-
Childhood Blindness
Wikipedia
External links [ edit ] Classification D ICD - 9-CM : 369.00 External resources Patient UK : Childhood blindness Scholia has a topic profile for Childhood blindness . v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
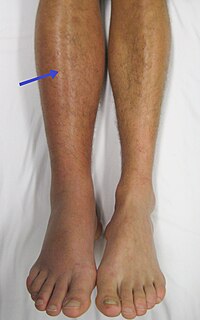
Ainhum
Wikipedia
Ainhum has been much confused with similar constrictions caused by other diseases such as leprosy , diabetic gangrene , syringomyelia , scleroderma or Vohwinkel syndrome . In this case, it is called pseudo-ainhum , treatable with minor surgery or intralesional corticosteroids, as with ainhum. [3] It has even been seen in psoriasis or it is acquired by the wrapping toes, penis or nipple with hairs, threads or fibers. [4] Oral retinoids, such as tretinoin, and antifibrotic agents like tranilast have been tested for pseudo-ainhum. [2] Impending amputation in Vohwinkel syndrome can sometimes be aborted by therapy with oral etretinate. [4] It is rarely seen in the United States but often discussed in the international medical literature. [5] Prevention [ edit ] Wearing shoes to protect barefoot trauma has shown decrease in incidence in ainhum. ... External links [ edit ] Classification D ICD - 10 : L94.6 ICD - 9-CM : 136.0 OMIM : 103400 MeSH : D000387 DiseasesDB : 29442 External resources eMedicine : derm/594 v t e Cutaneous keratosis, ulcer, atrophy, and necrobiosis Epidermal thickening keratoderma : Keratoderma climactericum Paraneoplastic keratoderma Acrokeratosis paraneoplastica of Bazex Aquagenic keratoderma Drug-induced keratoderma psoriasis Keratoderma blennorrhagicum keratosis : Seborrheic keratosis Clonal seborrheic keratosis Common seborrheic keratosis Irritated seborrheic keratosis Seborrheic keratosis with squamous atypia Reticulated seborrheic keratosis Dermatosis papulosa nigra Keratosis punctata of the palmar creases other hyperkeratosis : Acanthosis nigricans Confluent and reticulated papillomatosis Callus Ichthyosis acquisita Arsenical keratosis Chronic scar keratosis Hyperkeratosis lenticularis perstans Hydrocarbon keratosis Hyperkeratosis of the nipple and areola Inverted follicular keratosis Lichenoid keratosis Multiple minute digitate hyperkeratosis PUVA keratosis Reactional keratosis Stucco keratosis Thermal keratosis Viral keratosis Warty dyskeratoma Waxy keratosis of childhood other hypertrophy: Keloid Hypertrophic scar Cutis verticis gyrata Necrobiosis / granuloma Necrobiotic/palisading Granuloma annulare Perforating Generalized Subcutaneous Granuloma annulare in HIV disease Localized granuloma annulare Patch-type granuloma annulare Necrobiosis lipoidica Annular elastolytic giant-cell granuloma Granuloma multiforme Necrobiotic xanthogranuloma Palisaded neutrophilic and granulomatous dermatitis Rheumatoid nodulosis Interstitial granulomatous dermatitis / Interstitial granulomatous drug reaction Foreign body granuloma Beryllium granuloma Mercury granuloma Silica granuloma Silicone granuloma Zirconium granuloma Soot tattoo Tattoo Carbon stain Other/ungrouped eosinophilic dermatosis Granuloma faciale Dermis / localized CTD Cutaneous lupus erythematosus chronic: Discoid Panniculitis subacute : Neonatal ungrouped: Chilblain Lupus erythematosus–lichen planus overlap syndrome Tumid Verrucous Rowell's syndrome Scleroderma / Morphea Localized scleroderma Localized morphea Morphea–lichen sclerosus et atrophicus overlap Generalized morphea Atrophoderma of Pasini and Pierini Pansclerotic morphea Morphea profunda Linear scleroderma Atrophic / atrophoderma Lichen sclerosus Anetoderma Schweninger–Buzzi anetoderma Jadassohn–Pellizzari anetoderma Atrophoderma of Pasini and Pierini Acrodermatitis chronica atrophicans Semicircular lipoatrophy Follicular atrophoderma Linear atrophoderma of Moulin Perforating Kyrle disease Reactive perforating collagenosis Elastosis perforans serpiginosa Perforating folliculitis Acquired perforating dermatosis Skin ulcer Pyoderma gangrenosum Other Calcinosis cutis Sclerodactyly Poikiloderma vasculare atrophicans Ainhum / Pseudo-ainhum v t e Bone and joint disease Bone Inflammation endocrine : Osteitis fibrosa cystica Brown tumor infection : Osteomyelitis Sequestrum Involucrum Sesamoiditis Brodie abscess Periostitis Vertebral osteomyelitis Metabolic Bone density Osteoporosis Juvenile Osteopenia Osteomalacia Paget's disease of bone Hypophosphatasia Bone resorption Osteolysis Hajdu–Cheney syndrome Ainhum Gorham's disease Other Ischaemia Avascular necrosis Osteonecrosis of the jaw Complex regional pain syndrome Hypertrophic pulmonary osteoarthropathy Nonossifying fibroma Pseudarthrosis Stress fracture Fibrous dysplasia Monostotic Polyostotic Skeletal fluorosis bone cyst Aneurysmal bone cyst Hyperostosis Infantile cortical hyperostosis Osteosclerosis Melorheostosis Pycnodysostosis Joint Chondritis Relapsing polychondritis Other Tietze's syndrome Combined Osteochondritis Osteochondritis dissecans Child leg: hip Legg–Calvé–Perthes syndrome tibia Osgood–Schlatter disease Blount's disease foot Köhler disease Sever's disease spine Scheuermann's_disease arm: wrist Kienböck's disease elbow Panner disease
-
Maxillary Lateral Incisor Agenesis
Wikipedia
MSX1 consist of homeobox encoding sequence of 60 amino acid long DNA binding homeodomain. [5] The protein of MSX1 serves as a repressor for gene transcription and interchanges with other homeoproteins. [5] In studies of homozygous mice, it has been found that deletion of the MSX1 gene has resulted in a double cleft palate, deficiency of the alveolar bone, failure of incisor and molar development. [5] PAX9 [ edit ] PAX9 also plays a key role during embryogenesis. [5] In addition, encoded proteins by PAX9 genes have a 128 amino acid long DNA binding paired domain. [5] Studies suggest that all heterozygous mutations of PAX9 associated with lack of development were due to the loss of function in one of the protein copies, which resulted in haploinsufficiency . [5] Furthermore, mutations of other genes have been identified in syndromes and congenital abnormalities in which tooth agenesis is a regular characteristic. [6] Endogamy [ edit ] There have been studies that entail that a possible reason for maxillary lateral incisor agenesis was due to endogamy . ... PMID 20123092 . ^ a b c d e f Mostowska A, Kobielak A, Trzeciak WH (October 2003). "Molecular basis of non-syndromic tooth agenesis: mutations of MSX1 and PAX9 reflect their role in patterning human dentition". ... Retrieved 20 June 2013 . v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Diplopodia
Wikipedia
Comptes rendus de l'Académie des Sciences . 252 : 1863–1865. v t e Congenital malformations and deformations of musculoskeletal system / musculoskeletal abnormality Appendicular limb / dysmelia Arms clavicle / shoulder Cleidocranial dysostosis Sprengel's deformity Wallis–Zieff–Goldblatt syndrome hand deformity Madelung's deformity Clinodactyly Oligodactyly Polydactyly Leg hip Hip dislocation / Hip dysplasia Upington disease Coxa valga Coxa vara knee Genu valgum Genu varum Genu recurvatum Discoid meniscus Congenital patellar dislocation Congenital knee dislocation foot deformity varus Club foot Pigeon toe valgus Flat feet Pes cavus Rocker bottom foot Hammer toe Either / both fingers and toes Polydactyly / Syndactyly Webbed toes Arachnodactyly Cenani–Lenz syndactylism Ectrodactyly Brachydactyly Stub thumb reduction deficits / limb Acheiropodia Ectromelia Phocomelia Amelia Hemimelia multiple joints Arthrogryposis Larsen syndrome RAPADILINO syndrome Axial Skull and face Craniosynostosis Scaphocephaly Oxycephaly Trigonocephaly Craniofacial dysostosis Crouzon syndrome Hypertelorism Hallermann–Streiff syndrome Treacher Collins syndrome other Macrocephaly Platybasia Craniodiaphyseal dysplasia Dolichocephaly Greig cephalopolysyndactyly syndrome Plagiocephaly Saddle nose Vertebral column Spinal curvature Scoliosis Klippel–Feil syndrome Spondylolisthesis Spina bifida occulta Sacralization Thoracic skeleton ribs : Cervical Bifid sternum : Pectus excavatum Pectus carinatum
-
Neonatal Herpes Simplex
Wikipedia
External links [ edit ] Classification D ICD - 10 : P35.2 ICD - 9-CM : 771.2 , 054.xx External resources eMedicine : article/964866 v t e Infectious diseases – viral systemic diseases Oncovirus DNA virus HBV Hepatocellular carcinoma HPV Cervical cancer Anal cancer Penile cancer Vulvar cancer Vaginal cancer Oropharyngeal cancer KSHV Kaposi's sarcoma EBV Nasopharyngeal carcinoma Burkitt's lymphoma Hodgkin lymphoma Follicular dendritic cell sarcoma Extranodal NK/T-cell lymphoma, nasal type MCPyV Merkel-cell carcinoma RNA virus HCV Hepatocellular carcinoma Splenic marginal zone lymphoma HTLV-I Adult T-cell leukemia/lymphoma Immune disorders HIV AIDS Central nervous system Encephalitis / meningitis DNA virus Human polyomavirus 2 Progressive multifocal leukoencephalopathy RNA virus MeV Subacute sclerosing panencephalitis LCV Lymphocytic choriomeningitis Arbovirus encephalitis Orthomyxoviridae (probable) Encephalitis lethargica RV Rabies Chandipura vesiculovirus Herpesviral meningitis Ramsay Hunt syndrome type 2 Myelitis Poliovirus Poliomyelitis Post-polio syndrome HTLV-I Tropical spastic paraparesis Eye Cytomegalovirus Cytomegalovirus retinitis HSV Herpes of the eye Cardiovascular CBV Pericarditis Myocarditis Respiratory system / acute viral nasopharyngitis / viral pneumonia DNA virus Epstein–Barr virus EBV infection / Infectious mononucleosis Cytomegalovirus RNA virus IV : Human coronavirus 229E / NL63 / HKU1 / OC43 Common cold MERS coronavirus Middle East respiratory syndrome SARS coronavirus Severe acute respiratory syndrome SARS coronavirus 2 Coronavirus disease 2019 V , Orthomyxoviridae : Influenza virus A / B / C / D Influenza / Avian influenza V, Paramyxoviridae : Human parainfluenza viruses Parainfluenza Human orthopneumovirus hMPV Human digestive system Pharynx / Esophagus MuV Mumps Cytomegalovirus Cytomegalovirus esophagitis Gastroenteritis / diarrhea DNA virus Adenovirus Adenovirus infection RNA virus Rotavirus Norovirus Astrovirus Coronavirus Hepatitis DNA virus HBV ( B ) RNA virus CBV HAV ( A ) HCV ( C ) HDV ( D ) HEV ( E ) HGV ( G ) Pancreatitis CBV Urogenital BK virus MuV Mumps v t e Conditions originating in the perinatal period / fetal disease Maternal factors complicating pregnancy, labour or delivery placenta Placenta praevia Placental insufficiency Twin-to-twin transfusion syndrome chorion / amnion Chorioamnionitis umbilical cord Umbilical cord prolapse Nuchal cord Single umbilical artery presentation Breech birth Asynclitism Shoulder presentation Growth Small for gestational age / Large for gestational age Preterm birth / Postterm pregnancy Intrauterine growth restriction Birth trauma scalp Cephalohematoma Chignon Caput succedaneum Subgaleal hemorrhage Brachial plexus injury Erb's palsy Klumpke paralysis Affected systems Respiratory Intrauterine hypoxia Infant respiratory distress syndrome Transient tachypnea of the newborn Meconium aspiration syndrome Pleural disease Pneumothorax Pneumomediastinum Wilson–Mikity syndrome Bronchopulmonary dysplasia Cardiovascular Pneumopericardium Persistent fetal circulation Bleeding and hematologic disease Vitamin K deficiency bleeding HDN ABO Anti-Kell Rh c Rh D Rh E Hydrops fetalis Hyperbilirubinemia Kernicterus Neonatal jaundice Velamentous cord insertion Intraventricular hemorrhage Germinal matrix hemorrhage Anemia of prematurity Gastrointestinal Ileus Necrotizing enterocolitis Meconium peritonitis Integument and thermoregulation Erythema toxicum Sclerema neonatorum Nervous system Perinatal asphyxia Periventricular leukomalacia Musculoskeletal Gray baby syndrome muscle tone Congenital hypertonia Congenital hypotonia Infections Vertically transmitted infection Neonatal infection rubella herpes simplex mycoplasma hominis ureaplasma urealyticum Omphalitis Neonatal sepsis Group B streptococcal infection Neonatal conjunctivitis Other Miscarriage Perinatal mortality Stillbirth Infant mortality Neonatal withdrawal v t e Vertically transmitted infections Gestational Viruses Congenital rubella syndrome Congenital cytomegalovirus infection Neonatal herpes simplex Hepatitis B Congenital varicella syndrome HIV Fifth disease Bacteria Congenital syphilis Other Toxoplasmosis transplacental TORCH complex During birth transcervical Candidiasis Gonorrhea Listeriosis Late pregnancy Listeriosis Congenital cytomegalovirus infection By breastfeeding Breastfeeding Tuberculosis HIV
-
Stimulant Psychosis
Wikipedia
See also [ edit ] Amphetamine Delusional parasitosis Dopamine hypothesis of psychosis Excited delirium Psychosis Substance-induced psychosis Neuroleptic malignant syndrome References [ edit ] ^ a b World Health Organization (2018). ... PMID 15732884 . ^ "White Paper Report on Excited Delirium Syndrome" , ACEP Excited Delirium Task Force, American College of Emergency Physicians , 10 September 2009 ^ Murrie, Benjamin; Lappin, Julia; Large, Matthew; Sara, Grant (16 October 2019). ... External links [ edit ] Classification D ICD - 10 : F14 .5 & F15 .5 ICD - 9-CM : 292.1 v t e Psychoactive substance-related disorder General SID Substance intoxication / Drug overdose Substance-induced psychosis Withdrawal : Craving Neonatal withdrawal Post-acute-withdrawal syndrome (PAWS) SUD Substance abuse / Substance-related disorders Physical dependence / Psychological dependence / Substance dependence Combined substance use SUD Polysubstance dependence SID Combined drug intoxication (CDI) Alcohol SID Cardiovascular diseases Alcoholic cardiomyopathy Alcohol flush reaction (AFR) Gastrointestinal diseases Alcoholic liver disease (ALD): Alcoholic hepatitis Auto-brewery syndrome (ABS) Endocrine diseases Alcoholic ketoacidosis (AKA) Nervous system diseases Alcohol-related dementia (ARD) Alcohol intoxication Hangover Neurological disorders Alcoholic hallucinosis Alcoholic polyneuropathy Alcohol-related brain damage Alcohol withdrawal syndrome (AWS): Alcoholic hallucinosis Delirium tremens (DTs) Fetal alcohol spectrum disorder (FASD) Fetal alcohol syndrome (FAS) Korsakoff syndrome Positional alcohol nystagmus (PAN) Wernicke–Korsakoff syndrome (WKS, Korsakoff psychosis) Wernicke encephalopathy (WE) Respiratory tract diseases Alcohol-induced respiratory reactions Alcoholic lung disease SUD Alcoholism (alcohol use disorder (AUD)) Binge drinking Caffeine SID Caffeine-induced anxiety disorder Caffeine-induced sleep disorder Caffeinism SUD Caffeine dependence Cannabis SID Cannabis arteritis Cannabinoid hyperemesis syndrome (CHS) SUD Amotivational syndrome Cannabis use disorder (CUD) Synthetic cannabinoid use disorder Cocaine SID Cocaine intoxication Prenatal cocaine exposure (PCE) SUD Cocaine dependence Hallucinogen SID Acute intoxication from hallucinogens (bad trip) Hallucinogen persisting perception disorder (HPPD) Nicotine SID Nicotine poisoning Nicotine withdrawal SUD Nicotine dependence Opioids SID Opioid overdose SUD Opioid use disorder (OUD) Sedative / hypnotic SID Kindling (sedative–hypnotic withdrawal) benzodiazepine : SID Benzodiazepine overdose Benzodiazepine withdrawal SUD Benzodiazepine use disorder (BUD) Benzodiazepine dependence barbiturate : SID Barbiturate overdose SUD Barbiturate dependence Stimulants SID Stimulant psychosis amphetamine : SUD Amphetamine dependence Volatile solvent SID Sudden sniffing death syndrome (SSDS) Toluene toxicity SUD Inhalant abuse
-
Intermittent Explosive Disorder
Wikipedia
The text also clarified the disorder's relationship to other disorders such as ADHD and disruptive mood dysregulation disorder . [24] See also [ edit ] Episodic dyscontrol syndrome Passive–aggressive personality disorder References [ edit ] ^ a b c McElroy SL (1999). ... External links [ edit ] Classification D ICD - 10 : F63.8 ICD - 9-CM : 312.34 v t e Mental and behavioral disorders Adult personality and behavior Gender dysphoria Ego-dystonic sexual orientation Paraphilia Fetishism Voyeurism Sexual maturation disorder Sexual relationship disorder Other Factitious disorder Munchausen syndrome Intermittent explosive disorder Dermatillomania Kleptomania Pyromania Trichotillomania Personality disorder Childhood and learning Emotional and behavioral ADHD Conduct disorder ODD Emotional and behavioral disorders Separation anxiety disorder Movement disorders Stereotypic Social functioning DAD RAD Selective mutism Speech Stuttering Cluttering Tic disorder Tourette syndrome Intellectual disability X-linked intellectual disability Lujan–Fryns syndrome Psychological development ( developmental disabilities ) Pervasive Specific Mood (affective) Bipolar Bipolar I Bipolar II Bipolar NOS Cyclothymia Depression Atypical depression Dysthymia Major depressive disorder Melancholic depression Seasonal affective disorder Mania Neurological and symptomatic Autism spectrum Autism Asperger syndrome High-functioning autism PDD-NOS Savant syndrome Dementia AIDS dementia complex Alzheimer's disease Creutzfeldt–Jakob disease Frontotemporal dementia Huntington's disease Mild cognitive impairment Parkinson's disease Pick's disease Sundowning Vascular dementia Wandering Other Delirium Organic brain syndrome Post-concussion syndrome Neurotic , stress -related and somatoform Adjustment Adjustment disorder with depressed mood Anxiety Phobia Agoraphobia Social anxiety Social phobia Anthropophobia Specific social phobia Specific phobia Claustrophobia Other Generalized anxiety disorder OCD Panic attack Panic disorder Stress Acute stress reaction PTSD Dissociative Depersonalization disorder Dissociative identity disorder Fugue state Psychogenic amnesia Somatic symptom Body dysmorphic disorder Conversion disorder Ganser syndrome Globus pharyngis Psychogenic non-epileptic seizures False pregnancy Hypochondriasis Mass psychogenic illness Nosophobia Psychogenic pain Somatization disorder Physiological and physical behavior Eating Anorexia nervosa Bulimia nervosa Rumination syndrome Other specified feeding or eating disorder Nonorganic sleep Hypersomnia Insomnia Parasomnia Night terror Nightmare REM sleep behavior disorder Postnatal Postpartum depression Postpartum psychosis Sexual dysfunction Arousal Erectile dysfunction Female sexual arousal disorder Desire Hypersexuality Hypoactive sexual desire disorder Orgasm Anorgasmia Delayed ejaculation Premature ejaculation Sexual anhedonia Pain Nonorganic dyspareunia Nonorganic vaginismus Psychoactive substances, substance abuse and substance-related Drug overdose Intoxication Physical dependence Rebound effect Stimulant psychosis Substance dependence Withdrawal Schizophrenia , schizotypal and delusional Delusional Delusional disorder Folie à deux Psychosis and schizophrenia-like Brief reactive psychosis Schizoaffective disorder Schizophreniform disorder Schizophrenia Childhood schizophrenia Disorganized (hebephrenic) schizophrenia Paranoid schizophrenia Pseudoneurotic schizophrenia Simple-type schizophrenia Other Catatonia Symptoms and uncategorized Impulse control disorder Klüver–Bucy syndrome Psychomotor agitation Stereotypy
-
Muscle Weakness
Wikipedia
"Demonstration of delayed recovery from fatiguing exercise in chronic fatigue syndrome". Eur. J. Neurol . 6 (1): 63–9. doi : 10.1046/j.1468-1331.1999.610063.x . ... "Impaired oxygen delivery to muscle in chronic fatigue syndrome". Clin. Sci . 97 (5): 603–8, discussion 611–3. ... "Exercise capacity in chronic fatigue syndrome" . Arch. Intern. Med . 160 (21): 3270–7. doi : 10.1001/archinte.160.21.3270 . ... Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Clinical Working Case Definition, Diagnostic and Treatment Protocols . Journal of Chronic Fatigue Syndrome . 11 . pp. 7–115. doi : 10.1300/J092v11n01_02 .DMD, PMP22, AMPD1, GYG1, TBCD, MYOT, TTN, CSF3, CSF2, CAMKMT, SMN1, DES, SOD1, LMNA, VCP, FLNC, ETFDH, FBN1, IFIH1, CACNA1A, HLA-DRB1, MYH3, SYNE1, CLCN1, FGF23, TRNL1, FKTN, KCNJ11, DMPK, MSTO1, MPZ, ACAD9, AGL, DAG1, COL6A2, LRP4, TNFRSF11B, ALS2, TMEM126B, TTR, TOR1AIP1, TP53, SPTA1, SPG7, PROK2, SPP1, SPR, TRMT5, SNAP25, ACADVL, SPTB, SCNN1B, CEP126, SCNN1A, SDHA, SFRP4, SPARC, SDHD, SMPD1, SLC25A19, SLC4A1, SLC12A3, SLC34A1, HAMP, SLC22A5, SOX10, SMARCB1, SOS2, SOS1, SMN2, PTPN22, SARS1, SCN4A, PGK1, PMM2, PML, PLP1, FKRP, CDC73, PIGA, PHKB, PHKA1, PGM1, PFN1, PPOX, PFKM, PEX13, PEX7, SLC26A4, TBL1XR1, PDCD1, PDE11A, ARMC5, NUMA1, SLC25A24, CPLANE1, ATXN7, RAF1, XYLT2, POMT2, RYR1, RRAS, RPS6KA3, RIT1, IRF2BPL, RASA2, RARA, ALDH18A1, NABP1, PEX5, PTPN11, PSMB8, PSAP, PRPS1, PRPH, PRNP, PRKAR1A, PRKACA, TWNK, TGFB1, STAT3, STAT4, POLR3A, B4GAT1, AFG3L2, SEPTIN9, IL17RD, POMT1, CNNM2, TRPM7, SEMA3A, APTX, WARS2, QRICH1, TFG, RXYLT1, KLHL41, COQ7, OPTN, TSFM, SCO2, ERLIN2, SCN11A, EXOSC8, ISCU, NSMF, NDUFAF3, RTTN, SEPSECS, FLRT3, ABHD5, PIK3R5, KAT6B, ACTL6B, MRAS, ATP13A2, TRIM2, BICD2, AGTPBP1, LPIN1, ADA2, DPM3, MORC2, BCOR, TTC19, ADPRS, TSHR, AAAS, PAX8, ZBTB16, TMEM165, XK, VRK1, TTPA, NRAS, TRH, AGK, NKX2-1, TCN2, MLX, GMPPB, TACR3, SURF1, ABCC8, STAT5B, LZTR1, WDR11, DARS2, AIFM1, PREPL, POMGNT1, NFU1, HS6ST1, CHD7, TRIP4, LARGE1, SLC33A1, SLC7A7, CASK, LIMS2, ASCC1, CCN6, FGF17, HESX1, PEX11B, TRMU, PDE8B, SCNN1G, PNPLA8, HLA-DQB1, A2ML1, GCK, GCH1, GBE1, B4GALNT1, BTD, NPM1, TANGO2, FXN, FMR1, FOXE1, CHCHD10, FOXC2, C1QA, C1R, FGFR1, FGF8, DNAJC19, PROKR2, BRCA2, SYT2, SLC25A26, FDX2, ATP5F1D, HMBS, FAM111B, ATP7A, HLA-B, HEXB, CYP2R1, GJA1, SDHAF1, HBB, BCS1L, GPI, GNAS, BRAF, CCDC78, SLC34A3, EXT2, IFRD1, EXT1, CPT2, CAPN3, CCDC141, FEZF1, COL12A1, CAV1, COL6A1, COL5A2, COL5A1, COL4A1, COL1A1, CFL2, CCR6, CLCNKB, ERCC8, CHRND, CHRNB1, STAC3, SLC25A20, NKX2-5, CACNA1S, ETFB, ETFA, ERCC6, EPB42, HJV, B3GALNT2, DUSP6, C9orf72, CCN2, DCTN1, DCC, CYP27B1, CYP27A1, RNASEH1, CYP11B2, CYP11B1, HSPG2, IRF2BP2, ND5, MPV17, COX1, COX2, NDP, COX3, MTHFR, ANK1, ND1, ND2, ND3, NBN, ND4, NAGA, ND6, MYO9A, TRNE, TRNF, TRNH, TRNI, TRNK, C19orf12, POMK, ACTB, TRNP, ACY1, TRNQ, ALAS2, TRNS1, TRNS2, TRNT, TRNW, ATP6, TUBB6, KCNJ18, TIMM50, C12orf65, SLC25A46, LYRM7, IL12B, INS, PDX1, IRAK1, IRF5, ATP1A3, ITGA7, FIP1L1, D2HGDH, ANOS1, NF1, POMGNT2, KCNJ5, MECP2, NDUFB8, NDUFS2, NEFH, KISS1R, CRPPA, SPRY4, NEU1, L1CAM, ARSA, KRAS, TRNV, STMN1, SNURF, SNRPN, ACTA1, TPM2, NEB, GAA, SI, MYH7, DYSF, TPM3, MGAM, FHL1, ANO5, SGCA, AR, MB, IMMT, POLG, KIF1B, PABPN1, ACHE, DOK7, MYH2, ALB, IGF1, CAV3, AQP4, BIN1, PAX7, RAB7A, BEST1, MTM1, HMGCR, STIM1, GFPT1, LAMA2, UTRN, PIK3C2A, SELENON, DNM2, CRYAB, MYH8, COL13A1, GNE, ZMPSTE24, ACE2, MTMR14, NT5C1A, PIEZO2, AGRN, FSD1L, TNS3, YARS2, FSD1, TNFAIP8L2, SOST, MYPN, CHST14, SLC5A7, ALG2, TLR7, TAOK3, HCN1, ADSS1, PTRH2, PLF, PRMT8, ZC4H2, COPD, PLEKHM3, GLDN, WLS, ACADM, NOX4, FUS, GH1, GJB1, GSK3B, HDAC2, HEXA, HLA-DQA1, HSPB1, IGFALS, IGFBP1, IGHMBP2, IL2RA, ISG20, KCNH2, LEP, MAP6, MET, MIP, TRNM, MUSK, MYBPC1, NEFL, NOTCH1, NPTX2, MSTN, FES, OPA1, FBN2, SLC25A4, APP, ASAH1, BCL2, BRCA1, BTF3P11, CAT, CCND3, CFTR, CHKB, CHRNA4, CNTF, COL1A2, COL6A3, COX8A, CPOX, CRP, CYP19A1, DNAH8, DYNC1H1, EEF1A2, EMD, FABP3, NTF3, PDK4, CD274, PLA2G6, RNMT, APLN, COX5A, GTF2IRD1, MAD2L1BP, SLK, MATR3, MFN2, HNRNPDL, TRDN, MICU1, NDRG1, STK25, RBCK1, CUL9, NFASC, SMCHD1, TARDBP, MORC3, MMD, TNPO3, PRPF6, MCAT, TCAP, CNBP, PGD, VGF, PKM, PLA2G4A, PLAT, PPP1R1A, PRKAA1, PRKAA2, PRKAB1, REN, RYR2, ATXN1, SCN8A, CCL2, CCL18, SGCD, SHBG, SLC18A3, SNCA, SPRR2A, SPTBN1, TRIM21, RO60, TPM1, VEGFA, DUX4
-
Reactive Hypoglycemia
Wikipedia
It is recommended that the term reactive hypoglycemia be reserved for the pattern of postprandial hypoglycemia which meets the Whipple criteria (symptoms correspond to measurably low glucose and are relieved by raising the glucose), and that the term idiopathic postprandial syndrome be used for similar patterns of symptoms where abnormally low glucose levels at the time of symptoms cannot be documented. ... National Institutes of Health (NIH), a blood glucose level below 70 mg/dL (3.9 mmol/L) at the time of symptoms followed by relief after eating confirms a diagnosis for reactive hypoglycemia. [1] Contents 1 Signs and symptoms 2 Causes 3 Treatment 4 Postprandial syndrome 5 See also 6 References 7 Further reading 8 External links Signs and symptoms [ edit ] Symptoms vary according to individuals' hydration level and sensitivity to the rate and/or magnitude of decline of their blood glucose concentration. ... Suggestions include sugary foods that are quickly digested, such as: Dried fruit Soft drinks Juice Sugar as sweets, tablets or cubes. [25] The anti-hypertensive class of medication known as calcium channel blockers could be useful for reactive hypoglycemia as inhibition of the calcium channels on beta islet cells can help prevent an overproduction of insulin after a meal is eaten. [26] [27] Postprandial syndrome [ edit ] Main article: Idiopathic postprandial syndrome If there is no hypoglycemia at the time of the symptoms, this condition is called idiopathic postprandial syndrome. It might be an " adrenergic postprandial syndrome" — blood glucose levels are normal, but the symptoms are caused through autonomic adrenergic counterregulation. [28] Often, this syndrome is associated with emotional distress and anxious behaviour of the patient. [13] This is often seen in dysautonomic disorders as well. Dietary recommendations for reactive hypoglycemia can help to relieve symptoms of postprandial syndrome. See also [ edit ] Spontaneous hypoglycemia Refeeding syndrome References [ edit ] ^ a b c "Hypoglycemia."
-
Blepharitis
Wikipedia
The Meibomian glands may appear caked with oil or visibly obstructed. [2] Procedures [ edit ] Cultures of the eyelid margins can be a clear indicator for patients suffering from recurrent anterior blepharitis with severe inflammation, in addition to patients who are not responding to therapy. [2] Measurements of tear osmolarity may be beneficial in diagnosing concurrent dry eye syndrome (DES), which may be responsible for overlapping symptoms and would allow the physician to decipher between conditions and move forward with the most beneficial protocol for the patient. ... Patients with an inflammatory eyelid lesion that appears suspicious of malignancy should be referred to an appropriate specialist. [2] [26] Recent research [ edit ] A study conducted in November 2017, conveyed a correlation between blepharitis and early onset metabolic syndrome (MetS). To investigate the relationship between blepharitis and MetS, researchers used the Longitudinal Health Insurance Database in Taiwan. ... "Blepharitis as an early sign of metabolic syndrome: a nationwide population-based study". ... External links [ edit ] Classification D ICD - 10 : H01.0 ICD - 9-CM : 373.0 MeSH : D001762 DiseasesDB : 1455 External resources MedlinePlus : 001619 eMedicine : oph/81 Patient UK : Blepharitis Wikimedia Commons has media related to Blepharitis . blepharitis Resource Guide from the National Eye Institute (NEI). eMedicine Health: Eyelid Inflammation (blepharitis) v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma OnchocerciasisAPOE, UROS, WIPF1, XPA, XPC, SMC1A, TP63, SMC3, TBX4, TRAF3IP2, GJB6, PLXND1, PIGN, NIPBL, TINF2, MBTPS2, RTEL1, WRAP53, SETD5, NOP10, SLC39A4, NHP2, HDAC8, USB1, CTC1, WAS, TERT, MMP1, ERCC2, ERCC4, ERCC5, GATA1, GNAQ, DKC1, KMT2A, TERC, DDB2, CST6, PARN, PKP1, PLCD1, RAD21, REV3L, MSMO1, COL7A1, ST14, STAT1, ADAM17, ERCC3, LTB4R, IL4, MMP9, PSIP1, CX3CL1, LACRT
-
Running Injuries
Wikipedia
Common overuse injuries include shin splints , stress fractures , Achilles tendinitis , Iliotibial band syndrome , Patellofemoral pain (runner's knee), and plantar fasciitis . ... Stretching the calves before starting heavy exercise may help relieve tightness in the muscles. [16] Patellofemoral pain syndrome [ edit ] Patellofemoral pain syndrome is associated with pain in the knee and around the patella (kneecap). ... It can be caused by a single incident but is often the result of overuse or a sudden increase in physical activity. Iliotibial band syndrome [ edit ] Diagram indicating the location of the iliotibial band and pain associated with iliotibial band syndrome Iliotibial band syndrome (ITBS) is defined as inflammation of the iliotibial band on the outside of the knee. ... Recurrence is a common issue with iliotibial band syndrome, as pain goes away with a period of rest, but symptoms can easily come back as the runner returns to training. ... Retrieved 30 November 2020 . ^ Reshef, N; Guelich, DR (April 2012). "Medial tibial stress syndrome". Clinics in Sports Medicine . 31 (2): 273–290. doi : 10.1016/j.csm.2011.09.008 .
-
Toluene Toxicity
Wikipedia
Both a low-carbohydrate diet and fasting have been shown to induce CYP2E1 and as a result increase toluene metabolism. [12] A low protein diet may decrease total CYP content and thereby reduce the elimination rate of the drug. [12] Measure of exposure [ edit ] Hippuric acid has long been used as an indicator of toluene exposure; [14] however, there appears to be some doubt about its validity. [15] There is significant endogenous hippuric acid production by humans; which shows inter- and intra-individual variation influenced by factors such as diet, medical treatment, alcohol consumption, etc. [15] This suggests that hippuric acid may be an unreliable indicator of toluene exposure. [15] [16] It has been suggested that urinary hippuric acid, the traditional marker of toluene exposure is simply not sensitive enough to separate the exposed from the non-exposed. [17] This has led to the investigation of other metabolites as markers for toluene exposure. [16] Urinary o -cresol may be more reliable for the biomonitoring of toluene exposure because, unlike hippuric acid , o -cresol is not found at detectable levels in unexposed subjects. [16] o-Cresol may be a less sensitive marker of toluene exposure than hippuric acid. [18] o-Cresol excretion may be an unreliable method for measuring toluene exposure because o-cresol makes up <1% of total toluene elimination. [14] Benzylmercapturic acid , a minor metabolite of toluene, is produced from benzaldehyde . [19] In more recent years, studies have suggested the use of urinary benzylmercapturic acid as the best marker for toluene exposure, because: it is not detected in non-exposed subjects; it is more sensitive than hippuric acid at low concentrations; it is not affected by eating or drinking; it can detect toluene exposure down to approximately 15 ppm ; and it shows a better quantitative relationship with toluene than hippuric acid or o -cresol . [20] [21] Effects of long-term exposure [ edit ] Serious adverse behavioural effects are often associated with chronic occupational exposure [22] and toluene abuse related to the deliberate inhalation of solvents . [23] Long-term toluene exposure is often associated with effects such as: psychoorganic syndrome ; [24] visual evoked potential (VEP) abnormality; [24] toxic polyneuropathy , cerebellar , cognitive , and pyramidal dysfunctions ; [23] [24] optic atrophy ; hearing disorders [25] [26] and brain lesions . [23] The neurotoxic effects of long-term use (in particular repeated withdrawals ) of toluene may cause postural tremors by downregulating GABA receptors within the cerebellar cortex . [23] Treatment with GABA agonists such as benzodiazepines provide some relief from toluene-induced tremor and ataxia . [23] An alternative to drug treatment is ventral intermediate nucleus (vim) thalamotomy . [23] The tremors associated with toluene misuse do not seem to be a transient symptom, but an irreversible and progressive symptom which continues after solvent abuse has been discontinued. [23] There is some evidence that low-level toluene exposure may cause disruption in the differentiation of astrocyte precursor cells. [27] This does not appear to be a major hazard to adults; however, exposure of pregnant women to toluene during critical stages of fetal development could cause serious disruption to neuronal development. [27] References [ edit ] ^ a b c Shou, M; Lu T; Krausz KW; Sai Y; Yang T; Korzekwa KR; Gonzalez FJ; Gelboin HV (2000-04-14). ... Department of Health and Human Services (public domain) v t e Psychoactive substance-related disorder General SID Substance intoxication / Drug overdose Substance-induced psychosis Withdrawal : Craving Neonatal withdrawal Post-acute-withdrawal syndrome (PAWS) SUD Substance abuse / Substance-related disorders Physical dependence / Psychological dependence / Substance dependence Combined substance use SUD Polysubstance dependence SID Combined drug intoxication (CDI) Alcohol SID Cardiovascular diseases Alcoholic cardiomyopathy Alcohol flush reaction (AFR) Gastrointestinal diseases Alcoholic liver disease (ALD): Alcoholic hepatitis Auto-brewery syndrome (ABS) Endocrine diseases Alcoholic ketoacidosis (AKA) Nervous system diseases Alcohol-related dementia (ARD) Alcohol intoxication Hangover Neurological disorders Alcoholic hallucinosis Alcoholic polyneuropathy Alcohol-related brain damage Alcohol withdrawal syndrome (AWS): Alcoholic hallucinosis Delirium tremens (DTs) Fetal alcohol spectrum disorder (FASD) Fetal alcohol syndrome (FAS) Korsakoff syndrome Positional alcohol nystagmus (PAN) Wernicke–Korsakoff syndrome (WKS, Korsakoff psychosis) Wernicke encephalopathy (WE) Respiratory tract diseases Alcohol-induced respiratory reactions Alcoholic lung disease SUD Alcoholism (alcohol use disorder (AUD)) Binge drinking Caffeine SID Caffeine-induced anxiety disorder Caffeine-induced sleep disorder Caffeinism SUD Caffeine dependence Cannabis SID Cannabis arteritis Cannabinoid hyperemesis syndrome (CHS) SUD Amotivational syndrome Cannabis use disorder (CUD) Synthetic cannabinoid use disorder Cocaine SID Cocaine intoxication Prenatal cocaine exposure (PCE) SUD Cocaine dependence Hallucinogen SID Acute intoxication from hallucinogens (bad trip) Hallucinogen persisting perception disorder (HPPD) Nicotine SID Nicotine poisoning Nicotine withdrawal SUD Nicotine dependence Opioids SID Opioid overdose SUD Opioid use disorder (OUD) Sedative / hypnotic SID Kindling (sedative–hypnotic withdrawal) benzodiazepine : SID Benzodiazepine overdose Benzodiazepine withdrawal SUD Benzodiazepine use disorder (BUD) Benzodiazepine dependence barbiturate : SID Barbiturate overdose SUD Barbiturate dependence Stimulants SID Stimulant psychosis amphetamine : SUD Amphetamine dependence Volatile solvent SID Sudden sniffing death syndrome (SSDS) Toluene toxicity SUD Inhalant abuse v t e Poisoning Toxicity Overdose History of poison Inorganic Metals Toxic metals Beryllium Cadmium Lead Mercury Nickel Silver Thallium Tin Dietary minerals Chromium Cobalt Copper Iron Manganese Zinc Metalloids Arsenic Nonmetals Sulfuric acid Selenium Chlorine Fluoride Organic Phosphorus Pesticides Aluminium phosphide Organophosphates Nitrogen Cyanide Nicotine Nitrogen dioxide poisoning CHO alcohol Ethanol Ethylene glycol Methanol Carbon monoxide Oxygen Toluene Pharmaceutical Drug overdoses Nervous Anticholinesterase Aspirin Barbiturates Benzodiazepines Cocaine Lithium Opioids Paracetamol Tricyclic antidepressants Cardiovascular Digoxin Dipyridamole Vitamin poisoning Vitamin A Vitamin D Vitamin E Megavitamin-B 6 syndrome Biological 1 Fish / seafood Ciguatera Haff disease Ichthyoallyeinotoxism Scombroid Shellfish poisoning Amnesic Diarrhetic Neurotoxic Paralytic Other vertebrates amphibian venom Batrachotoxin Bombesin Bufotenin Physalaemin birds / quail Coturnism snake venom Alpha-Bungarotoxin Ancrod Batroxobin Arthropods Arthropod bites and stings bee sting / bee venom Apamin Melittin scorpion venom Charybdotoxin spider venom Latrotoxin / Latrodectism Loxoscelism tick paralysis Plants / fungi Cinchonism Ergotism Lathyrism Locoism Mushrooms Strychnine 1 including venoms , toxins , foodborne illnesses .
-
Cardiac Tamponade
Wikipedia
External links [ edit ] Classification D ICD - 10 : I31.9 ICD - 10-CM : I31.4 ICD - 9-CM : 423.3 MeSH : D002305 External resources MedlinePlus : 000194 eMedicine : med/283 emerg/412 Patient UK : Cardiac tamponade v t e Cardiovascular disease (heart) Ischaemic Coronary disease Coronary artery disease (CAD) Coronary artery aneurysm Spontaneous coronary artery dissection (SCAD) Coronary thrombosis Coronary vasospasm Myocardial bridge Active ischemia Angina pectoris Prinzmetal's angina Stable angina Acute coronary syndrome Myocardial infarction Unstable angina Sequelae hours Hibernating myocardium Myocardial stunning days Myocardial rupture weeks Aneurysm of heart / Ventricular aneurysm Dressler syndrome Layers Pericardium Pericarditis Acute Chronic / Constrictive Pericardial effusion Cardiac tamponade Hemopericardium Myocardium Myocarditis Chagas disease Cardiomyopathy Dilated Alcoholic Hypertrophic Tachycardia-induced Restrictive Loeffler endocarditis Cardiac amyloidosis Endocardial fibroelastosis Arrhythmogenic right ventricular dysplasia Endocardium / valves Endocarditis infective endocarditis Subacute bacterial endocarditis non-infective endocarditis Libman–Sacks endocarditis Nonbacterial thrombotic endocarditis Valves mitral regurgitation prolapse stenosis aortic stenosis insufficiency tricuspid stenosis insufficiency pulmonary stenosis insufficiency Conduction / arrhythmia Bradycardia Sinus bradycardia Sick sinus syndrome Heart block : Sinoatrial AV 1° 2° 3° Intraventricular Bundle branch block Right Left Left anterior fascicle Left posterior fascicle Bifascicular Trifascicular Adams–Stokes syndrome Tachycardia ( paroxysmal and sinus ) Supraventricular Atrial Multifocal Junctional AV nodal reentrant Junctional ectopic Ventricular Accelerated idioventricular rhythm Catecholaminergic polymorphic Torsades de pointes Premature contraction Atrial Junctional Ventricular Pre-excitation syndrome Lown–Ganong–Levine Wolff–Parkinson–White Flutter / fibrillation Atrial flutter Ventricular flutter Atrial fibrillation Familial Ventricular fibrillation Pacemaker Ectopic pacemaker / Ectopic beat Multifocal atrial tachycardia Pacemaker syndrome Parasystole Wandering atrial pacemaker Long QT syndrome Andersen–Tawil Jervell and Lange-Nielsen Romano–Ward Cardiac arrest Sudden cardiac death Asystole Pulseless electrical activity Sinoatrial arrest Other / ungrouped hexaxial reference system Right axis deviation Left axis deviation QT Short QT syndrome T T wave alternans ST Osborn wave ST elevation ST depression Strain pattern Cardiomegaly Ventricular hypertrophy Left Right / Cor pulmonale Atrial enlargement Left Right Athletic heart syndrome Other Cardiac fibrosis Heart failure Diastolic heart failure Cardiac asthma Rheumatic fever v t e Chest injury , excluding fractures Cardiac and circulatory system injuries vascular : Traumatic aortic rupture Thoracic aorta injury heart : Myocardial contusion / Commotio cordis Cardiac tamponade Hemopericardium Myocardial rupture Lung and lower respiratory tract injuries Pneumothorax Hemothorax Hemopneumothorax Pulmonary contusion Pulmonary laceration Tracheobronchial injury Diaphragmatic rupture v t e Trauma Principles Polytrauma Major trauma Traumatology Triage Resuscitation Trauma triad of death Assessment Clinical prediction rules Revised Trauma Score Injury Severity Score Abbreviated Injury Scale NACA score Investigations Diagnostic peritoneal lavage Focused assessment with sonography for trauma Management Principles Advanced trauma life support Trauma surgery Trauma center Trauma team Damage control surgery Early appropriate care Procedures Resuscitative thoracotomy Pathophysiology Injury MSK Bone fracture Joint dislocation Degloving Soft tissue injury Resp Flail chest Pneumothorax Hemothorax Diaphragmatic rupture Pulmonary contusion Cardio Internal bleeding Thoracic aorta injury Cardiac tamponade GI Blunt kidney trauma Ruptured spleen Neuro Penetrating head injury Traumatic brain injury Intracranial hemorrhage Mechanism Blast injury Blunt trauma Burn Penetrating trauma Crush injury Stab wound Ballistic trauma Electrocution Region Abdominal trauma Chest trauma Facial trauma Head injury Spinal cord injury Demographic Geriatric trauma Pediatric trauma Complications Posttraumatic stress disorder Wound healing Acute lung injury Crush syndrome Rhabdomyolysis Compartment syndrome Contracture Volkmann's contracture Embolism air fat Chronic traumatic encephalopathy Subcutaneous emphysema
-
Oral Manifestations Of Systemic Disease
Wikipedia
Other systemic diseases that can cause the tongue to form aphthous ulcers are: Crohn's disease and ulcerative colitis , Behcet's Syndrome , pemphigus vulgaris , herpes simplex , histoplasmosis , and reactive arthritis . [3] Contents 1 Cardiovascular and haematological system 2 Respiratory system 3 Renal System 4 Digestive System 5 Endocrine System 6 Skeletal System 7 Immune System 8 Nervous System 9 Muscular System 10 References. ... Patient with Diabetes have increase extent and severity of Periodontal Disease , increased prevalence of Dental Caries due to Xerostomia , can suffer from Burning Mouth Syndrome and Candidal infections as well as experiencing altered taste sensation, altered tooth eruption and hypertrophy of the parotid glands. ... Other complications include visual field defects, headaches , Diabetes, Sleep apnoea , Hypertension , Arthralgia and Arthritis and Carpal Tunnel Syndrome . [13] Arthralgia and Carpal Tunnel Syndrome both have an impact on a patients’ ability to maintain good oral hygiene practice and therefore may predispose them to Dental caries and Periodontal Disease. ... A CD4 count less than 200 is a diagnosis of Acquired Immunodeficiency Syndrome (AIDS) . Oral manifestation of HIV include candidiasis , Oral Hairy Leukoplakia , oral ulcers, oral warts , oral lymphoma and Kaposi Sarcoma . [13] Other presentations include gingivitis and oral malignancies. ... PMID 16916469 . v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
Optic Nerve Hypoplasia
Wikipedia
Delays may occur in unilateral (39%) as well as bilateral (78%) cases. [3] Cause [ edit ] Genetic risks [ edit ] Mutations of genes involved in transcription regulation , chromatin remodelling , α-dystroglycan glycosylation , cytoskeleton and scaffolding protein , RNA splicing , and the MAP kinase signalling pathway are currently known to cause ONH. [2] Many transcription factors for eye development are also involved in the morphogenesis of forebrain, which may explain why ONH is commonly a part of a syndrome involving brain malformations. [2] ONH impacts all ethnic groups, although in the United States, occurrence is lower in persons of Asian descent. [3] [7] [4] To date, there have been few reports of ONH occurrence in Asian countries, although it is uncertain why this is so. ... Epidemiology [ edit ] Optic nerve hypoplasia (ONH) is a congenital condition in which the optic nerve is underdeveloped (small). Many times, de Morsier’s Syndrome or septo-optic dysplasia (SOD) is associated with ONH, however, it is possible to have ONH without any additional issues like SOD. ... PMID 28501829 . ^ a b c d e f g h i j k l m n o Borchert, Mark, and Pamela Garcia-Filion. "The Syndrome of Optic Nerve Hypoplasia." Current Neurology and Neuroscience Reports. 8 (2008): 395-403. ^ a b c Garcia-Filion, Pamela, Karen Epport, Marvin Nelson, Colleen Azen, Mitchell E. ... External links [ edit ] Classification D ICD - 10 : Q14.2 ICD - 10-CM : H47.03 ICD - 9-CM : 377.43 , 743.57 - 743.58 OMIM : 165550 DiseasesDB : 31311 External resources Orphanet : 137902 v t e Diseases of the human eye Adnexa Eyelid Inflammation Stye Chalazion Blepharitis Entropion Ectropion Lagophthalmos Blepharochalasis Ptosis Blepharophimosis Xanthelasma Ankyloblepharon Eyelash Trichiasis Madarosis Lacrimal apparatus Dacryoadenitis Epiphora Dacryocystitis Xerophthalmia Orbit Exophthalmos Enophthalmos Orbital cellulitis Orbital lymphoma Periorbital cellulitis Conjunctiva Conjunctivitis allergic Pterygium Pseudopterygium Pinguecula Subconjunctival hemorrhage Globe Fibrous tunic Sclera Scleritis Episcleritis Cornea Keratitis herpetic acanthamoebic fungal Exposure Photokeratitis Corneal ulcer Thygeson's superficial punctate keratopathy Corneal dystrophy Fuchs' Meesmann Corneal ectasia Keratoconus Pellucid marginal degeneration Keratoglobus Terrien's marginal degeneration Post-LASIK ectasia Keratoconjunctivitis sicca Corneal opacity Corneal neovascularization Kayser–Fleischer ring Haab's striae Arcus senilis Band keratopathy Vascular tunic Iris Ciliary body Uveitis Intermediate uveitis Hyphema Rubeosis iridis Persistent pupillary membrane Iridodialysis Synechia Choroid Choroideremia Choroiditis Chorioretinitis Lens Cataract Congenital cataract Childhood cataract Aphakia Ectopia lentis Retina Retinitis Chorioretinitis Cytomegalovirus retinitis Retinal detachment Retinoschisis Ocular ischemic syndrome / Central retinal vein occlusion Central retinal artery occlusion Branch retinal artery occlusion Retinopathy diabetic hypertensive Purtscher's of prematurity Bietti's crystalline dystrophy Coats' disease Sickle cell Macular degeneration Retinitis pigmentosa Retinal haemorrhage Central serous retinopathy Macular edema Epiretinal membrane (Macular pucker) Vitelliform macular dystrophy Leber's congenital amaurosis Birdshot chorioretinopathy Other Glaucoma / Ocular hypertension / Primary juvenile glaucoma Floater Leber's hereditary optic neuropathy Red eye Globe rupture Keratomycosis Phthisis bulbi Persistent fetal vasculature / Persistent hyperplastic primary vitreous Persistent tunica vasculosa lentis Familial exudative vitreoretinopathy Pathways Optic nerve Optic disc Optic neuritis optic papillitis Papilledema Foster Kennedy syndrome Optic atrophy Optic disc drusen Optic neuropathy Ischemic anterior (AION) posterior (PION) Kjer's Leber's hereditary Toxic and nutritional Strabismus Extraocular muscles Binocular vision Accommodation Paralytic strabismus Ophthalmoparesis Chronic progressive external ophthalmoplegia Kearns–Sayre syndrome palsies Oculomotor (III) Fourth-nerve (IV) Sixth-nerve (VI) Other strabismus Esotropia / Exotropia Hypertropia Heterophoria Esophoria Exophoria Cyclotropia Brown's syndrome Duane syndrome Other binocular Conjugate gaze palsy Convergence insufficiency Internuclear ophthalmoplegia One and a half syndrome Refraction Refractive error Hyperopia Myopia Astigmatism Anisometropia / Aniseikonia Presbyopia Vision disorders Blindness Amblyopia Leber's congenital amaurosis Diplopia Scotoma Color blindness Achromatopsia Dichromacy Monochromacy Nyctalopia Oguchi disease Blindness / Vision loss / Visual impairment Anopsia Hemianopsia binasal bitemporal homonymous Quadrantanopia subjective Asthenopia Hemeralopia Photophobia Scintillating scotoma Pupil Anisocoria Argyll Robertson pupil Marcus Gunn pupil Adie syndrome Miosis Mydriasis Cycloplegia Parinaud's syndrome Other Nystagmus Childhood blindness Infections Trachoma Onchocerciasis
-
Diamond–blackfan Anemia
Wikipedia
This is in contrast to Shwachman–Bodian–Diamond syndrome , in which the bone marrow defect results primarily in neutropenia , and Fanconi anemia , where all cell lines are affected resulting in pancytopenia . ... Malformations are seen more frequently with DBA6 RPL5 and DBA7 RPL11 mutations. [5] The genetic abnormalities underpinning the combination of DBA with Treacher Collins syndrome (TCS)/ mandibulofacial dysostosis (MFD) phenotypes are heterogeneous, including RPS26 (the known DBA10 gene), TSR2 which encodes a direct binding partner of RPS26 , and RPS28 . [19] Molecular basis [ edit ] The phenotype of DBA patients suggests a hematological stem cell defect specifically affecting the erythroid progenitor population. ... External links [ edit ] Classification D ICD - 10 : D61.0 ICD - 9-CM : 284.01 OMIM : 105650 MeSH : D029503 External resources Patient UK : Diamond–Blackfan anemia GeneReviews/NCBI/NIH/UW entry on Diamond–Blackfan Anemia OMIM entries on Diamond–Blackfan Anemia Diamond–Blackfan anemia Genetics Home Reference v t e Diseases of red blood cells ↑ Polycythemia Polycythemia vera ↓ Anemia Nutritional Micro- : Iron-deficiency anemia Plummer–Vinson syndrome Macro- : Megaloblastic anemia Pernicious anemia Hemolytic (mostly normo- ) Hereditary enzymopathy : Glucose-6-phosphate dehydrogenase deficiency glycolysis pyruvate kinase deficiency triosephosphate isomerase deficiency hexokinase deficiency hemoglobinopathy : Thalassemia alpha beta delta Sickle cell disease / trait Hereditary persistence of fetal hemoglobin membrane : Hereditary spherocytosis Minkowski–Chauffard syndrome Hereditary elliptocytosis Southeast Asian ovalocytosis Hereditary stomatocytosis Acquired AIHA Warm antibody autoimmune hemolytic anemia Cold agglutinin disease Donath–Landsteiner hemolytic anemia Paroxysmal cold hemoglobinuria Mixed autoimmune hemolytic anemia membrane paroxysmal nocturnal hemoglobinuria Microangiopathic hemolytic anemia Thrombotic microangiopathy Hemolytic–uremic syndrome Drug-induced autoimmune Drug-induced nonautoimmune Hemolytic disease of the newborn Aplastic (mostly normo- ) Hereditary : Fanconi anemia Diamond–Blackfan anemia Acquired: Pure red cell aplasia Sideroblastic anemia Myelophthisic Blood tests Mean corpuscular volume normocytic microcytic macrocytic Mean corpuscular hemoglobin concentration normochromic hypochromic Other Methemoglobinemia Sulfhemoglobinemia Reticulocytopenia v t e Disorders of translation and posttranslational modification Translation Ribosome : Diamond–Blackfan anemia FMR1 Fragile X syndrome Fragile X-associated tremor/ataxia syndrome Premature ovarian failure 1 Initiation factor : Leukoencephalopathy with vanishing white matter snRNP : Retinitis pigmentosa 33 Posttranslational modification Protein folding Alzheimer's disease Huntington's disease Creutzfeldt–Jakob disease chaperonins: 3-Methylglutaconic aciduria 5 Protein targeting I-cell disease Ubiquitin E1 : X-linked spinal muscular atrophy 2 E3 : Johanson–Blizzard syndrome Von Hippel–Lindau disease 3-M syndrome Angelman syndrome Deubiquitinating enzyme : Machado–Joseph disease Aneurysmal bone cyst Multiple familial trichoepithelioma 1 SUMO OFC10 Other Multiple sulfatase deficiency Hyperproinsulinemia Ehlers–Danlos syndrome 6GATA1, RPS19, RPS24, RPS17, ADA2, RPL27, RPL26, RPL15, RPS27, RPS29, RPL35, TSR2, RPL18, RPL11, RPL5, RPS28, RPL35A, RPS7, RPS26, EPO, RPS10, RPL9, RPL31, RPS27A, RPL19, RPL36, RPL13, RPS15A, RPL23, RPS15, FLVCR1, TP53, RPSA, IQCG, DIPK1A, CD34, RPS14, LOH19CR1, ADA, KITLG, THPO, CSDE1, SBDS, HSPA4, IL3, RPL41, AHSA1, LEFTY1, KLF1, FLI1, GABARAPL2, GABARAPL1, BAMBI, RNF19A, CSF2, GRAP2, POLDIP2, MAPK14, CRK, MTUS1, COL3A1, CDA, DBA2, CD38, PRMT3, DDX21, LONP1, FPR2, TRIM27, MAPK8, MAPK1, PIM1, SERPINE1, RPS21, LRPAP1, LEP, IL9, IL1B, TFRC, TNF, CNBP, AIMP2, XRS, HBB, RMRP, TEC
-
Deep Vein Thrombosis
Wikipedia
VTE can occur as DVT only, as PE with DVT, or PE without DVT. [3] The most frequent long-term complication is post-thrombotic syndrome , which can cause pain, swelling, a sensation of heaviness, itching, and in severe cases, ulcers . [5] Also, recurrent VTE occurs in about 30% of those in the ten years following an initial VTE. [3] The mechanism of clot formation typically involves some combination of decreased blood flow rate , increased tendency to clot , and injury to the blood vessel wall . [9] Risk factors include recent surgery, older age, active cancer , obesity , personal history and family history of VTE, trauma, injuries, lack of movement, hormonal birth control , pregnancy and the period following birth , and antiphospholipid syndrome . ... This can cause increased pressure leading to compartment syndrome and decreased oxygenation leading to gangrene . ... Infection, including that of COVID-19 , increases risk. [44] [45] Inflammatory diseases [24] [46] such as Behçet's syndrome , [47] and some autoimmune diseases , [48] such as primary antiphospholipid syndrome [49] and systemic lupus erythematosus (SLE), [50] increase risk. SLE itself is frequently associated with secondary antiphospholipid syndrome. [51] Other associated conditions include heparin-induced thrombocytopenia , [52] thrombotic storm , [53] catastrophic antiphospholipid syndrome , [54] paroxysmal nocturnal hemoglobinuria , [55] nephrotic syndrome , [12] chronic kidney disease , [56] HIV , [57] polycythemia vera , [31] intravenous drug use, [58] and smoking. ... If neither of these two methods are feasible, then aspirin is suggested. [29] Prognosis [ edit ] DVT is most frequently a disease of older age that occurs in the context of nursing homes, hospitals, and active cancer. [3] It is associated with a 30-day mortality rate of about 6%, with PE being the cause of most of these deaths. [1] Proximal DVT is frequently associated with PE, unlike distal DVT, which is rarely if ever associated with PE. [21] Around 56% of those with proximal DVT also have PE, although a chest CT is not needed simply because of the presence of DVT. [1] If proximal DVT is left untreated, in the following 3 months approximately half of people will experience symptomatic PE. [8] Another frequent complication of proximal DVT, and the most frequent chronic complication, is post-thrombotic syndrome , where individuals have chronic venous symptoms. [5] Symptoms can include pain, itching, swelling, paresthesia , a sensation of heaviness, and in severe cases, leg ulcers . [5] After proximal DVT, an estimated 20–50% of people develop the syndrome, with 5–10% experiencing severe symptoms. [136] Post-thrombotic syndrome can also be a complication of distal DVT, though to a lesser extent than with proximal DVT. [137] Recurrence of DVT is another potential consequence.F2, SERPINC1, MTHFR, F5, PROC, F13A1, F3, TFPI, PLG, PLAT, LPA, KDR, EPO, JAK2, SERPINA10, PLAU, F8, F13B, CSF2, F7, PIGM, PROS1, PROCR, F9, HABP2, THBD, ABO, AKT1, SLC44A2, F10, SERPINE1, PMM2, F11-AS1, COX7A2L, FUNDC2, TSPAN15, COX8A, CRP, IL6, VWF, SELP, ACE, APOE, PC, VKORC1, CCL2, ADAMTS13, IL18, MMP2, F11, IL17A, CBS, C20orf181, APEX1, CPB2, CYP2C9, ZNF415, KLKB1, KNG1, ARHGEF7, LEP, RBBP6, PTS, PTEN, PRKCD, VEGFA, PRKRA, PLA2G6, NFKB1, POU2F3, TLR9, NOS3, CLEC1B, ASCC1, PECAM1, TNF, PLA2G1B, STAT3, PLA2G2A, MTRR, H3P40, ITGB3, APC, MIR195, MIR150, CD40, FGB, FGG, CYP4V2, MIR495, SERPIND1, MIR532, HLA-DPB1, MIR582, RN7SL263P, CXCR2, ALB, CXCL8, TNFSF11, CBSL, NNT, POTEKP, SIRT1, SLC9A8, MIR335, ACOT7, MICA, TP63, MIR411, FASTK, MIR483, DURS1, POTEM, PADI4, SETD1A, FHL5, LIPG, ADIPOQ, HNRNPA1P10, MIR21, PLA2G15, MIR205, MARCHF1, FTO, PPP1R3B, ACSF2, HAMP, FERMT3, SLC9A7, RETN, ACSS2, ACCS, TUBA1C, TSPAN18, ADI1, DNER, MIR136, MARCHF3, DAND5, PCSK9, IS1, GP6, SLC9A9, TSPAN33, ACTBL2, SLC9A4, MIRLET7E, MIR130A, CORO7, IL1R2, A2M, VTN, GCLC, ESR1, ESR2, FGA, FOXC2, GAS6, GCY, GGCX, HIF1A, EDN1, HMGB1, HNRNPA1, HRG, IFNA1, IFNA13, IFNG, IL2, EMD, DNASE1, IL9, AR, ACR, ACTG1, ACTG2, AMBP, ANXA2, APOH, FASLG, AVP, CYP3A4, BCL2, BDKRB2, CAD, ENTPD1, CDSN, CHI3L1, CYP2B6, IL4, IL10, VCAM1, SLC5A2, REN, S100A9, CCL7, CX3CL1, SELL, SELPLG, SLC2A1, SLC9A3, PTGS2, SLC9A5, SPP1, TCF21, TEK, TNFRSF1A, TP53, UGCG, PTPRC, PTGIR, ITGAM, MTR, LDLR, LMNA, MIF, MMP1, MMP3, MMP9, MMP14, MYH9, SERPINA3, NDUFB2, NFKBIL1, FURIN, SERPINF1, ABCB1, SERPINF2, PPP1R1A, PPP1R3C
-
Hypersexuality
Wikipedia
Hypersexuality may be a primary condition, or the symptom of another medical disease or condition; for example, Klüver-Bucy syndrome or bipolar disorder . Hypersexuality may also present as a side effect of medication such as drugs used to treat Parkinson's disease . ... Pick's disease causes damage to the temporal/frontal lobe of the brain; people with Pick's disease show a range of socially inappropriate behaviors. [39] Several neurological conditions such as Alzheimer's disease , autism , [40] [41] various types of brain injury, [42] Klüver–Bucy syndrome , [43] Kleine–Levin syndrome , [44] and many more neurodegenerative diseases can cause hypersexual behavior. ... "Neurocase: The Neural Basis of Cognition". Klüver–Bucy Syndrome, Hypersexuality, and the Law . 16 (2): 140–145. doi : 10.1080/13554790903329182 . ... PMID 3746322 . ^ National Institute of Neurological Disorders and Stroke. "NINDS Klüver-Bucy Syndrome Information Page" . Retrieved 2009-10-10 . ^ Arnulf I, Zeitzer JM, File J, Farber N, Mignot E (December 2005). "Kleine-Levin syndrome: a systematic review of 186 cases in the literature" .
-
Dysentery
Wikipedia
The cycle then begins again. [ citation needed ] Bacillary dysentery [ edit ] Main article: Bacillary dysentery Dysentery may also be caused by shigellosis , an infection by bacteria of the genus Shigella , and is then known as bacillary dysentery (or Marlow syndrome). The term bacillary dysentery etymologically might seem to refer to any dysentery caused by any bacilliform bacteria, but its meaning is restricted by convention to Shigella dysentery. ... External links [ edit ] Classification D ICD - 10 : A09.0 , A03.9 , A06.0 , A07.9 ICD - 9-CM : 004 , 007.9 , 009.0 MeSH : D004403 v t e Parasitic disease caused by Excavata protozoa Discicristata Trypanosomatida Trypanosomiasis T. brucei African trypanosomiasis T. cruzi Chagas disease Leishmaniasis Leishmania major / L. mexicana / L. aethiopica / L. tropica Cutaneous leishmaniasis L. braziliensis Mucocutaneous leishmaniasis L. donovani / infantum Visceral leishmaniasis Schizopyrenida Naegleria fowleri Primary amoebic meningoencephalitis Trichozoa Diplomonadida Giardia lamblia ( Giardiasis ) Trichomonadida Trichomonas vaginalis Trichomoniasis Dientamoeba fragilis Dientamoebiasis v t e Proteobacteria -associated Gram-negative bacterial infections α Rickettsiales Rickettsiaceae / ( Rickettsioses ) Typhus Rickettsia typhi Murine typhus Rickettsia prowazekii Epidemic typhus , Brill–Zinsser disease , Flying squirrel typhus Spotted fever Tick-borne Rickettsia rickettsii Rocky Mountain spotted fever Rickettsia conorii Boutonneuse fever Rickettsia japonica Japanese spotted fever Rickettsia sibirica North Asian tick typhus Rickettsia australis Queensland tick typhus Rickettsia honei Flinders Island spotted fever Rickettsia africae African tick bite fever Rickettsia parkeri American tick bite fever Rickettsia aeschlimannii Rickettsia aeschlimannii infection Mite-borne Rickettsia akari Rickettsialpox Orientia tsutsugamushi Scrub typhus Flea-borne Rickettsia felis Flea-borne spotted fever Anaplasmataceae Ehrlichiosis : Anaplasma phagocytophilum Human granulocytic anaplasmosis , Anaplasmosis Ehrlichia chaffeensis Human monocytotropic ehrlichiosis Ehrlichia ewingii Ehrlichiosis ewingii infection Rhizobiales Brucellaceae Brucella abortus Brucellosis Bartonellaceae Bartonellosis : Bartonella henselae Cat-scratch disease Bartonella quintana Trench fever Either B. henselae or B. quintana Bacillary angiomatosis Bartonella bacilliformis Carrion's disease , Verruga peruana β Neisseriales M+ Neisseria meningitidis/meningococcus Meningococcal disease , Waterhouse–Friderichsen syndrome , Meningococcal septicaemia M− Neisseria gonorrhoeae/gonococcus Gonorrhea ungrouped: Eikenella corrodens / Kingella kingae HACEK Chromobacterium violaceum Chromobacteriosis infection Burkholderiales Burkholderia pseudomallei Melioidosis Burkholderia mallei Glanders Burkholderia cepacia complex Bordetella pertussis / Bordetella parapertussis Pertussis γ Enterobacteriales ( OX− ) Lac+ Klebsiella pneumoniae Rhinoscleroma , Pneumonia Klebsiella granulomatis Granuloma inguinale Klebsiella oxytoca Escherichia coli : Enterotoxigenic Enteroinvasive Enterohemorrhagic O157:H7 O104:H4 Hemolytic-uremic syndrome Enterobacter aerogenes / Enterobacter cloacae Slow/weak Serratia marcescens Serratia infection Citrobacter koseri / Citrobacter freundii Lac− H2S+ Salmonella enterica Typhoid fever , Paratyphoid fever , Salmonellosis H2S− Shigella dysenteriae / sonnei / flexneri / boydii Shigellosis , Bacillary dysentery Proteus mirabilis / Proteus vulgaris Yersinia pestis Plague / Bubonic plague Yersinia enterocolitica Yersiniosis Yersinia pseudotuberculosis Far East scarlet-like fever Pasteurellales Haemophilus : H. influenzae Haemophilus meningitis Brazilian purpuric fever H. ducreyi Chancroid H. parainfluenzae HACEK Pasteurella multocida Pasteurellosis Actinobacillus Actinobacillosis Aggregatibacter actinomycetemcomitans HACEK Legionellales Legionella pneumophila / Legionella longbeachae Legionnaires' disease Coxiella burnetii Q fever Thiotrichales Francisella tularensis Tularemia Vibrionaceae Vibrio cholerae Cholera Vibrio vulnificus Vibrio parahaemolyticus Vibrio alginolyticus Plesiomonas shigelloides Pseudomonadales Pseudomonas aeruginosa Pseudomonas infection Moraxella catarrhalis Acinetobacter baumannii Xanthomonadaceae Stenotrophomonas maltophilia Cardiobacteriaceae Cardiobacterium hominis HACEK Aeromonadales Aeromonas hydrophila / Aeromonas veronii Aeromonas infection ε Campylobacterales Campylobacter jejuni Campylobacteriosis , Guillain–Barré syndrome Helicobacter pylori Peptic ulcer , MALT lymphoma , Gastric cancer Helicobacter cinaedi Helicobacter cellulitis v t e Diseases of the digestive system Upper GI tract Esophagus Esophagitis Candidal Eosinophilic Herpetiform Rupture Boerhaave syndrome Mallory–Weiss syndrome UES Zenker's diverticulum LES Barrett's esophagus Esophageal motility disorder Nutcracker esophagus Achalasia Diffuse esophageal spasm Gastroesophageal reflux disease (GERD) Laryngopharyngeal reflux (LPR) Esophageal stricture Megaesophagus Esophageal intramural pseudodiverticulosis Stomach Gastritis Atrophic Ménétrier's disease Gastroenteritis Peptic (gastric) ulcer Cushing ulcer Dieulafoy's lesion Dyspepsia Pyloric stenosis Achlorhydria Gastroparesis Gastroptosis Portal hypertensive gastropathy Gastric antral vascular ectasia Gastric dumping syndrome Gastric volvulus Buried bumper syndrome Gastrinoma Zollinger–Ellison syndrome Lower GI tract Enteropathy Small intestine ( Duodenum / Jejunum / Ileum ) Enteritis Duodenitis Jejunitis Ileitis Peptic (duodenal) ulcer Curling's ulcer Malabsorption : Coeliac Tropical sprue Blind loop syndrome Small bowel bacterial overgrowth syndrome Whipple's Short bowel syndrome Steatorrhea Milroy disease Bile acid malabsorption Large intestine ( Appendix / Colon ) Appendicitis Colitis Pseudomembranous Ulcerative Ischemic Microscopic Collagenous Lymphocytic Functional colonic disease IBS Intestinal pseudoobstruction / Ogilvie syndrome Megacolon / Toxic megacolon Diverticulitis / Diverticulosis / SCAD Large and/or small Enterocolitis Necrotizing Gastroenterocolitis IBD Crohn's disease Vascular : Abdominal angina Mesenteric ischemia Angiodysplasia Bowel obstruction : Ileus Intussusception Volvulus Fecal impaction Constipation Diarrhea Infectious Intestinal adhesions Rectum Proctitis Radiation proctitis Proctalgia fugax Rectal prolapse Anismus Anal canal Anal fissure / Anal fistula Anal abscess Hemorrhoid Anal dysplasia Pruritus ani GI bleeding Blood in stool Upper Hematemesis Melena Lower Hematochezia Accessory Liver Hepatitis Viral hepatitis Autoimmune hepatitis Alcoholic hepatitis Cirrhosis PBC Fatty liver NASH Vascular Budd–Chiari syndrome Hepatic veno-occlusive disease Portal hypertension Nutmeg liver Alcoholic liver disease Liver failure Hepatic encephalopathy Acute liver failure Liver abscess Pyogenic Amoebic Hepatorenal syndrome Peliosis hepatis Metabolic disorders Wilson's disease Hemochromatosis Gallbladder Cholecystitis Gallstone / Cholelithiasis Cholesterolosis Adenomyomatosis Postcholecystectomy syndrome Porcelain gallbladder Bile duct / Other biliary tree Cholangitis Primary sclerosing cholangitis Secondary sclerosing cholangitis Ascending Cholestasis / Mirizzi's syndrome Biliary fistula Haemobilia Common bile duct Choledocholithiasis Biliary dyskinesia Sphincter of Oddi dysfunction Pancreatic Pancreatitis Acute Chronic Hereditary Pancreatic abscess Pancreatic pseudocyst Exocrine pancreatic insufficiency Pancreatic fistula Other Hernia Diaphragmatic Congenital Hiatus Inguinal Indirect Direct Umbilical Femoral Obturator Spigelian Lumbar Petit's Grynfeltt-Lesshaft Undefined location Incisional Internal hernia Richter's Peritoneal Peritonitis Spontaneous bacterial peritonitis Hemoperitoneum Pneumoperitoneum Authority control GND : 4178684-1 NDL : 00570574
-
Spinocerebellar Ataxia
Wikipedia
CAG repeat , 19p Calcium channel gene SCA7 [14] ( ATXN7 ) 3rd–4th decade (0.5–60) 20 years (1–45; early onset correlates with shorter duration) Macular degeneration , upper motor neuron , slow saccades CAG repeat , 3p ( Ataxin 7 ) SCA8 [15] ( IOSCA ) 39 yrs (18–65) Normal lifespan Horizontal nystagmus (a rapid, involuntary, oscillatory motion of the eyeball ), instability, lack of coordination CTG repeat , [16] 13q SCA10 [17] ( ATXN10 ) 36 years 9 years ataxia , seizures Mexico Chromosome 22q linked pentanucleotide repeat SCA11 ( TTBK2 ) 30 yrs (15–70) Normal lifespan Mild, remain ambulatory (able to walk about on one's own) 15q SCA12 [18] ( PPP2R2B ) 33 yrs (8–55) Head and hand tremor , akinesia (loss of normal motor function, resulting in impaired muscle movement) CAG repeat , 5q SCA13 ( KCNC3 ) Childhood or adulthood depending on mutation Depending on KCNC3 (a kind of gene) Mental retardation 19q SCA14 [19] ( PRKCG ) 28 yrs (12–42) Decades (1–30) Myoclonus (a sudden twitching of muscles or parts of muscles, without any rhythm or pattern, occurring in various brain disorders) 19q SCA16 ( ITPR1 ) 39 yrs (20–66) 1–40 years Head and hand tremor 8q SCA17 ( TBP ) CAG repeat , 6q (TATA-binding protein) SCA19 , SCA22 ( KCND3 [20] ) Mild cerebellar syndrome , dysarthria SCA25 1.5–39 yrs Unknown ataxia with sensory neuropathy , vomiting and gastrointestinal pain . 2p SCA27 [21] ( FGF14 [20] ) 15–20 yrs Unknown ataxia with poor cognition , dyskinesias and tremor . ... Name OMIM RareDiseases Other Anemia, sideroblastic spinocerebellar ataxia; Pagon Bird Detter syndrome 301310 Disease ID 668 at NIH 's Office of Rare Diseases Friedreich's ataxia; Spinocerebellar ataxia, Friedreich 229300 Disease ID 6468 at NIH 's Office of Rare Diseases Infantile onset Spinocerebellar ataxia 605361 Disease ID 4062 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 1 164400 Disease ID 4071 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 2 183090 Disease ID 4072 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 3; Machado Joseph disease 109150 Disease ID 6801 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 4 600223 Disease ID 9970 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 5 600224 Disease ID 4953 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 7 164500 Disease ID 4955 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 8 603680 Disease ID 4956 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 13 605259 Disease ID 9611 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 18 607458 Disease ID 9976 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 19 607346 Disease ID 9969 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 20 608687 Disease ID 9997 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 21 607454 Disease ID 9999 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 23 610245 Disease ID 9950 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 25 608703 Disease ID 9996 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 26 609306 Disease ID 9995 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 28 610246 Disease ID 9951 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 30 117360 Disease ID 9975 at NIH 's Office of Rare Diseases Spinocerebellar ataxia 35 613908 Disease ID at NIH 's Office of Rare Diseases Spinocerebellar ataxia amyotrophy deafness syndrome Disease ID 2451 at NIH 's Office of Rare Diseases ORPHA:2074 at Orphanet Spinocerebellar ataxia, autosomal recessive 1 606002 Disease ID 4949 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, autosomal recessive 3 271250 Disease ID 9971 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, autosomal recessive 4 607317 Disease ID 4952 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, autosomal recessive 5 606937 Disease ID 9977 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, autosomal recessive 6 608029 Disease ID 4954 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, autosomal recessive 21 - mutation in SCYL1 Online Mendelian Inheritance in Man (OMIM): 616719 ORPHA:466794 Spinocerebellar ataxia, autosomal recessive, with axonal neuropathy 607250 Disease ID 10000 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, X-linked, 2 302600 Disease ID 9978 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, X-linked, 3 301790 Disease ID 9981 at NIH 's Office of Rare Diseases Spinocerebellar ataxia, X-linked, 4 301840 Disease ID 9980 at NIH 's Office of Rare Diseases Treatment [ edit ] Medication [ edit ] There is no cure for spinocerebellar ataxia, which is currently considered to be a progressive and irreversible disease, although not all types cause equally severe disability. [22] In general, treatments are directed towards alleviating symptoms, not the disease itself. ... Food & Drug Administration (FDA) [34] and the European Medicines Agency (EMA). [35] Published case series studies have demonstrated the effects of acute treatment with N-Acetyl-Leucine for the treatment of inherited cerebellar ataxias, including Spinocerebellar Ataxias. [36] [37] These studies further demonstrated that the treatment is well tolerated, with a good safety profile. [ citation needed ] A multinational clinical trial investigating N-Acetyl-L-Leucine for the treatment of a related inherited cerebellar ataxia, Ataxia-Telangiectasia , began in 2019. [38] IntraBio is also conducting parallel clinical trials with N-Acetyl-L-Leucine for the treatment of Niemann-Pick disease type C [39] and GM2 Gangliosidosis ( Tay-Sachs and Sandhoff Disease). [40] Future opportunities to develop N-Acetyl-Leucine include Lewy Body Dementia , [41] Amyotrophic lateral sclerosis , Restless Leg Syndrome , Multiple Sclerosis , and Migraine [42] Rehabilitation [ edit ] Physical therapists can assist patients in maintaining their level of independence through therapeutic exercise programmes. ... In GeneReviews Online Mendelian Inheritance in Man (OMIM): Spinocerebellar Ataxia, Autosomal Recessive 1; SCAR1 - 606002 Online Mendelian Inheritance in Man (OMIM): Senataxin; SETX - 608465 External links [ edit ] ataxia at NINDS msa at NINDS opca_doc at NINDS MedlinePlus Encyclopedia : Olivopontocerebellar atrophy Spinocerebellar ataxia 27 at NIH 's Office of Rare Diseases Spinocerebellar ataxia dysmorphism at NIH 's Office of Rare Diseases Classification D ICD - 10 : G11.1 ICD - 9-CM : 334 OMIM : 164400 MeSH : D020754 DiseasesDB : 12339 v t e Diseases of the nervous system , primarily CNS Inflammation Brain Encephalitis Viral encephalitis Herpesviral encephalitis Limbic encephalitis Encephalitis lethargica Cavernous sinus thrombosis Brain abscess Amoebic Brain and spinal cord Encephalomyelitis Acute disseminated Meningitis Meningoencephalitis Brain / encephalopathy Degenerative Extrapyramidal and movement disorders Basal ganglia disease Parkinsonism PD Postencephalitic NMS PKAN Tauopathy PSP Striatonigral degeneration Hemiballismus HD OA Dyskinesia Dystonia Status dystonicus Spasmodic torticollis Meige's Blepharospasm Athetosis Chorea Choreoathetosis Myoclonus Myoclonic epilepsy Akathisia Tremor Essential tremor Intention tremor Restless legs Stiff-person Dementia Tauopathy Alzheimer's Early-onset Primary progressive aphasia Frontotemporal dementia / Frontotemporal lobar degeneration Pick's Dementia with Lewy bodies Posterior cortical atrophy Vascular dementia Mitochondrial disease Leigh syndrome Demyelinating Autoimmune Inflammatory Multiple sclerosis For more detailed coverage, see Template:Demyelinating diseases of CNS Episodic/ paroxysmal Seizures and epilepsy Focal Generalised Status epilepticus For more detailed coverage, see Template:Epilepsy Headache Migraine Cluster Tension For more detailed coverage, see Template:Headache Cerebrovascular TIA Stroke For more detailed coverage, see Template:Cerebrovascular diseases Other Sleep disorders For more detailed coverage, see Template:Sleep CSF Intracranial hypertension Hydrocephalus Normal pressure hydrocephalus Choroid plexus papilloma Idiopathic intracranial hypertension Cerebral edema Intracranial hypotension Other Brain herniation Reye syndrome Hepatic encephalopathy Toxic encephalopathy Hashimoto's encephalopathy Both/either Degenerative SA Friedreich's ataxia Ataxia–telangiectasia MND UMN only: Primary lateral sclerosis Pseudobulbar palsy Hereditary spastic paraplegia LMN only: Distal hereditary motor neuronopathies Spinal muscular atrophies SMA SMAX1 SMAX2 DSMA1 Congenital DSMA Spinal muscular atrophy with lower extremity predominance (SMALED) SMALED1 SMALED2A SMALED2B SMA-PCH SMA-PME Progressive muscular atrophy Progressive bulbar palsy Fazio–Londe Infantile progressive bulbar palsy both: Amyotrophic lateral sclerosis v t e Non-Mendelian inheritance : anticipation Trinucleotide Polyglutamine (PolyQ), CAG Dentatorubral-pallidoluysian atrophy Huntington's disease Kennedy disease Spinocerebellar ataxia 1, 2, 3, 6, 7, 17 ( Machado-Joseph disease ) Non-polyglutamine CGG ( Fragile X syndrome ) GAA ( Friedreich's ataxia ) CTG ( Myotonic dystrophy type 1 ) CTG ( Spinocerebellar ataxia 8 ) CAG ( Spinocerebellar ataxia 12 ) Tetranucleotide CCTG ( Myotonic dystrophy type 2 ) Pentanucleotide ATTCT ( Spinocerebellar ataxia 10 ) v t e Inherited disorders of trafficking / vesicular transport proteins Vesicle formation Lysosome / Melanosome : HPS1 – HPS7 Hermansky–Pudlak syndrome LYST Chédiak–Higashi syndrome COPII : SEC23A Cranio-lenticulo-sutural dysplasia COG7 CDOG IIE APC: AP1S2 X-linked intellectual disability AP3B1 Hermansky–Pudlak syndrome 2 AP4M1 CPSQ3 Rab ARL6 BBS3 RAB27A Griscelli syndrome 2 CHM Choroideremia MLPH Griscelli syndrome 3 Cytoskeleton Myosin : MYO5A Griscelli syndrome 1 Microtubule : SPG4 Hereditary spastic paraplegia 4 Kinesin : KIF5A Hereditary spastic paraplegia 10 Spectrin : SPTBN2 Spinocerebellar ataxia 5 Vesicle fusion Synaptic vesicle : SNAP29 CEDNIK syndrome STX11 Hemophagocytic lymphohistiocytosis 4 Caveolae : CAV1 Congenital generalized lipodystrophy 3 CAV3 Limb-girdle muscular dystrophy 2B , Long QT syndrome 9 Vacuolar protein sorting : VPS33B ARC syndrome VPS13B Cohen syndrome DYSF Distal muscular dystrophy See also vesicular transport proteins Authority control NDL : 01033493