-
Cataract 38
Omim
A number sign (#) is used with this entry because of evidence that autosomal recessive cataract-38 (CTRCT38) is caused by homozygous mutation in the AGK gene (610345) on chromosome 7q34. See also Sengers syndrome (212350), a syndromic form of congenital cataract caused by mutation in AGK.
-
Generalized Erythema
Wikipedia
You can help Wikipedia by expanding it . v t e v t e Urticaria and erythema Urticaria ( acute / chronic ) Allergic urticaria Urticarial allergic eruption Physical urticaria Cold urticaria Familial Primary cold contact urticaria Secondary cold contact urticaria Reflex cold urticaria Heat urticaria Localized heat contact urticaria Solar urticaria Dermatographic urticaria Vibratory angioedema Pressure urticaria Cholinergic urticaria Aquagenic urticaria Other urticaria Acquired C1 esterase inhibitor deficiency Adrenergic urticaria Exercise urticaria Galvanic urticaria Schnitzler syndrome Urticaria-like follicular mucinosis Angioedema Episodic angioedema with eosinophilia Hereditary angioedema Erythema Erythema multiforme / drug eruption Erythema multiforme minor Erythema multiforme major Stevens–Johnson syndrome , Toxic epidermal necrolysis panniculitis ( Erythema nodosum ) Acute generalized exanthematous pustulosis Figurate erythema Erythema annulare centrifugum Erythema marginatum Erythema migrans Erythema gyratum repens Other erythema Necrolytic migratory erythema Erythema toxicum Erythroderma Palmar erythema Generalized erythema
-
Mineral Deficiency
Wikipedia
External links [ edit ] Classification D ICD - 10 : E58 - E61 ICD - 9-CM : 269.3 v t e Malnutrition Protein-energy malnutrition Kwashiorkor Marasmus Catabolysis Vitamin deficiency B vitamins B 1 Beriberi Wernicke–Korsakoff syndrome Wernicke's encephalopathy Korsakoff's syndrome B 2 Riboflavin deficiency B 3 Pellagra B 6 Pyridoxine deficiency B 7 Biotin deficiency B 9 Folate deficiency B 12 Vitamin B 12 deficiency Other A: Vitamin A deficiency Bitot's spots C: Scurvy D: Vitamin D deficiency Rickets Osteomalacia Harrison's groove E: Vitamin E deficiency K: Vitamin K deficiency Mineral deficiency Sodium Potassium Magnesium Calcium Iron Zinc Manganese Copper Iodine Chromium Molybdenum Selenium Keshan disease Growth Delayed milestone Failure to thrive Short stature Idiopathic General Anorexia Weight loss Cachexia Underweight This article about an endocrine, nutritional, or metabolic disease is a stub .
-
Microspherophakia
Wikipedia
This condition may be associated with a number of disorders including Peter's anomaly , Marfan syndrome , and Weill–Marchesani syndrome . [1] The spherical shape is caused by an underdeveloped zonule of Zinn , which doesn't exert enough force on the lens to make it form the usual oval shape. [2] It is a result of a homozygous mutation to the LTBP2 gene. [3] Contents 1 See also 2 References 3 Further reading 4 External links See also [ edit ] Ectopia lentis References [ edit ] ^ "Spherophakia" .
-
Cystica Profunda
Wikipedia
Some consider this synonymous, or closely related to solitary rectal ulcer syndrome , a consequence of internal rectal intussusception . ... See also [ edit ] Solitary rectal ulcer syndrome References [ edit ] ^ Ng, CF; Hull, DA; Feakins, RM; Baithun, S; Dorudi, S (Jan 2004).
-
Omodysplasia 2
Wikipedia
Mutations in the Frizzled Class Receptor 2 ( FZD2 ) gene have been associated with this condition. [1] Diagnosis [ edit ] Differential diagnosis [ edit ] Robinow syndrome Treatment [ edit ] There is no currently known treatment for this condition. History [ edit ] This condition was first described by Maroteaux et al in 1989. [2] References [ edit ] ^ Nagasaki K, Nishimura G, Kikuchi T, Nyuzuki H, Sasaki S, Ogawa Y, Saitoh A (2018) Nonsense mutations in FZD2 cause autosomal-dominant omodysplasia: Robinow syndrome-like phenotypes. Am J Med Genet A doi: 10.1002/ajmg.a.38623 ^ Maroteaux P, Sauvegrain J, Chrispin A, Farriaux, JP (1989) Omodysplasia.
-
Autism, Susceptibility To, 13
Omim
'Autism spectrum disorder,' sometimes referred to as ASD, is a broader phenotype encompassing the less severe disorders Asperger syndrome (see ASPG1; 608638) and pervasive developmental disorder, not otherwise specified (PDD-NOS). ... Mental retardation coexists in approximately two-thirds of individuals with ASD, except for Asperger syndrome, in which mental retardation is conspicuously absent (Jones et al., 2008).
-
Spondylospinal Thoracic Dysostosis
Omim
Clinical Features In 2 sibs, Johnson et al. (1997) described an apparently 'new' syndrome of spondylospinal thoracic dysostosis with a short, curved spine and fusion of the spinous processes, short thorax with 'crab-like' configuration of the ribs, pulmonary hypoplasia, severe arthrogryposis and multiple pterygia, and hypoplastic maxilla and mandible. ... Johnson et al. (1997) concluded that the disorder differed from the Jarcho-Levin syndrome (277300) because in their patients there was clearly a primary bone fusion of the spinus processes of the spinal column with secondary small chest cage; hence, their use of the term spondylospinal thoracic dysostosis.
-
Hypochloremia
Wikipedia
External links [ edit ] Classification D ICD - 10 : E87.8 ICD - 9-CM : 276.9 v t e Electrolyte imbalances Sodium High Salt poisoning Low Hypotonic Isotonic Cerebral salt-wasting syndrome Potassium High Low Chloride High Low Calcium High Low Symptoms and signs Chvostek sign Trousseau sign Milk-alkali syndrome Disorders of calcium metabolism Calcinosis ( Calciphylaxis , Calcinosis cutis ) Calcification ( Metastatic calcification , Dystrophic calcification ) Familial hypocalciuric hypercalcemia Phosphate High Low Magnesium High Low This medical treatment –related article is a stub .
-
Acute Zonal Occult Outer Retinopathy
Wikipedia
Acute zonal occult outer retinopathy Other names AZOOR Specialty Ophthalmology Acute zonal occult outer retinopathy (AZOOR) is an inflammatory retinopathy in the category of white dot syndromes typified by acute loss of one or more zones of outer retinal function associated with photopsia , minimal funduscopic changes and abnormal electroretinography findings. [1] [2] This retinal disease was first described by Gass in 1992. [3] Relatively little is known about the condition. Contents 1 Risk factors 2 Pathophysiology 3 References 4 External links Risk factors [ edit ] Caucasian females in their mid-thirties appear to be most susceptible but the disease may affect anyone regardless of age, sex or race. [3] Pathophysiology [ edit ] The disease mechanism is unknown but it is believed that it may be caused by a virus. [3] References [ edit ] ^ Quillen DA, Davis JB, Gottlieb JL, Blodi BA, Callanan DG, Chang TS, et al. The white dot syndromes. American Journal of Ophthalmology. 2004;137(3):538-50. ^ Carrasco L, Ramos M, Galisteo R, Pisa D, Fresno M, Gonzalez ME.
-
Branchiootorenal Spectrum Disorder
Gene_reviews
Diagnosis Branchiootorenal spectrum disorder comprises branchiootorenal (BOR) syndrome and branchiootic syndrome (BOS), two phenotypes that differ only by the presence or absence of renal abnormality. ... For this reason, these syndromes are best considered as one disorder known as branchiootorenal spectrum disorder. ... Heterozygous pathogenic variants were identified in 10 (4.0%) of 247 unrelated individuals with BORSD syndrome in whom an EYA1 or SIX5 pathogenic variant was not identified [Kochhar et al 2008]. ... Penetrance Based on careful clinical studies of large pedigrees, branchiootorenal spectrum disorder appears to have 100% penetrance, although expressivity is highly variable [Chang et al 2004]. Nomenclature BOR syndrome was originally known eponymously as Melnick-Fraser syndrome. ... Differential Diagnosis More than 400 genetic syndromes that include hearing loss have been described [Toriello & Smith 2013, Korver et al 2017].
-
Pseudohermaphroditism
Wikipedia
What seems like a female phenotype is altered by increased testosterone secretion. [9] Mutations affecting the androgen receptor (AR) gene may cause either complete or partial androgen insensitivity syndrome. Androgens (a term used to describe a group of sex steroid hormones) are responsible for male pseudohermaphroditism. ... Money's defenders have suggested that some of the allegations about the therapy sessions may have been the result of False memory syndrome . However, Reimer's brother and mother both agreed that the therapy was not "working" in the sense that Reimer wasn't in any way developing a female self-image during his treatment with Dr. ... Their sexuality (homosexual, heterosexual, bisexual etc.) is not necessarily determined by this syndrome. However scientifically precise the description "male" pseudohermaphrodite may be for such women, its social inappropriateness is in controversy. ... PMID 2190282 . ^ Patil V, Muktinaini S, Patil R, Verma A (June 2013). "Persistent müllerian duct syndrome: a case report" . The Indian Journal of Surgery . 75 (Suppl 1): 460–2. doi : 10.1007/s12262-013-0831-6 . ... External links [ edit ] Classification D ICD - 10 : Q56.1 - Q56.3 ICD - 9-CM : 752.7 MeSH : D012734 DiseasesDB : 14836 v t e Female congenital anomalies of the genitalia, including Intersex and DSD Internal Uterine malformation Müllerian agenesis Cervical agenesis Unicornuate uterus Uterus didelphys Bicornuate uterus Uterine septum Arcuate uterus Vagina Vaginal septum Vaginal hypoplasia Imperforate hymen Vaginal adenosis Cloacal exstrophy Vaginal atresia External Clitoromegaly Progestin-induced virilization Pseudohermaphroditism True hermaphroditism v t e Male congenital anomalies of the genitalia, including Intersex and DSD Internal Testicle Cryptorchidism Polyorchidism Monorchism Anorchia Sertoli cell-only syndrome True hermaphroditism Mixed gonadal dysgenesis Swyer syndrome Vas deferens Congenital absence of the vas deferens Other Persistent Müllerian duct syndrome External Penis Hypospadias Epispadias Chordee Micropenis Penile agenesis Diphallia Penoscrotal transposition Other Pseudohermaphroditism
-
Splenomegaly
Wikipedia
Splenomegaly may also come from bacterial infections, such as syphilis or an infection of the heart's inner lining ( endocarditis ). [13] Splenomegaly also occurs in mammals parasitized by Cuterebra fontinella . [14] The possible causes of moderate splenomegaly (spleen <1000 g) are many, and include: Splenomegaly grouped on the basis of the pathogenic mechanism Increased function Abnormal blood flow Infiltration Removal of defective RBCs spherocytosis thalassemia hemoglobinopathies nutritional anemias early sickle cell anemia Immune hyperplasia Response to infection (viral, bacterial, fungal, parasitic) mononucleosis , AIDS , [15] viral hepatitis subacute bacterial endocarditis , bacterial sepsis splenic abscess , typhoid fever brucellosis , leptospirosis , tuberculosis histoplasmosis malaria , leishmaniasis , trypanosomiasis ehrlichiosis [16] Disordered immunoregulation rheumatoid arthritis , including cases of Felty's syndrome systemic lupus erythematosus serum sickness familial hemophagocytic lymphohistiocytosis autoimmune hemolytic anemia autoimmune lymphoproliferative syndrome , an autosomal dominant disorder sarcoidosis drug reactions Extramedullary hematopoiesis myelofibrosis marrow infiltration by tumors , leukemias marrow damage by radiation , toxins Organ Failure cirrhosis Vascular hepatic vein obstruction portal vein obstruction Budd–Chiari syndrome splenic vein obstruction Infections hepatic schistosomiasis hepatic echinococcosis Metabolic diseases Gaucher disease Niemann–Pick disease alpha-mannosidosis Hurler syndrome and other mucopolysaccharidoses [17] amyloidosis Tangier disease Benign and malignant “infiltrations” leukemias (acute, chronic, lymphoid, and myeloid) lymphomas ( Hodgkins and non-Hodgkin's ) myeloproliferative disease metastatic tumors (commonly melanoma ) histiocytosis X hemangioma , lymphangioma splenic cysts hamartomas eosinophilic granuloma littoral cell angioma [18] [19] [20] Normal spleen (in green) The causes of massive splenomegaly (spleen >1000 g) are chronic myelogenous leukemia myelofibrosis malaria splenic marginal zone lymphoma Pathophysiology [ edit ] Splenomegaly can be classified based on its pathophysiologic mechanism: Congestive, by pooled blood (e.g., portal hypertension ) Infiltrative, by invasion by cells foreign to the splenic environment (e.g., metastases , myeloid neoplasms , lipid storage diseases ) Immune , by an increase in immunologic activity and subsequent hyperplasia (e.g., endocarditis , sarcoidosis , rheumatoid arthritis ) Neoplastic , when resident immune cells originate a neoplasm (e.g., lymphoma ). [1] Diagnosis [ edit ] Abdominal CT is the most accurate. ... As an adaptation [ edit ] An enlarged spleen may be an inherited, adaptive trait selected in populations that need extra oxygen carry capacity such as deep sea divers. [21] [22] See also [ edit ] Asplenia Hepatosplenomegaly Portal hypertension Sign (medicine) Splenic infarction Tropical splenomegaly syndrome References [ edit ] ^ a b Chapman, J; Azevedo, AM (2018), "article-29386", Splenomegaly , Treasure Island (FL): StatPearls Publishing, PMID 28613657 , retrieved 2019-02-26 ^ Ghazi, Ali (2010). ... External links [ edit ] Splenomegaly and hypersplenism at patient.info Classification D ICD - 10 : Q89.0 , R16.1 ICD - 9-CM : 759.0 , 789.2 MeSH : D013163 DiseasesDB : 12375 External resources MedlinePlus : 003276 eMedicine : ped/2139 med/2156 v t e Lymphatic disease : organ and vessel diseases Thymus Abscess Hyperplasia Hypoplasia DiGeorge syndrome Ectopic thymus Thymoma Thymic carcinoma Spleen Asplenia Asplenia with cardiovascular anomalies Accessory spleen Polysplenia Wandering spleen Splenomegaly Banti's syndrome Splenic infarction Splenic tumor Lymph node Lymphadenopathy Generalized lymphadenopathy Castleman's disease Intranodal palisaded myofibroblastoma Kikuchi disease Tonsils see Template:Respiratory pathology Lymphatic vessels Lymphangitis Lymphangiectasia Lymphedema Primary lymphedema Congenital lymphedema Lymphedema praecox Lymphedema tarda Lymphedema–distichiasis syndrome Milroy's disease Secondary lymphedema Bullous lymphedema Factitial lymphedema Postinflammatory lymphedema Postmastectomy lymphangiosarcoma Waldmann disease v t e Symptoms and signs relating to the human digestive system or abdomen Gastrointestinal tract Nausea Vomiting Heartburn Aerophagia Pagophagia Dysphagia oropharyngeal esophageal Odynophagia Bad breath Xerostomia Hypersalivation Burping Wet burp Goodsall's rule Chilaiditi syndrome Dance's sign Aaron's sign Arapov's sign Markle sign McBurney's point Sherren's triangle Radiologic signs : Hampton's line Klemm's sign Accessory liver : Councilman body Mallory body biliary: Boas' sign Courvoisier's law Charcot's cholangitis triad / Reynolds' pentad cholecystitis ( Murphy's sign Lépine's sign Mirizzi's syndrome ) Nardi test Defecation Flatulence Fecal incontinence Encopresis Fecal occult blood Rectal tenesmus Constipation Obstructed defecation Diarrhea Rectal discharge Psoas sign Obturator sign Rovsing's sign Hamburger sign Heel tap sign Aure-Rozanova's sign Dunphy sign Alder's sign Lockwood's sign Rosenstein's sign Abdomen Pain Abdominal pain Acute abdomen Colic Baby colic Abdominal guarding Blumberg sign Distension Abdominal distension Bloating Ascites Tympanites Shifting dullness Ascites Fluid wave test Masses Abdominal mass Hepatosplenomegaly Hepatomegaly Splenomegaly Other Jaundice Mallet-Guy sign Puddle sign Ballance's sign Aortic insufficiency Castell's sign Kehr's sign Cullen's sign Grey Turner's sign Hernia Howship–Romberg sign Hannington-Kiff sign Other Cupola sign Fothergill's sign Carnett's sign Sister Mary Joseph noduleOCLN, NRAS, HBB, PEPD, XIAP, KRAS, APOE, FAS, CYP1A2, KCNN3, STAT5B, NFE2L2, BDKRB1, FLT3, EIF2AK1, MECOM, NOTCH1, APC, AHR, MAPT, PSEN1, APP, DNASE2, TYMS, ABCB11, STX11, TNFSF11, ALMS1, TNFSF12, TNFRSF11A, ZAP70, AP3B1, GFI1B, DPM1, UROS, KLRC4, ABCA1, AP3D1, SH2B3, NPC2, AGPAT2, RNASEH2A, SEC23B, TCIRG1, RASGRP1, GNE, PLEKHM1, SLC7A7, PIEZO1, LPIN2, TTC37, SEC24C, ADAMTS3, UMPS, CLDN1, CYP7B1, TNFRSF1B, UFD1, TNFRSF4, SOX10, SMPD1, SLCO2A1, SLC4A1, SLC2A1, SKIV2L, SGSH, ATXN2, RREB1, RMRP, RHAG, RAG2, RAG1, RAB27A, PEX2, ABCD3, PTPRC, SPTA1, SPTB, AKR1D1, THPO, HIRA, TPP2, TPI1, TP53, VPS45, TNFRSF1A, TLR4, TGFB1, STAT4, TERT, TERC, TCF4, TBXAS1, TBX1, TALDO1, NEK4, KLF1, TNFRSF13B, DOLK, USB1, C15orf41, CARD11, CCDC115, ITCH, FERMT3, HSD3B7, ALPK1, CTC1, FAT4, NLRP1, CYBC1, GNPTAB, DDRGK1, VPS33A, DCLRE1C, ABCG8, ABCG5, NOD2, COX4I2, TMEM67, COG7, G6PC3, RNU4ATAC, NCF1, GPIHBP1, UBAC2, SUMF1, CAVIN1, JMJD1C, SAMD9L, IL23R, HJV, CCBE1, CDAN1, LACC1, HGSNAT, TNFRSF13C, NLRP3, PIGM, BACH2, NLRC4, HAMP, RTEL1, DCDC2, GLRX5, SBDS, FOXP3, SNX10, ICOS, OSTM1, LAT, BSCL2, SLC17A5, TINF2, IFT172, PSMB9, SF3B1, RPGRIP1L, VPS13A, NBEAL2, DYNC2LI1, ERAP1, CC2D2A, ADA2, WDR35, COG6, SCYL1, INPP5E, BTNL2, ALG1, NGLY1, NHP2, CHD7, SLC39A4, SLC30A10, NOP10, SLC29A3, STEAP3, WRAP53, MKS1, TET2, PTEN, PIK3R1, PSMB8, PSMB4, DKC1, DHCR24, DGUOK, CYBB, CYBA, CTSK, CTNS, CTLA4, CR2, CPOX, COMT, COL2A1, CCR1, CLCN7, ERCC8, LYST, CD81, DNASE1L3, EPB41, EPB42, G6PC, GLB1, GPC3, GBA, GATA2, GATA1, GALE, GAA, FUCA1, ERBB3, FOS, FMO3, FGA, GPC4, FAH, F5, ERCC6, CD40LG, SCARB2, CD28, FASLG, ATP7B, ATP6AP1, ATP6V1B2, ATM, ASAH1, ARVCF, ARSB, APOC2, B2M, APOA1, ANK1, ALDOA, ALAS2, AKT1, AGA, ADA, ATRX, CCND1, CD27, CALR, MS4A1, CD19, RUNX1, CAV1, CASR, CASP10, CASP8, CA2, BCL2, C4A, BTD, BRAF, BPGM, BMP2, BCR, BCL6, GNS, GP1BA, GP1BB, GPC1, NOTCH2, NFKB2, NFKB1, NEU1, NCF4, NCF2, NAGLU, MYD88, MVK, MMUT, MST1, MPL, MIF, MEFV, MCM4, MAN2B1, LYZ, PNP, OTC, PARN, PIK3CD, PSAP, PRKCD, PRF1, PPARG, PKHD1, PKLR, ABL1, PIK3CA, PDGFRA, PIK3C2A, PHYH, PHKG2, PHKA2, ABCB4, ATP8B1, PEX7, SH2D1A, LPL, IGH, HFE, IDUA, IDS, IRF8, HPGD, HLA-DRB1, HLA-B, HK1, HBG2, LMNA, HBG1, HBA2, HBA1, GYPC, GUSB, GPR35, GPI, IFNGR1, IL12A-AS1, IL1RN, IL2RA, LIPA, LIG4, LCAT, LBR, KCNN4, KCNH1, JAK2, ITK, INPPL1, IL12A, IL10, IL7R, IL6, IL2RG, IL2RB, HLA-DQB1, VEGFA, TNFRSF8
-
Alcohol Tolerance
Wikipedia
Sulfonic acids : Acamprosate Religion and alcohol Christian views on alcohol alcohol in the Bible Islam and alcohol History Bratt System Related Index of alcohol-related articles Austrian syndrome Ban on caffeinated alcoholic beverages Brief intervention Gateway drug effect Last call Mood disorder Non-alcoholic fatty liver disease Self-medication Spins Sober companion Sober living houses Sobering center Town drunk Category v t e Psychoactive substance-related disorder General SID Substance intoxication / Drug overdose Substance-induced psychosis Withdrawal : Craving Neonatal withdrawal Post-acute-withdrawal syndrome (PAWS) SUD Substance abuse / Substance-related disorders Physical dependence / Psychological dependence / Substance dependence Combined substance use SUD Polysubstance dependence SID Combined drug intoxication (CDI) Alcohol SID Cardiovascular diseases Alcoholic cardiomyopathy Alcohol flush reaction (AFR) Gastrointestinal diseases Alcoholic liver disease (ALD): Alcoholic hepatitis Auto-brewery syndrome (ABS) Endocrine diseases Alcoholic ketoacidosis (AKA) Nervous system diseases Alcohol-related dementia (ARD) Alcohol intoxication Hangover Neurological disorders Alcoholic hallucinosis Alcoholic polyneuropathy Alcohol-related brain damage Alcohol withdrawal syndrome (AWS): Alcoholic hallucinosis Delirium tremens (DTs) Fetal alcohol spectrum disorder (FASD) Fetal alcohol syndrome (FAS) Korsakoff syndrome Positional alcohol nystagmus (PAN) Wernicke–Korsakoff syndrome (WKS, Korsakoff psychosis) Wernicke encephalopathy (WE) Respiratory tract diseases Alcohol-induced respiratory reactions Alcoholic lung disease SUD Alcoholism (alcohol use disorder (AUD)) Binge drinking Caffeine SID Caffeine-induced anxiety disorder Caffeine-induced sleep disorder Caffeinism SUD Caffeine dependence Cannabis SID Cannabis arteritis Cannabinoid hyperemesis syndrome (CHS) SUD Amotivational syndrome Cannabis use disorder (CUD) Synthetic cannabinoid use disorder Cocaine SID Cocaine intoxication Prenatal cocaine exposure (PCE) SUD Cocaine dependence Hallucinogen SID Acute intoxication from hallucinogens (bad trip) Hallucinogen persisting perception disorder (HPPD) Nicotine SID Nicotine poisoning Nicotine withdrawal SUD Nicotine dependence Opioids SID Opioid overdose SUD Opioid use disorder (OUD) Sedative / hypnotic SID Kindling (sedative–hypnotic withdrawal) benzodiazepine : SID Benzodiazepine overdose Benzodiazepine withdrawal SUD Benzodiazepine use disorder (BUD) Benzodiazepine dependence barbiturate : SID Barbiturate overdose SUD Barbiturate dependence Stimulants SID Stimulant psychosis amphetamine : SUD Amphetamine dependence Volatile solvent SID Sudden sniffing death syndrome (SSDS) Toluene toxicity SUD Inhalant abuse
-
Infantile Esotropia
Wikipedia
The same condition had also previously been described by other ophthalmologists, notably Cianca (1962) who named it Cianca's Syndrome and noted the presence of manifest latent nystagmus , and Lang (1968) who called it Congenital Esotropia Syndrome and noted the presence of abnormal head postures. ... Cross-fixation [ edit ] Cross-fixation congenital esotropia , also called Cianci's syndrome is a particular type of large-angle infantile esotropia associated with tight medius rectus muscles. ... Further recent evidence indicates that a cause for infantile strabismus may lie with the input that is provided to the visual cortex . [6] In particular, neonates who suffer injuries that, directly or indirectly, perturb binocular inputs into the primary visual cortex (V1) have a far higher risk of developing strabismus than other infants. [7] Diagnosis [ edit ] Differential Diagnosis [ edit ] Clinically Infantile esotropia must be distinguished from: VIth Cranial nerve or abducens palsy Nystagmus Blockage Syndrome Esotropia arising secondary to central nervous system abnormalities (in cerebral palsy for example) Primary Constant esotropia Duane's Syndrome Treatment [ edit ] According to a Cochrane review of 2012, controversies remain regarding type of surgery, non-surgical intervention and age of intervention. [8] The aims of treatment are as follows: The elimination of any amblyopia A cosmetically acceptable ocular alignment Long-term stability of eye position Binocular cooperation Initially [ edit ] It is essential that a child with strabismus is presented to the ophthalmologist as early as possible for diagnosis and treatment in order to allow best possible monocular and binocular vision to develop. ... PMID 20508049 . ^ Babies' Development 'Catches Up' After Surgery To Fix Crossed Eyes , sciencedaily.com, 21 April 2008 (downloaded 4 October 2013) ^ Six-Year-Olds With Squint Less Likely to Be Invited to Birthday Parties, Study Suggests , sciencedaily.com, 19 August 2010 (downloaded 4 October 2013) External links [ edit ] Classification D External resources eMedicine : article/1198876 Infantile esotropia , Medscape, updated 30 May 2012 v t e Congenital malformations and deformations of eyes Adnexa Eyelid Ptosis Ectropion Entropion Distichia Blepharophimosis Ablepharon Marcus Gunn phenomenon Lacrimal apparatus Congenital lacrimal duct obstruction Globe Entire eye Anophthalmia ( Cystic eyeball , Cryptophthalmos ) Microphthalmia Lens Ectopia lentis Aphakia Iris Aniridia Anterior segment Axenfeld–Rieger syndrome Cornea Keratoglobus Megalocornea Other Buphthalmos Coloboma ( Coloboma of optic nerve ) Hydrophthalmos Norrie disease v t e Infants and their care Health ( Pediatrics ) Baby food Birth weight Breast pump Breastfeeding Breastfeeding and medications Bottle feeding Colic Immunizations Cradle cap Cross eyed Failure to thrive Immunization Infant and toddler safety Infant bathing Infant food safety Infant formula Infant massage Infant food safety Infant nutrition Infant respiratory distress syndrome Infant sleep training Neo-natal intensive care unit Newborn care and safety Oral rehydration therapy Pedialyte Preterm birth Shaken baby syndrome Soy formula Sudden infant death syndrome Breastfeeding and mental health Development Attachment parenting Baby-led weaning Baby talk Babbling Childbirth Congenital disorder Crawling Infant visual development Diaper rash Gestational age Infant cognitive development Kangaroo care Mother Nursery Rhyme Object permanence Parent Parenting Peekaboo Play Prenatal development Prenatal development table Teething Types of crying Walking Weaning Socialization and Culture Attachment Babysitting Child abuse Child custody Child's rights UN Child rights Circumcision Daycare Foster care Grandparent visitation Infant swimming Milk bank Nanny Wet nurse Infant care and equipment Baby bouncer Baby gate Baby monitor / Hidden camera Baby powder Baby shampoo Baby toy Baby walker Bib Baby swing Baby transport Bassinet Car seat safety Cloth diaper Cradle board Diaper Diaper bag Baby wipes Haberman Feeder High chair Infant bed (American 'crib' and 'cradle', British 'cot') Infant carrier Infant clothing Pacifier Playpen Stroller Supplemental nursing system Swaddling Swim diaper Teether Travel cot Other topics Baby shower Babywearing Child neglect Closed adoption Cry room Infant ear piercing Open adoption Prenatal cocaine exposure Neonatal withdrawal syndrome Parental child abduction Parental responsibility Parenting plan Paternity Paternity fraud
-
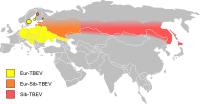
Tick-Borne Encephalitis
Wikipedia
Symptomatic brain damage requires hospitalization and supportive care based on syndrome severity. Anti-inflammatory drugs , such as corticosteroids , may be considered under specific circumstances for symptomatic relief. ... External links [ edit ] Classification D ICD - 10 : A84 ICD - 9-CM : 063 MeSH : D004675 DiseasesDB : 29274 External resources Patient UK : Tick-borne encephalitis Tickborne encephalitis at Centers for Disease Control and Prevention (CDC) Factsheet from Viral Special Pathogens Branch at the CDC v t e Infectious diseases – viral systemic diseases Oncovirus DNA virus HBV Hepatocellular carcinoma HPV Cervical cancer Anal cancer Penile cancer Vulvar cancer Vaginal cancer Oropharyngeal cancer KSHV Kaposi's sarcoma EBV Nasopharyngeal carcinoma Burkitt's lymphoma Hodgkin lymphoma Follicular dendritic cell sarcoma Extranodal NK/T-cell lymphoma, nasal type MCPyV Merkel-cell carcinoma RNA virus HCV Hepatocellular carcinoma Splenic marginal zone lymphoma HTLV-I Adult T-cell leukemia/lymphoma Immune disorders HIV AIDS Central nervous system Encephalitis / meningitis DNA virus Human polyomavirus 2 Progressive multifocal leukoencephalopathy RNA virus MeV Subacute sclerosing panencephalitis LCV Lymphocytic choriomeningitis Arbovirus encephalitis Orthomyxoviridae (probable) Encephalitis lethargica RV Rabies Chandipura vesiculovirus Herpesviral meningitis Ramsay Hunt syndrome type 2 Myelitis Poliovirus Poliomyelitis Post-polio syndrome HTLV-I Tropical spastic paraparesis Eye Cytomegalovirus Cytomegalovirus retinitis HSV Herpes of the eye Cardiovascular CBV Pericarditis Myocarditis Respiratory system / acute viral nasopharyngitis / viral pneumonia DNA virus Epstein–Barr virus EBV infection / Infectious mononucleosis Cytomegalovirus RNA virus IV : Human coronavirus 229E / NL63 / HKU1 / OC43 Common cold MERS coronavirus Middle East respiratory syndrome SARS coronavirus Severe acute respiratory syndrome SARS coronavirus 2 Coronavirus disease 2019 V , Orthomyxoviridae : Influenza virus A / B / C / D Influenza / Avian influenza V, Paramyxoviridae : Human parainfluenza viruses Parainfluenza Human orthopneumovirus hMPV Human digestive system Pharynx / Esophagus MuV Mumps Cytomegalovirus Cytomegalovirus esophagitis Gastroenteritis / diarrhea DNA virus Adenovirus Adenovirus infection RNA virus Rotavirus Norovirus Astrovirus Coronavirus Hepatitis DNA virus HBV ( B ) RNA virus CBV HAV ( A ) HCV ( C ) HDV ( D ) HEV ( E ) HGV ( G ) Pancreatitis CBV Urogenital BK virus MuV Mumps v t e Zoonotic viral diseases (A80–B34, 042–079 ) Arthropod -borne Mosquito -borne Bunyavirales Arbovirus encephalitides : La Crosse encephalitis LACV Batai virus BATV Bwamba Fever BWAV California encephalitis CEV Jamestown Canyon encephalitis Tete virus Tahyna virus TAHV Viral hemorrhagic fevers : Rift Valley fever RVFV Bunyamwera fever BUNV Ngari virus NRIV Flaviviridae Arbovirus encephalitides : Japanese encephalitis JEV Australian encephalitis MVEV KUNV Saint Louis encephalitis SLEV Usutu virus West Nile fever WNV Viral hemorrhagic fevers : Dengue fever DENV-1-4 Yellow fever YFV Zika fever Zika virus Togaviridae Arbovirus encephalitides : Eastern equine encephalomyelitis EEEV Western equine encephalomyelitis WEEV Venezuelan equine encephalomyelitis VEEV Chikungunya CHIKV O'nyong'nyong fever ONNV Pogosta disease Sindbis virus Ross River fever RRV Semliki Forest virus Reoviridae Banna virus encephalitis Tick -borne Bunyavirales Viral hemorrhagic fevers : Bhanja virus Crimean–Congo hemorrhagic fever (CCHFV) Heartland virus Severe fever with thrombocytopenia syndrome ( Huaiyangshan banyangvirus ) Tete virus Flaviviridae Arbovirus encephalitides : Tick-borne encephalitis TBEV Powassan encephalitis POWV Viral hemorrhagic fevers : Omsk hemorrhagic fever OHFV Kyasanur Forest disease KFDV AHFV Langat virus LGTV Orthomyxoviridae Bourbon virus Reoviridae Colorado tick fever CTFV Kemerovo tickborne viral fever Sandfly -borne Bunyavirales Adria virus (ADRV) Oropouche fever Oropouche virus Pappataci fever Toscana virus Sandfly fever Naples virus Rhabdoviridae Chandipura virus Mammal -borne Rodent -borne Arenaviridae Viral hemorrhagic fevers : Lassa fever LASV Venezuelan hemorrhagic fever GTOV Argentine hemorrhagic fever JUNV Brazilian hemorrhagic fever SABV Bolivian hemorrhagic fever MACV LUJV CHPV Bunyavirales Hemorrhagic fever with renal syndrome DOBV HTNV PUUV SEOV AMRV THAIV Hantavirus pulmonary syndrome ANDV SNV Herpesviridae Murid gammaherpesvirus 4 Bat -borne Filoviridae BDBV SUDV TAFV Marburg virus disease MARV RAVV Rhabdoviridae Rabies ABLV MOKV DUVV LBV CHPV Paramyxoviridae Henipavirus encephalitis HeV NiV Coronaviridae SARS-related coronavirus SARS-CoV MERS-CoV SARS-CoV-2 Primate -borne Herpesviridae Macacine alphaherpesvirus 1 Retroviridae Simian foamy virus HTLV-1 HTLV-2 Poxviridae Tanapox Yaba monkey tumor virus Multiple vectors Rhabdoviridae Rabies RABV Mokola virus Poxviridae Monkeypox v t e Tick-borne diseases and infestations Diseases Bacterial infections Rickettsiales Anaplasmosis Boutonneuse fever Ehrlichiosis ( Human granulocytic , Human monocytotropic , Human E. ewingii infection ) Scrub typhus Spotted fever rickettsiosis Pacific Coast tick fever American tick bite fever rickettsialpox Rocky Mountain spotted fever ) Spirochaete Baggio–Yoshinari syndrome Lyme disease Relapsing fever borreliosis Thiotrichales Tularemia Viral infections Bhanja virus Bourbon virus Colorado tick fever Crimean–Congo hemorrhagic fever Heartland bandavirus Kemerovo tickborne viral fever Kyasanur Forest disease Omsk hemorrhagic fever Powassan encephalitis Severe fever with thrombocytopenia syndrome Tete orthobunyavirus Tick-borne encephalitis Protozoan infections Babesiosis Other diseases Tick paralysis Alpha-gal allergy Southern tick-associated rash illness Infestations Tick infestation Species and bites Amblyomma Amblyomma americanum Amblyomma cajennense Amblyomma triguttatum Dermacentor Dermacentor andersoni Dermacentor variabilis Ixodes Ixodes cornuatus Ixodes holocyclus Ixodes pacificus Ixodes ricinus Ixodes scapularis Ornithodoros Ornithodoros gurneyi Ornithodoros hermsi Ornithodoros moubata Other Rhipicephalus sanguineus Authority control GND : 4155540-5 LCCN : sh85042978IL10, ERVK-6, ERVK-32, TLR3, CCR5, IFNL3, CD209, IVNS1ABP, CCL5, CCL4, PTPN11, CCL3, IL5, RSAD2, CXCL8, CRP, IL17F, AVP, CCL20, TIA1, TIAL1, TLR2, DSC3, TNF, OASL, TNFRSF11A, CCL4L2, CSF2, ERVW-1, GC, IL22, ARID1B, CD48, ERVK-20, CCL4L1, ENO2, CXCL2, HMGB1, CCL2, HSPA4, IFNAR1, IL1B, IL2, CXCR2, CXCL1, IRF3, LAMC2, LTF, MAPT, MIF, CXCL9, MMP9, PEPD, STS, RAF1, S100A1, S100B, SAT1, ANXA13
-
Salivary Gland Disease
Wikipedia
Second, this reduction may also impair the secretion of antimicrobial proteins and peptides. [5] Considering presence of many proteins and peptides with established antiviral properties in saliva, some of which can potentially inhibit virus replication especially coronavirus, it gives the impression that the protective effect of these salivary proteins against the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) might be the same. [6] Therefore, hyposalivation could be a potential risk factor for acute respiratory infection. ... This manifests as red patches or spots on a white background. [10] Autoimmune [ edit ] Sjögren's syndrome Graft-versus-host disease Inflammatory [ edit ] Post-irradiation sialadenitis Sarcoidosis —there may be parotitis alone or uveoparotitis (inflammation of both the parotid and the uvea of the eyes), which occurs in Heerfordt's syndrome . Cheilitis glandularis —This is inflammation of the minor salivary glands, usually in the lower lip, eversion and swelling of the lip. [9] Chronic sclerosing sialadenitis is a salivary gland manifestation of IgG4-related disease . [11] [12] Neurological [ edit ] Frey's syndrome Neoplastic [ edit ] Salivary gland neoplasm Diverticulum [ edit ] A salivary diverticulum (plural diverticuli ) is a small pouch or out-pocketing of the duct system of a major salivary gland . [13] Such diverticuli typically cause pooling of saliva and recurrent sialadenitis , [14] especially parotitis . [15] A diverticulum may also cause a sialolith to form. [16] [17] The condition can be diagnosed by sialography . [14] Affected individuals may "milk" the salivary gland to encourage flow of saliva through the duct. [14] Unknown [ edit ] Sialolithiasis - although several possibly coexisting factors have been suggested to be involved in the formation of salivary stones, including altered acidity of saliva, reduced salivary flow rate, abnormal calcium metabolism and abnormalities in the sphincter mechanism of the duct opening, the exact cause in many cases is unknown. ... External links [ edit ] Classification D MeSH : D012466 Wikimedia Commons has media related to Diseases and disorders of salivary glands . v t e Oral and maxillofacial pathology Lips Cheilitis Actinic Angular Plasma cell Cleft lip Congenital lip pit Eclabium Herpes labialis Macrocheilia Microcheilia Nasolabial cyst Sun poisoning Trumpeter's wart Tongue Ankyloglossia Black hairy tongue Caviar tongue Crenated tongue Cunnilingus tongue Fissured tongue Foliate papillitis Glossitis Geographic tongue Median rhomboid glossitis Transient lingual papillitis Glossoptosis Hypoglossia Lingual thyroid Macroglossia Microglossia Rhabdomyoma Palate Bednar's aphthae Cleft palate High-arched palate Palatal cysts of the newborn Inflammatory papillary hyperplasia Stomatitis nicotina Torus palatinus Oral mucosa – Lining of mouth Amalgam tattoo Angina bullosa haemorrhagica Behçet's disease Bohn's nodules Burning mouth syndrome Candidiasis Condyloma acuminatum Darier's disease Epulis fissuratum Erythema multiforme Erythroplakia Fibroma Giant-cell Focal epithelial hyperplasia Fordyce spots Hairy leukoplakia Hand, foot and mouth disease Hereditary benign intraepithelial dyskeratosis Herpangina Herpes zoster Intraoral dental sinus Leukoedema Leukoplakia Lichen planus Linea alba Lupus erythematosus Melanocytic nevus Melanocytic oral lesion Molluscum contagiosum Morsicatio buccarum Oral cancer Benign: Squamous cell papilloma Keratoacanthoma Malignant: Adenosquamous carcinoma Basaloid squamous carcinoma Mucosal melanoma Spindle cell carcinoma Squamous cell carcinoma Verrucous carcinoma Oral florid papillomatosis Oral melanosis Smoker's melanosis Pemphigoid Benign mucous membrane Pemphigus Plasmoacanthoma Stomatitis Aphthous Denture-related Herpetic Smokeless tobacco keratosis Submucous fibrosis Ulceration Riga–Fede disease Verruca vulgaris Verruciform xanthoma White sponge nevus Teeth ( pulp , dentin , enamel ) Amelogenesis imperfecta Ankylosis Anodontia Caries Early childhood caries Concrescence Failure of eruption of teeth Dens evaginatus Talon cusp Dentin dysplasia Dentin hypersensitivity Dentinogenesis imperfecta Dilaceration Discoloration Ectopic enamel Enamel hypocalcification Enamel hypoplasia Turner's hypoplasia Enamel pearl Fluorosis Fusion Gemination Hyperdontia Hypodontia Maxillary lateral incisor agenesis Impaction Wisdom tooth impaction Macrodontia Meth mouth Microdontia Odontogenic tumors Keratocystic odontogenic tumour Odontoma Dens in dente Open contact Premature eruption Neonatal teeth Pulp calcification Pulp stone Pulp canal obliteration Pulp necrosis Pulp polyp Pulpitis Regional odontodysplasia Resorption Shovel-shaped incisors Supernumerary root Taurodontism Trauma Avulsion Cracked tooth syndrome Vertical root fracture Occlusal Tooth loss Edentulism Tooth wear Abrasion Abfraction Acid erosion Attrition Periodontium ( gingiva , periodontal ligament , cementum , alveolus ) – Gums and tooth-supporting structures Cementicle Cementoblastoma Gigantiform Cementoma Eruption cyst Epulis Pyogenic granuloma Congenital epulis Gingival enlargement Gingival cyst of the adult Gingival cyst of the newborn Gingivitis Desquamative Granulomatous Plasma cell Hereditary gingival fibromatosis Hypercementosis Hypocementosis Linear gingival erythema Necrotizing periodontal diseases Acute necrotizing ulcerative gingivitis Pericoronitis Peri-implantitis Periodontal abscess Periodontal trauma Periodontitis Aggressive As a manifestation of systemic disease Chronic Perio-endo lesion Teething Periapical, mandibular and maxillary hard tissues – Bones of jaws Agnathia Alveolar osteitis Buccal exostosis Cherubism Idiopathic osteosclerosis Mandibular fracture Microgenia Micrognathia Intraosseous cysts Odontogenic : periapical Dentigerous Buccal bifurcation Lateral periodontal Globulomaxillary Calcifying odontogenic Glandular odontogenic Non-odontogenic: Nasopalatine duct Median mandibular Median palatal Traumatic bone Osteoma Osteomyelitis Osteonecrosis Bisphosphonate-associated Neuralgia-inducing cavitational osteonecrosis Osteoradionecrosis Osteoporotic bone marrow defect Paget's disease of bone Periapical abscess Phoenix abscess Periapical periodontitis Stafne defect Torus mandibularis Temporomandibular joints , muscles of mastication and malocclusions – Jaw joints, chewing muscles and bite abnormalities Bruxism Condylar resorption Mandibular dislocation Malocclusion Crossbite Open bite Overbite Overeruption Overjet Prognathia Retrognathia Scissor bite Maxillary hypoplasia Temporomandibular joint dysfunction Salivary glands Benign lymphoepithelial lesion Ectopic salivary gland tissue Frey's syndrome HIV salivary gland disease Necrotizing sialometaplasia Mucocele Ranula Pneumoparotitis Salivary duct stricture Salivary gland aplasia Salivary gland atresia Salivary gland diverticulum Salivary gland fistula Salivary gland hyperplasia Salivary gland hypoplasia Salivary gland neoplasms Benign: Basal cell adenoma Canalicular adenoma Ductal papilloma Monomorphic adenoma Myoepithelioma Oncocytoma Papillary cystadenoma lymphomatosum Pleomorphic adenoma Sebaceous adenoma Malignant: Acinic cell carcinoma Adenocarcinoma Adenoid cystic carcinoma Carcinoma ex pleomorphic adenoma Lymphoma Mucoepidermoid carcinoma Sclerosing polycystic adenosis Sialadenitis Parotitis Chronic sclerosing sialadenitis Sialectasis Sialocele Sialodochitis Sialosis Sialolithiasis Sjögren's syndrome Orofacial soft tissues – Soft tissues around the mouth Actinomycosis Angioedema Basal cell carcinoma Cutaneous sinus of dental origin Cystic hygroma Gnathophyma Ludwig's angina Macrostomia Melkersson–Rosenthal syndrome Microstomia Noma Oral Crohn's disease Orofacial granulomatosis Perioral dermatitis Pyostomatitis vegetans Other Eagle syndrome Hemifacial hypertrophy Facial hemiatrophy Oral manifestations of systemic disease
-
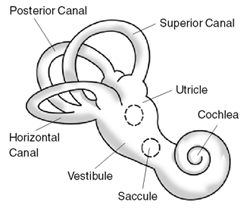
Vertigo, Benign Recurrent
Omim
Acetazolamide stopped or markedly decreased the frequency of vertigo attacks in the 3 patients treated, but had little affect on the chronic vestibular loss. The syndrome, referred to as Dandy syndrome by Belal (1980) and described by Dandy (1941), is characterized by the features reported here. Although some ototoxins, such as streptomycin and gentamicin, are relatively specific for the vestibular system, other causes of Dandy syndrome also produce severe bilateral hearing loss.
-
Arrhythmogenic Right Ventricular Cardiomyopathy
Orphanet
ARVC can be associated with palmoplantar keratoderma and woolly hair, the so-called cardio cutaneous syndromes (Naxos disease and Carvajal syndromes, see these terms). ... Genetic counseling In more than half of the patients, the disease is familial, primarily autosomal dominant with variable penetrance and polymorphic expressivity. Naxos disease and Carvajal syndrome show an autosomal recessive mode of inheritance.PKP2, RYR2, SCN5A, PPP1R13L, TMEM43, DSC2, DSG2, DSP, JUP, DES, LMNA, CTNNA3, DSG2-AS1, ACTN2, TGFB3, ARVD3, PLN, TTN, CTNNB1, MYBPC3, PPARG, GJA1, FLNC, CDH2, MYH7, PIK3CG, ISL1, TGFB1, EBI3, AKAP6, IL18R1, ERVK-15, TP63, HCN4, UVRAG, GJC1, HACD1, OBSCN, CELF1, MIR494, CELF2, CKAP4, LDB3, TPM1, MIR135B, ANKRD1, MIR21, ISM2, PRKAG2, PERP, GNPTAB, MMRN1, AAVS1, TJP1, MEF2C, ARVD4, CEBPA, ACE, ELAVL2, ESRRB, FABP4, FASN, GAPDH, GFAP, GJA5, GSK3B, KCNQ1, MET, STRN, PIK3CA, PIK3CB, PIK3CD, PLEC, PPARA, PRB1, PRKG1, REN, RPE65, RYR1, SCN10A, SLC8A1, KDM5A
-
Punctate Epithelial Erosions
Wikipedia
Cause [ edit ] Punctate epithelial erosions may be seen with different disorders: Rosacea Dry-eye syndrome Blepharitis Acute bacterial conjunctivitis [1] Trauma Exposure keratopathy from poor eyelide closure Ultraviolet or chemical burn Contact lens-related disorder such as toxicity or tight lens syndrome Trichiasis Entropion or ectropion Floppy eyelid syndrome Chemotherapy i.e. cytosine arabinoside Thygeson's Superficial Punctate Keratopathy Diagnosis [ edit ] This section is empty.