-
Hypertensive Disease Of Pregnancy
Wikipedia
This classification treats HELLP syndrome as a type of preeclampsia rather than a parallel entity. [9] Preeclampsia [ edit ] Preeclampsia is a condition that typically starts after the 20th week of pregnancy and is related to increased blood pressure and protein in the mother's urine (as a result of kidney problems). ... ISBN 978-0-9927545-5-6 . [1] ==External links== Hypertensive disease of pregnancy at Curlie v t e Pathology of pregnancy , childbirth and the puerperium Pregnancy Pregnancy with abortive outcome Abortion Ectopic pregnancy Abdominal Cervical Interstitial Ovarian Heterotopic Embryo loss Fetal resorption Molar pregnancy Miscarriage Stillbirth Oedema , proteinuria and hypertensive disorders Gestational hypertension Pre-eclampsia HELLP syndrome Eclampsia Other, predominantly related to pregnancy Digestive system Acute fatty liver of pregnancy Gestational diabetes Hepatitis E Hyperemesis gravidarum Intrahepatic cholestasis of pregnancy Integumentary system / dermatoses of pregnancy Gestational pemphigoid Impetigo herpetiformis Intrahepatic cholestasis of pregnancy Linea nigra Prurigo gestationis Pruritic folliculitis of pregnancy Pruritic urticarial papules and plaques of pregnancy (PUPPP) Striae gravidarum Nervous system Chorea gravidarum Blood Gestational thrombocytopenia Pregnancy-induced hypercoagulability Maternal care related to the fetus and amniotic cavity amniotic fluid Oligohydramnios Polyhydramnios Braxton Hicks contractions chorion / amnion Amniotic band syndrome Chorioamnionitis Chorionic hematoma Monoamniotic twins Premature rupture of membranes Obstetrical bleeding Antepartum placenta Circumvallate placenta Monochorionic twins Placenta accreta Placenta praevia Placental abruption Twin-to-twin transfusion syndrome Labor Amniotic fluid embolism Cephalopelvic disproportion Dystocia Shoulder dystocia Fetal distress Locked twins Nuchal cord Obstetrical bleeding Postpartum Pain management during childbirth placenta Placenta accreta Preterm birth Postmature birth Umbilical cord prolapse Uterine inversion Uterine rupture Vasa praevia Puerperal Breastfeeding difficulties Low milk supply Cracked nipples Breast engorgement Childbirth-related posttraumatic stress disorder Diastasis symphysis pubis Postpartum bleeding Peripartum cardiomyopathy Postpartum depression Postpartum psychosis Postpartum thyroiditis Puerperal fever Puerperal mastitis Other Concomitant conditions Diabetes mellitus Systemic lupus erythematosus Thyroid disorders Maternal death Sexual activity during pregnancy Category ^ Tinawi, Mohammad (8 January 2020).
-
Tinea Versicolor
Wikipedia
External links [ edit ] Classification D ICD - 10 : B36.0 ICD - 9-CM : 111.0 MeSH : D014010 DiseasesDB : 10071 External resources MedlinePlus : 001465 eMedicine : derm/423 Media related to Tinea versicolor at Wikimedia Commons v t e Diseases of the skin and appendages by morphology Growths Epidermal Wart Callus Seborrheic keratosis Acrochordon Molluscum contagiosum Actinic keratosis Squamous-cell carcinoma Basal-cell carcinoma Merkel-cell carcinoma Nevus sebaceous Trichoepithelioma Pigmented Freckles Lentigo Melasma Nevus Melanoma Dermal and subcutaneous Epidermal inclusion cyst Hemangioma Dermatofibroma (benign fibrous histiocytoma) Keloid Lipoma Neurofibroma Xanthoma Kaposi's sarcoma Infantile digital fibromatosis Granular cell tumor Leiomyoma Lymphangioma circumscriptum Myxoid cyst Rashes With epidermal involvement Eczematous Contact dermatitis Atopic dermatitis Seborrheic dermatitis Stasis dermatitis Lichen simplex chronicus Darier's disease Glucagonoma syndrome Langerhans cell histiocytosis Lichen sclerosus Pemphigus foliaceus Wiskott–Aldrich syndrome Zinc deficiency Scaling Psoriasis Tinea ( Corporis Cruris Pedis Manuum Faciei ) Pityriasis rosea Secondary syphilis Mycosis fungoides Systemic lupus erythematosus Pityriasis rubra pilaris Parapsoriasis Ichthyosis Blistering Herpes simplex Herpes zoster Varicella Bullous impetigo Acute contact dermatitis Pemphigus vulgaris Bullous pemphigoid Dermatitis herpetiformis Porphyria cutanea tarda Epidermolysis bullosa simplex Papular Scabies Insect bite reactions Lichen planus Miliaria Keratosis pilaris Lichen spinulosus Transient acantholytic dermatosis Lichen nitidus Pityriasis lichenoides et varioliformis acuta Pustular Acne vulgaris Acne rosacea Folliculitis Impetigo Candidiasis Gonococcemia Dermatophyte Coccidioidomycosis Subcorneal pustular dermatosis Hypopigmented Tinea versicolor Vitiligo Pityriasis alba Postinflammatory hyperpigmentation Tuberous sclerosis Idiopathic guttate hypomelanosis Leprosy Hypopigmented mycosis fungoides Without epidermal involvement Red Blanchable Erythema Generalized Drug eruptions Viral exanthems Toxic erythema Systemic lupus erythematosus Localized Cellulitis Abscess Boil Erythema nodosum Carcinoid syndrome Fixed drug eruption Specialized Urticaria Erythema ( Multiforme Migrans Gyratum repens Annulare centrifugum Ab igne ) Nonblanchable Purpura Macular Thrombocytopenic purpura Actinic/solar purpura Papular Disseminated intravascular coagulation Vasculitis Indurated Scleroderma / morphea Granuloma annulare Lichen sclerosis et atrophicus Necrobiosis lipoidica Miscellaneous disorders Ulcers Hair Telogen effluvium Androgenic alopecia Alopecia areata Systemic lupus erythematosus Tinea capitis Loose anagen syndrome Lichen planopilaris Folliculitis decalvans Acne keloidalis nuchae Nail Onychomycosis Psoriasis Paronychia Ingrown nail Mucous membrane Aphthous stomatitis Oral candidiasis Lichen planus Leukoplakia Pemphigus vulgaris Mucous membrane pemphigoid Cicatricial pemphigoid Herpesvirus Coxsackievirus Syphilis Systemic histoplasmosis Squamous-cell carcinoma v t e Fungal infection and mesomycetozoea Superficial and cutaneous ( dermatomycosis ): Tinea = skin ; Piedra ( exothrix / endothrix ) = hair Ascomycota Dermatophyte ( Dermatophytosis ) By location Tinea barbae / tinea capitis Kerion Tinea corporis Ringworm Dermatophytids Tinea cruris Tinea manuum Tinea pedis (athlete's foot) Tinea unguium/onychomycosis White superficial onychomycosis Distal subungual onychomycosis Proximal subungual onychomycosis Tinea corporis gladiatorum Tinea faciei Tinea imbricata Tinea incognito Favus By organism Epidermophyton floccosum Microsporum canis Microsporum audouinii Trichophyton interdigitale/mentagrophytes Trichophyton tonsurans Trichophyton schoenleini Trichophyton rubrum Trichophyton verrucosum Other Hortaea werneckii Tinea nigra Piedraia hortae Black piedra Basidiomycota Malassezia furfur Tinea versicolor Pityrosporum folliculitis Trichosporon White piedra Subcutaneous , systemic , and opportunistic Ascomycota Dimorphic (yeast+mold) Onygenales Coccidioides immitis / Coccidioides posadasii Coccidioidomycosis Disseminated coccidioidomycosis Primary cutaneous coccidioidomycosis .
-
Tibial Plateau Fracture
Wikipedia
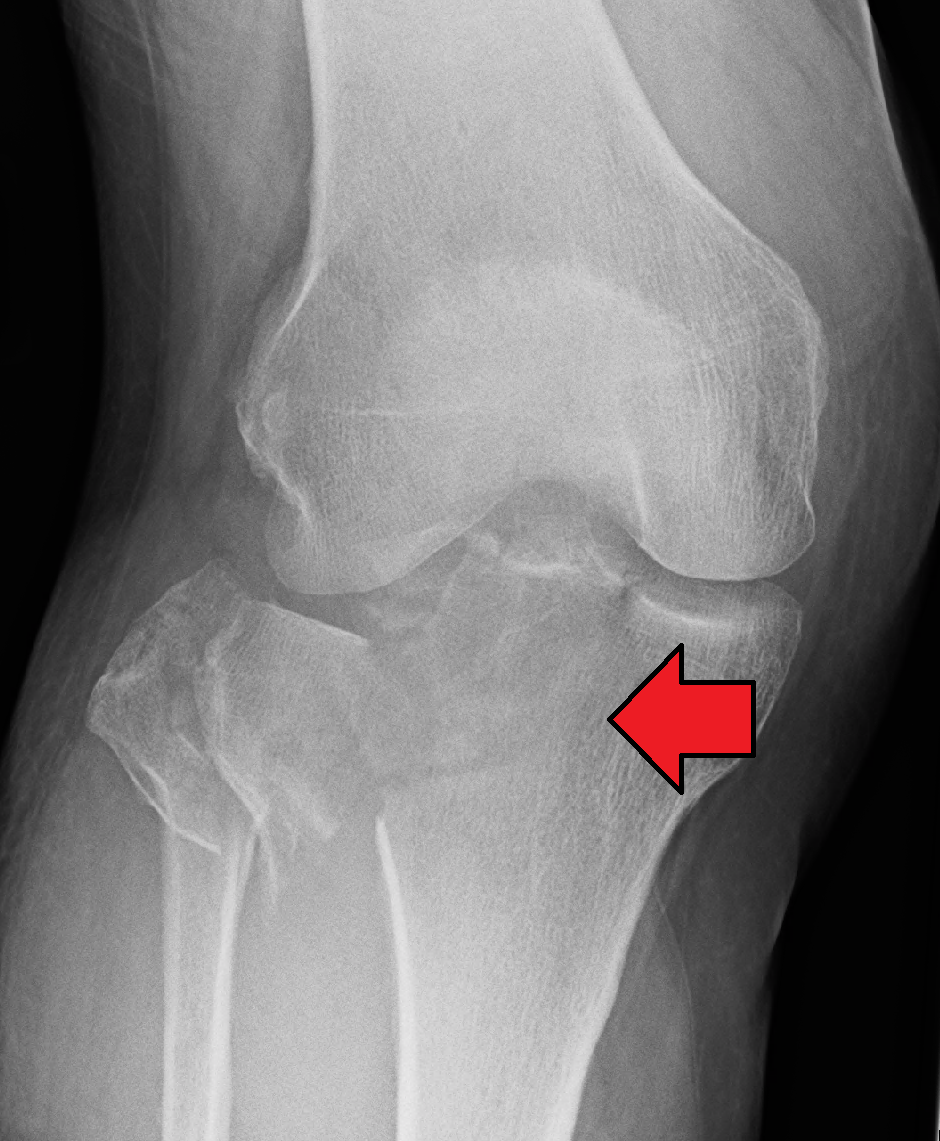
Tibial plateau fracture Other names Fractures of the tibial plateau A severe tibial plateau fracture with an associated fibular head fracture Specialty Orthopedics Symptoms Pain, swelling, decreased ability to move the knee [1] Complications Injury to the artery or nerve, compartment syndrome [1] Types Type I to Type VI [2] Causes Trauma (fall, motor vehicle collision ) [1] Risk factors Osteoporosis , skiing [2] Diagnostic method Suspected based on symptoms, confirmed with X-rays and CT scan [1] Differential diagnosis Patella fracture , fibular fracture , anterior cruciate ligament injury [2] Treatment Surgery, splinting [1] [2] Medication NSAIDs , opioids [1] [2] Prognosis Arthritis is common [2] Frequency ~1% of fractures [2] A tibial plateau fracture is a break of the upper part of the tibia (shinbone) that involves the knee joint . [1] Symptoms include pain, swelling , and a decreased ability to move the knee. [1] People are generally unable to walk. [2] Complication may include injury to the artery or nerve, arthritis , and compartment syndrome . [1] The cause is typically trauma such as a fall or motor vehicle collision . [1] Risk factors include osteoporosis and certain sports such as skiing. [2] Diagnosis is typically suspected based on symptoms and confirmed with X-rays and a CT scan . [1] Some fractures may not be seen on plain X-rays. [2] Pain may be managed with NSAIDs , opioids , and splinting . [1] [2] In those who are otherwise healthy, treatment is generally by surgery. [1] Occasionally, if the bones are well aligned and the ligaments of the knee are intact, people may be treated without surgery. [2] They represent about 1% of broken bones. [2] They occur most commonly in middle aged males and older females. [3] In the 1920s they were called a "fender fracture" due to their association with people being hit by a motor vehicle while walking. [2] Contents 1 Signs and symptoms 2 Cause 3 Mechanism 4 Diagnosis 4.1 Classification 5 Treatment 6 Epidemiology 7 References 8 External links Signs and symptoms [ edit ] Tibial plateau fractures typically presents with knee effusion , swelling of the knee soft tissues and inability to bear weight. ... A serious complication of tibial plateau fractures is compartment syndrome in which swelling causes compression of the nerves and blood vessels inside the leg and may ultimately lead to necrosis or cell death of the leg tissues. [ citation needed ] Cause [ edit ] Tibial plateau fractures may be divided into low energy or high energy fractures. ... Up to 33% of these fractures may be open, often with extensive soft tissue injuries and risk of compartment syndrome. Represents 20% of all tibial plateau fractures.
-
Hypochromic Anemia
Wikipedia
One acquired form of anemia is also known as Faber's syndrome . It may also occur from severe stomach or intestinal bleeding caused by ulcers or medications such as aspirin or bleeding from hemorrhoids . [19] [20] Hereditary forms [ edit ] Hypochromic anemia occurs in patients with hypochromic microcytic anemia with iron overload. ... External links [ edit ] Rare Anemias Foundation v t e Diseases of red blood cells ↑ Polycythemia Polycythemia vera ↓ Anemia Nutritional Micro- : Iron-deficiency anemia Plummer–Vinson syndrome Macro- : Megaloblastic anemia Pernicious anemia Hemolytic (mostly normo- ) Hereditary enzymopathy : Glucose-6-phosphate dehydrogenase deficiency glycolysis pyruvate kinase deficiency triosephosphate isomerase deficiency hexokinase deficiency hemoglobinopathy : Thalassemia alpha beta delta Sickle cell disease / trait Hereditary persistence of fetal hemoglobin membrane : Hereditary spherocytosis Minkowski–Chauffard syndrome Hereditary elliptocytosis Southeast Asian ovalocytosis Hereditary stomatocytosis Acquired AIHA Warm antibody autoimmune hemolytic anemia Cold agglutinin disease Donath–Landsteiner hemolytic anemia Paroxysmal cold hemoglobinuria Mixed autoimmune hemolytic anemia membrane paroxysmal nocturnal hemoglobinuria Microangiopathic hemolytic anemia Thrombotic microangiopathy Hemolytic–uremic syndrome Drug-induced autoimmune Drug-induced nonautoimmune Hemolytic disease of the newborn Aplastic (mostly normo- ) Hereditary : Fanconi anemia Diamond–Blackfan anemia Acquired: Pure red cell aplasia Sideroblastic anemia Myelophthisic Blood tests Mean corpuscular volume normocytic microcytic macrocytic Mean corpuscular hemoglobin concentration normochromic hypochromic Other Methemoglobinemia Sulfhemoglobinemia Reticulocytopenia
-
Tick Paralysis
Wikipedia
In the absence of a tick, the differential diagnosis includes Guillain–Barré syndrome . Early signs of tick poisoning could be a change of an animals' ‘voice’, weakness in the back legs or vomiting. [ citation needed ] Prevention [ edit ] No human vaccine is currently available for any tick-borne disease, except for tick-borne encephalitis . ... External links [ edit ] Classification D ICD - 10 : T63.4 ICD - 9-CM : 989.5 MeSH : D013985 DiseasesDB : 31779 SNOMED CT : 74225001 External resources MedlinePlus : 001359 v t e Poisoning Toxicity Overdose History of poison Inorganic Metals Toxic metals Beryllium Cadmium Lead Mercury Nickel Silver Thallium Tin Dietary minerals Chromium Cobalt Copper Iron Manganese Zinc Metalloids Arsenic Nonmetals Sulfuric acid Selenium Chlorine Fluoride Organic Phosphorus Pesticides Aluminium phosphide Organophosphates Nitrogen Cyanide Nicotine Nitrogen dioxide poisoning CHO alcohol Ethanol Ethylene glycol Methanol Carbon monoxide Oxygen Toluene Pharmaceutical Drug overdoses Nervous Anticholinesterase Aspirin Barbiturates Benzodiazepines Cocaine Lithium Opioids Paracetamol Tricyclic antidepressants Cardiovascular Digoxin Dipyridamole Vitamin poisoning Vitamin A Vitamin D Vitamin E Megavitamin-B 6 syndrome Biological 1 Fish / seafood Ciguatera Haff disease Ichthyoallyeinotoxism Scombroid Shellfish poisoning Amnesic Diarrhetic Neurotoxic Paralytic Other vertebrates amphibian venom Batrachotoxin Bombesin Bufotenin Physalaemin birds / quail Coturnism snake venom Alpha-Bungarotoxin Ancrod Batroxobin Arthropods Arthropod bites and stings bee sting / bee venom Apamin Melittin scorpion venom Charybdotoxin spider venom Latrotoxin / Latrodectism Loxoscelism tick paralysis Plants / fungi Cinchonism Ergotism Lathyrism Locoism Mushrooms Strychnine 1 including venoms , toxins , foodborne illnesses . Category Commons WikiProject v t e Tick-borne diseases and infestations Diseases Bacterial infections Rickettsiales Anaplasmosis Boutonneuse fever Ehrlichiosis ( Human granulocytic , Human monocytotropic , Human E. ewingii infection ) Scrub typhus Spotted fever rickettsiosis Pacific Coast tick fever American tick bite fever rickettsialpox Rocky Mountain spotted fever ) Spirochaete Baggio–Yoshinari syndrome Lyme disease Relapsing fever borreliosis Thiotrichales Tularemia Viral infections Bhanja virus Bourbon virus Colorado tick fever Crimean–Congo hemorrhagic fever Heartland bandavirus Kemerovo tickborne viral fever Kyasanur Forest disease Omsk hemorrhagic fever Powassan encephalitis Severe fever with thrombocytopenia syndrome Tete orthobunyavirus Tick-borne encephalitis Protozoan infections Babesiosis Other diseases Tick paralysis Alpha-gal allergy Southern tick-associated rash illness Infestations Tick infestation Species and bites Amblyomma Amblyomma americanum Amblyomma cajennense Amblyomma triguttatum Dermacentor Dermacentor andersoni Dermacentor variabilis Ixodes Ixodes cornuatus Ixodes holocyclus Ixodes pacificus Ixodes ricinus Ixodes scapularis Ornithodoros Ornithodoros gurneyi Ornithodoros hermsi Ornithodoros moubata Other Rhipicephalus sanguineus Authority control LCCN : sh85135249
-
Albinism
Mayo_clinic
Albinism related to rare hereditary syndromes can occur. For example, Hermansky-Pudlak syndrome includes a form of OCA , as well as bleeding and bruising problems and lung and bowel diseases. Chediak-Higashi syndrome includes a form of OCA , as well as immune problems with recurrent infections, problems with the brain and nerves, bleeding disorders, and other serious issues. ... People with Hermansky-Pudlak or Chediak-Higashi syndromes usually need regular specialized care for medical problems and to prevent complications.AP3D1, TYR, MITF, LYST, SLC45A2, TYRP1, OCA2, AP3B1, HPS1, GPR143, HPS5, LRMDA, HPS4, HPS6, DTNBP1, BLOC1S3, EPG5, CACNA1F, EDNRB, MC1R, FGL1, RAB27A, PAX6, FRMD7, VN1R17P, DCT, MRGPRX1, GPRC6A, OXER1, SLC38A8, GPR151, MRGPRX4, MRGPRX3, TFF1, HPS3, TCOF1, AGFG1, IDS, LGR6, INS, RTEL1, BLOC1S6, LPAR3, PLXNA2, FZD4, GPR166P
-
Epidermolysis Bullosa Simplex With Muscular Dystrophy
Omim
An alternative possibility is that this represents a pleiotropic syndrome. Favoring the latter possibility is the fact that De Weerdt and Castelein (1972) described a family with the same combination in a pattern of autosomal recessive inheritance. ... Laboratory studies showed increased creatine kinase, and electromyography showed a 25% decrement in responses to repetitive stimulation, consistent with a myasthenic syndrome. There were no antiacetylcholine receptor (AChR) antibodies. ... Selcen et al. (2011) reported another African American patient with EBS and a myasthenic syndrome. He developed skin vesicular skin eruptions at age 6 weeks, and muscle weakness and fatigue at age 3 years. ... Muscle studies at age 12 showed necrotic and regenerating fibers, and electromyography at age 15 showed a myasthenic syndrome. Detailed muscle studies in his adult life showed variation in fiber size, type 1 fiber predominance, internal nuclei, and subsarcolemmal calcium deposits.
-
Pimple
Wikipedia
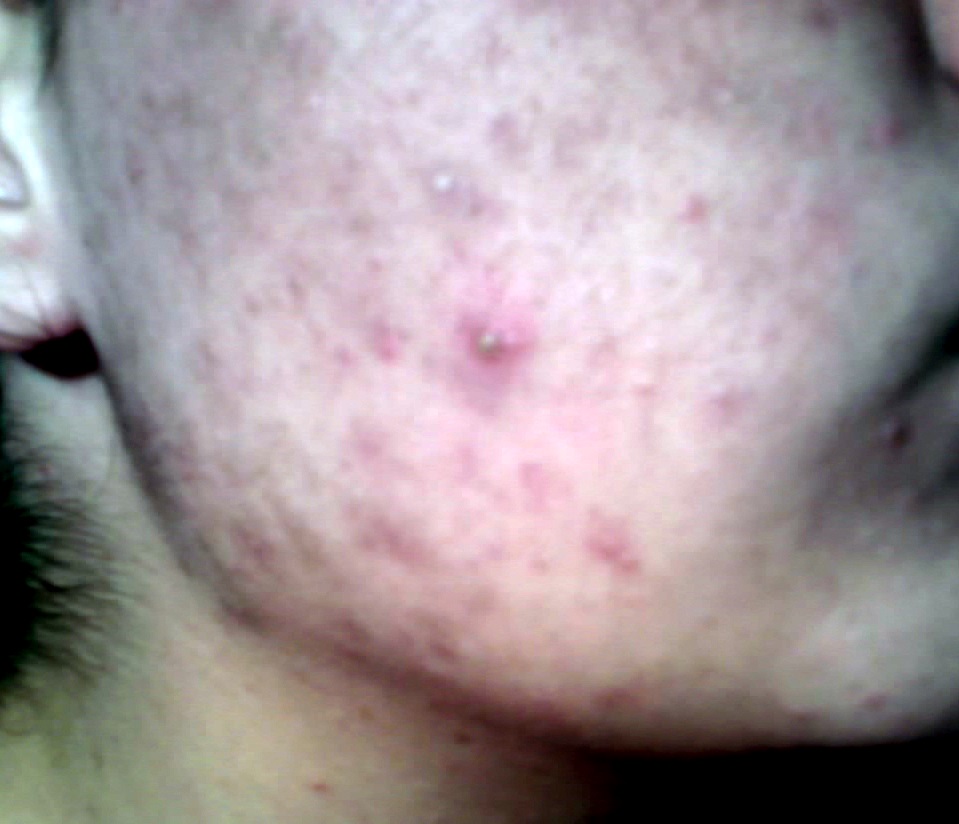
External links Listen to this article (1.6 megabytes) This audio file was created from a revision of this article dated 26 April 2010 ( 2010-04-26 ) , and does not reflect subsequent edits. ( Audio help · More spoken articles ) The dictionary definition of pimple at Wiktionary Classification D ICD - 10 : R23.8 ICD - 9-CM : 709.8 v t e Bacterial skin disease Gram +ve Firmicutes Staphylococcus Staphylococcal scalded skin syndrome Impetigo Toxic shock syndrome Streptococcus Impetigo Cutaneous group B streptococcal infection Streptococcal intertrigo Cutaneous Streptococcus iniae infection Erysipelas / Chronic recurrent erysipelas Scarlet fever Corynebacterium Erythrasma Listeriosis Clostridium Gas gangrene Dermatitis gangrenosa Mycoplasma Erysipeloid of Rosenbach Actinobacteria Mycobacterium-related: Aquarium granuloma Borderline lepromatous leprosy Borderline leprosy Borderline tuberculoid leprosy Buruli ulcer Erythema induratum Histoid leprosy Lepromatous leprosy Leprosy Lichen scrofulosorum Lupus vulgaris Miliary tuberculosis Mycobacterium avium-intracellulare complex infection Mycobacterium haemophilum infection Mycobacterium kansasii infection Papulonecrotic tuberculid Primary inoculation tuberculosis Rapid growing mycobacterium infection Scrofuloderma Tuberculosis cutis orificialis Tuberculosis verrucosa cutis Tuberculous cellulitis Tuberculous gumma Tuberculoid leprosy Cutaneous actinomycosis Nocardiosis Cutaneous diphtheria infection Arcanobacterium haemolyticum infection Group JK corynebacterium sepsis Gram -ve Proteobacteria α: Endemic typhus Epidemic typhus Scrub typhus North Asian tick typhus Queensland tick typhus Flying squirrel typhus Trench fever Bacillary angiomatosis African tick bite fever American tick bite fever Rickettsia aeschlimannii infection Rickettsialpox Rocky Mountain spotted fever Human granulocytotropic anaplasmosis Human monocytotropic ehrlichiosis Flea-borne spotted fever Japanese spotted fever Mediterranean spotted fever Flinders Island spotted fever Verruga peruana Brill–Zinsser disease Brucellosis Cat-scratch disease Oroya fever Ehrlichiosis ewingii infection β: Gonococcemia / Gonorrhea / Primary gonococcal dermatitis Melioidosis Cutaneous Pasteurella hemolytica infection Meningococcemia Glanders Chromobacteriosis infection γ: Pasteurellosis Tularemia Vibrio vulnificus Rhinoscleroma Haemophilus influenzae cellulitis Pseudomonal pyoderma / Pseudomonas hot-foot syndrome / Hot tub folliculitis / Ecthyma gangrenosum / Green nail syndrome Q fever Salmonellosis Shigellosis Plague Granuloma inguinale Chancroid Aeromonas infection ε: Helicobacter cellulitis Other Syphilid Syphilis Chancre Yaws Pinta Bejel Chlamydia infection Leptospirosis Rat-bite fever Lyme disease Lymphogranuloma venereum Unspecified pathogen Abscess Periapical abscess Boil/furuncle Hospital furunculosis Carbuncle Cellulitis Paronychia / Pyogenic paronychia Perianal cellulitis Acute lymphadenitis Pilonidal cyst Pyoderma Folliculitis Superficial pustular folliculitis Sycosis vulgaris Pimple Ecthyma Pitted keratolysis Trichomycosis axillaris Necrotizing fascitis Gangrene Chronic undermining burrowing ulcers Fournier gangrene Elephantiasis nostras Blistering distal dactylitis Botryomycosis Malakoplakia Gram-negative folliculitis Gram-negative toe web infection Pyomyositis Blastomycosis-like pyoderma Bullous impetigo Chronic lymphangitis Recurrent toxin-mediated perineal erythema Tick-borne lymphadenopathy Tropical ulcer v t e Symptoms and signs relating to skin and subcutaneous tissue Disturbances of skin sensation Hypoesthesia Paresthesia Formication Hyperesthesia Hypoalgesia Hyperalgesia Circulation Cyanosis Pallor Livedo Livedo reticularis Flushing Petechia Blanching Edema Peripheral edema Anasarca Other Rash Desquamation Induration Diaphoresis Mass Neck mass Skin Asboe-Hansen sign Auspitz's sign Borsari's sign Braverman's sign Crowe sign Dennie–Morgan fold Darier's sign Fitzpatrick's sign Florid cutaneous papillomatosis Gottron's sign Hutchinson's sign Janeway lesion Kerr's sign Koebner's phenomenon Koplik's spots Leser-Trelat sign Nikolsky's sign Pastia's sign Russell's sign Wickham striae Wolf's isotopic response Munro's microabscess Nails Aldrich-Mees' lines Beau's lines Muehrcke's lines Terry's nails
-
Exertional Rhabdomyolysis
Wikipedia
As the pressure builds in the muscle tissue, the surrounding tissue is crushed against underlying tissue and bone. [12] This is known as compartment syndrome which leads to greater death of the surrounding muscle tissue around the injury. [12] As the muscle dies this will cause pain to radiate from the affected area into the compartmentalized tissue. ... Along with muscle strength weakness associated with the muscles involved from loss of filament interaction. [ citation needed ] Compartment syndrome in muscle Dehydration is a common risk factor for exertional rhabdomyolsis because it causes a reduction of plasma volume during exertion. ... Misirli, Gesthimani. et al. “The Syndrome of Rhabdomyolsis: Complication and Treatment.” ... “Characteristics of patients with chronic exertional compartment syndrome .” Foot & Ankle International 34.10 (2013): 1349-1354.
-
Episodic Ataxia, Type 2
Omim
Imbrici et al. (2005) reported an Indian man with late-onset EA2 beginning at age 61, followed by a progressive cerebellar syndrome at age 62. The patient's medical history included juvenile-onset complex partial seizures and depression but no headaches. ... Mapping In a large family with this form of episodic ataxia, Litt et al. (1994) excluded linkage to 12p where the locus for the episodic ataxia/myokymia syndrome (EA1; 160120) had been mapped. ... Jen et al. (2007) provided a detailed review of the pathophysiology and molecular genetics of known episodic ataxia syndromes. Riant et al. (2010) identified 4 different exonic deletions in the CACNA1A gene in 4 (14%) of 27 patients with episodic ataxia, in whom sequencing analysis was negative for CACNA1A point mutations. ... INHERITANCE - Autosomal dominant HEAD & NECK Ears - Tinnitus Eyes - Ictal and interictal diplopia - Suppression of vestibuloocular reflex - Saccadic smooth pursuit - Gaze-evoked nystagmus - Interictal downbeat nystagmus - Ocular abnormalities often persist between attacks NEUROLOGIC Central Nervous System - Ataxia, episodic - Unsteadiness, episodic - Vertigo - Myotonia - Dysarthria - Migraine headache - Weakness - Paresthesias - Interictal downbeat nystagmus - Interictal vestibular dysfunction - Interictal dystonia may occur later in disease course - Interictal ataxia may occur later in disease course - EEG with paroxysmal activity - Atrophy of cerebellar vermis MISCELLANEOUS - Most common episodic ataxia syndrome - Onset usually in childhood or adolescence - Onset may occur in adulthood - Incomplete penetrance - Progressive ataxia - Episodes last from several hours to days - Frequency of episodes ranges from several per week to several per year - Symptoms precipitated by sudden movement, stress, exertion, exercise, fatigue, caffeine, alcohol, cigarettes - Favorable response of episodic attacks to acetazolamide - Phenotypic overlap with FHM1 ( 141500 ) and SCA6 ( 183086 ) MOLECULAR BASIS - Caused by mutation in the calcium channel, voltage-dependent, P/Q type, alpha 1A subunit gene (CACNA1A, 601011.0005 ) ▲ Close
-
Bile Acid Synthesis Defect, Congenital, 4
Omim
Hanson et al. (1975) noted that the 2 brothers reported by Eyssen et al. (1972) had other congenital anomalies, including frontal bossing, epicanthal folds, and simian creases, perhaps representing another disorder of peroxisomal defect (see, e.g., Zellweger syndrome, 214100; Bove et al., 2000). Hanson et al. (1975) reported 2 sibs with neonatal jaundice, hepatomegaly, and an abnormal bile acid pattern similar to that reported by Eyssen et al. (1972). ... Analysis of bile acids in urine, serum, and bile showed high concentrations of THCA similar to that seen in Zellweger syndrome and in the Alligator mississippiensis.
-
Neuroblastoma
Medlineplus
A tumor in the neck can cause nerve damage known as Horner syndrome, which leads to drooping eyelids, small pupils, decreased sweating, and red skin. ... In rare instances, individuals with neuroblastoma may develop opsoclonus myoclonus syndrome, which causes rapid eye movements and jerky muscle motions.
-
Lyme Disease
Medlineplus
A small percentage of individuals have symptoms that persist months or years after treatment, which is called post-treatment Lyme disease syndrome. A characteristic feature of Lyme disease, and the key feature of early localized infection, is a slowly expanding red rash on the skin (called erythema migrans) at the site of the tick bite; the rash is often bull's-eye shaped. ... Individuals with post-treatment Lyme disease syndrome report ongoing exhaustion (fatigue), muscle and joint achiness, headache, or difficulty concentrating even after treatment with antibiotics, when there is no evidence of the bacteria in the body.CFH, TLR2, FHL1, HPLH1, CXCL13, POLD3, DCN, HLA-DRB1, PLG, HNRNPD, IFNG, EBPL, ELK3, NUP37, UBXN2B, CDK5R1, HSPD1, CCNH, NT5C2, CD8B, TNF, CDK5R2, CDCA5, ATP6V0D1, MLIP, IL6, CXCL8, IL10, PRH1, CPVL, IL17A, JUN, TLR1, LAMC2, RMRP, RHBDL2, PRH2, MNAT1, IL12A, ANXA1, NRSN1, FCN2, ERVK-19, CD14, UPK3B, AK6, ERVK-9, CSF2, ENO2, EPHA5, KARS1, FN1, VHLL, GCHFR, ABCC11, DCTN3, SENP6, SRRM2, BRD4, RHOBTB2, ERVK-24, PHB2, CD300A, CHP1, ERVK-11, TMED10P1, PPP1R14A, ERVK-25, TMED10, STIP1, PTGES3, IFNL1, SORBS1, IL23R, CAP1, PDLIM7, HACD1, H3P7, H3P17, IL37, R3HCC1L, ERVK-18, LINC01672, SQSTM1, ERVK-7, MAK16, ERVK-8, GOLPH3, SELENOK, RAB22A, FAM20C, PNO1, HLP, ERVK-10, H3P6, NELFCD, TLR8, TLR7, EXOSC1, ERVK-21, RBM45, IL22, NOP53, SGSM3, RBMS3, FOXP3, TGFB1, RNMT, IFNB1, HK1, HLA-A, HMGB1, IFIT3, IFNA1, IFNA13, IGH, FGF1, IL1B, IRF7, KRT10, LNPEP, CD180, MAZ, HIF1A, ENO1, MIP, CD48, CALR, CANX, CD1B, CD28, CD38, CD40, CD68, EEF1A1, CCR7, CRP, MAPK14, CTAA1, DAG1, DYNC1H1, MBL2, MMP1, AOC3, TPT1, ABCC8, TRBV20OR9-2, TFPI, BGN, TLR5, TNFRSF1A, TTN, CXCL11, TUFM, VCAM1, ARHGEF5, YBX3, BLZF1, RRP1, SRI, CCL19, MMP9, MAPK1, MMP13, MPZ, COX1, NFKB1, SERPINB6, PRF1, PTBP1, CCL2, PTGS1, PTGS2, RAB5A, RAD51, RRAS, S100A8, H3P29
-
Alcohol Intolerance
Wikipedia
Stuffy nose and skin flushing are the most common symptoms when ingesting alcohol . [2] It may also be characterized as intolerance causing hangover symptoms similar to the "disulfiram-like reaction" of aldehyde dehydrogenase deficiency or chronic fatigue syndrome . Severe pain after drinking alcohol may indicate a more serious condition. [3] If people are intolerant, some nearly non-alcoholic beverages may be a problem, similar to alcohol-containing medications, vinegar , inhalation of alcohol or the vapour of alcohol-containing cleaning agents . ... Sulfonic acids : Acamprosate Religion and alcohol Christian views on alcohol alcohol in the Bible Islam and alcohol History Bratt System Related Index of alcohol-related articles Austrian syndrome Ban on caffeinated alcoholic beverages Brief intervention Gateway drug effect Last call Mood disorder Non-alcoholic fatty liver disease Self-medication Spins Sober companion Sober living houses Sobering center Town drunk Category This genetic disorder article is a stub .
-
B-Cell Immunodeficiency, Distal Limb Anomalies, And Urogenital Malformations
Omim
Description The BILU syndrome comprises humoral immunodeficiency, distal limb anomalies, dysmorphic facial features, and urogenital malformations inherited in an autosomal dominant pattern. The disorder referred to as Hoffman syndrome shows many similar features, suggesting that they represent the same disorder (summary by Hugle et al., 2011).
-
Congenital Disorder Of Glycosylation, Type I/iix
Omim
Huemer et al. (2000) reported a 6-year-old male patient with Budd-Chiari syndrome (600880) and glycoprotein abnormalities associated with CDG Ix. Budd-Chiari syndrome most likely developed after hepatic vein thrombosis caused by coagulation abnormalities resulting from hypoglycosylation and functional impairment of the anticoagulant proteins.
-
Large-Cell Lymphoma
Wikipedia
. ^ Large+cell+lymphoma at the US National Library of Medicine Medical Subject Headings (MeSH) External links [ edit ] Classification D ICD - 9-CM : 200.7 MeSH : D016403 v t e Leukaemias , lymphomas and related disease B cell ( lymphoma , leukemia ) (most CD19 CD20 ) By development/ marker TdT+ ALL ( Precursor B acute lymphoblastic leukemia/lymphoma ) CD5 + naive B cell ( CLL/SLL ) mantle zone ( Mantle cell ) CD22 + Prolymphocytic CD11c+ ( Hairy cell leukemia ) CD79a + germinal center / follicular B cell ( Follicular Burkitt's GCB DLBCL Primary cutaneous follicle center lymphoma ) marginal zone / marginal zone B-cell ( Splenic marginal zone MALT Nodal marginal zone Primary cutaneous marginal zone lymphoma ) RS ( CD15 +, CD30 +) Classic Hodgkin lymphoma ( Nodular sclerosis ) CD20+ ( Nodular lymphocyte predominant Hodgkin lymphoma ) PCDs / PP ( CD38 +/ CD138 +) see immunoproliferative immunoglobulin disorders By infection KSHV ( Primary effusion ) EBV Lymphomatoid granulomatosis Post-transplant lymphoproliferative disorder Classic Hodgkin lymphoma Burkitt's lymphoma HCV Splenic marginal zone lymphoma HIV ( AIDS-related lymphoma ) Helicobacter pylori ( MALT lymphoma ) Cutaneous Diffuse large B-cell lymphoma Intravascular large B-cell lymphoma Primary cutaneous marginal zone lymphoma Primary cutaneous immunocytoma Plasmacytoma Plasmacytosis Primary cutaneous follicle center lymphoma T/NK T cell ( lymphoma , leukemia ) (most CD3 CD4 CD8 ) By development/ marker TdT+ : ALL ( Precursor T acute lymphoblastic leukemia/lymphoma ) prolymphocyte ( Prolymphocytic ) CD30+ ( Anaplastic large-cell lymphoma Lymphomatoid papulosis type A ) Cutaneous MF+variants indolent: Mycosis fungoides Pagetoid reticulosis Granulomatous slack skin aggressive: Sézary disease Adult T-cell leukemia/lymphoma Non-MF CD30 -: Non-mycosis fungoides CD30− cutaneous large T-cell lymphoma Pleomorphic T-cell lymphoma Lymphomatoid papulosis type B CD30 +: CD30+ cutaneous T-cell lymphoma Secondary cutaneous CD30+ large-cell lymphoma Lymphomatoid papulosis type A Other peripheral Hepatosplenic Angioimmunoblastic Enteropathy-associated T-cell lymphoma Peripheral T-cell lymphoma not otherwise specified ( Lennert lymphoma ) Subcutaneous T-cell lymphoma By infection HTLV-1 ( Adult T-cell leukemia/lymphoma ) NK cell / (most CD56 ) Aggressive NK-cell leukemia Blastic NK cell lymphoma T or NK EBV ( Extranodal NK-T-cell lymphoma / Angiocentric lymphoma ) Large granular lymphocytic leukemia Lymphoid+ myeloid Acute biphenotypic leukaemia Lymphocytosis Lymphoproliferative disorders ( X-linked lymphoproliferative disease Autoimmune lymphoproliferative syndrome ) Leukemoid reaction Diffuse infiltrative lymphocytosis syndrome Cutaneous lymphoid hyperplasia Cutaneous lymphoid hyperplasia with bandlike and perivascular patterns with nodular pattern Jessner lymphocytic infiltrate of the skin General Hematological malignancy leukemia Lymphoproliferative disorders Lymphoid leukemiasBCL2, BCL6, HLA-DRB1, CHEK2, RAD54B, BCL10, FPGS, RAD54L, EPHX1, MTHFR, CYP2E1, CSF3, CSF2, IFNA2, TYMS, PRF1, CBS, CASP10, TFRC, SHMT1, BHMT, TNFRSF8, ALK, PDLIM7, PTPRC, NCAM1, ADA, BRAF, CHP1, NDRG2, H3P19, TNF, LOC102724971, LOC102723407, TP53, SLC35B2, NRSN1, ATAD1, VIM, TPPP, RTEL1, RFXANK, SCAPER, IGHV3-52, HDAC9, SIRPB1, CCT4, TMED2, SOX10, STAT3, MYC, SOD2, HSPA4, BTK, CASP3, CD9, CDKN2A, CLTA, ADAM3A, DCK, EZH2, NR3C1, GUCA1B, GUCY2D, HNMT, HSPA8, RNASEL, IFNB1, IGH, IL1B, IL4, CXCL8, IL10, IRF4, LIF, LMNB1, SERPINB2, PLG, RARA, H3P10
-
Spermatogenic Failure 6
Omim
Globozoospermia (also called round-headed spermatozoa) is a human infertility syndrome caused by spermatogenesis defects (Lalonde et al., 1988, Singh, 1992). ... Florke-Gerloff et al. (1984) suggested that the round-headed spermatozoa syndrome is polygenic in its inheritance.
-
Autism, Susceptibility To, 18
Omim
'Autism spectrum disorder,' sometimes referred to as ASD, is a broader phenotype encompassing the less severe disorders Asperger syndrome (see ASPG1; 608638) and pervasive developmental disorder, not otherwise specified (PDD-NOS). ... Mental retardation coexists in approximately two-thirds of individuals with ASD, except for Asperger syndrome, in which mental retardation is conspicuously absent (Jones et al., 2008).
-
Geriatric Trauma
Wikipedia
ISBN 9781455706051 . v t e Trauma Principles Polytrauma Major trauma Traumatology Triage Resuscitation Trauma triad of death Assessment Clinical prediction rules Revised Trauma Score Injury Severity Score Abbreviated Injury Scale NACA score Investigations Diagnostic peritoneal lavage Focused assessment with sonography for trauma Management Principles Advanced trauma life support Trauma surgery Trauma center Trauma team Damage control surgery Early appropriate care Procedures Resuscitative thoracotomy Pathophysiology Injury MSK Bone fracture Joint dislocation Degloving Soft tissue injury Resp Flail chest Pneumothorax Hemothorax Diaphragmatic rupture Pulmonary contusion Cardio Internal bleeding Thoracic aorta injury Cardiac tamponade GI Blunt kidney trauma Ruptured spleen Neuro Penetrating head injury Traumatic brain injury Intracranial hemorrhage Mechanism Blast injury Blunt trauma Burn Penetrating trauma Crush injury Stab wound Ballistic trauma Electrocution Region Abdominal trauma Chest trauma Facial trauma Head injury Spinal cord injury Demographic Geriatric trauma Pediatric trauma Complications Posttraumatic stress disorder Wound healing Acute lung injury Crush syndrome Rhabdomyolysis Compartment syndrome Contracture Volkmann's contracture Embolism air fat Chronic traumatic encephalopathy Subcutaneous emphysema