Seafood Soy Wheat Penicillin allergy Autoimmune Eosinophilic esophagitis Type II / ADCC IgM IgG Foreign Hemolytic disease of the newborn Autoimmune Cytotoxic Autoimmune hemolytic anemia Immune thrombocytopenic purpura Bullous pemphigoid Pemphigus vulgaris Rheumatic fever Goodpasture syndrome Guillain–Barré syndrome " Type V "/ receptor Graves' disease Myasthenia gravis Pernicious anemia Type III ( Immune complex ) Foreign Henoch–Schönlein purpura Hypersensitivity vasculitis Reactive arthritis Farmer's lung Post-streptococcal glomerulonephritis Serum sickness Arthus reaction Autoimmune Systemic lupus erythematosus Subacute bacterial endocarditis Rheumatoid arthritis Type IV / cell-mediated ( T cells ) Foreign Allergic contact dermatitis Mantoux test Autoimmune Diabetes mellitus type 1 Hashimoto's thyroiditis Multiple sclerosis Coeliac disease Giant-cell arteritis Postorgasmic illness syndrome Reactive arthritis GVHD Transfusion-associated graft versus host disease Unknown/ multiple Foreign Hypersensitivity pneumonitis Allergic bronchopulmonary aspergillosis Transplant rejection Latex allergy (I+IV) Autoimmune Sjögren syndrome Autoimmune hepatitis Autoimmune polyendocrine syndrome APS1 APS2 Autoimmune adrenalitis Systemic autoimmune disease
-
Mental Retardation, X-Linked, Syndromic, Turner Type
Omim
A number sign (#) is used with this entry because of evidence that the Turner type of X-linked syndromic mental retardation (MRXST) is caused by mutation in the HUWE1 gene (300697) on chromosome Xp11. ... Description Turner-type X-linked syndromic mental retardation (MRXST) is a neurodevelopmental disorder with a highly variable phenotype. ... Subsequently, HUWE1 mutations were found in patients with several other similar X-linked disorders, including Juberg-Marsidi syndrome and Brooks-Wisniewski-Brown syndrome, as well as nonspecific syndromic X-linked neurologic disorders with impaired intellectual development and additional features, thus indicating that they are all represent the same disorder. ... The initial clinical diagnosis was compatible with Say-Meyer syndrome (314320), although these patients were not part of the original family with that disorder. ... The patients initially had a clinical diagnosis compatible with Say-Meyer syndrome (314320), but were not part of the original family with that disorder.
-
Chylothorax
Wikipedia
Other conditions like tuberous sclerosis , congenital heart disease, trisomy 21 (Down syndrome) , Noonan syndrome , or Turner syndrome (missing X chromosome) are also possible causes of congenital chylothorax. Other, more rare causes of congenital chylothorax include Castleman's disease , yellow nail syndrome , Waldenström's macroglobulinemia , sarcoidosis , venous thrombosis , thoracic radiation , macroglobulinemia , amyloidosis , and a goiter . ... This causes the chyle to ooze extensively into the pleural cavity, leading to a chylothorax. In the case of yellow nail syndrome, or lymphedema, chylothorax is caused by hypoplasia or dilation of the lymph vessels. ... External links [ edit ] Classification D ICD - 10 : I89.8 , B74.9 with J91 ICD - 9-CM : 457.8 MeSH : D002916 DiseasesDB : 29612 SNOMED CT : 83035003 External resources eMedicine : med/381 v t e Cardiovascular disease (vessels) Arteries , arterioles and capillaries Inflammation Arteritis Aortitis Buerger's disease Peripheral artery disease Arteriosclerosis Atherosclerosis Foam cell Fatty streak Atheroma Intermittent claudication Critical limb ischemia Monckeberg's arteriosclerosis Arteriolosclerosis Hyaline Hyperplastic Cholesterol LDL Oxycholesterol Trans fat Stenosis Carotid artery stenosis Renal artery stenosis Other Aortoiliac occlusive disease Degos disease Erythromelalgia Fibromuscular dysplasia Raynaud's phenomenon Aneurysm / dissection / pseudoaneurysm torso : Aortic aneurysm Abdominal aortic aneurysm Thoracic aortic aneurysm Aneurysm of sinus of Valsalva Aortic dissection Aortic rupture Coronary artery aneurysm head / neck Intracranial aneurysm Intracranial berry aneurysm Carotid artery dissection Vertebral artery dissection Familial aortic dissection Vascular malformation Arteriovenous fistula Arteriovenous malformation Telangiectasia Hereditary hemorrhagic telangiectasia Vascular nevus Cherry hemangioma Halo nevus Spider angioma Veins Inflammation Phlebitis Venous thrombosis / Thrombophlebitis primarily lower limb Deep vein thrombosis abdomen Hepatic veno-occlusive disease Budd–Chiari syndrome May–Thurner syndrome Portal vein thrombosis Renal vein thrombosis upper limb / torso Mondor's disease Paget–Schroetter disease head Cerebral venous sinus thrombosis Post-thrombotic syndrome Varicose veins Gastric varices Portacaval anastomosis Caput medusae Esophageal varices Hemorrhoid Varicocele Other Chronic venous insufficiency Chronic cerebrospinal venous insufficiency Superior vena cava syndrome Inferior vena cava syndrome Venous ulcer Arteries or veins Angiopathy Macroangiopathy Microangiopathy Embolism Pulmonary embolism Cholesterol embolism Paradoxical embolism Thrombosis Vasculitis Blood pressure Hypertension Hypertensive heart disease Hypertensive emergency Hypertensive nephropathy Essential hypertension Secondary hypertension Renovascular hypertension Benign hypertension Pulmonary hypertension Systolic hypertension White coat hypertension Hypotension Orthostatic hypotension v t e Diseases of the respiratory system Upper RT (including URTIs , common cold ) Head sinuses Sinusitis nose Rhinitis Vasomotor rhinitis Atrophic rhinitis Hay fever Nasal polyp Rhinorrhea nasal septum Nasal septum deviation Nasal septum perforation Nasal septal hematoma tonsil Tonsillitis Adenoid hypertrophy Peritonsillar abscess Neck pharynx Pharyngitis Strep throat Laryngopharyngeal reflux (LPR) Retropharyngeal abscess larynx Croup Laryngomalacia Laryngeal cyst Laryngitis Laryngopharyngeal reflux (LPR) Laryngospasm vocal cords Laryngopharyngeal reflux (LPR) Vocal fold nodule Vocal fold paresis Vocal cord dysfunction epiglottis Epiglottitis trachea Tracheitis Laryngotracheal stenosis Lower RT / lung disease (including LRTIs ) Bronchial / obstructive acute Acute bronchitis chronic COPD Chronic bronchitis Acute exacerbation of COPD ) Asthma ( Status asthmaticus Aspirin-induced Exercise-induced Bronchiectasis Cystic fibrosis unspecified Bronchitis Bronchiolitis Bronchiolitis obliterans Diffuse panbronchiolitis Interstitial / restrictive ( fibrosis ) External agents/ occupational lung disease Pneumoconiosis Aluminosis Asbestosis Baritosis Bauxite fibrosis Berylliosis Caplan's syndrome Chalicosis Coalworker's pneumoconiosis Siderosis Silicosis Talcosis Byssinosis Hypersensitivity pneumonitis Bagassosis Bird fancier's lung Farmer's lung Lycoperdonosis Other ARDS Combined pulmonary fibrosis and emphysema Pulmonary edema Löffler's syndrome / Eosinophilic pneumonia Respiratory hypersensitivity Allergic bronchopulmonary aspergillosis Hamman-Rich syndrome Idiopathic pulmonary fibrosis Sarcoidosis Vaping-associated pulmonary injury Obstructive / Restrictive Pneumonia / pneumonitis By pathogen Viral Bacterial Pneumococcal Klebsiella Atypical bacterial Mycoplasma Legionnaires' disease Chlamydiae Fungal Pneumocystis Parasitic noninfectious Chemical / Mendelson's syndrome Aspiration / Lipid By vector/route Community-acquired Healthcare-associated Hospital-acquired By distribution Broncho- Lobar IIP UIP DIP BOOP-COP NSIP RB Other Atelectasis circulatory Pulmonary hypertension Pulmonary embolism Lung abscess Pleural cavity / mediastinum Pleural disease Pleuritis/pleurisy Pneumothorax / Hemopneumothorax Pleural effusion Hemothorax Hydrothorax Chylothorax Empyema/pyothorax Malignant Fibrothorax Mediastinal disease Mediastinitis Mediastinal emphysema Other/general Respiratory failure Influenza Common cold SARS Coronavirus disease 2019 Idiopathic pulmonary haemosiderosis Pulmonary alveolar proteinosis
-
Female Sexual Arousal Disorder
Wikipedia
Please help to improve this article by introducing more precise citations. ( February 2013 ) ( Learn how and when to remove this template message ) Female sexual arousal disorder Other names Candace syndrome, [1] female sexual interest/arousal disorder Specialty Psychiatry , gynaecology Female sexual arousal disorder ( FSAD ) is a disorder characterized by a persistent or recurrent inability to attain sexual arousal or to maintain arousal until the completion of a sexual activity . ... Archived from the original on 2007-04-26. v t e Female diseases of the pelvis and genitals Internal Adnexa Ovary Endometriosis of ovary Female infertility Anovulation Poor ovarian reserve Mittelschmerz Oophoritis Ovarian apoplexy Ovarian cyst Corpus luteum cyst Follicular cyst of ovary Theca lutein cyst Ovarian hyperstimulation syndrome Ovarian torsion Fallopian tube Female infertility Fallopian tube obstruction Hematosalpinx Hydrosalpinx Salpingitis Uterus Endometrium Asherman's syndrome Dysfunctional uterine bleeding Endometrial hyperplasia Endometrial polyp Endometriosis Endometritis Menstruation Flow Amenorrhoea Hypomenorrhea Oligomenorrhea Pain Dysmenorrhea PMS Timing Menometrorrhagia Menorrhagia Metrorrhagia Female infertility Recurrent miscarriage Myometrium Adenomyosis Parametrium Parametritis Cervix Cervical dysplasia Cervical incompetence Cervical polyp Cervicitis Female infertility Cervical stenosis Nabothian cyst General Hematometra / Pyometra Retroverted uterus Vagina Hematocolpos / Hydrocolpos Leukorrhea / Vaginal discharge Vaginitis Atrophic vaginitis Bacterial vaginosis Candidal vulvovaginitis Hydrocolpos Sexual dysfunction Dyspareunia Hypoactive sexual desire disorder Sexual arousal disorder Vaginismus Urogenital fistulas Ureterovaginal Vesicovaginal Obstetric fistula Rectovaginal fistula Prolapse Cystocele Enterocele Rectocele Sigmoidocele Urethrocele Vaginal bleeding Postcoital bleeding Other / general Pelvic congestion syndrome Pelvic inflammatory disease External Vulva Bartholin's cyst Kraurosis vulvae Vestibular papillomatosis Vulvitis Vulvodynia Clitoral hood or clitoris Persistent genital arousal disorder v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Sucrose Intolerance
Wikipedia
Sucrose intolerance can also be caused by irritable bowel syndrome , aging, or small intestine disease (secondary sucrose intolerance). ... External links [ edit ] Congenital sucrase-isomaltase deficiency , US National Library of Medicine What is sucrose intolerance , sucroseintolerance.com Classification D ICD - 10 : E74.3 ICD - 9-CM : 271.3 OMIM : 222900 MeSH : C538139 DiseasesDB : 29844 v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum v t e Inborn error of carbohydrate metabolism : monosaccharide metabolism disorders Including glycogen storage diseases (GSD) Sucrose , transport (extracellular) Disaccharide catabolism Congenital alactasia Sucrose intolerance Monosaccharide transport Glucose-galactose malabsorption Inborn errors of renal tubular transport ( Renal glycosuria ) Fructose malabsorption Hexose → glucose Monosaccharide catabolism Fructose : Essential fructosuria Fructose intolerance Galactose / galactosemia : GALK deficiency GALT deficiency / GALE deficiency Glucose ⇄ glycogen Glycogenesis GSD type 0 (glycogen synthase deficiency) GSD type IV (Andersen's disease, branching enzyme deficiency) Adult polyglucosan body disease (APBD) Glycogenolysis Extralysosomal: GSD type III (Cori's disease, debranching enzyme deficiency) GSD type VI (Hers' disease, liver glycogen phosphorylase deficiency) GSD type V (McArdle's disease, myophosphorylase deficiency) GSD type IX (phosphorylase kinase deficiency) Lysosomal ( LSD ): GSD type II (Pompe's disease, glucosidase deficiency) Glucose ⇄ CAC Glycolysis MODY 2 / HHF3 GSD type VII (Tarui's disease, phosphofructokinase deficiency) Triosephosphate isomerase deficiency Pyruvate kinase deficiency Gluconeogenesis PCD Fructose bisphosphatase deficiency GSD type I (von Gierke's disease, glucose 6-phosphatase deficiency) Pentose phosphate pathway Glucose-6-phosphate dehydrogenase deficiency Transaldolase deficiency 6-phosphogluconate dehydrogenase deficiency Other Hyperoxaluria Primary hyperoxaluria Pentosuria Aldolase A deficiency
-
Anal Fissure
Wikipedia
When fissures are found laterally, tuberculosis, occult abscesses, leukemic infiltrates, carcinoma, acquired immunodeficiency syndrome (AIDS) or inflammatory bowel disease should be considered as causes. [2] Some sexually transmitted infections can promote the breakdown of tissue resulting in a fissure. ... External links [ edit ] Classification D ICD - 10 : K60.0 - K60.2 ICD - 9-CM : 565.0 MeSH : D005401 DiseasesDB : 673 External resources MedlinePlus : 001130 eMedicine : med/3532 ped/2938 emerg/495 Wikimedia Commons has media related to Anal fissure . https://columbiasurgery.org/news/2014/04/01/new-protocol-treat-anal-fissures v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum
-
Indigestion
Wikipedia
It has been noted that one of the most frustrating aspects of treating functional dyspepsia is that these traditional agents have been shown to have little or no efficacy. [21] Acid suppression [ edit ] Antacids and sucralfate were found to be no better than placebo in a literature review. [22] H2-RAs have been shown to have marked benefit in poor quality trials (30% relative risk reduction [22] ), but only a marginal benefit in good quality trials. [21] Prokinetic agents would empirically seem to work well since delayed gastric emptying is considered a major pathophysiological mechanism in functional dyspepsia. [21] They have been shown in a meta-analysis to produce a relative risk reduction of up to 50%, but the studies evaluated to come to this conclusion used the drug cisapride which has since been removed from the market (now only available as an investigational agent) [23] due to serious adverse events such as torsades , and publication bias has been cited as a potential partial explanation for such a high benefit. [22] Modern prokinetic agents such as metoclopramide, erythromycin and tegaserod have little or no established efficacy and often result in substantial side effects. [22] Simethicone is of some value, as one trial suggests potential benefit over placebo and another shows equivalence with cisapride. [22] So, with the somewhat recent advent of the proton pump inhibitor (PPI) class of medications, the question of whether these new agents are superior to traditional therapy has arisen. [ citation needed ] Currently, PPIs are, depending on the specific drug, FDA indicated for erosive esophagitis , gastroesophageal reflux disease (GERD), Zollinger-Ellison syndrome , eradication of H. pylori, duodenal and gastric ulcers, and NSAID-induced ulcer healing and prevention, but not functional dyspepsia. ... External links [ edit ] Classification D ICD - 10 : K30 ICD - 9-CM : 536.8 MeSH : D004415 DiseasesDB : 30831 External resources MedlinePlus : 003260 Patient UK : Indigestion Look up indigestion in Wiktionary, the free dictionary. v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum PneumoperitoneumIFNG, CRH, GNB3, SLC6A4, TRPV1, S100A8, GAST, IL1B, ATP12A, CYP2C19, SSTR3, MIF, ATP4A, IL1RN, TNF, TPH1, TGFB1, SYMPK, SEMA4D, TP53, AGA, CELA3B, KCNIP3, SCN10A, UGT1A9, CHD7, CYSLTR2, IL17F, SLCO6A1, VMA21, GSTK1, MIR325, GGTLC5P, GGTLC3, GGT2, FOXP3, SLC26A4, PTGS2, PTGS1, CD14, CHGA, COMT, CTBP1, CYBA, DECR1, FAP, FHIT, GABPA, GGT1, PRLHR, HLA-DQB1, HP, HTR3A, IL17A, MCM5, NFE2L2, SERPINE1, SERPINB2, PPY, PTGDS, GGTLC4P
-
Combined Oxidative Phosphorylation Deficiency 15
Omim
Echocardiography showed short PR waves and delta waves consistent with Wolff-Parkinson-White syndrome. At age 21 years, she worked a menial job. ... That patient had global developmental delay, optic atrophy, impaired vision, pyramidal tract signs, incoordination, and Wolff-Parkinson-White syndrome. In a second family, a girl was first evaluated for obesity at age 5 years and was found to have a pituitary adenoma. ... Brain MRI showed mild signal abnormalities in the dorsal periventricular white matter and increased T2-weighted signal intensities in the caudate and putamen, consistent with Leigh syndrome (256000). The younger sister, aged 6 years, had short stature and mild intention tremor, but no ataxia. ... Seven patients had abnormal increased T2-weighted signal abnormalities in the basal ganglia and/or midbrain, consistent with classic Leigh syndrome, and some had additional subcortical white matter lesions. ... INHERITANCE - Autosomal recessive GROWTH Height - Short stature (in some patients) Weight - Obesity (in some patients) HEAD & NECK Head - Microcephaly (in some patients) Eyes - Decreased visual acuity (in some patients) - Strabismus (in some patients) - Optic atrophy (in some patients) - Nystagmus (in some patients) CARDIOVASCULAR Heart - Wolff-Parkinson-White syndrome (in some patients) - Ventricular septal hypertrophy (in some patients) - Ventricular septal defect (in some patients) MUSCLE, SOFT TISSUES - Hypotonia (in some patients) NEUROLOGIC Central Nervous System - Global developmental delay - Reading difficulties - Speech difficulties - Incoordination - Cognitive impairment - Ataxia - Gait instability - Pyramidal tract signs (in some patients) - Tremor (in some patients) - Seizures (rare) - T2-weighted hyperintensities in the basal ganglia, corpus callosum, and brainstem seen on MRI - Leigh syndrome - Subcortical white matter abnormalities LABORATORY ABNORMALITIES - Increased CSF lactate - Increased serum lactate (in some patients) - Patient fibroblasts and muscle show decreased activities of mitochondrial complexes I, III, and IV - Impaired mitochondrial translation MISCELLANEOUS - Highly variable phenotype - Onset in childhood MOLECULAR BASIS - Caused by mutation in the mitochondrial methionyl-tRNA formyltransferase gene (MTFMT, 611766.0001 ) ▲ Close
-
Baker's Cyst
Wikipedia
Baker's cyst Other names Popliteal cyst [1] Ultrasound image of Baker's cyst Specialty Rheumatology Symptoms None, swelling behind the knee, stiffness, pain [1] [2] Complications Deep vein thrombosis , peripheral neuropathy , ischemia , compartment syndrome [2] [3] Usual onset Gradual [1] Risk factors Knee problems such as osteoarthritis , meniscal tears , rheumatoid arthritis [1] [3] [4] Diagnostic method Confirmed by ultrasound or MRI [3] Differential diagnosis Deep venous thrombosis , aneurysms , ganglion , tumors [1] Treatment Supportive care , aspiration , surgery [1] Frequency c. 20% [2] [3] A Baker's cyst , also known as a popliteal cyst , is a type of fluid collection behind the knee . [4] Often there are no symptoms. [2] If symptoms do occur these may include swelling and pain behind the knee, or knee stiffness. [1] If the cyst breaks open, pain may significantly increase with swelling of the calf. [1] Rarely complications such as deep vein thrombosis , peripheral neuropathy , ischemia , or compartment syndrome may occur. [2] [3] Risk factors include other knee problems such as osteoarthritis , meniscal tears , or rheumatoid arthritis . [1] [3] [4] The underlying mechanism involves the flow of synovial fluid from the knee joint to the gastrocnemio-semimembranosus bursa , resulting in its expansion. [1] The diagnosis may be confirmed with ultrasound or magnetic resonance imaging (MRI). [3] Treatment is initially with supportive care . [1] If this is not effective aspiration and steroid injection or surgical removal may be carried out. [1] Around 20% of people have a Baker's cyst. [2] [3] They occur most commonly in those 35 to 70 years old. [4] It is named after the surgeon who first described it, William Morrant Baker (1838–1896). [5] Contents 1 Signs and symptoms 2 Cause 3 Diagnosis 4 Treatment 4.1 Exercise 5 References 6 External links Signs and symptoms [ edit ] Symptoms may include swelling behind the knee, stiffness, and pain. [1] If the cyst breaks open, pain may increase, and there may be swelling of the calf. [1] Rupture of a Baker's cyst may also cause bruising below the medial malleolus of the ankle (Crescent sign). ... External links [ edit ] Media related to Baker's cyst at Wikimedia Commons Classification D ICD - 10 : M71.2 ICD - 9-CM : 727.51 MeSH : D011151 DiseasesDB : 1224 External resources MedlinePlus : 001222 eMedicine : radio/72 Patient UK : Baker's cyst v t e Soft tissue disorders Capsular joint Synoviopathy Synovitis / Tenosynovitis Calcific tendinitis Stenosing tenosynovitis Trigger finger De Quervain syndrome Transient synovitis Ganglion cyst osteochondromatosis Synovial osteochondromatosis Plica syndrome villonodular synovitis Giant-cell tumor of the tendon sheath Bursopathy Bursitis Olecranon Prepatellar Trochanteric Subacromial Achilles Retrocalcaneal Ischial Iliopsoas Synovial cyst Baker's cyst Calcific bursitis Noncapsular joint Symptoms Ligamentous laxity Hypermobility Enthesopathy / Enthesitis / Tendinopathy upper limb Adhesive capsulitis of shoulder Impingement syndrome Rotator cuff tear Golfer's elbow Tennis elbow lower limb Iliotibial band syndrome Patellar tendinitis Achilles tendinitis Calcaneal spur Metatarsalgia Bone spur other/general: Tendinitis / Tendinosis Nonjoint Fasciopathy Fasciitis : Plantar Nodular Necrotizing Eosinophilic Fibromatosis / contracture Dupuytren's contracture Plantar fibromatosis Aggressive fibromatosis Knuckle pads